Submitted:
08 April 2024
Posted:
09 April 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Mechanism PBD in Reducing ISR and ST
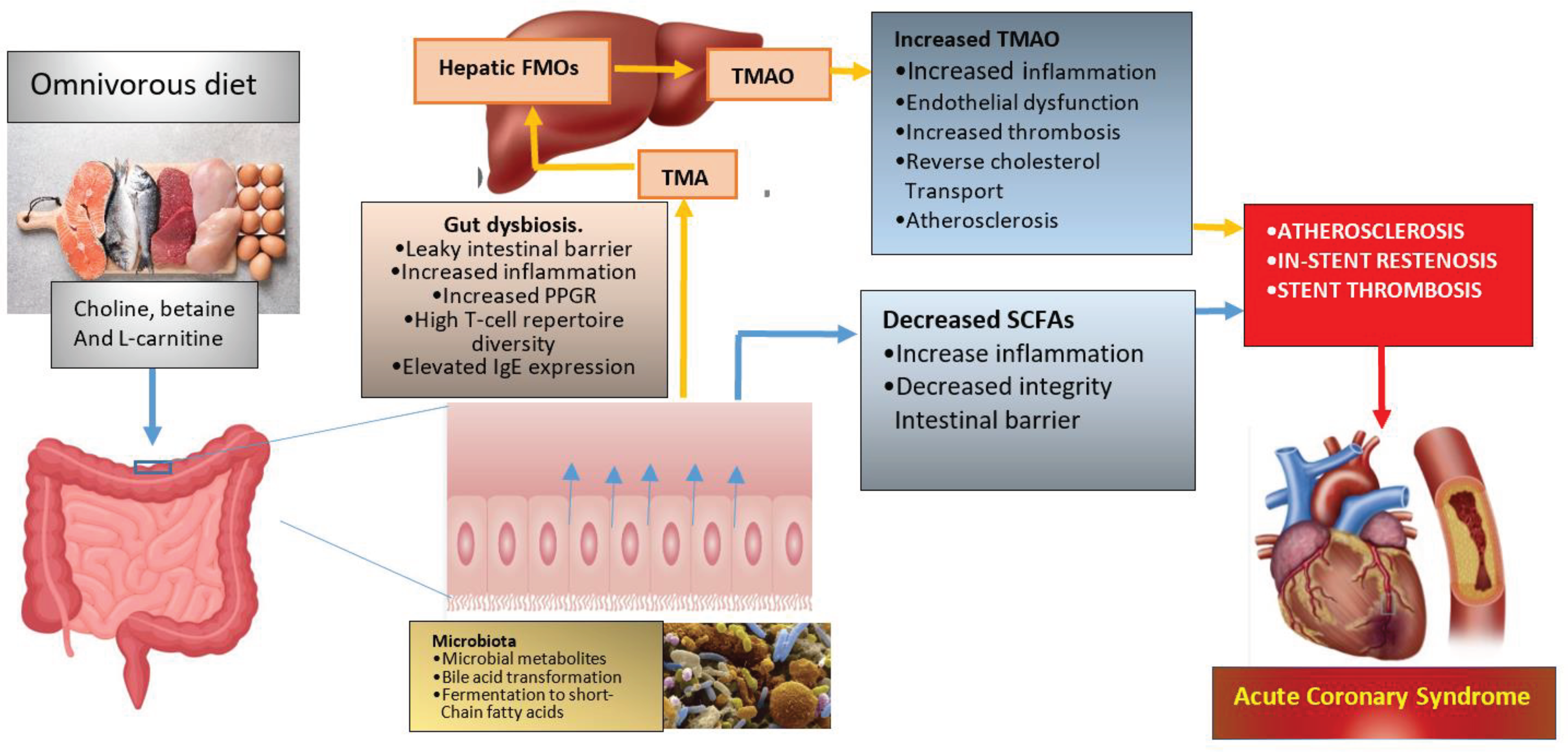
2.1. The Most Important Mechanism of How PBD Decreases the Risk of Atherosclerosis, ISR, and ST
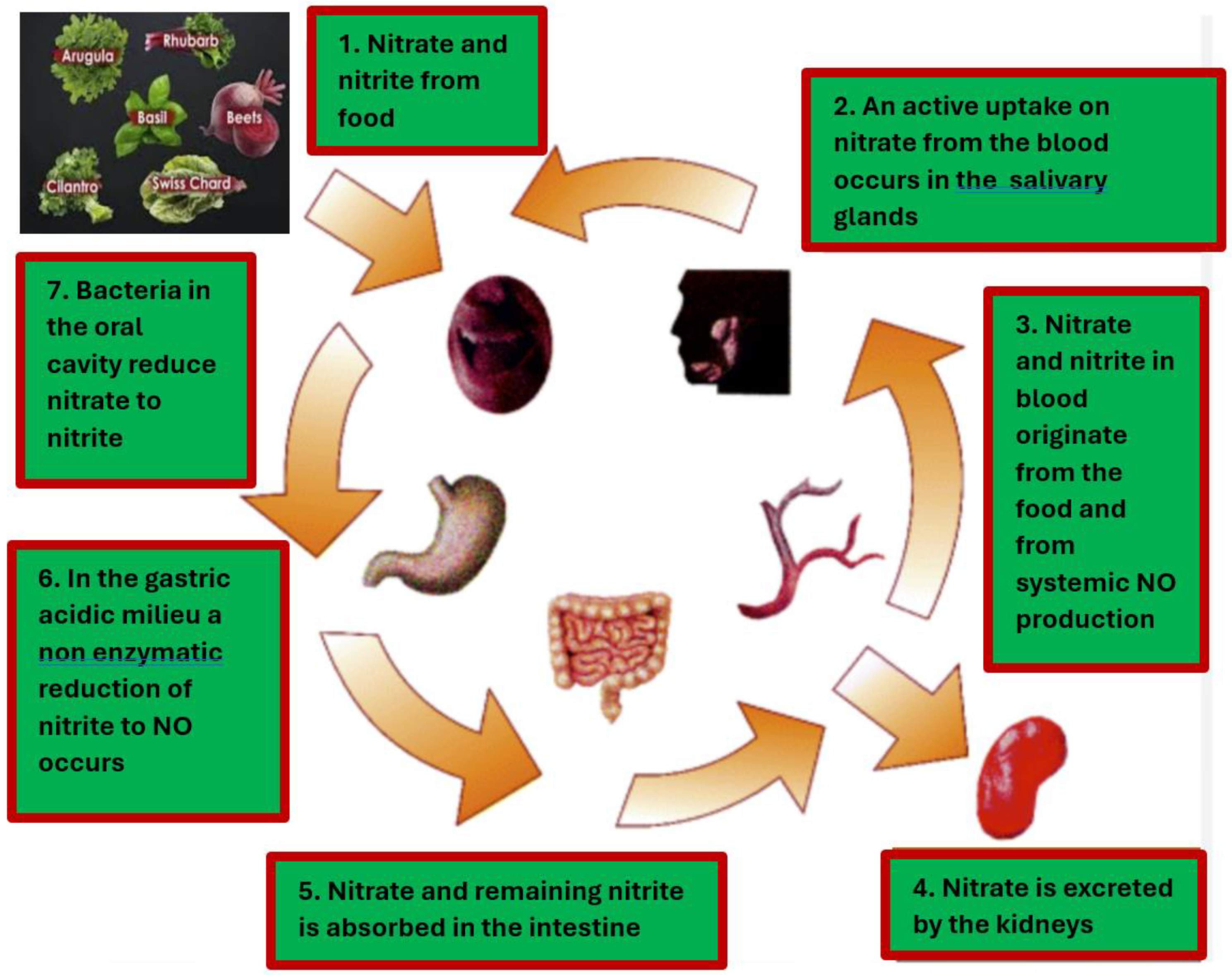
2.2. Mechanism of Nitric Oxide (NO) in Reducing Atherosclerosis, ISR, and ST
2.3. PBD as an Anti-Inflammation, Antioxidant, and a Crucial Factor in Repairing Endothelial Dysfunction
2.4. PBD Decreases Systemic Allergic Reactions and May Prevent Stent Hypersensitivity/Allergic Reaction
2.5. The Connection between Microbiota and ISR- ST
2.6. Caloric Restriction Is an Essential Factor in Combating Inflammation
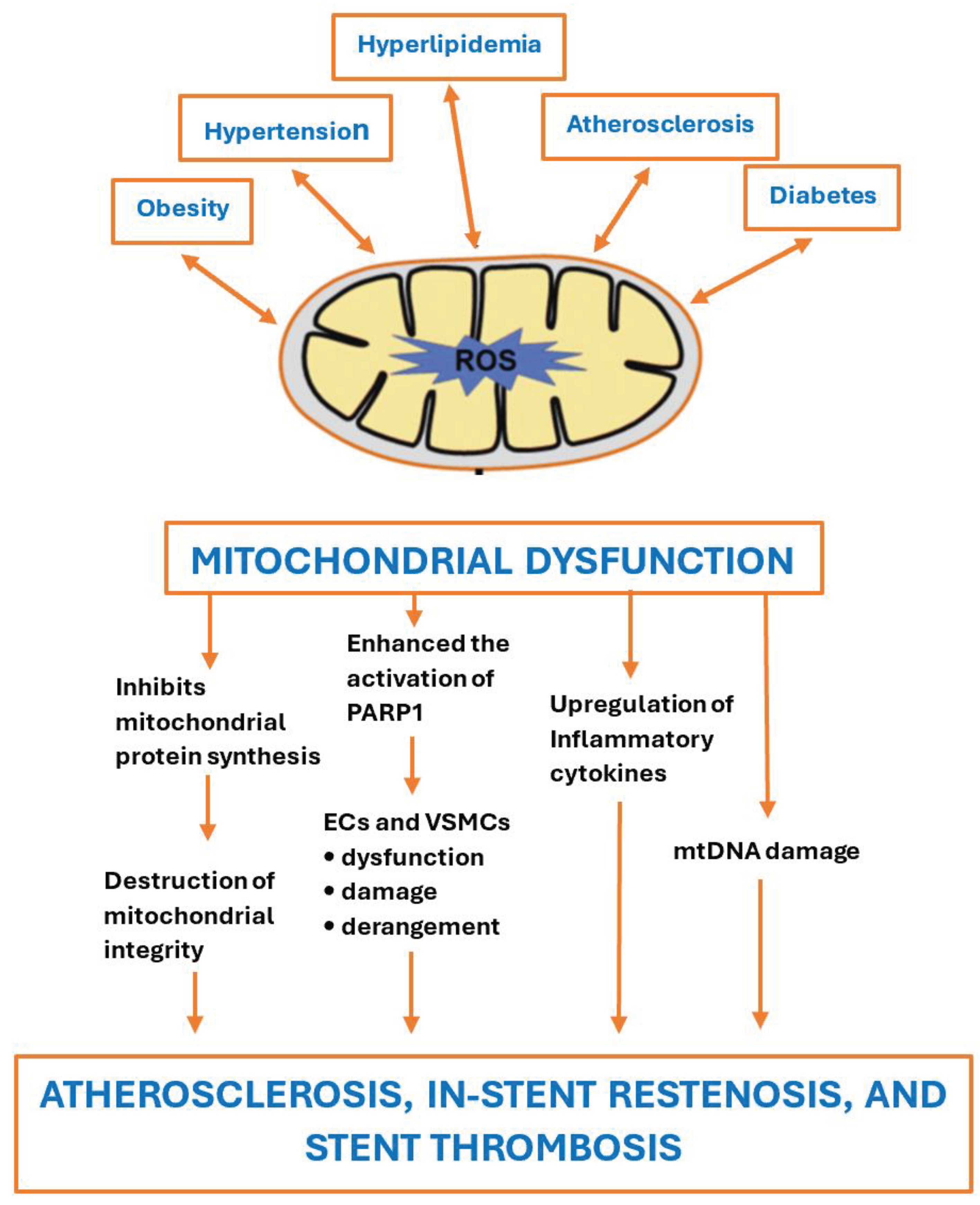
2.7. The Role of PBD as Mitochondrial Protectors
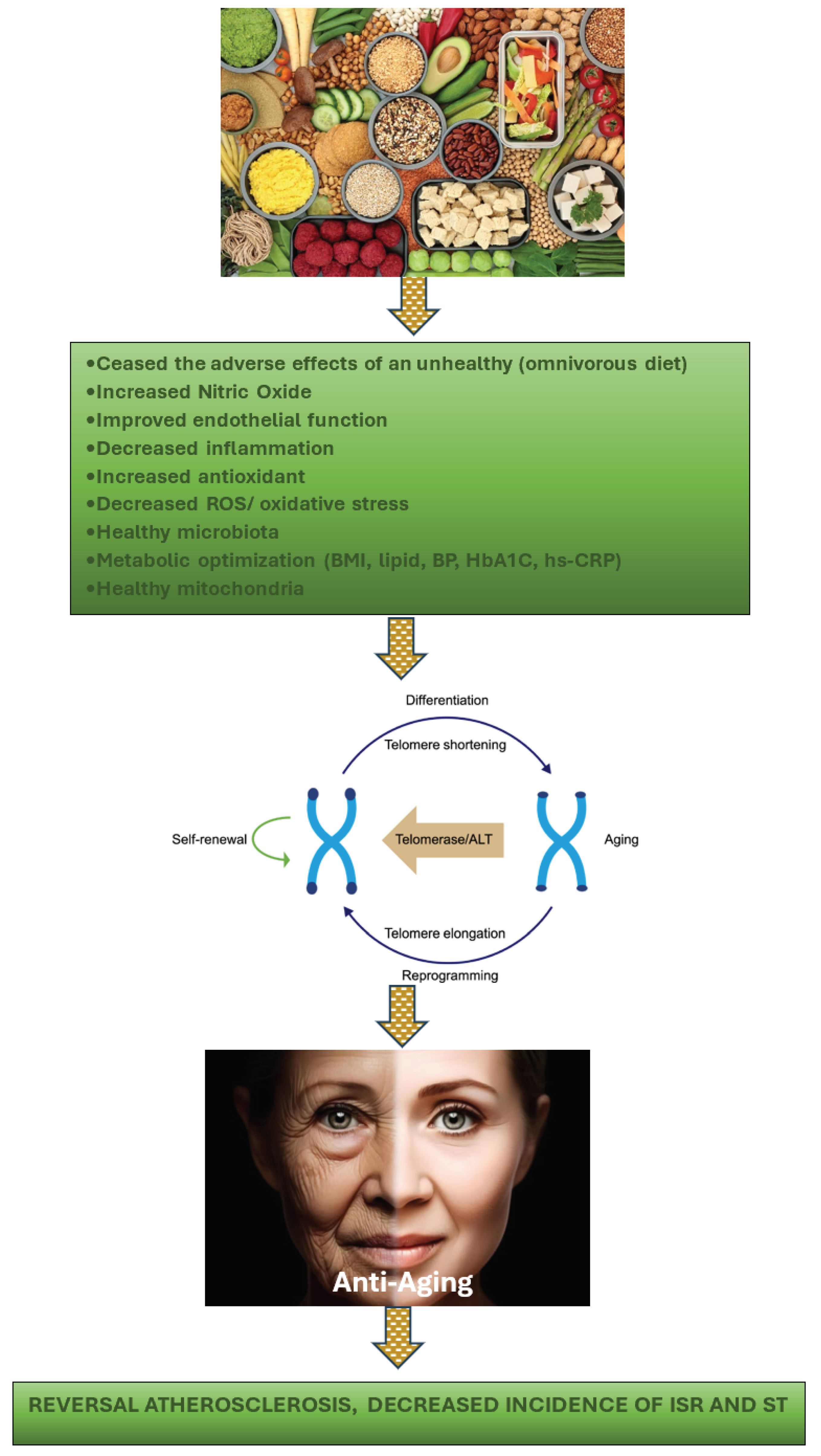
2.8. Potential Benefits of Telomere Manipulation in Atherosclerosis, ISR, and ST Utilizing PBD
3. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflict of Interests
References
- Mohamad, T.; Jyotsna, F.; Farooq, U.; et al. Individualizing Medicinal Therapy Post Heart Stent Implantation: Tailoring for Patient Factors. Cureus. 2023, 15, e43977. [Google Scholar] [CrossRef] [PubMed]
- Klein, L.W.; Nathan, S.; Maehera, A.; et al. SCAI Expert Consensus Statement on Management of In-Stent Restenosis and Stent Thrombosis. JSCAI 2023, 2, 100971. [Google Scholar] [CrossRef]
- Pelliccia, F.; Zimarino, M.; Niccoli, G.; et al. In-stent restenosis after percutaneous coronary intervention: emerging knowledge on biological pathways. Eur Heart J Open. 2023, 3, oead083. [Google Scholar] [CrossRef] [PubMed]
- Wolf, D.; Ley, K. Immunity and Inflammation in Atherosclerosis. Circ Res. 2019, 124, 315–327. [Google Scholar] [CrossRef] [PubMed]
- Aoki, J.; Tanabe, K. Mechanisms of drug-eluting stent restenosis. Cardiovasc Interv Ther. 2021, 36, 23–29. [Google Scholar] [CrossRef] [PubMed]
- Zheng, P.G.; Chen, P.; Wang, L.J.; et al. The association of the systemic immune-inflammation index and stent thrombosis in myocardial infarction patients after coronary stent implantation-a retrospectively study. J Thorac Dis. 2023, 15, 1726–1733. [Google Scholar] [CrossRef]
- Condello, F.; Spaccarotella, C.; Sorrentino, S.; et al. Stent Thrombosis and Restenosis with Contemporary Drug-Eluting Stents: Predictors and Current Evidence. J Clin Med. 2023, 12, 1238. [Google Scholar] [CrossRef]
- Khalid, W.; Arshad, M.S.; Ranjha, M.M.A.N.; et al. Functional constituents of plant-based foods boost immunity against acute and chronic disorders. Open Life Sci. 2022, 17, 1075–1093. [Google Scholar] [CrossRef]
- Peña-Jorquera, H.; Cid-Jofré, V.; Landaeta-Díaz, L.; et al. Plant-Based Nutrition: Exploring Health Benefits for Atherosclerosis, Chronic Diseases, and Metabolic Syndrome—A Comprehensive Review. Nutrients 2023, 15, 3244. [Google Scholar] [CrossRef]
- Salehin, S.; Rasmussen, P.; Mai, S.; et al. Plant Based Diet and Its Effect on Cardiovascular Disease. Int J Environ Res Public Health. 2023, 20, 3337. [Google Scholar] [CrossRef]
- Koutentakis, M.; Surma, S.; Rogula, S.; et al. The Effect of a Vegan Diet on the Cardiovascular System. J Cardiovasc Dev Dis. 2023, 10, 94. [Google Scholar] [CrossRef] [PubMed]
- Tucci, M.; Marino, M.; Martini, D.; et al. Plant-Based Foods and Vascular Function: A Systematic Review of Dietary Intervention Trials in Older Subjects and Hypothesized Mechanisms of Action. Nutrients. 2022, 14, 2615. [Google Scholar] [CrossRef] [PubMed]
- Islam, S.U.; Ahmed, M.B.; Ahsan, H.; et al. Recent Molecular Mechanisms and Beneficial Effects of Phytochemicals and Plant-Based Whole Foods in Reducing LDL-C and Preventing Cardiovascular Disease. Antioxidants (Basel). 2021, 10, 784. [Google Scholar] [CrossRef] [PubMed]
- Mehta, P.; Tawfeeq, S.; Padte, S.; et al. Plant-based diet and its effect on coronary artery disease: A narrative review. World J Clin Cases. 2023, 11, 4752–4762. [Google Scholar] [CrossRef] [PubMed]
- Bruns, A.; Greupner, T.; Nebl, J.; et al. Plant-based diets and cardiovascular risk factors: a comparison of flexitarians, vegans and omnivores in a cross-sectional study. BMC Nutr 2024, 10, 29. [Google Scholar] [CrossRef] [PubMed]
- Di Sotto, A.; Vitalone, A.; Di Giacomo, S. Plant-Derived Nutraceuticals and Immune System Modulation: An Evidence-Based Overview. Vaccines (Basel). 2020, 8, 468. [Google Scholar] [CrossRef] [PubMed]
- Xu, K.; Kh Al-ani, M.; Pan, X.; et al. Plant-Derived Products for Treatment of Vascular Intima Hyperplasia Selectively Inhibit Vascular Smooth Muscle Cell Functions. Evidence-Based Complementary and Alternative Medicine 2018, 2018, 3549312. [Google Scholar] [CrossRef]
- Monsalve, B.; Concha-Meyer, A.; Palomo, I.; et al. Mechanisms of Endothelial Protection by Natural Bioactive Compounds from Fruit and Vegetables. An Acad Bras Cienc. 2017, 89 (1 Suppl 0), 615–633. [Google Scholar] [CrossRef] [PubMed]
- Aquila, G.; Marracino, L.; Martino, V.; et al. The Use of Nutraceuticals to Counteract Atherosclerosis: The Role of the Notch Pathway. Oxid Med Cell Longev. 2019, 2019, 5470470. [Google Scholar] [CrossRef]
- Moss, J.; Dipak, R. Nutraceutical therapies for atherosclerosis. Nature Reviews Cardiology 2016, 13, 513–532. [Google Scholar] [CrossRef]
- Wei, T.; Liu, J.; Zhang, D.; et al. The Relationship Between Nutrition and Atherosclerosis. Front Bioeng Biotechnol. 2021, 9, 635504. [Google Scholar] [CrossRef] [PubMed]
- Mitu, O.; Cirneala, I.A.; Lupsan, A.I.; et al. The Effect of Vitamin Supplementation on Subclinical Atherosclerosis in Patients without Manifest Cardiovascular Diseases: Never-ending Hope or Underestimated Effect? Molecules 2020, 25, 1717. [Google Scholar] [CrossRef] [PubMed]
- Li, M.; Hou, J.; Gu, X.; et al. Incidence and risk factors of in-stent restenosis after percutaneous coronary intervention in patients from southern China. Eur J Med Res. 2022, 27, 12. [Google Scholar] [CrossRef] [PubMed]
- Rohman, M.S.; Waranugraha, Y.; Masbuchin, A.N.; et al. Coronary In-Stent Restenosis Predictors following Drug-Eluting Stent Implantation: A Meta-Analysis Study. J. Vasc. Dis. 2023, 2, 266–281. [Google Scholar] [CrossRef]
- Saleh, A.; Hammoudeh, A.; Tabbalat, R.; et al. Incidence and prognosis of stent thrombosis following percutaneous coronary intervention in Middle Eastern patients: The First Jordanian Percutaneous Coronary Intervention Registry (JoPCR1). Ann Saudi Med. 2016, 36, 17–22. [Google Scholar] [CrossRef] [PubMed]
- Marchio, P.; Guerra-Ojeda, S.; Vila, J.M.; et al. Targeting Early Atherosclerosis: A Focus on Oxidative Stress and Inflammation. Oxid Med Cell Longev. 2019, 2019, 8563845. [Google Scholar] [CrossRef]
- Adarsh Ray, Krushna Ch. Maharana.; et al. Endothelial dysfunction and its relation in different disorders: Recent update. Health Sciences Review 2023, 7, 100084. [CrossRef]
- Almeida, C.; Barata, P.; Fernandes, R. The influence of gut microbiota in cardiovascular diseases-a brief review. Porto Biomed J. 2021, 6, e106. [Google Scholar] [CrossRef] [PubMed]
- Pollicino, F.; Veronese, N.; Dominguez, L.J.; et al. Mediterranean diet and mitochondria: New findings. Exp Gerontol. 2023, 176, 112165. [Google Scholar] [CrossRef] [PubMed]
- Cinegaglia, N.; Antoniazzi, L.; Rosa, D.; et al. Shortening telomere is associated with subclinical atherosclerosis biomarker in omnivorous but not in vegetarian healthy men. Aging (Albany NY). 2019, 11, 5070–5080. [Google Scholar] [CrossRef]
- Napoli, C.; de Nigris, F.; Williams-Ignarro, S.; et al. Nitric oxide and atherosclerosis: an update. Nitric Oxide. 2006, 15, 265–79. [Google Scholar] [CrossRef] [PubMed]
- Naseem, K.M. The role of nitric oxide in cardiovascular diseases. Mol Aspects Med. 2005, 2, 33–65. [Google Scholar] [CrossRef] [PubMed]
- Torregrossa, A.C.; Aranke, M.; Bryan, N.S. Nitric Oxide and geriatric: Implications in diagnostics and treatment of the elderly. J Geriatr Cardiol. 2011, 8, 230–242. [Google Scholar] [PubMed]
- Babateen, A.M.; Shannon, O.M.; Mathers, J.C.; et al. Validity and reliability of test strips for the measurement of salivary nitrite concentration with and without the use of mouthwash in healthy adults. Nitric Oxide. 2019, 91, 15–22. [Google Scholar] [CrossRef] [PubMed]
- Salehzadeh, H.; Maleki, A.; Rezaee, R.; et al. The nitrate content of fresh and cooked vegetables and their health-related risks. PLoS One. 2020, 15, e0227551. [Google Scholar] [CrossRef] [PubMed]
- Neufingerl, N.; Eilander, A. Nutrient Intake and Status in Adults Consuming Plant-Based Diets Compared to Meat-Eaters: A Systematic Review. Nutrients. 2021, 14, 29. [Google Scholar] [CrossRef] [PubMed]
- Rajendran, S.; Shen, X.; Glawe, J.; et al. Nitric Oxide and Hydrogen Sulfide Regulation of Ischemic Vascular Growth and Remodeling. Compr Physiol. 2019, 9, 1213–1247. [Google Scholar] [CrossRef] [PubMed]
- Rao, J.; Pan Bei, H.; Yang, Y.; et al. Nitric Oxide-Producing Cardiovascular Stent Coatings for Prevention of Thrombosis and Restenosis. Front Bioeng Biotechnol. 2020, 8, 578. [Google Scholar] [CrossRef] [PubMed]
- Kabirian, F.; Brouki Milan, P.; Zamanian, A.; et al. Nitric oxide-releasing vascular grafts: A therapeutic strategy to promote angiogenic activity and endothelium regeneration. Acta Biomater. 2019, 92, 82–91. [Google Scholar] [CrossRef] [PubMed]
- Ornish, D.; Scherwitz, L.W.; Billings, J.H.; et al. Intensive lifestyle changes for reversal of coronary heart disease. JAMA. 1998, 280, 2001–7. [Google Scholar] [CrossRef] [PubMed]
- Esselstyn, C.B., Jr.; Gendy, G; Doyle, J; et al. A way to reverse CAD? J Fam Pract. 2014, 63, 356–364b. [Google Scholar] [PubMed]
- Rose, Stewart D. A Comprehensive Review of the Prevention and Treatment of Heart Disease with a Plant-Based Diet. Journal of Cardiology & Cardiovascular Therapy 2018. n. pag. [Google Scholar]
- Bilal, M.; Ashraf, S.; Zhao, X. Dietary Component-Induced Inflammation and Its Amelioration by Prebiotics, Probiotics, and Synbiotics. Front Nutr. 2022, 9, 931458. [Google Scholar] [CrossRef] [PubMed]
- Upadhyay, S.; Dixit, M. Role of Polyphenols and Other Phytochemicals on Molecular Signaling. Oxid Med Cell Longev. 2015, 2015, 504253. [Google Scholar] [CrossRef] [PubMed]
- Wu, Y.T.; Chen, L.; Tan, Z.B.; et al. Luteolin Inhibits Vascular Smooth Muscle Cell Proliferation and Migration by Inhibiting TGFBR1 Signaling. Front Pharmacol. 2018, 9, 1059. [Google Scholar] [CrossRef]
- Naruko, T.; Ueda, M.; Ehara, S.; et al. Persistent high levels of plasma oxidized low-density lipoprotein after acute myocardial infarction predict stent restenosis. Arterioscler Thromb Vasc Biol. 2006, 26, 877–883. [Google Scholar] [CrossRef] [PubMed]
- Batty, M.; Bennett, M.R.; Yu, E. The Role of Oxidative Stress in Atherosclerosis. Cells. 2022, 11, 3843. [Google Scholar] [CrossRef] [PubMed]
- Ganjali, S.; Mansouri, A.; Abbasifard, M.; et al. Association between Oxidative Burden and Restenosis: A Case-Control Study. Oxid Med Cell Longev. 2022, 2022, 3577761. [Google Scholar] [CrossRef] [PubMed]
- Li, P.; Ma, X.; Huang, G. Understanding thrombosis: the critical role of oxidative stress. Hematology 2024, 29, 2301633. [Google Scholar] [CrossRef] [PubMed]
- Chioncel, V.; Andrei, C.L.; Brezeanu, R.; et al. Some Perspectives on Hypersensitivity to Coronary Stents. Int J Gen Med. 2021, 14, 4327–4336. [Google Scholar] [CrossRef]
- Rakha, A.; Umar, N.; Rabail, R.; et al. Anti-inflammatory and anti-allergic potential of dietary flavonoids: A review. Biomed Pharmacother. 2022; 156, 113945. [Google Scholar] [CrossRef] [PubMed]
- Zhang, P. The Role of Diet and Nutrition in Allergic Diseases. Nutrients. 2023, 15, 3683. [Google Scholar] [CrossRef] [PubMed]
- Mehta, P.; Tawfeeq, S.; Padte, S.; et al. Plant-based diet and its effect on coronary artery disease: A narrative review. World J Clin Cases. 2023, 11, 4752–4762. [Google Scholar] [CrossRef] [PubMed]
- Tan, Y.; Zhou, J.; Liu, C.; et al. Association Between Plasma Trimethylamine N-oxide and Neoatherosclerosis in Patients With Very Late Stent Thrombosis. Can J Cardiol. 2020, 36, 1252–1260. [Google Scholar] [CrossRef] [PubMed]
- Kumar, A.; Chidambaram, V.; Mehta, J.L. Vegetarianism, microbiota, and cardiovascular health: looking back, and forward. Eur J Prev Cardiol. 2022, 29, 1895–1910. [Google Scholar] [CrossRef] [PubMed]
- Shen, X.; Li, L.; Sun, Z.; Zang, G.; et al. Gut Microbiota and Atherosclerosis-Focusing on the Plaque Stability. Front Cardiovasc Med. 2021, 8, 668532. [Google Scholar] [CrossRef] [PubMed]
- Peña-Jorquera, H.; Cid-Jofré, V.; Landaeta-Díaz, L.; et al. Plant-Based Nutrition: Exploring Health Benefits for Atherosclerosis, Chronic Diseases, and Metabolic Syndrome-A Comprehensive Review. Nutrients. 2023, 15, 3244. [Google Scholar] [CrossRef]
- Craig, W.J.; Mangels, A.R.; Fresán, U.; et al. The Safe and Effective Use of Plant-Based Diets with Guidelines for Health Professionals. Nutrients. 2021, 13, 4144. [Google Scholar] [CrossRef] [PubMed]
- Desai, D.; Desai, A.; Jamil, A.; et al. Re-defining the Gut Heart Axis: A Systematic Review of the Literature on the Role of Gut Microbial Dysbiosis in Patients With Heart Failure. Cureus. 2023, 15, e34902. [Google Scholar] [CrossRef] [PubMed]
- Bui, T.V.A.; Hwangbo, H.; Lai, Y.; et al. The Gut-Heart Axis: Updated Review for The Roles of Microbiome in Cardiovascular Health. Korean Circ J. 2023, 53, 499–518. [Google Scholar] [CrossRef]
- Sørensen, T.I.A.; Martinez, A.R.; Jørgensen, T.S.H. Epidemiology of Obesity. Handb Exp Pharmacol. 2022, 74, 3–27. [Google Scholar] [CrossRef] [PubMed]
- Kökten, T.; Hansmannel, F.; Ndiaye, N.C.; et al. Calorie Restriction as a New Treatment of Inflammatory Diseases. Adv Nutr. 2021, 12, 1558–1570. [Google Scholar] [CrossRef]
- Perry, C.A.; Gadde, K.M. The Role of Calorie Restriction in the Prevention of Cardiovascular Disease. Curr Atheroscler Rep. 2022, 24, 235–242. [Google Scholar] [CrossRef] [PubMed]
- Samad, F.; Ruf, W. Inflammation, obesity, and thrombosis. Blood. 2013, 122, 3415–22. [Google Scholar] [CrossRef] [PubMed]
- Yang, X.; Yang, Y.; Guo, J.; et al. Targeting the epigenome in in-stent restenosis: from mechanisms to therapy. Mol Ther Nucleic Acids. 2021, 23, 1136–1160. [Google Scholar] [CrossRef] [PubMed]
- Zhai, J.; Kongsberg, W.H.; Pan, Y.; et al. Caloric restriction induced epigenetic effects on aging. Front Cell Dev Biol. 2023, 10, 1079920. [Google Scholar] [CrossRef]
- Marchi, S.; Guilbaud, E.; Tait, S.W.G.; et al. Mitochondrial control of inflammation. Nat Rev Immunol. 2023, 23, 159–173. [Google Scholar] [CrossRef] [PubMed]
- Ciccarelli, G.; Conte, S.; Cimmino, G.; et al. Mitochondrial Dysfunction: The Hidden Player in the Pathogenesis of Atherosclerosis? Int J Mol Sci. 2023, 24, 1086. [Google Scholar] [CrossRef]
- Shemiakova, T.; Ivanova, E.; Wu, W.K.; et al. Atherosclerosis as Mitochondriopathy: Repositioning the Disease to Help Finding New Therapies. Front Cardiovasc Med. 2021, 8, 660473. [Google Scholar] [CrossRef]
- Qu, K.; Yan, F.; Qin, X.; et al. Mitochondrial dysfunction in vascular endothelial cells and its role in atherosclerosis. Front Physiol. 2022, 13, 1084604. [Google Scholar] [CrossRef]
- Suárez-Rivero, J.M.; Pastor-Maldonado, C.J.; Povea-Cabello, S.; et al. From Mitochondria to Atherosclerosis: The Inflammation Path. Biomedicines. 2021, 9, 258. [Google Scholar] [CrossRef]
- Niyazov, D.M.; Kahler, S.G.; Frye, R.E. Primary Mitochondrial Disease and Secondary Mitochondrial Dysfunction: Importance of Distinction for Diagnosis and Treatment. Mol Syndromol. 2016, 7, 122–137. [Google Scholar] [CrossRef]
- Pollicino, F.; Veronese, N.; Dominguez, L.J.; et al. Mediterranean diet and mitochondria: New findings. Exp Gerontol. 2023, 176, 112165. [Google Scholar] [CrossRef] [PubMed]
- Khalil, M.; Shanmugam, H.; Abdallah, H.; et al. The Potential of the Mediterranean Diet to Improve Mitochondrial Function in Experimental Models of Obesity and Metabolic Syndrome. Nutrients. 2022, 14, 3112. [Google Scholar] [CrossRef] [PubMed]
- Maluchenko, N.V.; Feofanov, A.V.; Studitsky, V.M. PARP-1-Associated Pathological Processes: Inhibition by Natural Polyphenols. Int J Mol Sci. 2021, 22, 11441. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- D'Angelo, S. Diet and Aging: The Role of Polyphenol-Rich Diets in Slow Down the Shortening of Telomeres: A Review. Antioxidants (Basel). 2023, 12, 2086. [Google Scholar] [CrossRef]
- Herrmann, W.; Herrmann, M. The Importance of Telomere Shortening for Atherosclerosis and Mortality. J Cardiovasc Dev Dis. 2020, 7, 29. [Google Scholar] [CrossRef]
- Liu, S.; Nong, W.; Ji, L.; et al. The regulatory feedback of inflammatory signaling and telomere/telomerase complex dysfunction in chronic inflammatory diseases. Exp Gerontol. 2023, 174, 112132. [Google Scholar] [CrossRef] [PubMed]
- Crous-Bou, M.; Molinuevo, J.L.; Sala-Vila, A. Plant-Rich Dietary Patterns, Plant Foods and Nutrients, and Telomere Length. Adv Nutr. 2019, 10 (Suppl_4), S296–S303. [Google Scholar] [CrossRef]
- Varun, B. Dwaraka, Lucia Aronica, Natalia Carreras-Gallo, Jennifer L Robinson, Tayler Hennings, Aaron Lin, Logan Turner, Ryan Smith, Tavis L. Mendez, Hannah Went, Emily R. Ebel, Matthew M. Carter, Erica D. Sonnenburg, Justin L. Sonnenburg, Christopher D. Gardner. Unveiling the Epigenetic Impact of Vegan vs. Omnivorous Diets on Aging: Insights from the Twins Nutrition Study (TwiNS). medRxiv 2023.12.26.23300543. [CrossRef]
- Boden, W.E. Interpreting the results of the COURAGE trial: a non-interventionalist perspective. Rev Cardiovasc Med. 2009, 10 (Suppl 2), S34–44. [Google Scholar] [CrossRef] [PubMed]
- Lopez-Sendon, J.; Moreno, R.; Tamargo, J. ISCHEMIA Trial: Key Questions and Answers. Eur Cardiol. 2021, 16, e34. [CrossRef] [PubMed] [PubMed Central]
- Pham, V.; Moroni, A.; Gall, E.; Benedetti, A.; Zivelonghi, C.; Picard, F. Revascularization and Medical Therapy for Chronic Coronary Syndromes: Lessons Learnt from Recent Trials, a Literature Review. J Clin Med. 2023, 12, 2833. [Google Scholar] [CrossRef] [PubMed]
- Virani, S.S.; Newby, L.K.; Arnold, S.V.; et al. 2023 AHA/ACC/ACCP/ASPC/NLA/PCNA Guideline for the Management of Patients With Chronic Coronary Disease: A Report of the American Heart Association/American College of Cardiology Joint Committee on Clinical Practice Guidelines. Circulation 2023, 148, e9–e119. [Google Scholar] [CrossRef] [PubMed]
- Rathod, K.S.; Jones, D.A.; Van-Eijl, T.J.; et al. Randomised, double-blind, placebo-controlled study investigating the effects of inorganic nitrate on vascular function, platelet reactivity and restenosis in stable angina: protocol of the NITRATE-OCT study. BMJ Open. 2016, 6, e012728. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




