Submitted:
07 July 2023
Posted:
11 July 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
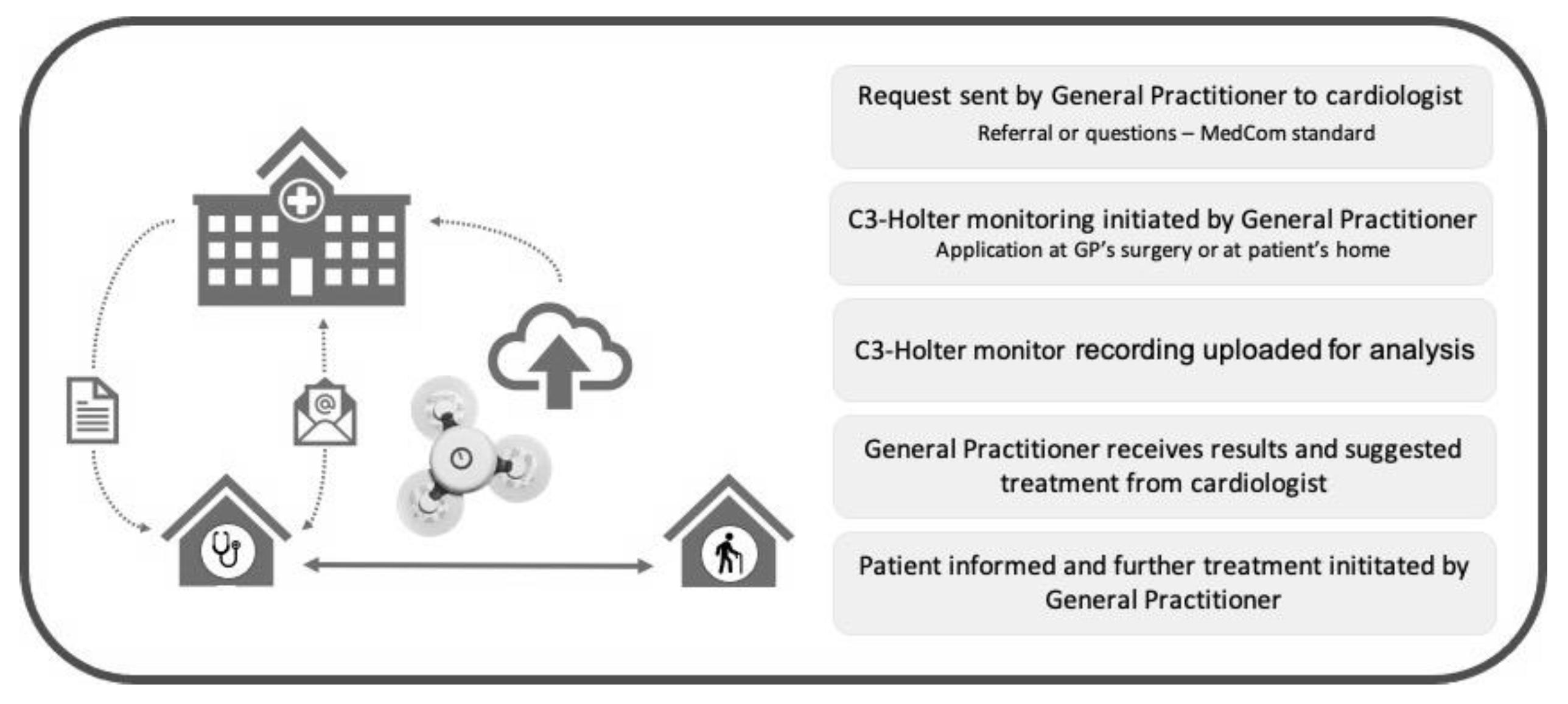
2.1. The CardioShare Model
2.2. Patient Reported Experiences
2.3. Participating Health Care Professionals’ Experiences
3. Results
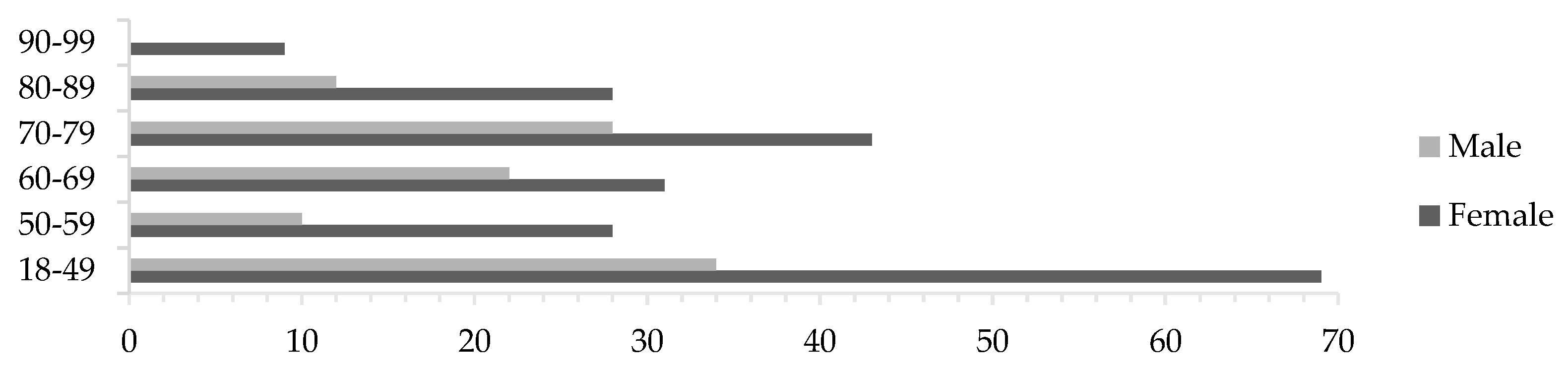
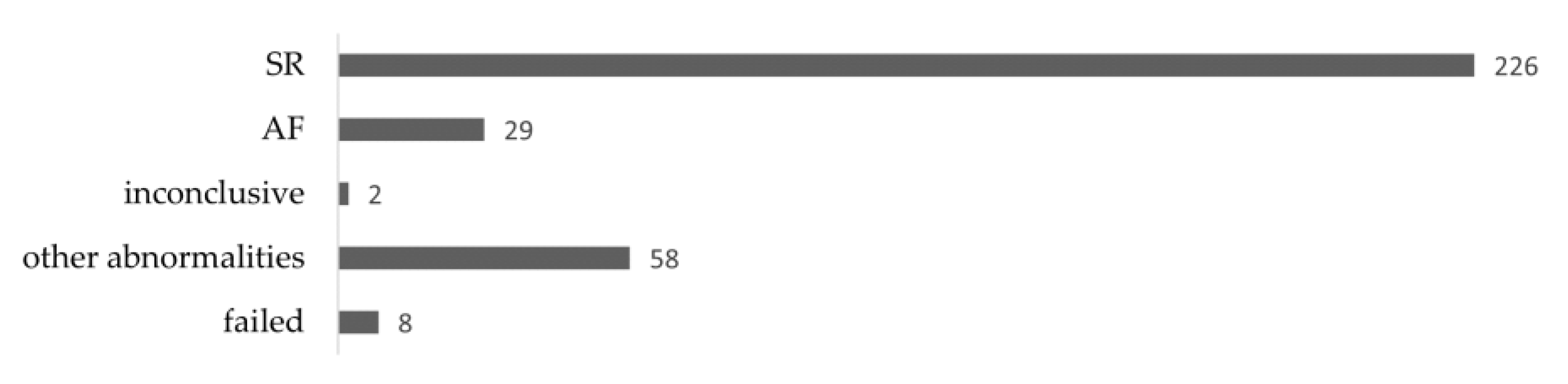
3.1. Clinical Randomized Study
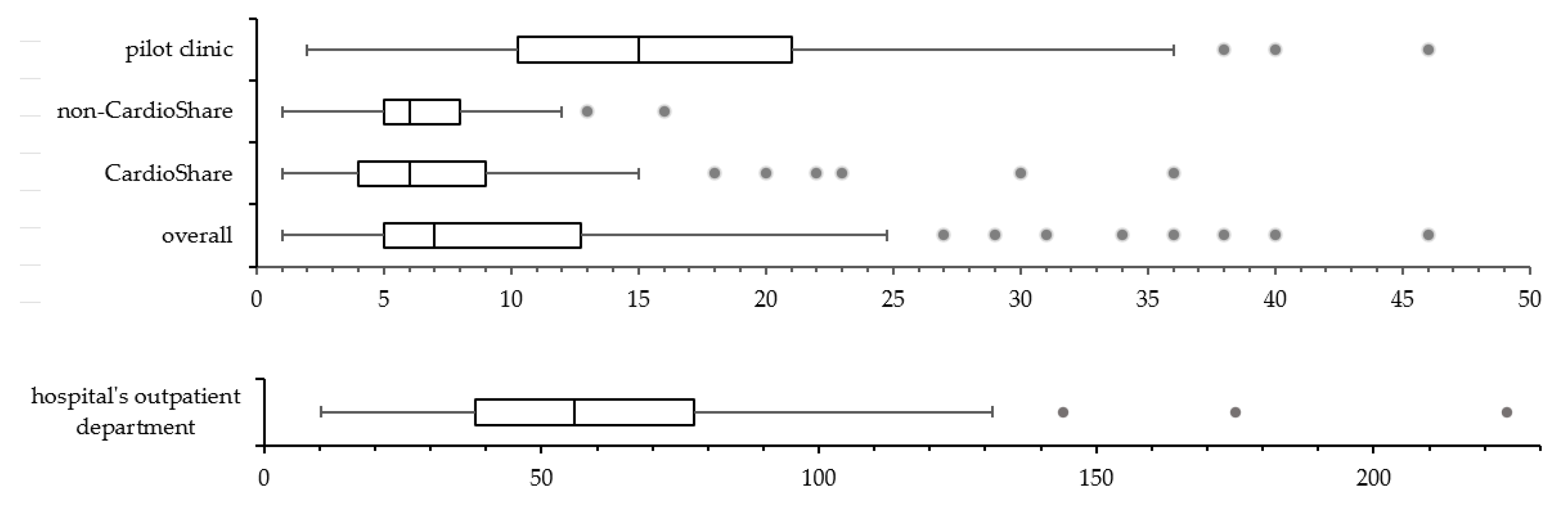
3.1.1. CardioShare Versus Non-CardioShare
3.1.2. Escalation Test
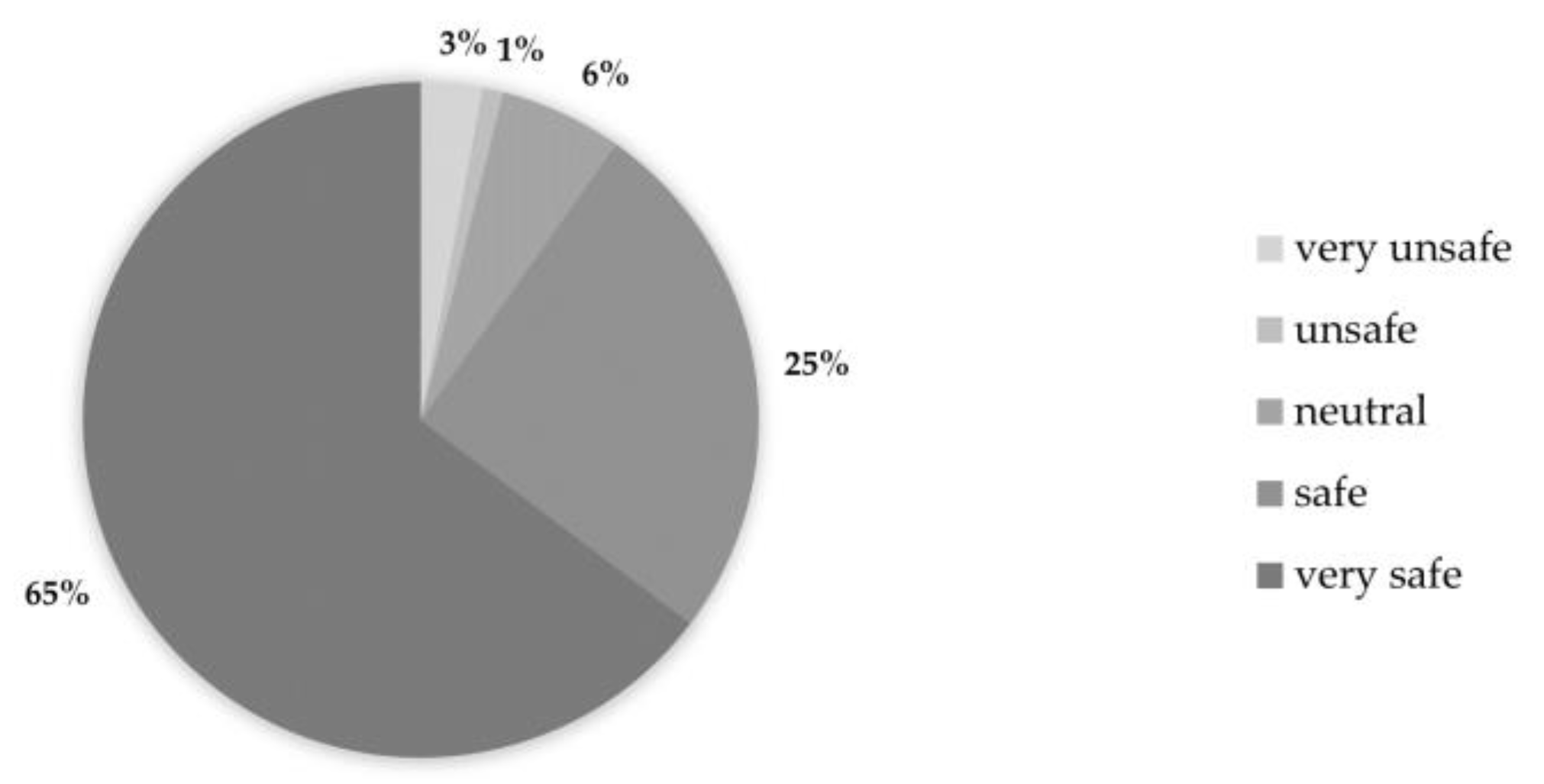
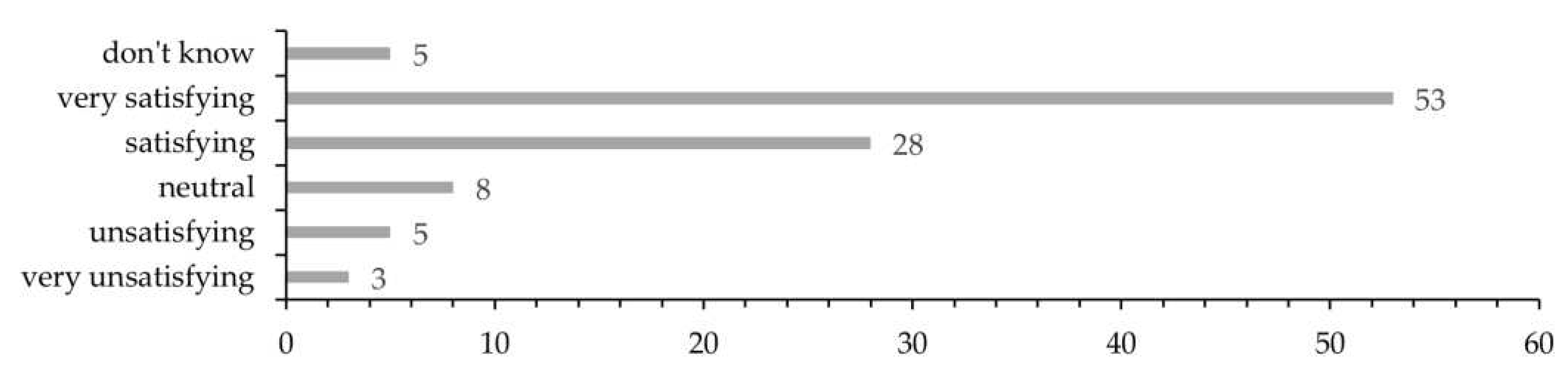
3.2. Survey
3.3. Semi-Structured Interviews with Patients
3.3.1. Patients Expericence a High Level of Professionalism and Quality Despite Not Being Seen by a Cardiologist
”I assume there is no big difference between the approaches. It’s just the consultation that’s different. I wasn’t nervous at all about quality.”
”I was told that cardiologists saw my recording. So, it actually was the specialists who did analyze it.”
”I think it is just fine that cardiologists give advice [on further treatment] to my GP.”
”It depends on the severeness. If I’m having heart pain or feeling that my heart skips beats, I’d prefer to be referred to cardiologists right away. I’m sure my doctor would do so.”
3.3.2. The C3-holter Device Is User Friendly and Easy to Handle.
“I did the usual things - went for a walk every day, played some golf.”
“It was only three days, so I let it be and just washed around it.”
“They explained how to replace the patches, and I am comfortable to do so.”
“After a shower, I took it back on without any problem.”
“I didn’t pay any attention to the device before my skin became itchy.”
“When you’ve been wearing it for three days, your skin has become very itchy, and you look forward to get rid of the device.”
“The indicator was flashing, when the device was attached properly, but at some point, it had changed, and I thought it might have loosened. After I put it back on, the indicator flashed like before.”
“The patches weren’t attached very well. There was flashing green or white light depending on my movements.”
“I quite liked the possibility to push the button when I was experiencing symptoms.”
“When I felt any kind of symptoms, there was this button I just could push to set a marker on the recording.”
3.3.3. Being Diagnosed by Their GP Makes the Patients Feel Safe and Secure
”It depends on, which one of the GPs I’m seeing.”
”In the old days I felt safe, because you always saw the same doctor. They kind of knew your journal. Today there are many different [doctors/GPs].”
”I think it’s just fine, if it works. I think it’s nice, because it does mean a lot to feel comfortable with the person [doctor / health professional] you’re seeing.”
”My doctor knows me and my medical history. A disease course can be broad, and specialists only look at things from their own discipline’s perspective.”
”There’s always a lot of waiting time. I prefer to see my GP.”
”I think it was nice, that the recording could be started right away.”
”When I need to go to the hospital I do need transportation help. I must be ready 90 minutes before, and then there’s waiting time and everything. I think it’s quite difficult.”
”I hadn’t got any feedback from my GP. That was strange.”
”I called them after two weeks, because I hadn’t heard anything yet. I was told that the recording was empty.”
3.4. Semi-Structured Interviews with GP’s and Nurses
3.4.1. The C3+ Sensor is User Friendly and Easy to Use in a GP’s Setting
“I think it was quite straight forward. I just had to get used to how to send the correspondence [to the cardiologist] and what to write, but it was actually quite quick to get it sorted out.”
“There are so many sentences, with all sorts of things, and there are actually only four things you have to do, so you could actually […] make a much simpler guide.”
3.4.2. Cooperation between GP and Cardiologist is Helpful and Appreciated
“It has been, in other words, completely impeccable in every way.”
“When you have to interpret the results, it's extremely nice to have a cardiologist backing you up.”
’’Being able to do a Holter monitoring is like a function we have wanted, it has been difficult to access, […], and suddenly it has moved very close.”
“I think it belongs excellently here, at this level where you have professional cooperation along the way.”
3.4.3. Patients Benefit from Holter Monitoring at their GP’s
“We have a huge population, we have two nursing homes for which we are primary doctors.”
“We've actually used it primarily for the unconclusive [patient group], where we thought they're not quite candidates for a hospital cardiology evaluation process.”
“Health can be measured in many ways; whether they don't get blood clots, or whether they are reassured in their fear of illness.”
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Appendix A

Appendix B
| Meaning Unit | Condensed Meaning Unit | Code | Category | Theme1 |
|---|---|---|---|---|
| “It wasn’t heavy or impractical in any way to wear the device. It was quite easy and didn’t bother me at all. I worked, went for a walk, and many other things.” | Device is not bothering; easy to wear; activities as usual | Everyday life with C3 monitor | Comfort | The device is user friendly / easy to use. |
| “My skin became very itchy when wearing it [the device].” | Patches causing itchy skin reaction | Source of annoyance | ||
| “You are kind of nervous whether the device might fall off. It actually did when I was playing golf. It was hot, and I was sweating a lot.” | Device fell of due to sweating while playing golf. | Technical problems | Reliability |
References
- Writing Committee Members; Fuster, V.; Rydén, L.E.; Cannom, D.S.; Crijns, H.J.; Curtis, A.B.; Ellenbogen, K.A.; Halperin, J.L.; Le Heuzey, J.-Y.; Kay, G.N.; et al. ACC/AHA/ESC 2006 guidelines for the management of patients with atrial fibrillation: full text: A report of the American College of Cardiology/American Heart Association Task Force on practice guidelines and the European Society of Cardiology Committee for Practice Guidelines (Writing Committee to Revise the 2001 Guidelines for the Management of Patients With Atrial Fibrillation) Developed in collaboration with the European Heart Rhythm Association and the Heart Rhythm Society. Europace 2006, 8, 651–745. [CrossRef]
- Lloyd-Jones, D.M., et al., Lifetime risk for development of atrial fibrillation: the Framingham Heart Study. Circulation, 2004. 110(9): p. 1042-6. [CrossRef]
- Benjamin, E.J., et al., Impact of atrial fibrillation on the risk of death: the Framingham Heart Study. Circulation, 1998. 98(10): p. 946-52. [CrossRef]
- Johansson, L.; Norberg, J.; Jansson, J.-H.; Bäckström, S. Estimating the prevalence of atrial fibrillation in a general population using validated electronic health data. Clin. Epidemiology 2013, 5, 475–481. [Google Scholar] [CrossRef] [PubMed]
- Potpara, T.S.; Polovina, M.M.; Marinkovic, J.M.; Lip, G.Y. A comparison of clinical characteristics and long-term prognosis in asymptomatic and symptomatic patients with first-diagnosed atrial fibrillation: The Belgrade Atrial Fibrillation Study. Int. J. Cardiol. 2013, 168, 4744–4749. [Google Scholar] [CrossRef] [PubMed]
- Dilaveris, P.E.; Kennedy, H.L. Silent atrial fibrillation: epidemiology, diagnosis, and clinical impact. Clin. Cardiol. 2017, 40, 413–418. [Google Scholar] [CrossRef] [PubMed]
- Hart, R.G. Atrial fibrillation and stroke prevention. N Engl J Med, 2003. 349(11): p. 1015-6. [CrossRef]
- Wachter, R.; Weber-Krüger, M.; Seegers, J.; Edelmann, F.; Wohlfahrt, J.; Wasser, K.; Gelbrich, G.; Hasenfuß, G.; Stahrenberg, R.; Liman, J.; et al. Age-dependent yield of screening for undetected atrial fibrillation in stroke patients: the Find-AF study. J. Neurol. 2013, 260, 2042–2045. [Google Scholar] [CrossRef] [PubMed]
- Connolly, S.J., et al., Dabigatran versus warfarin in patients with atrial fibrillation. N Engl J Med, 2009. 361(12): p. 1139-51. [CrossRef]
- Gladstone, D.J.; Bui, E.; Fang, J.; Laupacis, A.; Lindsay, M.P.; Tu, J.V.; Silver, F.L.; Kapral, M.K. Potentially Preventable Strokes in High-Risk Patients With Atrial Fibrillation Who Are Not Adequately Anticoagulated. Stroke 2009, 40, 235–240. [Google Scholar] [CrossRef] [PubMed]
- Patel, M.R., et al., Rivaroxaban versus warfarin in nonvalvular atrial fibrillation. N Engl J Med, 2011. 365(10): p. 883-91. [CrossRef]
- Granger, C.B., et al., Apixaban versus warfarin in patients with atrial fibrillation. N Engl J Med, 2011. 365(11): p. 981-92. [CrossRef]
- Giugliano, R.P., et al., Edoxaban versus warfarin in patients with atrial fibrillation. N Engl J Med, 2013. 369(22): p. 2093-104. [CrossRef]
- Shahid, F.; Shantsila, E.; Lip, G.Y.H. Recent advances in the understanding and management of atrial fibrillation: a focus on stroke prevention. F1000Research 2016, 5, 2887. [Google Scholar] [CrossRef] [PubMed]
- Lubitz, S.A., et al., Long-term outcomes of secondary atrial fibrillation in the community: the Framingham Heart Study. Circulation, 2015. 131(19): p. 1648-55. [CrossRef]
- Filardo, G.; Hamilton, C.; Hamman, B.; Hebeler, R.F.; Adams, J.; Grayburn, P. New-Onset Postoperative Atrial Fibrillation and Long-Term Survival After Aortic Valve Replacement Surgery. Ann. Thorac. Surg. 2010, 90, 474–479. [Google Scholar] [CrossRef] [PubMed]
- Saxena, A.; Dinh, D.; Dimitriou, J.; Reid, C.; Smith, J.; Shardey, G.; Newcomb, A. Preoperative atrial fibrillation is an independent risk factor for mid-term mortality after concomitant aortic valve replacement and coronary artery bypass graft surgery. Interact. Cardiovasc. Thorac. Surg. 2013, 16, 488–494. [Google Scholar] [CrossRef] [PubMed]
- Ahlsson, A.; Fengsrud, E.; Bodin, L.; Englund, A. Postoperative atrial fibrillation in patients undergoing aortocoronary bypass surgery carries an eightfold risk of future atrial fibrillation and a doubled cardiovascular mortality. Eur. J. Cardio-Thoracic Surg. 2010, 37, 1353–1359. [Google Scholar] [CrossRef] [PubMed]
- Pillarisetti, J.; Patel, A.; Bommana, S.; Guda, R.; Falbe, J.; Zorn, G.T.; Muehlebach, G.; Vacek, J.; Lai, S.M.; Lakkireddy, D. Atrial fibrillation following open heart surgery: long-term incidence and prognosis. J. Interv. Card. Electrophysiol. 2013, 39, 69–75. [Google Scholar] [CrossRef] [PubMed]
- Kaatz, S.; Douketis, J.D.; Zhou, H.; Gage, B.F.; White, R.H. Risk of stroke after surgery in patients with and without chronic atrial fibrillation. J. Thromb. Haemost. 2010, 8, 884–890. [Google Scholar] [CrossRef] [PubMed]
- Stevens, D.; Harrison, S.L.; Kolamunnage-Dona, R.; Lip, G.Y.H.; A Lane, D. The Atrial Fibrillation Better Care pathway for managing atrial fibrillation: a review. Europace 2021, 23, 1511–1527. [Google Scholar] [CrossRef] [PubMed]
- Thorpe, K.E.; Zwarenstein, M.; Oxman, A.D.; Treweek, S.; Furberg, C.D.; Altman, D.G.; Tunis, S.; Bergel, E.; Harvey, I.; Magid, D.J.; et al. A pragmatic–explanatory continuum indicator summary (PRECIS): a tool to help trial designers. J. Clin. Epidemiology 2009, 62, 464–475. [Google Scholar] [CrossRef] [PubMed]
- Ford, I. and J. Norrie, Pragmatic Trials. N Engl J Med, 2016. 375(5): p. 454-63. [CrossRef]
- Ladegaard, C.T.; Bamberg, C.; Aalling, M.; Jensen, D.M.; Kamstrup-Larsen, N.; Madsen, C.V.; Kamil, S.; Gudbergsen, H.; Saxild, T.; Schiøtz, M.L.; et al. Reaching Frail Elderly Patients to Optimize Diagnosis and Management of Atrial Fibrillation (REAFEL): A Feasibility Study of a Cross-Sectoral Shared-Care Model. Int. J. Environ. Res. Public Heal. 2022, 19, 7383. [Google Scholar] [CrossRef] [PubMed]
- Xue, Q.-L. The Frailty Syndrome: Definition and Natural History. Clin. Geriatr. Med. 2011, 27, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Schoon, Y.; Bongers, K.; Van Kempen, J.; Melis, R.; Rikkert, M.O. Gait speed as a test for monitoring frailty in community-dwelling older people has the highest diagnostic value compared to step length and chair rise time. Eur J Phys Rehabil Med 2014, 50, 693–701. [Google Scholar] [PubMed]
- Rosted, E.; Schultz, M.; Dynesen, H.; Dahl, M.; Sørensen, M.; Sanders, S. The Identification of Seniors at Risk screening tool is useful for predicting acute readmissions. Dan Med J 2014, 61, A4828. [Google Scholar] [PubMed]
- Erlingsson, C.; Brysiewicz, P. A hands-on guide to doing content analysis. Afr. J. Emerg. Med. 2017, 7, 93–99. [Google Scholar] [CrossRef] [PubMed]
| Frail elderly are aged ≥ 65 years and match at least one of the following: | |
| (1) | Need help with transportation to the hospital’s outpatient department |
| (2) | Need help with personal hygiene |
| (3) | Have reduced ability to walk (estimated to take > 5 s to walk 5 m) |
| (4) | Have unintentionally lost weight within the past year |
| (5) | Have cognitive difficulties (dementia, memory deficits, aphasia, etc.) |
| (6) | Have social problems due to abuse, ethnic background, language, etc. |
| (1) | Unresolved palpitations |
| (2) | Unclear episodes of dizziness |
| (3) | New atrial fibrillation diagnosis |
| (4) | Suspicion of other arrythmias in patients with known atrial fibrillation |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




