Submitted:
14 August 2023
Posted:
16 August 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
- Statistical Analysis
- Research ethics
3. Results
4. Discussion
| Variable | Group | N | % | |
|---|---|---|---|---|
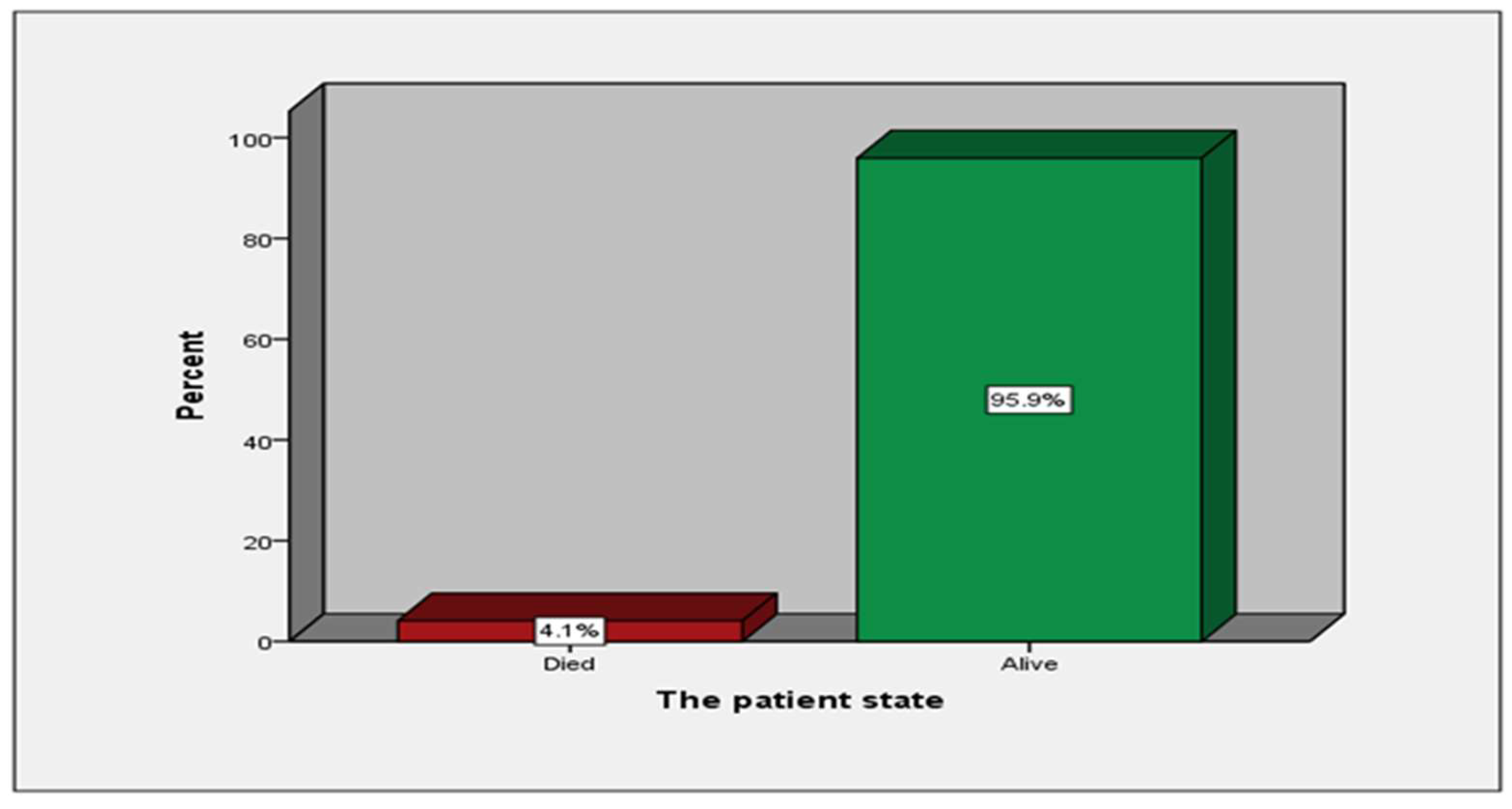
| Patient state | Died | 11 | (4.1%) | |
| Alive | 259 | (95.9%) | ||
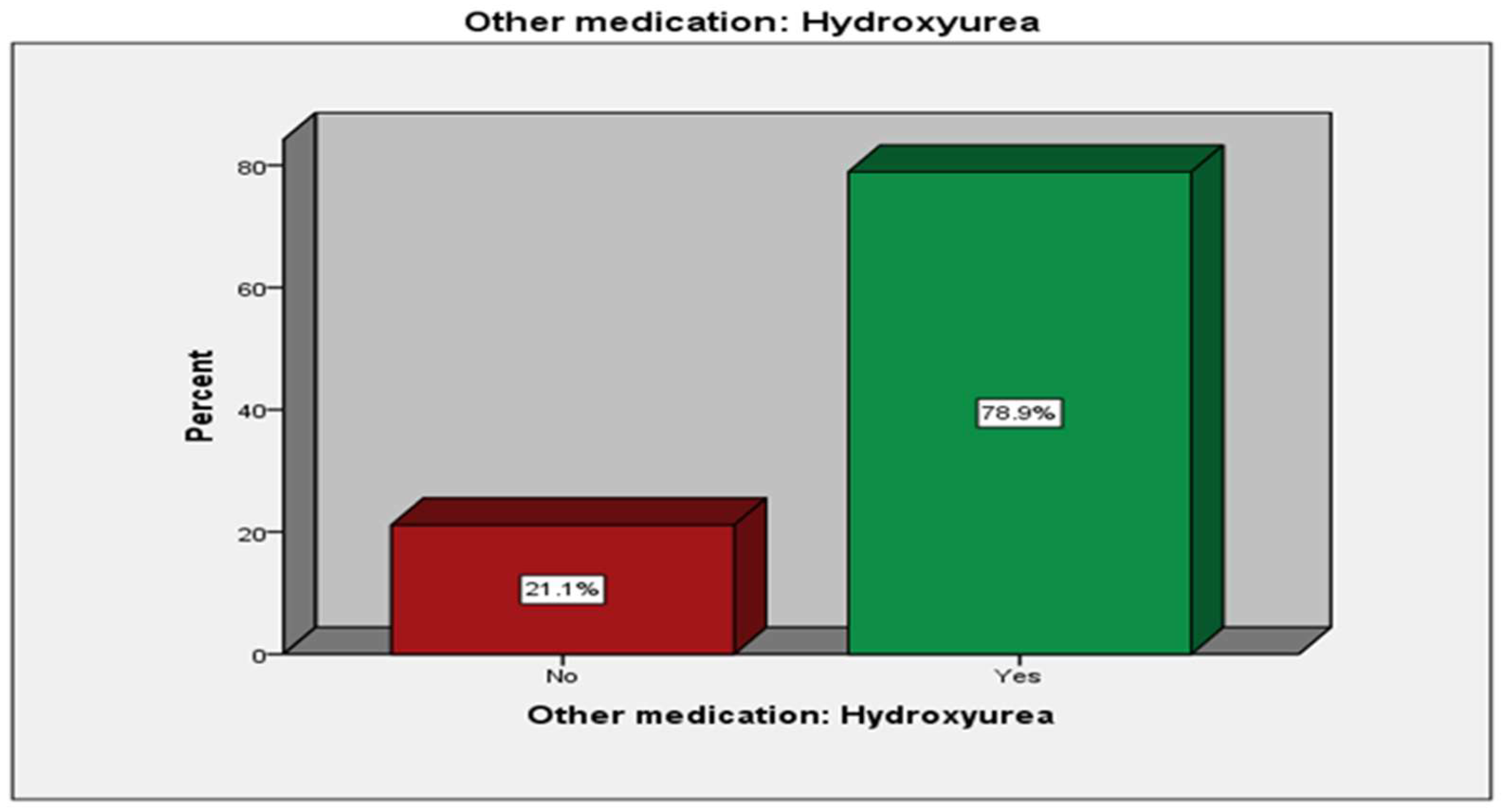
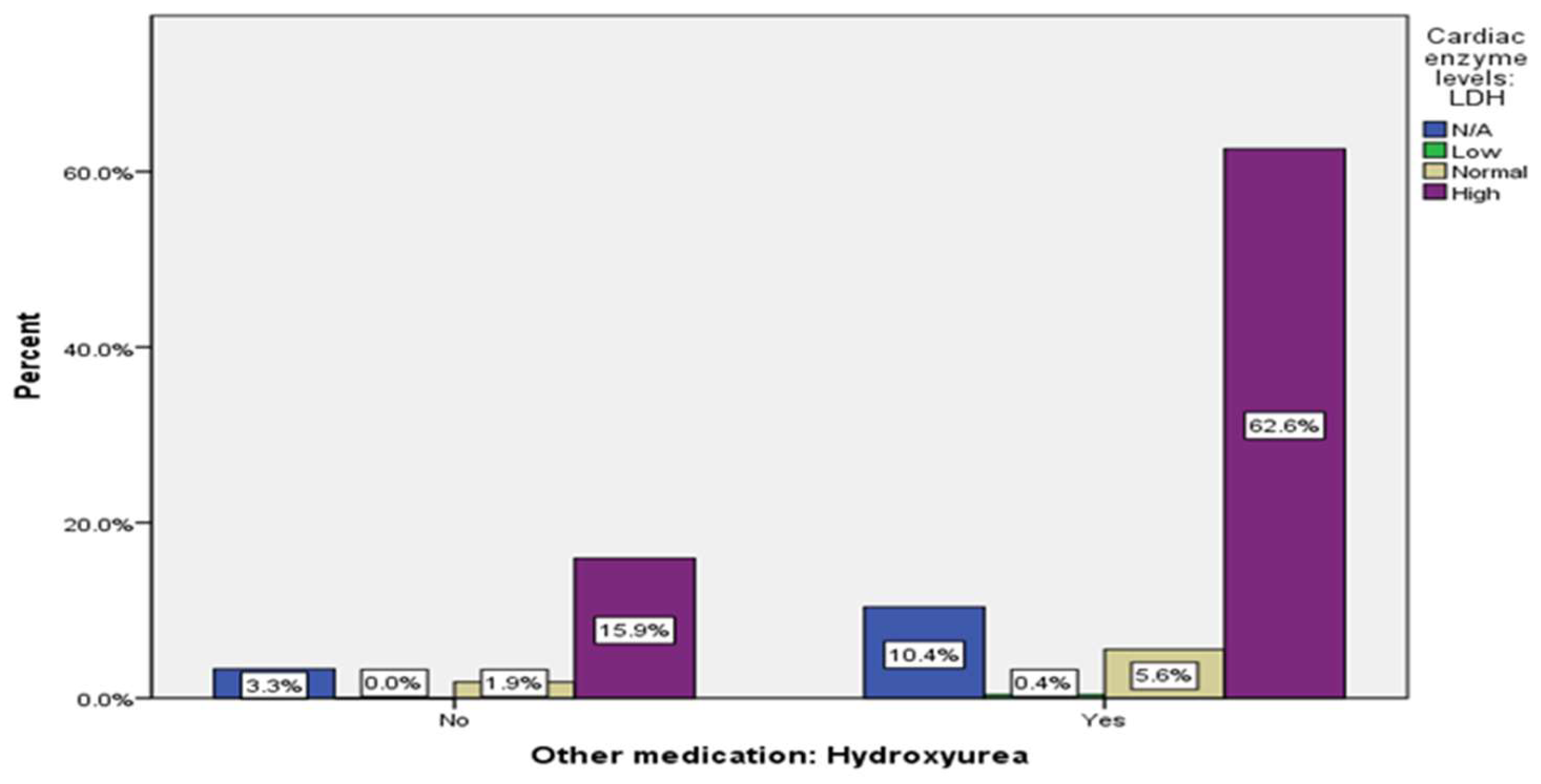
| Using Hydroxyurea | No | 57 | (21.1%) | |
| Yes | 213 | (78.9%) | ||
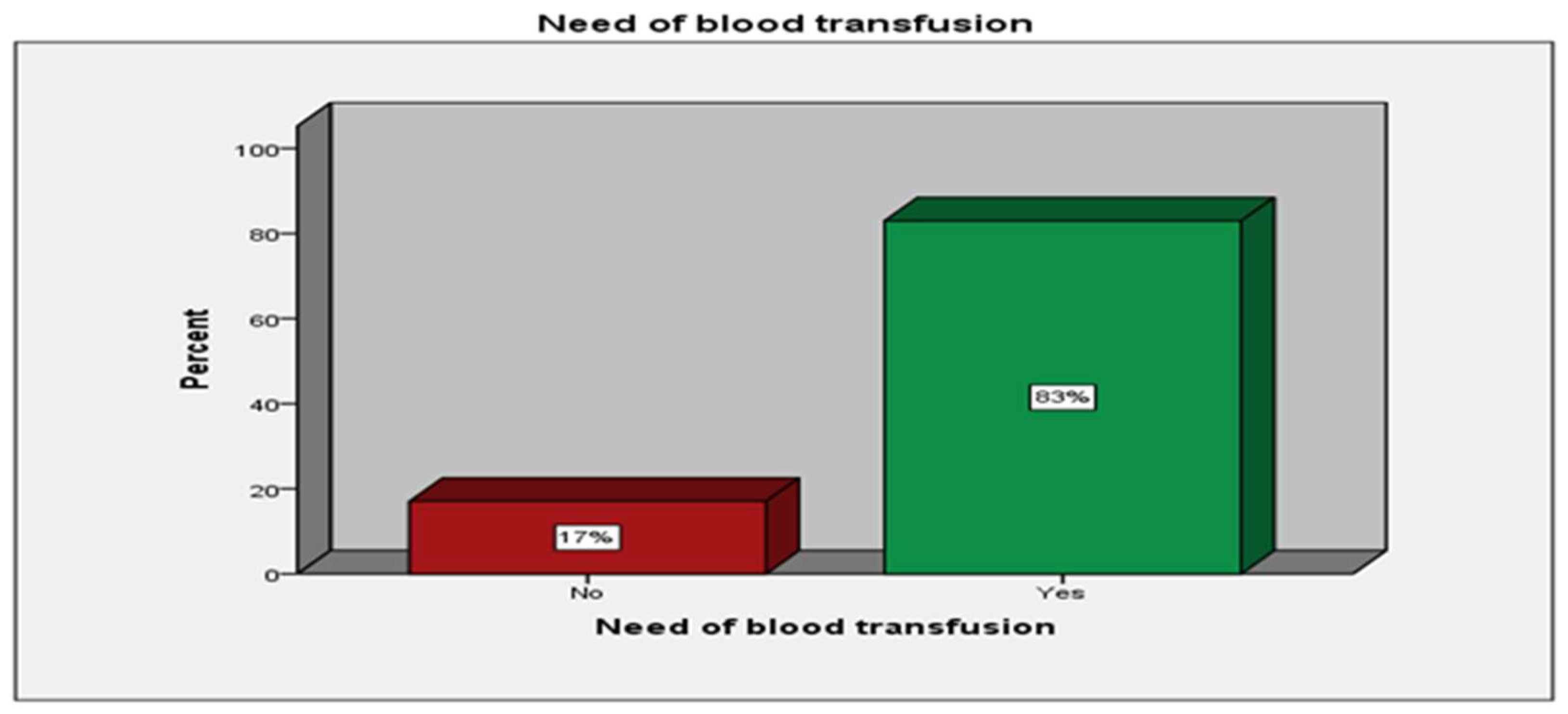
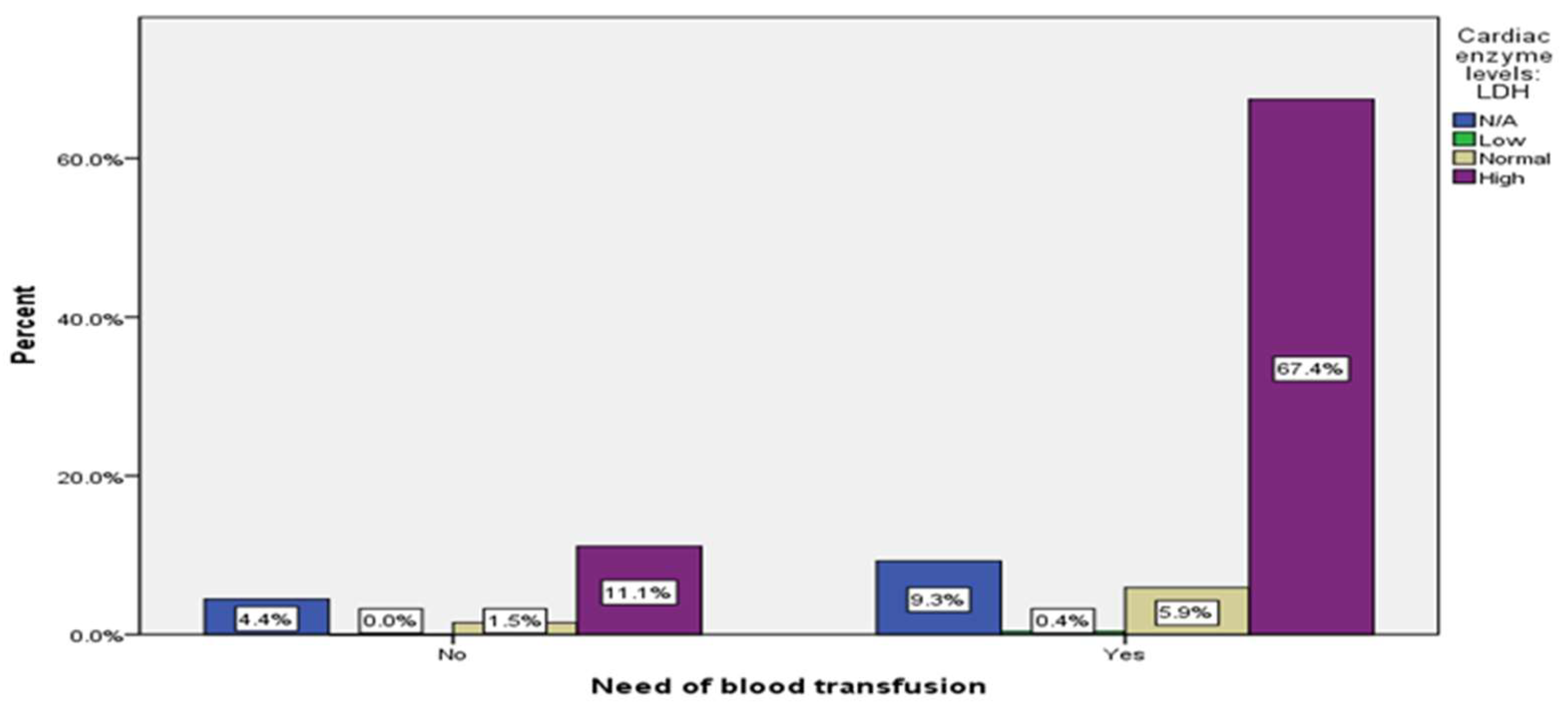
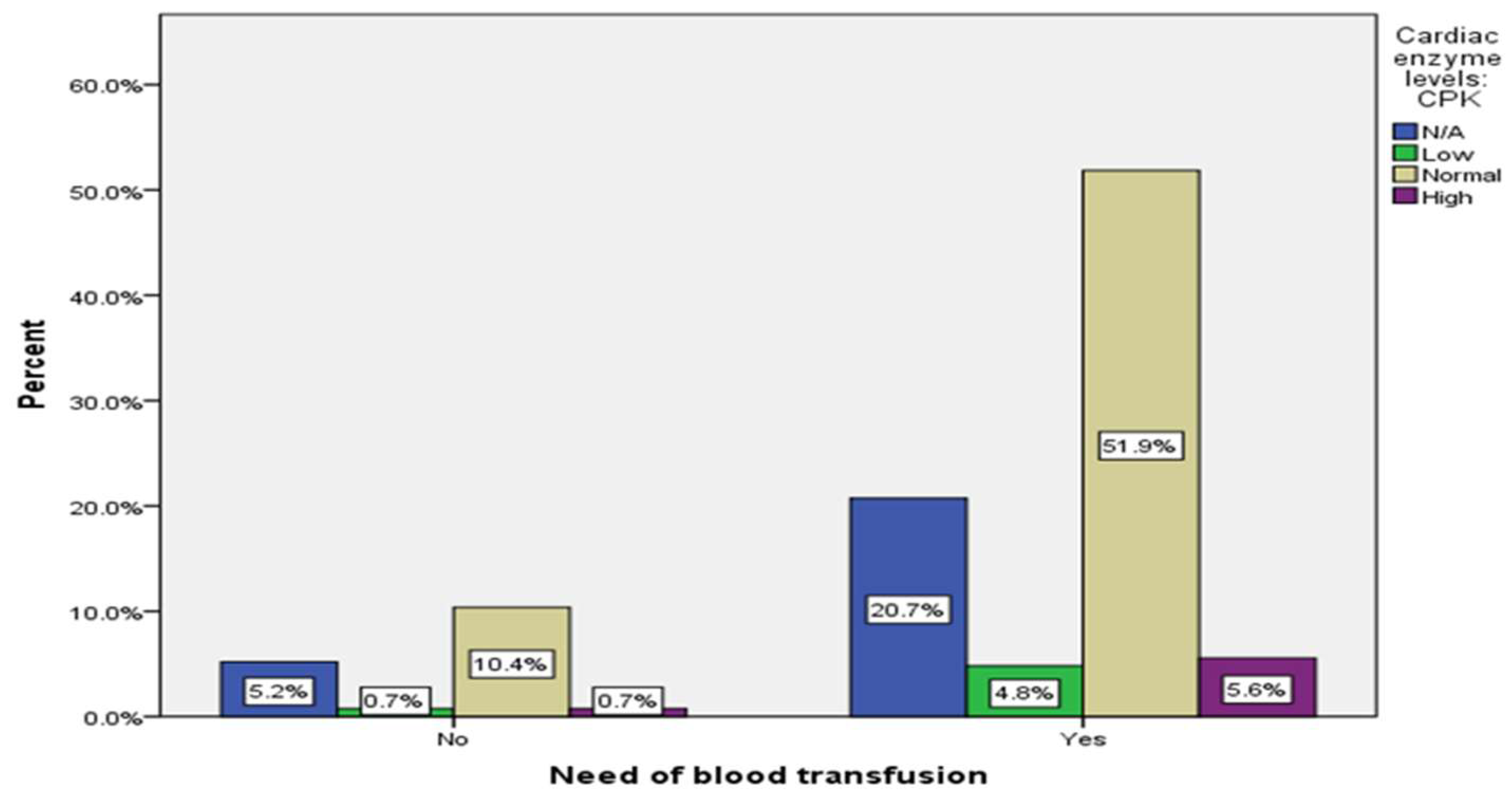
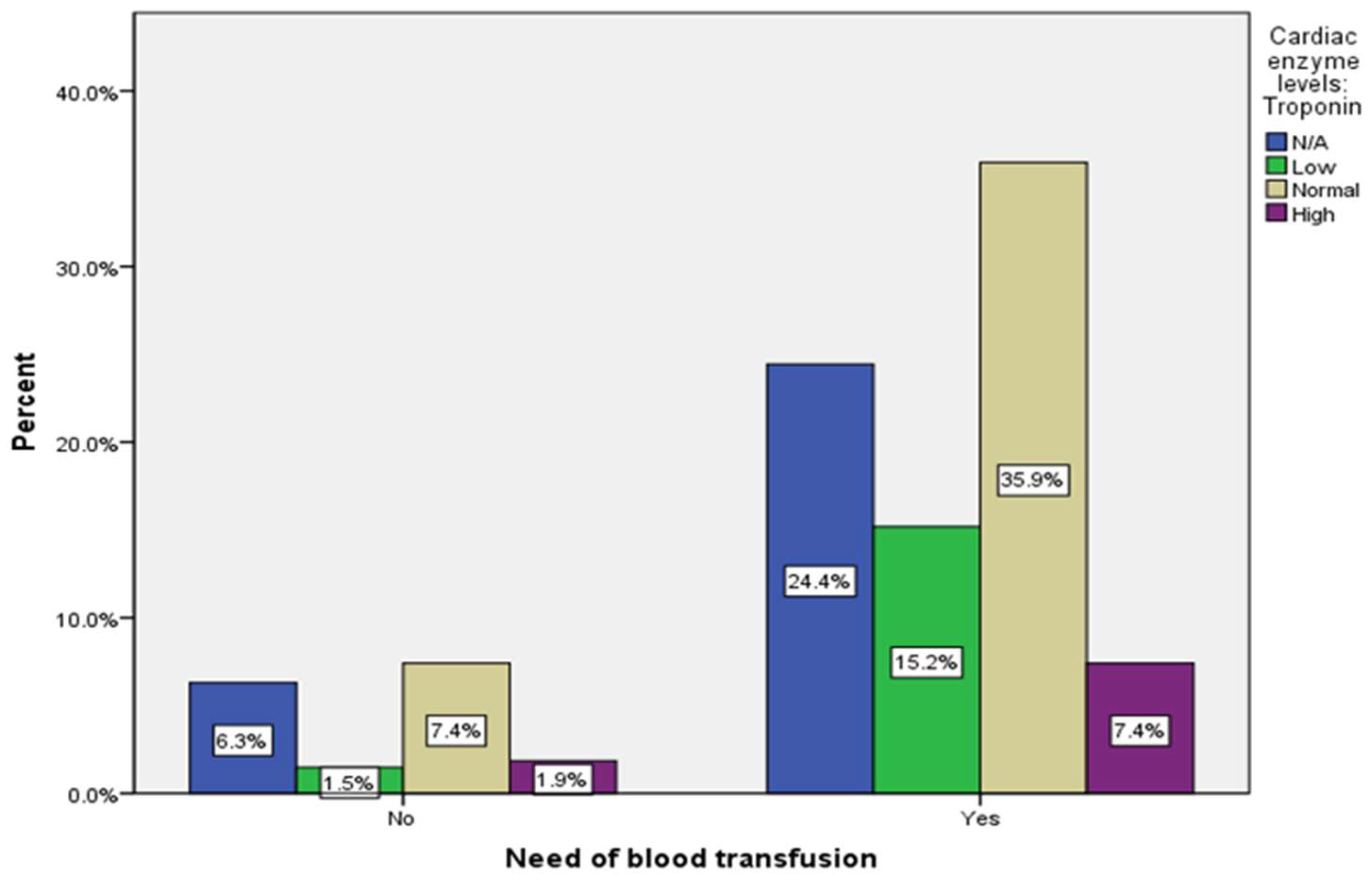
| Need for blood transfusion | No | 46 | (17%) | |
| Yes | 224 | (83%) | ||
| Age | Minimum | 0 | 3.7% | |
| Maximum | 2740 | 0.4% | ||
| Mean | 40 | |||
| Median | 7 | |||
| Standard deviation | 228 | |||
| Number of blood transfusion |
Simple transfusion |
Minimum | 0 | |
| Maximum | 180 | |||
| Mean | 12 | |||
| Standard deviation | 22 | |||
| Exchange transfusion | Minimum | 0 | ||
| Maximum | 94 | |||
| Mean | 7 | |||
| Standard deviation | 17 | |||
| Total transfusion | Minimum | 0 | ||
| Maximum | 215 | |||
| Mean | 20 | |||
| Standard deviation | 36 | |||
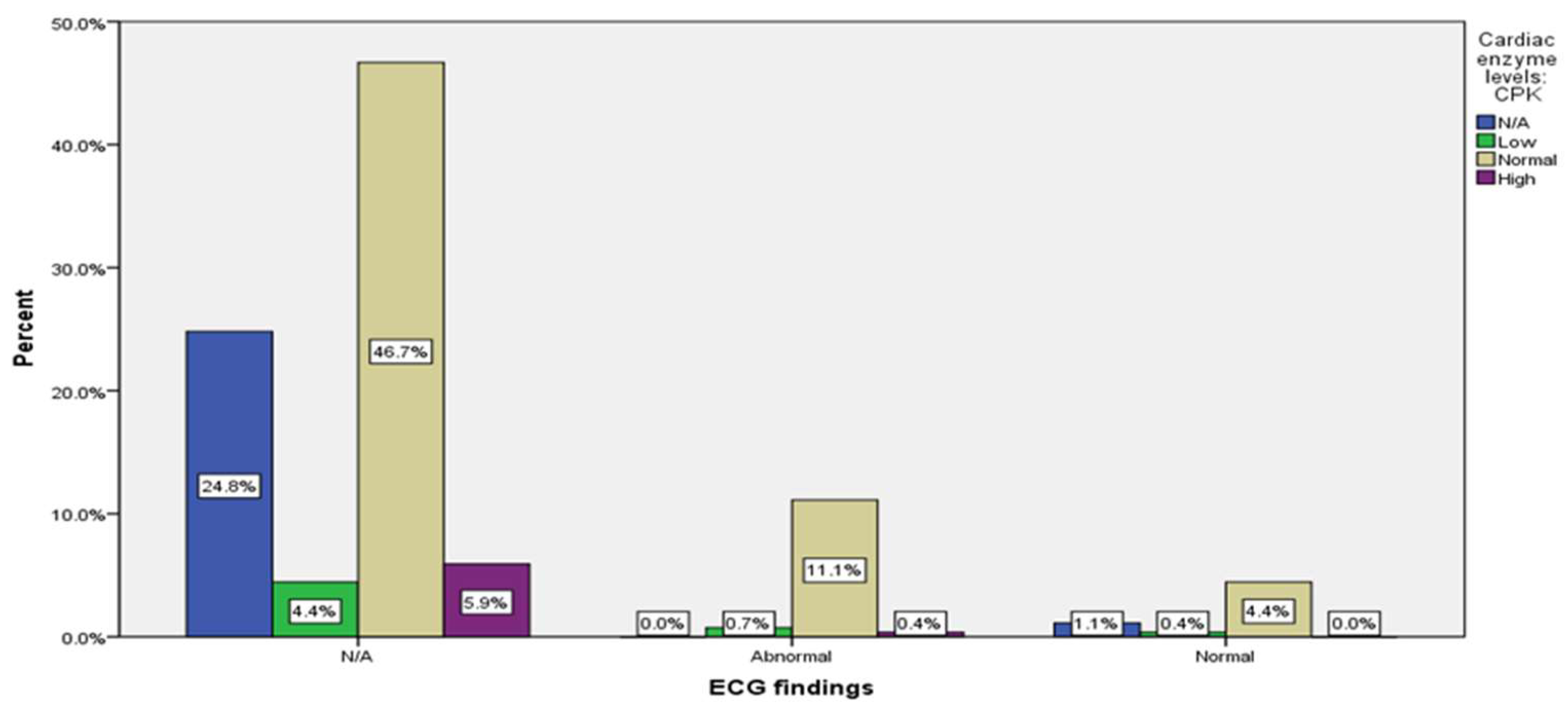
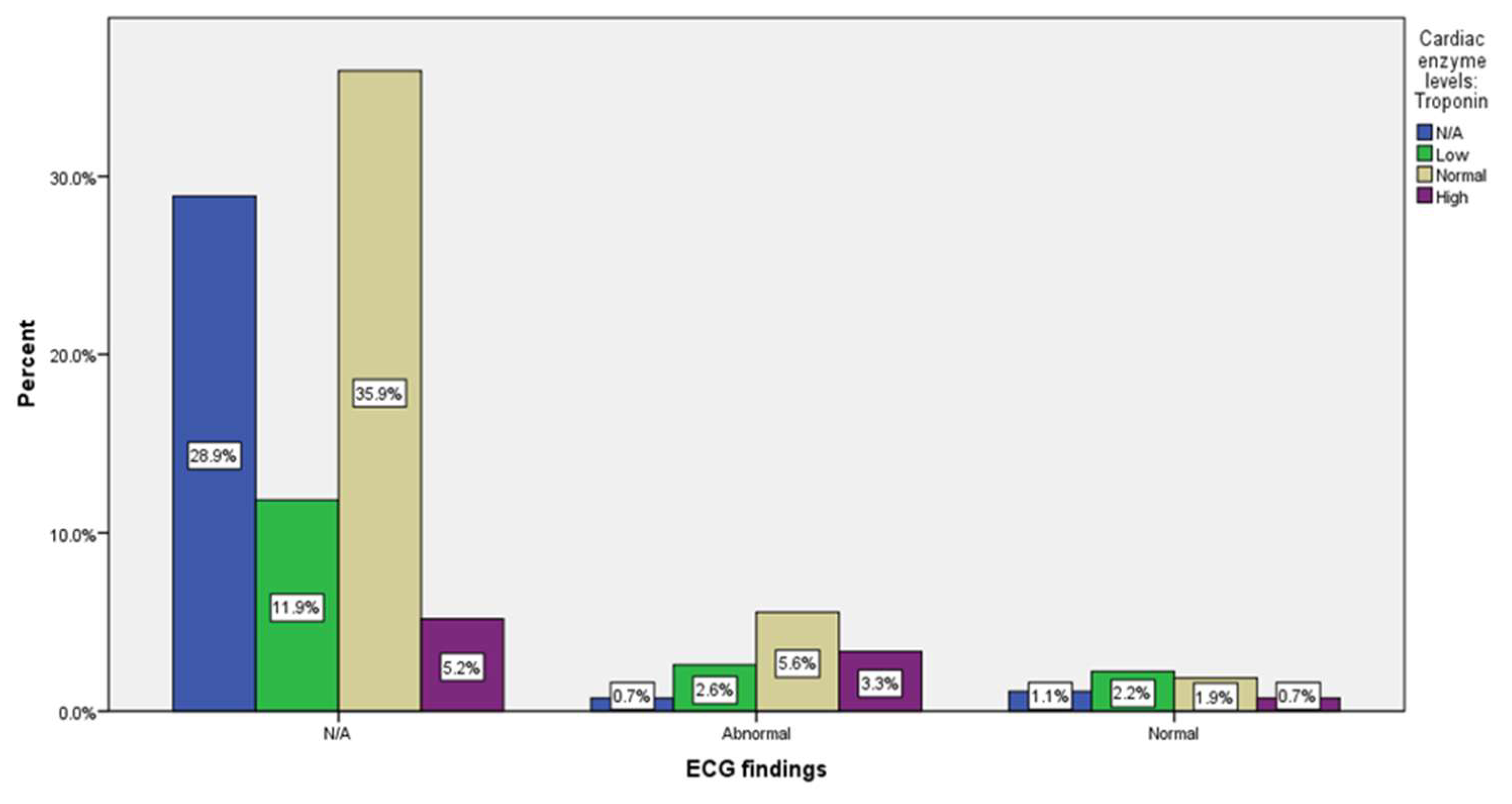
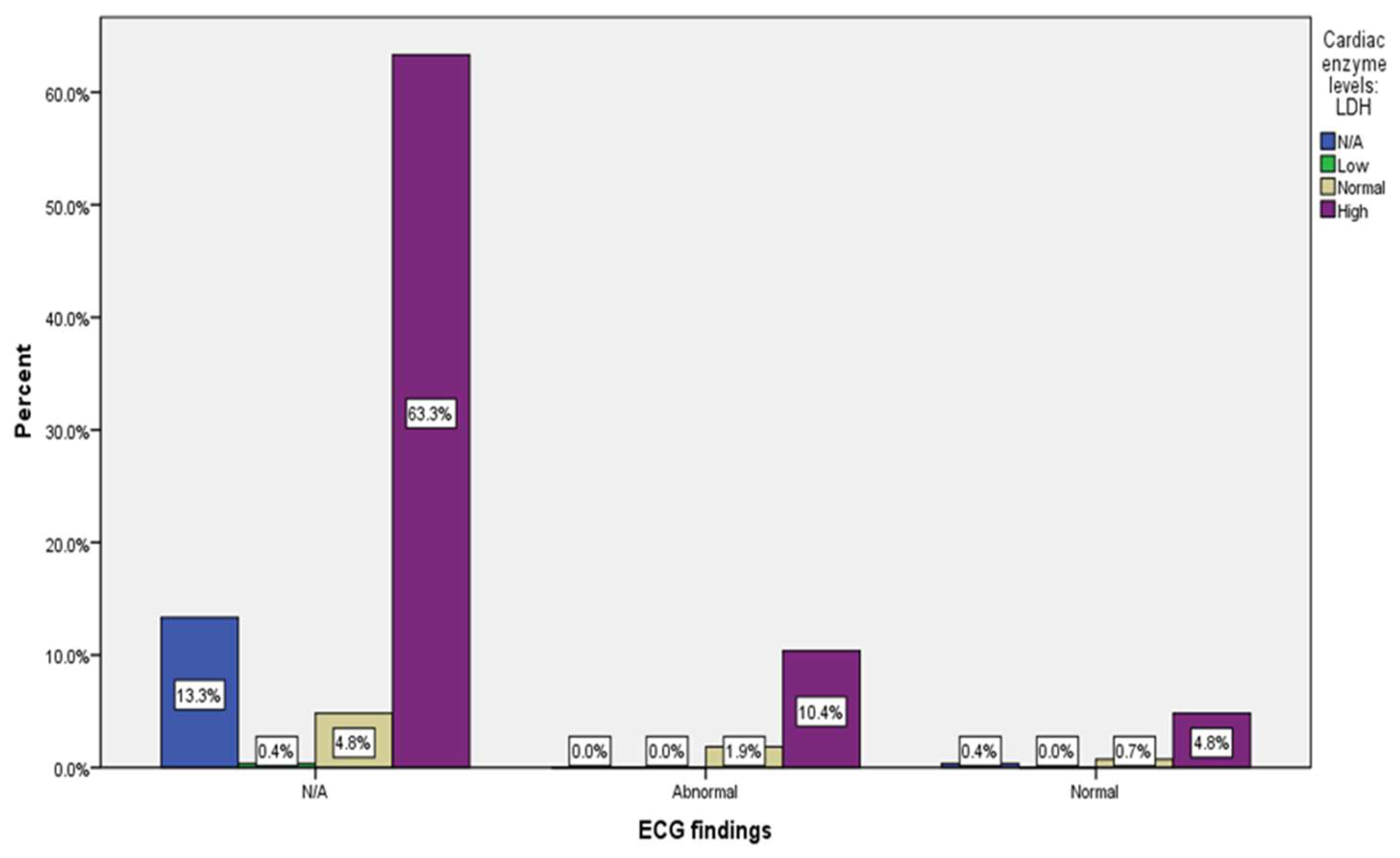
| ECG | N/A | 221 |
(81.9%) |
|
| Abnormal | 33 |
(12.2%) |
||
| Normal | 16 |
(5.9%) |
||
| Age | Minimum | 19 | ||
| Maximum | 82 | |||
| Mean | 32.2 | |||
| Median | 32 | |||
| Standard deviation | 8.78 | |||
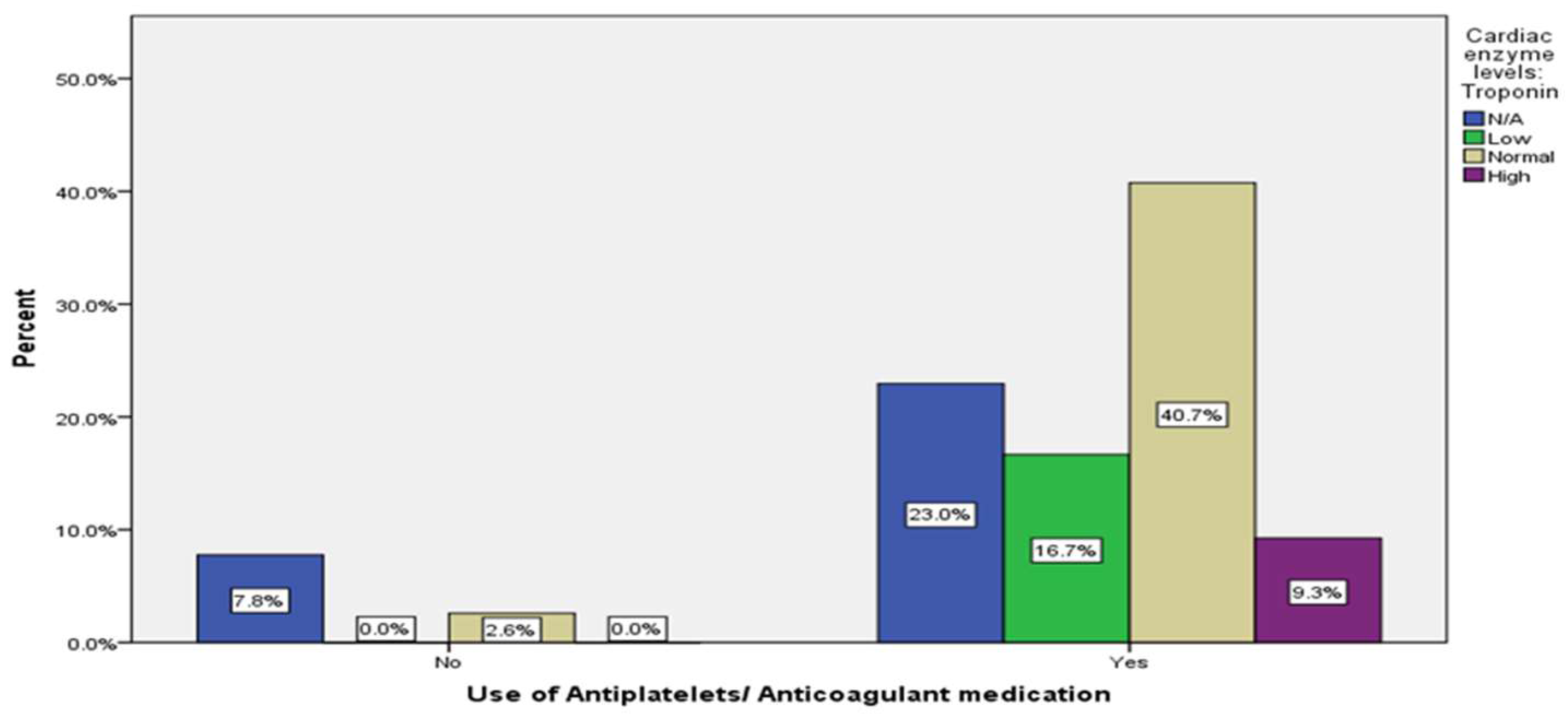
| Antiplatelets/ Anticoagulant medication | No | 28 |
(10.4%) |
|
| Yes | 242 |
(89.6%) |
||
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Sample Availability
Abbreviations
| SCD | Sickle cell disease |
| VOC | Vaso-occlusive crisis |
| Hgb | Beta-globin chain of hemoglobin |
| LDH | Lactate dehydrogenase |
| CK-MB | Creatine Kinase |
Appendix A
References
- Bunn, H.F. Pathogenesis and Treatment of Sickle Cell Disease. New England Journal of Medicine 1997, 337, 762–769. [Google Scholar] [CrossRef] [PubMed]
- Fitzhugh, C.; Lauder, N.; Jonassaint, J.; Telen, M.; Zhao, X.; Wright, E.; Gilliam, F.; De Castro, L. Cardiopulmonary Complications Leading to Premature Deaths in Adult Patients with Sickle Cell Disease. American journal of hematology 2010, 85. [Google Scholar] [CrossRef]
- Voskaridou, E.; Christoulas, D.; Terpos, E. Sickle-Cell Disease and the Heart: Review of the Current Literature. British Journal of Haematology 2012, 157, 664–673. [Google Scholar] [CrossRef] [PubMed]
- Gladwin, M.T.; Sachdev, V. Cardiovascular Abnormalities in Sickle Cell Disease. Journal of the American College of Cardiology 2012, 59, 1123–1133. [Google Scholar] [CrossRef]
- Balbaid, E.A.; Murad, M. abdulaziz; Abousada, H.J.; Banjar, A.Y.; Taj, M.A.; Bamohsen, N.K.; Alghubishi, S.A.; Alrsheedi, A.J.M.; Alshanbari, N.F.; Alsahaqi, R.S.N.; et al. Prevalence of Pulmonary Hypertension in Sickle Cell Anemiai Patient in KSA. Journal of Pharmaceutical Research International 2021, 214–220. [Google Scholar] [CrossRef]
- Agarwal, M.; Shah, M.; Patel, B.; Nolan, V.G.; Reed, G.L.; Oudiz, R.J.; Choudhary, G.; Maron, B.A. Association between Pulmonary Hypertension and Clinical Outcomes in Hospitalized Patients with Sickle Cell Disease. 2018, 198, 534–537. [Google Scholar] [CrossRef] [PubMed]
- Savale, L.; Habibi, A.; Lionnet, F.; Maitre, B.; Cottin, V.; Jais, X.; Chaouat, A.; Artaud-Macari, E.; Canuet, M.; Prevot, G.; et al. Clinical Phenotypes and Outcomes of Precapillary Pulmonary Hypertension of Sickle Cell Disease. European Respiratory Journal 2019, 54. [Google Scholar] [CrossRef]
- Howard, J.; Ataga, K.I.; Brown, R.C.; Achebe, M.; Nduba, V.; El-Beshlawy, A.; Hassab, H.; Agodoa, I.; Tonda, M.; Gray, S.; et al. Voxelotor in Adolescents and Adults with Sickle Cell Disease (HOPE): Long-Term Follow-up Results of an International, Randomised, Double-Blind, Placebo-Controlled, Phase 3 Trial. The Lancet Haematology 2021, 8, e323–e333. [Google Scholar] [CrossRef]
- Stankovic Stojanovic, K.; Lionnet, F. Lactate Dehydrogenase in Sickle Cell Disease. Clinica Chimica Acta 2016, 458, 99–102. [Google Scholar] [CrossRef]
- Kato, G.J.; McGowan, V.; Machado, R.F.; Little, J.A.; Taylor, J.; Morris, C.R.; Nichols, J.S.; Wang, X.; Poljakovic, M.; Morris, S.M.; et al. Lactate Dehydrogenase as a Biomarker of Hemolysis-Associated Nitric Oxide Resistance, Priapism, Leg Ulceration, Pulmonary Hypertension, and Death in Patients with Sickle Cell Disease. Blood 2006, 107, 2279–2285. [Google Scholar] [CrossRef]
- Kato, G.J.; Nouraie, S.M.; Gladwin, M.T. Lactate Dehydrogenase and Hemolysis in Sickle Cell Disease. Blood 2013, 122, 1091–1092. [Google Scholar] [CrossRef] [PubMed]
- van Vuren, A.J.; Minniti, C.P.; Mendelsohn, L.; Baird, J.H.; Kato, G.J.; van Beers, E.J. Lactate Dehydrogenase to Carboxyhemoglobin Ratio as a Biomarker of Heme Release to Heme Processing Is Associated with Higher Tricuspid Regurgitant Jet Velocity and Early Death in Sickle Cell Disease. American journal of hematology 2021, 96, E315–E318. [Google Scholar] [CrossRef] [PubMed]
- Kaur, K.; Huang, Y.; Raman, S.V.; Kraut, E.; Desai, P. Myocardial Injury and Coronary Microvascular Disease in Sickle Cell Disease. Haematologica 2021, 106, 2018. [Google Scholar] [CrossRef]
- Sachdev, V.; Rosing, D.R.; Thein, S.L. Cardiovascular Complications of Sickle Cell Disease. Trends in Cardiovascular Medicine 2020, 31, 187–193. [Google Scholar] [CrossRef] [PubMed]
- Akkus, N.I.; Rajpal, S.; Hilbun, J.; Dwary, A.; Smith, T.R.; Mina, G.; Reddy, P.C. Troponin Elevation in Sickle Cell Disease. Medical Principles and Practice 2021, 30, 437–442. [Google Scholar] [CrossRef] [PubMed]
- Agrawal, R.K.; Patel, R.K.; shah, V.; Nainiwal, L.; Trivedi, B. Hydroxyurea in Sickle Cell Disease: Drug Review. Indian Journal of Hematology and Blood Transfusion 2013, 30, 91–96. [Google Scholar] [CrossRef]
- Yawn, B.P.; Buchanan, G.R.; Afenyi-Annan, A.N.; Ballas, S.K.; Hassell, K.L.; James, A.H.; Jordan, L.; Lanzkron, S.M.; Lottenberg, R.; Savage, W.J.; et al. Management of Sickle Cell Disease: Summary of the 2014 Evidence-Based Report by Expert Panel Members. JAMA 2014, 312, 1033–1048. [Google Scholar] [CrossRef]
- Reham Wagdy; Suliman, H.; Bashayer Bamashmose; Abrar Aidaroos; Haneef, Z.; Arunima Samonti; Awn, F. Subclinical Myocardial Injury during Vaso-Occlusive Crisis in Pediatric Sickle Cell Disease. European Journal of Pediatrics 2018, 177, 1745–1752. [CrossRef]
- Azmet, F.R.; Al-Kasim, F.; Alashram, W.M.; Siddique, K. The Role of Hydroxyurea in Decreasing the Occurrence of Vasso-Occulusive Crisis in Pediatric Patients with Sickle Cell Disease at King Saud Medical City in Riyadh, Saudi Arabia. Saudi Medical Journal 2020, 41, 46–52. [Google Scholar] [CrossRef]
- Alkhalifah, S.A.; Alanazi, M.; Almasaoud, M.A.; Al-Malki, H.S.; Al-Murdhi, F.M.; Al-hazzaa, M.S.; Al-Mufarrij, S.M.; Albabtain, M.A.; Alshiakh, A.A.; AlRuthia, Y. The Impact of Hydroxyurea on the Rates of Vaso–Occlusive Crises in Patients with Sickle Cell Disease in Saudi Arabia: A Single–Center Study. BMC Emergency Medicine 2022, 22. [Google Scholar] [CrossRef]
- Akaba, Kingsley, et al. “Transfusion Therapy in Sickle Cell Disease.” Journal of Blood & Lymph, 2019. Available online: www.hilarispublisher.com/open-access/transfusion-therapy-in-sickle-cell-disease.pdf.
- Pannu, R.; Zhang, J.; Andraws, R.; Armani, A.; Patel, P.; Mancusi-Ungaro, P. Acute Myocardial Infarction in Sickle Cell Disease: A Systematic Review. Critical Pathways in Cardiology 2008, 7, 133–138. [Google Scholar] [CrossRef] [PubMed]
- Marouf, R. Blood Transfusion in Sickle Cell Disease. Hemoglobin 2011, 35, 495–502. [Google Scholar] [CrossRef] [PubMed]
- Mansi, I.A.; Rosner, F. Myocardial Infarction in Sickle Cell Disease. Journal of the National Medical Association 2002, 94, 448–452. [Google Scholar] [PubMed]
- Voskaridou, E.; Christoulas, D.; Terpos, E. Sickle-Cell Disease and the Heart: Review of the Current Literature. British Journal of Haematology 2012, 157, 664–673. [Google Scholar] [CrossRef]
- Dosunmu, A.; Akinbami, A.; Uche, E.; Adediran, A.; John-Olabode, S. Electrocardiographic Study in Adult Homozygous Sickle Cell Disease Patients in Lagos, Nigeria. Journal of Tropical Medicine 2016, 2016, 1–5. [Google Scholar] [CrossRef]
- Ali, G.O.M.; Abdal Gader, Y.S.; Abuzedi, E.S.; Attalla, B.A.I. Cardiac Manifestations of Sickle Cell Anaemia in Sudanese Children. Sudanese Journal of Paediatrics 2012, 12, 70–78. [Google Scholar]
- Srisuwananukorn, A.; Raslan, R.; Zhang, X.; Shah, B.N.; Han, J.; Gowhari, M.; Molokie, R.E.; Gordeuk, V.R.; Saraf, S.L. Clinical, Laboratory, and Genetic Risk Factors for Thrombosis in Sickle Cell Disease. Blood Advances 2020, 4, 1978–1986. [Google Scholar] [CrossRef]
- Charneski, L.; Congdon, H.B. Effects of Antiplatelet and Anticoagulant Medications on the Vasoocclusive and Thrombotic Complications of Sickle Cell Disease: A Review of the Literature. American Journal of Health-System Pharmacy 2010, 67, 895–900. [Google Scholar] [CrossRef]
| Variable | Groups | n (%) |
| Gender | Male | 126 (46.7) |
| Female | 144 (53.3) | |
| Age group | Less than 21 | 18 (6.7) |
| From 21 to 30 | 108 (40) | |
| From 31 to 40 | 101 (37.4) | |
| From 41 to 50 | 39 (14.4) | |
| More than 50 | 4 (1.5) | |
| Blood Group | A- | 4 (1.5) |
| A+ | 68 (25.2) | |
| AB+ | 11 (4.1) | |
| B- | 2 (0.7) | |
| B+ | 33 (12.2) | |
| O- | 8 (3.0) | |
| O+ | 144 (53.3) | |
| Nationality | Chadian | 21 (7.7) |
| Nigerian | 2 (0.7) | |
| Pakistani | 4 (1.5) | |
| Saudi | 163 (60.4) | |
| Sudanese | 11 (4.1) | |
| Syrian | 1 (0.4) | |
| Yemeni | 68 (25.2) | |
| Complication Related to the sickle cell disease | No | 181 (67) |
| Yes | 89 (33) | |
| Known chronic illness | Thalassemia | 78 (29) |
| Hypertension | 13 (4.8) | |
| Hepatitis C | 11 (4) | |
| Kidney disease | 10 (3.7) | |
| Epilepsy | 8 (3) | |
| Hypothyroidism | 7 (2.6) | |
| Asthma | 7 (2.6) | |
| Diabetes | 6 (2.2) | |
| Liver cirrhosis | 3 (1.1) | |
| Glucose-6-phosphate dehydrogenase deficiency | 3 (1.1) | |
| Heart Failure | 3 (1.1) | |
| Burkitt lymphoma | 2 (0.8) | |
| Ischemic heart disease | 1 (0.4) | |
| Crohn’s disease | 1 (0.4) | |
| Pulmonary hypertension | 1 (0.4) | |
| Lung fibrosis | 1 (0.4) | |
| Hereditary spherocytosis | 1 (0.4) | |
| Calculus of kidney | 1 (0.4) | |
| Dyslipidemia | 1 (0.4) | |
| Seckel syndrome | 1 (0.4) | |
| Lupus nephritis | 1 (0.4) | |
| Phenylketonuria | 1 (0.4) | |
| Calculus of gallbladder | 1 (0.4) | |
| Number of emergency room visits per year | 0 | |
| 1-3 | ||
| 4-12 | ||
| >12 |
| Variable | Group | |||
|---|---|---|---|---|
| N/A | Low | Normal | High | |
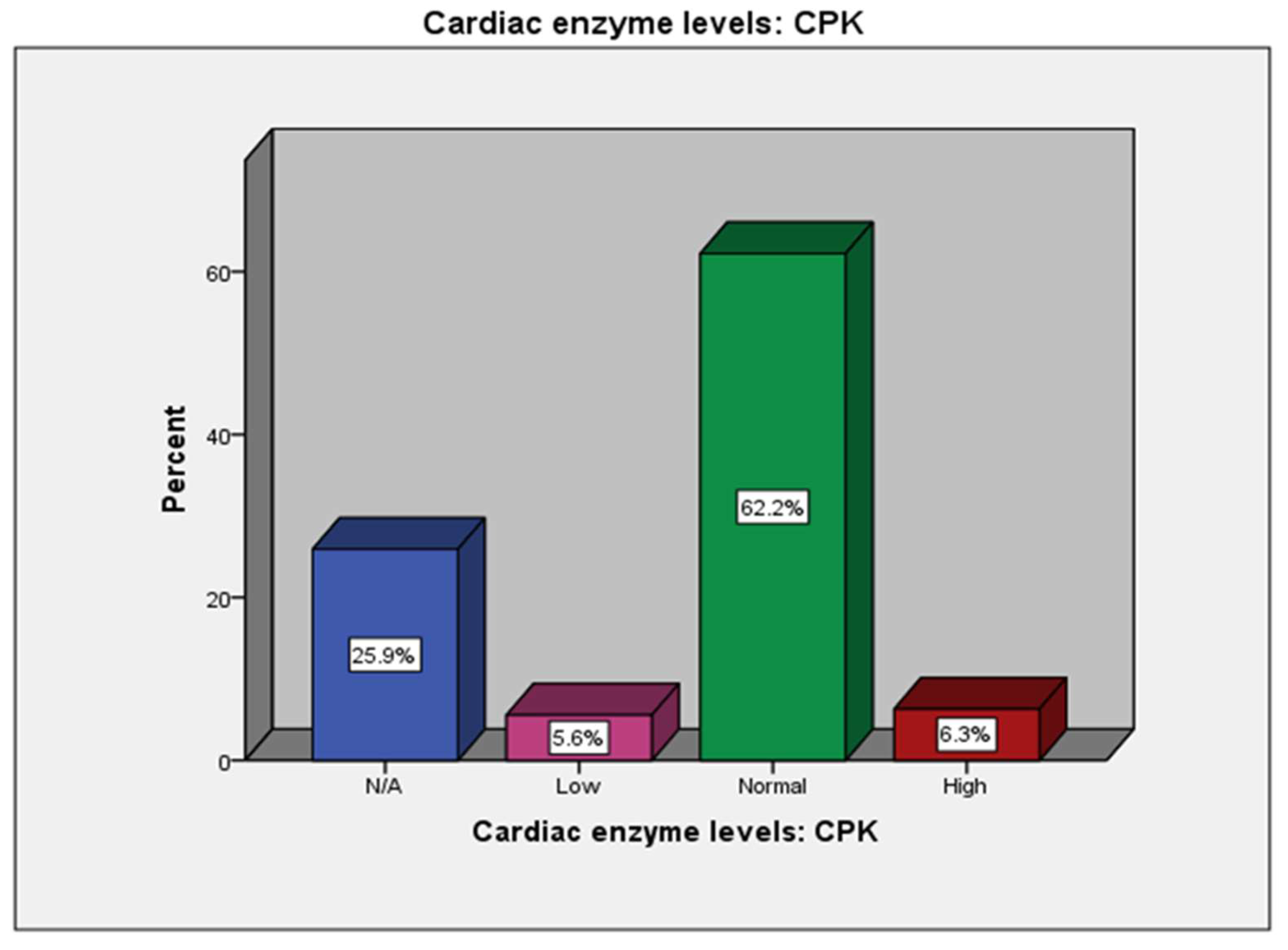
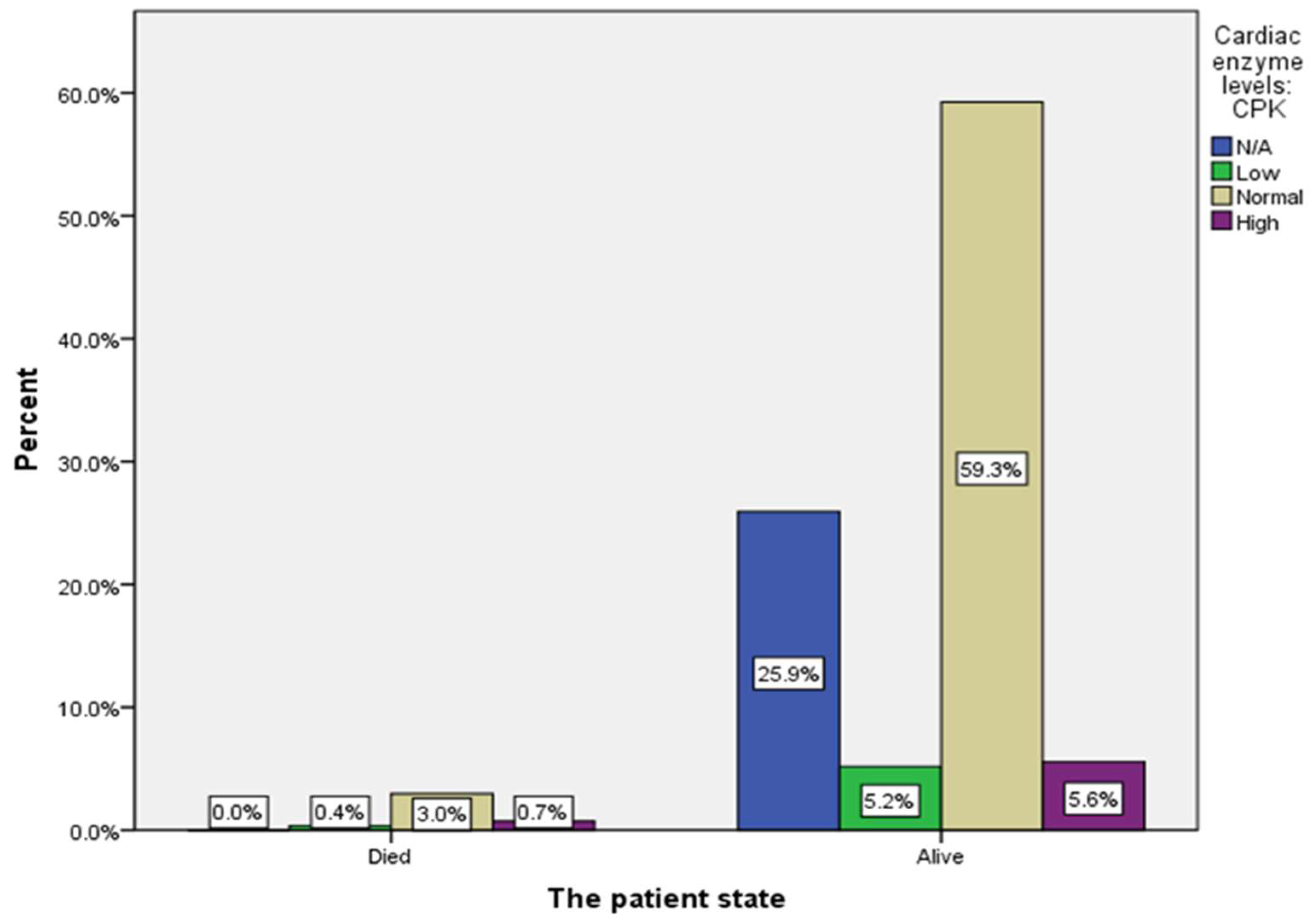
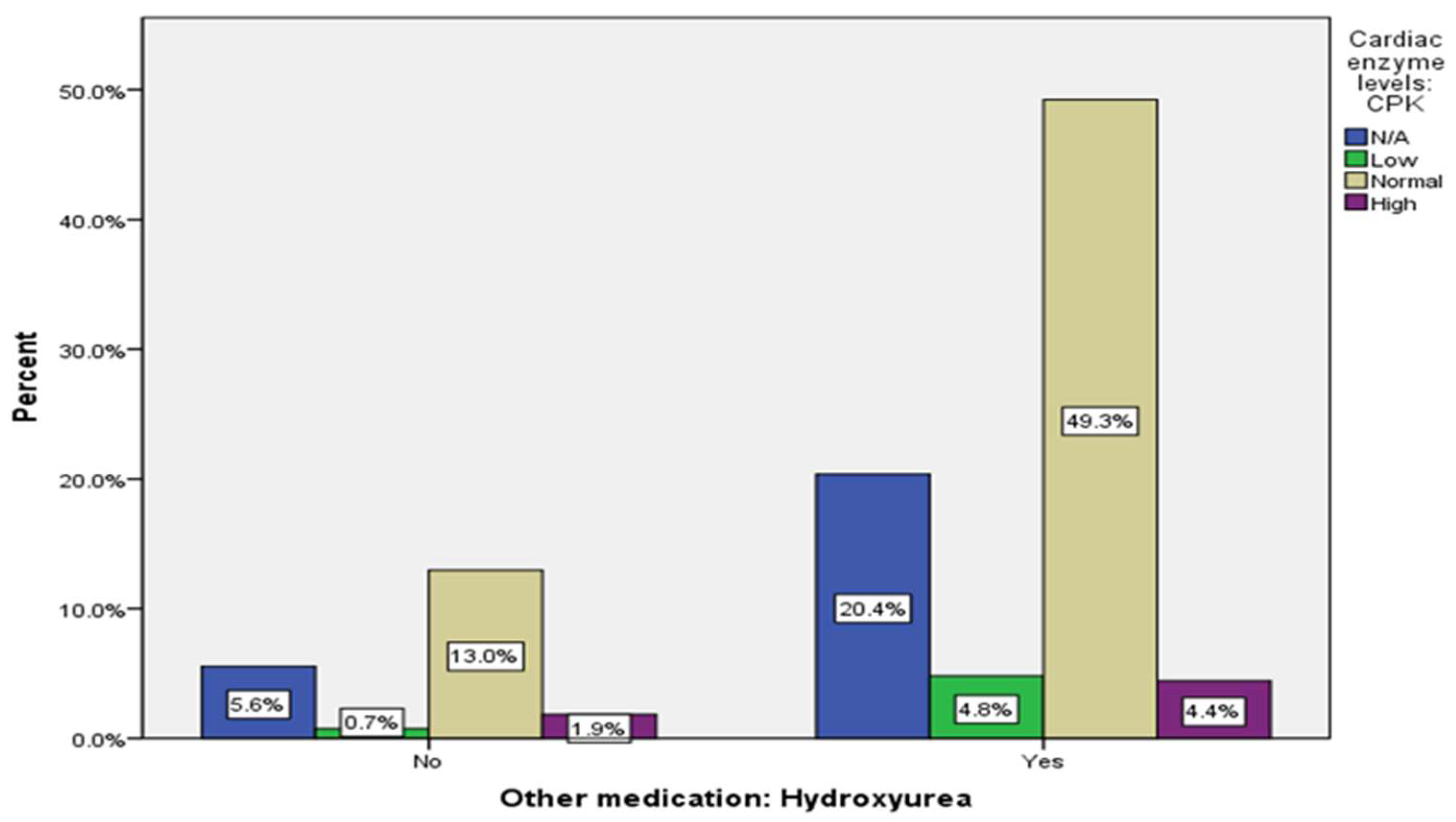
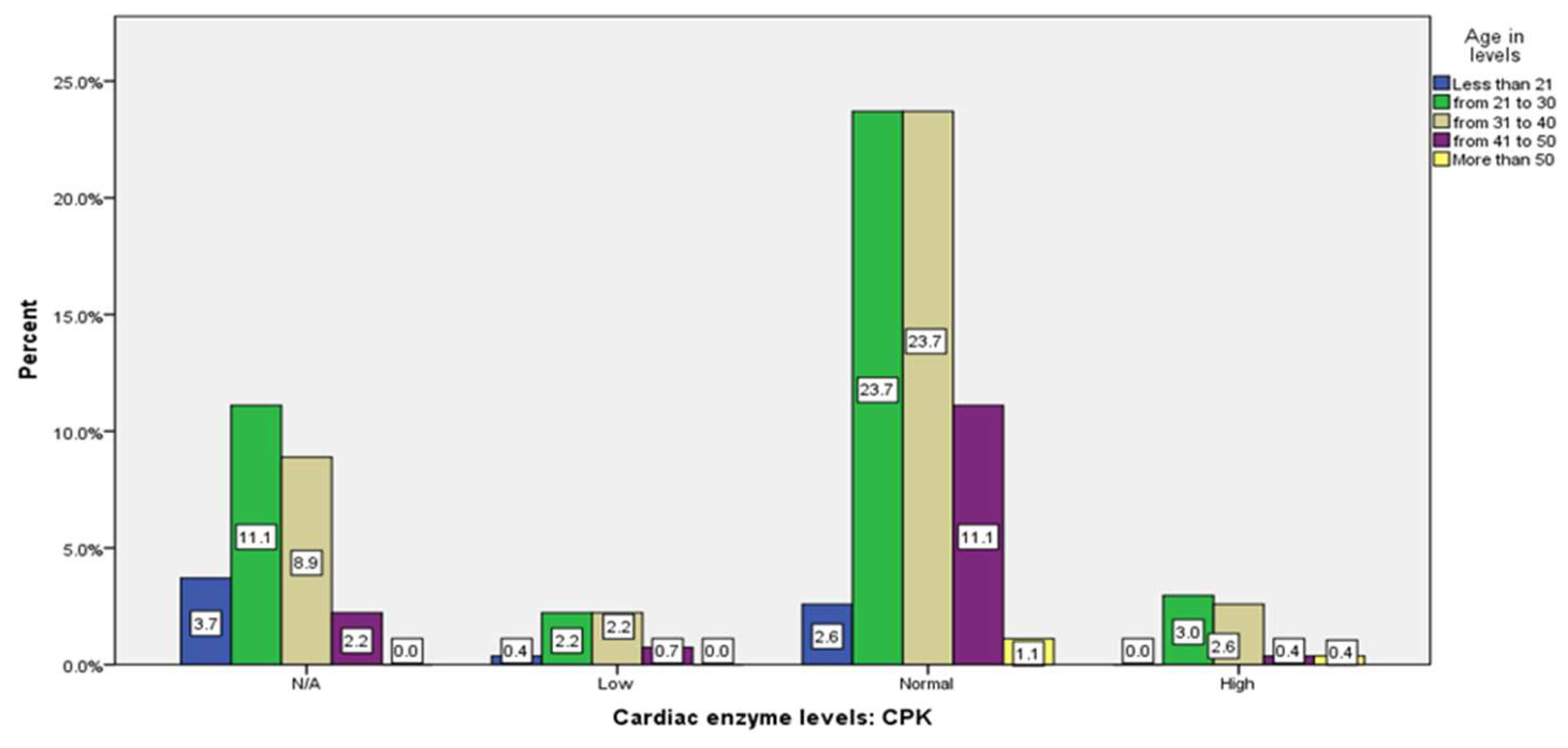
| Cardiac enzyme levels: CPK | 70 (25.9%) |
15 (5.6%) |
168 (62.2%) |
17 (6.3%) |
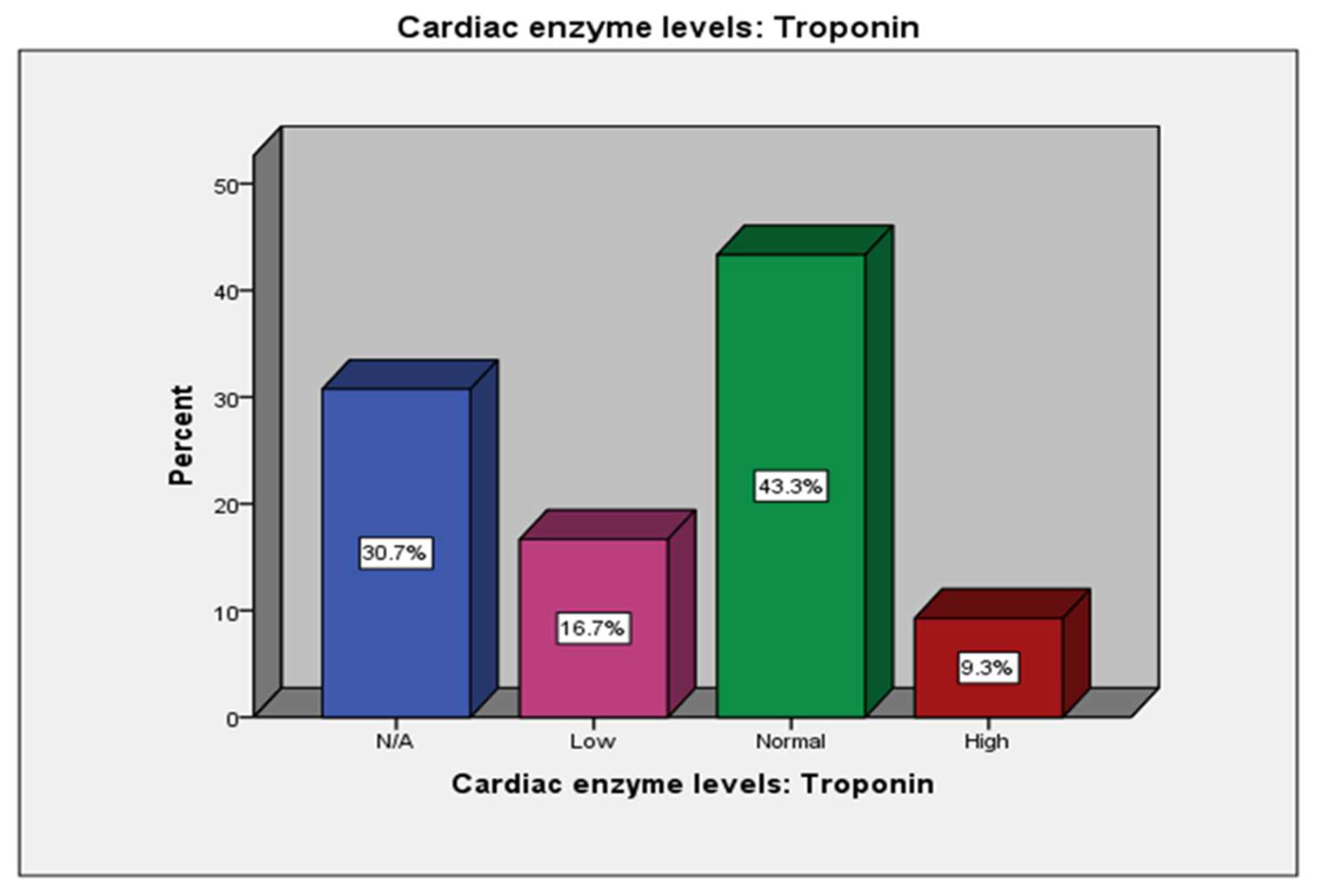
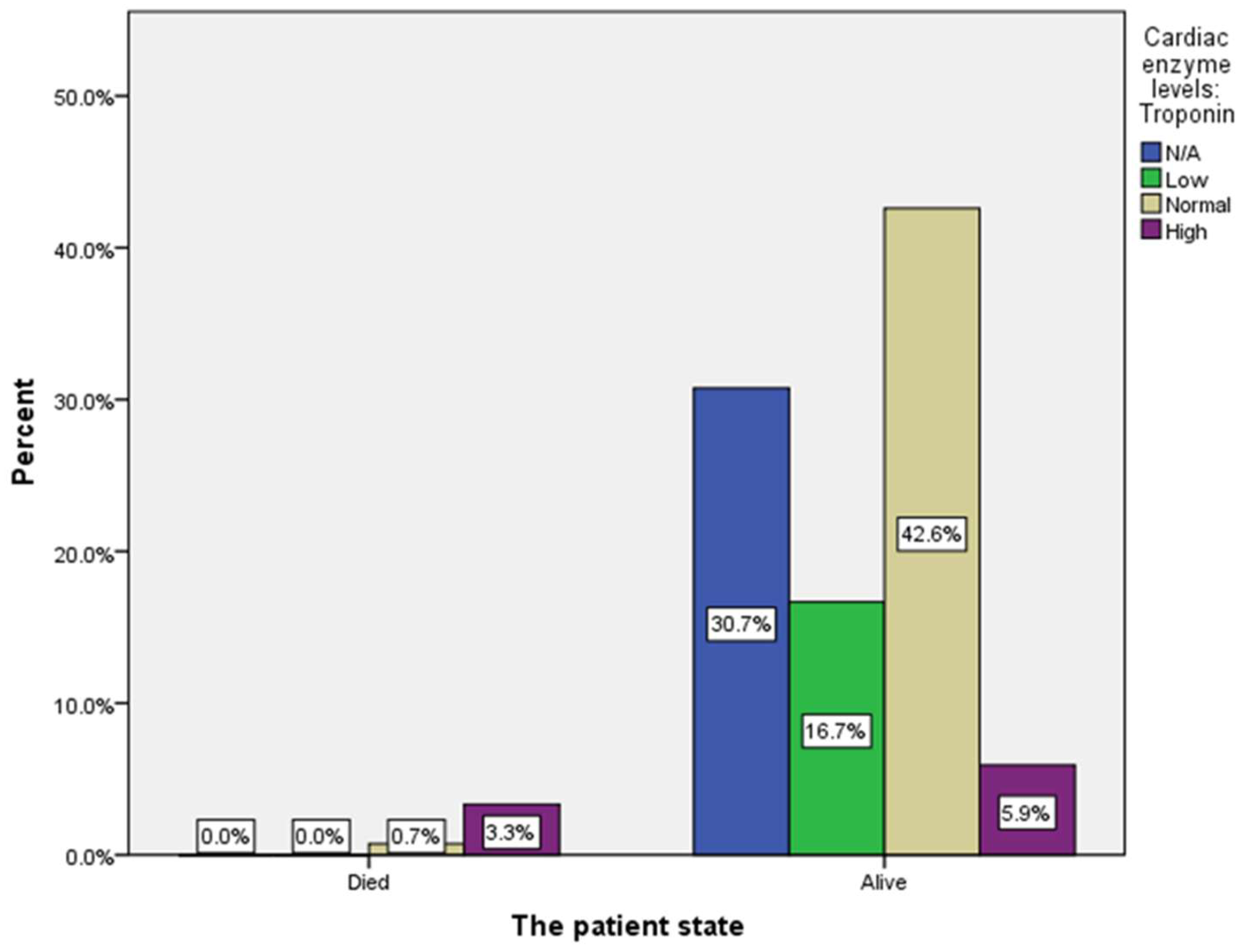
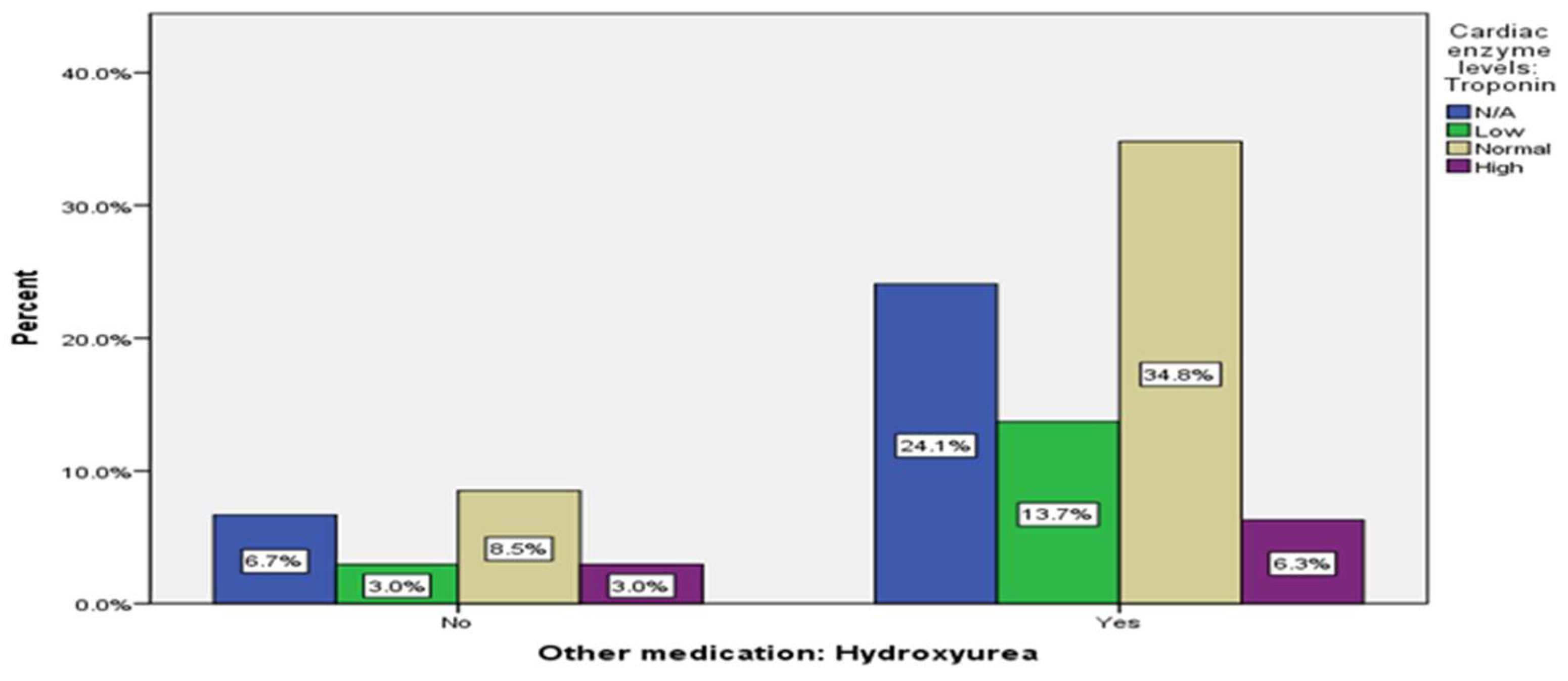
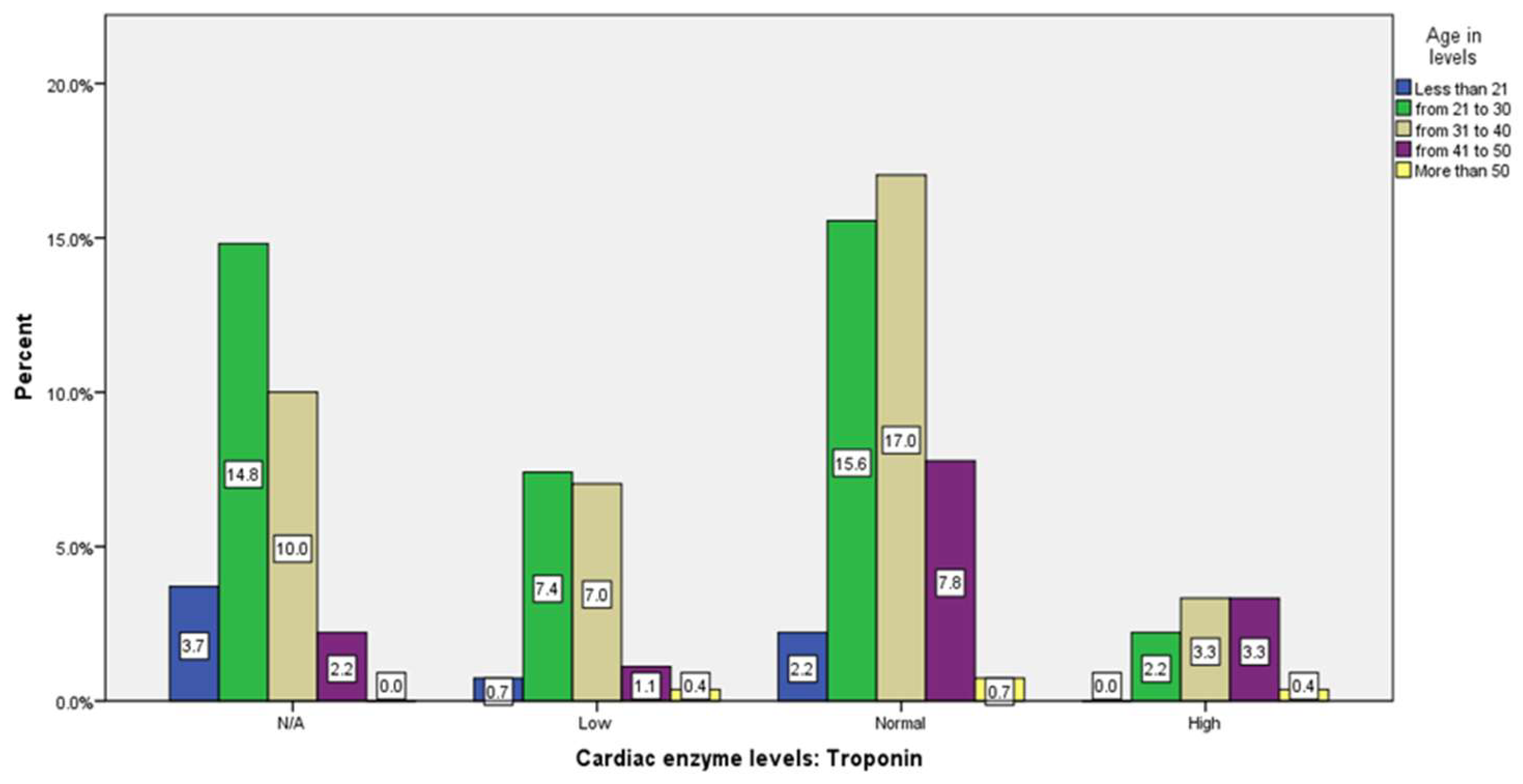
| Cardiac enzyme levels: Troponin | 83 (30.7%) |
45 (16.7%) |
117 (43.3%) |
25 (9.3%) |
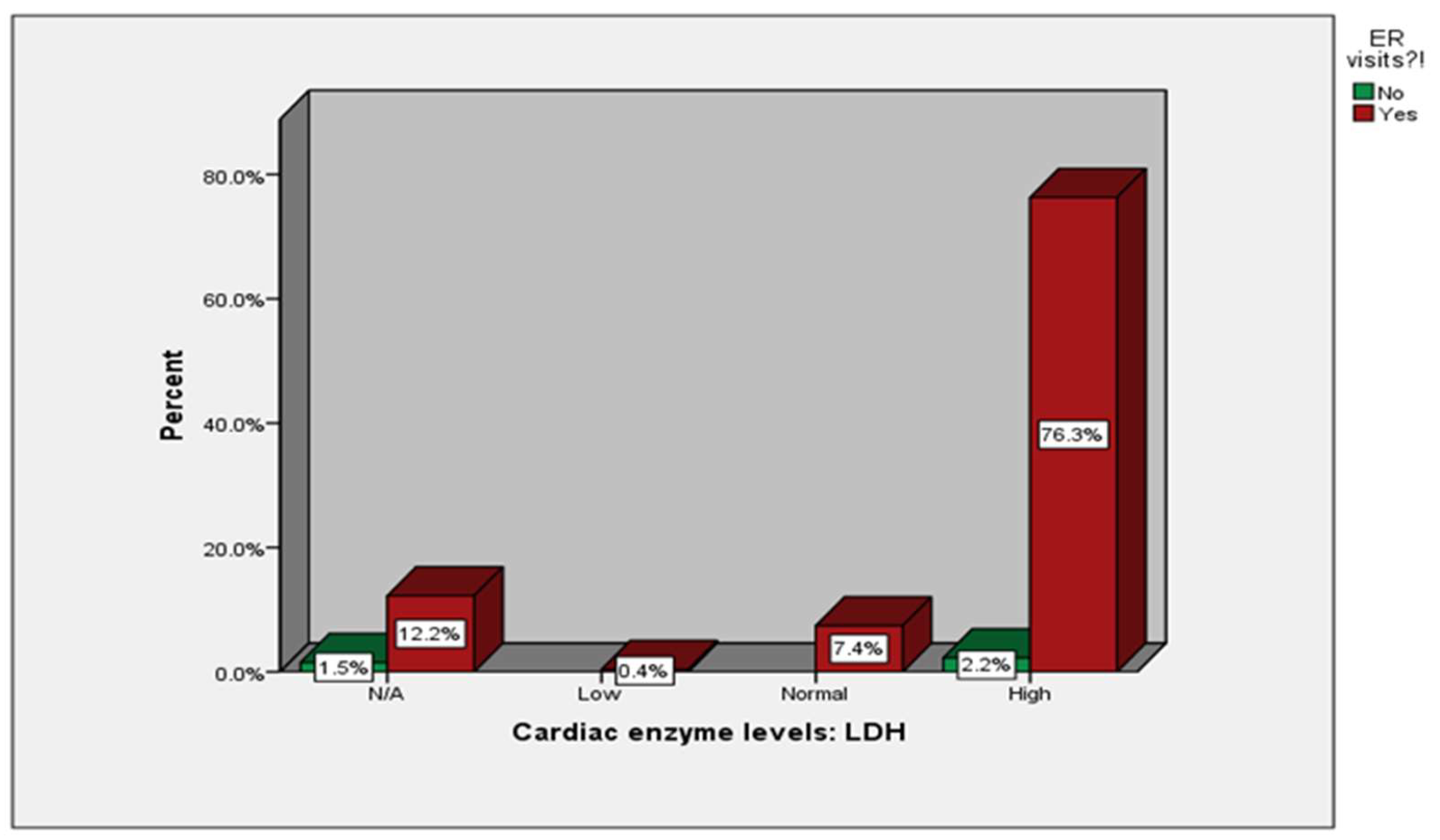
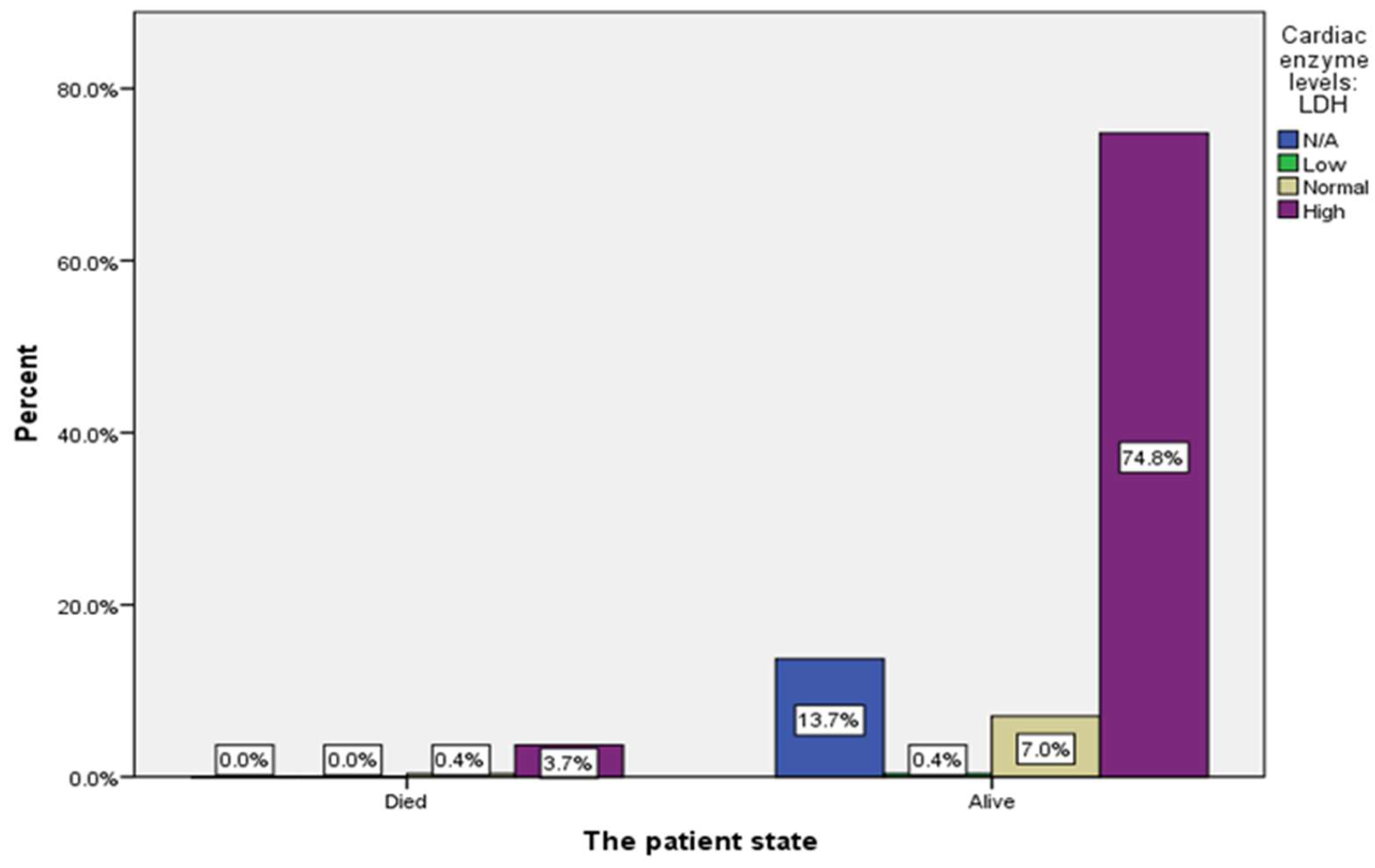
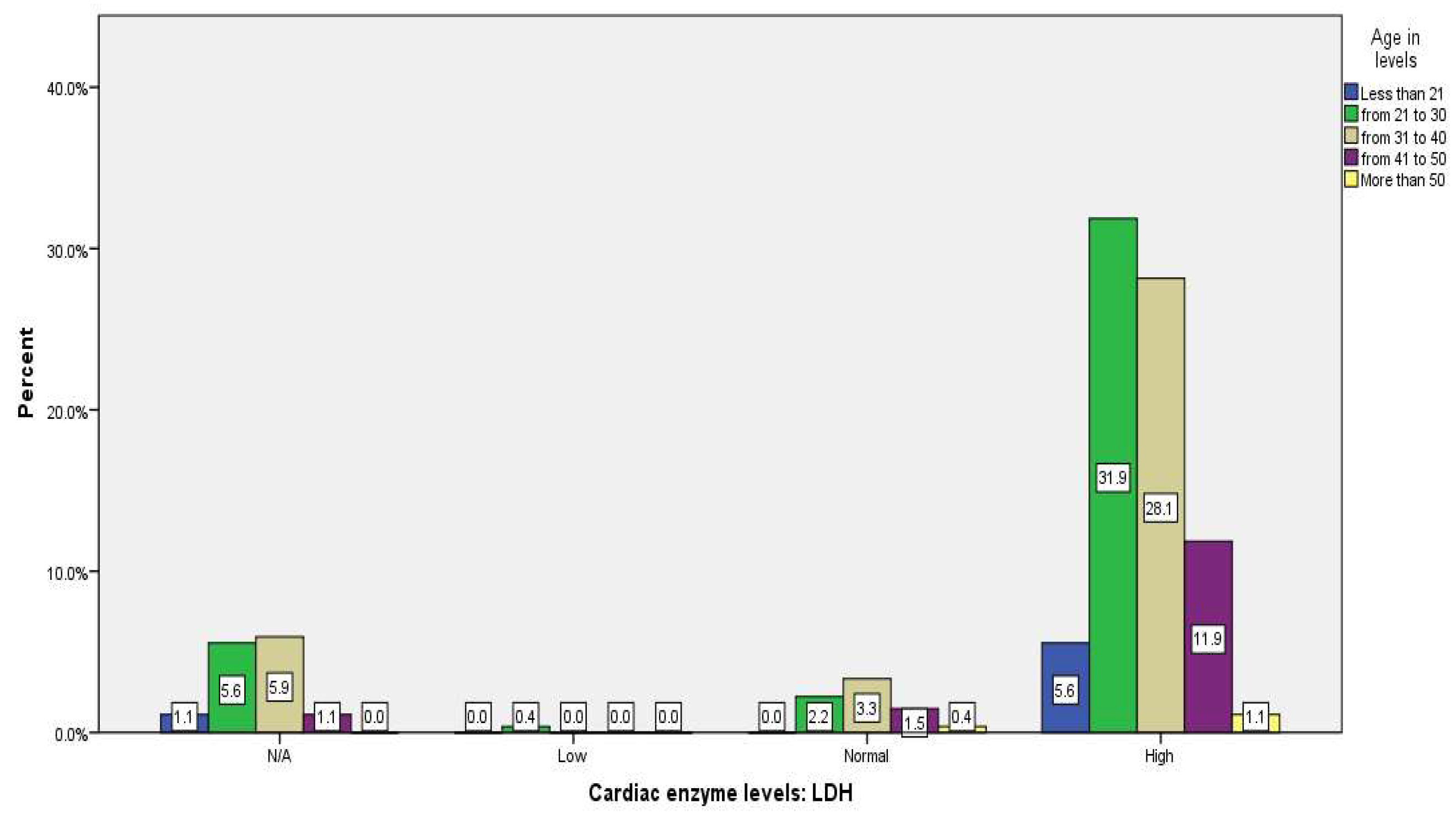
| Cardiac enzyme levels: LDH | 37 (13.7%) |
1 (0.4%) |
20 (7.4%) |
212 (78.5%) |
| Variable | Group | ER visits | Spearman’s Correlation | The patient's state | Rank biserial | Using Hydroxyurea | Rank biserial | Needing blood transfusion | Rank biserial | ECG findings | Rank biserial | Age Levels | Spearman’s | P-value | Antiplatelets/ Anticoagulant medication | Rank biserial | ||||||||||||||||
| No | Yes | Died | Alive | Correlation | Significant | No | Yes | Correlation | Significant | No | Yes | Correlation | Significant | N/A | Abnormal | Normal | Correlation | Significant | Less than 21 | 21-30 | 31-40 | 41-50 | More than 50 | Correlation coefficient | P-value | No | Yes | Correlation | Significant | |||
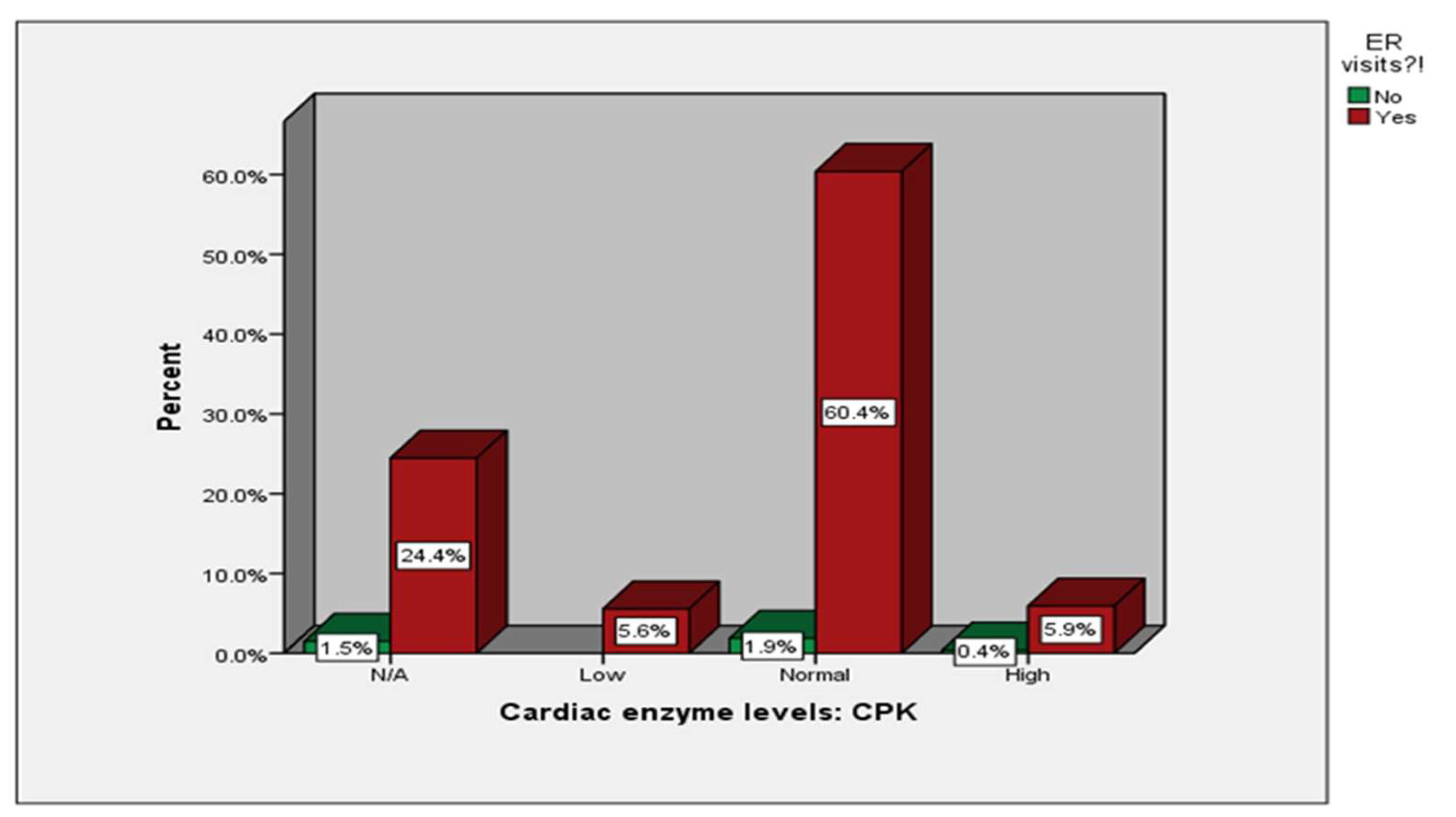
| Cardiac enzyme levels: CPK | N/A | 4 (1.5%) |
66 (24.4%) |
0.0001 |
0 (0%) |
70 (25.9%) |
0.049 | 0.489 | 15 (5.6%) |
55 (20.4%) |
0.079 | 0.265 | 14 (5.2%) |
56 (20.7%) |
0.011 | 0.876 | 67 (24.8%) |
0 (0%) |
3 (1.1%) |
0.071 | 0.640 | 10 (3.7%) |
30 (11.1%) |
24 (8.9%) |
6 (2.2%) |
0 (0%) |
0.18 | 0.003** | 20 (7.4%) |
50 (18.5%) |
0.059 | 0.410 |
| Low | 0 (0%) |
15 (5.6%) |
1 (0.4%) |
14 (5.2%) |
2 (0.7%) |
13 (4.8%) |
2 (0.7%) |
13 (4.8%) |
12 (4.4%) |
2 (0.7%) |
1 (0.4%) |
1 (0.4%) |
6 (2.2%) |
6 (2.2%) |
2 (0.7%) |
0 (0%) |
0 (0%) |
15 (5.6%) |
||||||||||||||
| Normal | 5 (1.9%) |
163 (60.4%) |
8 (3%) |
160 (59.3%) |
35 (13%) |
133 (49.3%) |
28 (10.4%) |
140 (51.9%) |
126 (46.7%) |
30 (11.1%) |
12 (4.4%) |
7 (2.6%) |
64 (23.7%) |
64 (23.7%) |
30 (11.1%) |
3 (1.1%) |
7 (2.6%) |
161 (59.6%) |
||||||||||||||
| High | 1 (0.4%) |
16 (5.9%) |
2 (0.7%) |
15 (5.6%) |
5 (1.9%) |
12 (4.4%) |
2 (0.7%) |
15 (5.6%) |
16 (5.9%) |
1 (0.4%) |
0 (0%) |
0 (0%) |
8 (3%) |
7 (2.6%) |
1 (0.4%) |
1 (0.4%) |
1 (0.4%) |
16 (5.9%) |
||||||||||||||
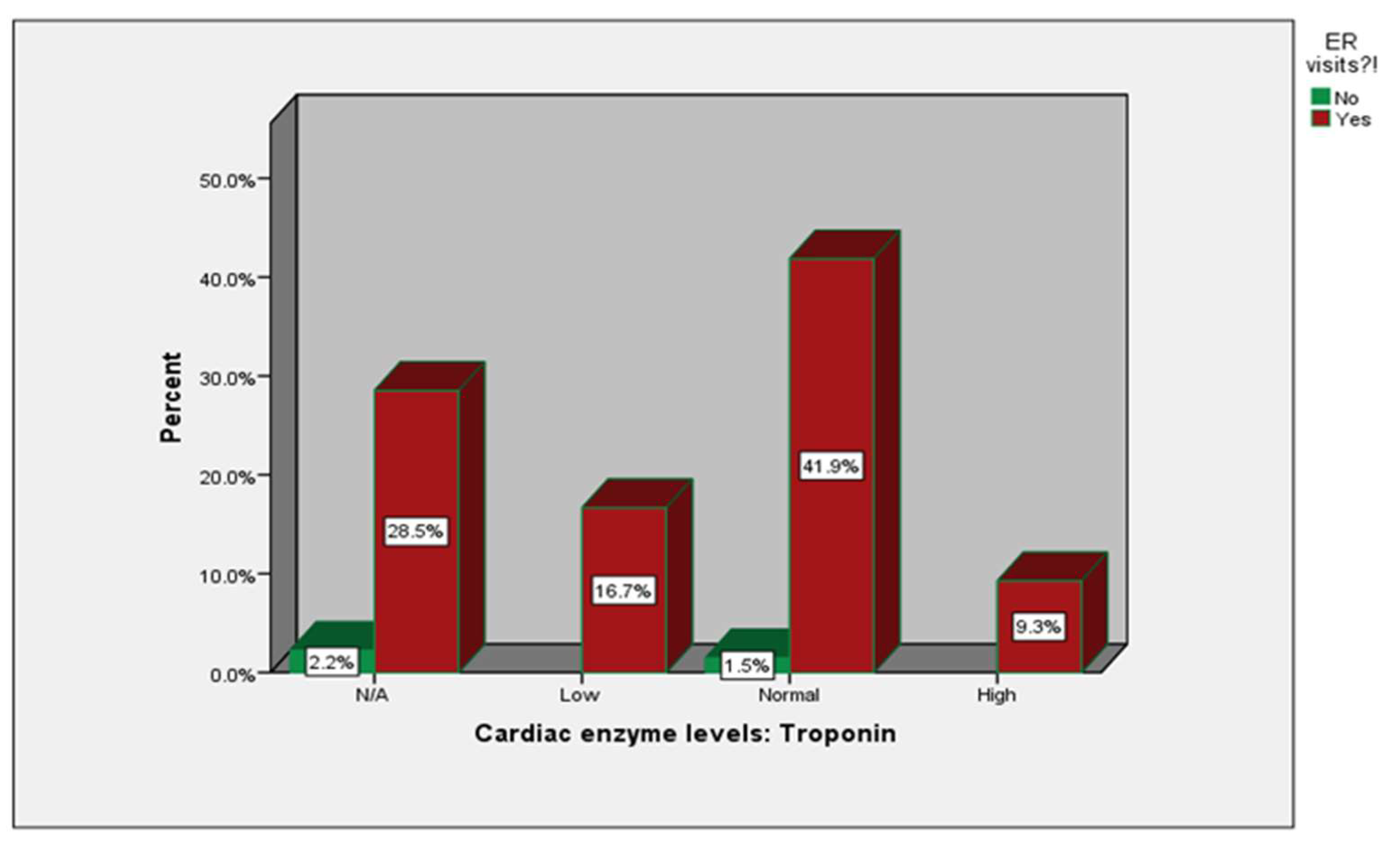
| Cardiac enzyme levels: Troponin | N/A | 6 (2.2%) |
77 (28.5%) |
0.0001 | 0 (0%) |
83 (30.7%) |
0.384 | 0.0001** | 18 (6.7%) |
65 (24.1%) |
0.088 | 0.231 | 17 (6.3%) |
66 (24.4%) |
0.102 |
0.164 |
78 (28.9%) |
2 (0.7%) |
3 (4.4%) |
0.232 | 0.130 | 10 (3.7%) |
40 (14.8%) |
27 (10%) |
6 (2.2%) |
0 (0%) |
0.29 |
0.0001 |
21 (7.8%) |
62 (23%) |
0.043 | 0.564 |
| Low | 0 (0%) |
45 (16.7%) |
0 (0%) |
45 (16.7%) |
8 (3%) |
37 (13.7%) |
4 (1.5%) |
41 (15.2%) |
32 (11.9%) |
7 (2.6%) |
6 (2.2%) |
2 (0.7%) |
20 (7.4%) |
19 (7%) |
3 (1.1%) |
1 (0.4%) |
0 (0%) |
45 (16>7%) |
||||||||||||||
| Normal | 4 (1.5%) |
113 (41.9%) |
2 (0.7%) |
115 (42.6%) |
23 (8.5%) |
94 (34.8%) |
20 (7.4%) |
97 (35.9%) |
97 (35.9%) |
15 (5.6%) |
5 (1.9%) |
6 (2.2%) |
42 (15.6%) |
46 (17%) |
21 (7.8%) |
2 (0.7%) |
7 (2.6%) |
110 (40>7%) |
||||||||||||||
| High | 0 (0%) |
25 (9.3%) |
9 (3.3%) |
16 (5.9%) |
8 (3%) |
17 (6.3%) |
5 (1.9%) |
20 (7.4%) |
14 (5.2%) |
9 (3.3%) |
2 (0.7%) |
0 (0%) |
6 (2.2%) |
9 (3.3%) |
9 (3.3%) |
1 (0.4%) |
0 (0%) |
25 (9.3%) |
||||||||||||||
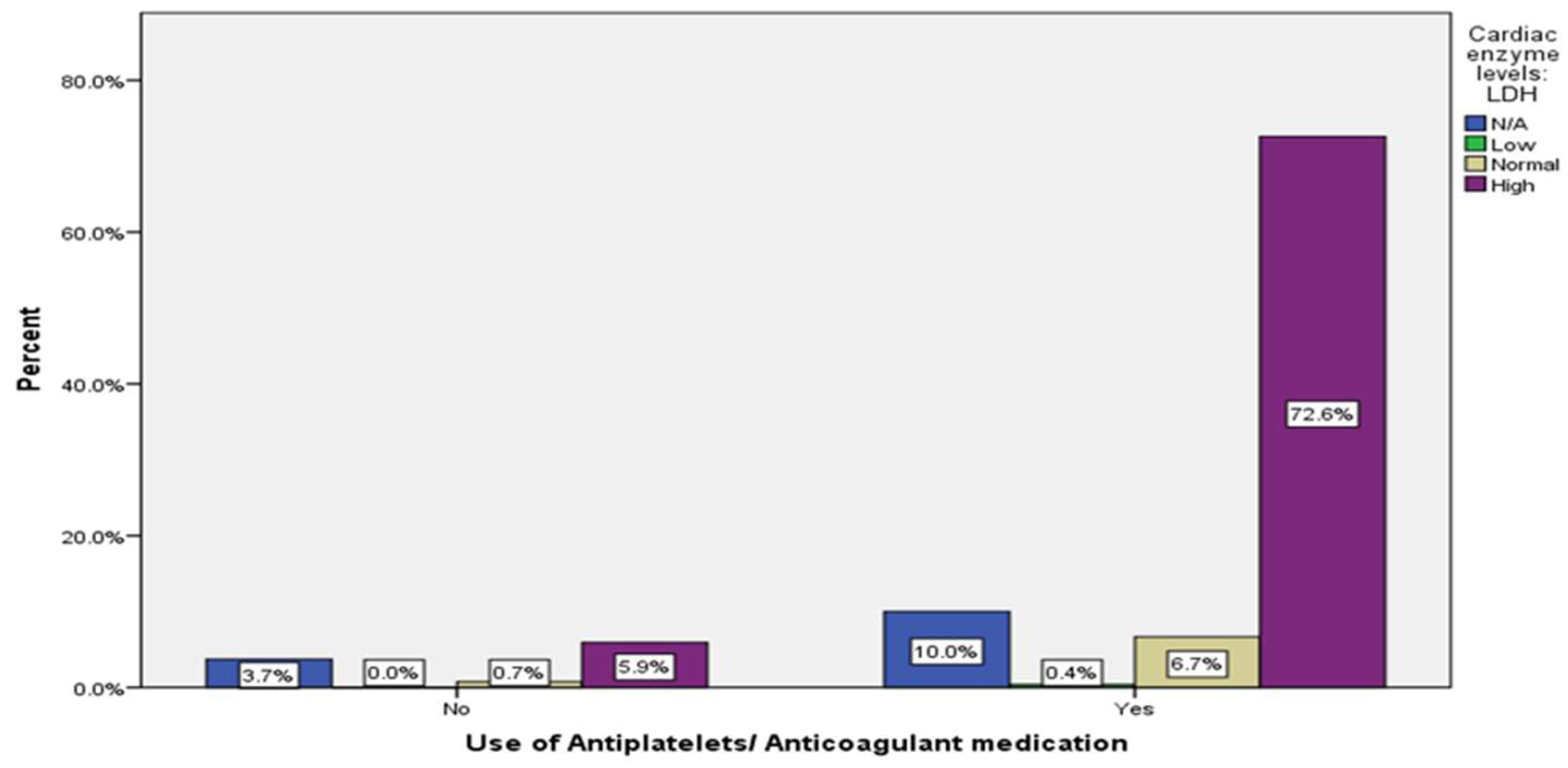
| Cardiac enzyme levels: LDH | N/A | 4 (1.5%) |
33 (12.2%) |
0.0001 | 0 (0%) |
37 (13.7%) |
0.0001 | 0.996 | 9 (3.3%) |
28 (10.4%) |
0.024 | 0.714 | 12 (4.4%) |
25 (9.3%) |
0.039 |
0.554 |
36 (13.3%) |
0 (0%) |
1 (0.4%) |
0.024 | 0.872 | 3 (1.1%) |
15 (5.6%) |
16 (5.9%) |
3 (1.1%) |
0 (0%) |
0.005 | 0.936 | 10 (3.7%) |
27 (10%) |
0.021 | 0.753 |
| Low | 0 (0%) |
1 (0.4%) |
0 (0%) |
1 (0.4%) |
0 (0%) |
1 (0.4%) |
0 (0%) |
1 (0.4%) |
1 (0.4%) |
0 (0%) |
0 (0%) |
0 (0%) |
1 (0.4%) |
0 (0%) |
0 (0%) |
0 (0%) |
0 (0%) |
1 (0.4%) |
||||||||||||||
| Normal | 0 (0%) |
20 (7.4%) |
1 (0.4%) |
19 (7%) |
5 (1.9%) |
15 (5.6%) |
4 (1.5%) |
16 (5.9%) |
13 (4.8%) |
5 (1.9%) |
2 (0.7%) |
0 (0%) |
6 (2.2%) |
9 (3.3%) |
4 (1.5%) |
1 (0.4%) |
2 (0.&%) |
18 (6.7%) |
||||||||||||||
| High | 10 (2.2%) |
206 (76.3%) |
10 (3.7%) |
202 (74.8%) |
43 (15.9%) |
169 (62.6%) |
30 (11.1%) |
182 (67.4%) |
171 (63.3%) |
28 (10.4%) |
13 (4.8%) |
15 (5.6%) |
86 (31.9%) |
76 (28.1%) |
32 (11.9%) |
3 (1.1%) |
16 (5.9%) |
196 (72.6%) |
||||||||||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




