Submitted:
11 January 2024
Posted:
12 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Population and Study Design
2.2. Data Collection
2.3. Objectives
2.4. Statistical Analysis
3. Results
3.1. Patient characteristics
3.2. Infection characteristics
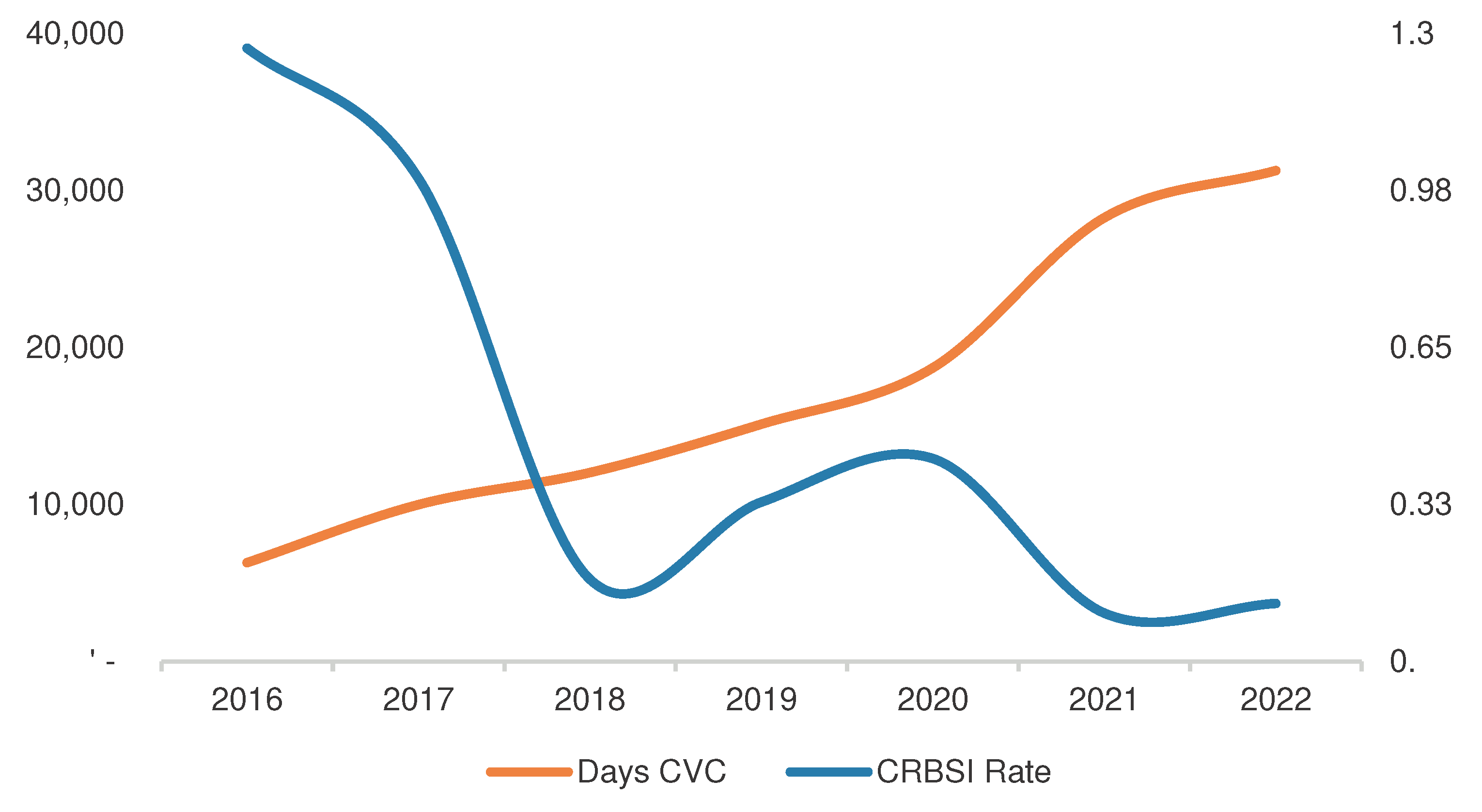
3.3. Evolution of Incidence Over the Study Period
4. Discussion
5. Conclusions
Funding
Conflicts of Interest
References
- Allon, M. Dialysis catheter-related bacteremia: Treatment and prophylaxis. Am J Kidney Dis. 2004, 44, 779–791. [Google Scholar] [CrossRef]
- Martin K, Poy Lorenzo YS, Mia Leung PY, Chung S, O’flaherty E, Barket N, Ierino F. Clinical outcomes and risk factors for tunneled hemodialysis catheter-related bloodstream infections. OFID 2020, 7. [CrossRef] [PubMed]
- Ibeas J et al. Guía Clínica española de acceso vascular para hemodiálisis. NEFROLOGÍA. 2017, 37, 1-19. [CrossRef]
- Lok C.E. et al. KDOQI Clinical Practice Guideline for Vascular Access. Am J Kidney Dis. 2019, 75.
- United States Renal Data System: 2020 USRDS Annual Data Report: Epidemiology of Kidney Disease in the United Stated, bETHESTA, md, national Institutes od Health, National Institute os Diabetes and Digestive and Kidney Diseases, 2020.
- Mokrzycki MH, Zhang M, Golestaneh L, Laut J, O Rosenberg S. An interventional controlled trial comparing 2 management models for treatment of tunneled cuffed catheter bacteremia: A collabo-rative team model versus usual physician-managed care. Am J Kidney Dis 2006, 48, 587-59. [CrossRef] [PubMed]
- Heidempergher M, Sabiu G, Orani MA, Tripepi G, Gallieni M. Targeting covid-19 prevention in hemodialysis, facilities is associated with a drastic reduction In central venous catheter-related in-fections. Journal of Nephrology 2021, 34, 345-35. [CrossRef] [PubMed]
- Johansen KL, Gilberston DT, Wetmore JB, Peng Y, Liu J, Winhandi ED. Catheter-associated bloodstream infections among patients on hemodialysis. Clin J Am Soc Nephrol. 2022, 17, 429-433. [CrossRef]
- Pisoni RL, Zepel L, Port FK, Robinson BM. Trends in US vascular access use, patient preferences, and related practices: An update from the US Dopps Practice Monitor with international compari-sons. Am J Kidney Dis. 2015, 65, 905-91. [CrossRef]
- Almenara-Tejederas M, Rodríguez-Pérez MA, Moyano-Franco MJ, de Cueto-López M, Rodrí-guez-Baño J, Salgueira-Lazo M. Tunneled catheter-related bacteremia in hemodialysis patients: In-cidencia, risk factors and outcomes. A 14-year observational study. Journal of Nephrology. 2022, 36, 203.21. [CrossRef]
- Lok CE, Thumma JR, McCullough KP, Gillespie BW, Fluck RJ, Marshall MR, Kawanishi H, Ro-binson BM, Pisoni RL. Catheter-related infection and septicemia: Impact of seasonality and modifi-able practices from the Dopps. Semin Dial 2013, 27, 72–77. [CrossRef] [PubMed]
- Farrington CA, Allon M. Complications of hemodialysis catheter bloodstream infections: Impact of infecting organism. Am J Nephrol. 2019, 50, 126-132. [CrossRef]
- Marr KA, Sexton DJ, Conlon PJ, Corey GR, Schwab SJ, Kirkland KB. Catheter-related bactere-mia and outcome of attempted catheter salvage in patients undergoing hemodialysis. Ann Intern Med. 1997, 127, 27. [CrossRef]
- Beathard, GA. Beathard GA. Management of bacteremia associated with tunneled-cuffed hemodialysis cathe-ters. JASN. 1999; 10(5): 1045-1049.
- Phillips J, Chan DT, Swaminathan R, Patankar K, Boudville N, Lim WH. Haemodialysis vascular catheter-related blood stream infection: Organism types and clinical outcomes. Nephrology. 2023, 28, 249-253. [CrossRef]
- Maya ID, Carlton D, Estrada E, Allon M. Treatment of dialysis catheter-related Staphylococcus aureus bacteremia with an antibiotic lock: A quality improvement report. Am J Kidney Dis. 2007, 50, 289-295. [CrossRef]
- Costerson JW, Stewart PS, Greenberg EP. Bacterial biofilms: A common cause of persistent infection. Science. 1999, 284, 1318-132. [CrossRef]
- Paharik AE, Horswill AR. The staphylococcal biofilm: Adhesins, regulation, and host response. Microbiol Spectr. 2016, 4. Microbiol Spectr. [CrossRef]
- Shahar S, Mustafar R, Kamaruzaman L, Periyasamy P, Pau KB, Ramli R. Catheter-related bloodstream infections and catheter colonization among haemodialysis patients: Prevalence, risk factors and outcomes. Int J Nephrol. 2021, 1-9. [CrossRef]
- Abe R, Oda S, Sadahiro T, Nakamura M, Hirayama Y, Tateishi Y, Shinozaki K, Hirasawa H. Gram-negative bacteremia induces greater magnitude of inflammatory responde than gram-positive bacteremia. Cria Care. 2010, 14, R27.
- González R, Redondo MC, Caro I, Ojeda MD, García AM, Huerga MC, Gómez M, Molina MC, García S, Fernández R, Canovas Y. Estudio de la eficacia del sellado con taurolidina y nitrato 4% para hemodiálisis en la prevención de infección y trombosis. Enferm Nefro. 2014, 17, 22.27. [CrossRef]
| Age (mean, SD) | 67 (+11.016) |
| Male (n,%) | 39 (74.6%) |
| Charlson index (median, IR) | 8 (6-9) |
Etiology of CKD
|
29 (43.3%) 19 (28.4%) 11 (16.4%) 1 (1.5%) 3 (4.5%) 4 (6%) |
| Months in hemodialysis (median, IR) | 24 (4-48) |
| Kidney transplant (n,%) | 6 (9%) |
Site of catheter
|
60 (89.5%) 7 (10.5%) |
| Catheter half-life until infection (median, IR) | 240 (28-930) |
| Immunosuppressive treatment (n,%) | 4 (7.7%) |
| Early infection (n,%) | 17 (25.3%) |
Season of infection
|
16 (23.9%) 29 (43.3%) 11 (16.4%) 11 (16.4%) |
Microbiological isolation
|
34 (50.7%) 6 (9%) 1 (1.5%) 4 (6%) 7 (10.4%) 2 (3%) 1 (1.5%) 1 (1.5%) 1 (1.5%) 1 (1.5%) 1 (1.5%) 1 (1.5%) 1 (1.5%) |
| Days of hospitalization (median, IR) | 7 (5-12) |
| ICU admissions (n,%) | 5 (7.4%) |
| Metastasic complications (n,%) | 2 (2.9%) |
| Catheter removal (n,%) | 45 (67.1%) |
| Patients with recurrence of bacteriemia (n,%) | 10 (19.2%) |
| Comparative years | OR | CI 95% | p |
|---|---|---|---|
| 2016-2017 | 1.26 | 0.5-3.21 | 0.6 |
| 2016-2018 | 7,64 | 1.62-36.02 | 0.01 |
| 2016-2019 | 3,84 | 1.35-11.75 | 0.01 |
| 2016-2020 | 2.97 | 1.1-7.92 | 0.02 |
| 2016-2021 | 11.97 | 3.17-45.6 | <0.001 |
| 2016-2022 | 1.93 | 2.9-33.01 | P<0.001 |
| 2017-2018 | 6.02 | 1.21-27.49 | 0.02 |
| 2017-2019 | 3.02 | 1.03-8.85 | 0.04 |
| 2017-2020 | 2.34 | 0.92-5.93 | 0.07 |
| 2017-2021 | 9.43 | 2.59-34.29 | <0.001 |
| 2017-2022 | 7.82 | 2.45-24.96 | <0.001 |
| 2018-2019 | 0.5 | 0.97-2.59 | 0.4 |
| 2018-2020 | 0.38 | 0.08-1.83 | 0.4 |
| 2018-2021 | 1.56 | 0.26-9.37 | 0.6 |
| 2018-2022 | 1.29 | 0.23-7.09 | 0.7 |
| 2019-2020 | 1.29 | 0.25-2.36 | 0.6 |
| 2019-2021 | 3.11 | 0.74-13.04 | 0.1 |
| 2019-2022 | 2.58 | 0.69-9.63 | 0.1 |
| 2020-2021 | 4.02 | 1.06-15.19 | 0.03 |
| 2020-2022 | 3.34 | 1.1-11.1 | 0.05 |
| 2021-2022 | 0.82 | 0.18-3.7 | 0.8 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




