Submitted:
05 February 2024
Posted:
06 February 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Prevalence, Diagnosis, and Risk Factors
2.1. Prevalence and Diagnostic Criteria for NODAT in Kidney Transplant Recipients
2.2. Risk Factors for NODAT
2.2.1. Age
2.2.2. Gender
2.2.3. Genetic Predisposition to NODAT
2.2.4. Obesity
2.2.5. Immunosuppressive Agents
2.2.6. Viral Infection
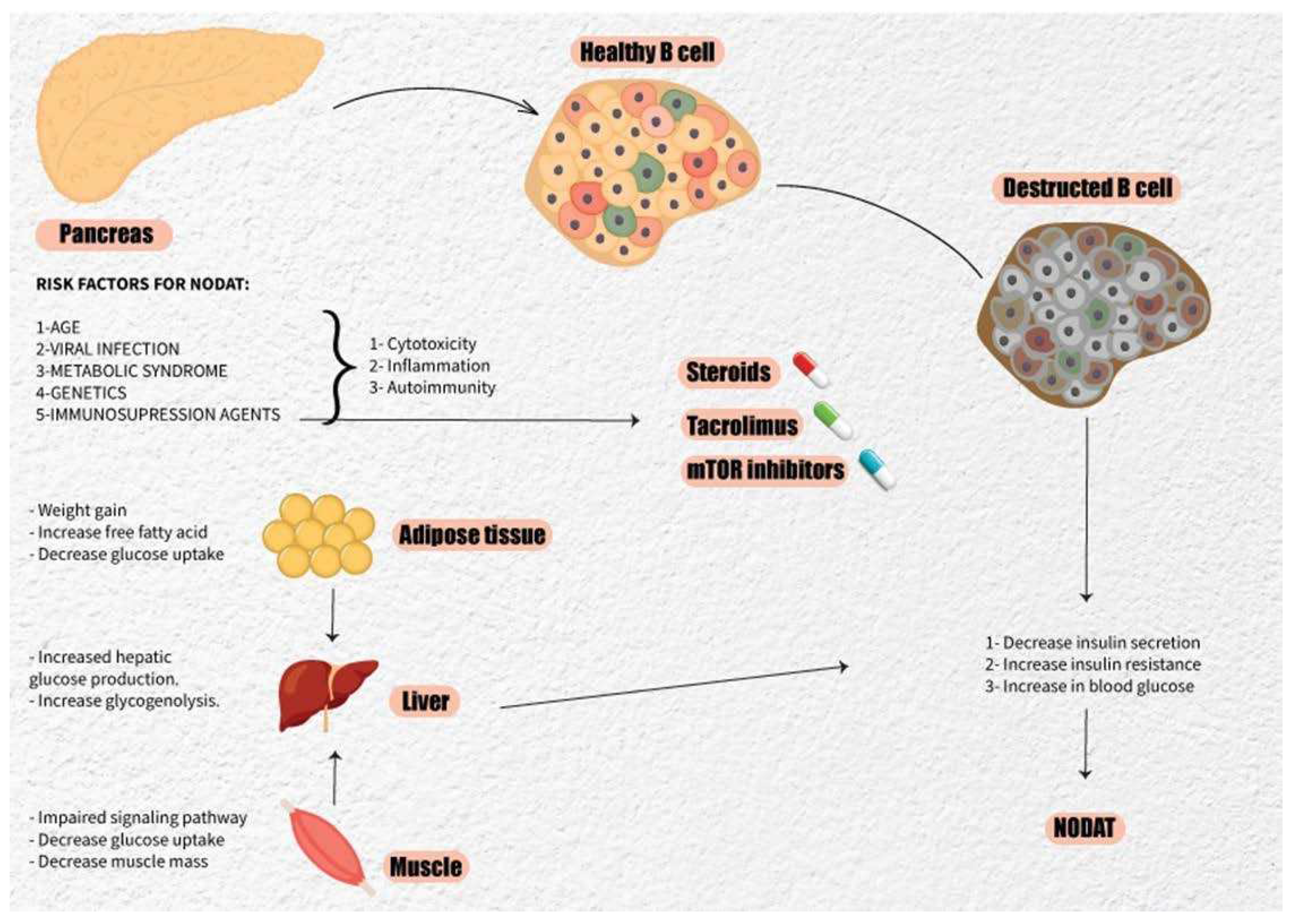
3. Pathophysiology of NODAT
3.1. Insulin Resistance
3.3. Role of Immunosuppressive Medications
3.3.1. Glucocorticoids
3.3.2. CNIs
3.3.3. Sirolimus
3.3.4. Everolimus
4. Management and Treatment
4.1. Pharmacological Management of NODAT
4.1.1. Immunosuppressive Drug Adjustments
4.1.2. Antidiabetic Medications
4.2. Potential Novel Therapies or Approaches
4.3. Lifestyle Interventions and Dietary Considerations
5. Complications and Long-Term Consequences
5.1. Short-Term Complications of NODAT
5.2. Long-Term Consequences on Graft and Patient Survival
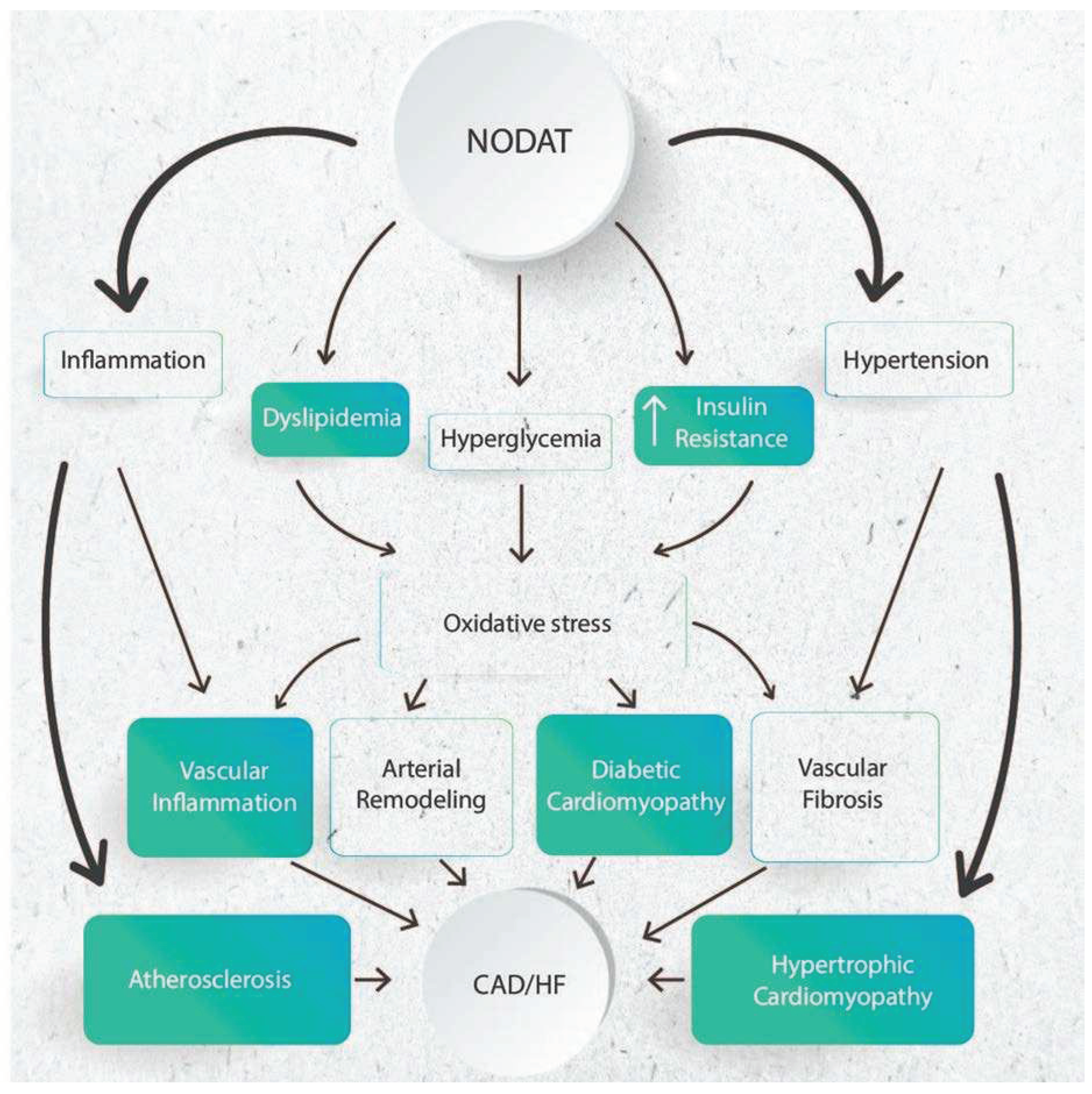
5.3. Impact on Cardiovascular Health
6. Prevention Strategies
6.1. Strategies for Preventing NODAT Pre-Transplant
6.2. Early Post-Transplant Interventions to Minimize NODAT Risk
7. Current Ongoing Research in the Field
8. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- R A Gatchalian and, D.J. Leehey, Mortality among patients on dialysis, patients on dialysis awaiting transplantation, and transplant recipients. 2000.
- Addendum. 2. Classification and Diagnosis of Diabetes: <i>Standards of Medical Care in Diabetes—2021</i>. Diabetes Care 2021;44(Suppl. 1):S15–S33. Diabetes Care 2021, 44, 2182–2182. [CrossRef]
- Hecking, M. , et al. , Management of post-transplant diabetes: immunosuppression, early prevention, and novel antidiabetics. Transplant International, 2021, 34, 27–48. [Google Scholar] [CrossRef] [PubMed]
- Hecking, M. , et al. , Novel views on new-onset diabetes after transplantation: development, prevention and treatment. Nephrology Dialysis Transplantation, 2013, 28, 550–566. [Google Scholar] [CrossRef] [PubMed]
- Hagen, M. , A 6-year prospective study on new onset diabetes mellitus, insulin release and insulin sensitivity in renal transplant recipients. Nephrology Dialysis Transplantation, 2003, 18, 2154–2159. [Google Scholar] [CrossRef]
- Porrini, E.L. , et al., Clinical evolution of post-transplant diabetes mellitus. Nephrology Dialysis Transplantation, 2016, 31, 495–505. [Google Scholar] [CrossRef] [PubMed]
- Bertram L Kasiske 1, J.J.S. , David Gilbertson, Arthur J Matas, Diabetes mellitus after kidney transplantation in the United States. American Journal of Transplantation, 2003.
- Jenssen, T. and A. Hartmann, Post-transplant diabetes mellitus in patients with solid organ transplants. Nature Reviews Endocrinology, 2019, 15, 172–188. [Google Scholar] [CrossRef]
- Davidson, J. , AlanDantal, JacquesDotta, FrancescoHaller, HermannHernandez, DomingoKasiske, Bertram L. Kiberd, BryceKrentz, AndrewLegendre, ChristopheMarchetti, PieroMarkell, Marianavan der Woude, Fokko J.Wheeler, David C., NEW-ONSET DIABETES AFTER TRANSPLANTATION: 2003 INTERNATIONAL CONSENSUS GUIDELINES. 2003, 75, ss3–ss24. [Google Scholar] [CrossRef]
- Katwal, P.C. , et al., The Effect of Anemia and the Goal of Optimal HbA1c Control in Diabetes and Non-Diabetes. Cureus, 2020.
- Didier Ducloux and, C. Courivaud, Prevention of Post-Transplant Diabetes Mellitus: Towards a Personalized Approach. Journal of Personalized Medicine, 2022.
- Adnan Sharif Dr and, S.C. MD, Posttransplantation diabetes—state of the art. 2016; 4, 337-349. [Google Scholar] [CrossRef]
- Adachi, H. , et al., Long-term retrospective observation study to evaluate effects of adiponectin on skeletal muscle in renal transplant recipients. Scientific Reports, 2020, 10. [Google Scholar] [CrossRef]
- Houmard, J.A. , et al., , Skeletal Muscle GLUT4 Protein Concentration and Aging in Humans. Diabetes, 1995, 44, 555–560. [Google Scholar] [CrossRef]
- T. Abe, T.O., H. Tahara, H. Tashiro, K. Ishiyama, K. Ide, M. Ohira, and H. Ohdan, Risk Factors for Development of New-Onset Diabetes Mellitus and.
- Progressive Impairment of Glucose Metabolism After Living-Donor.
- Liver Transplantation. Transplantation Proceedings, 2014; 55(10).
- Cosio, F.G. , et al,, Post-transplant diabetes mellitus: Increasing incidence in renal allograft recipients transplanted in recent years. Kidney International, 2001, 59, 732–737. [Google Scholar] [CrossRef] [PubMed]
- Da-Wei Li, et al. Risk factors for new onset diabetes mellitus after liver transplantation: A meta-analysis.
- Li DW, Lu TF, Hua XW, Dai HJ, Cui XL, Zhang JJ, Xia Q. Risk factors for new onset diabetes mellitus after liver transplantation: A meta-analysis. World J Gastroenterol 2015, 21, 6329–6340, World Journal of Gastroenterology, 2015. [CrossRef]
- Romanowski, M. , et al., adiponectin and leptin gene polymorphisms in patients with post-transplant diabetes mellitus. Pharmacogenomics, 2015, 16, 1243–1252. [Google Scholar] [CrossRef] [PubMed]
- Jøran Hjelmesaeth 1, A.F. , Trond Jenssen, Jan Frystyk, Thor Ueland, Monica Hagen, Anders Hartmann, Hypoadiponectinemia is associated with insulin resistance and glucose intolerance after renal transplantation: impact of immunosuppressive and antihypertensive drug therapy. CJASN, 2006.
- Monica Szabo, B.M. , Katalin Csép, Theodora Benedek, Genetic Approaches to the Study of Gene Variants and Their Impact on the Pathophysiology of Type 2 Diabetes. Biochemical Genetics, 2018.
- Yang Gyun Kim 1, C.-G.I. , Tae Won Lee, Sang Ho Lee, Kyung Hwan Jeong, Ju Young Moon, Joo-Ho Chung, Su Kang Kim, Yeong Hoon Kim, Association of genetic polymorphisms of interleukins with new-onset diabetes after transplantation in renal transplantation. TRANSPLANTATION, 2012.
- Yan Chen 1, M.S.S. , Jae Wook Yang, David Min, Ian V Hutchinson, Genetic polymorphisms of the transcription factor NFATc4 and development of new-onset diabetes after transplantation in Hispanic kidney transplant recipients. TRANSPLANTATION, 2012.
- Bruna B Nicoletto 1, G.C.S. , Natasha K O Fonseca, Analaura Centenaro, Roberto C Manfro, Luís Henrique S Canani, Luiz Felipe Santos Gonçalves, Association between 276G/T adiponectin gene polymorphism and new-onset diabetes after kidney transplantation. 2013.
- Cron, D.C. , et al., Using analytic morphomics to describe body composition associated with post-kidney transplantation diabetes mellitus. Clinical Transplantation, 2017, 31, e13040. [Google Scholar] [CrossRef] [PubMed]
- Marit Elizabeth von Düring 1 2, T.J. , Jens Bollerslev 2 4, Anders Åsberg 1 5 6, Kristin Godang 4, Ivar Anders Eide 1 2, Dag Olav Dahle 1 2, Anders Hartmann 1 2, Visceral fat is better related to impaired glucose metabolism than body mass index after kidney transplantation. 2015.
- Després, J.-. and I. Lemieux, Abdominal obesity and metabolic syndrome. Nature, 2006, 444, 881–887. [Google Scholar] [CrossRef] [PubMed]
- Hung-Tien Kuo 1, M.S.S. , Xiaoyi Ye, Pavani Reddy, Paul Martin, Suphamai Bunnapradist, Risk factors for new-onset diabetes mellitus in adult liver transplant recipients, an analysis of the Organ Procurement and Transplant Network/United Network for Organ Sharing database. TRANSPLANTATION, 2010.
- Roy D Bloom 1, V.R. , Francis Weng, Robert A Grossman, Debbie Cohen, Kevin C Mange, Association of Hepatitis C with Posttransplant Diabetes in Renal Transplant Patients on Tacrolimus. JASN, 2002.
- Burra, P. Becchetti, and G. Germani, NAFLD and liver transplantation: Disease burden, current management and future challenges. JHEP Reports, 2020, 2, 100192. [Google Scholar] [CrossRef] [PubMed]
- A V Ekstrand 1, J.G.E. , C Grönhagen-Riska, P J Ahonen, L C Groop, Insulin resistance and insulin deficiency in the pathogenesis of posttransplantation diabetes in man. TRANSPLANTATION, 1992.
- Morten B Jørgensen 1, M.H. , Gerrit van Hall 2, Claus Bistrup 3, Jesper M Hansen 4, Elisabeth R Mathiesen 5, Bo Feldt-Rasmussen 1, The impact of kidney transplantation on insulin sensitivity. TRANSPLANT INTERNATIONAL, 2017.
- J H Nam 1, J.I.M. , S I Kim, S W Kang, K H Choi, K Park, C W Ahn, B S Cha, Y D Song, S K Lim, K R Kim, H C Lee, K B Huh, beta-Cell dysfunction rather than insulin resistance is the main contributing factor for the development of postrenal transplantation diabetes mellitus. TRANSPLANTATION, 2001.
- Zelle, D.M. , et al., Pancreatic β-Cell Dysfunction and Risk of New-Onset Diabetes After Kidney Transplantation. Diabetes Care, 2013, 36, 1926–1932. [Google Scholar] [CrossRef] [PubMed]
- Halden, T.A.S. , et al., GLP-1 Restores Altered Insulin and Glucagon Secretion in Posttransplantation Diabetes. Diabetes Care, 2016, 39, 617–624. [Google Scholar] [CrossRef] [PubMed]
- Leendert H Oterdoom 1, A.P.J.d.V. , Ron T Gansevoort, Willem J van Son, Jaap J Homan van der Heide, Rutger J Ploeg, Paul E de Jong, Reinold O B Gans, Stephan J L Bakker, Determinants of insulin resistance in renal transplant recipients. TRANSPLANTATION, 2007.
- Pereira, M.J. , et al., Cyclosporine A and Tacrolimus Reduce the Amount of GLUT4 at the Cell Surface in Human Adipocytes: Increased Endocytosis as a Potential Mechanism for the Diabetogenic Effects of Immunosuppressive Agents. The Journal of Clinical Endocrinology & Metabolism, 2014, 99, E1885–E1894. [Google Scholar] [CrossRef] [PubMed]
- Harini A Chakkera 1, L.J.M. , Calcineurin inhibition and new-onset diabetes mellitus after transplantation. TRANSPLANTATION, 2013.
- Talchai, C. , et al., Pancreatic β Cell Dedifferentiation as a Mechanism of Diabetic β Cell Failure. Cell, 2012, 150, 1223–1234. [Google Scholar] [CrossRef] [PubMed]
- Bensellam, M. -C. Jonas, and D.R. Laybutt, Mechanisms of β-cell dedifferentiation in diabetes: recent findings and future research directions. Journal of Endocrinology, 2018, 236, R109–R143. [Google Scholar] [CrossRef] [PubMed]
- Rodríguez-Rodríguez, A.E. , et al., Post-Transplant Diabetes Mellitus and Prediabetes in Renal Transplant Recipients: An Update. Nephron, 2021, 145, 317–329. [Google Scholar] [CrossRef] [PubMed]
- PfüTzner, A. , et al., Fasting Intact Proinsulin Is a Highly Specific Predictor of Insulin Resistance in Type 2 Diabetes. Diabetes Care, 2004, 27, 682–687. [Google Scholar] [CrossRef] [PubMed]
- Ebru Sulanc 1, J.T.L. , Susan E Puumala, Gerald C Groggel, Lucille E Wrenshall, R Brian Stevens, New-onset diabetes after kidney transplantation: an application of 2003 International Guidelines. TRANSPLANTATION, 2005.
- Lane, J.T. and S. Dagogo-Jack, Approach to the Patient with New-Onset Diabetes after Transplant (NODAT). The Journal of Clinical Endocrinology & Metabolism, 2011, 96, 3289–3297. [Google Scholar] [CrossRef] [PubMed]
- Sharif, A. , Preventing and managing hyperglycemia in kidney transplant patients. Current Opinion in Nephrology and Hypertension, 2012.
- Antonio Perez 1, S.J.-C. Ignasi Saigi, M Rosa Bernal-Lopez, Inka Miñambres, Ricardo Gomez-Huelgas, Glucocorticoid-induced hyperglycemia. Journal of Diabetes 2014. [Google Scholar] [CrossRef]
- Axelrod, D.A. , et al., Posttransplant Diabetes Mellitus and Immunosuppression Selection in Older and Obese Kidney Recipients. Kidney Medicine, 2022, 4, 100377. [Google Scholar] [CrossRef] [PubMed]
- Midtvedt, K. , JøranHartmann, AndersLund, KirstenPaulsen, DagEgeland, ThoreJenssen, Trond, Insulin Resistance after Renal Transplantation : The Effect of Steroid Dose Reduction and Withdrawal. JASN, 2004, 15. [Google Scholar] [CrossRef] [PubMed]
- Chakkera, H. Kudva, and B. Kaplan, Calcineurin Inhibitors: Pharmacologic Mechanisms Impacting Both Insulin Resistance and Insulin Secretion Leading to Glucose Dysregulation and Diabetes Mellitus. Clinical Pharmacology & Therapeutics, 2017, 101, 114–120. [Google Scholar] [CrossRef] [PubMed]
- Heisel, O. , et al., New Onset Diabetes Mellitus in Patients Receiving Calcineurin Inhibitors: A Systematic Review and Meta-Analysis. American Journal of Transplantation, 2004, 4, 583–595. [Google Scholar] [CrossRef] [PubMed]
- Charlton, M. , et al., Everolimus Is Associated With Less Weight Gain Than Tacrolimus 2 Years After Liver Transplantation. Transplantation, 2017, 101, 2873–2882. [Google Scholar] [CrossRef]
- Fraenkel, M. , et al., mTOR Inhibition by Rapamycin Prevents β-Cell Adaptation to Hyperglycemia and Exacerbates the Metabolic State in Type 2 Diabetes. Diabetes, 2008, 57, 945–957. [Google Scholar] [CrossRef] [PubMed]
- Johnston, O. , et al., Sirolimus Is Associated with New-Onset Diabetes in Kidney Transplant Recipients. Journal of the American Society of Nephrology, 2008, 19, 1411–1418. [Google Scholar] [CrossRef] [PubMed]
- Annalisa Teutonico 1, P.F.S. , Salvatore Di Paolo, Glucose metabolism in renal transplant recipients: effect of calcineurin inhibitor withdrawal and conversion to Sirolimus. JASN, 2005.
- Montero, N.M. , PhD1; Quero, Maria MD1; Melilli, Edoardo MD, PhD1; Pérez-Sáez, María José MD, PhD2; Redondo-Pachón, Dolores MD, PhD2; Bestard, Oriol MD, PhD1; Crespo, Marta MD, PhD2; Cruzado, Josep M. MD, PhD1; Pascual, Julio MD, PhD2, Mammalian Target of Rapamycin Inhibitors Combined With Calcineurin Inhibitors as Initial Immunosuppression in Renal Transplantation: A Meta-analysis. TRANSPLANTATION, 2019. [Google Scholar]
- Stefan Berger 1, C.S. , Oliver Witzke 3 4, Helio Tedesco 5, Steve Chadban 6, Shamkant Mulgaonkar 7, Yasir Qazi 8, Johan W. de Fijter 9, Federico Oppenheimer 10, Josep M. Cruzado 11, Yoshihiko Watarai 12, Pablo Massari 13, Christophe Legendre 14, Franco Citterio 15, Mitchell Henry 16, Titte R. Srinivas 17, Flavio Vincenti 18, Maria Pilar Hernandez Gutierrez 19, Ana Maria Marti 19, Peter Bernhardt 19…Julio Pascual 20, Two-year outcomes in de novo renal transplant recipients receiving everolimus-facilitated calcineurin inhibitor reduction regimen from the TRANSFORM study. 2019.
- Phuong-Thu T Pham 1, P.-C.T.P. , Gerald S Lipshutz, Alan H Wilkinson, New onset diabetes mellitus after solid organ transplantation. Endocrinology and Metabolism Clinics of North America, 2007.
- Cehic, M.G. , et al., Management Strategies for Posttransplant Diabetes Mellitus after Heart Transplantation: A Review. Journal of Transplantation, 2018, 2018, 1–14. [Google Scholar] [CrossRef] [PubMed]
- Oliver Thomusch 1, M.W. , Mirian Opgenoorth 3, Andreas Pascher 4, Rainer Peter Woitas 5, Oliver Witzke 6, Bernd Jaenigen 1, Markus Rentsch 7, Heiner Wolters 8, Thomas Rath 9, Tülay Cingöz 10, Urs Benck 11, Bernhard Banas 12, Christian Hugo 13, Rabbit-ATG or basiliximab induction for rapid steroid withdrawal after renal transplantation (Harmony): an open-label, multicentre, randomised controlled trial. the lancet, 2016.
- Haller, M.C. , et al., Steroid withdrawal after renal transplantation: a retrospective cohort study. BMC Medicine, 2017, 15. [Google Scholar] [CrossRef] [PubMed]
- E Steve Woodle 1, M.R.F. , John Pirsch, Fuad Shihab, A Osama Gaber, Paul Van Veldhuisen; Astellas Corticosteroid Withdrawal Study Group, A prospective, randomized, double-blind, placebo-controlled multicenter trial comparing early (7 day) corticosteroid cessation versus long-term, low-dose corticosteroid therapy. 2008.
- Sneha Palepu 1, G.V.R.P. , New-onset diabetes mellitus after kidney transplantation: Current status and future directions. world journal of diabetes 2015. [Google Scholar] [CrossRef]
- Chadban, S. , New-onset diabetes after transplantation--should it be a factor in choosing an immunosuppressant regimen for kidney transplant recipients. Nephrology Dialysis Transplantation, 2008, 23, 1816–1818. [Google Scholar] [CrossRef] [PubMed]
- Manfred Hecking 1, M.H. , Dominik Döller, Johannes Werzowa, Andrea Tura, Jinyao Zhang, Hilal Tekoglu, Johannes Pleiner, Thomas Wrba, Susanne Rasoul-Rockenschaub, Ferdinand Mühlbacher, Sabine Schmaldienst, Wilfred Druml, Walter H Hörl, Michael Krebs, Michael Wolzt, Giovanni Pacini, Friedrich K Port, Marcus D Säemann, Early basal insulin therapy decreases new-onset diabetes after renal transplantation. JASN, 2012.
- Chowdhury, T.A. , et al., Association of British Clinical Diabetologists and Renal Association guidelines on the detection and management of diabetes post solid organ transplantation. Diabetic Medicine 2021, 38. [Google Scholar] [CrossRef] [PubMed]
- Vest, L.S. , et al., Metformin use in the first year after kidney transplant, correlates, and associated outcomes in diabetic transplant recipients: A retrospective analysis of integrated registry and pharmacy claims data. Clinical Transplantation, 2018, 32, e13302. [Google Scholar] [CrossRef] [PubMed]
- B Richter 1, E.B.-E. , K Bergerhoff, C L Lerch, Dipeptidyl peptidase-4 (DPP-4) inhibitors for type 2 diabetes mellitus. Cochrane Library, 2008.
- Wajchenberg, B.L. , β-Cell Failure in Diabetes and Preservation by Clinical Treatment. Endocrine Reviews, 2007, 28, 187–218. [Google Scholar] [CrossRef] [PubMed]
- Vijay Shivaswamy 1, R.G.B. , Cara C Clure 3, Brendan Ottemann 3, John S Davis 4, Jennifer L Larsen 5, Frederick G Hamel 5, Tacrolimus and Sirolimus have distinct effects on insulin signaling in male and female rats. Translational Research, 2014.
- Delos Santos, R.B. , et al., Sitagliptin Versus Placebo to Reduce the Incidence and Severity of Posttransplant Diabetes Mellitus After Kidney Transplantation-A Single-center, Randomized, Double-blind Controlled Trial. Transplantation, 2023, 107, 1180–1187. [Google Scholar] [CrossRef] [PubMed]
- Defronzo, R.A. , et al., Effects of Exenatide (Exendin-4) on Glycemic Control and Weight Over 30 Weeks in Metformin-Treated Patients With Type 2 Diabetes. Diabetes Care, 2005, 28, 1092–1100. [Google Scholar] [CrossRef] [PubMed]
- Garber, A.J. , Long-Acting Glucagon-Like Peptide 1 Receptor Agonists. Diabetes Care, 2011, 34 (Supplement_2), S279-S284. [Google Scholar] [CrossRef] [PubMed]
- Priyamvada Singh 1, M.T. , Todd E Pesavento 1, Kenneth Washburn 1, Debbie Walsh 1, Shumei Meng 1, Comparison of the glucagon-like-peptide-1 receptor agonists dulaglutide and liraglutide for the management of diabetes in solid organ transplant: A retrospective study. Diabetes, Obesity and Metabolism, 2020.
- Heerspink, H.J.L. , et al., Renoprotective effects of sodium-glucose cotransporter-2 inhibitors. Kidney International, 2018, 94, 26–39. [Google Scholar] [CrossRef] [PubMed]
- Aditi Ujjawal 1, B.S. , Ashish Verma 3, Sodium-glucose cotransporter-2 inhibitors (SGLT2i) in kidney transplant recipients: what is the evidence? Therapeutic Advances in Endocrinology and Metabolism, 2022.
- Jin, J. , et al., Effect of Empagliflozin on Tacrolimus-Induced Pancreas Islet Dysfunction and Renal Injury. American Journal of Transplantation, 2017, 17, 2601–2616. [Google Scholar] [CrossRef]
- Ko, E.J. , et al., Effect of dual inhibition of DPP4 and SGLT2 on tacrolimus-induced diabetes mellitus and nephrotoxicity in a rat model. American Journal of Transplantation, 2022, 22, 1537–1549. [Google Scholar] [CrossRef] [PubMed]
- Michael A Nauck 1, J.W. , Juris J Meier 2, Treatment of type 2 diabetes: challenges, hopes, and anticipated successes. The Lancet Diabetes & Endocrinology 2021. [Google Scholar] [CrossRef]
- Chakkera, H.A. , et al., Can New-Onset Diabetes After Kidney Transplant Be Prevented? Diabetes Care, 2013, 36, 1406–1412. [Google Scholar] [CrossRef] [PubMed]
- William C Knowler 1, E.B.-C. , Sarah E Fowler, Richard F Hamman, John M Lachin, Elizabeth A Walker, David M Nathan; Diabetes Prevention Program Research Group, Reduction in the incidence of type 2 diabetes with lifestyle intervention or metformin. 2002.
- Shahrad Taheri 1, H.Z. , Odette Chagoury 3, Sara Elhadad 3, Salma Hayder Ahmed 3, Neda El Khatib 4, Rasha Abou Amona 4, Katie El Nahas 4, Noor Suleiman 5, Abdulla Alnaama 6, Abdulla Al-Hamaq 4, Mary Charlson 7, Martin T Wells 8, Samya Al-Abdulla 6, Abdul Badi Abou-Samra 5, Effect of intensive lifestyle intervention on bodyweight and glycaemia in early type 2 diabetes (DIADEM-I): an open-label, parallel-group, randomised controlled trial. The Lancet Diabetes & Endocrinology 2020. [Google Scholar] [CrossRef]
- Kulli Kuningas 1, J.D. , Reena Mair 2, Helen Smith 3, Mary Dutton 1, Edward Day 4, And Adnan Sharif 1 5, Comparing Glycaemic Benefits of Active Versus Passive Lifestyle Intervention in Kidney Allograft Recipients: A Randomized Controlled Trial. transplantation, 2020.
- Byambasukh, O. , et al., Physical Activity and the Development of Post-Transplant Diabetes Mellitus, and Cardiovascular- and All-Cause Mortality in Renal Transplant Recipients. Journal of Clinical Medicine, 2020, 9, 415. [Google Scholar] [CrossRef] [PubMed]
- Osté, M.C.J. , et al., Mediterranean style diet is associated with low risk of new-onset diabetes after renal transplantation. BMJ Open Diabetes Research & Care, 2017, 5, e000283. [Google Scholar] [CrossRef]
- Merz, K.E. and D.C. Thurmond, Role of Skeletal Muscle in Insulin Resistance and Glucose Uptake. Comprehensive Physiology, 2020: p. 785-809.
- Cohen, J.B. , et al., Bariatric surgery before and after kidney transplantation: long-term weight loss and allograft outcomes. Surgery for Obesity and Related Diseases, 2019, 15, 935–941. [Google Scholar] [CrossRef] [PubMed]
- Do Carmo Chaves, A.E.C. , et al., Early retinal neurovascular findings in post-transplant diabetes mellitus patients without clinical signs of diabetic retinopathy. International Journal of Retina and Vitreous, 2023, 9. [Google Scholar] [CrossRef] [PubMed]
- J P Boudreaux, L.M. , D M Canafax, N Ascher, D E Sutherland, W Payne, R L Simmons, J S Najarian, D S Fryd, The impact of cyclosporine and combination immunosuppression on the incidence of posttransplant diabetes in renal allograft recipients. TRANSPLANTATION, 1987.
- Krista L Lentine 1, D.C.B. , Mark A Schnitzler, Incidence and predictors of myocardial infarction after kidney transplantation. JASN, 2005.
- Rianne P Wauters 1, F.G.C. , Maria L Suarez Fernandez, Yogish Kudva, Pankaj Shah, Vicente E Torres, Cardiovascular consequences of new-onset hyperglycemia after kidney transplantation. Transplantation, 2012.
- Cosio, F.G. , et al., New onset hyperglycemia and diabetes are associated with increased cardiovascular risk after kidney transplantation. Kidney International, 2005, 67, 2415–2421. [Google Scholar] [CrossRef] [PubMed]
- Giacco, F. and M. Brownlee, Oxidative Stress and Diabetic Complications. Circulation Research, 2010, 107, 1058–1070. [Google Scholar] [CrossRef] [PubMed]
- Brownlee, M. , The Pathobiology of Diabetic Complications. Diabetes, 2005, 54, 1615–1625. [Google Scholar] [CrossRef] [PubMed]
- Esteban Porrini 1, P.D. , Alejandra Alvarez, Marian Cobo, Lourdes Pérez, José M González-Posada, Luis Hortal, Roberto Gallego, José J García, Maria Checa, Adelaida Morales, Eduardo Salido, Domingo Hernández, Armando Torres, The combined effect of pre-transplant triglyceride levels and the type of calcineurin inhibitor in predicting the risk of new onset diabetes after renal transplantation. 2008.
- Henrik Andreas Bergrem 1, T.G.V. , Anders Hartmann, Harald Bergrem, Jøran Hjelmesaeth, Trond Jenssen, Glucose tolerance before and after renal transplantation. 2010.
- Chen, T. , et al., New onset diabetes mellitus after liver transplantation and hepatitis C virus infection: meta-analysis of clinical studies. Transplant International, 2009, 22, 408–415. [Google Scholar] [CrossRef] [PubMed]
- Ponticelli, C. Favi, and M. Ferraresso, New-Onset Diabetes after Kidney Transplantation. Medicina, 2021, 57, 250. [Google Scholar] [CrossRef] [PubMed]
- Hare, M.J.L. E. Shaw, and P.Z. Zimmet, Current controversies in the use of haemoglobin A<sub>1c</sub>. Journal of Internal Medicine, 2012, 271, 227–236. [Google Scholar] [CrossRef] [PubMed]
- Jenssen, T. and A.Hartmann, Emerging treatments for posttransplantation diabetes mellitus. Nature Reviews Nephrology, 2015, 11, 465–477. [Google Scholar] [CrossRef] [PubMed]
- Sharif, A. , et al., Proceedings From an International Consensus Meeting on Posttransplantation Diabetes Mellitus: Recommendations and Future Directions. American Journal of Transplantation, 2014, 14, 1992–2000. [Google Scholar] [CrossRef] [PubMed]
- Dai, C. , et al., Tacrolimus- and sirolimus-induced human β cell dysfunction is reversible and preventable. JCI Insight, 2020, 5. [Google Scholar] [CrossRef] [PubMed]
- Iatcu, C.O. Steen, and M.Covasa, Gut Microbiota and Complications of Type-2 Diabetes. Nutrients, 2021, 14, 166. [Google Scholar] [CrossRef] [PubMed]
- Lee, C.B. , et al., The Relationship between the Gut Microbiome and Metformin as a Key for Treating Type 2 Diabetes Mellitus. International Journal of Molecular Sciences, 2021, 22, 3566. [Google Scholar] [CrossRef]
- Lecamwasam, A. and E.I. Ekinci, Novel Associations of Empagliflozin on the Gut Microbiome and Metabolome in Type 2 Diabetes. The Journal of Clinical Endocrinology & Metabolism, 2022, 107, e4246–e4247. [Google Scholar] [CrossRef] [PubMed]
| Test | Result |
|---|---|
| Fasting Glucose | ≥ 126 mg/dL (7 mmol/L) on more than one occasion. |
| Random Glucose | ≥ 200 mg/dL (11.1 mmol/L) with symptoms. |
| Two-hour glucose after a 75-g OGTT | ≥ 200 mg/dL (11.1 mmol/L). |
| HbA1c | > 6.5% |
|
Modifiable risk factors |
Immuno suppression Rejection episodes Obesity Metabolic syndrome Hepatitis C virus infection |
|
Non-modifiable risk factors |
Age Ethnicity Male gender Family history of diabetes |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




