Submitted:
23 February 2024
Posted:
23 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
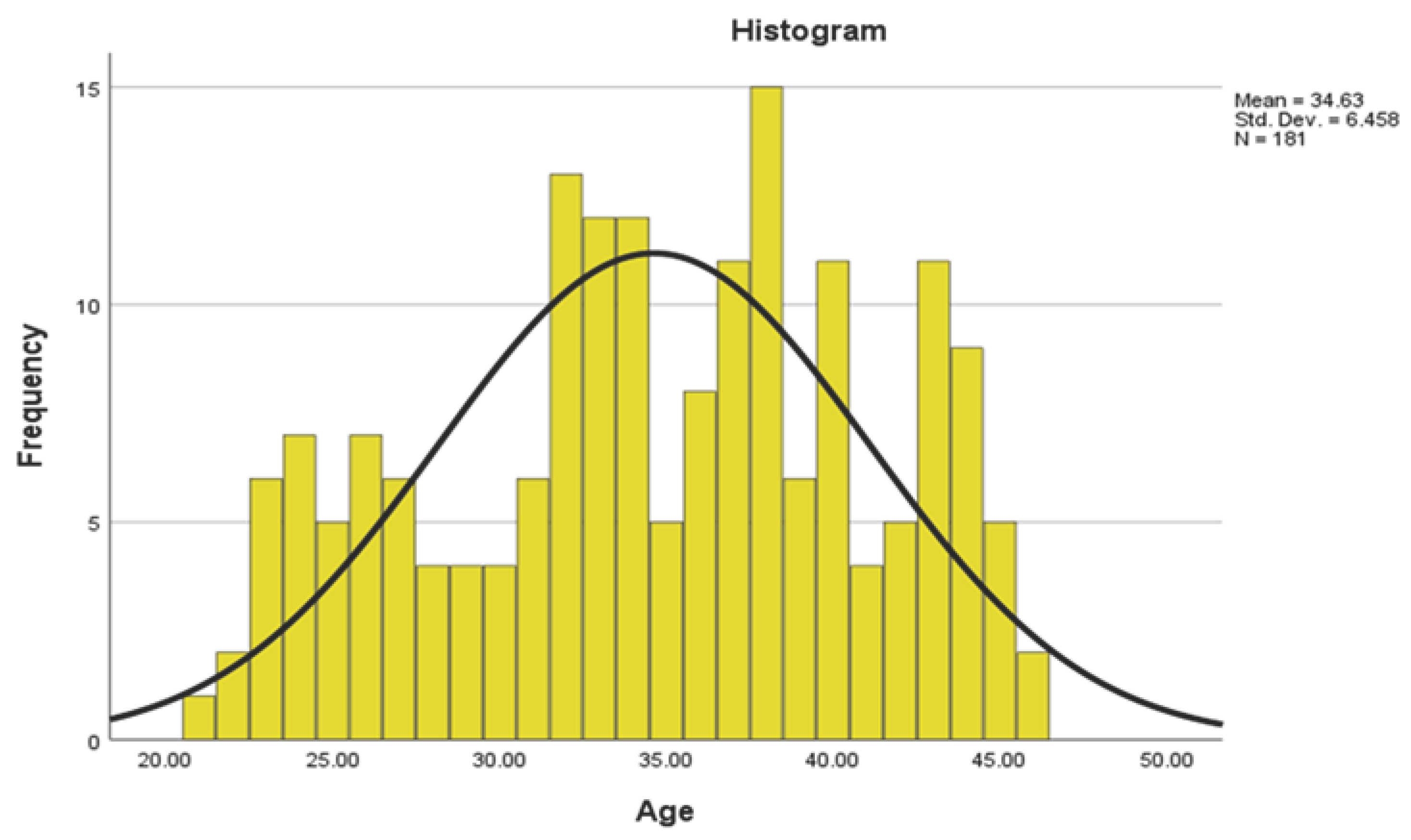
3.1. Maternal age
3.2. Maternal characteristics
3.3. Neonatal outcome
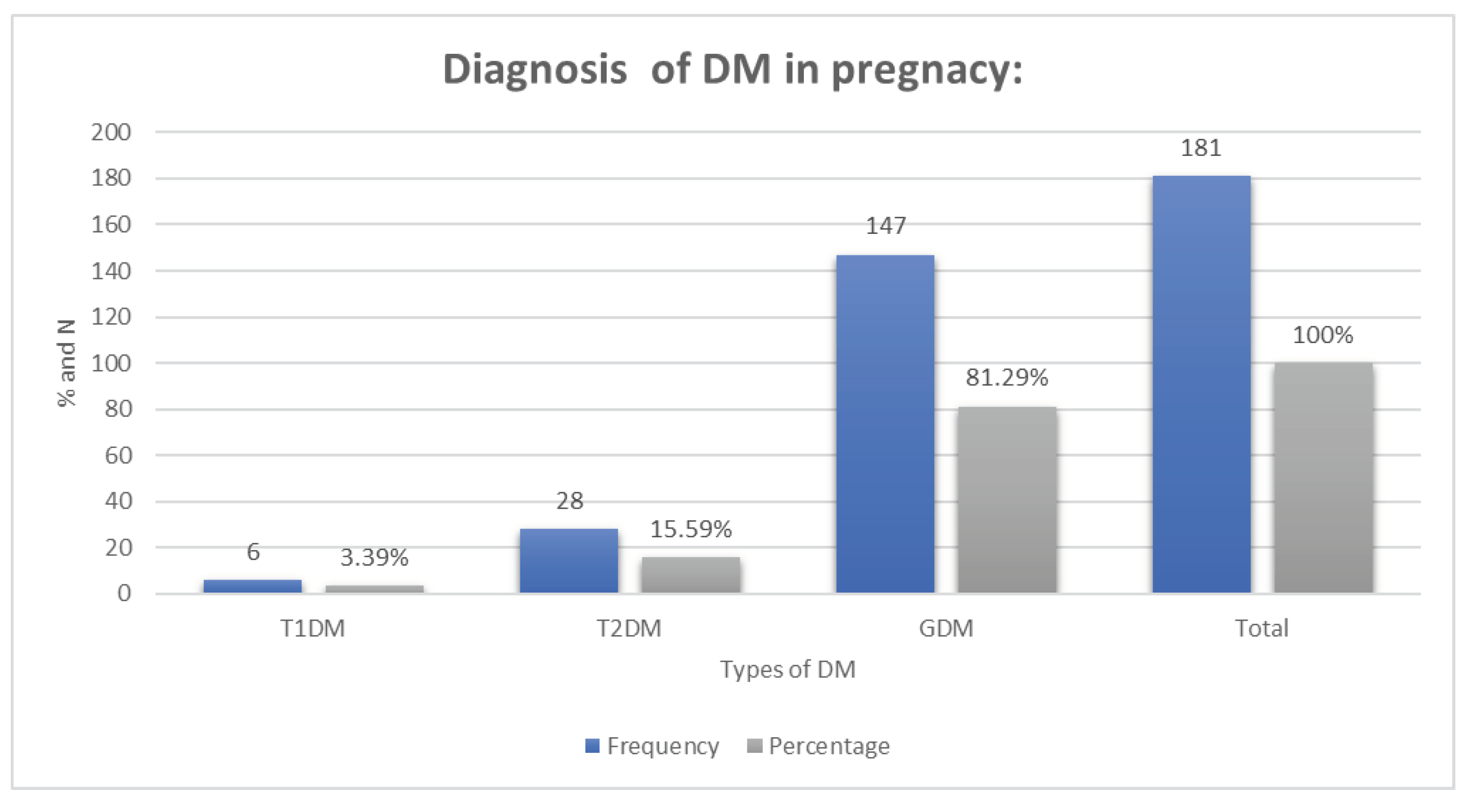
3.4. Diagnosis of DM in pregnancy
3.5. Logistics regression
4. Discussion
5. Conclusions and recommendation
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Cho NH, Shaw JE, Karuranga S, Huang Y, da Rocha Fernandes JD, Ohlrogge AW, Malanda BI. IDF Diabetes Atlas: Global estimates of diabetes prevalence for 2017 and projections for 2045. Diabetes research and clinical practice. 2018 Apr 1;138:271-81. [CrossRef]
- American Diabetes Association. 2. Classification and diagnosis of diabetes: standards of medical care in diabetes—2021. Diabetes care. 2021 Jan 1;44(Supplement_1):S15-33. [CrossRef]
- Prakash GT, Das AK, Habeebullah S, Bhat V, Shamanna SB. Maternal and neonatal outcome in mothers with gestational diabetes mellitus. Indian journal of endocrinology and metabolism. 2017 Nov;21(6):854. [CrossRef]
- Shahbazian H, Nouhjah S, Shahbazian N, Jahanfar S, Latifi SM, Aleali A, Shahbazian N, Saadati N. Gestational diabetes mellitus in an Iranian pregnant population using IADPSG criteria: Incidence, contributing factors and outcomes. Diabetes & Metabolic Syndrome: Clinical Research & Reviews. 2016 Oct 1;10(4):242-6. [CrossRef]
- Alqurashi KA, Aljabri KS, Bokhari SA. Prevalence of diabetes mellitus in a Saudi community. Annals of Saudi medicine. 2011 Jan;31(1):19-23. [CrossRef]
- Gojnic M, Todorovic J, Stanisavljevic D, Jotic A, Lukic L, Milicic T, Lalic N, Lalic K, Stoiljkovic M, Stanisavljevic T, Stefanovic A. Maternal and fetal outcomes among pregnant women with diabetes. International Journal of Environmental Research and Public Health. 2022 Mar 20;19(6):3684. [CrossRef]
- Alsaedi SA, Altalhi AA, Nabrawi MF, Aldainy AA, Wali RM. Prevalence and risk factors of gestational diabetes mellitus among pregnant patients visiting National Guard primary health care centers in Saudi Arabia. Saudi medical journal. 2020 Feb;41(2):144. [CrossRef]
- Wahabi H, Fayed A, Esmaeil S, Mamdouh H, Kotb R. Prevalence and complications of pregestational and gestational diabetes in Saudi women: analysis from Riyadh Mother and Baby cohort study (RAHMA). BioMed research international. 2017 Oct;2017. [CrossRef]
- Gasim, T. Gestational diabetes mellitus: maternal and perinatal outcomes in 220 Saudi women. Oman medical journal. 2012 Mar;27(2):140. [CrossRef]
- Mitanchez D, Yzydorczyk C, Simeoni U. What neonatal complications should the pediatrician be aware of in case of maternal gestational diabetes? World J Diabetes. 2015; 6 (5): 734–43. [CrossRef]
- Gualdani E, Di Cianni G, Seghieri M, Francesconi P, Seghieri G. Pregnancy outcomes and maternal characteristics in women with pregestational and gestational diabetes: A retrospective study on 206,917 singleton live births. Acta Diabetologica. 2021 Sep;58:1169-76. [CrossRef]
- Behboudi-Gandevani S, Amiri M, Bidhendi Yarandi R, Ramezani Tehrani F. The impact of diagnostic criteria for gestational diabetes on its prevalence: a systematic review and meta-analysis. Diabetology & metabolic syndrome. 2019 Dec;11(1):1-8. [CrossRef]
- Anjum SK, Yashodha HT. A study of neonatal outcome in infants born to diabetic mothers at a tertiary care hospital. Int J Contemp Pediatr. 2018 Mar;5(2):489-92. [CrossRef]
- Mackin ST, Nelson SM, Kerssens JJ, Wood R, Wild S, Colhoun HM, Leese GP, Philip S, Lindsay RS. Diabetes and pregnancy: national trends over a 15 year period. Diabetologia. 2018 May;61(5):1081-8. [CrossRef]
- Ali DS, Davern R, Rutter E, Coveney C, Devine H, Walsh JM, Higgins M, Hatunic M. Pre-gestational diabetes and pregnancy outcomes. Diabetes Therapy. 2020 Dec;11:2873-85. [CrossRef]
- Seghieri G, Di Cianni G, Seghieri M, Lacaria E, Corsi E, Lencioni C, Gualdani E, Voller F, Francesconi P. Risk and adverse outcomes of gestational diabetes in migrants: A population cohort study. Diabetes Research and Clinical Practice. 2020 May 1;163:108128. [CrossRef]
- Muche AA, Olayemi OO, Gete YK. Effects of gestational diabetes mellitus on risk of adverse maternal outcomes: a prospective cohort study in Northwest Ethiopia. BMC pregnancy and childbirth. 2020 Dec;20(1):1-3. [CrossRef]
- Alfadhli EM, Osman EN, Basri TH, Mansuri NS, Youssef MH, Assaaedi SA, Aljohani BA. Gestational diabetes among Saudi women: prevalence, risk factors and pregnancy outcomes. Annals of Saudi medicine. 2015 May;35(3):222-30. [CrossRef]
- Ovesen PG, Jensen DM, Damm P, Rasmussen S, Kesmodel US. Maternal and neonatal outcomes in pregnancies complicated by gestational diabetes. A nation-wide study. The Journal of Maternal-Fetal & Neonatal Medicine. 2015 Sep 22;28(14):1720-4. [CrossRef]
- Kruit H, Mertsalmi S, Rahkonen L. Planned vaginal and planned cesarean delivery outcomes in pregnancies complicated with pregestational type 1 diabetes–A three-year academic tertiary hospital cohort study. BMC Pregnancy and Childbirth. 2022 Mar 2;22(1):173. [CrossRef]
- Magro-Malosso ER, Saccone G, Chen M, Navathe R, Di Tommaso M, Berghella V. Induction of labour for suspected macrosomia at term in non-diabetic women: a systematic review and meta-analysis of randomized controlled trials. BJOG: An International Journal of Obstetrics & Gynaecology. 2017 Feb;124(3):414-21. [CrossRef]
- Bayoumi MA, Masri RM, Matani N, Hendaus MA, Masri MM, Chandra P, Langtree LJ, D’Souza S, Olayiwola NO, Shahbal S, Elmalik EE. Maternal and neonatal outcomes in mothers with diabetes mellitus in Qatari population. BMC pregnancy and childbirth. 2021 Dec;21(1):1-1. [CrossRef]
- Li MF, Ma L, Yu TP, Zhu Y, Chen MY, Liu Y, Li LX. Adverse maternal and neonatal outcomes in pregnant women with abnormal glucose metabolism. Diabetes Research and Clinical Practice. 2020 Mar 1;161:108085. [CrossRef]
- Silva AL, Amaral AR, Oliveira DS, Martins L, Silva MR, Silva JC. Desfechos neonatais de acordo com diferentes terapêuticas do diabetes mellitus gestacional. Jornal de Pediatria. 2017 Jan;93:87-93. [CrossRef]
- Yang GR, Dye TD, Li D. Effects of pre-gestational diabetes mellitus and gestational diabetes mellitus on macrosomia and birth defects in upstate New York. Diabetes research and clinical practice. 2019 Sep 1;155:107811. [CrossRef]
- Hoang TT, Marengo LK, Mitchell LE, Canfield MA, Agopian AJ. Original findings and updated meta-analysis for the association between maternal diabetes and risk for congenital heart disease phenotypes. American journal of epidemiology. 2017 Jul 1;186(1):118-28. [CrossRef]
- He XJ, Qin FY, Hu CL, Zhu M, Tian CQ, Li L. Is gestational diabetes mellitus an independent risk factor for macrosomia: a meta-analysis?. Archives of gynecology and obstetrics. 2015 Apr;291:729-35. [CrossRef]
- Al-Qahtani, MH. Infants of diabetic mothers: 4 years analysis of neonatal care unit in a teaching hospital, Saudi Arabia. Saudi Journal of Medicine and Medical Sciences. 2014 Sep 1;2(3):151. [CrossRef]
- Li Y, Wang W, Zhang D. Maternal diabetes mellitus and risk of neonatal respiratory distress syndrome: a meta-analysis. Acta diabetologica. 2019 Jul 1;56:729-40. [CrossRef]
- Capobianco G, Gulotta A, Tupponi G, Dessole F, Virdis G, Cherchi C, De Vita D, Petrillo M, Olzai G, Antonucci R, Saderi L. Fetal Growth and Neonatal Outcomes in Pregestational Diabetes Mellitus in a Population with a High Prevalence of Diabetes. Journal of Personalized Medicine. 2022 Aug 16;12(8):1320. [CrossRef]
- Birch MN, Frank Z, Caughey AB. Rates of neonatal sepsis by maternal diabetes and chronic hypertension [12D]. Obstetrics & Gynecology. 2019 May 1;133:45S-4S. [CrossRef]
- Stacey T, Tennant PW, McCowan LM, Mitchell EA, Budd J, Li M, Thompson JM, Martin B, Roberts D, Heazell AE. Gestational diabetes and the risk of late stillbirth: a case–control study from England, UK. BJOG: An International Journal of Obstetrics & Gynaecology. 2019 Jul;126(8):973-82. [CrossRef]
- Battarbee AN, Venkatesh KK, Aliaga S, Boggess KA. The association of pregestational and gestational diabetes with severe neonatal morbidity and mortality. Journal of Perinatology. 2020 Feb;40(2):232-9. [CrossRef]
| Maternal characteristics: | T1DM | T2DM | GDM | Total | p- Value | |
|---|---|---|---|---|---|---|
| Nationality | Saudi | 6 | 26 | 136 | 168 (92.8%) | 0.056 |
| Non-Saudi | 0 | 2 | 11 | 13 (7.2%) | ||
| Region: | City (urban) | 5 | 24 | 119 | 148 (81.8%) | |
| Village (rural) | 1 | 1 | 24 | 26 (14.4%) | 0.076 | |
| Outside the region | 0 | 3 | 4 | 7 (3.9%) | ||
| Family history of diabetes | Yes | 0 | 7 | 33 | 40 (22.1%) |
0.061 |
| No | 6 | 21 | 114 | 141 (77.9%) | ||
| Time diagnosed DM | Before pregnancy (pre-GDM) | 6 | 28 | 0 | 34 (18.8%) |
0.010* |
| During pregnancy (GDM) | 0 | 0 | 147 | 147 (81.2%) | ||
| Number of pregnancies | 1-2 | 4 | 6 | 56 | 66 (36.5%) | |
| 3-4 | 2 | 13 | 61 | 76 (42%) | 0.074 | |
| More than 5 | 0 | 9 | 30 | 39 (21.5%) | ||
| Types of delivery | Vaginal | 0 | 1 | 8 | 9 (5%) | 0.049* |
| CS | 6 | 27 | 139 | 172 (95%) | ||
| History of neonatal death | Yes | 1 | 3 | 8 | 12 (6.6%) | 0.096 |
| No | 5 | 25 | 139 | 169 (93.4%) | ||
| Birth weight | <2.5 LBW | 5 | 5 | 11 | 21 (11.6%) | |
| 2.5-3.99 Normal | 1 | 20 | 107 | 128 (70.7%) | 0.078 | |
| ≥4 more than 4 kg (Macrosomia) | 0 | 3 | 29 | 32 (17.7%) |
| Neonatal outcome: | T1DM | T2DM | GDM | Total | p-Value | |
|---|---|---|---|---|---|---|
| RDS | 2 | 3 | 11 | 16 (8.8%) | 0.102 | |
| Prematurity | 1 | 0 | 0 | 1 (0.6%) | 0.128 | |
| Hypoglycemia | 0 | 0 | 1 | 1 (0.6%) | 0.017* | |
| Congenital heart disease | 0 | 13 | 26 | 39 (21.5%) | 0.076 | |
| Development and Growth disorder | 0 | 2 | 0 | 2 (1.1%) | 0.062 | |
| DM | 0 | 1 | 2 | 3 (1.7%) | 0.073 | |
| LBW | 5 | 5 | 11 | 21 (11.6%) | 0.106 | |
| More than 4 kg (Macrosomia) | 0 | 3 | 25 | 28 (15.5%) | 0.050* | |
| Sepsis | 2 | 1 | 9 | 12 (6.6%) | 0.111 | |
| Neonatal death | 0 | 0 | 1 | 1 (0.6%) | 0.017* | |
| Normal | 1 | 9 | 77 | 87 (48.06%) | 0.066 | |
| Neonatal outcomes | Cure | 3 | 11 | 92 | 106 (59.6%) | |
| Died | 0 | 0 | 1 | 1 (0.6%) | 0.080 | |
| Developed complications then improve | 2 | 15 | 49 | 66 (36.5%) | ||
| Developed complication | 1 | 2 | 5 | 8 (4.4%) | ||
| NICU admission | 3 | 13 | 49 | 65 (35.9%) | 0.077 |
| Neonatal outcomes in MDM mothers: | Odd ratio (OR), 95% Confidence interval (CI) |
|---|---|
| Macrosomia | OR = 1.74, 95% CI: 1.38-2.19 |
| LBW | OR = 1.32, 95% CI: 1.06-1.66 |
| RDS | OR = 1.57, 95% CI: 1.28-1.93 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




