Submitted:
20 February 2024
Posted:
21 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Demographics and Baseline Patient Characteristics
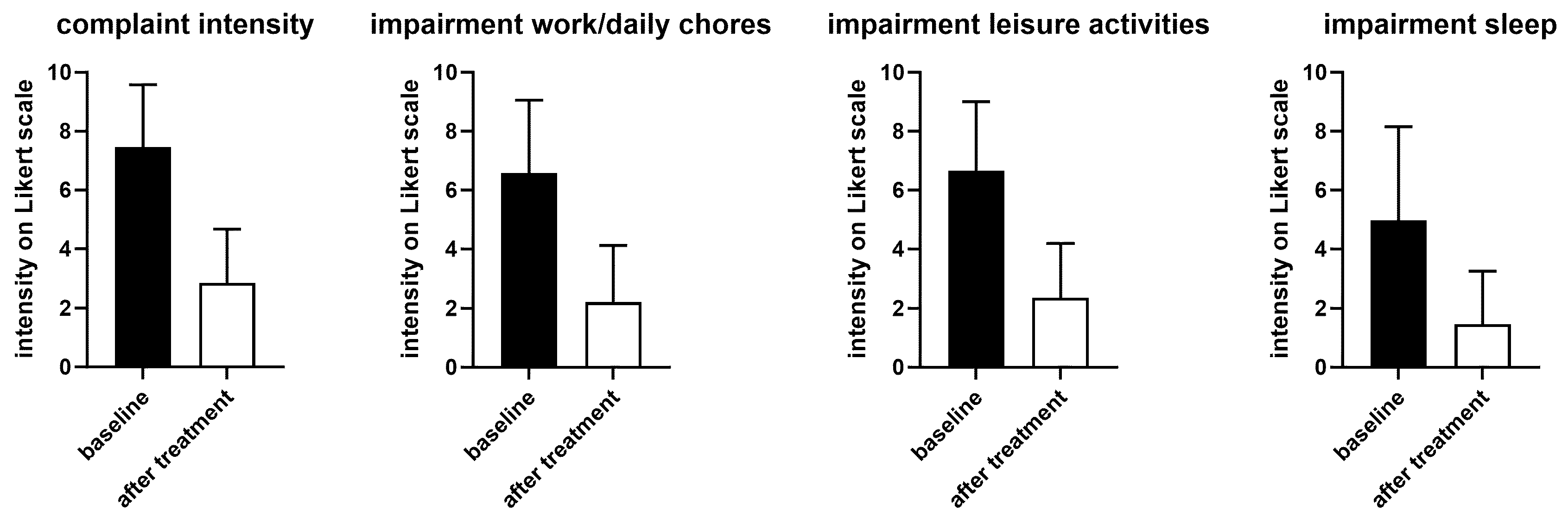
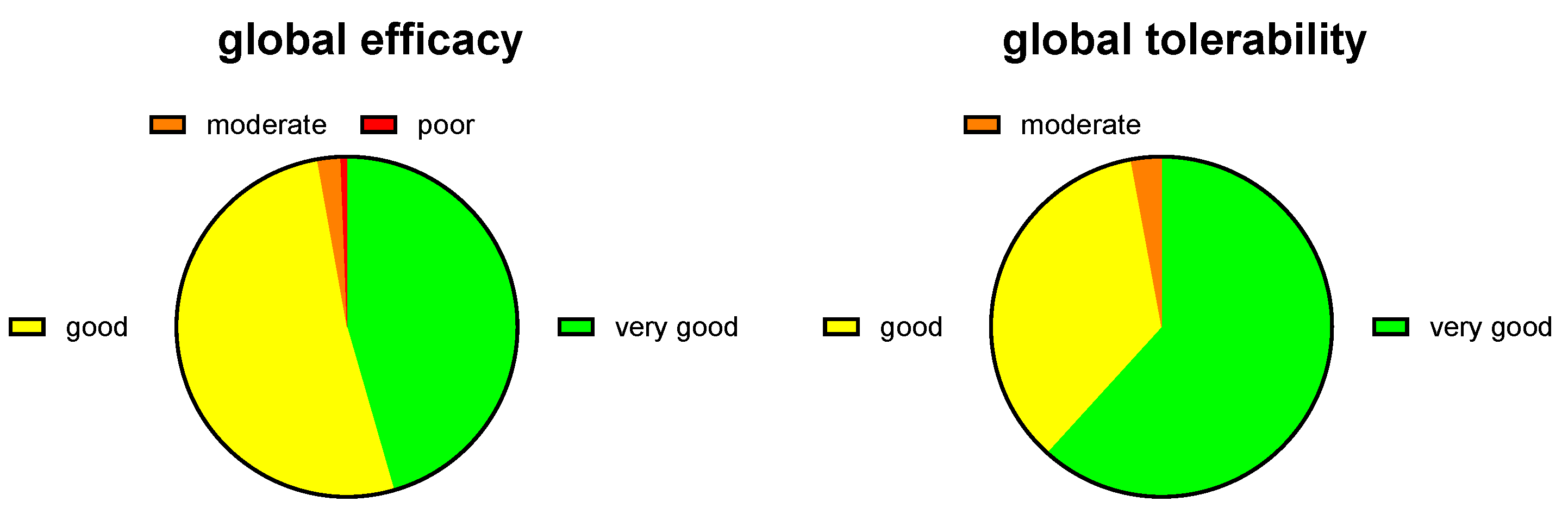
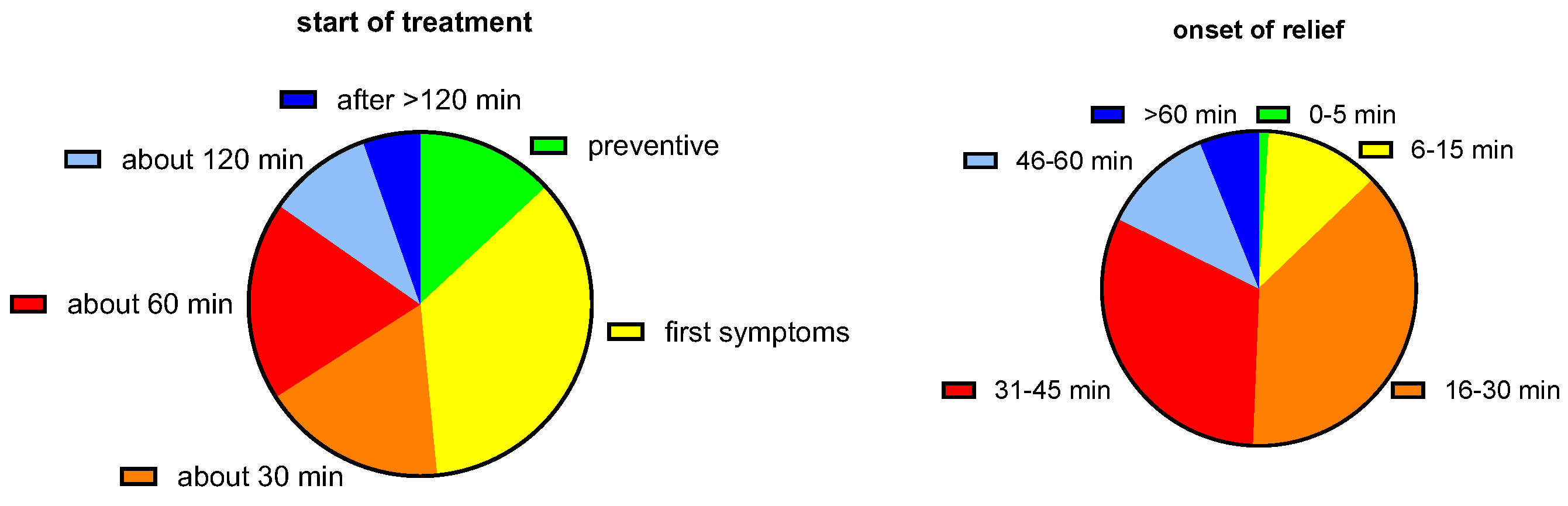
3.2. Treatment Responses
4. Discussion
4.1. Critique of Methods
4.2. Characterization of Women Using PLUS for the Treatment of Dysmenorrhea Symptoms
4.3. Outcomes in Women Using PLUS for the Treatment of Dysmenorrhea Symptoms
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Ju, H.; Jones, M.; Mishra, G. The prevalence and risk factors of dysmenorrhea. Epidemiol. Rev. 2014, 36, 104–113. [Google Scholar] [CrossRef] [PubMed]
- Osayande, A.S.; Mehulic, S. Diagnosis and initial management of dysmenorrhea. Am. Fam. Physician 2014, 89, 341–346. [Google Scholar]
- McKenna, K.A.; Fogleman, C.D. Dysmenorrhea. Am. Fam. Physician 2021, 104, 164–170. [Google Scholar] [PubMed]
- Grandi, G.; Ferrari, S.; Xholli, A.; Cannoletta, M.; Palma, F.; Romani, C.; Volpe, A.; Cagnacci, A. Prevalence of menstrual pain in young women: what is dysmenorrhea? J. Pain Res. 2012, 5, 169–174. [Google Scholar] [CrossRef] [PubMed]
- Schwab, R.; Anić, K.; Stewen, K.; Schmidt, M.W.; Kalb, S.R.; Kottmann, T.; Brenner, W.; Domidian, J.S.; Krajnak, S.; Battista, M.J.; Hasenburg, A. Pain experience and social support of endometriosis patients during the COVID-19 pandemic in Germany - results of a web-based cross-sectional survey. PLoS One 2021, 16, e0256433. [Google Scholar] [CrossRef]
- Schwab, R.; Stewen, K.; Kottmann, T.; Anic, K.; Schmidt, M.W.; Elger, T.; Theis, S.; Kalb, S.R.; Brenner, W.; Hasenburg, A. Mental health and social support are key predictors of resilience in German women with endometriosis during the COVID-19 pandemic. J Clin Med 2022, 11. [Google Scholar] [CrossRef]
- Shrestha, R.; Bhandari, M.S.; Shrestha, S.S.; Shrestha, J.T.M.; Shrestha, U. Self-medication in Primary Dysmenorrhea among Undergraduate Students in a Medical College: A Descriptive Cross-sectional Study. JNMA J. Nepal Med. Assoc. 2022, 60, 1011–1015. [Google Scholar] [CrossRef]
- Schwab, R.; Stewen, K.; Kottmann, T.; Schmidt, M.W.; Anic, K.; Theis, S.; Hamoud, B.H.; Elger, T.; Brenner, W.; Hasenburg, A. Factors Associated with Increased Analgesic Use in German Women with Endometriosis during the COVID-19 Pandemic. J Clin Med 2022, 11. [Google Scholar] [CrossRef]
- Tytgat, G.N. Hyoscine butylbromide: a review of its use in the treatment of abdominal cramping and pain. Drugs 2007, 67, 1343–1357. [Google Scholar] [CrossRef]
- Jesuíno, F.; Reis, J.P.; Whitaker, J.C.P.; Campos, A.; Pastor, M.V.D.; Cechinel Filho, V.; Quintão, N.L.M. Effect of Synadenium grantii and its isolated compound on dysmenorrhea behavior model in mice. Inflammopharmacology 2019, 27, 613–620. [Google Scholar] [CrossRef]
- Picallo, R. [Treatment of dysmenorrhea with buscopan compositum]. Rev. Esp. Obstet. Ginecol. 1958, 17, 219–222. [Google Scholar] [PubMed]
- Odeblad, E. The therapeutic efficacy of Buscopan in primary dysmenorrhea. Z.Ther. 1975, 13, 473–475. [Google Scholar]
- Hernández Bueno, J.A.; de la Jara Díaz, J.; Sedeño Cruz, F.; Llorens Torres, F. [Analgesic-antispasmodic effect and safety of lysine clonixinate and L-hyoscinbutylbromide in the treatment of dysmenorrhea]. Ginecol. Obstet. Mex. 1998, 66, 35–39. [Google Scholar]
- de los Santos, A.R.; Zmijanovich, R.; Pérez Macri, S.; Martí, M.L.; Di Girolamo, G. Antispasmodic/analgesic associations in primary dysmenorrhea double-blind crossover placebo-controlled clinical trial. Int. J. Clin. Pharmacol. Res. 2001, 21, 21–29. [Google Scholar]
- Storr, M.; Weigmann, H.; Landes, S.; Michel, M.C. Self-medication for the treatment of abdominal cramps and pain - a real-life comparison of three frequently used preparations. Journal of Clinical Medicine 2022, 11, 6361. [Google Scholar] [CrossRef] [PubMed]
- Davis, S.R.; Lambrinoudaki, I.; Lumsden, M.; Mishra, G.D.; Pal, L.; Rees, M.; Santoro, N.; Simoncini, T. Menopause. Nat Rev Dis Primers 2015, 1, 15004. [Google Scholar] [CrossRef]
- Gaul, C.; Gräter, H.; Weiser, T. Results from a pharmacy-based patient survey on the use of a fixed combination analgesic containing acetylsalicylic acid, paracetamol and caffeine by self-diagnosing and self-treating patients. Springerplus 2016, 5, 721. [Google Scholar] [CrossRef]
- Klimek, L.; Schumacher, H.; Schütt, T.; Gräter, H.; Mück, T.; Michel, M.C. Factors associated with efficacy of an ibuprofen/pseudoephedrine combination drug in pharmacy customers with common cold symptoms. Int. J. Clin. Pract. 2017, 71, e12907. [Google Scholar] [CrossRef]
- Kardos, P.; Beeh, K.-M.; Sent, U.; Mueck, T.; Gräter, H.; Michel, M.C. Characterization of differential patient profiles and therapeutic responses of pharmacy customers for four ambroxol formulations. BMC Pharmacology and Toxicology 2018, 19, 40. [Google Scholar] [CrossRef]
- Gaul, C.; Gräter, H.; Weiser, T.; Michel, M.C.; Lampert, A.; Plomer, M.; Förderreuther, S. Impact of the neck and/or shoulder pain on self-reported headache treatment responses – results from a pharmacy-based patient survey. Front. Neurol. 2022, 13, 902020. [Google Scholar] [CrossRef]
- Müller-Lissner, S.; Schäfer, E.; Kondla, A. Symptoms and their interpretation in patients self-treating abdominal cramping and pain with a spasmolytic (butylscoplolamine bromide) - a pharmacy-based survey. Pharmacology & Pharmacy 2011, 2, 82–87. [Google Scholar] [CrossRef]
- Vollert, J.; Schenker, E.; Macleod, M.; Bespalov, A.; Wuerbel, H.; Michel, M.; Dirnagl, U.; Potschka, H.; Waldron, A.-M.; Wever, K.; et al. Systematic review of guidelines for internal validity in the design, conduct and analysis of preclinical biomedical experiments involving laboratory animals. BMJ Open Science 2020, 4, e100046. [Google Scholar] [CrossRef]
- Michel, M.C.; Murphy, T.J.; Motulsky, H.J. New author guidelines for displaying data and reporting data analysis and statistical methods in experimental biology. Drug Metabolism and Disposition 2020, 48, 64–74. [Google Scholar] [CrossRef]
- Amrhein, V.; Greenland, S.; McShane, B. Scientists rise up against statistical significance. Nature 2019, 567, 305–307. [Google Scholar] [CrossRef] [PubMed]
- Göbel, H.; Gessner, U.; Petersen-Braun, M.; Weingärtner, U. Acetylsalicylic acid in self-medication of migraine. A pharmacy-based observational study. Schmerz 2007, 21, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Michel, M.C.; Murphy, T.J.; Motulsky, H.J. New author guidelines for displaying data and reporting data analysis and statistical methods in experimental biology. J. Pharmacol. Exp. Ther. 2020, 372, 136–147. [Google Scholar] [CrossRef] [PubMed]
| Complaint | Incidence (number of days/month) |
|---|---|
| Complaints in the past 30 days | |
| Cramps and pain | 4.51 ± 3.97 (3; 2-5)) |
| Bloating | 4.34 ± 5.42 (3; 0-6) |
| Flatulence | 4.54 ± 6.03 (2; 0-7) |
| Trigger | Incidence (%) |
|---|---|
| Stress | 80 (25.3) |
| Bloating | 57 (18.0) |
| Nutrition | 45 (14.2) |
| Too little physical activity | 30 (9.5) |
| Food intolerance | 30 (9.5) |
| Sluggish bowels | 28 (8.9) |
| Constipation | 27 (8.5) |
| Flatulence | 25 (7.9) |
| Diarrhea | 18 (5.7) |
| Unfavorable intestinal bacteria | 14 (4.4) |
| Infection | 12 (3.8) |
| Heartburn | 9 (2.8) |
| Environmental pollution | 4 (1.3) |
| Other | 193 (61.1) |
| Unknown | 29 (9.2) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




