Submitted:
05 October 2023
Posted:
06 October 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Statistical Analysis
3. Results
I. Clinical diagnoses, indications for surgical treatment
II. Type of thyroid surgery
III. Postoperative complications.
IV. Secondary surgeries on the thyroid gland
4. Discussion
Conclusions:
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
Abbreviations
References
- Choroby tarczycy u Polaków. Statystyki, objawy, leczenie. Available online: http://zdrowie.wprost.pl/medycyna/choroby/10398657/choroby-tarczycy-u-polakow-statystyki-objawy-leczenie.html. (accessed on 15 October 2022).
- Fortuny, J.V.; Guigard, S.; Karenovics, W.; Triponez, F. Surgery of the thyroid: recent developments and perspective. Swiss Med Wkly. 2015, 145, 14144. [Google Scholar] [CrossRef] [PubMed]
- Terris, D.J.; et al. Incisions in thyroid and parathyroid surgery. In Surgery and Parathyroid Surgery, 2nd ed.; SAUNDERS: Philadelphia, USA, 2013; pp. 403–406. [Google Scholar]
- Halsted, W.S. The operative story of goitre. The author’s operation. J Am Med Assoc. 1920, 74, 693–694. [Google Scholar]
- Mitrecic, M.Z.; Kaplan, E.L.; Gaz, R.D. Mitrecic, M.Z.; Kaplan, E.L.; Gaz, R.D., et al. History of thyroid and parathyroid surgery. In:. Surgery of the thyroid and parathyroid glands.; SAUNDERS: Philadelphia, USA, 2003; pp. 3–14.
- Hannan, S.A. The magnificent seven: a history of modern thyroid surgery. Int J Surg. 2006, 4, 187–191. [Google Scholar] [CrossRef] [PubMed]
- Patel, N.; Scott-Coombes, D. Impact of surgical volume and surgical outcome assessing registers on the quality of thyroid surgery. Best Pract Res Clin Endocrinol Metab. 2019, 33. [Google Scholar] [CrossRef] [PubMed]
- Shedd, D.P.; Burget, G.C. Identification of the recurrent laryngeal nerve. Arch Surg. 1966, 92, 861–864. [Google Scholar] [CrossRef] [PubMed]
- Randolph, G.W.; Dralle, H.; Abdullah, H.; Barczynski, M.; Bellantone, R.; Brauckhoff, M.; Carnaille, B.; Cherenko, S.; Chiang, F.Y.; Dionigi, G.; et al. Electrophysiologic recurrent laryngeal nerve monitoring during thyroid and parathyroid surgery: international standards guideline statement. Laryngoscope 2011, 121. [Google Scholar] [CrossRef] [PubMed]
- Barczyński, M.; Randolph, G.W.; Cernea, C.R.; Dralle, H.; Dionigi, G.; Alesina, P.F.; Mihai, R.; Finck, C.; Lombardi, D.; Hartl, D.M.; et al. External branch of the superior laryngeal nerve monitoring during thyroid and parathyroid surgery: International Neural Monitoring Study Group Standards Guideline Statement. Laryngoscope 2013, 123. [Google Scholar] [CrossRef]
- Orloff, L.A.; Wiseman, S.M.; Bernet, V.J.; Fahey, T.J., 3rd; Shaha, A.R.; Shindo, M.L.; Snyder, S.K.; Stack, B.C., Jr.; Sunwoo, J.B.; Wang, M.B. American Thyroid Association Statement on Postoperative Hypoparathyroidism: Diagnosis, Prevention, and Management in Adults. Thyroid 2018, 28, 830–841. [Google Scholar] [CrossRef] [PubMed]
- Barbieri, D.; Indelicato, P.; Vinciguerra, A.; Salerno, E.; Battista, R.A.; Di Marco, F.; Giordano, L.; Luce, F.L.; Bondi, S.; Trimarchi, M.; Bussi, M. The impact of near-infrared autofluorescence on postoperative hypoparathyroidism during total thyroidectomy: a case-control study. Endocrine 2023, 79, 392–399. [Google Scholar] [CrossRef] [PubMed]
- de Vries, L.H.; Aykan, D.; Lodewijk, L.; Damen, J.A.A.; Borel Rinkes, I.H.M.; Vriens, M.R. Outcomes of Minimally Invasive Thyroid Surgery - A Systematic Review and Meta-Analysis. Front Endocrinol (Lausanne). 2021, 12, 719397. [Google Scholar] [CrossRef]
- Lee, C.R.; Chung, W.Y. ; Robotic surgery for thyroid disease. Minerva Chir. 2015, 70, 331–339. [Google Scholar] [CrossRef] [PubMed]
- Anuwong, A.; Ketwong, K.; Jitpratoom, P.; Sasanakietkul, T.; Duh, Q.Y. Safety and Outcomes of the Transoral Endoscopic Thyroidectomy Vestibular Approach. JAMA Surg. 2018, 153, 21–27. [Google Scholar] [CrossRef]
- Wojciechowska, U.; Didkowska, J. Zachorowania i zgony na nowotwory złośliwe w Polsce. Krajowy Rejestr Nowotworów, Narodowy Instytut Onkologii im. Marii Skłodowskiej-Curie – Państwowy Instytut Badawczy. Avaliable online: http://onkologia.org.pl/raporty (accessed on 23.12.2021).
- Li, M.; Dal Maso, L.; Vaccarella, S. Global trends in thyroid cancer incidence and the impact of overdiagnosis. Lancet Diabetes Endocrinol. 2020, 8, 468–470. [Google Scholar] [CrossRef] [PubMed]
- Vaccarella, S.; Franceschi, S.; Bray, F.; Wild, C.P.; Plummer, M.; Dal Maso, L. Worldwide Thyroid-Cancer Epidemic? The Increasing Impact of Overdiagnosis. N Engl J Med. 2016, 375, 614–617. [Google Scholar] [CrossRef] [PubMed]
- Kahaly, G.J. Management of Graves Thyroidal and Extrathyroidal Disease: An Update. J Clin Endocrinol Metab. 2020, 105, 3704–3720. [Google Scholar] [CrossRef]
- Patel, K.N.; Yip, L.; Lubitz, C.C.; Grubbs, E.G.; Miller, B.S.; Shen, W.; Angelos, P.; Chen, H.; Doherty, G.M.; Fahey, T.J., 3rd; et al. The American Association of Endocrine Surgeons Guidelines for the Definitive Surgical Management of Thyroid Disease in Adults. Ann Surg. 2020, 271, e21–e93. [Google Scholar] [CrossRef] [PubMed]
- Papini, E.; Monpeyssen, H.; Frasoldati, A.; Hegedüs, L. 2020 European Thyroid Association Clinical Practice Guideline for the Use of Image-Guided Ablation in Benign Thyroid Nodules. Eur Thyroid J. 2020, 9, 72–185. [Google Scholar] [CrossRef] [PubMed]
- Cherenfant, J.; Gage, M.; Mangold, K.; Du, H.; Moo-Young, T.; Winchester, D.J.; Prinz, R.A. Trends in thyroid surgery in Illinois. Surgery 2013, 154, 1016–1023. [Google Scholar] [CrossRef] [PubMed]
- Al-Qurayshi, Z.; Robins, R.; Hauch, A.; Randolph, G.W.; Kandil, E. Association of Surgeon Volume With Outcomes and Cost Savings Following Thyroidectomy: A National Forecast. JAMA Otolaryngol Head Neck Surg. 2016, 142, 32–39. [Google Scholar] [CrossRef]
- Gourin, C.G.; Tufano, R.P.; Forastiere, A.A.; Koch, W.M.; Pawlik, T.M.; Bristow, R.E. Volume-based trends in thyroid surgery. Arch Otolaryngol Head Neck Surg. 2010, 136, 1191–1198. [Google Scholar] [CrossRef] [PubMed]
- van Gerwen, M.; Alsen, M.; Alpert, N.; Sinclair, C.; Taioli, E. Trends for In- and Outpatient Thyroid Cancer Surgery in Older Adults in New York State, 2007-2017. J Surg Res. 2022, 273, 64–70. [Google Scholar] [CrossRef] [PubMed]
- Chandrasekhar, S.S.; Randolph, G.W.; Seidman, M.D.; Rosenfeld, R.M.; Angelos, P.; Barkmeier-Kraemer, J.; Benninger, M.S.; Blumin, J.H.; Dennis, G.; Hanks, J.; et al. Clinical Practice Guideline: improving voice outcomes after thyroid surgery. Otolaryngology–Head and Neck Surgery 2013, 148, 1–37. [Google Scholar] [CrossRef] [PubMed]
- Jeannon, J.P.; Orabi, A.A.; Bruch, G.A.; Abdalsalam, H.A.; Simo, R. Diagnosis of recurrent laryngeal nerve palsy after thyroidectomy: A systematic review. International Journal of Clinical Practice 2009, 63, 624–629. [Google Scholar] [CrossRef]
- Główny Urząd Statystyczny. Stan zdrowia ludności Polski w 2019 r. Available online: http://stat.gov.pl/obszary-tematyczne/zdrowie/zdrowie/stan-zdrowia-ludnosci-polski-w-2019-r-,26,1.html. (accessed on 12 December 2021).
- Miranda-Filho, A.; Lortet-Tieulent, J.; Bray, F.; Cao, B.; Franceschi, S.; Vaccarella, S.; Dal Maso, L. Thyroid cancer incidence trends by histology in 25 countries: a population-based study. Lancet Diabetes Endocrinol. 2021, 9, 225–234. [Google Scholar] [CrossRef] [PubMed]
- Roman, B.R.; Morris, L.G.; Davies, L. The thyroid cancer epidemic, 2017 perspective. Curr Opin Endocrinol Diabetes Obes. 2017, 24, 332–336. [Google Scholar] [CrossRef] [PubMed]
- Seib, C.D.; Sosa, J.A. Evolving Understanding of the Epidemiology of Thyroid Cancer. Endocrinol Metab Clin North Am. 2019, 48, 23–35. [Google Scholar] [CrossRef] [PubMed]
- Zaridze, D.; Maximovitch, D.; Smans, M.; Stilidi, I. Thyroid cancer overdiagnosis revisited. Cancer Epidemiol. 2021, 74, 102014. [Google Scholar] [CrossRef] [PubMed]
- Subekti, I.; Pramono, L.A. Current Diagnosis and Management of Graves' Disease. Acta Med Indones. 2018, 50, 177–182. [Google Scholar] [PubMed]
- Wiersinga, W.M.; Poppe, K.G.; Effraimidis, G. Hyperthyroidism: aetiology, pathogenesis, diagnosis, management, complications, and prognosis. Lancet Diabetes Endocrinol. 2023, 11, 282–298. [Google Scholar] [CrossRef] [PubMed]
- Gan, T.; Randle, R.W. The Role of Surgery in Autoimmune Conditions of the Thyroid. Surg Clin North Am. 2019, 99, 633–648. [Google Scholar] [CrossRef] [PubMed]
- Inversini, D.; Morlacchi, A.; Melita, G.; Del Ferraro, S. , Boeri, C.; Portinari, M.; Cancellieri, A.; Frattini, F.; Rizzo, A.G.; Dionigi, G. Thyroidectomy in elderly patients aged ≥70 years. Gland Surg. 2017, 6, 587–590. [Google Scholar] [CrossRef] [PubMed]
- Canu, G.L.; Medas, F.; Cappellacci, F.; Podda, M.G.; Romano, G.; Erdas, E.; Calò, P.G. Can thyroidectomy be considered safe in obese patients? A retrospective cohort study. BMC Surg. 2020, 20, 275. [Google Scholar] [CrossRef] [PubMed]
- Jatzko, G.R.; Lisborg, P.H.; Muller, M.G.; Vette, V.M. Recurrent nerve palsy after thyroid operations-principal nerve identification and a literature review. Surgery 1994, 115, 139–144. [Google Scholar] [PubMed]
- Colak, T.; Akca, T.; Kanik, A.; Yapici, D.; Aydin, S. Total versus subtotal thyroidectomy for the management of benign multinodular goiter in an endemic region. ANZ J Surg. 2004, 74, 974–978. [Google Scholar] [CrossRef] [PubMed]
- Robert, J.; Mariéthoz, S.; Pache, J.C.; Bertin, D.; Caulfield, A.; Murith, N.; Peytremann, A.; Goumaz, M.; Garcia, B.; Martin-Du Pan, R.; et al. Short- and long-term results of total vs subtotal thyroidectomies in the surgical treatment of Graves' disease. Swiss Surg. 2001, 7, 20–24. [Google Scholar] [CrossRef] [PubMed]
- Tezelman, S.; Borucu, I.; Senyurek Giles, Y.; Tunca, F.; Terzioglu, T. The change in surgical practice from subtotal to near-total or total thyroidectomy in the treatment of patients with benign multinodular goiter. World J Surg. 2009, 33, 400–405. [Google Scholar] [CrossRef] [PubMed]
- Wojtczak, B.; Kaliszewski, K.; Sutkowski, K.; Głód, M.; Barczyński, M. The learning curve for intraoperative neuromonitoring of the recurrent laryngeal nerve in thyroid surgery. Langenbecks Arch Surg. 2017, 402, 701–708. [Google Scholar] [CrossRef] [PubMed]
- Wojtczak, B.; Kaliszewski, K.; Sutkowski, K.; Głód, M.; Barczyński, M. Evaluating the introduction of intraoperative neuromonitoring of the recurrent laryngeal nerve in thyroid and parathyroid surgery. Arch Med Sci. 2018, 14, 321–328. [Google Scholar] [CrossRef]
- Wojtczak, B.; Kaliszewski, K.; Sutkowski, K.; Bolanowski, M.; Barczyński, M. A functional assessment of anatomical variants of the recurrent laryngeal nerve during thyroidectomies using neuromonitoring. Endocrine 2018, 59, 82–89. [Google Scholar] [CrossRef]
- Edafe, O.; Cochrane, E.; Balasubramanian, S.P. Reoperation for Bleeding After Thyroid and Parathyroid Surgery: Incidence, Risk Factors, Prevention, and Management. World J Surg. 2020, 44, 1156–1162. [Google Scholar] [CrossRef] [PubMed]
- Miccoli, P.; Frustaci, G.; Fosso, A.; Miccoli, M.; Materazzi, G. Surgery for recurrent goiter: complication rate and role of the thyroid-stimulating hormone-suppressive therapy after the first operation. Langenbecks Arch Surg. 2015, 400, 253–258. [Google Scholar] [CrossRef] [PubMed]
- Wojtczak, B.; Barczyński, M. Intermittent neural monitoring of the recurrent laryngeal nerve in surgery for recurrent goiter. Gland Surg. 2016, 5, 481–489. [Google Scholar] [CrossRef] [PubMed]
- Głód, M.; Marciniak, D.; Kaliszewski, K.; Sutkowski, K.; Rudnicki, J.; Bolanowski, M.; Wojtczak, B. Analysis of Risk Factors for Phonation Disorders after Thyroid Surgery. Biomedicines 2022, 10, 2280. [Google Scholar] [CrossRef] [PubMed]
- Chou, R.; Dana, T.; Haymart, M.; Leung, A.M.; Tufano, R.P.; Sosa, J.A.; Ringel, M.D. Active Surveillance Versus Thyroid Surgery for Differentiated Thyroid Cancer: A Systematic Review. Thyroid 2022, 32, 351–367. [Google Scholar] [CrossRef] [PubMed]
- Tufano, R.P.; Pace-Asciak, P.; Russell, J.O.; Suárez, C.; Randolph, G.W.; López, F.; Shaha, A.R.; Mäkitie, A.; Rodrigo, J.P.; Kowalski, L.P.; et al. Update of Radiofrequency Ablation for Treating Benign and Malignant Thyroid Nodules. The Future Is Now. Front Endocrinol (Lausanne). 2021, 12, 698689. [Google Scholar] [CrossRef] [PubMed]
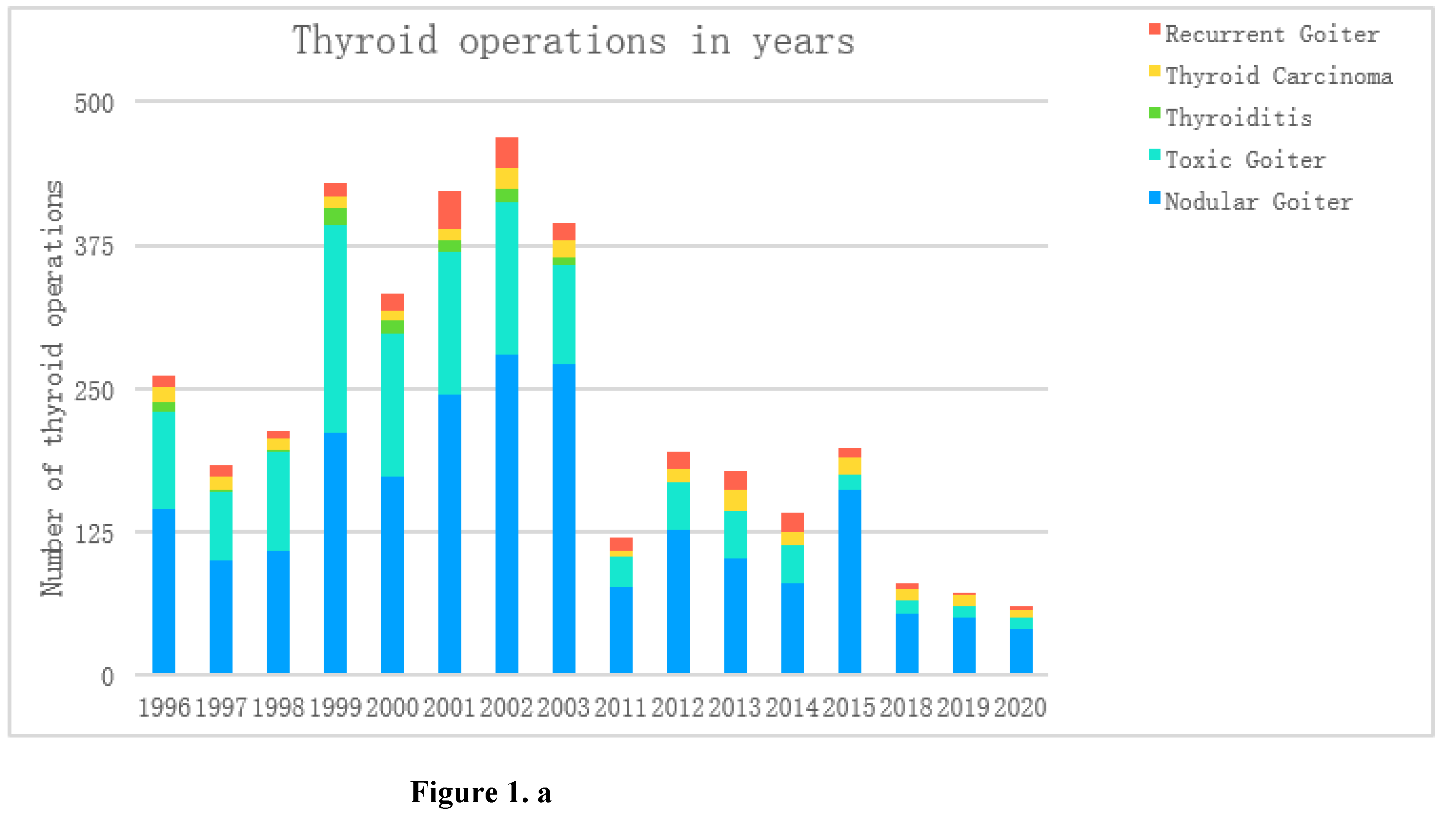
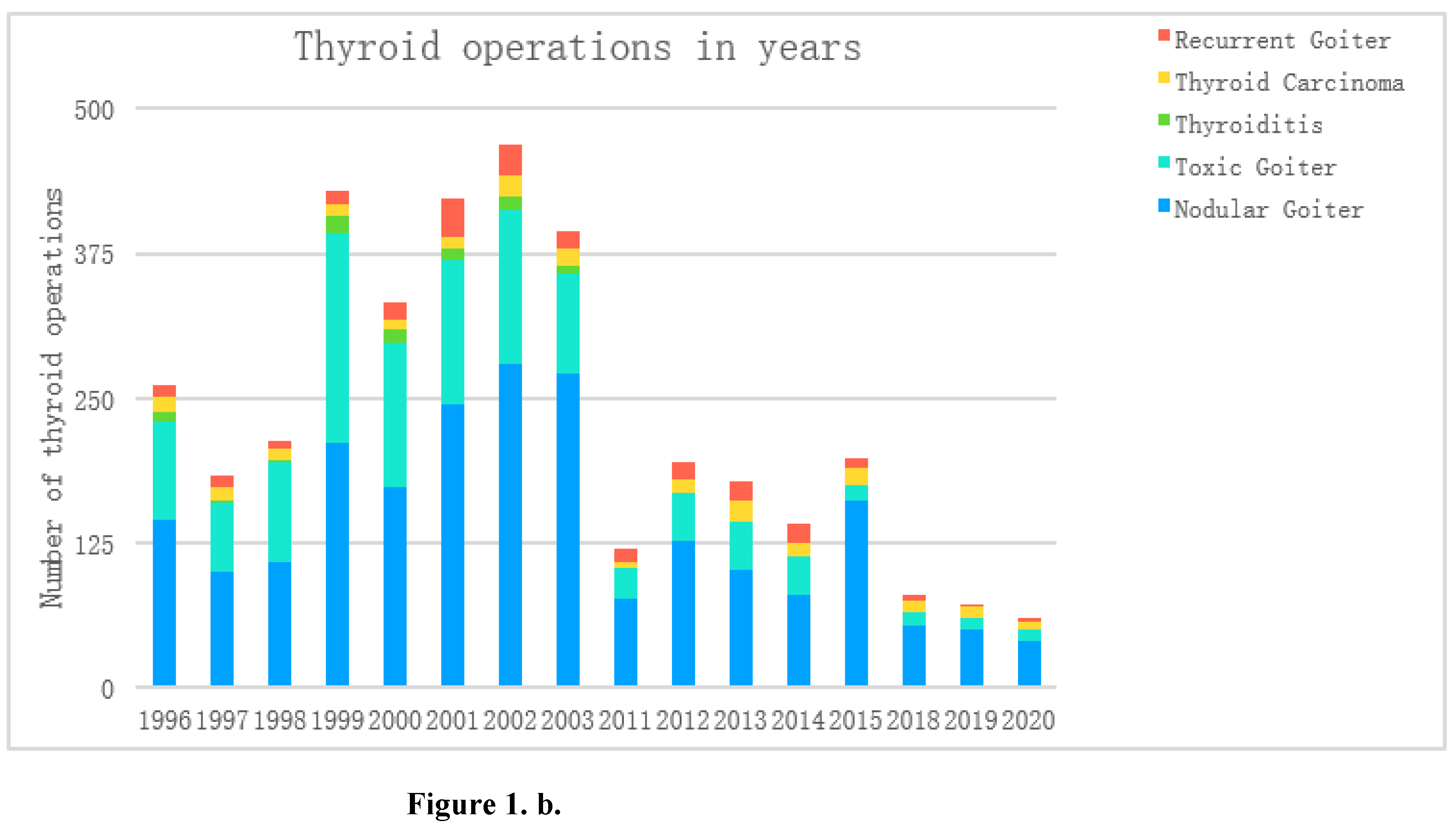
| Thyroid surgery, years | I Period (1996-2003) |
II Period (2011-2015, 2018-2020) |
p level |
|---|---|---|---|
| Number of patients, n (%) | 2707 (100%) | 1041 (100%) | - |
| Number of RLN at risk of injury (RLN/at risk) | 5414 (100%) | 1871 (100%) | - |
| Age, mean ± standard deviation Minimum / maximum age [years]. |
13.65±54.38 15/75 |
14.54±53.2 16/86 |
p>0.05 |
|
2 334 (86.22%) 373 (13.78%) |
836 (80.3%) 205 (19.7%) |
p<0.00001 |
|
2451 (90.5%):256 (9.5%)9:1 | 856 (82.2%):185 (17.8%) 5:1 |
p<0.00001 |
|
3.0±24.01 | 4.2±27.07 | p>0.05 |
| Thyroid volume (V), mean ± standard deviation V minimum / maximum [ml] |
26.6±51.26 5/210 |
37.5±43.35 1/650 |
p>0.05 |
| Number of patients, n | 2702 | 100% | 1041 | 100% | Statistic | |
| I group(1996-2003) | II (2011-2015, 2018-2020) | chi2, (df=1) | p level | |||
| Primary surgery, n (%) | 2575 | 95.12% | 962 | 92.41% | 10.41 | p=0.00130 |
| Secondary surgery, n (%) | 132 | 4.88% | 79 | 7.59% | 10.41 | p=0.00130 |
| Nodular goiter | 1625 | 60.03% | 741 | 71.18% | 40.17 | p<0.00001 |
| Toxic nodular goiter | 640 | 23.64% | 145 | 13.93% | 42.84 | p<0.00001 |
| Graves disease | 273 | 10.08% | 50 | 4.80% | 26.64 | p<0.00001 |
| Inflammatory goitre | 68 | 2.51% | 0 | 0 % | 26.63 | p<0.00001 |
| Carcinoma | 101 | 3.73% | 105 | 10.09% | 58.47 | p<0.00001 |
| Papillary thyroid cancer | 61 | 2.25% | 92 | 8.84% | 83.25 | p<0.00001 |
| Follicular thyroid cancer | 17 | 0.63% | 8 | 0.77% | 0.22 | p=0.63600 |
| Medullary thyroid cancer | 7 | 0.26% | 2 | 0.19% | 0.14 | p=0.70960 |
| Anaplastic thyroid cancer | 6 | 0.22% | 2 | 0.19% | 0.03 | p=0.86080 |
| Hurtle cell carcinoma | 4 | 0.15% | 1 | 0.10% | 0.15 | p=0.69770 |
| Thyroid lymphoma | 2 | 0.07% | 0 | 0 % | 0.77 | p=0.38040 |
| Metastases in thyroid | 4 | 0.15% | 0 | 0 % | 1.54 | p=0.21460 |
| Retrosternal goiter, n (%) | 736 | 27.19 % | 238 | 22.86% | 7.32 | p=0.00680 |
| Tracheal displacement / constriction, n (%) | 803 | 29.66% | 400 | 38.42% | 26.48 | p<0.00001 |
| Years | Total number of patients n, (%) |
Nodular Goiter n, (%) |
Toxic Goiter n, (%) |
Thyroiditisn, (%) |
Thyroid Carcinoma n, (%) |
Recurrent Goiter n, (%) |
||||||
| 1996 | 261 | 100.0 | 144 | 55.2 | 85 | 32.6 | 8 | 3.1 | 14 | 5.4 | 10 | 3.8 |
| 1997 | 183 | 100.0 | 100 | 54.6 | 59 | 32.2 | 2 | 1.1 | 11 | 6.0 | 11 | 6.0 |
| 1998 | 213 | 100.0 | 108 | 50.7 | 87 | 40.8 | 1 | 0.5 | 10 | 4.7 | 7 | 3.3 |
| 1999 | 430 | 100.0 | 211 | 49.1 | 181 | 42.1 | 15 | 3.5 | 11 | 2.6 | 12 | 2.8 |
| 2000 | 333 | 100.0 | 173 | 52.0 | 125 | 37.5 | 11 | 3.3 | 8 | 2.4 | 16 | 4.8 |
| 2001 | 423 | 100.0 | 245 | 57.9 | 125 | 29.6 | 9 | 2.1 | 10 | 2.4 | 34 | 8.0 |
| 2002 | 469 | 100.0 | 280 | 59.7 | 133 | 28.4 | 12 | 2.6 | 18 | 3.8 | 26 | 5.5 |
| 2003 | 395 | 100.0 | 271 | 68.6 | 86 | 21.8 | 7 | 1.8 | 15 | 3.8 | 16 | 4.1 |
| 2011 | 119 | 100.0 | 76 | 63.9 | 27 | 22.7 | 0 | 0.0 | 5 | 4.2 | 11 | 9.2 |
| 2012 | 194 | 100.0 | 127 | 65.5 | 40 | 20.6 | 0 | 0.0 | 12 | 6.2 | 15 | 7.7 |
| 2013 | 178 | 100.0 | 102 | 57.3 | 41 | 23.0 | 0 | 0.0 | 18 | 10.1 | 17 | 9.6 |
| 2014 | 141 | 100.0 | 79 | 56.0 | 34 | 24.1 | 0 | 0.0 | 11 | 7.8 | 17 | 12.1 |
| 2015 | 198 | 100.0 | 161 | 81.3 | 14 | 7.1 | 0 | 0.0 | 14 | 7.1 | 9 | 4.5 |
| 2018 | 79 | 100.0 | 53 | 67.1 | 12 | 15.2 | 0 | 0.0 | 10 | 12.7 | 4 | 5.1 |
| 2019 | 72 | 100.0 | 50 | 69.4 | 10 | 13.9 | 0 | 0.0 | 9 | 12.5 | 3 | 4.2 |
| 2020 | 60 | 100.0 | 39 | 65.0 | 10 | 16.7 | 0 | 0.0 | 8 | 13.3 | 3 | 5.0 |
| Number of patients, n | 2702 | 100% | 1041 | 100% | Statistic | |
| I (1996-2003) | II (2011-2015, 2018-2020) | chi2, (df=1) | p level | |||
| Total thyroidectomy | 46 | 1.70 % | 737 | 70.80% | 2172.12 | p<0.00001 |
| Excision of a thyroid lobe with the isthmus | 0 | 0.00% | 211 | 20.27% | 581.41 | p<0.00001 |
| Wedge shaped resection | 12 | 0.44% | 0 | - | 4.63 | p=0.03140 |
| Dunhill procedure | 214 | 7.91% | 47 | 4.51% | 13.34 | p=0.00030 |
| Subtotal bilateral thyroidectomy | 2429 | 89.73% | 46 | 4.42% | 2439.78 | p<0.00001 |
| Cytoreduction of the thyroid gland | 6 | 0.22% | 0 | - | 2.31 | p=0.12850 |
| Complications | I (1996-2003) |
II (2011-2015, 2018-2020) |
Statistic | ||||
| Total number, n |
% | Totalnumber, n | % | chi2, df=1 | p level | ||
|
Thyroid operation Primary Secondary |
2707 2575 132 |
100% | 1041 962 79 |
100% | |||
| Bleeding Primary operation Secondary operation |
25 25 0 |
0.92% 0.97% 0% |
9 8 1 |
0.86% 0.83% 1.27% |
0.03 0.15 1.68 |
p=0.8646 p=0.7014 p=0.1951 |
|
| Hypoparathyroidism/ Clinical Primary operation Secondary operation |
131 120 11 |
4.84% 4.66% 8.33% |
93 81 12 |
8.93% 8.42% 15.19% |
22.43 18.47 2.39 |
p<0.00001 p<0.00001 p=0.1219 |
|
| Hypoparathyroidism/ Biochemical Primary operation Secondar operationy |
0 0 0 |
0 0 0 |
133 110 23 |
12.78% 11.43% 29.11% |
358.58 303.89 43.13 |
p<0.00001 p<0.00001 p<0.00001 |
|
| Unilateral vocal fold paresis |
Total Primary operation Secondary operation |
224 204 20 |
8.27% 7.92% 15.15 |
68 60 8 |
6.53% 6.24% 10.13% |
3.18 2.88 1.08 |
p=0.0746 p=0.0897 p=0.2978 |
| Transient: Primary operation Secondary operation |
21 16 5 |
0.78% 0.62% 3.79 |
22 20 2 |
2.11% 2.08% 2.53% |
11.86 14.77 0.24 |
p=0.0006 p=0.0001 p=0.6219 |
|
| Permanent Primary operation Secondary operation |
203 188 15 |
7.5% 7.3% 11.36% |
46 40 6 |
4.42% 4.16% 7.59% |
11.5 11.47 0.78 |
p=0.0007 p=0.0007 p=0.3762 |
|
| Bilateral vocal Foldparesis |
Total Primary operation Secondary operation |
28 23 5 |
1.03% 0.89% 3.79% |
7 5 2 |
0.67% 0.52% 2.53% |
1.06 1.24 0.24 |
p=0.3022 p=0.2648 p=0.6219 |
| Transient Primary operation Secondary operation |
1 0 1 |
0.04% 0% 0.76% |
3 1 2 |
0.29% 0.10% 2.53% |
4.45 2.681.11 |
p=0.0349 p=0.1018 p=0.2921 |
|
| Permanent Primary operation Secondary operation |
27 23 4 |
1.0% 0.89% 3.03% |
4 4 0 |
0.38% 0.42% 0 |
3.45 2.11 2.44 |
p=0.0634 p=0.1466 p=0.1183 |
|
| RLN at risk, n (100%) | 5414 5150 264 |
100% | 1871 1736 135 |
100% | |||
| RLN injury |
Total Primary operation Secondary operation |
280 250 30 |
5.17% 4.85% 11.36% |
82 72 10 |
4.38% 4.15% 7.41% |
1.81 1.46 1.55 |
p=0.1785 p=0.2277 p=0.2132 |
| TransientPrimary operation Secondary operation |
22 16 6 |
0.41% 0.32% 2.27% |
25 23 2 |
1.34% 1.32% 1.48% |
18.75 23.71 0.28 |
p<0.00001 p<0.00001 p=0.5937 |
|
| Permanent Primary operation Secondary operation |
258 234 24 |
4.77% 4.54% 9.09% |
57 49 8 |
3.05% 2.82% 5.93% |
9.93 9.76 1.21 |
p=0.0016 p=0.0018 p=0.2708 |
|
| Secondary thyroid surgery: | ||||
|
I (1996-2003) |
II (2011-2015,2018-2020) | Statistic | ||
|
Total Number of patients, n (%) |
132 (4.88%) |
79 (7.59%) |
chi2, df=1 10.41 |
p level p=0.0013 |
| Diagnosis: | ||||
| Nodular goiterToxic GoiterThyroiditisCancer | 93 (70.45%) 32 (24.24%) 3 (2.27%) 4 (3.03%) |
54 (68.35%) 7 (8.86%) (-) 18 (22.78%) |
0.10 7.76 1.82 20.65 |
p=0.7481 p=0.0053 p=0.1772 p<0.00001 |
| Thyroid operation: | ||||
| Subtotal bilateral thyroidectomy | 104 (78.78%) | 5 (6.32%) | 103.91 | p<0.00001 |
| Dunhill procedure | 14 (10.6%) | 2 (2.53%) | 4.6 | p=0.0320 |
| Total thyroidectomy | 14 (10.6%) | 44 (55.7%) | 50.41 | p<0.00001 |
| Excision of a thyroid lobe with the isthmus | - | 28 (35.44%) | - | - |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




