Submitted:
22 March 2024
Posted:
25 March 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and methods
Data sources and Study Population
Statistical Analysis
Results
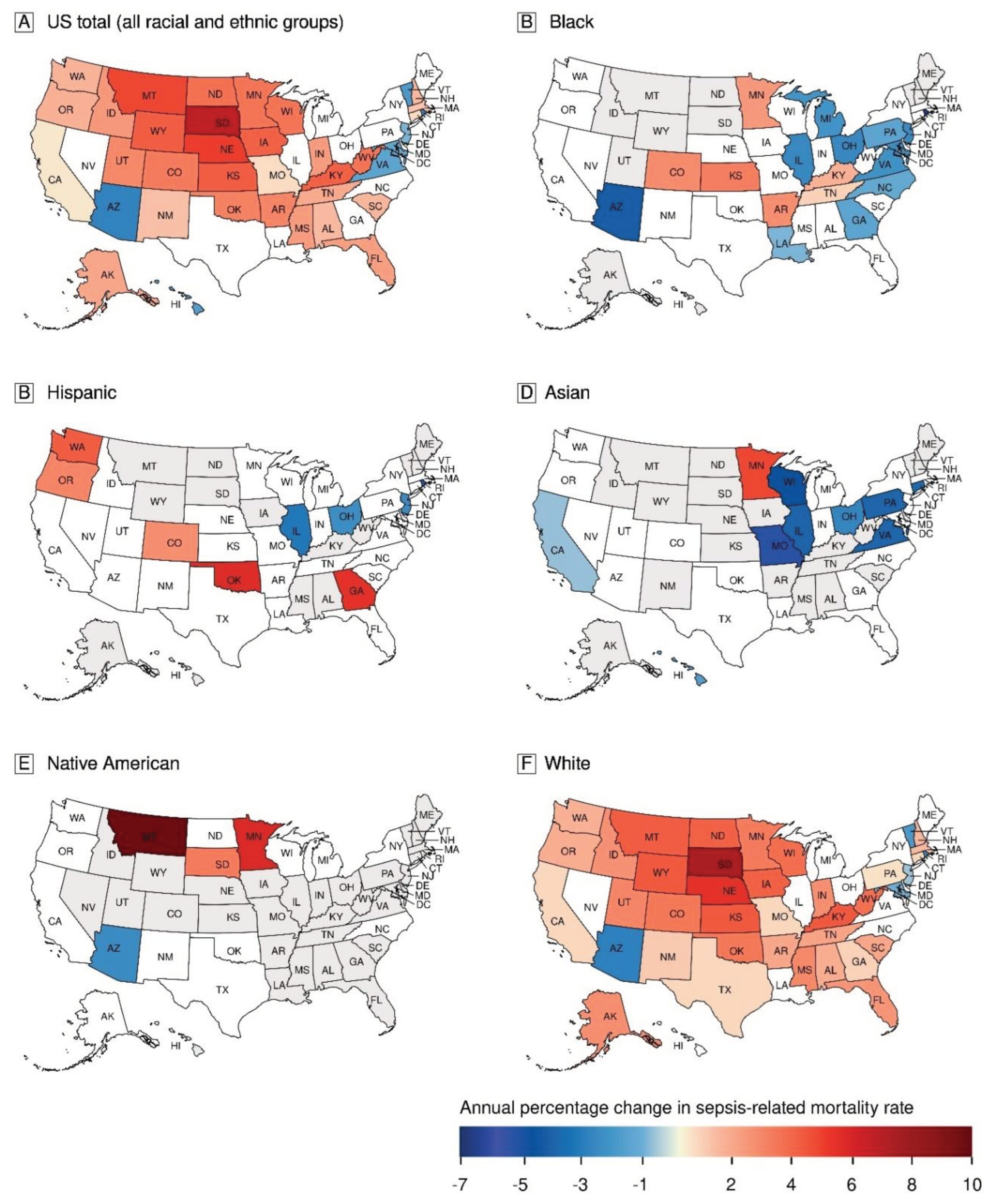
Trends of State-Level Sepsis-Related Mortality
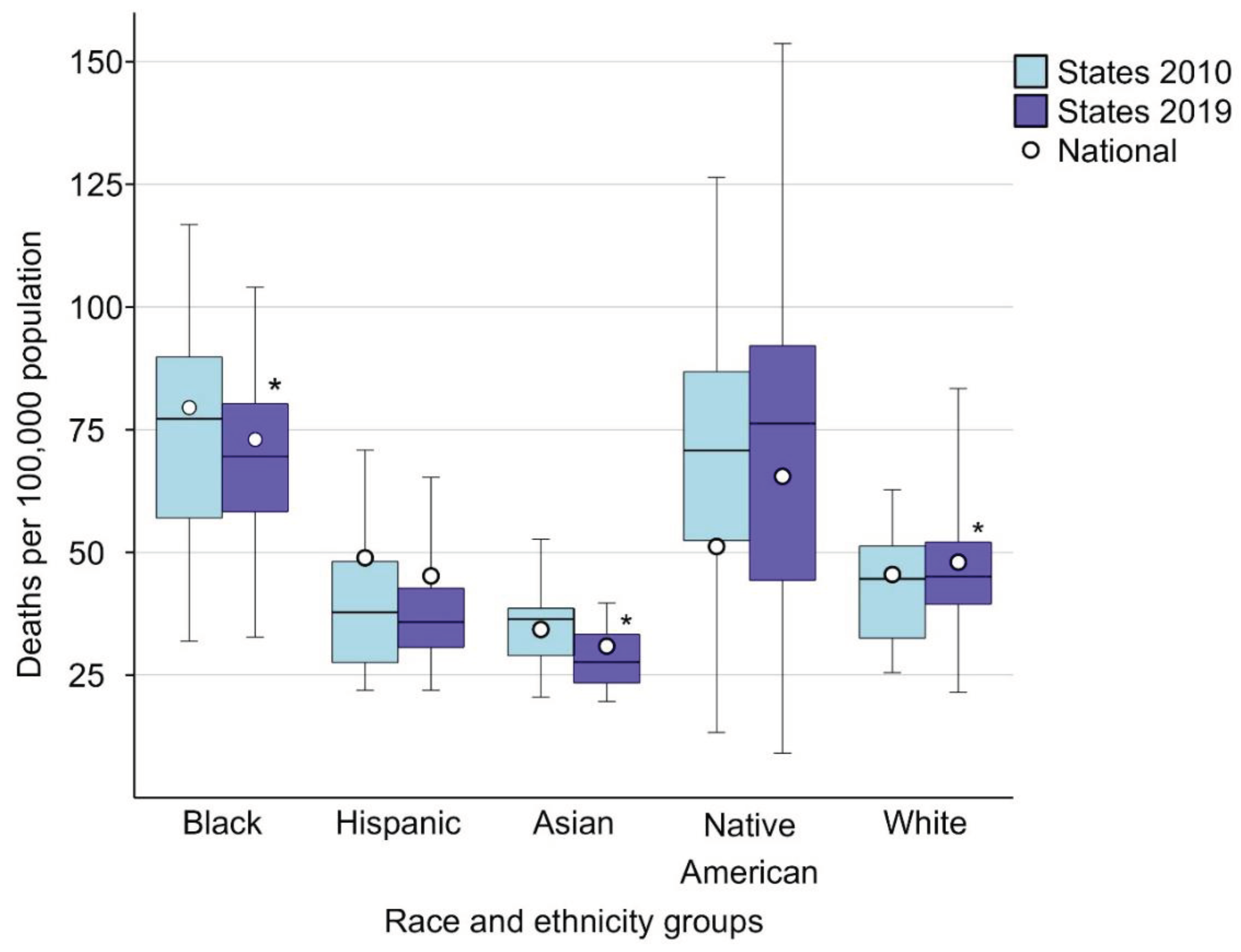
Inequalities in Sepsis-Related Mortality across States
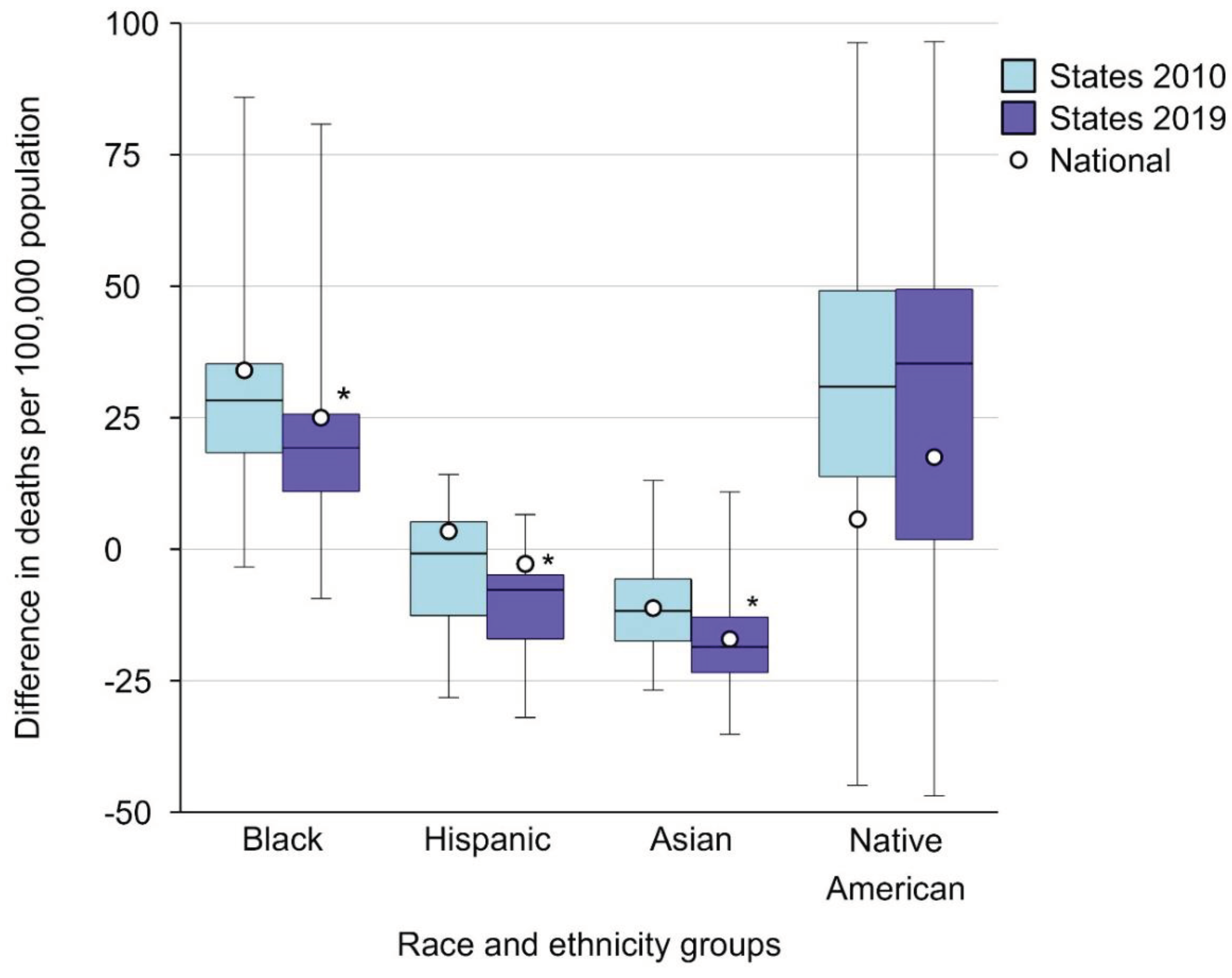
Inequalities in Within-State Sepsis-Related Mortality Gaps across States
Discussion
Study Limitations
Conclusions
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Conflicts of Interest
References
- Rudd, K.E.; Johnson, S.C.; Agesa, K.M.; Shackelford, K.A.; Tsoi, D.; Kievlan, D.R.; Colombara, D.V.; Ikuta, K.S.; Kissoon, N.; Finfer, S.; et al. Global, regional, and national sepsis incidence and mortality, 1990-2017: Analysis for the Global Burden of Disease Study. Lancet 2020, 395, 200–211. [Google Scholar] [CrossRef]
- Kempker, J.A.; Kramer, M.R.; Waller, L.A.; Martin, G.S. Risk Factors for Septicemia Deaths and Disparities in a Longitudinal US Cohort. Open Forum Infect. Dis. 2018, 5, ofy305. [Google Scholar] [CrossRef] [PubMed]
- Ford, D.W.M.; Goodwin, A.J.M.; Simpson, A.N.; Johnson, E.; Nadig, N.M.; Simpson, K.N.D. A Severe Sepsis Mortality Prediction Model and Score for Use With Administrative Data. Crit. Care Med. 2016, 44, 319–327. [Google Scholar] [CrossRef] [PubMed]
- Prest, J.; Sathananthan, M.; Jeganathan, N. Current Trends in Sepsis-Related Mortality in the United States*. Crit. Care Med. 2021, 49, 1276–1284. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.E.; Devereaux, R.S.; Yealy, D.M.; Safford, M.M.; Howard, G. National variation in United States sepsis mortality: A descriptive study. Int. J. Heal. Geogr. 2010, 9, 9. [Google Scholar] [CrossRef] [PubMed]
- Barnato, A.E.; Alexander, S.L.; Linde-Zwirble, W.T.; Angus, D.C. Racial variation in the incidence, care, and outcomes of severe sepsis: Analysis of population, patient, and hospital characteristics. Am J Respir Crit Care Med. 2008, 177, 279–284. [Google Scholar] [CrossRef] [PubMed]
- Engoren, M.; Jewell, E.S.; Douville, N.; Moser, S.; Maile, M.D.; Bauer, M.E. Genetic variants associated with sepsis. PLoS ONE 2022, 17, e0265052. [Google Scholar] [CrossRef] [PubMed]
- Zhong, X.; Ashiru-Oredope, D.; Pate, A.; Martin, G.P.; Sharma, A.; Dark, P.; Felton, T.; Lake, C.; MacKenna, B.; Mehrkar, A.; et al. Clinical and health inequality risk factors for non-COVID-related sepsis during the global COVID-19 pandemic: A national case-control and cohort study. EClinicalMedicine 2023, 66, 102321. [Google Scholar] [CrossRef] [PubMed]
- Wang, H.E.; Shapiro, N.I.; Griffin, R.; Safford, M.M.; Judd, S.; Howard, G. Chronic Medical Conditions and Risk of Sepsis. PLoS ONE 2012, 7, e48307. [Google Scholar] [CrossRef]
- Sheikh, F.B.; Douglas, W.B.; Catenacci, V.B.; Machon, C.B.; Fox-Robichaud, A.E.M. Social Determinants of Health Associated With the Development of Sepsis in Adults: A Scoping Review. Crit. Care Explor. 2022, 4, e0731. [Google Scholar] [CrossRef]
- Goodwin, A.J.; Nadig, N.R.; McElligott, J.T.; Simpson, K.N.; Ford, D.W. Where You Live Matters: The Impact of Place of Residence on Severe Sepsis Incidence and Mortality. Chest. 2016, 150, 829–836. [Google Scholar] [CrossRef] [PubMed]
- Elixhauser, A. (Agency for Healthcare Research and Quality), Friedman, B. (Agency for Healthcare Research and Quality) and Stranges, E. (Thomson Reuters). Septicemia in U.S. Hospitals, 2009. HCUP Statistical Brief #122. October 2011. Agency for Healthcare Research and Quality, Rockville, MD.
- Wang, Y.; Liu, Z.; Yang, L.; Zhou, J.; Li, J.; Liao, H.L.; Tian, X.J. Sepsis-related hospital admissions and ambient air pollution: A time series analysis in 6 Chinese cities. BMC Public Heal. 2021, 21, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Rosier, F.; Brisebarre, A.; Dupuis, C.; Baaklini, S.; Puthier, D.; Brun, C.; Pradel, L.C.; Rihet, P.; Payen, D. Genetic Predisposition to the Mortality in Septic Shock Patients: From GWAS to the Identification of a Regulatory Variant Modulating the Activity of a CISH Enhancer. Int. J. Mol. Sci. 2021, 22, 5852. [Google Scholar] [CrossRef] [PubMed]
- Lusk, J.B.; Blass, B.; Mahoney, H.; Hoffman, M.N.; Clark, A.G.; Bae, J.; Ashana, D.C.; Cox, C.E.; Hammill, B.G. Neighborhood socioeconomic deprivation, healthcare access, and 30-day mortality and readmission after sepsis or critical illness: Findings from a nationwide study. Crit. Care 2023, 27, 1–11. [Google Scholar] [CrossRef] [PubMed]
- Chang, J.; Medina, M.; Kim, S.J. Is patients' rurality associated with in-hospital sepsis death in US hospitals? Front Public Health. 2023, 11, 1169209. [Google Scholar] [CrossRef]
- Honda, T.J.; Kazemiparkouhi, F.; Henry, T.D.; Suh, H.H. Long-term PM2.5 exposure and sepsis mortality in a US medicare cohort. BMC Public Heal. 2022, 22, 1–9. [Google Scholar] [CrossRef]
- Guo, Q.; Qu, P.; Cui, W.; Liu, M.; Zhu, H.; Chen, W.; Sun, N.; Geng, S.; Song, W.; Li, X.; et al. Organism type of infection is associated with prognosis in sepsis: An analysis from the MIMIC-IV database. BMC Infect. Dis. 2023, 23, 1–11. [Google Scholar] [CrossRef]
- Association between source of infection and hospital mortality in patients who have septic shock. Therapy of Septic Shock Database Research Group; Leligdowicz, A.; Dodek, P.M.; Norena, M.; Wong, H.; Kumar, A.; Kumar, A. Co-operative Antimicrobial. Am J Respir Crit Care Med. 2014, 189, 1204–1213. [Google Scholar]
- Seymour, C.W.; Gesten, F.; Prescott, H.C.; Friedrich, M.E.; Iwashyna, T.J.; Phillips, G.S.; Lemeshow, S.; Osborn, T.; Terry, K.M.; Levy, M.M. Time to Treatment and Mortality during Mandated Emergency Care for Sepsis. N Engl J Med. 2017, 376, 2235–2244. [Google Scholar] [CrossRef]
- Cimiotti, J.P.; Becker, E.R.; Li, Y.; Sloane, D.M.; Fridkin, S.K.; West, A.B.; Aiken, L.H. Association of Registered Nurse Staffing With Mortality Risk of Medicare Beneficiaries Hospitalized With Sepsis. JAMA Heal. Forum 2022, 3, e221173. [Google Scholar] [CrossRef]
- Gaieski, D.F.; Edwards, J.M.; Kallan, M.J.; Mikkelsen, M.E.; Goyal, M.; Carr, B.G. The Relationship between Hospital Volume and Mortality in Severe Sepsis. Am. J. Respir. Crit. Care Med. 2014, 190, 665–674. [Google Scholar] [CrossRef]
- Wang, H.E.; Donnelly, J.P.; Shapiro, N.I.; Hohmann, S.F.; Levitan, E.B. Hospital Variations in Severe Sepsis Mortality. Am. J. Med Qual. 2014, 30, 328–336. [Google Scholar] [CrossRef]
- Rush, B.M.; Danziger, J.; Walley, K.R.M.; Kumar, A.M.; Celi, L.A. Treatment in Disproportionately Minority Hospitals Is Associated With Increased Risk of Mortality in Sepsis: A National Analysis*. Crit. Care Med. 2020, 48, 962–967. [Google Scholar] [CrossRef]
- Shankar-Hari, M.; Rubenfeld, G.D. Race, Ethnicity, and Sepsis: Beyond Adjusted Odds Ratios. Crit Care Med. 2018, 46, 1009–1010. [Google Scholar] [CrossRef]
- DiMeglio, M.; Dubensky, J.; Schadt, S.; Potdar, R.; Laudanski, K. Factors Underlying Racial Disparities in Sepsis Management. Healthcare 2018, 6, 133. [Google Scholar] [CrossRef]
- CMS to Improve Quality of Care during Hospital Inpatient Stays. CMS.gov Fact Sheet. 2014. Available online: https://www.cms.gov/newsroom/fact-sheets/cms-improve-quality-care-during-hospital-inpatient-stays (accessed on 14 November 2023).
- Evans, L.; Rhodes, A.; Alhazzani, W.; Antonelli, M.; Coopersmith, C.M.; French, C.; Machado, F.R.; Mcintyre, L.; Ostermann, M.; Prescott, H.C.; et al. Surviving Sepsis Campaign: International Guidelines for Management of Sepsis and Septic Shock 2021. Crit. Care Med. 2021, 49, e1063–e1143. [Google Scholar] [CrossRef]
- Kempker, J.A.; Wang, H.E.; Martin, G.S. Sepsis is a preventable public health problem. Crit. Care 2018, 22, 1–3. [Google Scholar] [CrossRef]
- von Elm, E.; Altman, D.G.; Egger, M.; Pocock, S.J.; Gøtzsche, P.C.; Vandenbroucke, J.P.; STROBE Initiative. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: Guidelines for reporting observational studies. PLoS Med. 2007, 4, e296. [Google Scholar] [CrossRef]
- CDC WONDER. Centers for Disease Control and Prevention. Available online: https://wonder.cdc.gov/mcd.html (accessed on 23 September 2023).
- Office of Management and Budget. Recommendation from the Interagency Committee for the Review of the Racial and Ethnic Standards to the Office of Management and Budget Concerning Changes to the Standards for Classification of Federal Data on Race and Ethnicity. Federal Register 1997, 62, 36873–36946. [Google Scholar]
- Melamed, A.; Sorvillo, F.J. The burden of sepsis-associated mortality in the United States from 1999 to 2005: An analysis of multiple-cause-of-death data. Crit. Care 2009, 13, R28. [Google Scholar] [CrossRef] [PubMed]
- Vaughan, A.S.; Coronado, F.; Casper, M.; Loustalot, F.; Wright, J.S. County-Level Trends in Hypertension-Related Cardiovascular Disease Mortality-United States, 2000 to 2019. J Am Heart Assoc. 2022, 11, e024785. [Google Scholar] [CrossRef] [PubMed]
- Rhee, C.; Klompas, M. Sepsis trends: Increasing incidence and decreasing mortality, or changing denominator? J. Thorac. Dis. 2020, 12, S89–S100. [Google Scholar] [CrossRef] [PubMed]
- Parra-Calderón, C.L.; Sanz, F.; McIntosh, L.D. The Challenge of the Effective Implementation of FAIR Principles in Biomedical Research. Methods Inf. Med. 2020, 59, 117–118. [Google Scholar] [CrossRef]
- Arias, E.; Schauman, W.S.; Eschbach, K.; Sorlie, P.D.; Backlund, E. The validity of race and Hispanic origin reporting on death certificates in the United States. 2008, 1–23.
- Shappell, C.N.; Klompas, M.; Chan, C.; Chen, T.; Kanjilal, S.; McKenna, C.; Rhee, C.; CDC Prevention Epicenters Program. Use of Electronic Clinical Data to Track Incidence and Mortality for SARS-CoV-2-Associated Sepsis. JAMA Netw Open. 2023, 6, e2335728. [Google Scholar] [CrossRef]
| 2010 | 2019 | |||||
|---|---|---|---|---|---|---|
| Group | Deaths | AAMRa (95% CI)b | Deaths | AAMR (95% CI) | APCc,d (95% CI) | p valued |
| All | 159982 | 48.4 (48.1-48.6) | 201478 | 49.8 (49.6-50.0) | +0.9 (+0.4 to +1.5) | 0.0013 |
| Race and ethnicity | ||||||
| Black | 24587 | 79.5 (78.5-80.5) | 29416 | 73.0 (72.1-73.9) | -0.7 (-1.1 to -0.2) | 0.0043 |
| Hispanic | 12217 | 48.9 (48.0-49.9) | 18074 | 45.2 (44.5-45.9) | -0.2 (-0.7 to +0.3) | 0.3691 |
| Asian | 4006 | 34.3 (33.2-35.4) | 6247 | 30.9 (30.1-31.7) | -0.7 (-1.1 to -0.2) | 0.0039 |
| Native American | 1187 | 51.2 (48.0-54.3) | 1705 | 65.5 (62.3-68.7) | +0.5 (-0.4 to +1.5) | 0.2762 |
| White | 117985 | 45.5 (45.3-45.8) | 146034 | 48.0 (47.2-48.7) | +1.4 (+0.8 to +2.0) | <0.0001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




