Submitted:
10 March 2024
Posted:
11 March 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
- We develop a gait parameter estimation and health information extraction framework using footstep-induced floor vibrations, which is the first ubiquitous gait analysis system of this kind and covers the most extensive range of standard gait health metrics in medical practices, to the best of our knowledge.
- We characterize the footstep-induced floor vibration with respect to various gait characteristics across the two most typical floor types to extract features that are sensitive to gait but are adaptable to the changing floor types, improving the scalability of our method for ubiquitous deployment in people’s homes with different floors.
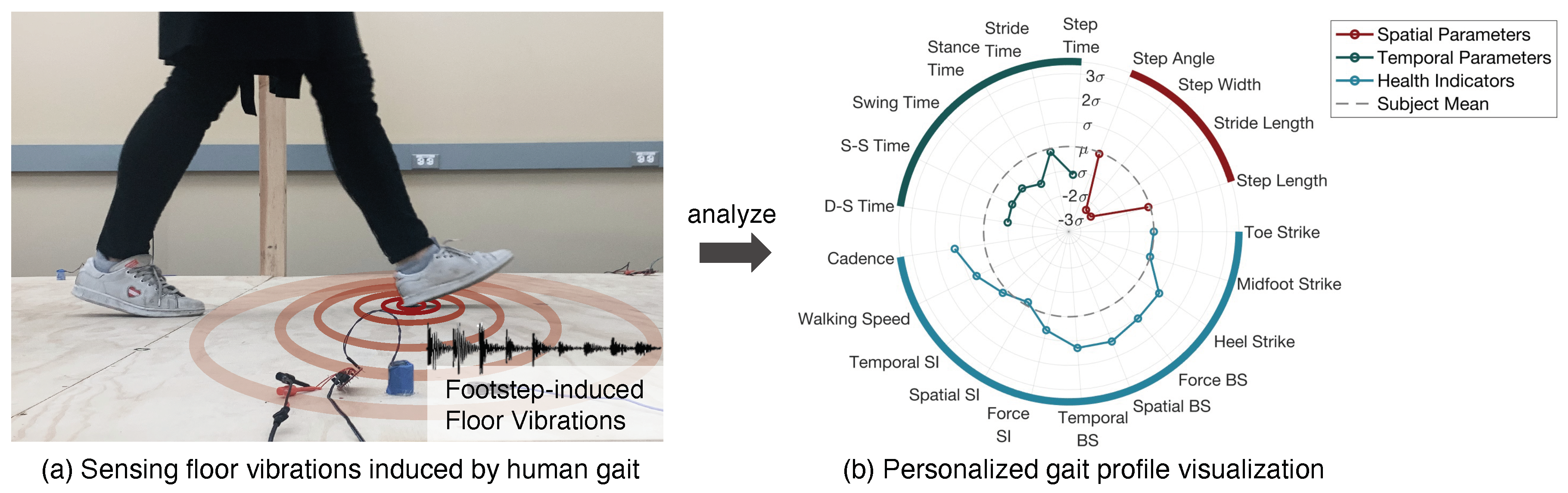
- We evaluate our approach through a real-world experiment with 20 subjects across two most typical floor types and achieve promising accuracy in estimating spatio-temporal gait parameters and gait health indicators, which are summarized through personalized gait diagrams for effective visualization.
2. Characterization of Footstep-Induced Floor Vibrations for Gait Health Monitoring
2.1. Physical Insight behind Footstep-Induced Floor Vibrations
2.2. Relationship between Gait Characteristics and Footstep-Induced Floor Vibrations
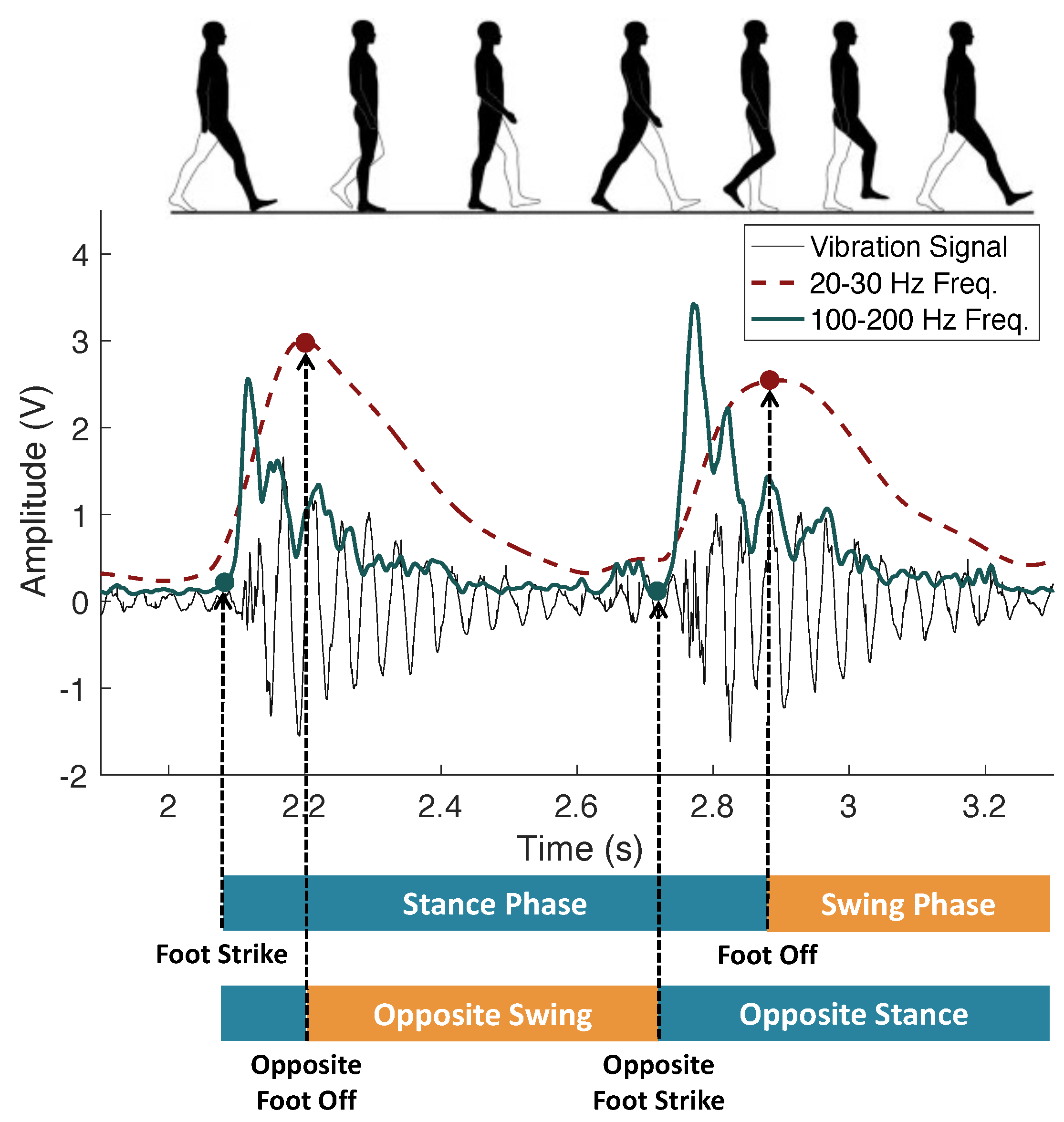
2.2.1. Temporal Gait Characteristics
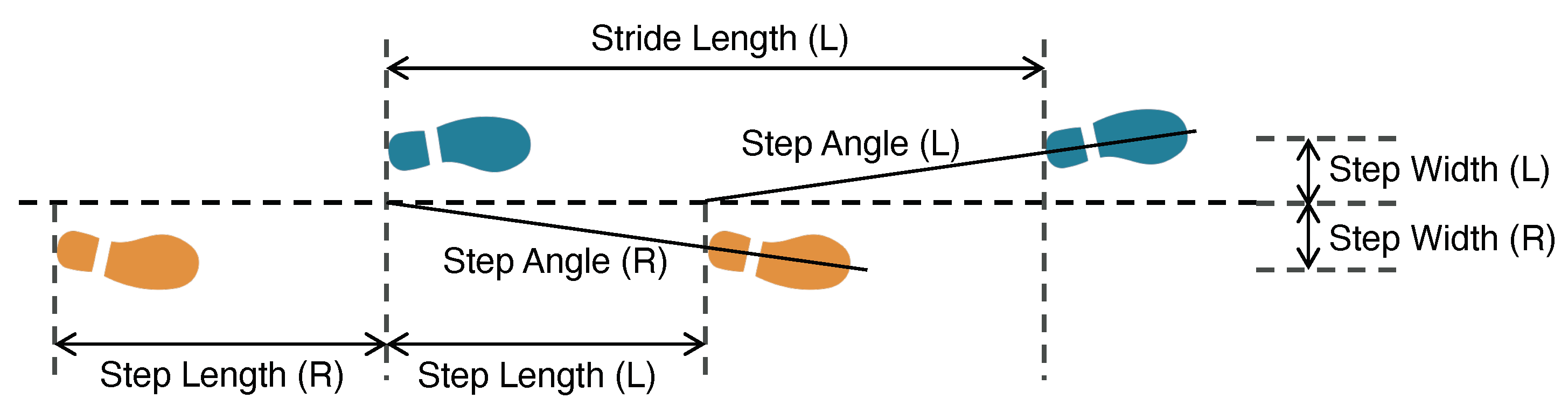
2.2.2. Spatial Gait Characteristics
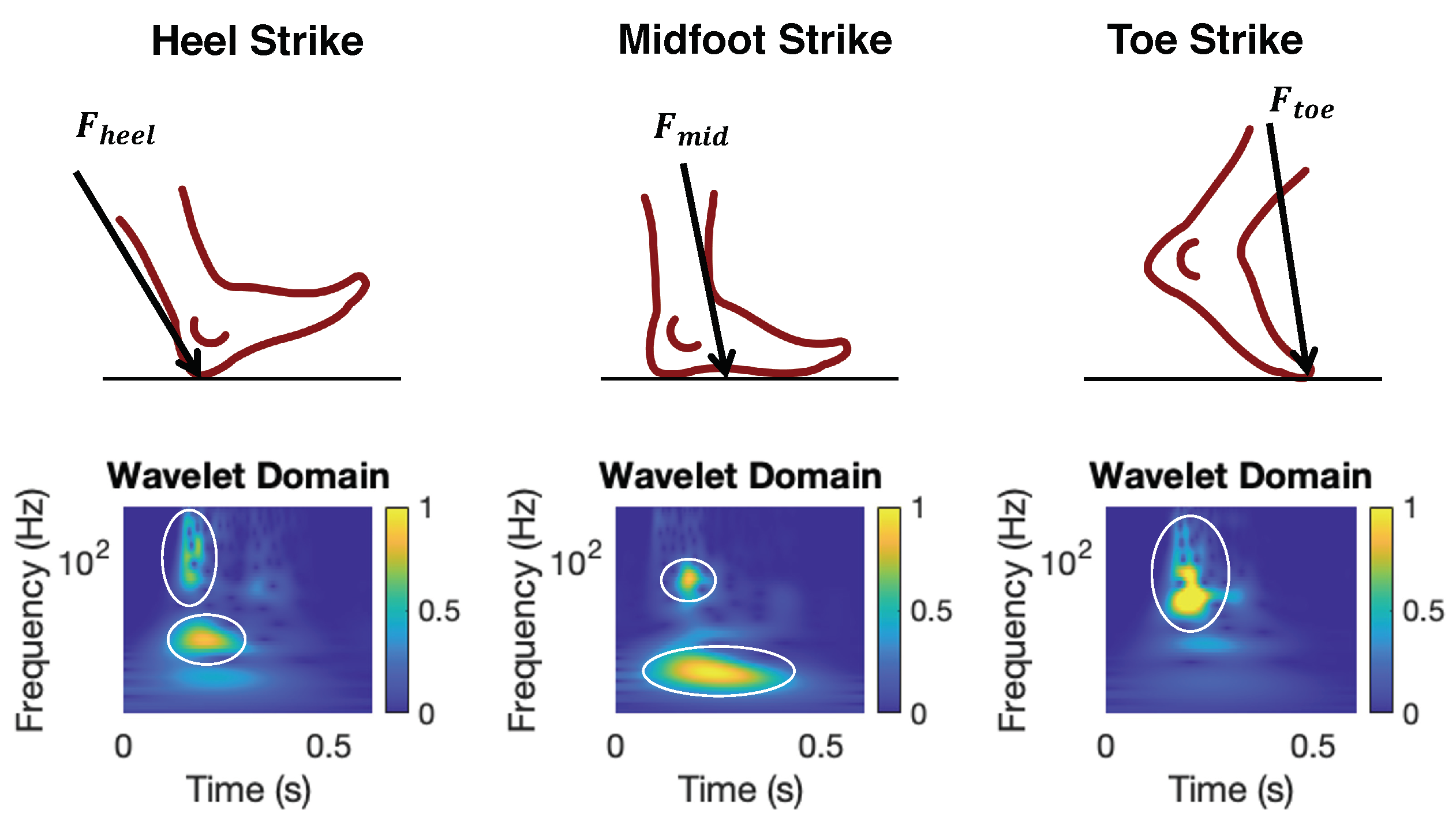
2.2.3. Gait Health Indicators
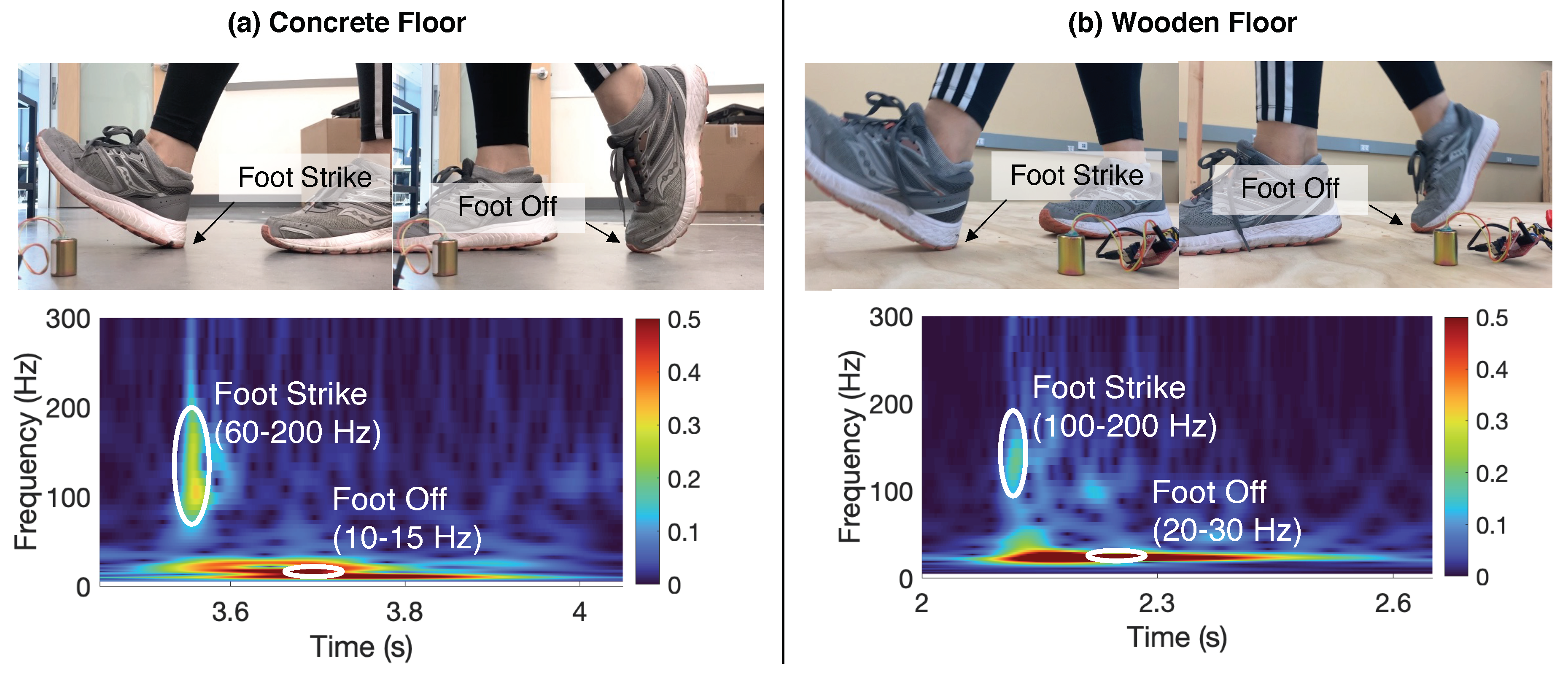
2.3. Effect of Floor Types on Floor Vibration-Based Gait Health Monitoring
2.3.1. Floor Type Influence on Temporal Parameter Estimation
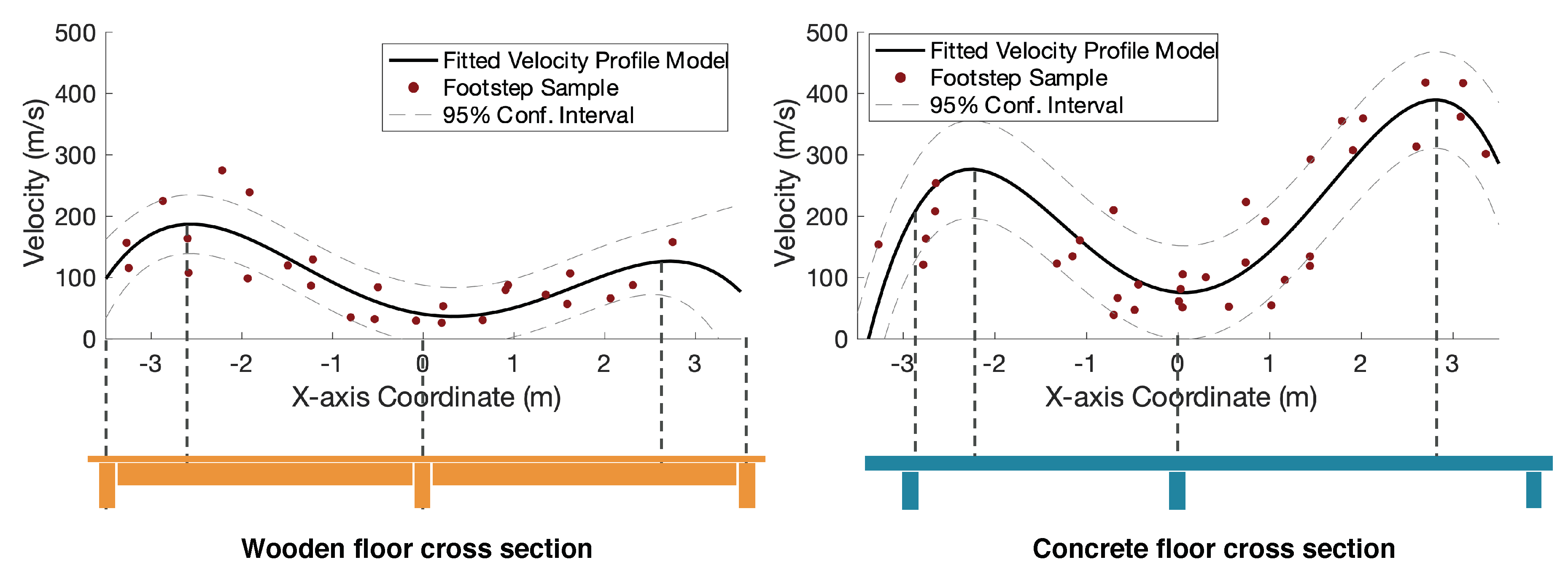
2.3.2. Floor Type Influence on Spatial Parameter Estimation
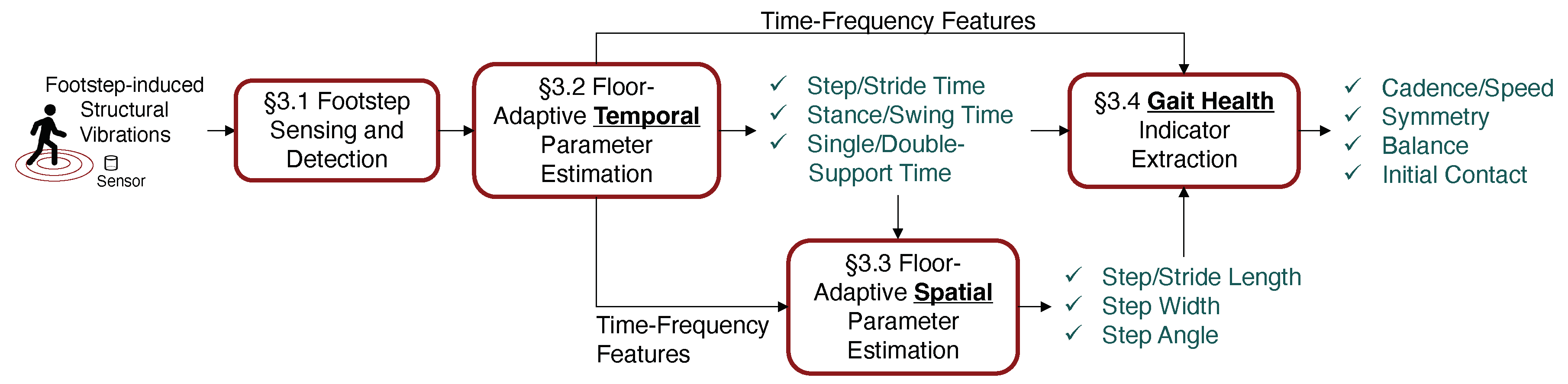
3. Gait Analysis Framework through Footstep-Induced Floor Vibrations
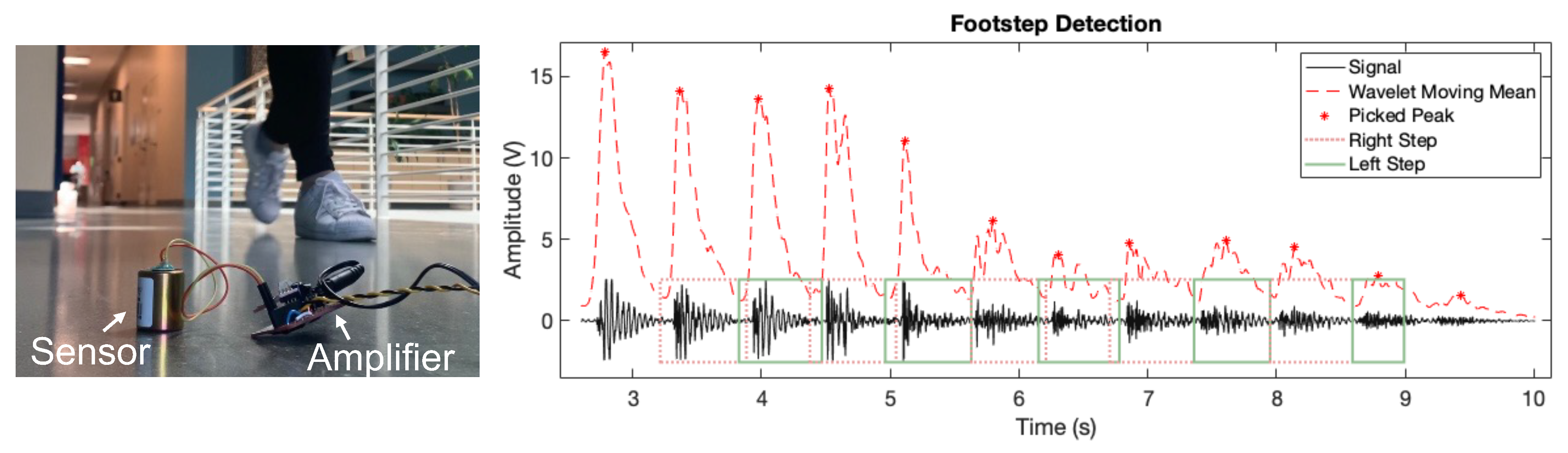
3.1. Footstep Sensing and Detection
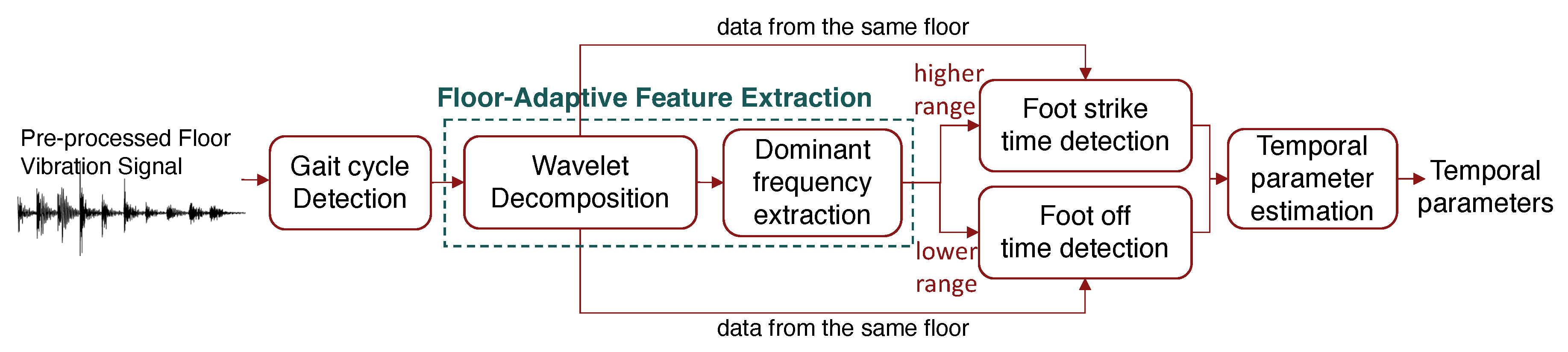
3.2. Floor-Adaptive Temporal Parameter Estimation
- Step Time =
- Stride Time =
- Stance Time =
- Swing Time =
- Single-Support Time =
- Double-Support Time 1 =
- Double-Support Time 2 =
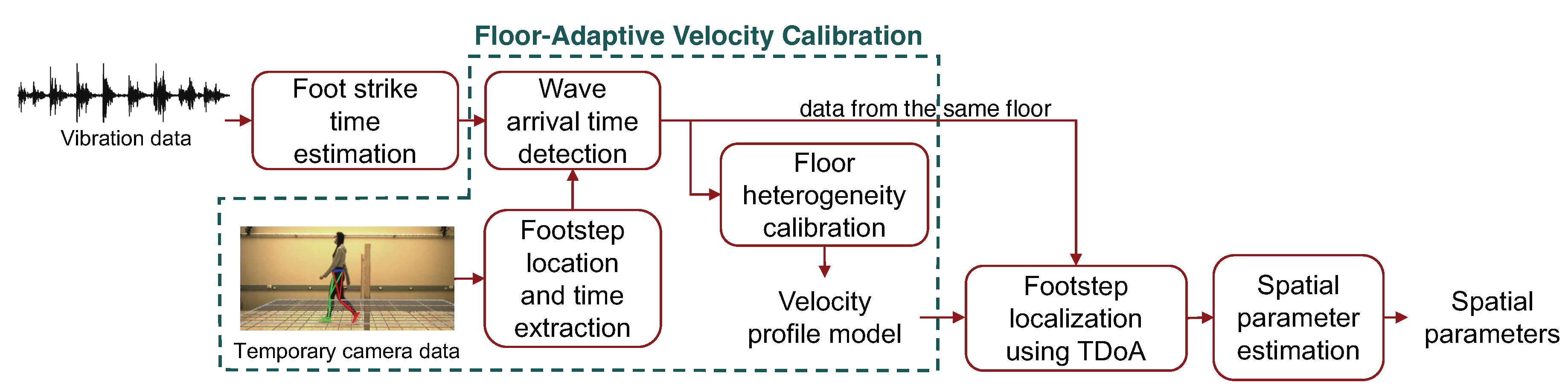
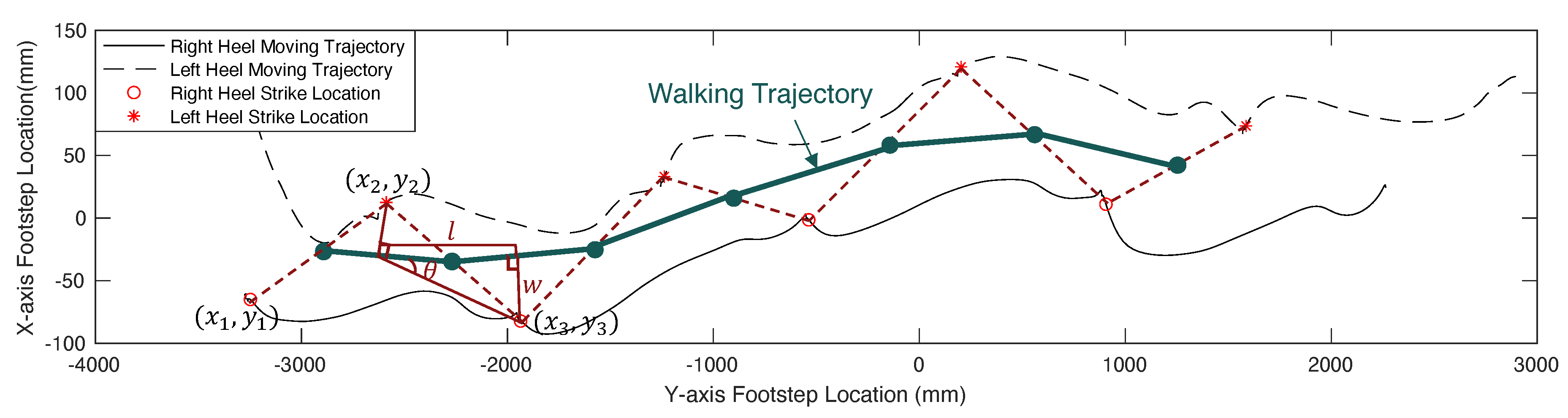
3.3. Floor-Adaptive Spatial Parameter Estimation
-
Step Length:
- Step Width:
- Step Angle:
- Stride Length:
3.4. Gait Health Indicator Extraction
3.4.1. Cadence/Walking Speed Estimation
3.4.2. Left-Right Symmetry Estimation
3.4.3. Gait Balance Quantification
3.4.4. Initial Contact Type Prediction
4. Evaluation
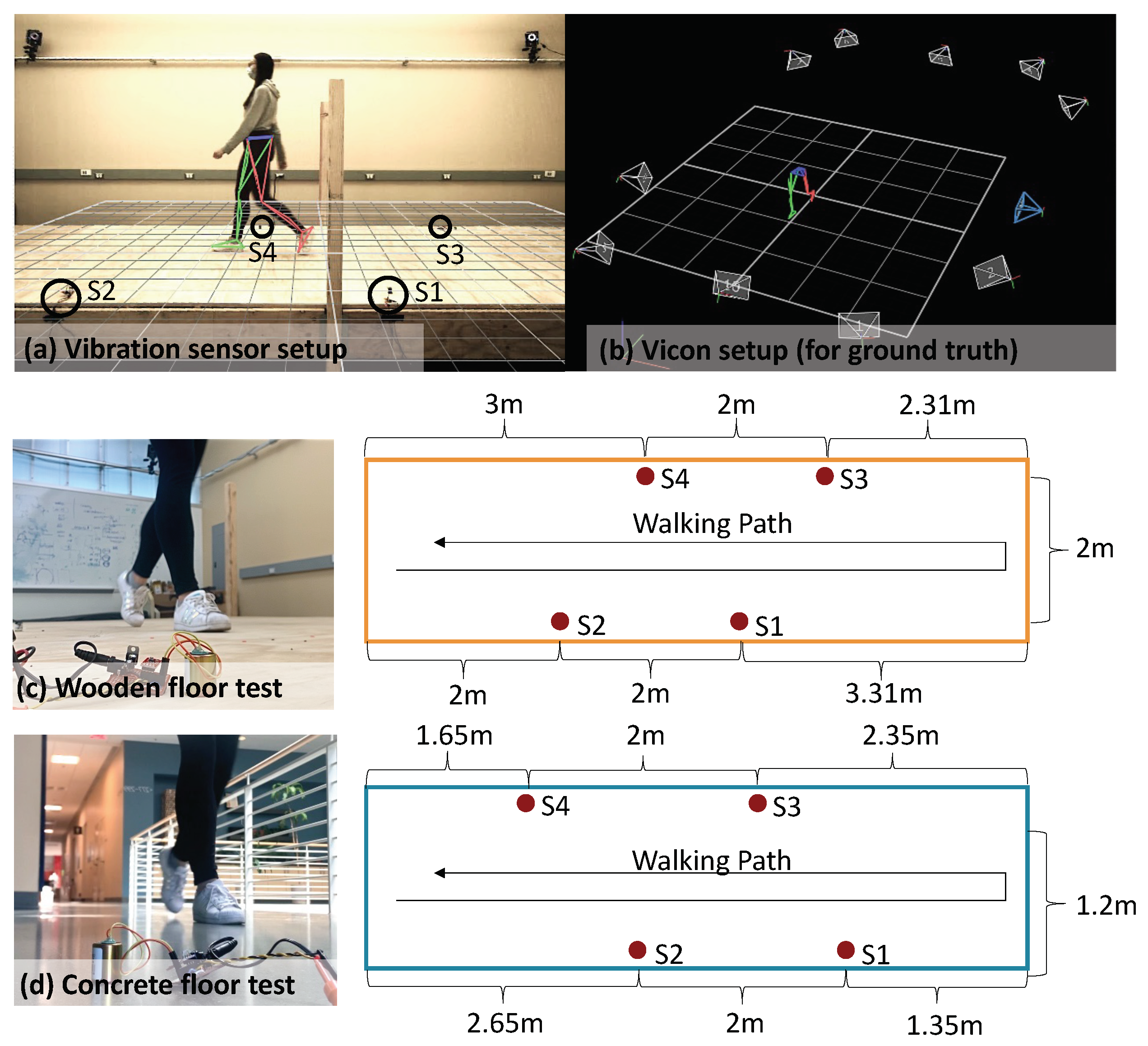
4.1. Real-World Experiment Setup
4.2. Results and Discussion
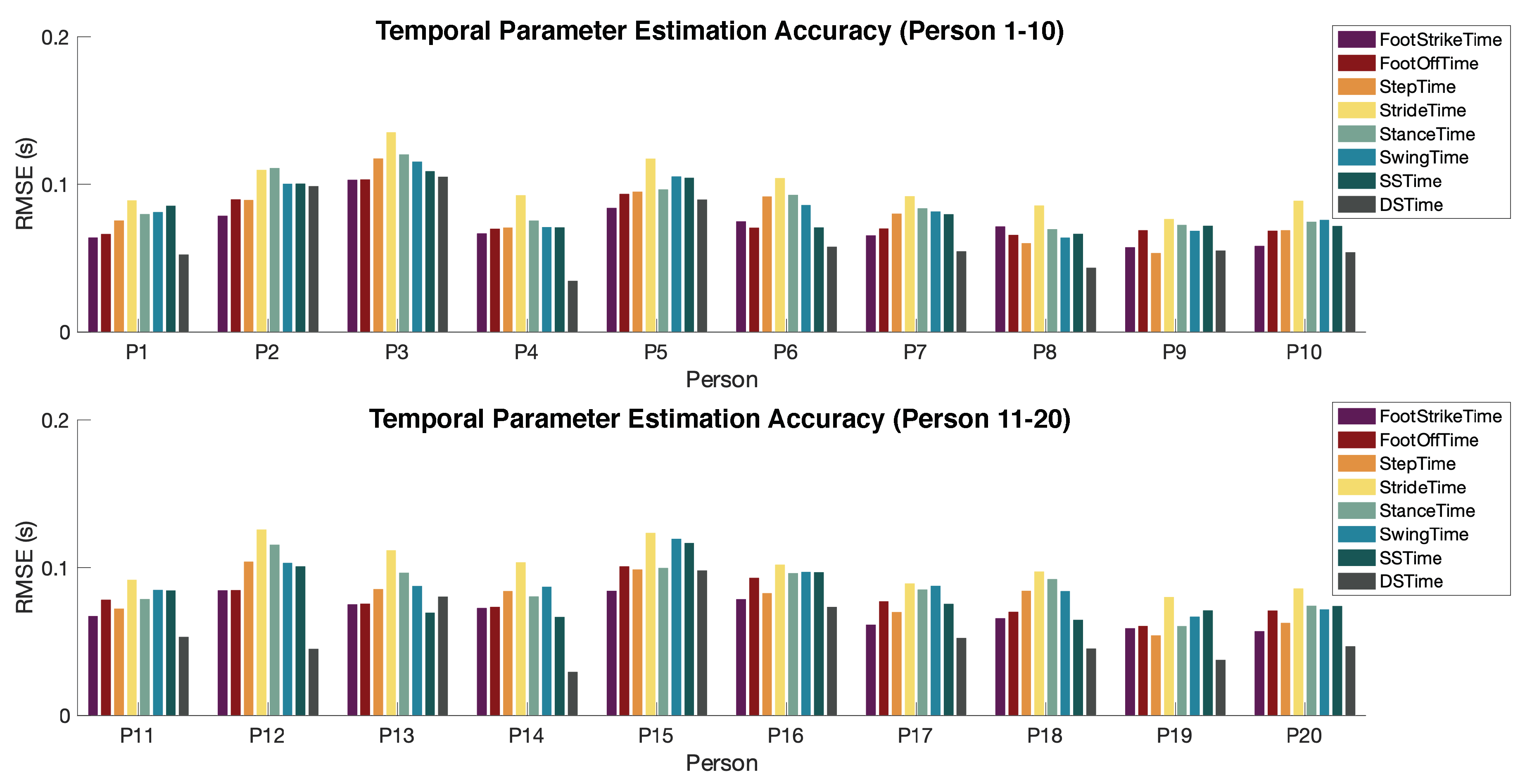
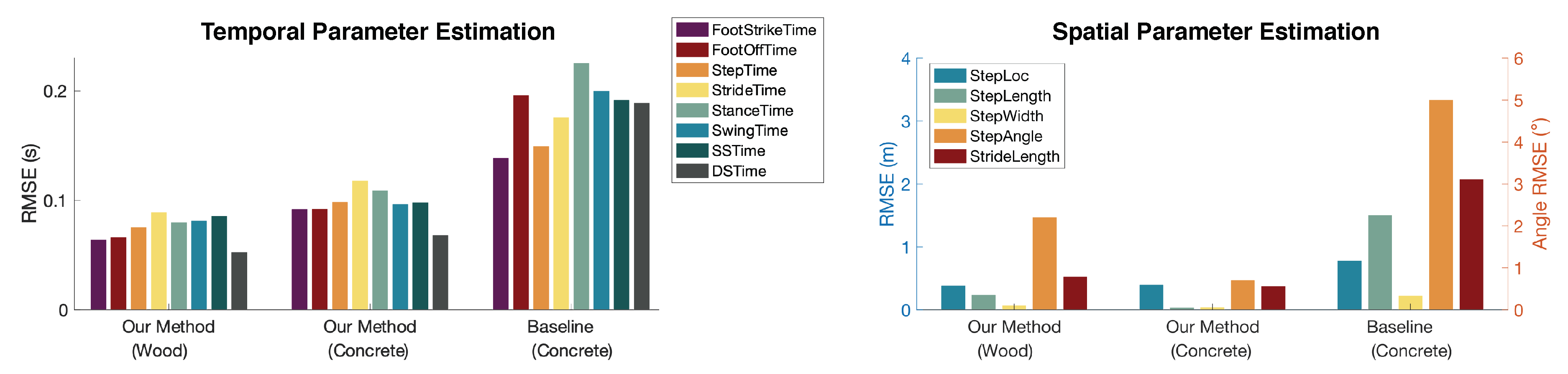
4.2.1. Temporal Parameter Estimation Accuracy
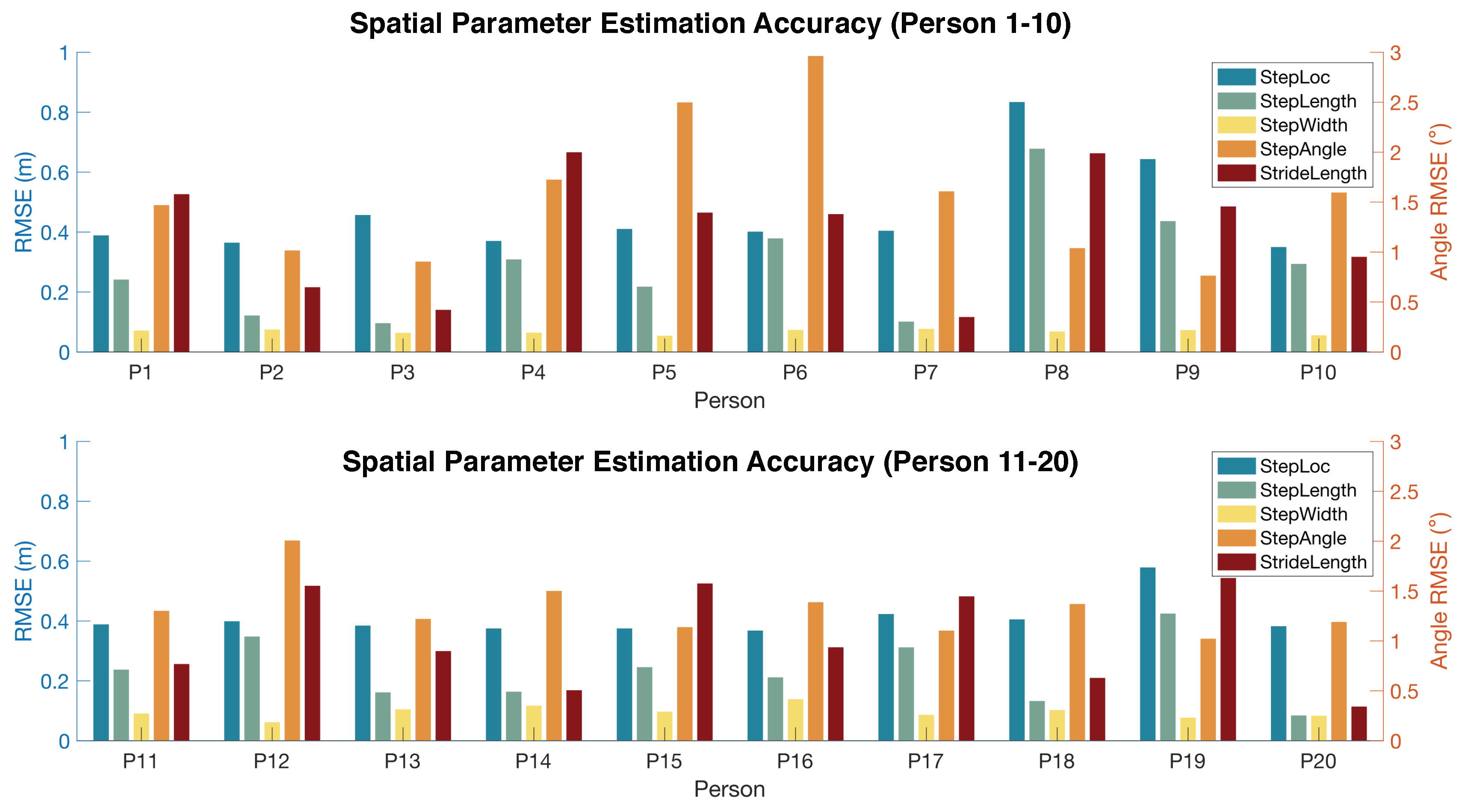
4.2.2. Spatial Parameter Estimation Accuracy
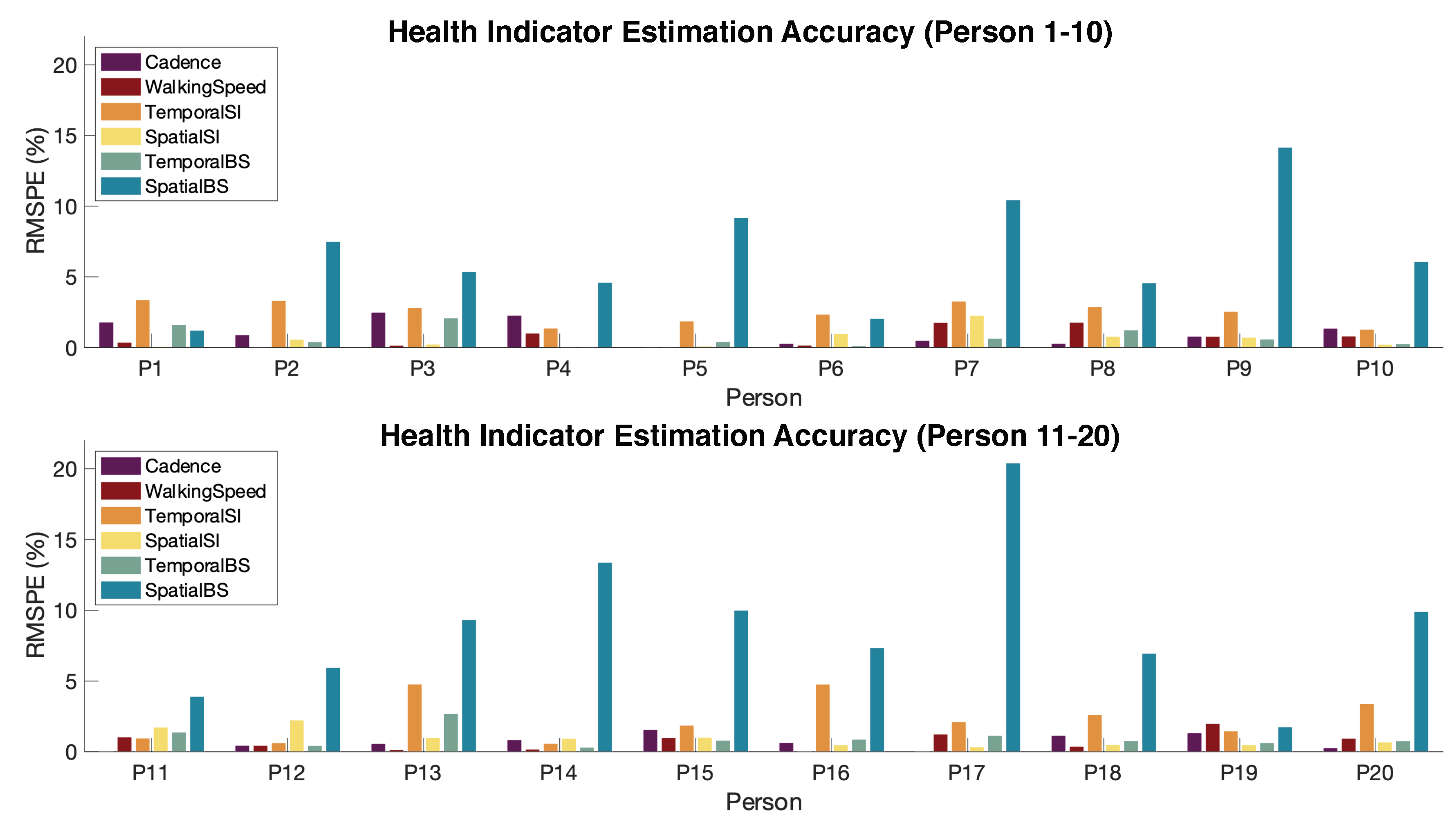
4.2.3. Gait Health Indicator Extraction Accuracy
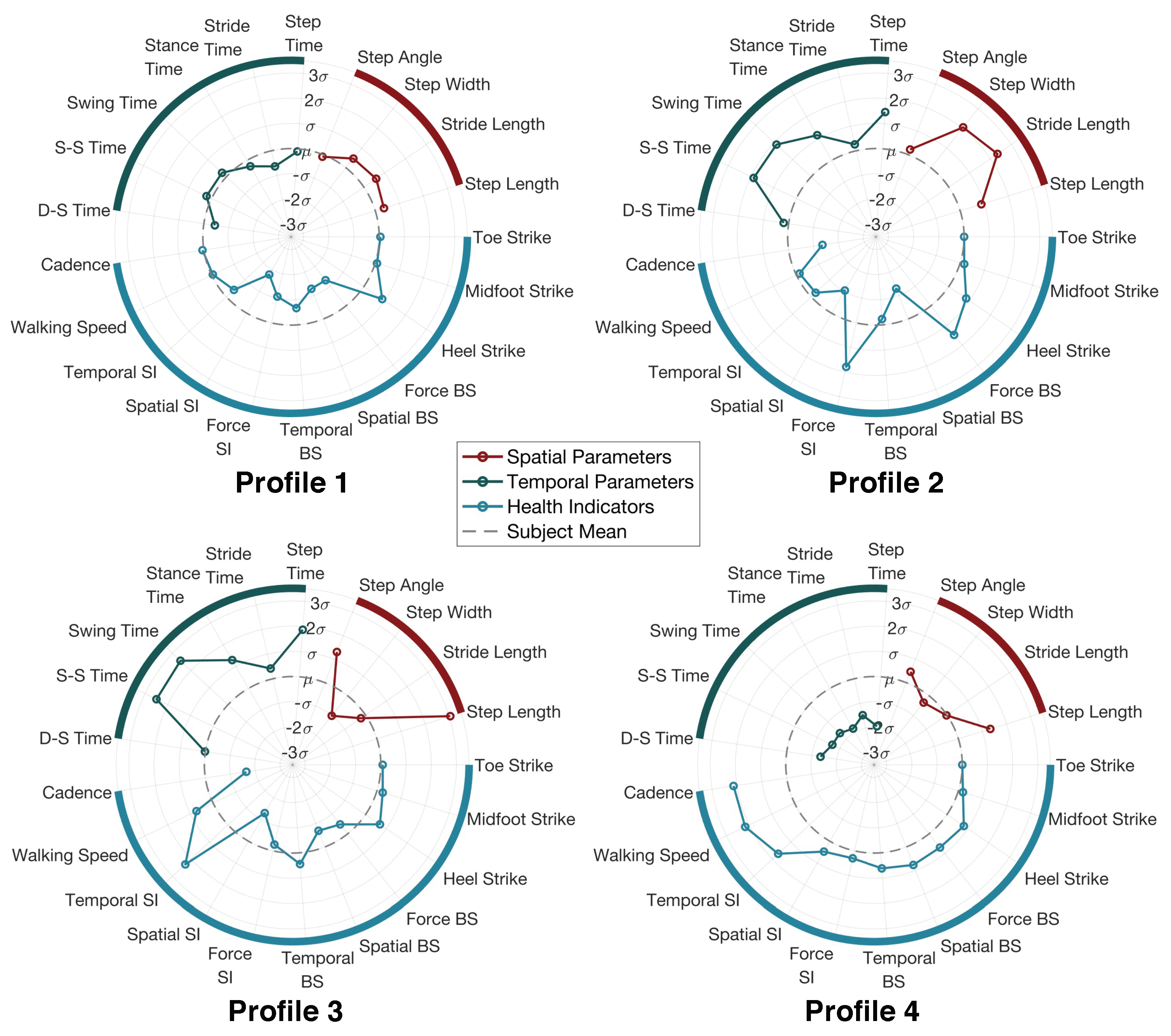
4.2.4. Personalized Gait Profile
- Profile 1 “The Steady Walker": This person’s gait parameters are all within one standard deviation from the mean value. It means this person has a gait pattern that is close to the average of all walkers during the experiment. The person also has a low score for symmetry and balance, which indicates that the person has good symmetry and stability.
- Profile 2 “The Wide-Based Walker": This person has a significantly larger step width than the rest of the subjects. As a result, the stride length and step time may also increase due to the wide base. On the other hand, the footstep forces are less symmetrical and balanced compared to the other subjects. This may be the root cause of the large step width because a wider base can typically help to maintain balance.
- Profile 3 “The Large-Step Walker": This person has a significantly larger step length and step time than the rest of the subjects. This means that the person takes large steps so that the during of each step also increases. As a result, the person still has a high walking speed while having a low cadence. Based on our record, this is the tallest person among all subjects, which explains this special gait profile.
- Profile 4 “The Quick Walker": This person has significantly smaller values in all temporal parameters while keeping the spatial parameters around the average. This means that the person takes medium steps but with quick left-right foot alternations. As a result, the person has a high cadence and high walking speed.
4.3. Discussion on the Effect of Human and Environmental Variables
4.3.1. Effect of Floor Types
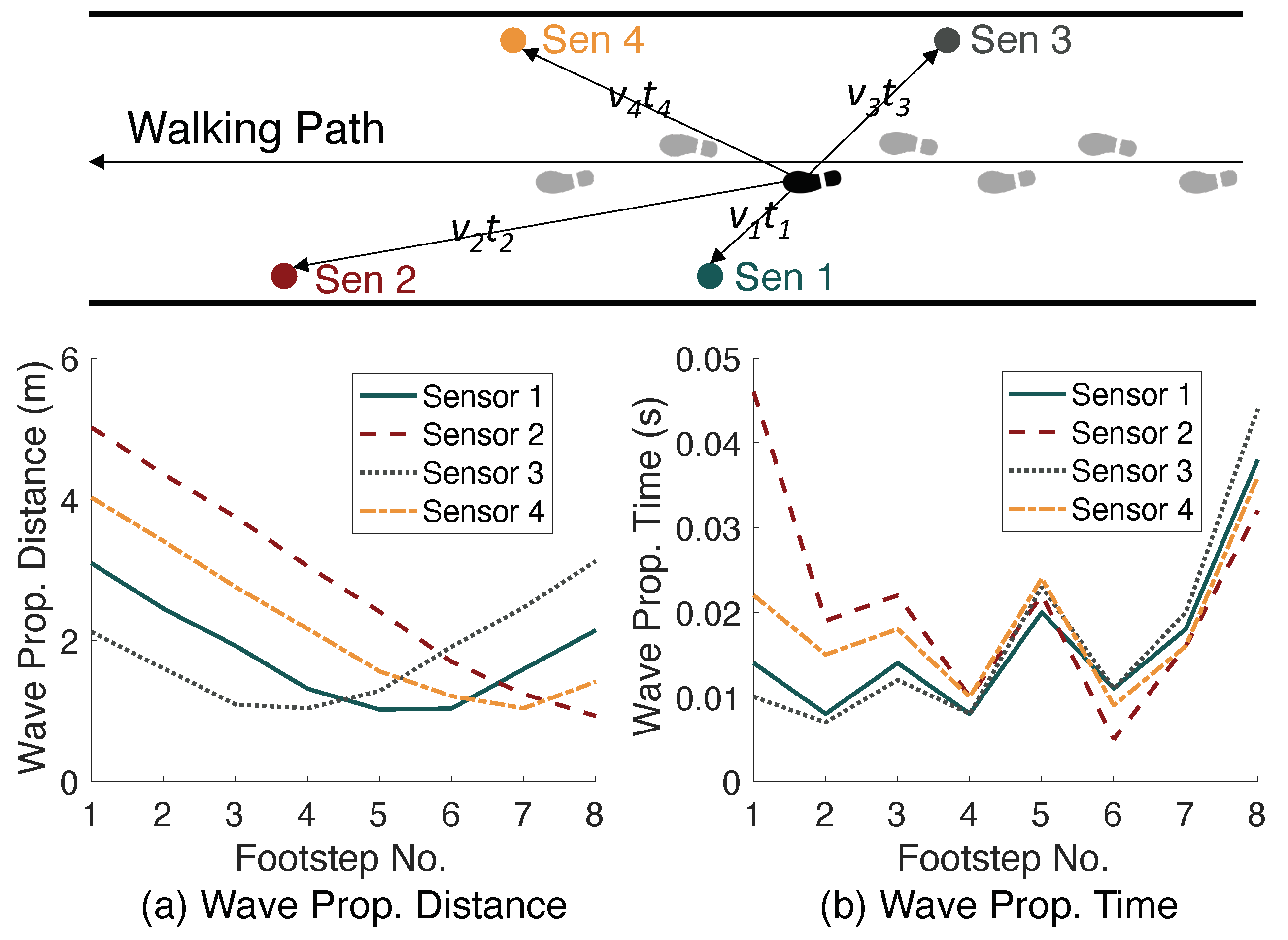
4.3.2. Effect of Sensor Locations
4.3.3. Effect of Walking Paths
4.3.4. Effect of Gait Abnormalities
4.4. Comparison with the Existing Sensing Systems
4.4.1. Comparison among Different Sensing Modalities
4.4.2. Comparison within the Floor Vibration Sensing
5. Future Work
- Explore downstream tasks for detection and tracking of neuromuscular/musculoskeletal disorders and estimation of fall risks: We will collect data from patients with a specific type of neurological/musculoskeletal disorder (e.g., Parkinson’s, cerebral palsy, muscular dystrophy) or who have higher risks of falls. By comparing the vibration signals from healthy individuals with those from patients, we can identify differences in gait parameters and use this information to develop algorithms that assist with early diagnosis and continuous tracking of their health conditions. Existing work with muscular dystrophy patients has obtained promising accuracy in disease detection [32].
- Conduct larger scale field experiment with more complex walking scenarios: We will conduct field experiments in more realistic and less controlled settings such as homes, hospitals, and public places, which will provide a better understanding of the generalizability of the system and the potential for ubiquitous adoption.
- Integrate with other sensing technologies: Our system has the potential to be integrated with other technologies such as wearable sensors/mobile devices/cameras. Such integration can provide users with a more accurate and comprehensive gait health assessment, capturing force, motion, and muscle activation. In addition, other sources of health records such as a person’s daily habits and medical/injury history can also be fused with the vibration data, which can enable personalized health recommendations and interventions, tailored to the individual’s unique needs.
6. Conclusion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Kirtley, C. Chapter 1 - The temporal-spatial parameters. In Clinical Gait Analysis; Kirtley, C., Ed.; Churchill Livingstone: Edinburgh, 2006; pp. 15–37. [Google Scholar] [CrossRef]
- Baker, R. Gait analysis methods in rehabilitation. Journal of neuroengineering and rehabilitation 2006, 3, 1–10. [Google Scholar] [CrossRef]
- Whittle, M.W. Gait analysis: an introduction; Butterworth-Heinemann: 2014.
- Kharb, A.; Saini, V.; Jain, Y.; Dhiman, S. A review of gait cycle and its parameters. IJCEM International Journal of Computational Engineering & Management 2011, 13, 78–83. [Google Scholar]
- Sadeghi, H.; Allard, P.; Prince, F.; Labelle, H. Symmetry and limb dominance in able-bodied gait: a review. Gait & posture 2000, 12, 34–45. [Google Scholar]
- Chang, F.M.; Rhodes, J.T.; Flynn, K.M.; Carollo, J.J. The role of gait analysis in treating gait abnormalities in cerebral palsy. Orthopedic Clinics 2010, 41, 489–506. [Google Scholar] [CrossRef] [PubMed]
- Morgan, D.; Funk, M.; Crossley, M.; Basran, J.; Kirk, A.; Dal Bello-Haas, V. The potential of gait analysis to contribute to differential diagnosis of early stage dementia: current research and future directions. Canadian Journal on Aging/La Revue canadienne du vieillissement 2007, 26, 19–32. [Google Scholar] [CrossRef] [PubMed]
- Von Schroeder, H.P.; Coutts, R.D.; Lyden, P.D.; Billings, E.; Nickel, V.L. Gait parameters following stroke: a practical assessment. Journal of rehabilitation research and development 1995, 32, 25–25. [Google Scholar]
- Cebolla, E.C.; Rodacki, A.L.; Bento, P.C. Balance, gait, functionality and strength: comparison between elderly fallers and non-fallers. Brazilian journal of physical therapy 2015, 19, 146–151. [Google Scholar] [CrossRef] [PubMed]
- Bergen, G.; Stevens, M.R.; Burns, E.R. Falls and fall injuries among adults aged ≥ 65 years—United States, 2014. Morbidity and Mortality Weekly Report 2016, 65, 993–998. [Google Scholar] [CrossRef] [PubMed]
- Sutherland, D.H. The evolution of clinical gait analysis part I: kinesiological EMG. Gait & posture 2001, 14, 61–70. [Google Scholar]
- Sutherland, D.H. The evolution of clinical gait analysis: Part II Kinematics. Gait & posture 2002, 16, 159–179. [Google Scholar]
- Sutherland, D.H. The evolution of clinical gait analysis part III–kinetics and energy assessment. Gait & posture 2005, 21, 447–461. [Google Scholar]
- Simon, S.R. Quantification of human motion: gait analysis—benefits and limitations to its application to clinical problems. Journal of biomechanics 2004, 37, 1869–1880. [Google Scholar] [CrossRef]
- Yang, C.; Ugbolue, U.C.; Kerr, A.; Stankovic, V.; Stankovic, L.; Carse, B.; Kaliarntas, K.T.; Rowe, P.J. Autonomous gait event detection with portable single-camera gait kinematics analysis system. Journal of Sensors 2016, 2016. [Google Scholar] [CrossRef]
- Muro-De-La-Herran, A.; Garcia-Zapirain, B.; Mendez-Zorrilla, A. Gait analysis methods: An overview of wearable and non-wearable systems, highlighting clinical applications. Sensors 2014, 14, 3362–3394. [Google Scholar] [CrossRef] [PubMed]
- Tao, W.; Liu, T.; Zheng, R.; Feng, H. Gait analysis using wearable sensors. Sensors 2012, 12, 2255–2283. [Google Scholar] [CrossRef] [PubMed]
- Givon, U.; Zeilig, G.; Achiron, A. Gait analysis in multiple sclerosis: characterization of temporal–spatial parameters using GAITRite functional ambulation system. Gait & posture 2009, 29, 138–142. [Google Scholar]
- di Biase, L.; Pecoraro, P.M.; Pecoraro, G.; Caminiti, M.L.; Di Lazzaro, V. Markerless radio frequency indoor monitoring for telemedicine: gait analysis, indoor positioning, fall detection, tremor analysis, vital signs and sleep monitoring. Sensors 2022, 22, 8486. [Google Scholar] [CrossRef]
- Drira, S.; Reuland, Y.; Olsen, N.F.; Pai, S.G.; Smith, I.F. Occupant-detection strategy using footstep-induced floor vibrations. In Proceedings of the Proceedings of the 1st ACM International Workshop on Device-Free Human Sensing, 2019, pp. 31–34. [CrossRef]
- Alwan, M.; Rajendran, P.J.; Kell, S.; Mack, D.; Dalal, S.; Wolfe, M.; Felder, R. A smart and passive floor-vibration based fall detector for elderly. In Proceedings of the 2006 2nd International Conference on Information & Communication Technologies. IEEE, 2006, Vol. 1, pp. 1003–1007. [CrossRef]
- Pan, S.; Mirshekari, M.; Zhang, P.; Noh, H.Y. Occupant traffic estimation through structural vibration sensing. In Proceedings of the Sensors and Smart Structures Technologies for Civil, Mechanical, and Aerospace Systems 2016. SPIE, 2016, Vol. 9803, pp. 41–52. [CrossRef]
- Pan, S.; Berges, M.; Rodakowski, J.; Zhang, P.; Noh, H.Y. Fine-Grained Activity of Daily Living (ADL) Recognition Through Heterogeneous Sensing Systems With Complementary Spatiotemporal Characteristics. Frontiers in Built Environment 2020, 6. [Google Scholar] [CrossRef]
- Pan, S.; Yu, T.; Mirshekari, M.; Fagert, J.; Bonde, A.; Mengshoel, O.J.; Noh, H.Y.; Zhang, P. Footprintid: Indoor pedestrian identification through ambient structural vibration sensing. Proceedings of the ACM on Interactive, Mobile, Wearable and Ubiquitous Technologies 2017, 1, 1–31. [Google Scholar] [CrossRef]
- Dong, Y.; Fagert, J.; Zhang, P.; Noh, H.Y. Stranger Detection and Occupant Identification Using Structural Vibrations. In Proceedings of the European Workshop on Structural Health Monitoring: EWSHM 2022-Volume 1. Springer, 2022, pp. 905–914. [CrossRef]
- Drira, S.; Reuland, Y.; Pai, S.G.; Noh, H.Y.; Smith, I.F. Model-based occupant tracking using slab-vibration measurements. Frontiers in Built Environment 2019, 5, 63. [Google Scholar] [CrossRef]
- Davis, B.T.; Caicedo, J.M.; Hirth, V.A. Force estimation and event localization (feel) of impacts using structural vibrations. Journal of Engineering Mechanics 2021, 147, 04020154. [Google Scholar] [CrossRef]
- Mirshekari, M.; Pan, S.; Fagert, J.; Schooler, E.M.; Zhang, P.; Noh, H.Y. Occupant localization using footstep-induced structural vibration. Mechanical Systems and Signal Processing 2018, 112, 77–97. [Google Scholar] [CrossRef]
- Hahm, K.S.; Anthony, B.W. In-home Health Monitoring using Floor-based Gait Tracking. Internet of Things 2022, 19, 100541. [Google Scholar] [CrossRef]
- Dong, Y.; Liu, J.; Noh, H.Y. GaitVibe+: Enhancing Structural Vibration-based Footstep Localization Using Temporary Cameras for In-home Gait Analysis. arXiv preprint arXiv:2212.03377 2022. arXiv:2212.03377 2022. [CrossRef]
- Alwan, M.; Dalal, S.; Kell, S.; Felder, R.; et al. Derivation of basic human gait characteristics from floor vibrations. In Proceedings of the 2003 Summer Bioengineering Conference, June, 2003, pp. 25–29.
- Dong, Y.; Zou, J.J.; Liu, J.; Fagert, J.; Mirshekari, M.; Lowes, L.; Iammarino, M.; Zhang, P.; Noh, H.Y. MD-Vibe: physics-informed analysis of patient-induced structural vibration data for monitoring gait health in individuals with muscular dystrophy. In Proceedings of the Adjunct proceedings of the 2020 ACM international joint conference on pervasive and ubiquitous computing and proceedings of the 2020 ACM international symposium on wearable computers, 2020, pp. 525–531. [CrossRef]
- Dong, Y.; Noh, H.Y. Structure-Agnostic Gait Cycle Segmentation for In-Home Gait Health Monitoring through Footstep-Induced Structural Vibrations. https://doi.org/10.1007/978-3-031-36663-58. [CrossRef]
- Mirshekari, M.; Fagert, J.; Pan, S.; Zhang, P.; Noh, H.Y. Step-level occupant detection across different structures through footstep-induced floor vibration using model transfer. Journal of Engineering Mechanics 2020, 146, 04019137. [Google Scholar] [CrossRef]
- Dong, Y.; Zhu, J.; Noh, H.Y. Re-vibe: vibration-based indoor person re-identification through cross-structure optimal transport. In Proceedings of the Proceedings of the 9th ACM International Conference on Systems for Energy-Efficient Buildings, Cities, and Transportation, 2022, pp. 348–352. [CrossRef]
- Rainer, J.; Pernica, G. Vertical dynamic forces from footsteps. Canadian Acoustics 1986, 14, 12–21. [Google Scholar]
- Mazarakis, G.P.; Avaritsiotis, J.N. A prototype sensor node for footstep detection. In Proceedings of the Proceeedings of the Second European Workshop on Wireless Sensor Networks, 2005. IEEE, 2005, pp. 415–418. [CrossRef]
- Allen, D.E.; Pernica, G. Control of floor vibration; Institute for Research in Construction Ottawa, 1998.
- Toratti, T.; Talja, A. Classification of human induced floor vibrations. Building acoustics 2006, 13, 211–221. [Google Scholar] [CrossRef]
- Krohn, C.E. Geophone ground coupling. Geophysics 1984, 49, 722–731. [Google Scholar] [CrossRef]
- Öberg, T.; Karsznia, A.; Öberg, K. Basic gait parameters: reference data for normal subjects, 10-79 years of age. Journal of rehabilitation research and development 1993, 30, 210–210. [Google Scholar]
- Hof, A.L.; van Bockel, R.M.; Schoppen, T.; Postema, K. Control of lateral balance in walking: experimental findings in normal subjects and above-knee amputees. Gait & posture 2007, 25, 250–258. [Google Scholar]
- Patterson, K.K.; Gage, W.H.; Brooks, D.; Black, S.E.; McIlroy, W.E. Evaluation of gait symmetry after stroke: A comparison of current methods and recommendations for standardization. Gait & Posture 2010, 31, 241–246. [Google Scholar] [CrossRef]
- Godi, M.; Franchignoni, F.; Caligari, M.; Giordano, A.; Turcato, A.M.; Nardone, A. Comparison of reliability, validity, and responsiveness of the mini-BESTest and Berg Balance Scale in patients with balance disorders. Physical therapy 2013, 93, 158–167. [Google Scholar] [CrossRef]
- Brach, J.S.; Studenski, S.; Perera, S.; VanSwearingen, J.M.; Newman, A.B. Stance time and step width variability have unique contributing impairments in older persons. Gait & posture 2008, 27, 431–439. [Google Scholar]
- Oetgen, M.E.; Peden, S. Idiopathic toe walking. JAAOS-Journal of the American Academy of Orthopaedic Surgeons 2012, 20, 292–300. [Google Scholar] [CrossRef]
- Alvarez, C.; De Vera, M.; Beauchamp, R.; Ward, V.; Black, A. Classification of idiopathic toe walking based on gait analysis: development and application of the ITW severity classification. Gait & posture 2007, 26, 428–435. [Google Scholar]
- Hicks, R.; Durinick, N.; Gage, J.R. Differentiation of idiopathic toe-walking and cerebral palsy. Journal of pediatric orthopedics 1988, 8, 160–163. [Google Scholar] [CrossRef]
- Sensor Nederlands, B. SM-24 geophone element. Online: http://www. iongeo. com/Products_Services/Land_Systems/Geophones.
- Chen, J.; Benesty, J.; Huang, Y.; Doclo, S. New insights into the noise reduction Wiener filter. IEEE Transactions on audio, speech, and language processing 2006, 14, 1218–1234. [Google Scholar] [CrossRef]
- Büssow, R. An algorithm for the continuous Morlet wavelet transform. Mechanical Systems and Signal Processing 2007, 21, 2970–2979. [Google Scholar] [CrossRef]
- Brach, J.S.; Perera, S.; Studenski, S.; Katz, M.; Hall, C.; Verghese, J. Meaningful change in measures of gait variability in older adults. Gait & Posture 2010, 31, 175–179. [Google Scholar]
- Fagert, J.; Mirshekari, M.; Pan, S.; Lowes, L.; Iammarino, M.; Zhang, P.; Noh, H.Y. Structure-and sampling-adaptive gait balance symmetry estimation using footstep-induced structural floor vibrations. Journal of Engineering Mechanics 2021, 147, 04020151. [Google Scholar] [CrossRef]
- Windolf, M.; Götzen, N.; Morlock, M. Systematic accuracy and precision analysis of video motion capturing systems—exemplified on the Vicon-460 system. Journal of biomechanics 2008, 41, 2776–2780. [Google Scholar] [CrossRef] [PubMed]
- Manual, M.S.U. DAQ M Series 2008.
- Wall, J.; Crosbie, J. Accuracy and reliability of temporal gait measurement. Gait & Posture 1996, 4, 293–296. [Google Scholar]
- Xu, X.; McGorry, R.W.; Chou, L.S.; Lin, J.h.; Chang, C.c. Accuracy of the Microsoft Kinect™ for measuring gait parameters during treadmill walking. Gait & posture 2015, 42, 145–151. [Google Scholar]
- Mansour, K.B.; Rezzoug, N.; Gorce, P. Analysis of several methods and inertial sensors locations to assess gait parameters in able-bodied subjects. Gait & Posture 2015, 42, 409–414. [Google Scholar]
- Stolze, H.; Kuhtz-Buschbeck, J.; Mondwurf, C.; Jöhnk, K.; Friege, L. Retest reliability of spatiotemporal gait parameters in children and adults. Gait & posture 1998, 7, 125–130. [Google Scholar]
- Enright, P.L.; Sherrill, D.L. Reference equations for the six-minute walk in healthy adults. American journal of respiratory and critical care medicine 1998, 158, 1384–1387. [Google Scholar] [CrossRef] [PubMed]
- Roether, C.L.; Omlor, L.; Christensen, A.; Giese, M.A. Critical features for the perception of emotion from gait. Journal of vision 2009, 9, 15–15. [Google Scholar] [CrossRef]
- Doi, T.; Yamaguchi, R.; Asai, T.; Komatsu, M.; Makiura, D.; Shimamura, M.; Hirata, S.; Ando, H.; Kurosaka, M. The effects of shoe fit on gait in community-dwelling older adults. Gait & posture 2010, 32, 274–278. [Google Scholar]
- Uhlrich, S.D.; Falisse, A.; Kidziński, .; Muccini, J.; Ko, M.; Chaudhari, A.S.; Hicks, J.L.; Delp, S.L. OpenCap: 3D human movement dynamics from smartphone videos. BioRxiv 2022, pp. 2022–07.
- Abinaya, B.; Latha, V.; Suchetha, M. An advanced gait monitoring system based on air pressure sensor embedded in a shoe. Procedia Engineering 2012, 38, 1634–1643. [Google Scholar] [CrossRef]
- Lin, F.; Wang, A.; Zhuang, Y.; Tomita, M.R.; Xu, W. Smart Insole: A Wearable Sensor Device for Unobtrusive Gait Monitoring in Daily Life. IEEE Transactions on Industrial Informatics 2016, 12, 2281–2291. [Google Scholar] [CrossRef]
- Wei, J. Comparing the MEMS accelerometer and the analog geophone. The Leading Edge 2013, 32, 1206–1210. [Google Scholar] [CrossRef]
| Gait Parameter | Mean (Ours) | Std (Ours) | Mean (Prev.1) | Std (Prev.1) |
|---|---|---|---|---|
| Walking Speed (m/s) | 1.184 | 0.140 | 1.267 | 0.209 |
| Cadence (step/min) | 104.1 | 8.566 | 114.0 | 9.300 |
| Step Time (s) | 0.581 | 0.046 | 0.541 | 0.041 |
| Stride Time (s) | 1.258 | 0.172 | 1.090 | 0.100 |
| Stance Time (s) | 0.747 | 0.066 | 0.632 | 0.045 |
| Swing Time (s) | 0.415 | 0.033 | 0.418 | 0.025 |
| Single-support Time (s) | 0.415 | 0.033 | 0.415 | 0.025 |
| Double-support Time (s) | 0.167 | 0.026 | 0.133 | 0.030 |
| Step Length (m) | 0.678 | 0.062 | 0.613 | 0.049 |
| Step Width (m) | 0.086 | 0.023 | 0.091 | 0.024 |
| Step Angle (°) | 4.123 | 1.287 | 4.290 | 1.800 |
| Stride Length (m) | 1.415 | 0.214 | 1.398 | 0.150 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




