Submitted:
02 January 2024
Posted:
03 January 2024
You are already at the latest version
Abstract
Keywords:
Introduction
Patient Presentation
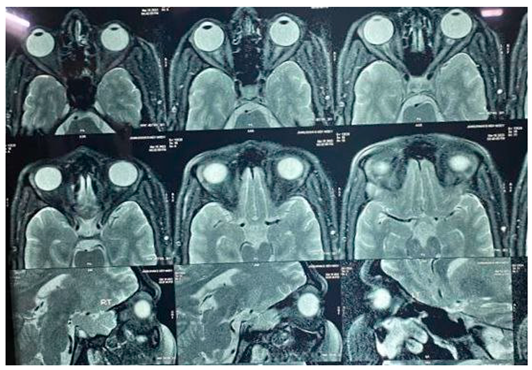
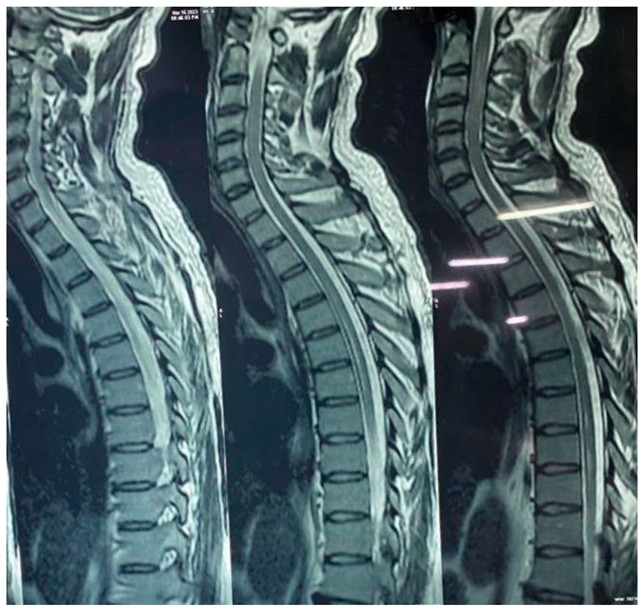
- Bilateral optic neuritis.
- Brain appears unremarkable.
- Abnormal signal /oedema involving spinal cord.
- Neuromyelitis Optica Spectrum Disorder (NMOSD)
- Multiple Sclerosis
- Myelin Oligodendrocyte Glycoprotein Antibody Associated Disease (MOGAD)
- Acute Disseminated Encephalomyelitis (ADEM)
- Idiopathic Transverse Myelitis
- Idiopathic Optic Neuritis
- 1gm Methylprednisolone I.V Pulse Therapy: The patient received an initial course of intravenous Methylprednisolone pulse therapy, resulting in mild clinical improvement.
- Plasma Exchange Therapy (PLEX) and Physiotherapy: Subsequently, the patient underwent five cycles of Plasma Exchange Therapy (PLEX) alongside physiotherapy sessions to address the symptoms and promote recovery.
- IV Cyanocobalamin (1500 micrograms OD): As part of the treatment regimen, the patient was administered intravenous Cyanocobalamin at a daily dose of 1500 micrograms.
- Pain Management: Pain management was a crucial aspect of the patient's care. Initially, a Tramadol trial was administered, followed by a transition to Gabapentin (300mg TDS) to manage pain effectively.
- Prednisolone: To continue addressing the autoimmune component of NMOSD.
- Mycophenolate Mofetil: As part of the long-term immunosuppressive therapy plan.
Discussion
- At least 1 Core Clinical Characteristic
- Positive Test for AQP4-IgG Using the Best Available Detection Method
- Exclusion of Alternative Diagnoses
- At least 2 Core Clinical Characteristics Resulting from One or More Clinical Attacks and Meeting All of the Following Requirements:
- At least 1 Core Clinical Characteristic Must Be One of the Following:
- Optic Neuritis
- Acute Myelitis with Longitudinally Extensive Transverse Myelitis (LETM)
- Area Postrema Syndrome (episode of otherwise unexplained hiccups or nausea and vomiting)
- Dissemination in Space (2 or More Different Core Clinical Characteristics)
- Fulfillment of Additional MRI Requirements, as Applicable
- Negative Tests for AQP-4 IgG Using the Best Available Detection Method, or Testing Unavailable
- Exclusion of Alternative Diagnosis
- Optic Neuritis
- Acute Myelitis
- Area Postrema Syndrome (episode of otherwise unexplained hiccups or nausea and vomiting)
- Acute Brainstem Syndrome
- Symptomatic Narcolepsy or Acute Diencephalic Clinical Syndrome with NMOSD-Typical Diencephalic MRI Lesions
- Symptomatic Cerebral Syndrome with NMOSD-Typical Brain Lesions
- Acute Optic Neuritis: Requires brain MRI showing either (a) normal findings or only nonspecific white matter lesions, OR (b) optic nerve MRI with a T2-hyperintense lesion or T1-weighted gadolinium-enhancing lesion extending over >1/2 optic nerve length or involving the optic chiasm.
- Acute Myelitis: Requires associated intramedullary MRI lesion extending over >= 3 contiguous segments (LETM) OR >=3 contiguous segments of focal spinal cord atrophy in patients with a history compatible with acute myelitis.
- Area Postrema Syndrome: Requires associated dorsal medulla/area postrema lesions.
- Acute Brainstem Syndrome: Requires associated periependymal brainstem lesions.
References
- Jarius S, Wildemann B. The history of neuromyelitis optica. J Neuroinflammation. 2013;10:8. Published 2013 Jan 15. [CrossRef]
- Huda S, Whittam D, Bhojak M, Chamberlain J, Noonan C, Jacob A. Neuromyelitis optica spectrum disorders. Clin Med (Lond). 2019;19(2):169-176. [CrossRef]
- Wu Y, Zhong L, Geng J. Neuromyelitis optica spectrum disorder: Pathogenesis, treatment, and experimental models. Mult Scler Relat Disord. 2019;27:412-418. [CrossRef]
- Wingerchuk DM, Banwell B, Bennett JL, et al. International consensus diagnostic criteria for neuromyelitis optica spectrum disorders. Neurology. 2015;85(2):177-189. [CrossRef]
- Hor JY, Asgari N, Nakashima I, et al. Epidemiology of Neuromyelitis Optica Spectrum Disorder and Its Prevalence and Incidence Worldwide. Front Neurol. 2020;11:501. Published 2020 Jun 26. [CrossRef]
- Kessler RA, Mealy MA, Levy M. Treatment of Neuromyelitis Optica Spectrum Disorder: Acute, Preventive, and Symptomatic. Curr Treat Options Neurol. 2016;18(1):2. [CrossRef]
- Page 3477, Chapter 445 : Neuromyelitis Optica, Harrison’s principles of Internal Medicine 21st edition Volume -2 , ISBN : 978-1-26-426851-1, MHID: 1-26-426851-3.
- Mitsdoerffer M, Kuchroo V, Korn T. Immunology of neuromyelitis optica: a T cell-B cell collaboration. Ann N Y Acad Sci. 2013;1283:57-66. [CrossRef]
- Meca-Lallana JE, Gómez-Ballesteros R, Pérez-Miralles F, et al. Impact of Neuromyelitis Optica Spectrum Disorder on Quality of Life from the Patients' Perspective: An Observational Cross-Sectional Study. Neurol Ther. 2022;11(3):1101-1116. [CrossRef]
- Levin MH, Bennett JL, Verkman AS. Optic neuritis in neuromyelitis optica. Prog Retin Eye Res. 2013;36:159-171. [CrossRef]
- Abboud H, Salazar-Camelo A, George N, et al. Symptomatic and restorative therapies in neuromyelitis optica spectrum disorders. J Neurol. 2022;269(4):1786-1801. [CrossRef]
| Higher mental function | Normal |
| Motor system | Muscle bulk and tone were normal in left upper limb. Reduced in Right upper and lower limb and left lower limb. Power : +5 in Left upper limb +1 in Left lower limb +1 in Right upper limb 0 in Right lower limb |
| Cranial Nerve examination | No light perception bilaterally Rest cranial nerves normal. |
| Sensory system | Normal |
| Reflexes | Biceps reflex : +2 Bilaterally Triceps reflex : +2 bilaterally Ankle reflex : +2 bilaterally Knee reflex : 0 bilaterally |
| Hb | 8.1 mg/dl |
| Platelets | 358 * 103 / cmm |
| RBC count | 3.21* 106 / cmm |
| Total WBC count | 12.11 * 103 / cmm |
| S. AQP-4 IgG | Negative |
| Physical examination | Normal |
| CSF Protein | 107.7 mg/dl |
| CSF Glucose | 60.38 mg/dl |
| CSF Chloride | 125.98 mmol/lit |
| CSF Total Cell Count | 30 (Lymphocytes – 100%) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




