Submitted:
02 January 2024
Posted:
03 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Characteristics of patients with non-infectious uveitis (NIU)
3.2. Need for IS and/or BT treatment.
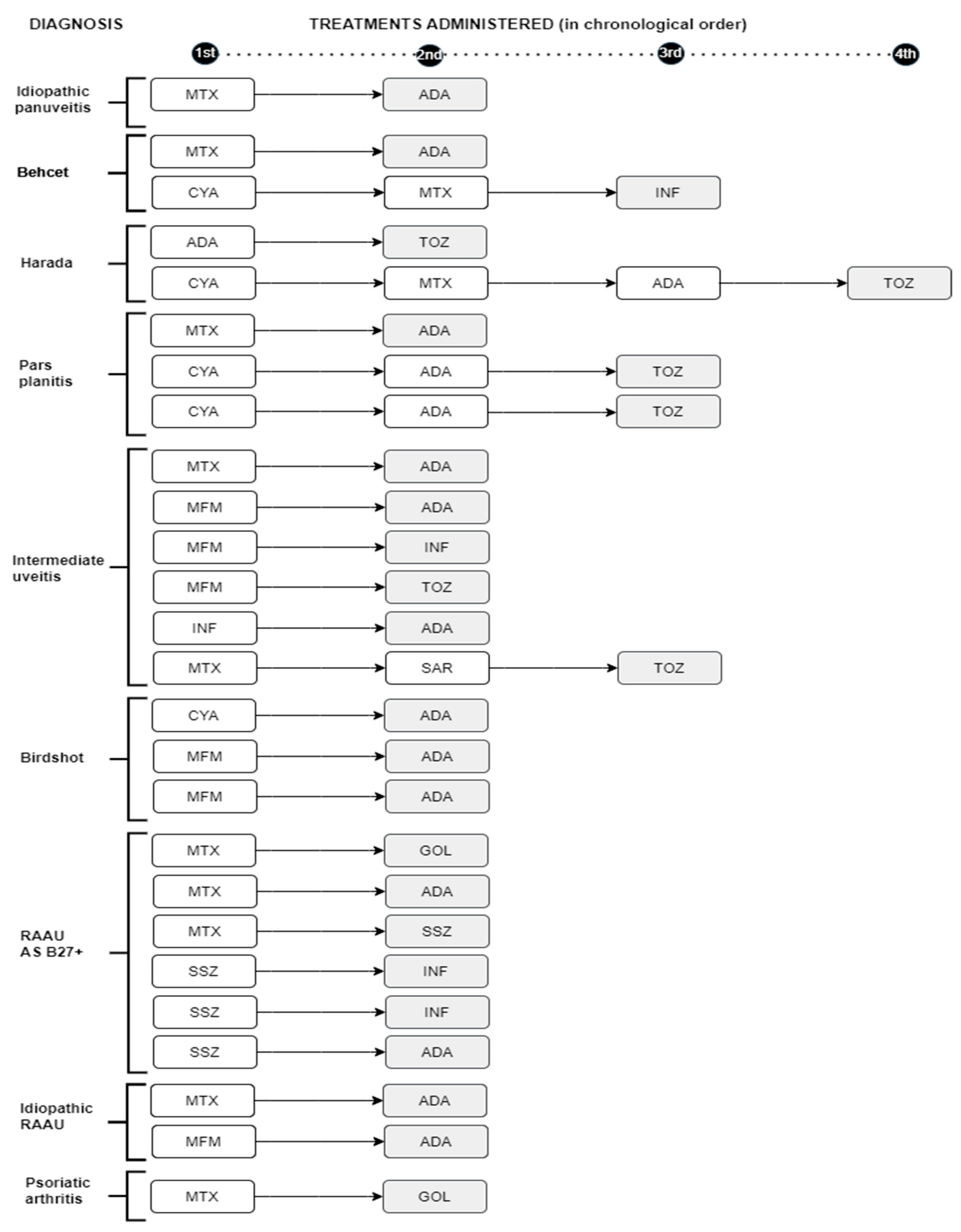
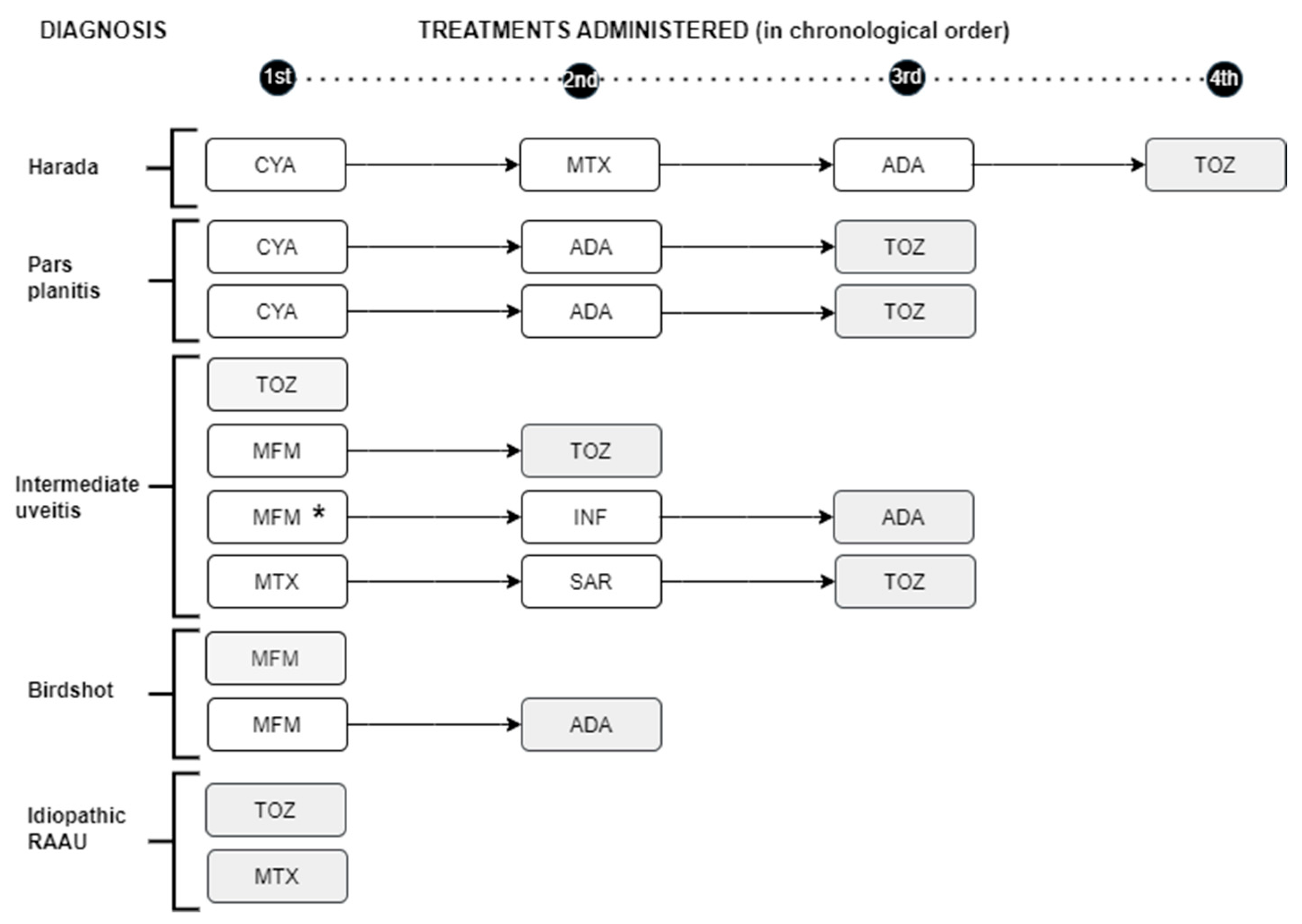
3.3. Response to treatment
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Conflicts of Interest
References
- E.Cunningham ET, Zierhut M. Vision Loss in Uveitis. Ocular Immunology and Inflammation. 2021;29(6):1037-9.
- Tomkins-Netzer O, Talat L, Bar A, Lula A, Taylor SRJ, Joshi L, et al. Long-term clinical outcome and causes of vision loss in patients with uveitis. Ophthalmology. 2014;121(12):2387-92.
- de Smet MD, Taylor SRJ, Bodaghi B, Miserocchi E, Murray PI, Pleyer U, et al. Understanding uveitis: the impact of research on visual outcomes. Prog Retin Eye Res. 2011;30(6):452-70.
- Rosenbaum JT, Bodaghi B, Couto C, Zierhut M, Acharya N, Pavesio C, et al. New observations and emerging ideas in diagnosis and management of non-infectious uveitis: A review. Semin Arthritis Rheum. 2019;49(3):438-45.
- van Laar JAM, Rothova A, Missotten T, Kuijpers RWAM, van Hagen PM, van Velthoven MEJ. Diagnosis and treatment of uveitis; not restricted to the ophthalmologist. J Clin Transl Res. 2015;1(2):94-9.
- Lowder C, Belfort R, Lightman S, Foster CS, Robinson MR, Schiffman RM, et al. Dexamethasone intravitreal implant for noninfectious intermediate or posterior uveitis. Arch Ophthalmol. 2011;129(5):545-53.
- Callanan DG, Jaffe GJ, Martin DF, Pearson PA, Comstock TL. Treatment of posterior uveitis with a fluocinolone acetonide implant: three-year clinical trial results. Arch Ophthalmol. 2008;126(9):1191-201.
- Jabs DA, Rosenbaum JT, Foster CS, Holland GN, Jaffe GJ, Louie JS, et al. Guidelines for the use of immunosuppressive drugs in patients with ocular inflammatory disorders: recommendations of an expert panel. Am J Ophthalmol. 2000;130(4):492-513.
- Nguyen QD, Hatef E, Kayen B, Macahilig CP, Ibrahim M, Wang J, et al. A cross-sectional study of the current treatment patterns in noninfectious uveitis among specialists in the United States. Ophthalmology. 2011;118(1):184-90.
- Dick AD, Rosenbaum JT, Al-Dhibi HA, Belfort R, Brézin AP, Chee SP, et al. Guidance on Noncorticosteroid Systemic Immunomodulatory Therapy in Noninfectious Uveitis: Fundamentals Of Care for UveitiS (FOCUS) Initiative. Ophthalmology. 2018;125(5):757-73.
- Suhler EB, Adán A, Brézin AP, Fortin E, Goto H, Jaffe GJ, et al. Safety and Efficacy of Adalimumab in Patients with Noninfectious Uveitis in an Ongoing Open-Label Study: VISUAL III. Ophthalmology. 2018;125(7):1075-87.
- Jaffe GJ, Dick AD, Brézin AP, Nguyen QD, Thorne JE, Kestelyn P, et al. Adalimumab in Patients with Active Noninfectious Uveitis. N Engl J Med. 2016;375(10):932-43.
- Takeuchi M, Kezuka T, Sugita S, Keino H, Namba K, Kaburaki T, et al. Evaluation of the long-term efficacy and safety of infliximab treatment for uveitis in Behçet’s disease: a multicenter study. Ophthalmology. 2014;121(10):1877-84.
- Levy-Clarke G, Jabs DA, Read RW, Rosenbaum JT, Vitale A, Van Gelder RN. Expert panel recommendations for the use of anti-tumor necrosis factor biologic agents in patients with ocular inflammatory disorders. Ophthalmology. 2014;121(3):785-796.e3.
- Sepah YJ, Sadiq MA, Chu DS, Dacey M, Gallemore R, Dayani P, et al. Primary (Month-6) Outcomes of the STOP-Uveitis Study: Evaluating the Safety, Tolerability, and Efficacy of Tocilizumab in Patients With Noninfectious Uveitis. Am J Ophthalmol. 2017;183:71-80.
- Leclercq M, Andrillon A, Maalouf G, Sève P, Bielefeld P, Gueudry J, et al. Anti-Tumor Necrosis Factor α versus Tocilizumab in the Treatment of Refractory Uveitic Macular Edema: A Multicenter Study from the French Uveitis Network. Ophthalmology. 2021;S0161-6420(21)00900-3.
- Deschenes J, Murray PI, Rao NA, Nussenblatt RB, International Uveitis Study Group. International Uveitis Study Group (IUSG): clinical classification of uveitis. Ocul Immunol Inflamm. 2008;16(1):1-2.
- Jabs DA, Nussenblatt RB, Rosenbaum JT, Standardization of Uveitis Nomenclature (SUN) Working Group. Standardization of uveitis nomenclature for reporting clinical data. Results of the First International Workshop. Am J Ophthalmol. 2005;140(3):509-16.
- Pistilli M, Joffe MM, Gangaputra SS, Pujari SS, Jabs DA, Levy-Clarke GA, et al. Visual Acuity Outcome over Time in Non-Infectious Uveitis. Ocul Immunol Inflamm. 2021;29(6):1064-71.
- Hunter RS, Skondra D, Papaliodis G, Sobrin L. Role of OCT in the diagnosis and management of macular edema from uveitis. Semin Ophthalmol. 2012;27(5-6):236-41.
- Gómez-Gómez A, Loza E, Rosario MP, Espinosa G, Morales JMGR de, Herreras JM, et al. Efficacy and safety of immunomodulatory drugs in patients with anterior uveitis: A systematic literature review. Medicine (Baltimore). 2017;96(42):e8045.
- Gómez-Gómez A, Loza E, Rosario MP, Espinosa G, de Morales JMGR, Herrera JM, et al. Efficacy and safety of immunomodulatory drugs in patients with non-infectious intermediate and posterior uveitis, panuveitis and macular edema: A systematic literature review. Seminars in Arthritis and Rheumatism. 2020;50(6):1299-306.
- García-Aparicio A, Alonso Martín L, López Lancho R, Quirós Zamorano R, Del Olmo Perez L, Sánchez Fernández S, et al. Epidemiology of Uveitis in a Spanish Region: Prevalence and Etiology. Ophthalmic Epidemiol. 2021;28(3):227-36.
- Millán-Longo C, Peiteado D, Schlincker A, Hidalgo V, Pieren A, Balsa A, et al. Use of Immunomodulatory Drugs at a Uveitis Clinic. Reumatol Clin (Engl Ed). 2019;15(5):271-6.
- Chang JHM, Wakefield D. Uveitis: a global perspective. Ocul Immunol Inflamm. 2002;10(4):263-79.
- Wang L, Guo Z, Zheng Y, Li Q, Yuan X, Hua X. Analysis of the clinical diagnosis and treatment of uveitis. Annals of Palliative Medicine. 2021;10(12):127822788-127812788.
- Bajwa A, Osmanzada D, Osmanzada S, Khan I, Patrie J, Xin W, et al. Epidemiology of uveitis in the mid-Atlantic United States. Clin Ophthalmol. 2015;9:889-901.
- Foster CS, Kothari S, Anesi SD, Vitale AT, Chu D, Metzinger JL, et al. The Ocular Immunology and Uveitis Foundation preferred practice patterns of uveitis management. Surv Ophthalmol. 2016;61(1):1-17.
- Muñoz-Fernández S, García-Aparicio AM, Hidalgo MV, Platero M, Schlincker A, Bascones ML, et al. Methotrexate: an option for preventing the recurrence of acute anterior uveitis. Eye (Lond). 2009;23(5):1130-3.
- Rathinam SR, Babu M, Thundikandy R, Kanakath A, Nardone N, Esterberg E, et al. A Randomized Clinical Trial Comparing Methotrexate and Mycophenolate Mofetil for Noninfectious Uveitis. Ophthalmology. 2014;121(10):1863-70.
- Guillot X, Prati C, Sondag M, Wendling D. Etanercept for treating axial spondyloarthritis. Expert Opin Biol Ther. 2017;17(9):1173-81.
- Wang F, Wang NS. Etanercept therapy-associated acute uveitis: a case report and literature review. Clin Exp Rheumatol. 2009;27(5):838-9.
- Benitez-Del-Castillo JM, Garcia-Sanchez J, Iradier T, Bañares A. Sulfasalazine in the prevention of anterior uveitis associated with ankylosing spondylitis. Eye (Lond). 2000;14 ( Pt 3A):340-3.
- Gómez-Gómez A, Loza E, Rosario MP, Espinosa G, de Morales JMGR, Herrera JM, et al. Efficacy and safety of immunomodulatory drugs in patients with non-infectious intermediate and posterior uveitis, panuveitis and macular edema: A systematic literature review. Semin Arthritis Rheum. 2020;50(6):1299-306.
- Shen E, Rathinam SR, Babu M, Kanakath A, Thundikandy R, Lee SM, et al. Outcomes of Vogt-Koyanagi-Harada Disease: A Subanalysis From a Randomized Clinical Trial of Antimetabolite Therapies. American Journal of Ophthalmology. 2016;168:279-86.
- Fardeau C, Champion E, Massamba N, LeHoang P. Uveitic macular edema. Eye (Lond). 2016;30(10):1277-92.
- Vegas-Revenga N, Calvo-Río V, Mesquida M, Adán A, Hernández MV, Beltrán E, et al. Anti-IL6-Receptor Tocilizumab in Refractory and Noninfectious Uveitic Cystoid Macular Edema: Multicenter Study of 25 Patients. Am J Ophthalmol. 2019;200:85-94.
- Suhler EB, Jaffe GJ, Fortin E, Lim LL, Merrill PT, Dick AD, et al. Long-Term Safety and Efficacy of Adalimumab in Patients with Noninfectious Intermediate Uveitis, Posterior Uveitis, or Panuveitis. Ophthalmology. 2021;128(6):899-909.
- Heissigerová J, Callanan D, de Smet MD, Srivastava SK, Karkanová M, Garcia-Garcia O, et al. Efficacy and Safety of Sarilumab for the Treatment of Posterior Segment Noninfectious Uveitis (SARIL-NIU): The Phase 2 SATURN Study. Ophthalmology. 2019;126(3):428-37.
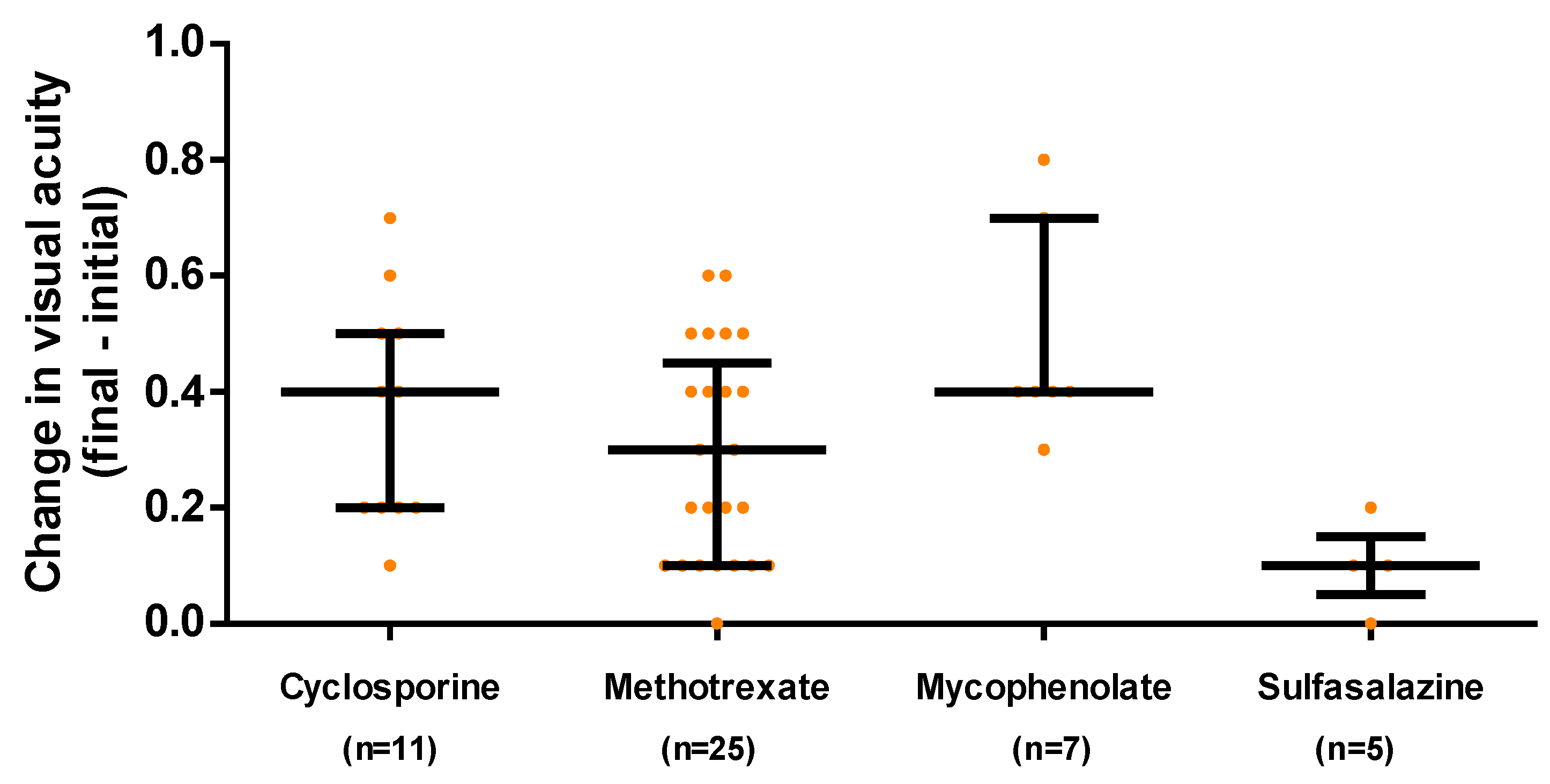
| Total N=356 |
No TTO IS/BT N = 290 (81.5%) |
With TTO IS/BT N= 66 (18.5%) |
p-valor | |
| Female Male |
180 (50.6) 176 (49.4) |
146 (50.3) 144 (49.7) |
34 (51.5) 32 (48.5) |
0.864 |
| Age (median [Q1Q3]) To diagnosis At the start of treatment Time diagnosis-initiation TTO |
42.8 [31.5, 54.0] |
42.0 [32.0, 55.0] |
38.0 [30.0, 47.0] 42.5 [34.0, 50.0] 2 [1, 4] |
0.027 Not applicable Not applicable |
| N. º outbreaks 1º outbreak 2º outbreak >= 3º outbreak |
157 (44.1) 35 (9.8) 164 (45.9) |
134 (46.2) 30 (10.3) 126 (43.4) |
23 (34.9) 5 (7.6) 38 (57.6) |
0.197 |
| Laterality Unilateral Bilateral |
271 (76.1) 85 (23.9) |
236 (81.4) 54 (18.6) |
31 (47.0) 35 (53.0) |
<0.001 |
| Anatomic Location Anterior Intermedia Posterior Panuveítis |
265 (74.4) 34 (9.6) 28 (7.9) 29 (8.2) |
233 (80.3) 22 (7.6) 18 (6.2) 17 (5.9) |
32 (48.5) 12 (18.2) 10 (15.2) 12 (18.2) |
<0.001 |
| Etiology Idiopathic AS HLA B27+ Pars planitis Associated with HLA B27 IBD AS HLA B27- Behcet Other white dots syndrome Posner Sarcoidosis Psoriatic arthritis Harada syndrome Birdshot APPC For drugs Intermedia associated MS Associated Sjögren 1ª Cogan’s syndrome Systemic lupus erythematosus TINU Undetermined |
154 (43.3) 76 (21.4) 19 (5.3) 17 (4.8) 13 (3.7) 12 (3.4) 11 (3.1) 8 (2.3) 7 (2.0) 7 (2.0) 6 (1.7) 5 (1.4) 4 (1.1) 4 (1.1) 4 (1.1) 3 (0.8) 2 (0.6) 1 (0.3) 1 (0.3) 1 (0.3) 1 (0.3) |
133 (45.9) 58 (20.0) 14 (4.8) 16 (5.5) 10 (3.5) 11 (3.8) 5 (1.7) 7 (2.4) 7 (2.4) 7 (2.4) 4 (1.4) 3 (1.0) 0 4 (1.4) 4 (1.4) 1 (0.3) 2 (0.7) 1 (0.3) 1 (0.3) 1 (0.3) 1 (0.3) |
21 (31.8) 18 (27.3) 5 (7.6) 1 (1.5) 3 (4.6) 1 (1.5) 6 (9.1) 1 (1.52) 0 0 2 (3.0) 2 (3.0) 4 (6.1) 0 0 2 (3.0) 0 0 0 0 0 |
Not applicable |
| Systemic CS treatment Orals Intravenous |
43 (12.1) 26 (7) 17 (4.8) |
19 (6.5) 14 (4.8) 5 (1.7) |
24 (36.4) 12 (18.2) 12 (18.2) |
<0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




