Submitted:
22 August 2023
Posted:
23 August 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Study Participants
2.2. Recruitment
2.3. Data Collection
2.4. Measures
2.4.1. Demographic survey
2.4.2. Functional Ambulation Measure
2.4.3. Life Satisfaction Questionnaire – 11
2.4.4. Spinal Cord Independence Measure – III
2.4.5. 12- Item Short-Form Survey
2.4.6. Semi-Structured Interviews
2.5. Data analysis
2.5.1. Quantitative
2.5.2. Qualitative
3. Results
3.1. Quantitative
3.2. Qualitative
3.2.1. Low Quality of Life (N= 5)
3.2.2. Moderate Quality of Life (N= 9)
3.2.3. High Quality of Life (N=10)
4. Discussion
4.1. Contributors to Low Quality of Life
4.2. Barriers to Quality of Life among Those with Low and Moderate Quality of Life
4.3. Facilitators to Quality of Life among Those with Moderate and High Quality of Life
4.4. Facilitators to High Quality of Life
5. Limitations and Future Directions
6. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
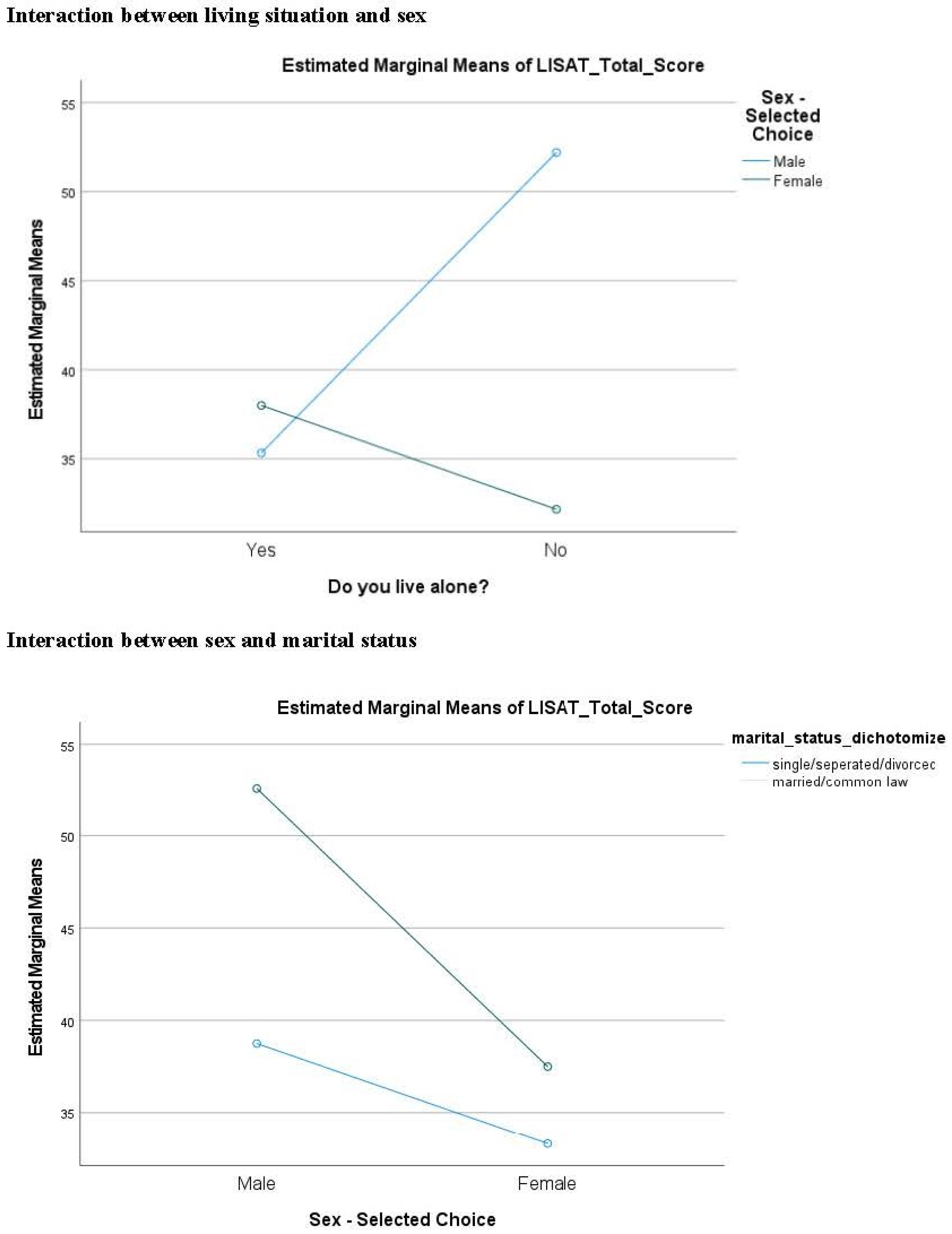
Appendix A
References
- Noonan, V.K.; Fingas, M.; Farry, A.; Baxter, D.; Singh, A.; Fehlings, M.G. , et al. Incidence and prevalence of spinal cord injury in Canada: a national perspective. Neuroepidemiology. 2012, 38, 219–226. [Google Scholar] [CrossRef]
- Rick Hansen SCI Registry Community Report [Internet]. Vancouver: Praxis Spinal Cord Institute. c2017 - [Cited 2023 Feb 27]. Available from: https://praxisinstitute.org/wpcontent/uploads/2019/10/RHSCIR_CommunityReport_2017.pdf/RHSCIR_CommunityReport_2017.
- Noreau, L.; Noonan, V.K.; Cobb, J.; Leblond, J.; Dumont, F.S. Spinal cord injury community survey: a national, comprehensive study to portray the lives of Canadians with spinal cord injury. Top Spinal Cord Inj Rehabil. 2014, 20, 249–264. [Google Scholar] [CrossRef]
- Rick Hansen Spinal Cord Injury Registry - A look at traumatic spinal cord injury in Canada in 2019. [Internet]. Vancouver : Praxis Spinal Cord Institute. c2021 [cited 2023 Feb 27]. Available from: https://praxisinstitute.org/wpcontent/uploads/2021/02/RHSCIR-2019-Report_WEB.pdf.
- Brotherton, S.S.; Krause, J.S.; Nietert, P.J. Falls in individuals with incomplete spinal cord injury. Spinal Cord. 2007, 45, 37–40. [Google Scholar] [CrossRef]
- Nijendijk JHB, Post MWM, Asbeck van FWA. Epidemiology of traumatic spinal cord injuries in the Netherlands in 2010. Spinal Cord. 2014, 52, 258–263. [CrossRef]
- Scivoletto, G.; Tamburella, F.; Laurenza, L.; Torre, M.; Molinari, M. Who is going to walk? A review of the factors influencing walking recovery after spinal cord injury. Front Hum Neurosci. 2014, 8, 41. [Google Scholar] [CrossRef]
- DiPiro, N.D.; Saunders, L.L.; Brotherton, S.; Kraft, S.; Krause, J.S. Pain and fatigue as mediators of the relationship between mobility aid usage and depressive symptomatology in ambulatory individuals with SCI. Spinal Cord. 2014, 52, 316–321. [Google Scholar] [CrossRef] [PubMed]
- Freixes, O.; Rivas, M.E.; Agrati PEBochkezanian, V.; Waldman, S.V.; Olmos, L.E. Fatigue level in spinal cord injury AIS D community ambulatory subjects. Spinal Cord. 2012, 50, 422–425. [Google Scholar] [CrossRef]
- Ginis KAM, Papathomas A, Perrier MJ, Smith B; SHAPE-SCI Research Group. Psychosocial factors associated with physical activity in ambulatory and manual wheelchair users with spinal cord injury: a mixed-methods study. Disabil Rehabil. 2017, 39(2), 187–192. [CrossRef]
- Jannings, W.; Pryor, J. The experiences and needs of persons with spinal cord injury who can walk. Disabil Rehabil. 2012, 34, 1820–1826. [Google Scholar] [CrossRef]
- Anderson, C.J.; Vogel, L.C.; Chlan, K.M.; Betz, R.R.; McDonald, C.M. Depression in adults who sustained spinal cord injuries as children or adolescents. J Spinal Cord Med. 2007, 30(Suppl 1), S76–S82. [Google Scholar] [CrossRef]
- Riordan, A.; Kelly, E.H.; Klaas, S.J.; Vogel, L.C. Psychosocial outcomes among youth with spinal cord injury by neurological impairment. J Spinal Cord Med. 2015, 38, 76–83. [Google Scholar] [CrossRef]
- Whiteneck, G.G. The 44th annual John Stanley Coulter Lecture. Measuring what matters: key rehabilitation outcomes. Arch Phys Med Rehabil. 1994, 75, 1073–1076. [Google Scholar] [CrossRef]
- Ginis KAM, Latimer AE, Arbour-Nicitopoulos KP, Buchholz AC, Bray SR, Craven BC, et al. Leisure time physical activity in a population-based sample of people with spinal cord injury part I: demographic and injury-related correlates. Arch Phys Med Rehabil. 2010, 91, 722–728. [CrossRef]
- Sakakibara BM, Hitzig SL, Miller WC, Eng JJ; SCIRE Research Team. An evidence-based review on the influence of aging with a spinal cord injury on subjective quality of life. Spinal Cord. 2012, 50, 570–578. [CrossRef]
- Tomasone, J.R.; Wesch, N.N.; Ginis, K.A.M.; Noreau, L. Spinal cord injury, physical activity, and quality of life: a systematic review. Kinesiol Rev. 2013, 2, 113–129. [Google Scholar] [CrossRef]
- Leduc, B.E.; Lepage, Y. Health-related quality of life after spinal cord injury. Disabil Rehabil. 2002, 24, 196–202. [Google Scholar] [CrossRef] [PubMed]
- Putzke, J.D.; Elliott, T.R.; Richards, J.S. Marital status and adjustment one year post spinal cord injury. J Clin Psychol Med Settings. 2001, 8, 101–107. [Google Scholar] [CrossRef]
- Kulik A, Neyaskina Y, Frizen M, Shiryaeva O; Surikova Y. Unique nature of the quality of life in the context of extreme climatic, geographical and specific socio-cultural living conditions. Int J Environ Sci Educ. 2016, 11, 6581–6591.
- Lannem, A.M.; Sorensen, M.; Froslie, K.F.; Hjeltnes, N. Incomplete spinal cord injury, exercise and life satisfaction. Spinal Cord. 2009, 47, 295–300. [Google Scholar] [CrossRef]
- Jorgensen, S.; Hedgren, L.; Sundelin, A.; Lexell, J. Global and domain-specific life satisfaction among older adults with long-term spinal cord injury. J Spinal Cord Med. 2021, 44, 322–330. [Google Scholar] [CrossRef]
- Ames H, Wilson C, Barnett SD, Njoh E, Ottomanelli L. Does functional motor incomplete (AIS D) spinal cord injury confer unanticipated challenges? Rehabil Psychol. 2017, 62, 401–406. [CrossRef]
- Creswell, J.W.; Plano Clark, V.L.; Gutmann, M.; Hanson, W.E. Advanced mixed methods research designs. In: Tashakkori A, Teddlie C, editors. Handbook of Mixed Methods in Social and Behavioral Research. California: Sage; 2003. pp. 209–240.
- Creswell, J.W.; Plano Clark, V.L. Designing and Conducting Mixed Methods Research. 2nd ed. California: Sage, 2011.
- Sandelowski, M. Whatever happened to qualitative description? . Res Nurs Health. 2000, 23, 334–340. [Google Scholar] [CrossRef]
- O'Cathain, A.; Murphy, E.; Nicholl, J. The quality of mixed methods studies in health services research. J Health Serv Res Policy. 2008, 13, 92–98. [Google Scholar] [CrossRef]
- Tong, A.; Sainsbury, P.; Craig, J. Consolidated criteria for reporting qualitative research (COREQ): a 32-item checklist for interviews and focus groups. Int J Qual Health Care. 2007, 19, 349–357. [Google Scholar] [CrossRef]
- Mehrholz, J.; Wagner, K.; Rutte, K.; Meissner, D.; Pohl, M. Predictive validity and responsiveness of the Functional Ambulation Category in hemiparetic patients after stroke. Arch Phys Med Rehabil. 2007, 88, 1314–1319. [Google Scholar] [CrossRef] [PubMed]
- Fugl-Meyer, A.R.; Bränholm, I.B.; Fugl-Meyer, K.S. Happiness and domain-specific life satisfaction in adult Northern Swedes. Clin Rehabil. 1991, 5, 25–33. [Google Scholar] [CrossRef]
- Melin, R.; Fugl-Meyer, K.S.; Fugl-Meyer, A.R. Life satisfaction in 18-64 years old Swedes in relation to education, employment situation, health and physical activity. J Rehabil Med. 2003, 35, 84–90. [Google Scholar] [CrossRef]
- Catz A, Itzkovich M, Agranov E, Ring H, Tamir A. spinal cord independence measure: a new disability scale for patients with spinal cord lesions. Spinal Cord. 1997, 35, 850–856. [CrossRef]
- Ware, J.J.; Sherbourne, C. The MOS 36-item short-form health survey (SF-36)-I. conceptual framework and item selection. Med Care. 1992, 30, 473–483. [Google Scholar]
- Sullivan, G.M.; Feinn, R. Using effect size—Or why the P value is not enough. J Grad Med Educ. 2012, 4, 279–282. [Google Scholar] [CrossRef]
- Prion, S.; Haerling, K.A. Making sense of methods and measurement: Spearman-Rho ranked-ordered coefficient. Clin. Simul. Nurs. 2014, 10, 535–536. [Google Scholar] [CrossRef]
- Cohen, J. Statistical Power Analysis for the Behavioral Sciences. New York: Routledge Academic; 1988.
- Morrow, S.L. Quality and trustworthiness in qualitative research in counseling psychology. J Couns Psychol. 2005, 52, 250–260. [Google Scholar] [CrossRef]
- Faulkner, S.L.; Trotter, S.P. Data Saturation. The International Encyclopedia of Communication Research Methods. New Jersey: Wiley Blackwell; 2017.
- Fusch, P.I.; Ness, L.R. Are we there yet? Data saturation in qualitative research. Qual. Rep. 2015, 20, 1408–1416. [Google Scholar]
- Guest, G.; Bunce, A.; Johnson, L. How many interviews are enough? An experiment with data saturation and variability. Field Methods. 2006;18, 59–82. [CrossRef]
- Dey, I. Grounding Grounded Theory: Guidelines for Qualitative Inquiry. San Diego: Academic Press; 1999.
- Archibald, M.M.; Ambagtsheer, R.C.; Casey, M.G.; Lawless, M. Using Zoom Videoconferencing for Qualitative Data Collection: Perceptions and Experiences of Researchers and Participants. Int J Qual Meth. 2019, 18, 1–8. [Google Scholar] [CrossRef]
- Barclay, L.; Callaway, L.; McDonald, R.; Farnworth, L.; Brown, G.; Broom, L. Time Use following Spinal Cord Injury: An Examination of the Literature. Brit Occup Ther. 2011, 74, 573–580. [Google Scholar] [CrossRef]
- Brown, M.; Gordon, W.; Spielman, L.; Haddad, L. Participation by Individuals with Spinal Cord Injury in Social and Recreational Activity Outside the Home. Top Spinal Cord Inj Rehabil. 2002, 7, 83–100. [Google Scholar] [CrossRef]
- Whiteneck, G.; Meade, M.A.; Dijkers, M.; Tate, D.G.; Bushnik, T.; Forchheimer, M.B. Environmental factors and their role in participation and life satisfaction after spinal cord injury. Arch Phys Med Rehabil. 2004, 85, 1793–1803. [Google Scholar] [CrossRef]
- Watson, A.C.; Larson, J.E. Personal Responses to Disability Stigma: From Self-Stigma to Empowerment. Rehabilitation Education. 2007, 20, 235–246. [Google Scholar] [CrossRef]
- Cresswell, T.; Dorow, S.; Roseman, S. Putting mobility theory to work: Conceptualizing employment-related geographical mobility. Environ Plann A. 2016, 48, 1787–1803. [Google Scholar] [CrossRef]
- Kerstin W, Gabriele B, Richard L. What promotes physical activity after spinal cord injury? An interview study from a patient perspective. Disabil Rehabil. 2006, 28, 481–488. [CrossRef]
- Conti A, Clari M, Nolan M, Wallace E, Tommasini M, Mozzone S, et al. The Relationship Between Psychological and Physical Secondary Conditions and Family Caregiver Burden in Spinal Cord Injury: A Correlational Study. Top Spinal Cord Inj Rehabil. 2019, 25, 271–280. [CrossRef]
- Craig, A.; Nicholson, K.P.; Guest, R.; Tran, Y.; Middleton, J. Adjustment following chronic spinal cord injury: Determining factors that contribute to social participation. BR J Health Psychol. 2015, 20, 807–823. [Google Scholar] [CrossRef] [PubMed]
- Rivers CS, Fallah N, Noonan VK, Whitehurst DG, Schwartz CE, Finkelstein JA, et al. Health conditions: effect on function, health related quality of life, and life satisfaction after traumatic spinal cord injury. A prospective observational Registry Cohort Study. Arch Phys Med Rehabil. 2018, 99, 443–451. [CrossRef]
- Stillman, M.D.; Barber, J.; Burns, S.; Williams, S.; Hoffman, J.M. Complications of spinal cord injury over the first year after discharge from inpatient rehabilitation. Arch Phys Med Rehabil. 2017, 98, 1800–1805. [Google Scholar] [CrossRef]
- van Koppenhagen CF, Post MW, van der Woude LH, de Groot S, de Witte LP, van Asbeck FW, et al. Recovery of life satisfaction in persons with spinal cord injury during inpatient rehabilitation. Am J Phys Med Rehabil 2009, 88, 887–895. [CrossRef]
- Bushnik, T. Access to equipment, participation, and quality of life in aging individuals with high tetraplegia (C1-C4). Top Spinal Cord Inj Rehabil. 2002, 7, 17–27. [Google Scholar] [CrossRef]
- Bushnik, T.; Charlifue, S. Longitudinal study of individuals with high tetraplegia (C1-C4) 14 to 24 years postinjury. Top Spinal Cord Inj Rehabil. 2005, 10, 79–93. [Google Scholar] [CrossRef]
- DeVivo, M.J.; Chen, Y. Trends in new injuries, prevalent cases, and aging with spinal cord injury. Arch Phys Med Rehabil. 2011, 92, 332–338. [Google Scholar] [CrossRef]
- Kalpakjian CZ, Houlihan B, Meade MA, Karana-Zebari D, Heinemann AW, Dijkers MP, et al. Marital status, marital transitions, well-being, and spinal cord injury: an examination of the effects of sex and time. Arch Phys Med Rehabil. 2011, 92, 433–440. [CrossRef]
- Kemp, B.J.; Krause, J.S. Depression and life satisfaction among people ageing with post-polio and spinal cord injury. Disabil Rehabil. 1999, 21, 241–249. [Google Scholar] [CrossRef]
- Krause, J.S. Longitudinal changes in adjustment after spinal cord injury: a 15-year study. Arch Phys Med Rehabil. 1992, 73, 564–568. [Google Scholar]
- Krause, J.S.; Coker, J.L. Aging after spinal cord injury: A 30-year longitudinal study. J Spinal Cord Med 2006, 29, 371–376. [Google Scholar] [CrossRef]
- Post, M.W.; Reinhardt, J.D. Participation and Life Satisfaction in Aged People with Spinal Cord Injury: Does Age at Onset Make a Difference? . Top Spinal Cord Inj Rehabil. 2015, 21, 233–240. [Google Scholar] [CrossRef]
- Putzke, J.D.; Richards, J.S.; Hicken, B.L.; DeVivo, M.J. Predictors of life satisfaction: a spinal cord injury cohort study. Arch Phys Med Rehabil. 2002, 83, 555–561. [Google Scholar] [CrossRef]
- Stensman, R. Adjustment to traumatic spinal cord injury. A longitudinal study of self-reported quality of life. Paraplegia. 1994, 32, 416–422. [Google Scholar] [CrossRef]
- van Leeuwen CM, Post MW, Hoekstra T, van der Woude LH, de Groot S, Snoek GJ et al. Trajectories in the course of life satisfaction after spinal cord injury: identification and predictors. Arch Phys Med Rehabil. 2011, 92, 207–213. [CrossRef]
- Charlifue, S.W.; Gerhart, K.; Whiteneck, G.G. Conceptualizing and quantifying functional change: An examination of aging with spinal cord injury. Top Geriatr Rehabil. 1998, 13, 35–48. [Google Scholar] [CrossRef]
- Charlifue, S.W.; Weitzenkamp, D.A.; Whiteneck, G.G. Longitudinal outcomes in spinal cord injury: aging, secondary conditions, and well-being. Arch Phys Med Rehabil. 1999, 80, 1429–1434. [Google Scholar] [CrossRef] [PubMed]
- Charlifue, S.; Gerhart, K. Community integration in spinal cord injury of long duration. NeuroRehabilitation. 2004, 19, 91–101. [Google Scholar] [CrossRef] [PubMed]
- Pershouse KJ, Barker RN, Kendall MB, Buettner PG, Kuipers P, Schuurs SB et al. Investigating changes in quality of life and function along the lifespan for people with spinal cord injury. Arch Phys Med Rehabil. 2012, 93, 413–419. [CrossRef]
- Savic, G.; Charlifue, S.; Glass, C.; Soni, B.M.; Gerhart, K.A.; Jamous, M. British Ageing with SCI study: Changes in physical and psychological outcomes over time. Top Spinal Cord Inj Rehabil. 2010, 15, 41–53. [Google Scholar] [CrossRef]
- Krause, J.S. Adjustment after spinal cord injury: a 9-year longitudinal study. Arch Phys Med Rehabil. 1997, 78, 651–657. [Google Scholar] [CrossRef]
- Goffman, E. Stigma Notes on the Management of Spoiled Identity. New Jersey: Prentice-Hall; 1963.
- Vogel, D.L.; Bitman, R.L.; Hammer, J.H.; Wade, N.G. Is stigma internalized? The longitudinal impact of public stigma on self-stigma. J Couns Psychol. 2013, 60, 311–316. [Google Scholar] [CrossRef]
- Kanuha, V.K. “The Social Process of "Passing" to Manage Stigma: Acts of Internalized Oppression or Acts of Resistance? ”. J Sociol Soc Welfare. 1999, 26, 27–46. [Google Scholar] [CrossRef]
- Abramson, D.M.; Park, Y.S.; Stehling-Ariza, T.; Redlener, I. Children as bellwethers of recovery: dysfunctional systems and the effects of parents, households, and neighborhoods on serious emotional disturbance in children after Hurricane Katrina. Disaster Med Public Health Prep. 2010, 4, S17–S27. [Google Scholar] [CrossRef] [PubMed]
- Cicchetti, D. A developmental psychopathology perspective on bipolar disorder. In: Miklowitz D, Cicchetti D, editors. Understanding bipolar disorder: A developmental psychopathology perspective. New York : Guilford press; 2010. pp. 1–34.
- Kassis, W.; Artz, S.; Moldenhauer, S. Laying Down the Family Burden: A Cross-Cultural Analysis of Resilience in the Midst of Family Violence. Child and Youth Services. 2013, 34, 37–63. [Google Scholar] [CrossRef]
- Tol WA, Barbui C, Galappatti A, Silove D, Betancourt TS, Souza R et al. Mental health and psychosocial support in humanitarian settings: linking practice and research. Lancet. 2011, 378, 1581–1591. [CrossRef]
- Dijkers, M.P. Quality of life of individuals with spinal cord injury: a review of conceptualization, measurement, and research findings. J Rehabil Res Dev. 2005, 42 (Suppl. 1), 87–110. [Google Scholar] [CrossRef]
- Dowler, R.; Richards, J.S.; Putzke, J.D.; Gordon, W.; Tate, D. Impact of demographic and medical factors on satisfaction with life after spinal cord injury: a normative study. J Spinal Cord Med. 2001, 24, 87–91. [Google Scholar] [CrossRef]
- Jörgensen, S.; Iwarsson, S.; Lexell, J. Secondary Health Conditions, Activity Limitations, and Life Satisfaction in Older Adults With Long-Term Spinal Cord Injury. PM R. 2017, 9, 356–366. [Google Scholar] [CrossRef] [PubMed]
- Kagawa-Singer, M.; Padilla, G.V.; Ashing-Giwa, K. Health-related quality of life and culture. Semin Oncol Nurs. 2010, 26, 59–67. [Google Scholar] [CrossRef] [PubMed]
- Carr, D.; Freedman, V.A.; Cornman, J.C.; Schwarz, N. Happy Marriage, Happy Life? Marital Quality and Subjective Well-Being in Later Life. J Marriage Fam. 2014, 76, 930–948. [Google Scholar] [CrossRef] [PubMed]
- Haas, B.M.; Price, L.; Freeman, J.A. Qualitative evaluation of a community peer support service for people with spinal cord injury. Spinal Cord. 2013, 51, 295–299. [Google Scholar] [CrossRef]
- Ljungberg, I.; Kroll, T.; Libin, A.; Gordon, S. Using peer mentoring for people with spinal cord injury to enhance self-efficacy beliefs and prevent medical complications. J Clin Nurs. 2011, 20, 351–358. [Google Scholar] [CrossRef]
- Veith, E.M.; Sherman, J.E.; Pellino, T.A.; Tasui, N.Y. Qualitative analysis of the peer-mentoring relationship among individuals with spinal cord injury. Rehabil Psychol. 2006, 51, 289–298. [Google Scholar] [CrossRef]
- Siebers, T.A. Disability Theory. United States: University of Michigan Press; 2009.
- Martz, E.; Livneh, H. Psychosocial adaptation to disability within the context of positive psychology: findings from the literature. J Occup Rehabil. 2016, 26, 4–12. [Google Scholar] [CrossRef]
- Fujikawa M, Lee E, Chan F, Catalano D, Hunter C, Bengtson K et al. The Connor - Davidson resilience scale as a positive psychology measure for people with spinal cord injuries. Rehabil Res Policy Educ. 2013, 27, 213–22.
- White, B.; Driver, S.; Warren, A.M. Resilience and indicators of adjustment during rehabilitation from a spinal cord injury. Rehabil Psychol. 2010, 55, 23–32. [Google Scholar] [CrossRef]
- Masten, A.S. Resilience in children threatened by extreme adversity: frameworks for research, practice, and translational synergy. Dev Psychopathol. 2011, 23, 493–506. [Google Scholar] [CrossRef]
- Ungar, M. Social ecological complexity and resilience processes. Behav Brain Sci.2015; 38: e124. [CrossRef]
- Theron, L.C.; Liebenberg, L.; Ungar, M. Youth resilience and culture: Commonalities and complexities. Netherlands: Springer; 2015.
- Bonanno, G.A.; Kennedy, P.; Galatzer-Levy, I.R.; Lude, P.; Elfström, M.L. Trajectories of resilience, depression, and anxiety following spinal cord injury. Rehabil Psychol. 2012, 57, 236–247. [Google Scholar] [CrossRef] [PubMed]
- deRoon-Cassini TA, Mancini AD, Rusch MD, Bonanno GA. Psychopathology and resilience following traumatic injury: a latent growth mixture model analysis. Rehabil Psychol. 2010, 55, 1–11. [CrossRef]
- Lee, K.H.; Xu, H.; Wu, B. Gender differences in quality of life among community-dwelling older adults in low- and middle-income countries: results from the Study on global AGEing and adult health (SAGE). BMC Public Health. 2020, 20, 114. [Google Scholar] [CrossRef] [PubMed]
| Variable | Label (Potential range) | [Mean ± SD] / N (%) | Low Quality of Life (N=5) N (%)/ Mean ± SD |
Moderate Quality of life (N=9) N (%)/ [Mean ± SD] |
High Quality of Life (N=10) N (%)/ [Mean ± SD] |
Statistic 1U/ 2(H) / 3[rs] |
Cohen’s d / (f) |
P |
|---|---|---|---|---|---|---|---|---|
| Gender | Male | 13 (54.16) [48.31±10.68] | 1 (20.00) | 4 (44.44) | 8 (80.00) | 30.001 | 1.12 | 0.02 |
| Female | 11 (45.83) [34.82± 13.28] | 4 (80.00) | 5 (55.56) | 2 (20.00) | ||||
| Type of injury4 | Traumatic | 14 (58.30) [45.79±13.05] |
2 (40.00) | 4(44.44) | 8 (80.00) | 32.001 | 0.29 | 0.41 |
| Non Traumatic | 6 (25.00) [40.67± 14.62] |
1 (20.00) | 3(33.33) | 2 (20.00) | ||||
| Level of spinal cord injury | Cervical | 9 (37.50) | - | 4 (44.44) | 4 (40.00) | (0.58)2 | (0.03) | 0.75 |
| Thoracic | 6 (25.00) | 2 (40.00) | 2 (22.22) | 3 (30.00) | ||||
| Lumbar | 9 (37.50) | 3 (60.00) | 3 (33.33) | 3 (30.00) | ||||
| Attended rehabilitation | Yes | 16 (66.67) [46.38±10.36] |
1 (20.00) | 7 (77.78) | 8 (80.00) | 29.001 | 0.957 | 0.032 |
| No | 8 (33.33) [33.62±15.76] |
4 (80.00) | 2 (22.22) | 2 (20.00) | ||||
| Employed | Yes | 4 (16.67) [43.75±16.86] | 1 (20.00) | 1 (11.11) | 2 (20.00) | 34.501 | 0.13 | 0.67 |
| No | 20 (83.33) [41.80±13.28] | 4 (80.00) | 8 (88.89) | 8(80.00) | ||||
| Marital Status | Never married/Separate/ Divorce |
11 (45.83) [35.27±14.16] |
5 (100.00) | 3 (33.33) | 3 (30.00) | 37.001 | 1.02 | 0.04 |
| Married/ Common Law | 13 (54.17) [47.92± 10.24] | - | 6 (66.67) | 7 (70.00) | ||||
| Location of residence | City | 13 (54.16) | 3 (60.00) | 3 (33.33) | 7 (70.00) | (1.49)2 | (0.06) | 0.48 |
| Suburban | 7 (29.17) | - | 5 (55.56) | 2 (20.00) | ||||
| Rural | 4 (16.67) | 2 (40.00) | 1 (11.11) | 1 (10.00) | ||||
| Living situation | Live alone | 8 (33.33) [37.00±14.21] |
3 (60.00) |
3 (33.33) |
2 (20.00) |
44.501 | 0.57 | 0.23 |
| Live with somebody |
16 (66.67) [44.69± 12.88] | 2 (40.00) | 6 (66.67) | 8 (80.00) | ||||
| Level of education | 2=High school | 7 (29.17) | [3.60 ± 1.14] | [3.56±1.51] | [3.70±1.57] | [0.07]3 | - | 0.72 |
| 3=College/Trade School | 5 (20.83) | |||||||
| 4=University degree | 5 (20.83) | |||||||
| 5=Graduate studies | 4 (16.67) | |||||||
| 6=Postgraduate | 3 (12.50) | |||||||
| Number of Years Living with an injury | (2 – 52) | [21.88 ± 16.30] | [26.20±16.92] | [27.67±18.53] | [14.50±12.01] | [-0.40] 3 | - | 0.05 |
| Gross annual income 5 | (1-7)6 | [1.83 ± 2.88] | [2.20 ± 2.39] | [0.78±2.39] | [2.60±3.44] | [0.15] 3 | - | 0.48 |
| Age (Years) | (27 – 72) | [54.60 ± 14.60] | [50.60±15.44] | [54.22±12.17] | [57.30±16.95] | [0.19]3 | - | 0.37 |
| 12 – Item Short-form health survey: Mental component scores | (22 -60) | [39.95 ± 11.11] | [29.77±5.29] | [36.04±7.34] | [48.56±9.99] | [0.74]3 | - | <0.01 |
| 12 – Item Short-form health survey:Physical component scores | (20 -57) | [35.10 ± 9.86] | [28.99±10.36] | [29.95±4.63] | [42.80±8.27] | [0.68]3 | - | <0.01 |
| Spinal cord independence measure - III | (38 -100) | [79.04 ±13.90] | [70.20±18.19] | [75.44±13.72] | [86.70±7.62] | [0.34]3 | - | 0.11 |
| Functional ambulatory category | 4=Ambulate independently level surface only | 12 (50.00) [38.50±12.52] |
3(60.00) | 6(66.67) | 3(30.00) | 46.501 | 0.54 | 0.14 |
| 5=Ambulate independently | 12 (50.00) [45.75±14.08] |
2(40.00) | 3(33.33) | 7(70.00) | ||||
| Life satisfaction questionnaire – 11 | (20- 64) | [42.13 ± 13.54] | [22±2.35] | [39±4.44] | [55±5.46] | - | - | - |
| Low Quality of life (P1, P6, P11, P13, P14) | Moderate Quality of life (P4, P5, P7, P9, P10, P15, P16, P18, P20) | High Quality of life (P3, P2, P8, P17, P12, P19, P21, P22, P23, P24) | |
|---|---|---|---|
| Potential Barriers to Quality of Life |
|
|
|
| Potential Facilitators to Quality of Life |
|
|
|
| Topic | Quotation | Participant information |
|---|---|---|
| Feeling socially isolated | ||
| Losing friends because of pain intolerance | ‘I have ongoing and significant pain, difficulty sitting, and difficulty walking. I can't sit in an upright position for very long without pain, I can sit in my wheelchair for about two hours but I couldn't sit in a regular kitchen chair on a couch. I wasn't able to go to see friends anymore for lunch or coffee because I couldn't sit. I went a long time without a wheelchair before I was finally approved for one.’ | P11, female, 63 years old, T6 |
| Losing human contact and preferred in person interaction | ‘I miss some of the important people in my life because we are not able to connect in the same way. Phone calls are not the same as actually going out and meeting people, person to person, and doing something fun together or going out for a meal or hanging out at a social event, it’s not the same connection.’ | P14, female, 51 years old, thoracic |
| Having financial concerns | ||
| Identifying financial need as barrier for participation | ‘That’s been a barrier because of the low income that I get from my pension. If I wanted to get an electric assistive device this is kind of expensive, I do need home adaptations right now, but those cost a high price so I have to adapt myself to my house set up for the time being which is tiring and consumes most of my energy.’ | P06, a 31-year-old male, injured in the lumbar region |
| Being judged | ||
| Feeling invisible | ‘That’s pretty much an everyday occurrence. People treat me like this because I’m physically disabled and think I’m mentally disabled and they’ll ask the person I’m with the question, instead of asking me, which is very infuriating because I’m an adult and you know, highly competent, I can talk for myself.’ | P14, female, 51 years old, thoracic |
| Experiencing prejudice | ‘Discrimination happens all the time because people have attitudinal barriers. They’re straight-up rude and basically kind of treat you like you’re a non-human. And that pretty much is all the time because I look physically disabled when I’m out and about, I get stares, I get looks, it’s pretty much constant.’ | P14, female, 51 years old, thoracic |
| Feeling left out due to city layout and infrastructure | ||
| Experiencing accessibility challenges in the built environment | ‘The area where I live is a bit hilly. So it's difficult either using my walker/ my cane /my wheelchair; there are some streets I can't go on. I find that some of those curb cuts on the sidewalk are steep and sometimes I have to get out of my wheelchair and push it up the curb cuts, then I can get back in. Some of the stores in the area I live have a couple of steps up or down, to get into the stores, so of course, I don't go there. If a place is not wheelchair accessible I don't go there.’ | P11, female, 63 years old, T6 |
| Expressing that spinal cord injury was due to medical negligence | ||
| Expressing deterioration in health due to medical negligence | ‘If I would've had the machine to help me breathe, my health, my walking, and everything else would never have deteriorated. I never had to end up in the hospital and now I have to go to the hospital to see a cardiologist, All because I didn't get the right rehabilitation for my deteriorating leg, hip, and back muscles with the machine to help me breathe.’ | P01, female, 40 years old, T6-T7 |
| Expressing a degradation in mobility | ||
| Feeling like prematurely aging | ‘It's like living with a 121-year-old woman, that's what I'm like. I bring in the groceries from the car using the walker, I'll be paralyzed in bed for 8 - 14 hours. So right after I - I lie in bed for 13 hours, sometimes slept all day, like I was just paralyzed, just couldn't do a thing. in six months I'll get paralyzed 130 times and could not move.’ | P13, female, 68-year-old, L3-L5 |
| Topic | Quotation | Participant information | |
|---|---|---|---|
| Feeling judged | |||
| Feeling hyper visible | ‘They don’t realize maybe how disabled I am, why I’m disabled, or why I’m using a cane. So, even when I’m in a wheelchair, I always have my canes with me (move or go somewhere, where I can’t go with my wheelchair), so if I stand up and use the canes, I kind of get this look, oh why are you using your canes? Why are you using a chair then? I might get a strange look.’ | P16, female, 67 years old, C3-C4 | |
| Expressing a positive experience with abled bodied people | ‘I've been lucky because, in pickleball and ping pong and all the other sport-type activities I wanted to join, I never had to join through a disability-specific organization because I've always been accepted by able-bodied people to join as a guy in a wheelchair.’ | P09, male, 67 years old, C6- C7 | |
| Experiencing a decrease in mobility | |||
| Acknowledging a decrease in mobility after surgery | ‘Before I could walk with 2 poles, but now I cannot walk with them instead I have to use a walker, without the walker it's just that I look like I’m a little drunk because my coordination is not there all the time. My equilibrium is not what it used to be, if I unexpectedly come on a change in the terrain I'm walking on, it's a big problem for me because I can't react normally and could end up falling. I look like I'm drunk really and that saddens me.’ | P18, male, 54 years old, lumbar | |
| Learning to adapt to life after injury | |||
| Navigating through challenges | ‘I have turned my wheelchair into a tricycle, so Vancouver is full of hills, … now perfectly able to go up and down hills anywhere I want. The apartment that I have has been completely modified for accessibility, the cabinets come down to my level, I have a cooktop and a kitchen sink that can come down to my level, and the entire washroom is accessible for me in my wheelchair. So my apartment does not have barriers for me.’ | P09, male, 67 years old, C6- C7 | |
| Making peace with things I cannot do | ‘I would be getting up most of the mornings with back pain, but I had been living with back pain the majority of the time, and I've just gotten used to it. And I functioned with it.’ | P10, female, 46 years old, C5-C6 | |
| Adjusting to their routine | ‘My day is very limited in what I did in my day. A lot of tasks would take me twice as long to do. I have to make sure I'm not sitting too long because then the pain kicks in, but at the same time, I can't do movement for long periods. If I do go on the treadmill I need to sleep that day for 20 minutes to an hour.’ | P10, female, 46 years old, C5-C6 | |
| Appreciating their support system | |||
| Feeling blessed to have support | ‘I'll have meetings with my pastor who's also a good friend, so mentally, I do alright. With my boyfriend's family and abled-bodied friends I feel [I am] in an inclusive environment and it just I feel supported.’ | P04, female, 36 years old, C5 – C6 | |
| Expressing a support system gives courage to keep moving forward in life | ‘I have friends and they are always looking for places for me to rest, which is nice. We’ll just sit here for a while. Because they know I have limits and I do get tired. They don’t want me to fall over because then they have to pick me up - which has happened a few times.’ | P07, male, 62 years old male, C6-C7 | |
| Having financial stability | |||
| Showing gratitude that partner still has a job | ‘At the moment I'm very fortunate with my husband that he has a good job and he's working. At the moment we're okay financially.’ | P10, female, 46 years old, C5-C6 | |
| Feeling fortunate for financial stability | ‘I'm very fortunate that I did not lose my job [because of the pandemic]. I worked for 5 years after my accident, then I retired. I have a good federal pension, so COVID has had no impact and my accident has had minimal impact. I was well insured when I had my accident so that helped me very well. I have no financial issues that arise after my accident. I don't have to wait for approval for spending money, to go somewhere, whatever it is.’ | P09, male, 67 years old, C6- C7 | |
| Topic | Quotation | Participant information |
|---|---|---|
| Demonstrating resilience | ||
| Expressing determination to recover from injury | ‘It took me three months to make it out to the end of the driveway after I got out of the hospital. I must've fallen at least twice a day. My problem was my feet, I'd be walking along and all of a sudden one leg would go out. It took a long time to learn to keep the feet going where I wanted to, even after I managed to learn to get the feet to go where I wanted to, I had to watch it. I could go for a walk but I wouldn't see anything besides the concrete (laugh).’ | P03, male, 67 years old, C5-C6 |
| Seeing progress over time | ‘Recently because I'm still seeing progressing like I'm still seeing improvement in my recovery, so that's why I'm still attacking this uh as aggressively, now I can walk 50 meters without needing a walking device, and I feel fortunate that I can walk.’ | P22, male, 49 years old, C6 |
| Learning to adapt to life after injury | ||
| Facing challenges | ‘I don't look at barriers, I look at them more like challenges, I usually come up with a way of um modifying something so I can still do it. I'll give you an example I started deer hunting, and my wife said, "Why don't you go and get some venison," because I grew up on that when we were young with our families. So I got my bow and go out and did that, but I couldn't carry the deer on my shoulders as I could before, so I made a kind of a sled and a harness and ski poles.’ | P08, male, 72 years old, lumbar |
| Appreciating their support system | ||
| Being thankful for having support | ‘If my wife, wasn’t there, I would be struggling at this point. I really would. And so, she has been, she’s been my rock type of thing. She’s really helped. And I couldn’t like I said I don’t think I would be here if it wasn’t for that because there’s thoughts, you know right after, and I didn’t see a future, I didn’t see anything. And that was really difficult.’ | P24, male, 68 years old, L3-L5 |
| Feeling a sense of belongingness to a group | ‘I feel included and welcomed [at the spinal cord injury organization]. Well, I have the same problems, in terms of bowels and bladder, if you went to a family physician, they may see one or two cases in their whole time, in their practice. Whereas, the people who specialize in this, so, or the people in the ambulatory group, you’re talking to people who do it 24/7, and have these problems. So, they have much better answers than, the doctors. So, it’s quite good and powerful to have this cohort. Just talking to each other about the problems we face.’ | P24, male, 68 years old, L3-L5 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




