Submitted:
20 January 2024
Posted:
22 January 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Methods
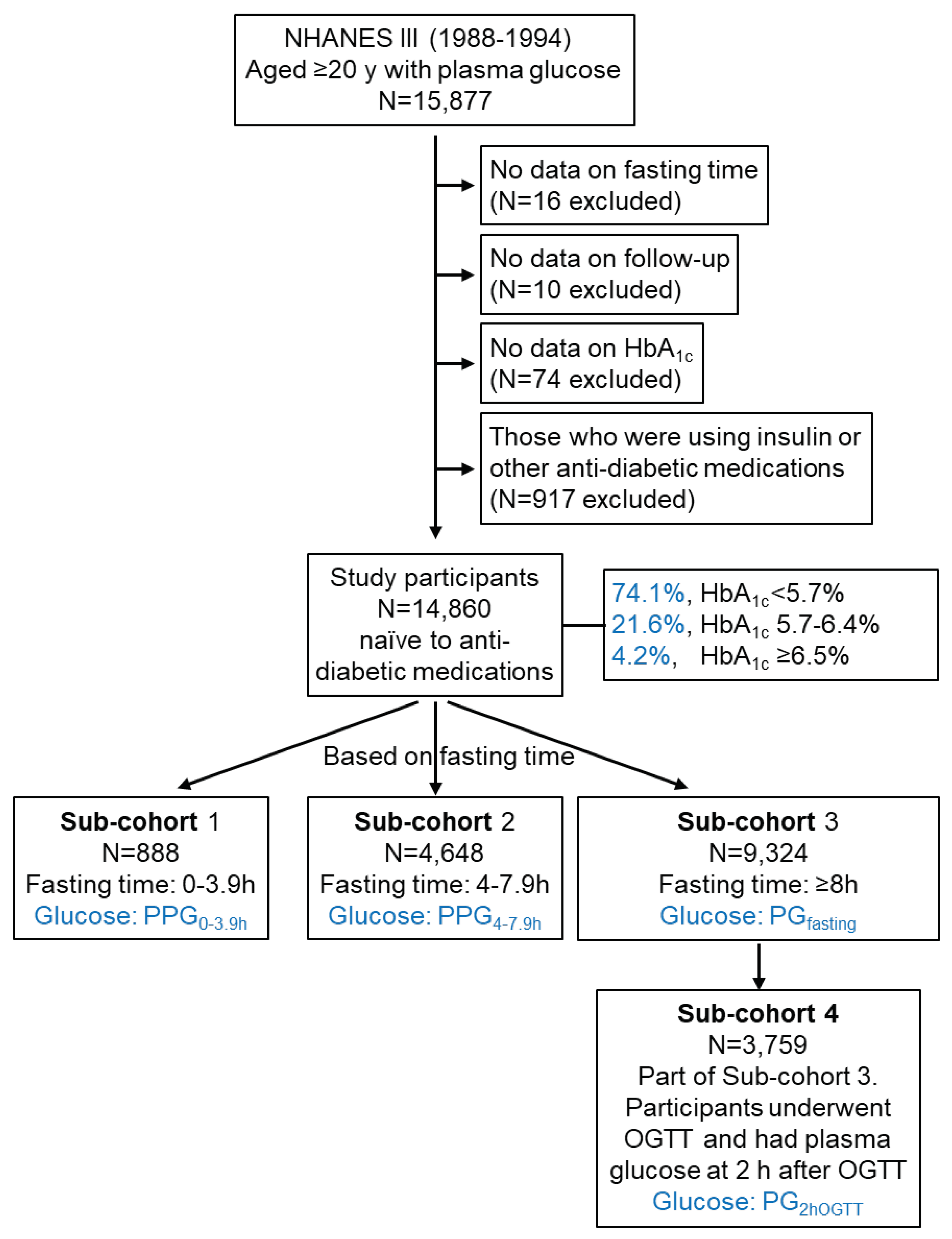
Study Participants
Exposures
Outcomes
Confounders
Statistical Analyses
Results
General Characteristics
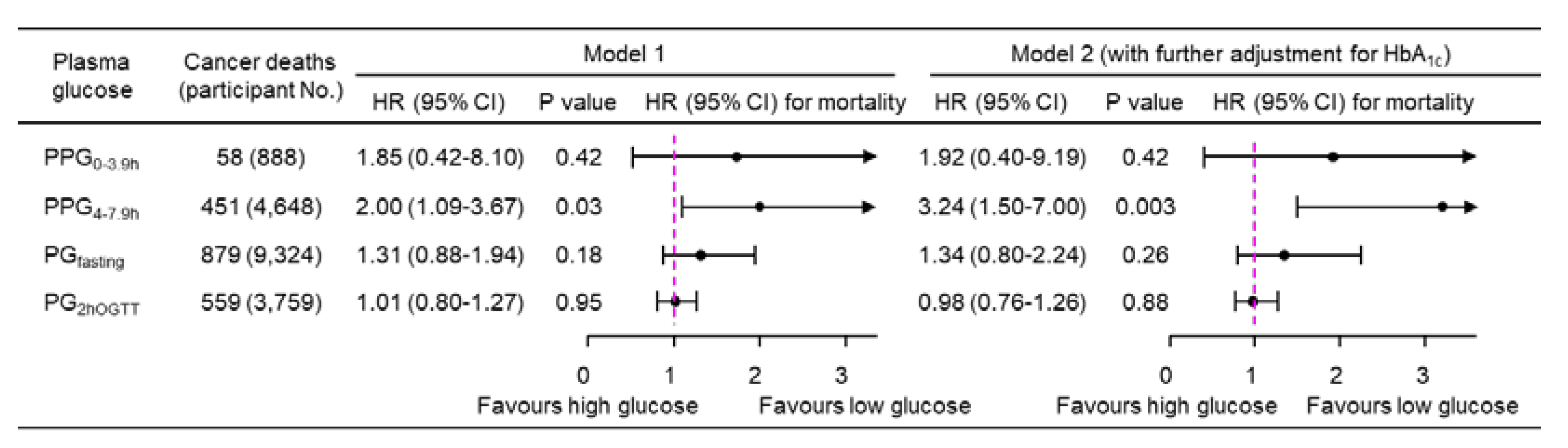
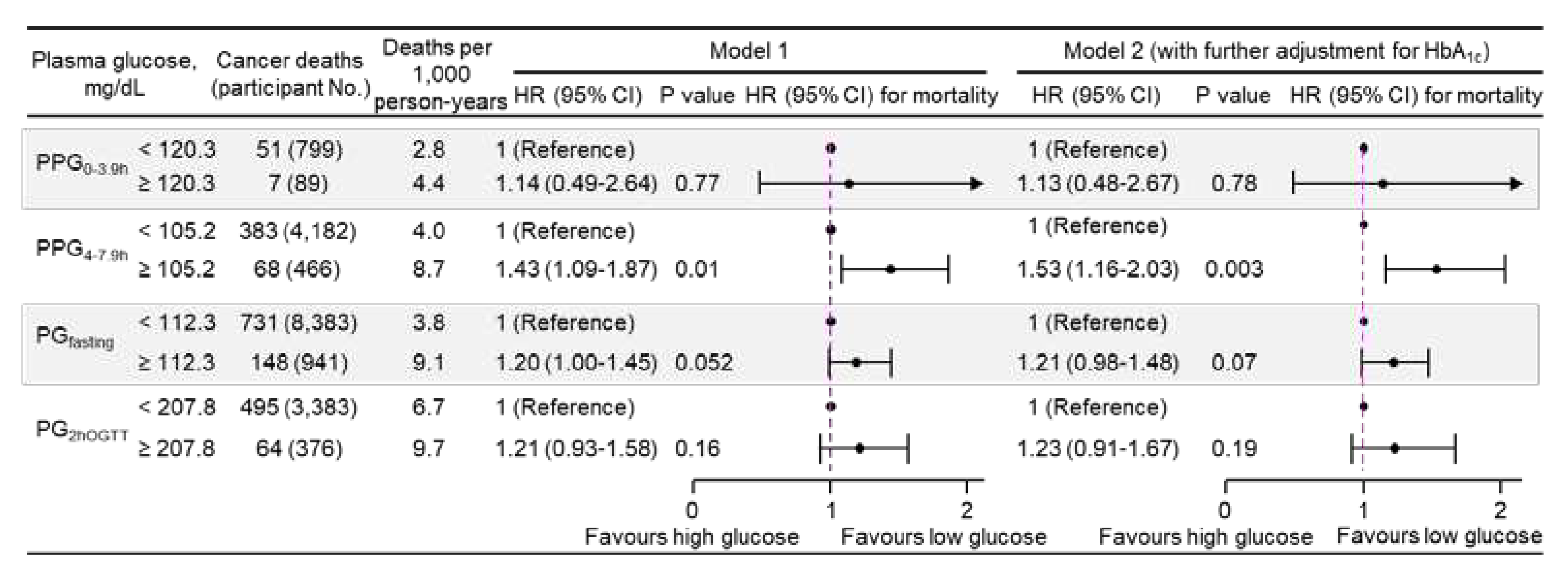
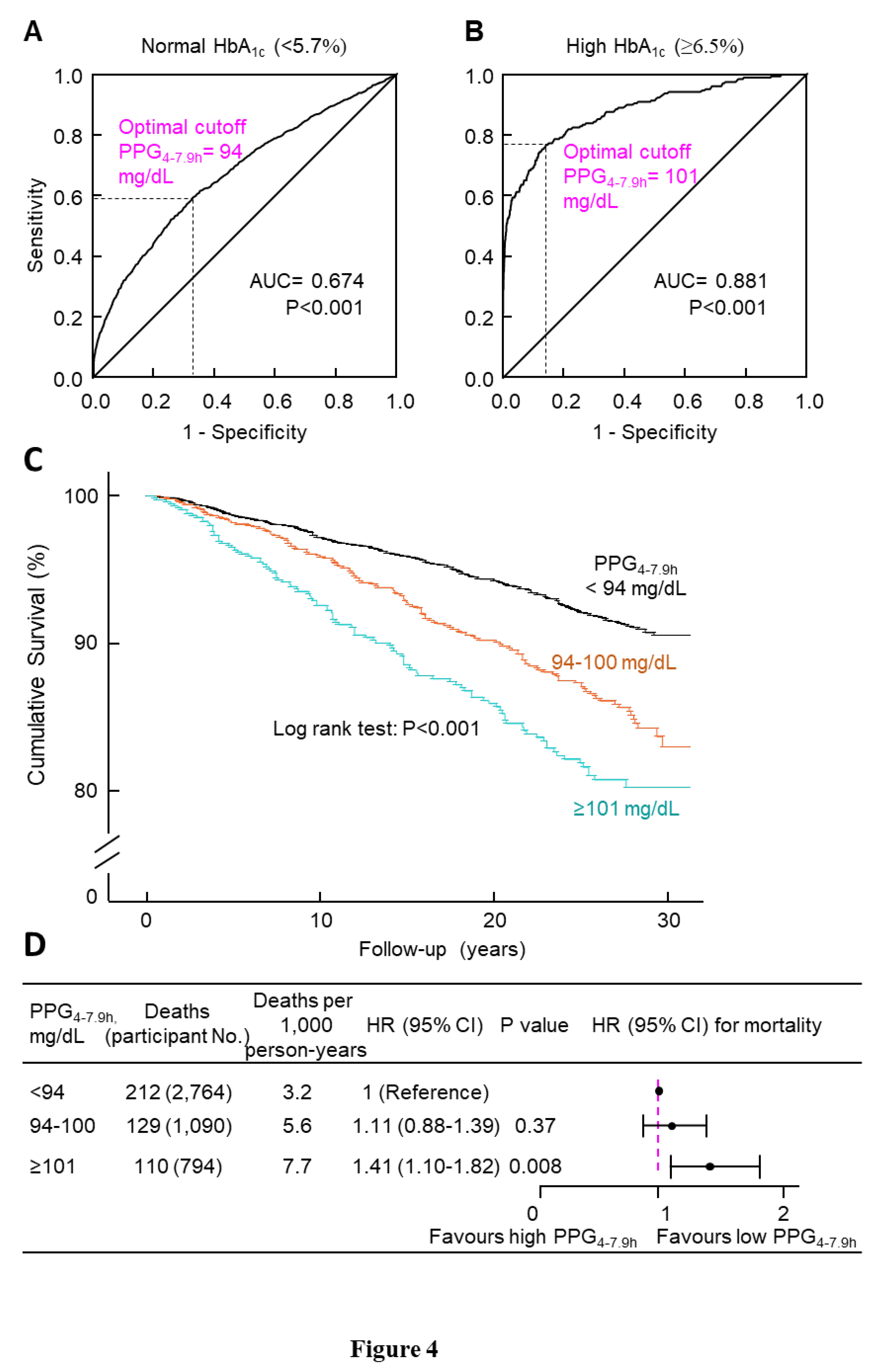
Association of Plasma Glucose with Mortality
Association of PPG4-7.9h with Cancer Mortality in Those with or without a Prior Diagnosis of Cancer
Variation of PPG4-7.9h over the Duration from 4 to 7.9 h
Discussion
Strengths and Limitations
Conclusions
Supplementary Materials
Author Contributions
Conflict of Interest Disclosures
Funding/Support
Role of the Funder/Sponsor
Data Sharing Statement
References
- Sung H, Ferlay J, Siegel RL, et al. Global Cancer Statistics 2020: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA: A Cancer Journal for Clinicians. 2021;71(3):209-249. [CrossRef]
- Vigneri P, Frasca F, Sciacca L, Pandini G, Vigneri R. Diabetes and cancer. Endocr Relat Cancer. 2009;16(4):1103-23. [CrossRef]
- Bjornsdottir HH, Rawshani A, Rawshani A, et al. A national observation study of cancer incidence and mortality risks in type 2 diabetes compared to the background population over time. Scientific Reports. 2020;10(1):17376. [CrossRef]
- Ballotari P, Vicentini M, Manicardi V, et al. Diabetes and risk of cancer incidence: results from a population-based cohort study in northern Italy. BMC Cancer. 2017;17(1):703. [CrossRef]
- Lam EKK, Batty GD, Huxley RR, et al. Associations of diabetes mellitus with site-specific cancer mortality in the Asia-Pacific region. Ann Oncol. 2011;22(3):730-738. https://doi.org/10.1093/annonc/mdq405. [CrossRef]
- Wang M, Sperrin M, Rutter MK, Renehan AG. Cancer is becoming the leading cause of death in diabetes. The Lancet. 2023;401(10391):1849. https://doi.org/10.1016/S0140-6736(23)00445-2. [CrossRef]
- Woo V, Shestakova MV, Ørskov C, Ceriello A. Targets and tactics: the relative importance of HbA, fasting and postprandial plasma glucose levels to glycaemic control in type 2 diabetes. Int J Clin Pract. 2008;62(12):1935-42. https://doi.org/10.1111/j.1742-1241.2008.01941.x. [CrossRef]
- Ceriello A, Colagiuri S, Gerich J, Tuomilehto J. Guideline for management of postmeal glucose. Nutr Metab Cardiovasc Dis. 2008;18(4):S17-33. https://doi.org/10.1016/j.numecd.2008.01.012. [CrossRef]
- Gerich JE. Clinical significance, pathogenesis, and management of postprandial hyperglycemia. Arch Intern Med. 2003;163(11):1306-16. [CrossRef]
- Peter R, Okoseime OE, Rees A, Owens DR. Postprandial glucose - a potential therapeutic target to reduce cardiovascular mortality. Curr Vasc Pharmacol. 2009;7(1):68-74. [CrossRef]
- Association AD. Postprandial Blood Glucose. Diabetes Care. 2001;24(4):775-778. [CrossRef]
- Takao T, Takahashi K, Suka M, Suzuki N, Yanagisawa H. Association between postprandial hyperglycemia at clinic visits and all-cause and cancer mortality in patients with type 2 diabetes: A long-term historical cohort study in Japan. Diabetes Res Clin Pract. 2019;148:152-159. [CrossRef]
- Eichenlaub MM, Khovanova NA, Gannon MC, Nuttall FQ, Hattersley JG. A Glucose-Only Model to Extract Physiological Information from Postprandial Glucose Profiles in Subjects with Normal Glucose Tolerance. J Diabetes Sci Technol. 2022;16(6):1532-1540. [CrossRef]
- Wang Y, Fang Y. Late non-fasting plasma glucose predicts cardiovascular mortality independent of hemoglobin A1c. Sci Rep. 2022;12:7778. [CrossRef]
- Wang Y. Definition, prevalence, and risk factors of low sex hormone-binding globulin in US adults. J Clin Endocrinol Metab. 2021;106(10):e3946–e3956. [CrossRef]
- Gunter EW, Lewis BG, Koncikowski SM. Laboratory Procedures Used for the Third National Health and Nutrition Examination Survey (NHANES III), 1988-1994. https://wwwn.cdc.gov/nchs/data/nhanes3/manuals/labman.pdf.
- Wang Y, Fang Y, Magliano DJ, et al. Fasting triglycerides are positively associated with cardiovascular mortality risk in people with diabetes. Cardiovasc Res. 2023;119(3):826–834. [CrossRef]
- Wang Y, Fang Y, Witting PK, et al. Dietary fatty acids and mortality risk from heart disease in US adults: an analysis based on NHANES. Scientific Reports. 2023;13(1):1614. [CrossRef]
- Wang Y, Fang Y, Sobey CG, Drummond GR. Prior cancer diagnosis and mortality profile in US adults. Am J Med Sci. 2023;365(2):176-183. [CrossRef]
- Wang Y. Higher fasting triglyceride predicts higher risks of diabetes mortality in US adults. Lipids in Health and Disease. 2021;20(1):181. [CrossRef]
- Fang Y, Wang Y. Fasting status modifies the association between triglyceride and all-cause mortality: A cohort study. Health Sci Rep. 2022;5:e642. [CrossRef]
- Kim H, Hu EA, Rebholz CM. Ultra-processed food intake and mortality in the USA: results from the Third National Health and Nutrition Examination Survey (NHANES III, 1988-1994). Public Health Nutr. 2019;22(10):1777-1785. [CrossRef]
- El Saadany T, Richard A, Wanner M, Rohrmann S. Sex-specific effects of leisure-time physical activity on cause-specific mortality in NHANES III. Prev Med. 2017;101:53-59. [CrossRef]
- Kubo Y, Noguchi T, Hayashi T, Tomiyama N, Ochi A, Hayashi H. Eating alone and weight change in community-dwelling older adults during the coronavirus pandemic: A longitudinal study. Nutrition. 2022;102:111697. [CrossRef]
- Wang Y. Stage 1 hypertension and risk of cardiovascular disease mortality in United States adults with or without diabetes. J Hypertens. 2022;40:794–803. [CrossRef]
- World Health Organization. Key facts-Diabetes. Availabe at https://www.who.int/news-room/fact-sheets/detail/diabetes. Accessed on 18 October 2023.
- American Diabetes Association. 2. Classification and Diagnosis of Diabetes: Standards of Medical Care in Diabetes—2021. Diabetes Care. 2021;44(the Supplement):S15-S33. [CrossRef]
- Diagnosis TECot, Mellitus CoD. Report of the Expert Committee on the Diagnosis and Classification of Diabetes Mellitus. Diabetes Care. 1997;20(7):1183-1197. [CrossRef]
- Wang Y, Zhang W, Qian T, et al. Reduced renal function may explain the higher prevalence of hyperuricemia in older people. Scientific Reports. 2021;11(1):1302. [CrossRef]
- Wang Y, Fang Y. Postabsorptive homeostasis model assessment for insulin resistance is a reliable biomarker for cardiovascular disease mortality and all-cause mortality. Diabetes Epidemiology and Management. 2021;6:100045. [CrossRef]
- Perkins NJ, Schisterman EF. The inconsistency of "optimal" cutpoints obtained using two criteria based on the receiver operating characteristic curve. Am J Epidemiol. 2006;163(7):670-5. [CrossRef]
- O’Neal TB, Luther EE. Dawn Phenomenon. StatPearls. StatPearls Publishing; 2022.
- Tjaden AH, Edelstein SL, Arslanian S, et al. Reproducibility of Glycemic Measures Among Dysglycemic Youth and Adults in the RISE Study. J Clin Endocrinol Metab. 2023;108(10):e1125-e1133. [CrossRef]
- Libman IM, Barinas-Mitchell E, Bartucci A, Robertson R, Arslanian S. Reproducibility of the oral glucose tolerance test in overweight children. J Clin Endocrinol Metab. 2008;93(11):4231-7. [CrossRef]
- Ko GT, Chan JC, Woo J, et al. The reproducibility and usefulness of the oral glucose tolerance test in screening for diabetes and other cardiovascular risk factors. Ann Clin Biochem. 1998;35 ( Pt 1):62-7. [CrossRef]
- Mandrekar JN. Receiver Operating Characteristic Curve in Diagnostic Test Assessment. Journal of Thoracic Oncology. 2010;5(9):1315-1316. [CrossRef]
- Peter R, Dunseath G, Luzio SD, Chudleigh R, Roy Choudhury S, Owens DR. Daytime variability of postprandial glucose tolerance and pancreatic B-cell function using 12-h profiles in persons with Type 2 diabetes. Diabet Med. 2010;27(3):266-73. [CrossRef]
- Avignon A, Radauceanu A, Monnier L. Nonfasting plasma glucose is a better marker of diabetic control than fasting plasma glucose in type 2 diabetes. Diabetes Care. 1997;20(12):1822-6. [CrossRef]
- Zhou XH, Qiao Q, Zethelius B, et al. Diabetes, prediabetes and cancer mortality. Diabetologia. 2010;53(9):1867-76. [CrossRef]
- Vander Heiden MG, Cantley LC, Thompson CB. Understanding the Warburg Effect: The Metabolic Requirements of Cell Proliferation. Science. 2009;324(5930):1029-1033. [CrossRef]
- Parekh N, Lin Y, Hayes RB, Albu JB, Lu-Yao GL. Longitudinal associations of blood markers of insulin and glucose metabolism and cancer mortality in the third National Health and Nutrition Examination Survey. Cancer Causes & Control. 2010;21(4):631-642. [CrossRef]
- Hsu CN, Chang CH, Lin YS, Lin JW, Caffrey JL. Association of serum C-peptide concentrations with cancer mortality risk in pre-diabetes or undiagnosed diabetes. PLoS One. 2013;8(2):e55625. [CrossRef]
- Otten J, Tavelin B, Söderberg S, Rolandsson O. Fasting C-peptide at type 2 diabetes diagnosis is an independent risk factor for total and cancer mortality. Diabetes Metab Res Rev. 2022;38(3):e3512. [CrossRef]
- Simon D, Senan C, Balkau B, Saint-Paul M, Thibult N, Eschwège E. Reproducibility of HbA1c in a healthy adult population: the Telecom Study. Diabetes Care. 1999;22(8):1361-1363. [CrossRef]
- Ramdass V, Caskey E, Sklarz T, et al. Association Between Obesity and Cancer Mortality: An Internal Medicine Outpatient Clinic Perspective. J Clin Med Res. 2021;13(7):377-386. [CrossRef]
- Nakanishi S, Yamada M, Hattori N, Suzuki G. Relationship between HbA(1)c and mortality in a Japanese population. Diabetologia. 2005;48(2):230-4. [CrossRef]
- Darras P, Mattman A, Francis GA. Nonfasting lipid testing: the new standard for cardiovascular risk assessment. CMAJ. 2018;190(45):E1317-E1318. [CrossRef]
- Grundy SM, Stone NJ, Bailey AL, et al. 2018 AHA/ACC/AACVPR/AAPA/ABC/ACPM/ADA/AGS/APhA/ASPC/NLA/PCNA Guideline on the Management of Blood Cholesterol: A Report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation. 2019;139(25):e1082-e1143. [CrossRef]
- Giovannucci E, Harlan DM, Archer MC, et al. Diabetes and cancer: a consensus report. Diabetes Care. 2010;33(7):1674-85. [CrossRef]
- Menke A, Muntner P, Batuman V, Silbergeld EK, Guallar E. Blood lead below 0.48 micromol/L (10 microg/dL) and mortality among US adults. Circulation. 2006;114(13):1388-94. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



