Submitted:
10 August 2023
Posted:
11 August 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials
3. Methods
3.1. Solubility studies
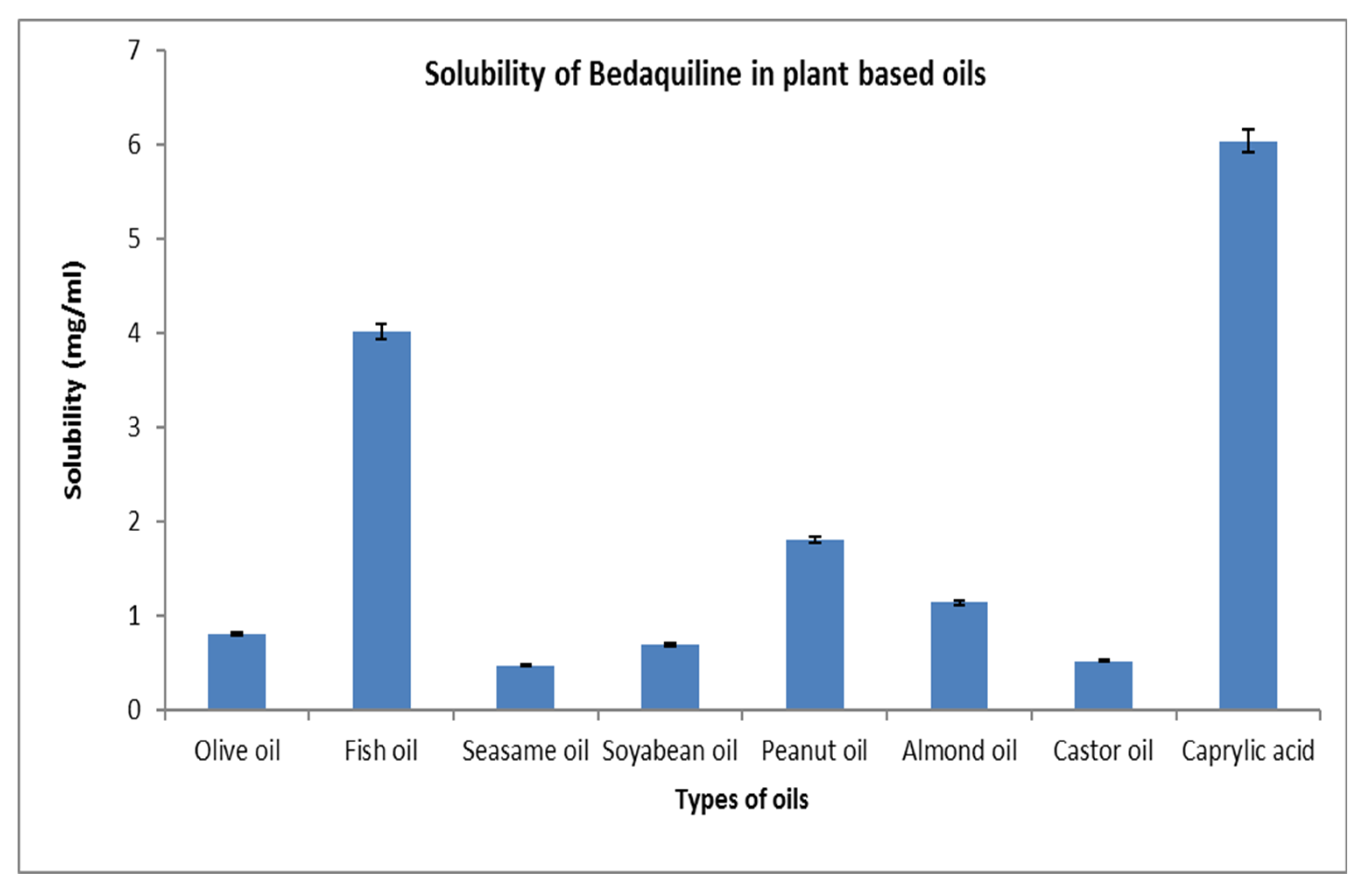
3.1.1. Selection of oil
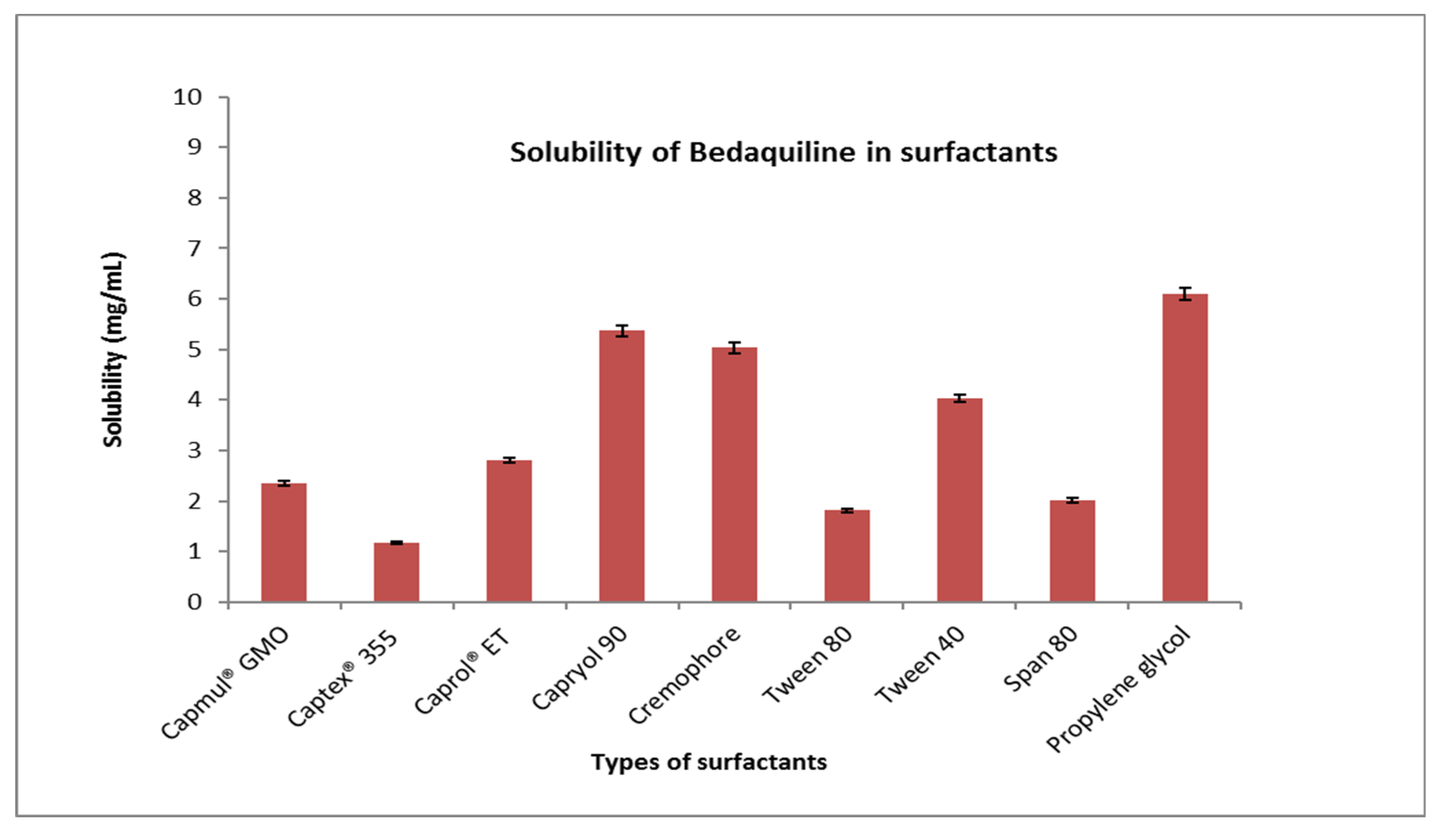
3.1.2. Selection of surfactant and co-surfactant
3.2. Pseudo-ternary phase diagram
3.3. Quality by design (QbD) approach incorporation
3.4. Risk assessment using Ishikawa
3.5. Formulation and optimization of SNEDDS using Box Behnken design
3.6. Characterization of SNEDDS
3.6.1. Droplet size, PdI, and zeta potential
3.6.2. Transmission electron microscopy (TEM)
3.6.3. Entrapment efficacy
3.6.4. Self-emulsification time
3.6.5. Dilution studies
3.7. In vitro drug release study
3.8. Stability studies
3.9. Cell toxicity studies
3.10. Statistical analysis
4. Results and discussion
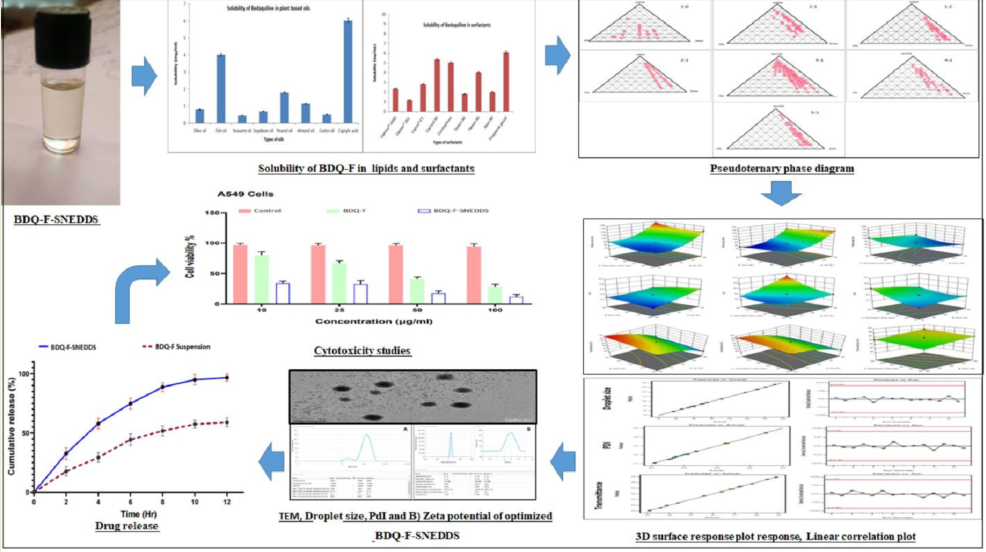
4.1. Solubility study
4.2. Pseudoternary phase diagrams
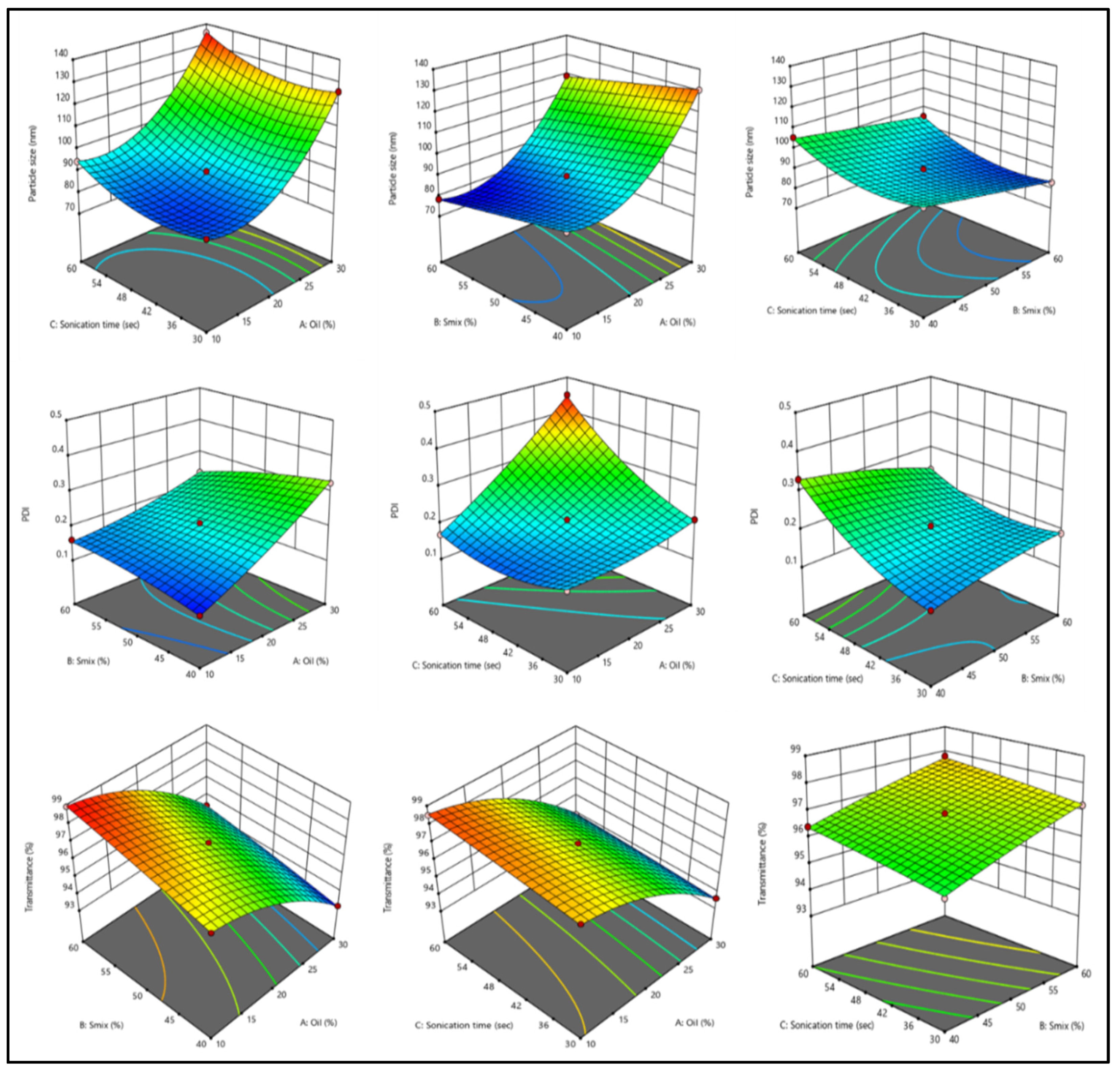
4.3. Optimization using BBD
4.3.1. Effect of independent variables on droplet size
4.3.2. Effect of independent variables on PdI
4.3.3. Effect of independent variables on transmittance
4.4. Validation and Point prediction
4.5. Characterization
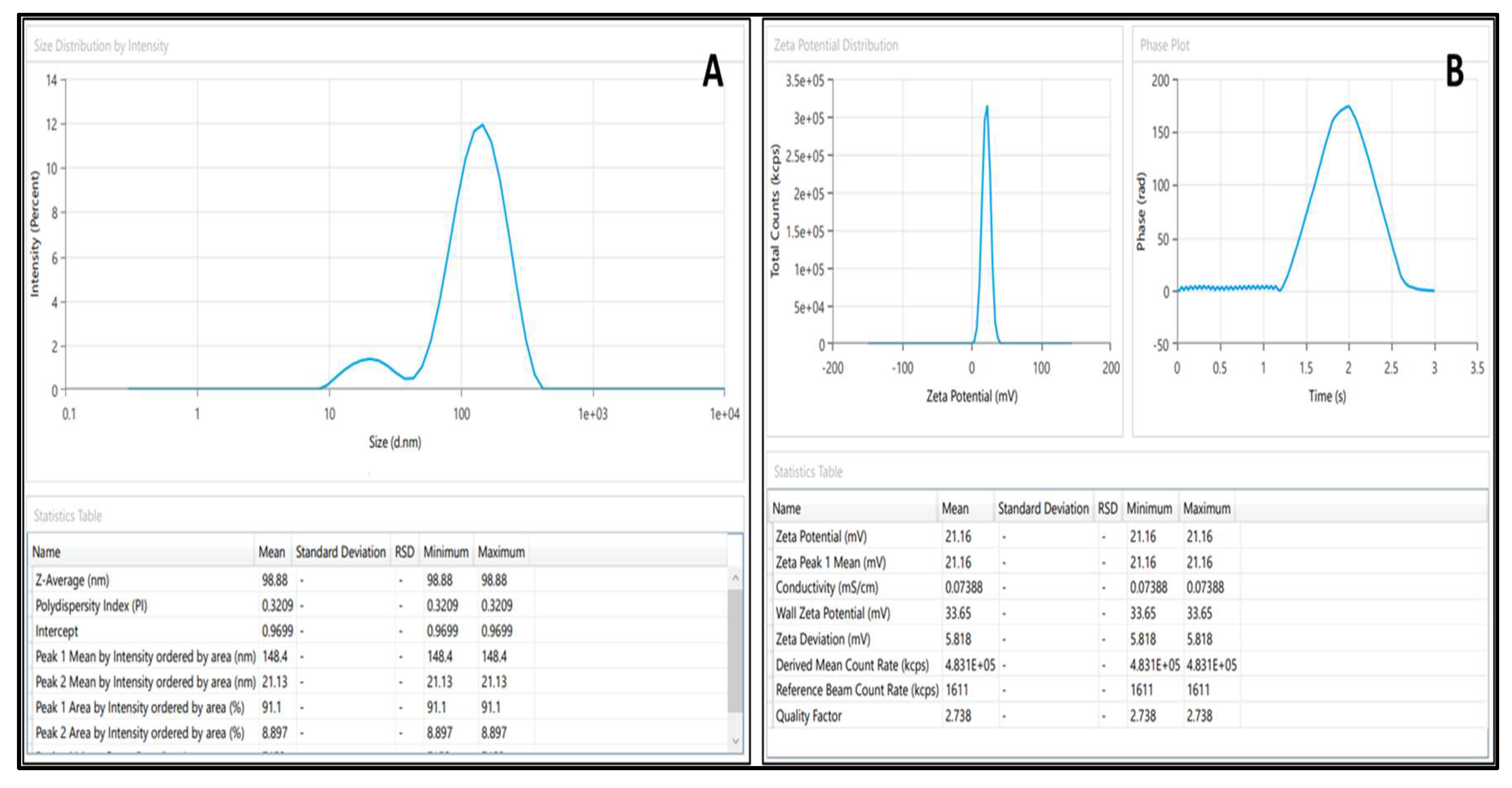
4.5.1. Droplet size and PdI
4.5.2. Zeta potential
4.5.3. Transmission electron microscopy
4.5.4. Entrapment efficacy
4.5.5. Self-emulsification time
4.5.6. Dilution study
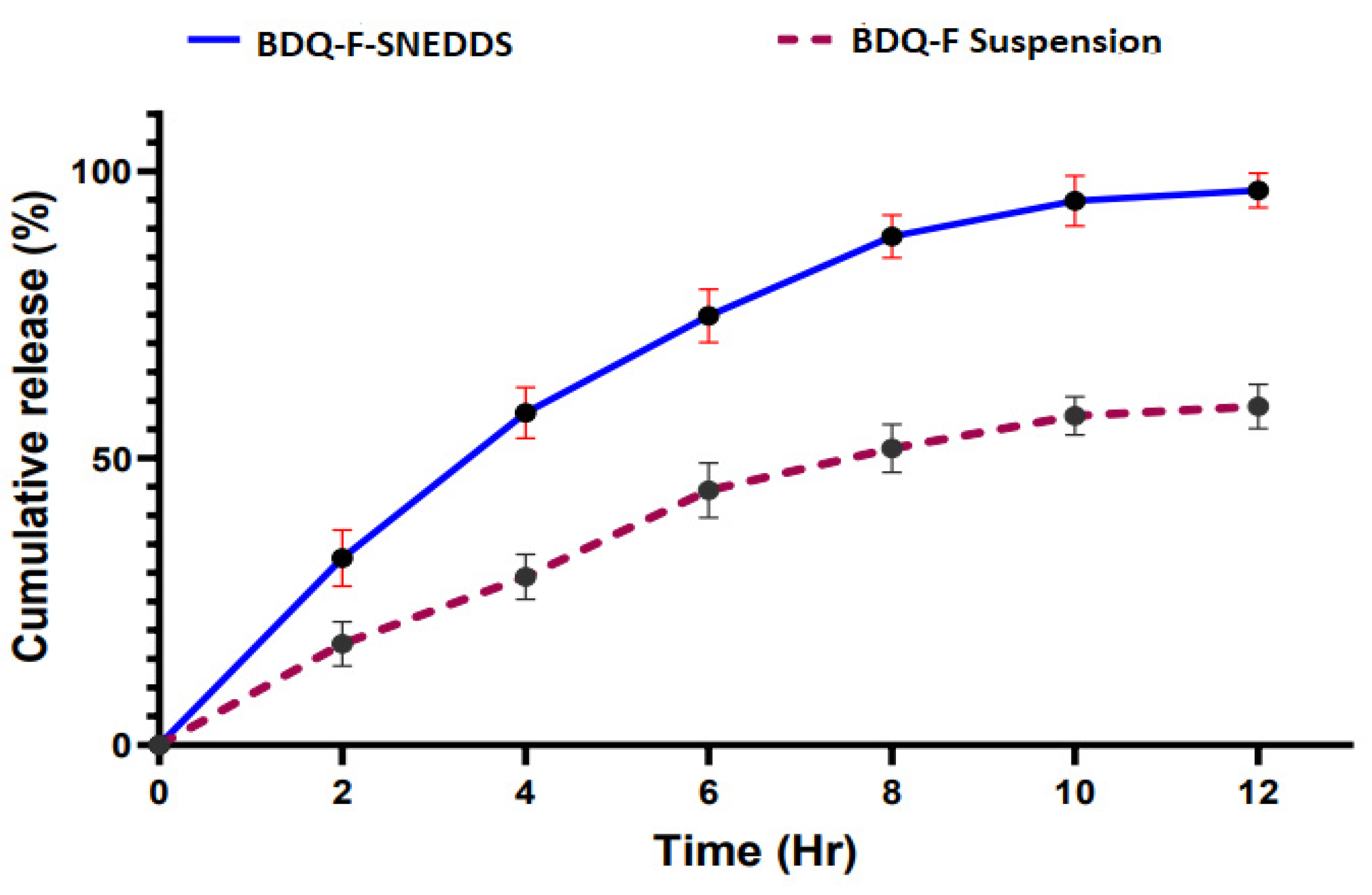
4.5.7. In vitro drug release
4.5.8. Stability study
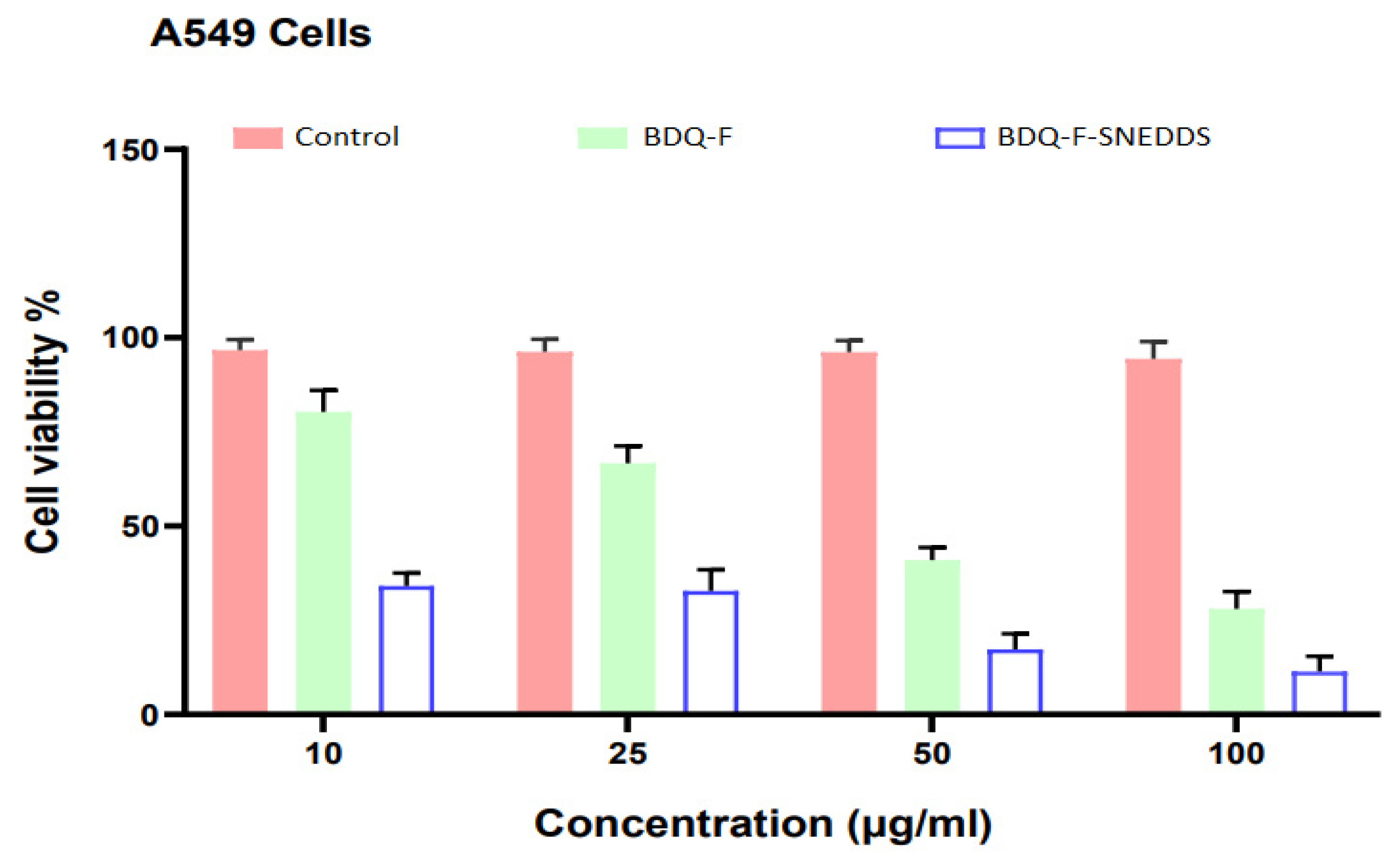
4.5.9. Cell cytotoxicity
5. Conclusion
Supplementary Materials
Author Contributions
Funding
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Global tuberculosis report 2020 2020. Available from: https://www.who.int/publications/i/item/9789240013131.
- Ndjeka N, Schnippel K, Master I, Meintjes G, Maartens G, Romero R, et al. High treatment success rate for multidrug-resistant and extensively drug-resistant tuberculosis using a bedaquiline-containing treatment regimen. 2018;52(6). [CrossRef]
- Zhou L, Yang L, Tilton S, Wang JJJops. Development of a high throughput equilibrium solubility assay using miniaturized shake-flask method in early drug discovery. 2007;96(11):3052-71. [CrossRef]
- WHO. WHO Coronavirus (COVID-19) Dashboard. Available from: https://covid19.who.int/.
- Lange C, Dheda K, Chesov D, Mandalakas AM, Udwadia Z, Horsburgh CR. Management of drug-resistant tuberculosis. The Lancet. 2019;394(10202):953-66. [CrossRef]
- Rawal T, Butani S. Combating tuberculosis infection: a forbidding challenge. Indian Journal of Pharmaceutical Sciences. 2016;78(1):8. [CrossRef]
- Ginsberg AM, Spigelman M. Challenges in tuberculosis drug research and development. Nature medicine. 2007;13(3):290-4. [CrossRef]
- Cox E, Laessig K. FDA approval of bedaquiline—the benefit–risk balance for drug-resistant tuberculosis. New England Journal of Medicine. 2014;371(8):689-91. [CrossRef]
- Chahine EB, Karaoui LR, Mansour HJAoP. Bedaquiline: a novel diarylquinoline for multidrug-resistant tuberculosis. 2014;48(1):107-15. [CrossRef]
- Guo H, Courbon GM, Bueler SA, Mai J, Liu J, Rubinstein JL. Structure of mycobacterial ATP synthase with the TB drug bedaquiline. bioRxiv. 2020:2020.08.06.225375. [CrossRef]
- Ibrahim M, Andries K, Lounis N, Chauffour A, Truffot-Pernot C, Jarlier V, et al. Synergistic Activity of R207910 Combined with Pyrazinamide against Murine Tuberculosis. Antimicrobial Agents and Chemotherapy. 2007;51(3):1011-5. [CrossRef]
- Diacon AH, Donald PR, Pym A, Grobusch M, Patientia RF, Mahanyele R, et al. Randomized Pilot Trial of Eight Weeks of Bedaquiline (TMC207) Treatment for Multidrug-Resistant Tuberculosis: Long-Term Outcome, Tolerability, and Effect on Emergence of Drug Resistance. Antimicrobial Agents and Chemotherapy. 2012;56(6):3271-6. [CrossRef]
- Gomes MJ, Martins S, Ferreira D, Segundo MA, Reis S. Lipid nanoparticles for topical and transdermal application for alopecia treatment: development, physicochemical characterization, and in vitro release and penetration studies. International journal of nanomedicine. 2014;9:1231. [CrossRef]
- Kakkar AK, Dahiya N. Bedaquiline for the treatment of resistant tuberculosis: promises and pitfalls. Tuberculosis. 2014;94(4):357-62. [CrossRef]
- Singh B, Bandopadhyay S, Kapil R, Singh R, Katare OP. Self-emulsifying drug delivery systems (SEDDS): formulation development, characterization, and applications. Critical Reviews™ in Therapeutic Drug Carrier Systems. 2009;26(5). [CrossRef]
- Mu H, Holm R, Müllertz A. Lipid-based formulations for oral administration of poorly water-soluble drugs. International journal of pharmaceutics. 2013;453(1):215-24. [CrossRef]
- Beg S, Sandhu PS, Batra RS, Khurana RK, Singh B. QbD-based systematic development of novel optimized solid self-nanoemulsifying drug delivery systems (SNEDDS) of lovastatin with enhanced biopharmaceutical performance. Drug Delivery. 2015 2015/08/18;22(6):765-84. [CrossRef]
- Singh B, Singh R, Bandyopadhyay S, Kapil R, Garg B. Optimized nanoemulsifying systems with enhanced bioavailability of carvedilol. Colloids and Surfaces B: Biointerfaces. 2013 2013/01/01/;101:465-74. [CrossRef]
- Bandyopadhyay S, Katare OP, Singh B. Optimized self nano-emulsifying systems of ezetimibe with enhanced bioavailability potential using long chain and medium chain triglycerides. Colloids and Surfaces B: Biointerfaces. 2012 2012/12/01/;100:50-61. [CrossRef]
- Dhawan S, Kapil R, Singh B. Formulation development and systematic optimization of solid lipid nanoparticles of quercetin for improved brain delivery. Journal of Pharmacy and Pharmacology. 2011;63(3):342-51. [CrossRef]
- Raza K, Singh B, Singal P, Wadhwa S, Katare OP. Systematically optimized biocompatible isotretinoin-loaded solid lipid nanoparticles (SLNs) for topical treatment of acne. Colloids and Surfaces B: Biointerfaces. 2013 2013/05/01/;105:67-74. [CrossRef]
- Singh B, Mehta G, Kumar R, Bhatia A, Ahuja N, Katare O. Design, development and optimization of nimesulide-loaded liposomal systems for topical application. Current drug delivery. 2005;2(2):143-53. [CrossRef]
- Zhou L, Yang L, Tilton S, Wang J. Development of a high throughput equilibrium solubility assay using miniaturized shake-flask method in early drug discovery. Journal of pharmaceutical sciences. 2007;96(11):3052-71. [CrossRef]
- Czajkowska-Kośnik A, Szekalska M, Amelian A, Szymańska E, Winnicka K. Development and Evaluation of Liquid and Solid Self-Emulsifying Drug Delivery Systems for Atorvastatin. Molecules. 2015;20(12):21010-22. PubMed PMID: doi:10.3390/molecules201219745. [CrossRef]
- Joseph E, Reddi S, Rinwa V, Balwani G, Saha R. DoE based Olanzapine loaded poly-caprolactone nanoparticles decreases extrapyramidal effects in rodent model. International journal of pharmaceutics. 2018 Apr 25;541(1-2):198-205. PubMed PMID: 29474898. Epub 2018/02/24. eng. [CrossRef]
- Yadav P, Rastogi V, Verma A. Application of Box–Behnken design and desirability function in the development and optimization of self-nanoemulsifying drug delivery system for enhanced dissolution of ezetimibe. Future Journal of Pharmaceutical Sciences. 2020 2020/03/02;6(1):7. [CrossRef]
- Syukri Y, Martien R, Lukitaningsih E, Nugroho AE. Novel Self-Nano Emulsifying Drug Delivery System (SNEDDS) of andrographolide isolated from Andrographis paniculata Nees: characterization, in-vitro and in-vivo assessment. Journal of Drug Delivery Science and Technology. 2018;47:514-20. [CrossRef]
- Balakumar K, Raghavan CV, selvan NT, prasad RH, Abdu S. Self nanoemulsifying drug delivery system (SNEDDS) of rosuvastatin calcium: design, formulation, bioavailability and pharmacokinetic evaluation. Colloids and surfaces B, Biointerfaces. 2013 Dec 1;112:337-43. PubMed PMID: 24012665. Epub 2013/09/10. eng. [CrossRef]
- Chinchole A, Poul B, Panchal C, Chavan D. A review on stability guidelines by ICH and USFDA guidelines for new formulation and dosage form. PharmaTutor. 2014;2(8):32-53.
- Singh SK, Dadhania P, Vuddanda PR, Jain A, Velaga S, Singh S. Intranasal delivery of asenapine loaded nanostructured lipid carriers: formulation, characterization, pharmacokinetic and behavioural assessment. RSC Advances. 2016;6(3):2032-45. [CrossRef]
- Patil SM, Sawant SS, Kunda NK. Pulmonary delivery of bedaquiline-loaded cubosomes for non-small cell lung cancer (NSCLC) treatment. Drug Delivery to the Lungs. 2021;32.
- Shahba AA-W, Mohsin K, Alanazi FK, Abdel-Rahman SI. Optimization of self-nanoemulsifying formulations for weakly basic lipophilic drugs: role of acidification and experimental design. Brazilian Journal of Pharmaceutical Sciences. 2016;52:653-67. [CrossRef]
- Solans C, Izquierdo P, Nolla J, Azemar N, Garcia-Celma MJ. Nano-emulsions. Current Opinion in Colloid & Interface Science. 2005 2005/10/01/;10(3):102-10. [CrossRef]
- Limbani MD, Patel L. Studies on drug solubilization and role of lipid vehicle in pseudo ternary phase diagram in formulation development of SNEDDS containing poorly water soluble drug. Int J Pharm Sci Rev Res. 2016;40(2):228-37.
- Marasini N, Yan YD, Poudel BK, Choi HG, Yong CS, Kim JO. Development and Optimization of Self-Nanoemulsifying Drug Delivery System with Enhanced Bioavailability by Box–Behnken Design and Desirability Function. Journal of Pharmaceutical Sciences. 2012 2012/12/01/;101(12):4584-96. [CrossRef]
- Shanmugam S, Baskaran R, Balakrishnan P, Thapa P, Yong CS, Yoo BK. Solid self-nanoemulsifying drug delivery system (S-SNEDDS) containing phosphatidylcholine for enhanced bioavailability of highly lipophilic bioactive carotenoid lutein. European Journal of Pharmaceutics and Biopharmaceutics. 2011;79(2):250-7. [CrossRef]
- Rodríguez-Rodríguez R, Espinosa-Andrews H, Morales-Hernández N, Lobato-Calleros C, Vernon-Carter EJ. Mesquite gum/chitosan insoluble complexes: relationship between the water state and viscoelastic properties. Journal of Dispersion Science and Technology. 2019 2019/09/02;40(9):1345-52. [CrossRef]
- Nasr A, Gardouh A, Ghorab M. Novel Solid Self-Nanoemulsifying Drug Delivery System (S-SNEDDS) for Oral Delivery of Olmesartan Medoxomil: Design, Formulation, Pharmacokinetic and Bioavailability Evaluation. Pharmaceutics. 2016 Jun 27;8(3). PubMed PMID: 27355963. Pubmed Central PMCID: PMC5039439. Epub 2016/06/30. eng. [CrossRef]
- Alhakamy NA, Aldawsari HM, Hosny KM, Ahmad J, Akhter S, Kammoun AK, et al. Formulation design and pharmacokinetic evaluation of docosahexaenoic acid containing self-nanoemulsifying drug delivery system for oral administration. Nanomaterials and Nanotechnology. 2020;10:1847980420950988. [CrossRef]
- Shukla SK, Kulkarni NS, Farrales P, Kanabar DD, Parvathaneni V, Kunda NK, et al. Sorafenib Loaded Inhalable Polymeric Nanocarriers against Non-Small Cell Lung Cancer. Pharmaceutical research. 2020 Mar 12;37(3):67. PubMed PMID: 32166411. Epub 2020/03/14. eng. [CrossRef]

| Variables | Levels used | |
|---|---|---|
| Independent variables | Low (-1) | High (+1) |
| X1: Oil (%) | 10 | 30 |
| X2: Smix (%) | 40 | 60 |
| X3: Sonication time (min) | 30 | 60 |
| Dependent variables | Constraints | |
| Droplet size (nm) | Minimize | |
| PDI | Minimize | |
| Transmittance (%) | Maximize | |
| Dilution (folds) | Droplet size (nm) | PDI | Transmittance (%) |
|---|---|---|---|
| 50 | 99.8 | 0.34 | 97.8 |
| 100 | 95.9 | 0.39 | 97.1 |
| 200 | 95.1 | 0.42 | 96.4 |
| At a temperature 40 ± 2 ºC Humidity 75 ± 5 % | |||
| Testing Parameters | Initial | 3 Months | 6 Months |
| Physical Appearance | Clear | Clear | Clear |
| Phase Separation | No phase separation | No | No |
| Caking | No caking | No | No |
| Size (nm) | 98.88 ± 0.19 | 99.81 ± 0.72 | 103.04 ± 0.83 |
| PDI | 0.34 ± 0.392 | 0.39 ± 0.321 | 0.452 ± 0.43 |
| Entrapment Efficiency | 98.3 % | 87.7% | 76.2% |
| At a temperature 25 ± 2 ºC Humidity 60 ± 5 % | |||
| Physical Appearance | Clear | Clear | Clear |
| Phase Separation | No phase separation | No | No |
| Caking | No caking | No | No |
| Size (nm) | 98.88 ± 0.32 | 99.95 ± 0.45 | 103.07 ± 0.52 |
| PDI % | 0.340 ± 0.392 | 0.400 ± 0.321 | 0.45 ± 0.43 |
| Entrapment Efficiency | 98.3 % | 85.6% | 75.1% |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (https://creativecommons.org/licenses/by/4.0/).




