Submitted:
16 February 2024
Posted:
19 February 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Materials and Methods
Histopathologic Assessment
Biochemical Assessment
Measurements of TAS/TOS
TAS Measurement
TOS Measurement
Oxidative Stress Index
Paraoxanase (PON) Measurement
Statistical Analysis
Results
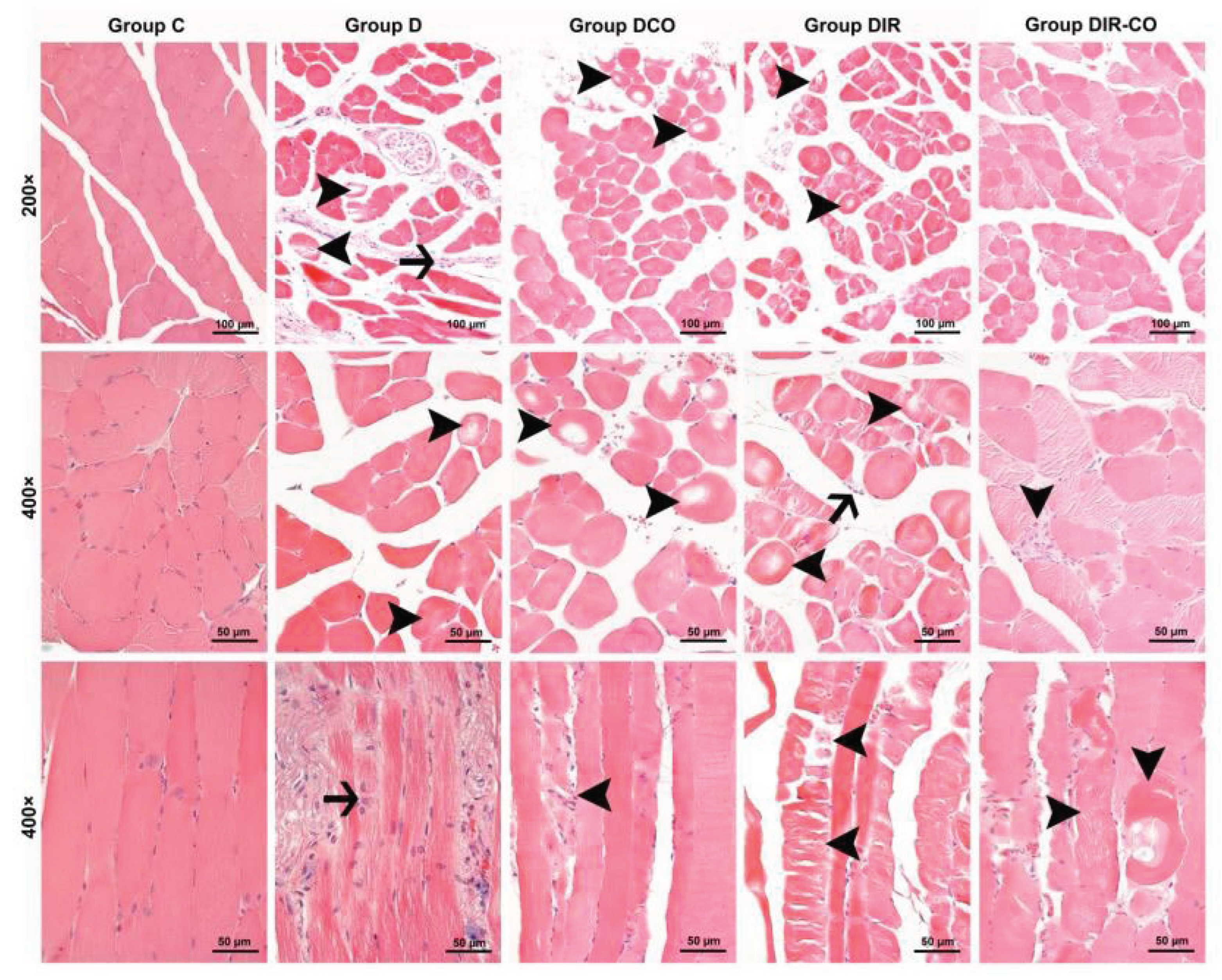
Histopathologic Findings
Biochemical Findings
Discussion
Author Contributions
Funding
Ethics approval and consent to participate
Patient Consent for Publication
Availability of data and materials
Acknowledgments
Competing interests
References
- Corrick RM, Tu H, Zhang D, Barksdale A.N, Muelleman R.L, Wadman M.C et al. Dexamethasone protects against tourniquet-induced acute ischemia-reperfusion injury in mouse hindlimb. Front Physiol, 2018; 9: 244. [CrossRef]
- Dong X, Xing Q, Li Y, Han X, Sun L. Dexmedetomidine protects against ischemia reperfusion injury in rat skeletal muscle. J Surg Res 2014;186:240-5. [CrossRef]
- Eltzschig H.K, Eckle T. Ischemia and reperfusion–from mechanism to translation. Nat Med. 2011 7;17(11):1391-401. [CrossRef]
- Wu M.Y, Yiang G.T, Liao W.T, Tsai A.P, Cheng Y.L, Cheng P.W et al. Current mechanistic concepts in ıschemia and reperfusion ınjury. Cell Physiol Biochem. 2018;46(4):1650-1667. [CrossRef]
- Kalogeris T, Baines C.P, Krenz M, Korthuis R. J. Cell Biology of Ischemia/Reperfusion Injury. Int Rev Cell Mol Biol. 2012; 298: 229–317. [CrossRef]
- Zheng Y, Ley S.H, Hu F.B. Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nat Rev Endocrinol. 2018;14(2):88–98. [CrossRef]
- Guariguata L, Whiting DR, Hambleton I, et al. Global estimates of diabetes prevalence for 2013 and projections for 2035. Diab Res clin pract. 2014; 103(2): 137–149. [CrossRef]
- Lejay A, Fang F, John R,Van J.A.D, Barr M, Thaveau F. et al. Ischemia-reperfusion injury, ischemic conditioning and diabetes mellitus. Journal of Molecular and Cellular Cardiology 2016; 91:11–22. [CrossRef]
- Rajeshkumar S, Naik P. Synthesis and biomedical applications of cerium oxide nanoparticles – A review. Biotechnology Reports 2018;17:1–5. [CrossRef]
- Singh K.R, Nayak V, Sarkar T, Singh R.P. Cerium oxide nanoparticles: properties, biosynthesis and biomedical application. RSC Adv. 2020;10(45):27194-27214. [CrossRef]
- Tuncay A, Sivgin V, Ozdemirkan A, Sezen S.C, Boyunaga H, Kucuk A et al. The effect of cerium oxide on lung tissue in lower extremity ischemia-reperfusion injury in sevoflurane administered rats. Int J Nanomedicine. 2020;15:7481-7489. [CrossRef]
- Gobut H, Kucuk A, Şengel N, Arslan M, Ozdemir C, Mortas T et al. Effects of cerium oxide (CeO2) on liver tissue in liver ischemia-reperfusion injury in rats undergoing desflurane anesthesia. BMC Anesthesiol. 2023;23(1):40. [CrossRef]
- Zhao Y, Yang Y, Wen Y, Zhao M, Dong Y. Effect of cerium oxide nanoparticles on myocardial cell apoptosis induced by myocardial ischemia-reperfusion injury. Cell Mol Biol (Noisy-le-grand). 2022;68(3):43-50. [CrossRef]
- Yesil S, Ozdemir C, Arslan M, Gundogdu A.C, Kavutcu M, Atan A. Protective effect of cerium oxide on testicular function and oxidative stress after torsion/detorsion in adult male rats. Exp Ther Med. 2022 Nov 15;25(1):1. [CrossRef]
- Erkanlı K, Kayalar N, Erkanlı G, Ercan F, Sener G, Kırali K. Melatonin protects against ischemia/reperfusion injury in skeletal muscle. J. Pineal Res. 2005; 39:238–242. [CrossRef]
- Hsieh K.F, Shih J.M, Shih Y.M, Pai M.H, Yeh S.L. Arginine administration increases circulating endothelial progenitor cells and attenuates tissue injury in a mouse model of hind limb ischemia/reperfusion. Nutrition 2018; 55-56: 29–35. [CrossRef]
- Kumar K, Railton C, Tawfic Q. Tourniquet Application during Anesthesia: “What We Need to Know?”. J Anaesthesiol Clin Pharmacol. 2016;32(4):424-430. [CrossRef]
- Orhan M, Tuna A.T, Ünal Y,Arslan M,Yazar H, Sezen Ş.C et al. The effects of amantadine on lung tissue in lower limb ischemia/reperfusion injury model in rats Turkish Journal of Thoracic and Cardiovascular Surgery 2021;29(1):77-83. [CrossRef]
- Mansour Z, Charles A.L, Kindo M, Pottecher J, Chamaraux-Tran T N, Lejay A et al. Remote effects of lower limb ischemia-reperfusion: Impaired lung, unchanged liver, and stimulated kidney oxidative capacities. Biomed Res Int 2014; 2014:392390. [CrossRef]
- Kao M.C, Yang C.H, Chou W.C, Sheu J.R, Huang C.J Cepharanthine mitigates lung injury in lower limb ischemia-reperfusion. J Surg Res. 2015;199(2):647-56. [CrossRef]
- Pottecher J, Adamopoulos C, Anne Lejay A, Bouitbir J, Charles A.L, Meyer A et al. Diabetes worsens skeletal muscle mitochondrial function, oxidative stress, and apoptosis after lower-limb ischemia-reperfusion: Implication of the RISK and SAFE pathways? Front Physiol. 2018 22;9:579. [CrossRef]
- Barnes J.A, Eid M.A, Creager M.A, Goodney P.P. Epidemiology and risk of amputation in patients with diabetes mellitus and peripheral artery disease. Arterioscler Thromb Vasc Biol. 2020; 40(8):1808-1817. [CrossRef]
- Lejay A, Meyer A, Schlagowski A.I, Charles A.L, Singh F, Bouitbir J et al. Mitochondria: mitochondrial participation in ischemia-reperfusion injury in skeletal muscle. Int J Biochem Cell Biol 2014;50:101-105. [CrossRef]
- Hussain T, Tan B, Yin Y, Blachier F, Tossou M.C, Rahu N. Oxidative stress and inflammation: What polyphenols can do for us? Oxid. Med. Cell. Longevity 2016; 2016:7432797. [CrossRef]
- Erel O. A new automated colorimetric method for measuring total oxidant status. Clin Biochem. 2005;38(12):1103–1111. [CrossRef]
- Karapinar O.S, Pinar N, Özcan O, Özgür T, Dolapçıoğlu K. Protective effect of alpha-lipoic acid in methotrexate-induced ovarian oxidative injury and decreased ovarian reserve in rats. Gynecol Endocrinol 2017;33:653–9. [CrossRef]
- 27. Cannistrà M, Ruggiero M, Zullo A, Gallelli G, Serafini S, Maria M et al. Hepatic ischemia-reperfusion injury: A systematic review of literature and the role of current drugs and biomarkers. Int J Surg. 2016;33:57–70. [CrossRef]
- Kasprzak M.P, Iskra M, Majewski W, Budzyń-Napierała M, Gryszczyńska B, Strzyżewski K et al. PON1 status evaluation in patients with chronic arterial occlusion of lower limbs due to atherosclerosis obliterans. Arch Med Sci. 2014;10(6):1101-8. [CrossRef]
- Nyoka M, Choonara Y.E, Kumar P, Kondiah P.P.D, Pillay V. Synthesis of cerium oxide nanoparticles using various methods: Implications for biomedical applications. Nanomaterials (Basel). 2020;10(2):242. [CrossRef]
- Casals E, Zeng M, Parra-Robert M, Fernández-Varo G, Morales-Ruiz M, Jiménez W. Cerium oxide nanoparticles: Advances in biodistribution, toxicity and preclinical exploration. Small. 2020;16(20):e1907322. [CrossRef]
- Ozdemirkan A, Kucuk A, Gunes I, Arslan M, Tuncay A, Sivgin V et al. The effect of cerium oxide on lung injury following lower extremity ischemia-reperfusion injury in rats under desflurane anesthesia. Saudi Med J. 2021;42(11):1247-1251. [CrossRef]
- Al Shoyaib A, Archie S.R, Karamyan V.T. Intraperitoneal route of drug administration: should it be used in experimental animal studies? Pharm Res 2020; 37: 12. [CrossRef]
- Park I.S, Mahapatra C, Park J.S, Dashnyam K, Kim J.W, Ahn J.C et al. Revascularization and limb salvage following critical limb ischemia by nanoceria-induced Ref-1/APE1-dependent angiogenesis. Biomaterials. 2020;242:119919. [CrossRef]
- Bayaraa O, Dashnyam K, Singh R.J, Mandakhbayar N, Lee J.H, Park J.T et al. Nanoceria-GO-intercalated multicellular spheroids revascularize and salvage critical ischemic limbs through anti-apoptotic and pro-angiogenic functions. Biomaterials. 2023;292:121914. [CrossRef]
| Group C (n=6) |
Group D (n=8) |
Group DCO (n=8) |
Group DIR (n=8) |
Group DIR-CO (n=8) |
P** | |
|---|---|---|---|---|---|---|
| Disorganization and degeneration of muscle cells | 0.29±.0.18 | 0.85±0.34 | 1.50±0.27* | 2.86±0.14*,†,‡ | 1.72±0.18*,†,§ | <0.001 |
| Inflammatory cell infiltration | 0.00±.0.00 | 0.57±.0.29* | 0.87±.0.13* | 1.43±.0.20*,†,‡ | 0.85±.0.14*,§ | <0.001 |
| Total injury score | 0.29±.0.18 | 1.42±0.57* | 2.37±0.32* | 4.29±0.28*,†,‡ | 2.57±0.20*,†,§ | <0.001 |
| Group C (n=6) |
Group D (n=8) |
Group DCO (n=8) |
Group DIR (n=8) |
Group DIR-CO (n=8) |
P** | |
|---|---|---|---|---|---|---|
| TAS (nmol/mL) | 1.46±0.18 | 1.09±0.04* | 1.12±0.09* | 0.81±0.04*,†,‡ | 1.03±0.02* | 0.001 |
| TOS (IU/mg.pro) | 5.49±1.00 | 13.99±0.66* | 13.17±1.21* | 28.58±3.14*,†,‡ | 16.20±1.94*,§ | <0.001 |
| OSI | 3.80±0.58 | 12.93±0.53* | 11.94±1.22* | 36.09±4.66*,†,‡ | 15.87±1.97*,§ | <0.001 |
| PON (IU/mg.pro) | 295.57±21.65 | 355.86±11.15 | 340.38±20.2 | 455.86±29.44*,†,‡ | 362.57±17.13*,§ | <0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




