Submitted:
30 June 2023
Posted:
04 July 2023
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Sample Selection:
2.2. PSG recordings
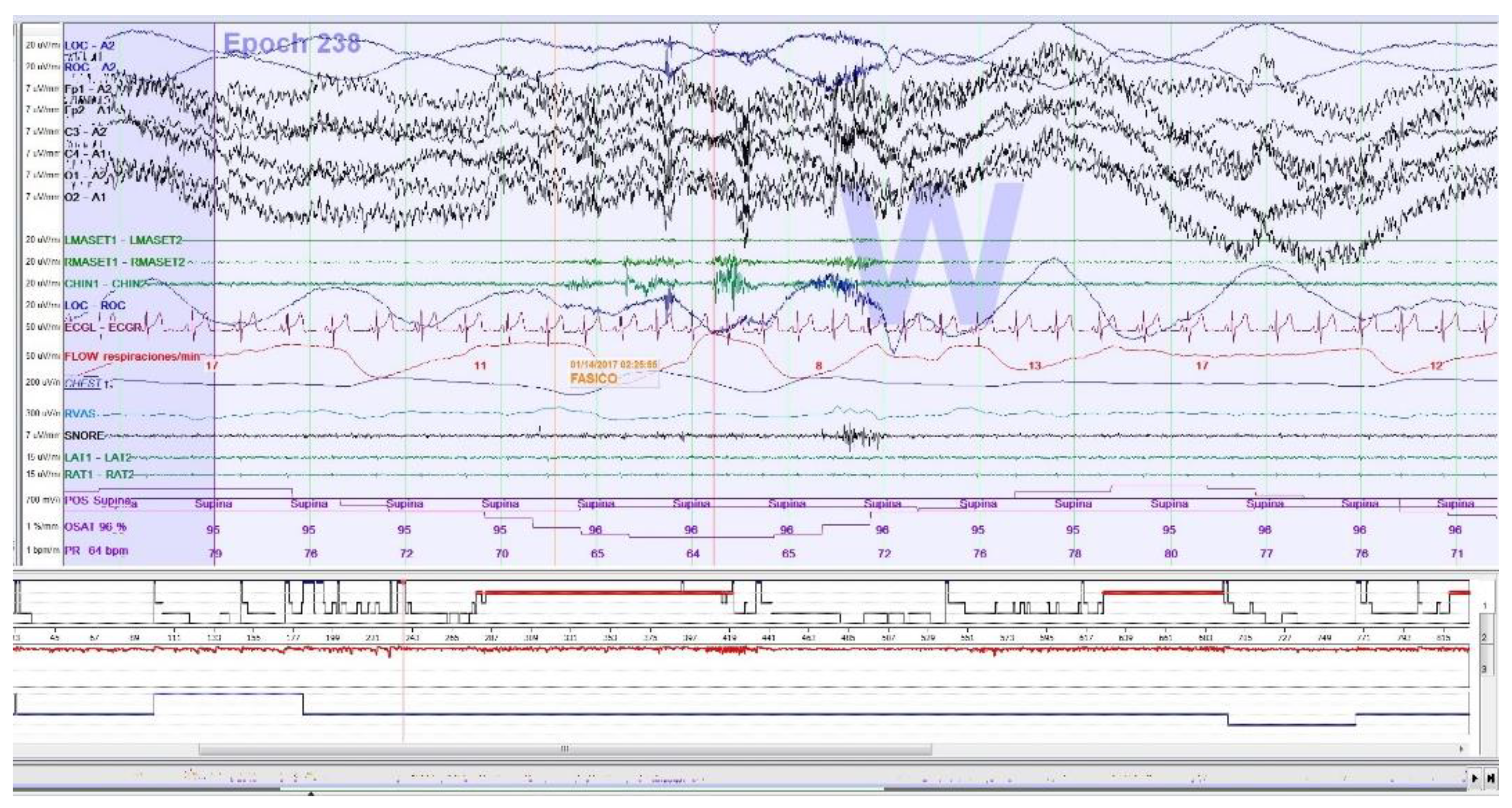
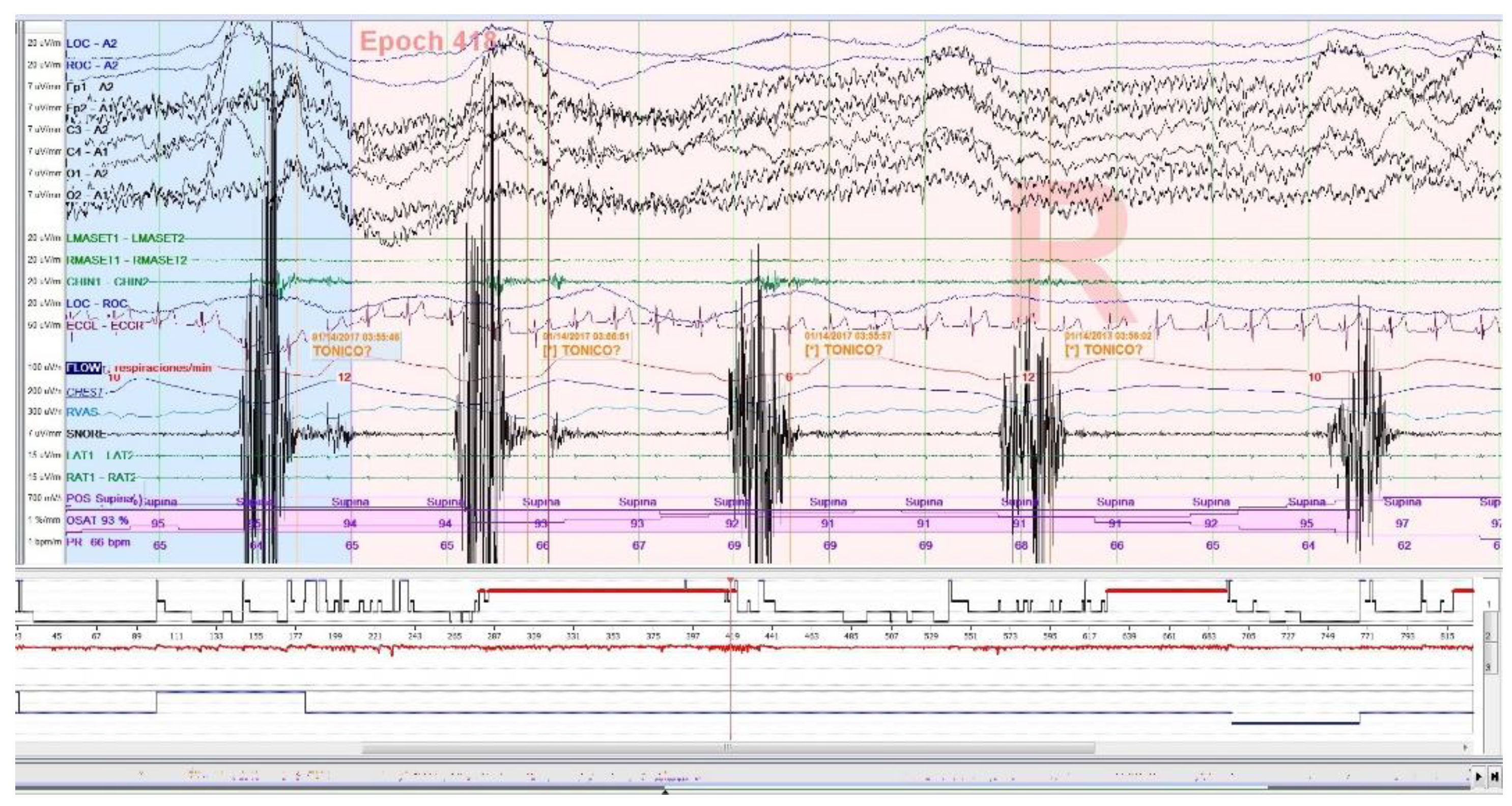
2.2.1. PSG Sleep Bruxism Analysis
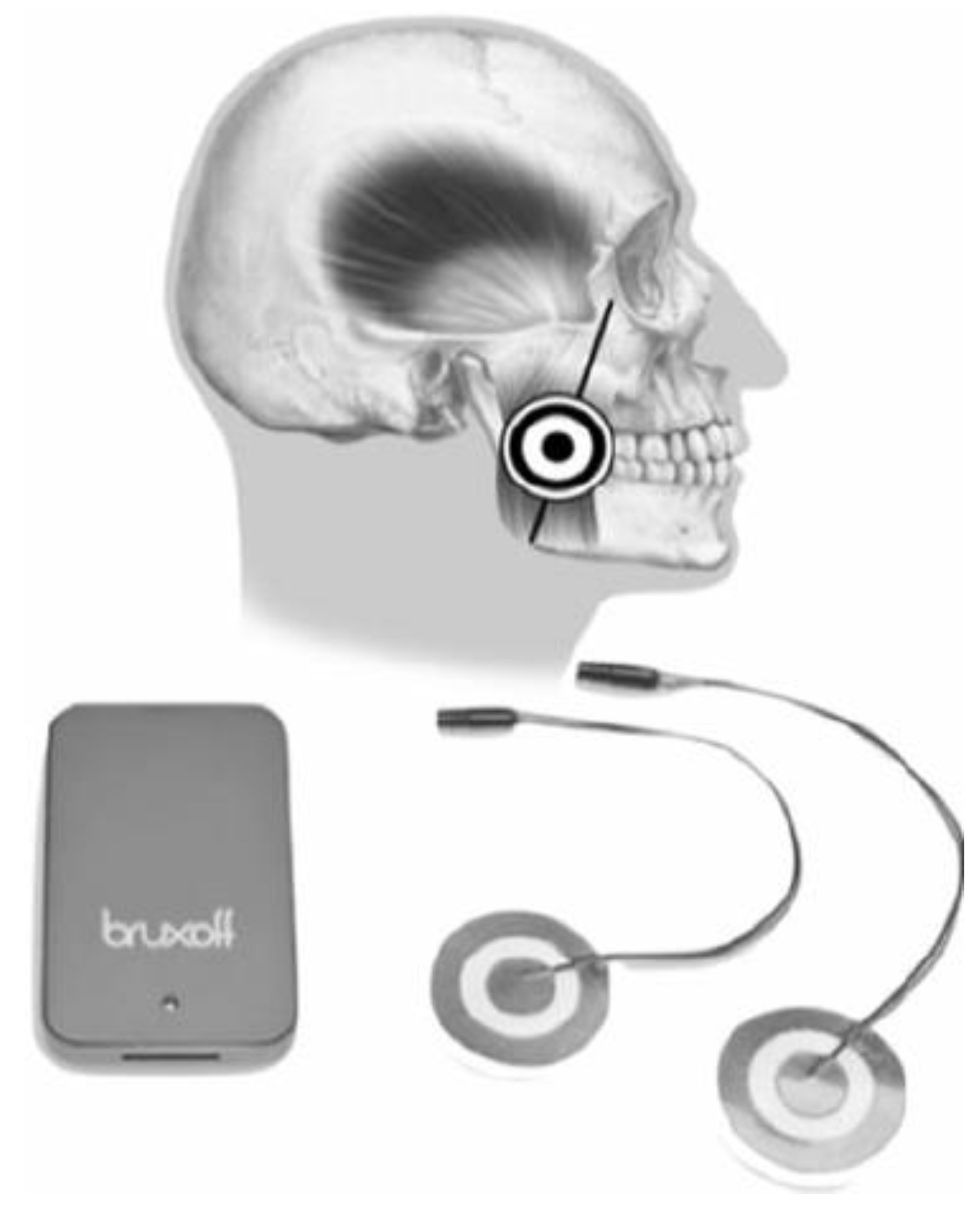
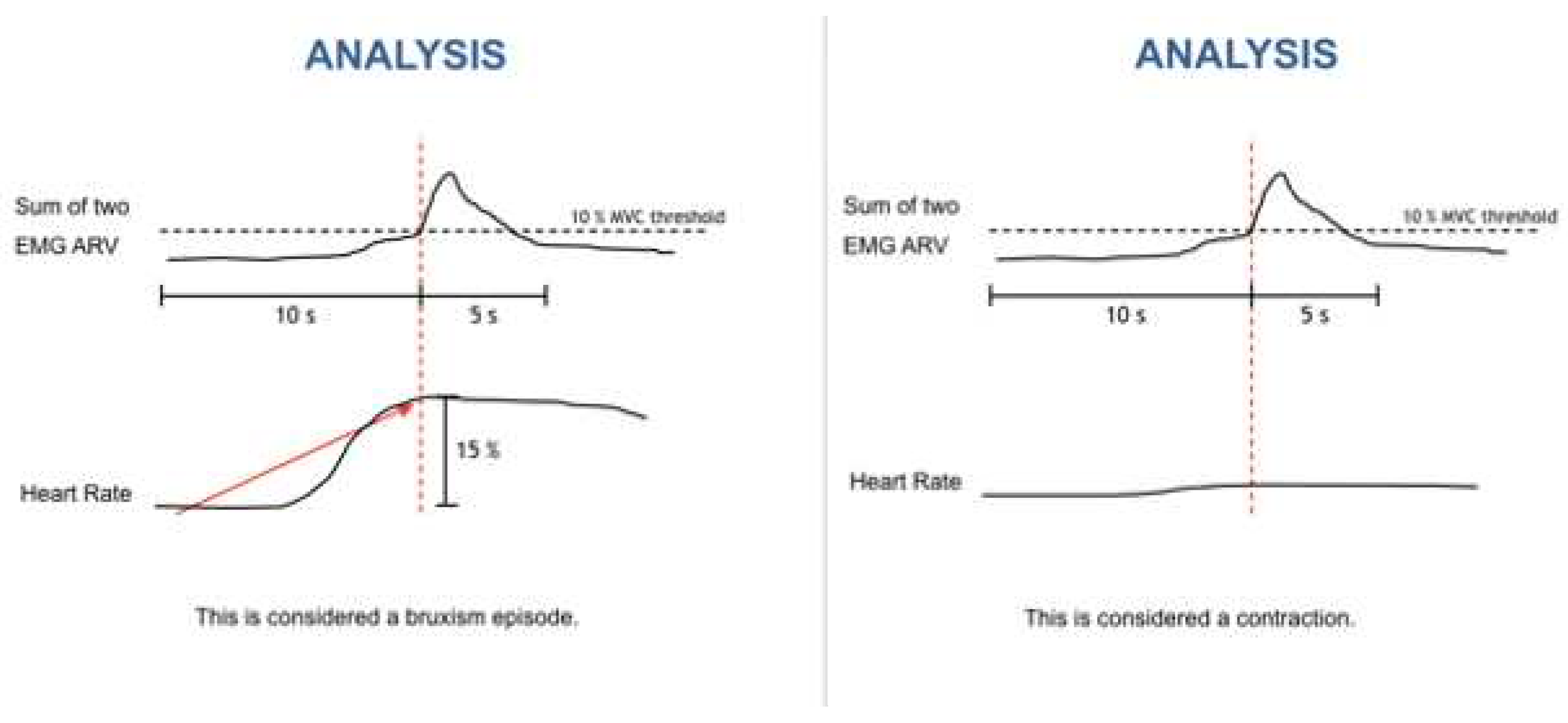
2.3. Bruxoff Sleep Bruxism Analysis
2.4. Statistical analysis
3. Results
4. Discussion
Limitations
5. Conclusions
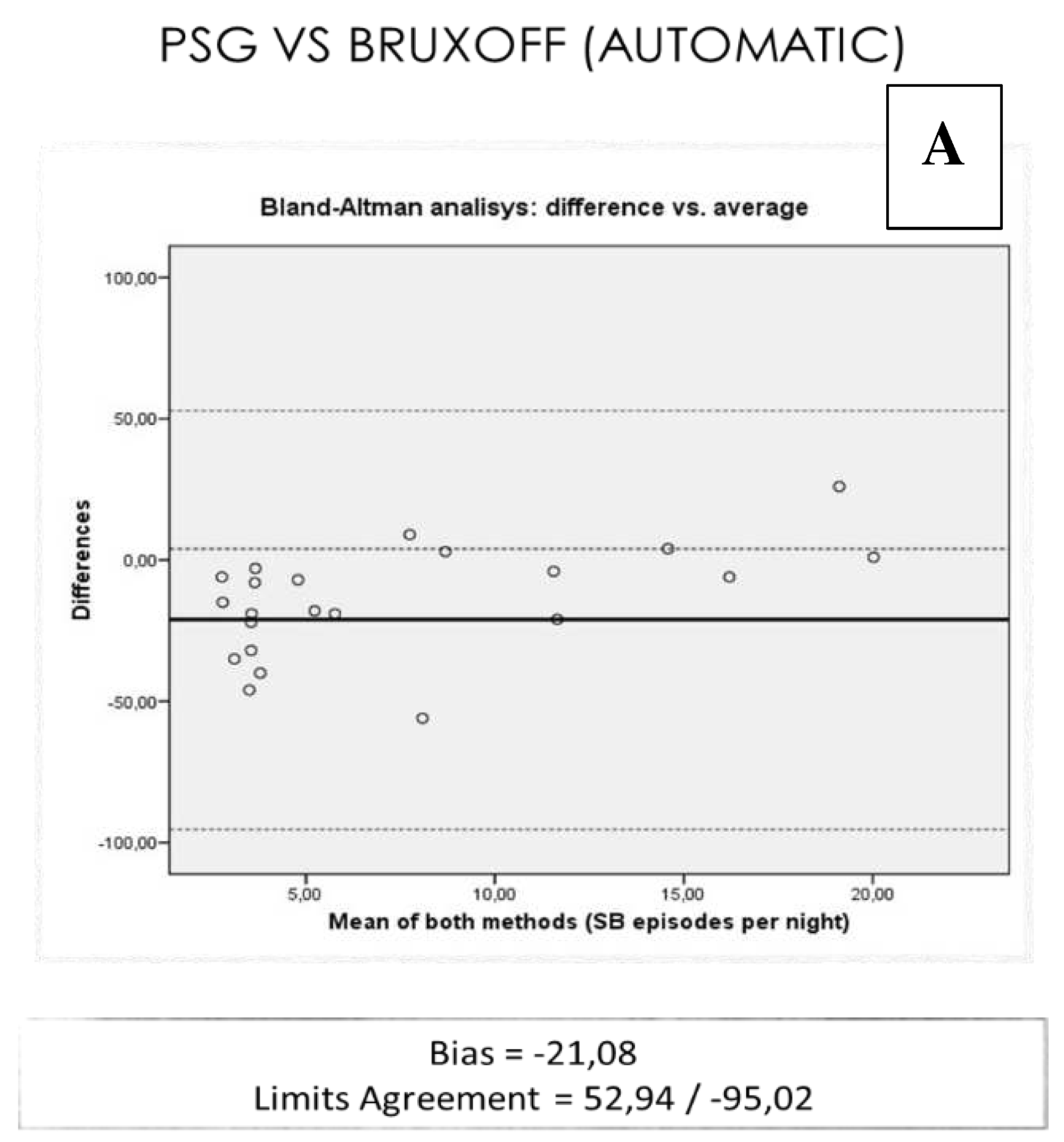
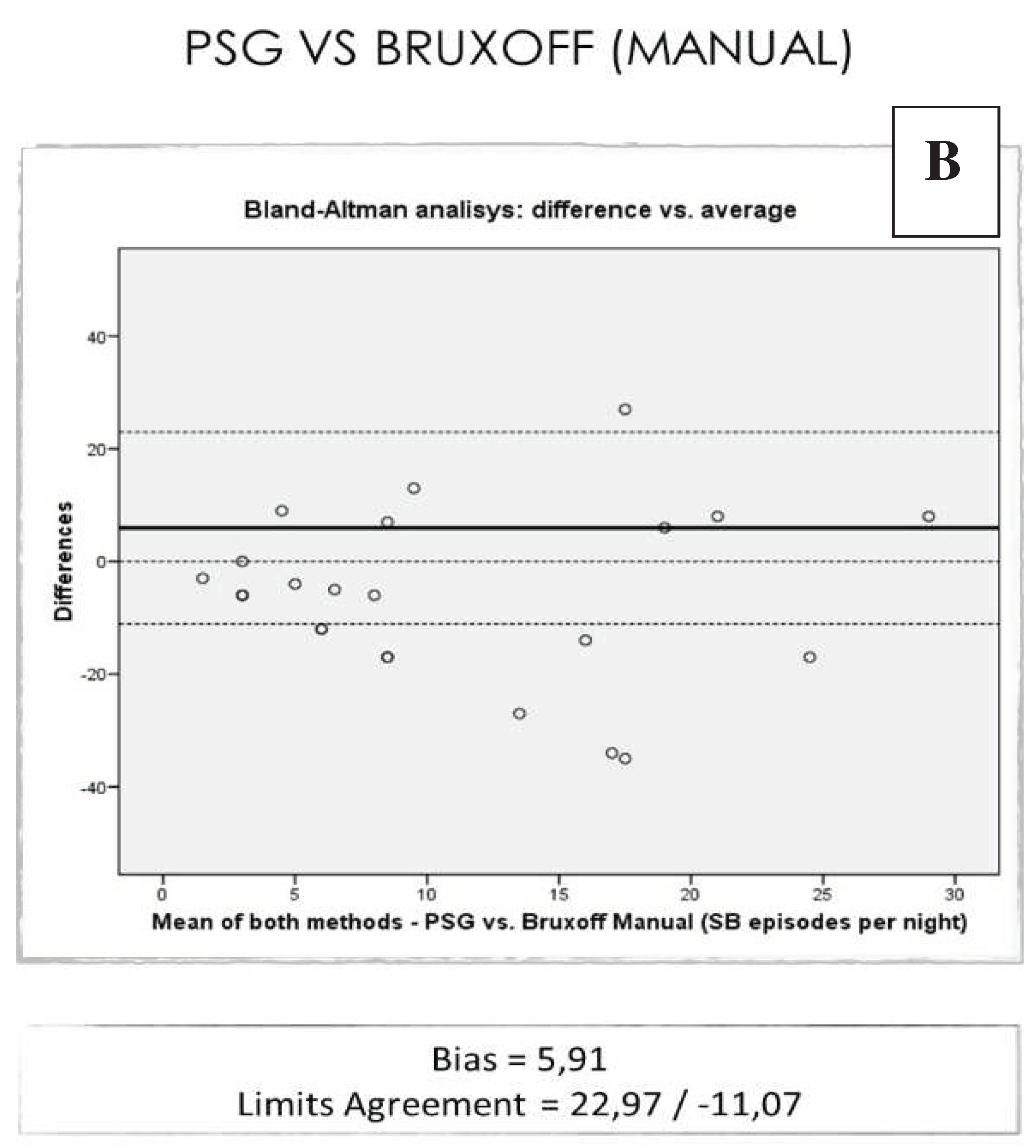
- There is no concordance between the results obtained in the PSG neurophysiologic analysis and those obtained by means of the EMG-EKG device automatic and manual analysis for the diagnosis of SB in a population mostly with OSA.
- There is EMG activity in OSA patients which could act as a confounding factor in the analysis of SB episodes with portable devices.
- It would be recommended to clarify the analysis scores to differentiate the muscle activity consecutive to the apnea episode from the masticatory muscle activity that meets the criteria for SB, especially for the programming of portable devices algorithms.
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Lobbezoo F, Ahlberg J, Raphael KG, Wetselaar P, Glaros AG, Kato T, et al. International consensus on the assessment of bruxism: Report of a work in progress. J Oral Rehabil 2018, 45, 837–844. [CrossRef]
- Carra MC, Bruni O, Huynh N. Topical review: sleep bruxism, headaches, and sleep-disordered breathing in children and adolescents. J Orofac Pain. 2021, 26, 267–276.
- Lavigne G, Manzini C, Huynh N. Sleep bruxism. In: Elsevier Saunders, editor. Principles and Practice of Sleep Medicine. 5th ed. St. Louis; 2011. p. 1129–39.
- Glaros AG. Incidence of diurnal and nocturnal bruxism. J Prosthet Dent. 1981, 45, 545–549. [CrossRef] [PubMed]
- Allen JD, Rivera-Morales WC, Zwemer JD. The Occurrence of Temporomandibular Disorder Symptoms in Healthy Young Adults With and Without Evidence of Bruxism. CRANIO®. 1990, 8, 312–318.
- Reding GR, Rubright WC, Zimmerman SO. Incidence of bruxism. J Dent Rest. 1866, 45, 1198–1204. [CrossRef]
- Laberge L, Tremblay RE, Vitaro F, Montplaisir J, PhD C. Development of Parasomnias From Childhood to Early Adolescence. Pediatrics 2000, 106, 67–74. [CrossRef] [PubMed]
- Manfredini D, Winocur E, Guarda-Nardini L, Paesani D, Lobbezoo F. Epidemiology of Bruxism in Adults: A Systematic Review of the Literature. J Orofac Pain. 2013, 27, 99–110. [CrossRef] [PubMed]
- Kato T, Mikami A, Sugita H, Muraki H, Okura M, Ohi M, et al. Negative association between self-reported jaw symptoms and apnea–hypopnea index in patients with symptoms of obstructive sleep apnea syndrome: a pilot study. Sleep and Breathing 2013, 17, 373–379. [CrossRef]
- Roehrs T, Carskadon MA, Dement WC, Roth T. Day- time sleepiness and alertness. In: Saunders, editor. Principles and Practice of Sleep Medicine. Philadelphia; 2000. p. 43–52.
- Bassiri AG, Guilleminault C. Clinical features and evaluation of obstructive sleep apnea–hypopnea syndrome. In: Saunders WB, editor. Principles and Practices of Sleep Medicine. Philadelphia; 2000. p. 869–78.
- Young T, Peppard PE, Gottlieb DJ. Epidemiology of Obstructive Sleep Apnea. Am J Respir Crit Care Med. 2002, 165, 1217–1239. [CrossRef]
- INOKO Y, SHIMIZU K, MORITA O, KOHNO M. Relationship between masseter muscle activity and sleep-disordered breathing. Sleep Biol Rhythms. 2004, 2, 67–68. [CrossRef]
- Saito M, Yamaguchi T, Mikami S, Watanabe K, Gotouda A, Okada K, et al. Temporal association between sleep apnea-hypopnea and sleep bruxism events. J Sleep Res. 2014, 23, 196–203. [CrossRef] [PubMed]
- Saito M, Yamaguchi T, Mikami S, Watanabe K, Gotouda A, Okada K, et al. Weak association between sleep bruxism and obstructive sleep apnea. A sleep laboratory study. Sleep and Breathing 2016, 20, 703–709. [CrossRef]
- Hosoya H, Kitaura H, Hashimoto T, Ito M, Kinbara M, Deguchi T, et al. Relationship between sleep bruxism and sleep respiratory events in patients with obstructive sleep apnea syndrome. Sleep and Breathing 2014, 18, 837–844. [CrossRef]
- da Costa Lopes AJ, Cunha TCA, Monteiro MCM, Serra-Negra JM, Cabral LC, Júnior PCS. Is there an association between sleep bruxism and obstructive sleep apnea syndrome? A systematic review. Sleep and Breathing 2020, 24, 913–921. [CrossRef] [PubMed]
- Manfredini D, Guarda-Nardini L, Marchese-Ragona R, Lobbezoo F. Theories on possible temporal relationships between sleep bruxism and obstructive sleep apnea events. An expert opinion. Sleep and Breathing 2015, 19, 1459–1465. [CrossRef] [PubMed]
- Tan M, Yap A, Chua A, Wong J, Parot M, Tan K. Prevalence of Sleep Bruxism and Its Association with Obstructive Sleep Apnea in Adult Patients: A Retrospective Polysomnographic Investigation. J Oral Facial Pain Headache 2019, 33, 269–277. [CrossRef]
- Castroflorio T, Deregibus A, Bargellini A, Debernardi C, Manfredini D. Detection of sleep bruxism: comparison between an electromyographic and electrocardiographic portable holter and polysomnography. J Oral Rehabil. 2014, 41, 163–169. [CrossRef]
- Manfredini D, Ahlberg J, Castroflorio T, Poggio CE, Guarda-Nardini L, Lobbezoo F. Diagnostic accuracy of portable instrumental devices to measure sleep bruxism: a systematic literature review of polysomnographic studies. J Oral Rehabil. 2014, 41, 836–842. [CrossRef]
- Winck M, Drummond M, Viana P, Pinho JC, Winck JC. Sleep bruxism associated with obstructive sleep apnoea syndrome – A pilot study using a new portable device. Revista Portuguesa de Pneumologia (English Edition). 2017 Jan;23(1):22–6.
- Sjöholm TT, Lowe AA, Miyamoto K, Fleetham JA, Ryan CF. Sleep bruxism in patients with sleep-disordered breathing. Arch Oral Biol 2000, 45, 889–896. [CrossRef]
- Lavigne G, Kato T, Herrero Babiloni A, Huynh N, Dal Fabbro C, Svensson P, et al. Research routes on improved sleep bruxism metrics: Toward a standardised approach. J Sleep Res. 2021 Oct 6;30(5). [CrossRef]
- The AASM Manual for the Scoring of Sleep and Associated Events. Vol. 2.6. 2020.
- Okeson JP, Phillips BA, Berry DT, Cook YR, Cabelka JF. Nocturnal bruxing events in subjects with sleep-disordered breathing and control subjects. J Craniomandib Disord. 1991;5(4)():258–64. [PubMed]
- Kato T, Blanchet PJ, Montplaisir JY, Lavigne GJ. Sleep bruxism and other disorders with orofacial activity during sleep. In: Butter-worth Heinemann, editor. Sleep and Movement Disorders. Philadelphia; 2003. p. 273–85.
- Lavigne GJ, Manzini C, Kato T. Sleep bruxism. Principles and practice of sleep medicine. 4th ed. Elsevier Saunder, editor. Philadelphia; 2005. 946–959 p.
- Miyawaki S, Lavigne GJ, Pierre M, Guitard F, Montplaisir JY, Kato T. Association between sleep bruxism, swallowing-related laryngeal movement, and sleep positions. Sleep. 2003 Jun 15;26(4)(PMID: 12841373):461–5. [CrossRef]
- Macaluso GM, Guerra P, Di Giovanni G, Boselli M, Parrino L, Terzano MG. Sleep Bruxism is a Disorder Related to Periodic Arousals During Sleep. J Dent Res. 1998 Apr 8;77(4):565–73. [CrossRef]
- Rundo JV, Downey R. Polysomnography. In 2019. p. 381–92.
- Lavigne GJ, Rompre PH, Montplaisir JY. Sleep Bruxism: Validity of Clinical Research Diagnostic Criteria in a Controlled Polysomnographic Study. J Dent Res. 1996 Jan 8;75(1):546–52. [CrossRef]
- Yanez-Regonesi F, Eisa E, Judge S, Carlson C, Okeson J, Moreno-Hay I. Diagnostic accuracy of a portable device (Bruxoff®) to measure sleep bruxism. J Oral Rehabil. 2023 Apr 25;50(4):258–66. [CrossRef]
- Castroflorio T, Deregibus A, Bargellini A, Debernardi C, Manfredini D. Detection of sleep bruxism: comparison between an electromyographic and electrocardiographic portable holter and polysomnography. J Oral Rehabil. 2014 Mar;41(3):163–9. [CrossRef]
- Deregibus A, Castroflorio T, Bargellini A, Debernardi C. Reliability of a portable device for the detection of sleep bruxism. Clin Oral Investig. 2014 Nov 28;18(8):2037–43. [CrossRef]
- von Elm E, Altman DG, Egger M, Pocock SJ, Gøtzsche PC, Vandenbroucke JP. The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) statement: guidelines for reporting observational studies. J Clin Epidemiol. 2008 Apr;61(4):344–9. [CrossRef]
- American Academy of Sleep Medicine. Sleep related breathing disorders in adults: Recommendations for syndrome definition and measurement techniques in clinical research. Sleep. 1999;22:667–89.
- Schiffman E, Ohrbach R, Truelove E, Look J, Anderson G, Goulet JP, et al. Diagnostic Criteria for Temporomandibular Disorders (DC/TMD) for Clinical and Research Applications: Recommendations of the International RDC/TMD Consortium Network* and Orofacial Pain Special Interest Group†. J Oral Facial Pain Headache. 2014 Jan;28(1):6–27. [CrossRef]
- De Leeuw R, Klasser GD. Orofacial Pain, Guidelines for assessment, diagnosis, and management. 5a ed. The American Academy of Orofacial Pain, editor. 2008.
- Lavigne GJ, Rompré PH, Poirier G, Huard H, Kato T, Montplaisir JY. Rhythmic Masticatory Muscle Activity during Sleep in Humans. J Dent Res. 2001 Feb 8;80(2):443–8. [CrossRef]
- Ward SLD. Principles and practice of sleep medicine, third edition. Edited by Meir H. Kryger, Thomas Roth, and William C. Dement. Philadelphia, W. B. Saunders Co., 2000, 1,336 pp. Pediatr Pulmonol. 2001 May;31(5):398–398.
- Kato T, Thie NM, Huynh N, Miyawaki S, Lavigne GJ. Topical review: sleep bruxism and the role of peripheral sensory influences. J Orofac Pain. 2003;Summer 17 (3)():191–213. [PubMed]
- Manfredini D, Ahlberg J, Wetselaar P, Svensson P, Lobbezoo F. The bruxism construct: From cut-off points to a continuum spectrum. J Oral Rehabil. 2019 Nov 2;46(11):991–7. [CrossRef]
- Raphael KG, Santiago V, Lobbezoo F. Is bruxism a disorder or a behaviour? Rethinking the international consensus on defining and grading of bruxism. J Oral Rehabil. 2016 Oct;43(10):791–8. [CrossRef]
- Ommerborn MA, Walentek N, Bergmann N, Franken M, Gotter A, Schäfer R. Validation of a new diagnostic method for quantification of sleep bruxism activity. Clin Oral Investig. 2022 Jun 23;26(6):4351–9. [CrossRef]
- Stuginski-Barbosa J, Porporatti AL, Costa YM, Svensson P, Conti PCR. Diagnostic validity of the use of a portable single-channel electromyography device for sleep bruxism. Sleep and Breathing. 2016 ;20(2):695–702. [CrossRef]
 |
 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




