Submitted:
02 January 2024
Posted:
03 January 2024
You are already at the latest version
Abstract
Keywords:
1. Introduction
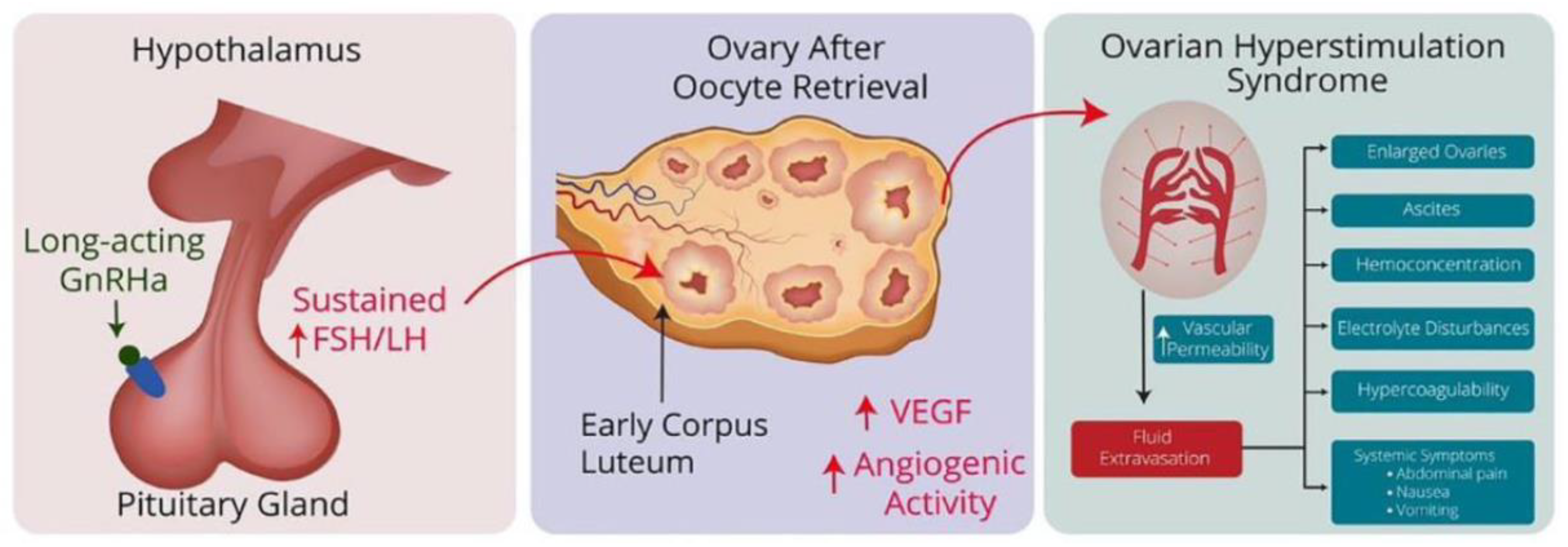
2. Pathophysiology of ovarian hyperstimulation syndrome
3. Clinical presentation of ovarian hyperstimulation syndrome
4. Interventions to reduce the risk of OHSS during COS
5. OHSS in cancer patients referred for fertility preservation
6. GnRH Antagonists for Ovarian Suppression: A Comprehensive Clinical Evaluation
7. Conclusion
References
- Chai, W.; He, H.; Li, F.; Zhang, W.; He, C. Spontaneous ovarian hyperstimulation syndrome in a nonpregnant female patient: a case report and literature review. J Int Med Res 2020, 48, 300060520952647. [Google Scholar] [CrossRef] [PubMed]
- Li, H.W.; Lee, V.C.; Lau, E.Y.; Yeung, W.S.; Ho, P.C.; Ng, E.H. Cumulative live-birth rate in women with polycystic ovary syndrome or isolated polycystic ovaries undergoing in-vitro fertilisation treatment. J Assist Reprod Genet 2014, 31, 205–211. [Google Scholar] [CrossRef]
- Nastri, C.O.; Teixeira, D.M.; Moroni, R.M.; Leitao, V.M.; Martins, W.P. Ovarian hyperstimulation syndrome: pathophysiology, staging, prediction and prevention. Ultrasound Obstet Gynecol 2015, 45, 377–393. [Google Scholar] [CrossRef] [PubMed]
- Goldfarb, S.B.; Turan, V.; Bedoschi, G.; Taylan, E.; Abdo, N.; Cigler, T.; Bang, H.; Patil, S.; Dickler, M.N.; Oktay, K.H. Impact of adjuvant chemotherapy or tamoxifen-alone on the ovarian reserve of young women with breast cancer. Breast Cancer Res Treat 2021, 185, 165–173. [Google Scholar] [CrossRef]
- Ingold, C.; Navarro, P.A.; de Oliveira, R.; Barbosa, C.P.; Bedoschi, G. Risk of ovarian hyperstimulation syndrome in women with malignancies undergoing treatment with long-acting gonadotropin-releasing hormone agonist after controlled ovarian hyperstimulation for fertility preservation: a systematic review. Ther Adv Reprod Health 2023, 17, 26334941231196545. [Google Scholar] [CrossRef]
- Ingold, C.; Bedoschi, G. Safety and efficacy concerns of long-acting GnRHa trigger for ovulation induction in oncological patients undergoing oocyte cryopreservation: a call for caution and further investigation. ESMO Open 2023, 8, 101825. [Google Scholar] [CrossRef] [PubMed]
- Timmons, D.; Montrief, T.; Koyfman, A.; Long, B. Ovarian hyperstimulation syndrome: A review for emergency clinicians. Am J Emerg Med 2019, 37, 1577–1584. [Google Scholar] [CrossRef]
- Bates, D.O.; Harper, S.J. Regulation of vascular permeability by vascular endothelial growth factors. Vascul Pharmacol 2002, 39, 225–237. [Google Scholar] [CrossRef]
- Grossman, L.C.; Michalakis, K.G.; Browne, H.; Payson, M.D.; Segars, J.H. The pathophysiology of ovarian hyperstimulation syndrome: an unrecognized compartment syndrome. Fertil Steril 2010, 94, 1392–1398. [Google Scholar] [CrossRef]
- Delvigne, A.; Rozenberg, S. Review of clinical course and treatment of ovarian hyperstimulation syndrome (OHSS). Hum Reprod Update 2003, 9, 77–96. [Google Scholar] [CrossRef]
- Gil Navarro, N.; Garcia Grau, E.; Pina Perez, S.; Ribot Luna, L. Ovarian torsion and spontaneous ovarian hyperstimulation syndrome in a twin pregnancy: A case report. Int J Surg Case Rep 2017, 34, 66–68. [Google Scholar] [CrossRef]
- Budev, M.M.; Arroliga, A.C.; Falcone, T. Ovarian hyperstimulation syndrome. Crit Care Med 2005, 33, S301–306. [Google Scholar] [CrossRef]
- Serour, G.I.; Aboulghar, M.; Mansour, R.; Sattar, M.A.; Amin, Y.; Aboulghar, H. Complications of medically assisted conception in 3,500 cycles. Fertil Steril 1998, 70, 638–642. [Google Scholar] [CrossRef]
- Mor, Y.S.; Schenker, J.G. Ovarian hyperstimulation syndrome and thrombotic events. Am J Reprod Immunol 2014, 72, 541–548. [Google Scholar] [CrossRef]
- Abramov, Y.; Elchalal, U.; Schenker, J.G. Febrile morbidity in severe and critical ovarian hyperstimulation syndrome: a multicentre study. Hum Reprod 1998, 13, 3128–3131. [Google Scholar] [CrossRef] [PubMed]
- Marek, D.; Sovova, E.; Dostal, J.; Oborna, I.; Kocianova, E.; Machac, S.; Talas, M.; Lukl, J.; Brezinova, J. Incidence of pericardial effusion in females stimulated in "in vitro fertilization" program. Echocardiography 2006, 23, 729–733. [Google Scholar] [CrossRef] [PubMed]
- Macklon, N.S.; Stouffer, R.L.; Giudice, L.C.; Fauser, B.C. The science behind 25 years of ovarian stimulation for in vitro fertilization. Endocr Rev 2006, 27, 170–207. [Google Scholar] [CrossRef] [PubMed]
- Al-Inany, H.G.; Youssef, M.A.; Ayeleke, R.O.; Brown, J.; Lam, W.S.; Broekmans, F.J. Gonadotrophin-releasing hormone antagonists for assisted reproductive technology. Cochrane Database Syst Rev 2016, 4, CD001750. [Google Scholar] [CrossRef]
- Fatemi, H.M.; Popovic-Todorovic, B.; Humaidan, P.; Kol, S.; Banker, M.; Devroey, P.; Garcia-Velasco, J.A. Severe ovarian hyperstimulation syndrome after gonadotropin-releasing hormone (GnRH) agonist trigger and "freeze-all" approach in GnRH antagonist protocol. Fertil Steril 2014, 101, 1008–1011. [Google Scholar] [CrossRef]
- Reddy, J.; Turan, V.; Bedoschi, G.; Moy, F.; Oktay, K. Triggering final oocyte maturation with gonadotropin-releasing hormone agonist (GnRHa) versus human chorionic gonadotropin (hCG) in breast cancer patients undergoing fertility preservation: an extended experience. J Assist Reprod Genet 2014, 31, 927–932. [Google Scholar] [CrossRef]
- Ferraretti, A.P.; Gianaroli, L.; Magli, C.; Fortini, D.; Selman, H.A.; Feliciani, E. Elective cryopreservation of all pronucleate embryos in women at risk of ovarian hyperstimulation syndrome: efficiency and safety. Hum Reprod 1999, 14, 1457–1460. [Google Scholar] [CrossRef] [PubMed]
- Gomez, R.; Gonzalez-Izquierdo, M.; Zimmermann, R.C.; Novella-Maestre, E.; Alonso-Muriel, I.; Sanchez-Criado, J.; Remohi, J.; Simon, C.; Pellicer, A. Low-dose dopamine agonist administration blocks vascular endothelial growth factor (VEGF)-mediated vascular hyperpermeability without altering VEGF receptor 2-dependent luteal angiogenesis in a rat ovarian hyperstimulation model. Endocrinology 2006, 147, 5400–5411. [Google Scholar] [CrossRef]
- Bedoschi, G.M.; Navarro, P.A.; Oktay, K.H. Novel insights into the pathophysiology of chemotherapy-induced damage to the ovary. Panminerva Med 2019, 61, 68–75. [Google Scholar] [CrossRef] [PubMed]
- Oktay, K.; Harvey, B.E.; Partridge, A.H.; Quinn, G.P.; Reinecke, J.; Taylor, H.S.; Wallace, W.H.; Wang, E.T.; Loren, A.W. Fertility Preservation in Patients With Cancer: ASCO Clinical Practice Guideline Update. J Clin Oncol 2018, 36, 1994–2001. [Google Scholar] [CrossRef] [PubMed]
- Lambertini, M.; Peccatori, F.A.; Demeestere, I.; Amant, F.; Wyns, C.; Stukenborg, J.B.; Paluch-Shimon, S.; Halaska, M.J.; Uzan, C.; Meissner, J.; et al. Fertility preservation and post-treatment pregnancies in post-pubertal cancer patients: ESMO Clinical Practice Guidelines(dagger). Ann Oncol 2020, 31, 1664–1678. [Google Scholar] [CrossRef] [PubMed]
- Preservation, E.G.G. o. F. F.; Anderson, R.A.; Amant, F.; Braat, D.; D'Angelo, A.; Chuva de Sousa Lopes, S.M.; Demeestere, I.; Dwek, S.; Frith, L.; Lambertini, M.; et al. ESHRE guideline: female fertility preservation. Hum Reprod Open 2020, 2020, hoaa052. [Google Scholar] [CrossRef]
- Practice Committee of the American Society for Reproductive Medicine. Electronic address, a. a. o. Fertility preservation in patients undergoing gonadotoxic therapy or gonadectomy: a committee opinion. Fertil Steril 2019, 112, 1022–1033. [Google Scholar] [CrossRef]
- Bedoschi, G.; Oktay, K. Current approach to fertility preservation by embryo cryopreservation. Fertil Steril 2013, 99, 1496–1502. [Google Scholar] [CrossRef]
- Oktay, K.; Turan, V.; Bedoschi, G.; Pacheco, F.S.; Moy, F. Fertility Preservation Success Subsequent to Concurrent Aromatase Inhibitor Treatment and Ovarian Stimulation in Women With Breast Cancer. J Clin Oncol 2015, 33, 2424–2429. [Google Scholar] [CrossRef]
- Oktay, K.; Marin, L.; Bedoschi, G.; Pacheco, F.; Sugishita, Y.; Kawahara, T.; Taylan, E.; Acosta, C.; Bang, H. Ovarian transplantation with robotic surgery and a neovascularizing human extracellular matrix scaffold: a case series in comparison to meta-analytic data. Fertil Steril 2022, 117, 181–192. [Google Scholar] [CrossRef]
- Marin, L.; Bedoschi, G.; Kawahara, T.; Oktay, K.H. History, Evolution and Current State of Ovarian Tissue Auto-Transplantation with Cryopreserved Tissue: a Successful Translational Research Journey from 1999 to 2020. Reprod Sci 2020, 27, 955–962. [Google Scholar] [CrossRef]
- Turan, V.; Bedoschi, G.; Rodriguez-Wallberg, K.; Sonmezer, M.; Pacheco, F.S.; Oktem, O.; Taylor, H.; Oktay, K. Utility of Gonadotropin-Releasing Hormone Agonists for Fertility Preservation: Lack of Biologic Basis and the Need to Prioritize Proven Methods. J Clin Oncol 2019, 37, 84–86. [Google Scholar] [CrossRef]
- Oktay, K.; Bedoschi, G. Appraising the Biological Evidence for and Against the Utility of GnRHa for Preservation of Fertility in Patients With Cancer. J Clin Oncol 2016, 34, 2563–2565. [Google Scholar] [CrossRef]
- Oktay, K.; Turan, V.; Bedoschi, G. Reply to M. Lambertini et al. J Clin Oncol 2017, 35, 807–809. [Google Scholar] [CrossRef] [PubMed]
- Oktay, K.; Taylan, E.; Rodriguez-Wallberg, K.A.; Bedoschi, G.; Turan, V.; Pacheco, F. Goserelin does not preserve ovarian function against chemotherapy-induced damage. Ann Oncol 2018, 29, 512–513. [Google Scholar] [CrossRef] [PubMed]
- Maggi, R.; Cariboni, A.M.; Marelli, M.M.; Moretti, R.M.; Andre, V.; Marzagalli, M.; Limonta, P. GnRH and GnRH receptors in the pathophysiology of the human female reproductive system. Hum Reprod Update 2016, 22, 358–381. [Google Scholar] [CrossRef]
- Roness, H.; Gavish, Z.; Cohen, Y.; Meirow, D. Ovarian follicle burnout: a universal phenomenon? Cell Cycle 2013, 12, 3245–3246. [Google Scholar] [CrossRef]
- Marin, L.; Vitagliano, A.; Capobianco, G.; Dessole, F.; Ambrosini, G.; Andrisani, A. Which is the optimal timing for starting chemoprotection with gonadotropin-releasing hormone agonists after oocyte cryopreservation? Reflections on a critical case of ovarian hyperstimulation syndrome. J Gynecol Obstet Hum Reprod 2021, 50, 101815. [Google Scholar] [CrossRef] [PubMed]
- Abdel-Rahman, O. Impact of timeliness of adjuvant chemotherapy and radiotherapy on the outcomes of breast cancer; a pooled analysis of three clinical trials. Breast 2018, 38, 175–180. [Google Scholar] [CrossRef] [PubMed]
- Wang, N.; Chen, Z.; Guo, X.; Cheng, H.; Wang, P.; Wang, T.; Wang, L.; Tash, D.; Ren, P.; Zhu, B.; et al. Sudden Death Due to Severe Ovarian Hyperstimulation Syndrome: An Autopsy-Centric Case Report. Am J Forensic Med Pathol 2021, 42, 88–91. [Google Scholar] [CrossRef]
- Padula, A.M. GnRH analogues--agonists and antagonists. Anim Reprod Sci 2005, 88, 115–126. [Google Scholar] [CrossRef] [PubMed]
- Herbst, K.L. Gonadotropin-releasing hormone antagonists. Curr Opin Pharmacol 2003, 3, 660–666. [Google Scholar] [CrossRef] [PubMed]
- Bedoschi, G.; Navarro, P.A. Oncofertility programs still suffer from insufficient resources in limited settings. J Assist Reprod Genet 2022, 39, 953–955. [Google Scholar] [CrossRef] [PubMed]
- Lainas, G.T.; Kolibianakis, E.M.; Sfontouris, I.A.; Zorzovilis, I.Z.; Petsas, G.K.; Tarlatzi, T.B.; Tarlatzis, B.C.; Lainas, T.G. Outpatient management of severe early OHSS by administration of GnRH antagonist in the luteal phase: an observational cohort study. Reprod Biol Endocrinol 2012, 10, 69. [Google Scholar] [CrossRef]
- Lainas, G.T.; Kolibianakis, E.M.; Sfontouris, I.A.; Zorzovilis, I.Z.; Petsas, G.K.; Lainas, T.G.; Tarlatzis, B.C. Serum vascular endothelial growth factor levels following luteal gonadotrophin-releasing hormone antagonist administration in women with severe early ovarian hyperstimulation syndrome. BJOG 2014, 121, 848–855. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2024 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



