Submitted:
27 June 2023
Posted:
27 June 2023
Read the latest preprint version here
Abstract
Keywords:
1. Introduction
2. Pediatric Spine Anatomy
2.1. Contrast to Adults
2.2. Skeletal Maturation
2.3. CNS Development
3. Pediatric SCI Epidemiology
3.1. Incidence
3.2. Etiology
3.3. Pathophysiology
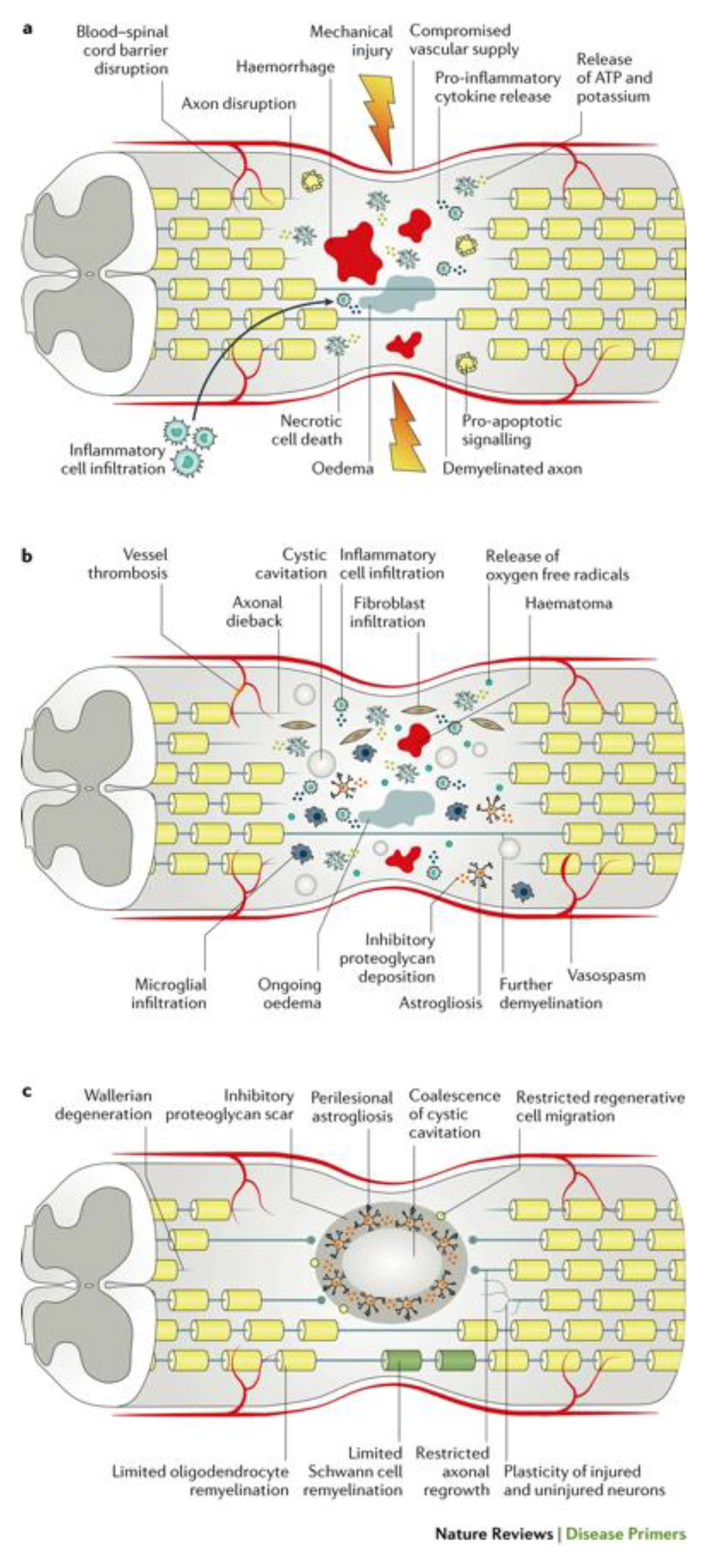
3.3.1. Traumatic SCI
3.3.1.1. Primary Injury
3.3.1.2. Secondary Injury
3.3.2. Non-Traumatic SCI
3.3.3. Developmental Variants and Anomalies
4. Pediatric SCI Diagnosis
4.1. X-ray, CT(A), MRI
4.2. Contrast to Adults
4.2.1. Upper Cervical Spine Injuries
4.2.1.1. Craniocervical Junction Injuries
4.2.1.2. Atlas Injuries
4.2.1.3. Atlanto-axial injuries
4.2.1.4. Axis Injuries
4.2.2. Subaxial Cervical Spine Injuries
4.3. SCIWORA
5. Pediatric SCI Classification
6. Pediatric SCI Management
6.1. Steroidal Therapy
6.2. Cardiovascular Management
6.3. Surgical Timing
7. Complication Management
7.1. VTE Prophylaxis
7.2. Autonomic Dysreflexia (AD)
7.3. Pain and Spasticity
7.4. Bowel and Bladder
7.5. Spinal Deformity and Hip Dislocation
7.6. Hypercalcemia
8. Pediatric SCI Recovery
8.1. Rehabilitation
9. Experimental Research and Future Treatments
9.1. Cell-Based Therapies:
9.1.1. Neural Stem Cells (NSCs):
9.1.2. Mesenchymal Stem Cells (MSCs):
9.1.3. Olfactory Ensheathing Cells (OECs):
9.1.4. Schwann Cells:
9.2. Biomaterial Scaffolds:
9.2.1. QL6
9.2.2. Hyaluronan/Methylcellulose (HAMC)
9.2.3. Granulocyte Colony-Stimulating Factor (G-CSF)
9.3. Trials
9.4. Functional Electrical Stimulation
References
- Dowdell, J.; Mikhail, C.; Robinson, J.; Allen, A. Anatomy of the Pediatric Spine and Spine Injuries in Young Athletes. Ann. Jt. 2018, 3. [Google Scholar] [CrossRef]
- Gupta, A.; Saha, U. Spinal Anesthesia in Children: A Review. J. Anaesthesiol. Clin. Pharmacol. 2014, 30, 10–18. [Google Scholar] [CrossRef]
- Sanders, J.O. Normal Growth of the Spine and Skeletal Maturation. Semin. Spine Surg. 2015, 27, 16–20. [Google Scholar] [CrossRef]
- Skórzewska, A.; Grzymisławska, M.; Bruska, M.; Lupicka, J.; Woźniak, W. Ossification of the Vertebral Column in Human Foetuses: Histological and Computed Tomography Studies. Folia Morphol. 2013, 72, 230–238. [Google Scholar] [CrossRef]
- Zhang, Y.; Al Mamun, A.; Yuan, Y.; Lu, Q.; Xiong, J.; Yang, S.; Wu, C.; Wu, Y.; Wang, J. Acute Spinal Cord Injury: Pathophysiology and Pharmacological Intervention (Review). Mol. Med. Rep. 2021, 23, 417. [Google Scholar] [CrossRef] [PubMed]
- Copp, A.J.; Greene, N.D.E. Genetics and Development of Neural Tube Defects. J. Pathol. 2010, 220, 217–230. [Google Scholar] [CrossRef]
- Obernier, K.; Alvarez-Buylla, A. Neural Stem Cells: Origin, Heterogeneity and Regulation in the Adult Mammalian Brain. Dev. Camb. Engl. 2019, 146, dev156059. [Google Scholar] [CrossRef] [PubMed]
- Mandai, K.; Rikitake, Y.; Mori, M.; Takai, Y. Nectins and Nectin-Like Molecules in Development and Disease. Curr. Top. Dev. Biol. 2015, 112, 197–231. [Google Scholar] [CrossRef]
- National Institute on Disability and Rehabilitation Research, O. 9. National Institute on Disability and Rehabilitation Research, O. of S. E. and R. Services. U. S. D. of Education. 2004 Annual Statistical Report for the Model Spinal Cord Injury Care System, 2004. Available online: https://www.nscisc.uab.edu/PublicDocuments/reports/pdf/2004StatReport.pdf.
- Parent, S.; Mac-Thiong, J.-M.; Roy-Beaudry, M.; Sosa, J.F.; Labelle, H. Spinal Cord Injury in the Pediatric Population: A Systematic Review of the Literature. J. Neurotrauma 2011, 28, 1515–1524. [Google Scholar] [CrossRef]
- Apple, D.F.; Anson, C.A.; Hunter, J.D.; Bell, R.B. Spinal Cord Injury in Youth. Clin. Pediatr. (Phila.) 1995, 34, 90–95. [Google Scholar] [CrossRef]
- Caird, M.S.; Reddy, S.; Ganley, T.J.; Drummond, D.S. Cervical Spine Fracture-Dislocation Birth Injury: Prevention, Recognition, and Implications for the Orthopaedic Surgeon. J. Pediatr. Orthop. 2005, 25, 484–486. [Google Scholar] [CrossRef]
- Lee, C.-C.; Chou, I.-J.; Chang, Y.-J.; Chiang, M.-C. Unusual Presentations of Birth Related Cervical Spinal Cord Injury. Front. Pediatr. 2020, 8, 514. [Google Scholar] [CrossRef] [PubMed]
- Jain, N.B.; Ayers, G.D.; Peterson, E.N.; Harris, M.B.; Morse, L.; O’Connor, K.C.; Garshick, E. Traumatic Spinal Cord Injury in the United States, 1993-2012. JAMA 2015, 313, 2236–2243. [Google Scholar] [CrossRef] [PubMed]
- Klimo, P.; Rao, G.; Brockmeyer, D. Congenital Anomalies of the Cervical Spine. Neurosurg. Clin. N. Am. 2007, 18, 463–478. [Google Scholar] [CrossRef] [PubMed]
- Spinal Cord Injury. National Institute of Neurological Disorders and Stroke. Available online: https://www.ninds.nih.gov/health-information/disorders/spinal-cord-injury (accessed on 11 June 2023).
- Brown, R.L.; Brunn, M.A.; Garcia, V.F. Cervical Spine Injuries in Children: A Review of 103 Patients Treated Consecutively at a Level 1 Pediatric Trauma Center. J. Pediatr. Surg. 2001, 36, 1107–1114. [Google Scholar] [CrossRef]
- Karthikeyan, V.; Breitbart, S.C.; Malhotra, A.K.; Fung, A.; Short, E.; Schmitz, A.; Lebel, D.E.; Ibrahim, G.M. Management of Perinatal Cervical Spine Injury Using Custom-Fabricated External Orthoses: Design Considerations, Narrative Literature Review, and Experience from the Hospital for Sick Children. Illustrative Cases. J. Neurosurg. Case Lessons 2023, 5. [Google Scholar] [CrossRef]
- David, G.; Mohammadi, S.; Martin, A.R.; Cohen-Adad, J.; Weiskopf, N.; Thompson, A.; Freund, P. Traumatic and Nontraumatic Spinal Cord Injury: Pathological Insights from Neuroimaging. Nat. Rev. Neurol. 2019, 15, 718–731. [Google Scholar] [CrossRef] [PubMed]
- Ahuja, C.S.; Wilson, J.R.; Nori, S.; Kotter, M.R.N.; Druschel, C.; Curt, A.; Fehlings, M.G. Traumatic Spinal Cord Injury. Nat. Rev. Dis. Primer 2017, 3, 1–21. [Google Scholar] [CrossRef]
- Anjum, A.; Yazid, M.D.; Fauzi Daud, M.; Idris, J.; Ng, A.M.H.; Selvi Naicker, A.; Ismail, O.H.R.; Athi Kumar, R.K.; Lokanathan, Y. Spinal Cord Injury: Pathophysiology, Multimolecular Interactions, and Underlying Recovery Mechanisms. Int. J. Mol. Sci. 2020, 21, 7533. [Google Scholar] [CrossRef]
- Hausmann, O.N. Post-Traumatic Inflammation Following Spinal Cord Injury. Spinal Cord 2003, 41, 369–378. [Google Scholar] [CrossRef]
- Schwab, J.M.; Zhang, Y.; Kopp, M.A.; Brommer, B.; Popovich, P.G. The Paradox of Chronic Neuroinflammation, Systemic Immune Suppression, Autoimmunity after Traumatic Chronic Spinal Cord Injury. Exp. Neurol. 2014, 258, 121–129. [Google Scholar] [CrossRef]
- Tator, C.H.; Fehlings, M.G. Review of the Secondary Injury Theory of Acute Spinal Cord Trauma with Emphasis on Vascular Mechanisms. J. Neurosurg. 1991, 75, 15–26. [Google Scholar] [CrossRef]
- Silver, J.; Miller, J.H. Regeneration beyond the Glial Scar. Nat. Rev. Neurosci. 2004, 5, 146–156. [Google Scholar] [CrossRef]
- Sofroniew, M.V. Reactive Astrocytes in Neural Repair and Protection. Neurosci. Rev. J. Bringing Neurobiol. Neurol. Psychiatry 2005, 11, 400–407. [Google Scholar] [CrossRef] [PubMed]
- Osorio, M.; Reyes, M.R.; Massagli, T.L. Pediatric Spinal Cord Injury. Curr. Phys. Med. Rehabil. Rep. 2014, 2, 158–168. [Google Scholar] [CrossRef]
- O’Brien, W.T.; Shen, P.; Lee, P. The Dens: Normal Development, Developmental Variants and Anomalies, and Traumatic Injuries. J. Clin. Imaging Sci. 2015, 5, 38. [Google Scholar] [CrossRef] [PubMed]
- Karwacki, G.M.; Schneider, J.F. Normal Ossification Patterns of Atlas and Axis: A CT Study. AJNR Am J Neuroradiol 2012, 33, 1882–1887. [Google Scholar] [CrossRef] [PubMed]
- Piatt, J.H.; Grissom, L.E. Developmental Anatomy of the Atlas and Axis in Childhood by Computed Tomography. J. Neurosurg. Pediatr. 2011, 8, 235–243. [Google Scholar] [CrossRef]
- Sherk, H.H.; Nicholson, J.T.; Chung, S.M. Fractures of the Odontoid Process in Young Children. J. Bone Joint Surg. Am. 1978, 60, 921–924. [Google Scholar] [CrossRef]
- McGrory, B.J.; Klassen, R.A.; Chao, E.Y.; Staeheli, J.W.; Weaver, A.L. Acute Fractures and Dislocations of the Cervical Spine in Children and Adolescents. J. Bone Joint Surg. Am. 1993, 75, 988–995. [Google Scholar] [CrossRef]
- Connolly, B.; Emery, D.; Armstrong, D. The Odontoid Synchondrotic Slip: An Injury Unique to Young Children. Pediatr. Radiol. 1995, 25 Suppl 1, S129–133. [Google Scholar] [CrossRef]
- Brenner, D.; Elliston, C.; Hall, E.; Berdon, W. Estimated Risks of Radiation-Induced Fatal Cancer from Pediatric CT. AJR Am. J. Roentgenol. 2001, 176, 289–296. [Google Scholar] [CrossRef]
- Rozzelle, C.J.; Aarabi, B.; Dhall, S.S.; Gelb, D.E.; Hurlbert, R.J.; Ryken, T.C.; Theodore, N.; Walters, B.C.; Hadley, M.N. Management of Pediatric Cervical Spine and Spinal Cord Injuries. Neurosurgery 2013, 72 Suppl 2, 205–226. [Google Scholar] [CrossRef]
- Herman, M.J.; Brown, K.O.; Sponseller, P.D.; Phillips, J.H.; Petrucelli, P.M.; Parikh, D.J.; Mody, K.S.; Leonard, J.C.; Moront, M.; Brockmeyer, D.L.; Anderson, R.C.E.; Alder, A.C.; Anderson, J.T.; Bernstein, R.M.; Booth, T.N.; Braga, B.P.; Cahill, P.J.; Joglar, J.M.; Martus, J.E.; Nesiama, J.-A. O.; Pahys, J.M.; Rathjen, K.E.; Riccio, A.I.; Schulz, J.F.; Stans, A.A.; Shah, M.I.; Warner, W.C.; Yaszay, B. Pediatric Cervical Spine Clearance: A Consensus Statement and Algorithm from the Pediatric Cervical Spine Clearance Working Group. J. Bone Joint Surg. Am. 2019, 101, e1. [Google Scholar] [CrossRef]
- Hadley, M.N.; Zabramski, J.M.; Browner, C.M.; Rekate, H.; Sonntag, V.K. Pediatric Spinal Trauma. Review of 122 Cases of Spinal Cord and Vertebral Column Injuries. J. Neurosurg. 1988, 68, 18–24. [Google Scholar] [CrossRef]
- Mahan, S.T.; Mooney, D.P.; Karlin, L.I.; Hresko, M.T. Multiple Level Injuries in Pediatric Spinal Trauma. J. Trauma 2009, 67, 537–542. [Google Scholar] [CrossRef]
- Viccellio, P.; Simon, H.; Pressman, B.D.; Shah, M.N.; Mower, W.R.; Hoffman, J.R.; NEXUS Group. A Prospective Multicenter Study of Cervical Spine Injury in Children. Pediatrics 2001, 108, E20. [Google Scholar] [CrossRef] [PubMed]
- Alexiades, N.G.; Parisi, F.; Anderson, R.C.E. Pediatric Spine Trauma: A Brief Review. Neurosurgery 2020, 87, E1–E9. [Google Scholar] [CrossRef]
- Hadley, M.N.; Walters, B.C.; Grabb, P.A.; Oyesiku, N.M.; Przybylski, G.J.; Resnick, D.K.; Ryken, T.C. Management of Pediatric Cervical Spine and Spinal Cord Injuries. Neurosurgery 2002, 50 (Suppl 3), S85–99. [Google Scholar] [CrossRef] [PubMed]
- Ralston, M.E.; Chung, K.; Barnes, P.D.; Emans, J.B.; Schutzman, S.A. Role of Flexion-Extension Radiographs in Blunt Pediatric Cervical Spine Injury. Acad. Emerg. Med. Off. J. Soc. Acad. Emerg. Med. 2001, 8, 237–245. [Google Scholar] [CrossRef] [PubMed]
- Lui, T.N.; Lee, S.T.; Wong, C.W.; Yeh, Y.S.; Tzaan, W.C.; Chen, T.Y.; Hung, S.Y. C1-C2 Fracture-Dislocations in Children and Adolescents. J. Trauma 1996, 40, 408–411. [Google Scholar] [CrossRef]
- Pang, D.; Nemzek, W.R.; Zovickian, J. Atlanto-Occipital Dislocation: Part 1--Normal Occipital Condyle-C1 Interval in 89 Children. Neurosurgery 2007, 61, 514–521. [Google Scholar] [CrossRef]
- Berne, J.D.; Velmahos, G.C.; El-Tawil, Q.; Demetriades, D.; Asensio, J.A.; Murray, J.A.; Cornwell, E.E.; Belzberg, H.; Berne, T.V. Value of Complete Cervical Helical Computed Tomographic Scanning in Identifying Cervical Spine Injury in the Unevaluable Blunt Trauma Patient with Multiple Injuries: A Prospective Study. J. Trauma 1999, 47, 896–902. [Google Scholar] [CrossRef] [PubMed]
- Anderson, F.A.; Wheeler, H.B.; Goldberg, R.J.; Hosmer, D.W.; Patwardhan, N.A.; Jovanovic, B.; Forcier, A.; Dalen, J.E. A Population-Based Perspective of the Hospital Incidence and Case-Fatality Rates of Deep Vein Thrombosis and Pulmonary Embolism. The Worcester DVT Study. Arch. Intern. Med. 1991, 151, 933–938. [Google Scholar] [CrossRef]
- Achildi, O.; Betz, R.R.; Grewal, H. Lapbelt Injuries and the Seatbelt Syndrome in Pediatric Spinal Cord Injury. J. Spinal Cord Med. 2007, 30 (Suppl 1), S21–S24. [Google Scholar] [CrossRef]
- Wang, J.-Z.; Yang, M.; Meng, M.; Li, Z.-H. Clinical Characteristics and Treatment of Spinal Cord Injury in Children and Adolescents. Chin. J. Traumatol. Zhonghua Chuang Shang Za Zhi 2023, 26, 8–13. [Google Scholar] [CrossRef]
- McAllister, A.S.; Nagaraj, U.; Radhakrishnan, R. Emergent Imaging of Pediatric Cervical Spine Trauma | RadioGraphics, 2019. [CrossRef]
- Nypaver, M.; Treloar, D. Neutral Cervical Spine Positioning in Children. Ann. Emerg. Med. 1994, 23, 208–211. [Google Scholar] [CrossRef] [PubMed]
- Leonard, J.R.; Jaffe, D.M.; Kuppermann, N.; Olsen, C.S.; Leonard, J.C. Cervical Spine Injury Patterns in Children | Pediatrics | American Academy of Pediatrics. Pediatrics 2014, 133, e1179–e1188. [Google Scholar] [CrossRef]
- Plessis, J.-P. du; Dix-Peek, S.; Hoffman, E.B.; Wieselthaler, N.; Dunn, R.N. Pediatric Atlanto-Occipital Dissociation: Radiographic Findings and Clinical Outcome. Evid.-Based Spine-Care J. 2012, 03, 019–026. [Google Scholar] [CrossRef] [PubMed]
- Beckmann, N.M.; Chinapuvvula, N.R.; Zhang, X.; West, O.C. Epidemiology and Imaging Classification of Pediatric Cervical Spine Injuries: 12-Year Experience at a Level 1 Trauma Center. Am. J. Roentgenol. 2020, 214, 1359–1368. [Google Scholar] [CrossRef]
- Neeman, Z.; Bloom, A.I. Occipital Condyle Fractures in the Pediatric Population. RadioGraphics 2003, 23, 1699–1701. [Google Scholar] [CrossRef]
- Junewick, J.J. Pediatric Craniocervical Junction Injuries | AJR. Pediatr. Imaging 2011, 196. [Google Scholar]
- Riascos, R.; Bonfante, E.; Cotes, C.; Guirguis, M.; Hakimelahi, R.; West, C. Imaging of Atlanto-Occipital and Atlantoaxial Traumatic Injuries: What the Radiologist Needs to Know. RadioGraphics 2015, 35, 2121–2134. [Google Scholar] [CrossRef] [PubMed]
- Karkos, P.D.; Benton, J.; Leong, S.C.; Mushi, E.; Sivaji, N.; Assimakopoulos, D.A. Grisel’s Syndrome in Otolaryngology: A Systematic Review. Int. J. Pediatr. Otorhinolaryngol. 2007, 71, 1823–1827. [Google Scholar] [CrossRef] [PubMed]
- Fielding, J.W.; Hawkins, R.J. Atlanto-Axial Rotatory Fixation. (Fixed Rotatory Subluxation of the Atlanto-Axial Joint). J. Bone Joint Surg. Am. 1977, 59, 37–44. [Google Scholar] [CrossRef]
- Ghanem, I.; El Hage, S.; Rachkidi, R.; Kharrat, K.; Dagher, F.; Kreichati, G. Pediatric Cervical Spine Instability. J. Child. Orthop. 2008, 2, 71–84. [Google Scholar] [CrossRef]
- Arvin, B.; Fournier-Gosselin, M.-P.; Fehlings, M.G. Os Odontoideum: Etiology and Surgical Management. Neurosurgery 2010, 66, A22. [Google Scholar] [CrossRef]
- Shaw, M.; Burnett, H.; Wilson, A.; Chan, O. Pseudosubluxation of C2 on C3 in Polytraumatized Children — Prevalence and Significance. Clin. Radiol. 1999, 54, 377–380. [Google Scholar] [CrossRef] [PubMed]
- Vaccaro, A.R.; Koerner, J.D.; Radcliff, K.E.; Oner, F.C.; Reinhold, M.; Schnake, K.J.; Kandziora, F.; Fehlings, M.G.; Dvorak, M.F.; Aarabi, B.; Rajasekaran, S.; Schroeder, G.D.; Kepler, C.K.; Vialle, L.R. AOSpine Subaxial Cervical Spine Injury Classification System | SpringerLink. Eur. Spine J. 2015, 25, 2173–2184. [Google Scholar] [CrossRef]
- Swischuk, L.E.; Swischuk, P.N.; John, S.D. Wedging of C-3 in Infants and Children: Usually a Normal Finding and Not a Fracture. Radiology 1993, 188, 523–526. [Google Scholar] [CrossRef]
- Wang, M.X.; Beckmann, N.M. Imaging of Pediatric Cervical Spine Trauma. Emerg. Radiol. 2021, 28, 127–141. [Google Scholar] [CrossRef] [PubMed]
- Farrell, C.A.; Hannon, M.; Lee, L.K. Pediatric Spinal Cord Injury without Radiographic Abnormality in the Era of Advanced Imaging. Curr. Opin. Pediatr. 2017, 29, 286–290. [Google Scholar] [CrossRef]
- Shen, H.; Tang, Y.; Huang, L.; Yang, R.; Wu, Y.; Wang, P.; Shi, Y.; He, X.; Liu, H.; Ye, J. Applications of Diffusion-Weighted MRI in Thoracic Spinal Cord Injury without Radiographic Abnormality. Int. Orthop. 2007, 31, 375–383. [Google Scholar] [CrossRef]
- Pittman, T.; Bucholz, R.; Williams, D. Efficacy of Barbiturates in the Treatment of Resistant Intracranial Hypertension in Severely Head-Injured Children. Pediatr. Neurosci. 1989, 15, 13–17. [Google Scholar] [CrossRef]
- Dickman, C.A.; Zabramski, J.M.; Hadley, M.N.; Rekate, H.L.; Sonntag, V.K. Pediatric Spinal Cord Injury without Radiographic Abnormalities: Report of 26 Cases and Review of the Literature. J. Spinal Disord. 1991, 4, 296–305. [Google Scholar] [CrossRef]
- Pang, D. Spinal Cord Injury without Radiographic Abnormality in Children, 2 Decades Later. Neurosurgery 2004, 55, 1325–1342. [Google Scholar] [CrossRef] [PubMed]
- Rozzelle, C.J.; Aarabi, B.; Dhall, S.S.; Gelb, D.E.; Hurlbert, R.J.; Ryken, T.C.; Theodore, N.; Walters, B.C.; Hadley, M.N. Spinal Cord Injury without Radiographic Abnormality (SCIWORA). Neurosurgery 2013, 72 Suppl 2, 227–233. [Google Scholar] [CrossRef]
- International Standards for Neurological Classification of SCI (ISNCSCI) Worksheet. American Spinal Injury Association. Available online: https://asia-spinalinjury.org/international-standards-neurological-classification-sci-isncsci-worksheet/ (accessed on 11 June 2023).
- Mulcahey, M.J.; Gaughan, J.P.; Chafetz, R.S.; Vogel, L.C.; Samdani, A.F.; Betz, R.R. Interrater Reliability of the International Standards for Neurological Classification of Spinal Cord Injury in Youths with Chronic Spinal Cord Injury. Arch. Phys. Med. Rehabil. 2011, 92, 1264–1269. [Google Scholar] [CrossRef] [PubMed]
- Mulcahey, M.J.; Calhoun, C.L.; Sinko, R.; Kelly, E.H.; Vogel, L.C. The Spinal Cord Independence Measure (SCIM)-III Self Report for Youth. Spinal Cord 2016, 54, 204–212. [Google Scholar] [CrossRef]
- Benmelouka, A.; Shamseldin, L.S.; Nourelden, A.Z.; Negida, A. A Review on the Etiology and Management of Pediatric Traumatic Spinal Cord Injuries. Adv. J. Emerg. Med. 2019, 4, e28. [Google Scholar] [CrossRef] [PubMed]
- Seid, T.; Ramaiah, R.; Grabinsky, A. Pre–Hospital Care of Pediatric Patients with Trauma. Int. J. Crit. Illn. Inj. Sci. 2012, 2, 114–120. [Google Scholar] [CrossRef]
- Wang, M.Y.; Hoh, D.J.; Leary, S.P.; Griffith, P.; McComb, J.G. High Rates of Neurological Improvement Following Severe Traumatic Pediatric Spinal Cord Injury. Spine 2004, 29, 1493–1497. [Google Scholar] [CrossRef]
- Spinal Cord Injury in Children - Injuries; Poisoning. Merck Manuals Professional Edition. Available online: https://www.merckmanuals.com/en-ca/professional/injuries-poisoning/spinal-trauma/spinal-cord-injury-in-children (accessed on 12 June 2023).
- Caruso, M.C.; Daugherty, M.C.; Moody, S.M.; Falcone, R.A.; Bierbrauer, K.S.; Geis, G.L. Lessons Learned from Administration of High-Dose Methylprednisolone Sodium Succinate for Acute Pediatric Spinal Cord Injuries. J. Neurosurg. Pediatr. 2017, 20, 567–574. [Google Scholar] [CrossRef] [PubMed]
- Fehlings, M.G.; Tetreault, L.A.; Wilson, J.R.; Kwon, B.K.; Burns, A.S.; Martin, A.R.; Hawryluk, G.; Harrop, J.S. A Clinical Practice Guideline for the Management of Acute Spinal Cord Injury: Introduction, Rationale, and Scope. Glob. Spine J. 2017, 7 (Suppl 3), 84S–94S. [Google Scholar] [CrossRef] [PubMed]
- Zeng, L.; Wang, Y.-L.; Shen, X.-T.; Zhang, Z.-C.; Huang, G.-X.; Alshorman, J.; Serebour, T.B.; Tator, C.H.; Sun, T.-S.; Zhang, Y.-Z.; Guo, X.-D.; Chinese Orthopaedic Association; Spinal Cord Injury and Rehabilitation Group; Chinese Association of Rehabilitation Medicine; Group of Spinal Injury and Functional Reconstruction; Neuroregeneration & Neurorestoration Professional Committee; Association of Chinese Research Hospital; Sino-Canada Spinal and Spinal Cord Injury Center. Guidelines for Management of Pediatric Acute Hyperextension Spinal Cord Injury. Chin. J. Traumatol. Zhonghua Chuang Shang Za Zhi 2023, 26, 2–7. [Google Scholar] [CrossRef] [PubMed]
- Arora, B.; Suresh, S. Spinal Cord Injuries in Older Children: Is There a Role for High-Dose Methylprednisolone? Pediatr Emerg Care 2011, 27, 1192–1194. [Google Scholar] [CrossRef]
- Lemley, K.; Bauer, P. Pediatric Spinal Cord Injury: Recognition of Injury and Initial Resuscitation, in Hospital Management, and Coordination of Care. J. Pediatr. Intensive Care 2015, 4, 27–34. [Google Scholar] [CrossRef]
- Gerardi, M.J.; Sacchetti, A.D.; Cantor, R.M.; Santamaria, J.P.; Gausche, M.; Lucid, W.; Foltin, G.L. Rapid-Sequence Intubation of the Pediatric Patient. Pediatric Emergency Medicine Committee of the American College of Emergency Physicians. Ann. Emerg. Med. 1996, 28, 55–74. [Google Scholar] [CrossRef]
- Squair, J.W.; Bélanger, L.M.; Tsang, A.; Ritchie, L.; Mac-Thiong, J.-M.; Parent, S.; Christie, S.; Bailey, C.; Dhall, S.; Street, J.; Ailon, T.; Paquette, S.; Dea, N.; Fisher, C.G.; Dvorak, M.F.; West, C.R.; Kwon, B.K. Spinal Cord Perfusion Pressure Predicts Neurologic Recovery in Acute Spinal Cord Injury. Neurology 2017, 89, 1660–1667. [Google Scholar] [CrossRef]
- Walters, B.C.; Hadley, M.N.; Hurlbert, R.J.; Aarabi, B.; Dhall, S.S.; Gelb, D.E.; Harrigan, M.R.; Rozelle, C.J.; Ryken, T.C.; Theodore, N.; American Association of Neurological Surgeons; Congress of Neurological Surgeons. Guidelines for the Management of Acute Cervical Spine and Spinal Cord Injuries: 2013 Update. Neurosurgery 2013, 60 (CN_suppl_1), 82–91. [Google Scholar] [CrossRef]
- Aarabi, B.; Akhtar-Danesh, N.; Chryssikos, T.; Shanmuganathan, K.; Schwartzbauer, G.T.; Simard, J.M.; Olexa, J.; Sansur, C.A.; Crandall, K.M.; Mushlin, H.; Kole, M.J.; Le, E.J.; Wessell, A.P.; Pratt, N.; Cannarsa, G.; Lomangino, C.; Scarboro, M.; Aresco, C.; Oliver, J.; Caffes, N.; Carbine, S.; Mori, K. Efficacy of Ultra-Early (< 12 h), Early (12-24 h), and Late (>24-138.5 h) Surgery with Magnetic Resonance Imaging-Confirmed Decompression in American Spinal Injury Association Impairment Scale Grades A, B, and C Cervical Spinal Cord Injury. J. Neurotrauma 2020, 37, 448–457. [Google Scholar] [CrossRef] [PubMed]
- Du, J.P.; Fan, Y.; Liu, J.J.; Zhang, J.N.; Meng, Y.B.; Mu, C.C.; Hao, D.J. Decompression for Traumatic Thoracic/Thoracolumbar Incomplete Spinal Cord Injury: Application of AO Spine Injury Classification System to Identify the Timing of Operation. World Neurosurg. 2018, 116, e867–e873. [Google Scholar] [CrossRef]
- Haghnegahdar, A.; Behjat, R.; Saadat, S.; Badhiwala, J.; Farrokhi, M.R.; Niakan, A.; Eghbal, K.; Barzideh, E.; Shahlaee, A.; Ghaffarpasand, F.; Ghodsi, Z.; Vaccaro, A.R.; Sadeghi-Naini, M.; Fehlings, M.G.; Guest, J.D.; Derakhshan, P.; Rahimi-Movaghar, V. A Randomized Controlled Trial of Early versus Late Surgical Decompression for Thoracic and Thoracolumbar Spinal Cord Injury in 73 Patients. Neurotrauma Rep. 2020, 1, 78–87. [Google Scholar] [CrossRef] [PubMed]
- Qadir, I.; Riew, K.D.; Alam, S.R.; Akram, R.; Waqas, M.; Aziz, A. Timing of Surgery in Thoracolumbar Spine Injury: Impact on Neurological Outcome. Glob. Spine J. 2020, 10, 826–831. [Google Scholar] [CrossRef] [PubMed]
- Silverstein, M.D.; Heit, J.A.; Mohr, D.N.; Petterson, T.M.; O’Fallon, W.M.; Melton, L.J. Trends in the Incidence of Deep Vein Thrombosis and Pulmonary Embolism: A 25-Year Population-Based Study. Arch. Intern. Med. 1998, 158, 585–593. [Google Scholar] [CrossRef]
- Thompson, A.J.; McSwain, S.D.; Webb, S.A.; Stroud, M.A.; Streck, C.J. Venous Thromboembolism Prophylaxis in the Pediatric Trauma Population. J. Pediatr. Surg. 2013, 48, 1413–1421. [Google Scholar] [CrossRef]
- Jones, T.; Ugalde, V.; Franks, P.; Zhou, H.; White, R.H. Venous Thromboembolism after Spinal Cord Injury: Incidence, Time Course, and Associated Risk Factors in 16,240 Adults and Children. Arch. Phys. Med. Rehabil. 2005, 86, 2240–2247. [Google Scholar] [CrossRef]
- Hauser, B.M.; Hoffman, S.E.; Gupta, S.; Zaki, M.M.; Xu, E.; Chua, M.; Bernstock, J.D.; Khawaja, A.; Smith, T.R.; Proctor, M.R.; Zaidi, H.A. Association of Venous Thromboembolism Following Pediatric Traumatic Spinal Injuries with Injury Severity and Longer Hospital Stays. J. Neurosurg. Spine 2022, 36, 153–159. [Google Scholar] [CrossRef]
- Consortium for Spinal Cord Medicine. Prevention of Venous Thromboembolism in Individuals with Spinal Cord Injury: Clinical Practice Guidelines for Health Care Providers, 3rd Ed.: Consortium for Spinal Cord Medicine. Top. Spinal Cord Inj. Rehabil. 2016, 22, 209–240. [Google Scholar] [CrossRef]
- Vogel, L.C.; Lubicky, J.P. Lower Extremity Compartment Syndrome in an Adolescent with Spinal Cord Injury. J. Spinal Cord Med. 2001, 24, 278–283. [Google Scholar] [CrossRef]
- Monagle, P.; Chan, A.K.C.; Goldenberg, N.A.; Ichord, R.N.; Journeycake, J.M.; Nowak-Göttl, U.; Vesely, S.K. Antithrombotic Therapy in Neonates and Children: Antithrombotic Therapy and Prevention of Thrombosis, 9th Ed: American College of Chest Physicians Evidence-Based Clinical Practice Guidelines. Chest 2012, 141 (2 Suppl), e737S–e801S. [Google Scholar] [CrossRef] [PubMed]
- Schottler, J.; Vogel, L.C.; Sturm, P. Spinal Cord Injuries in Young Children: A Review of Children Injured at 5 Years of Age and Younger. Dev. Med. Child Neurol. 2012, 54, 1138–1143. [Google Scholar] [CrossRef]
- Lakra, C.; Swayne, O.; Christofi, G.; Desai, M. Autonomic Dysreflexia in Spinal Cord Injury. Pract. Neurol. 2021, 21, 532–538. [Google Scholar] [CrossRef] [PubMed]
- Eldahan, K.C.; Rabchevsky, A.G. Autonomic Dysreflexia after Spinal Cord Injury: Systemic Pathophysiology and Methods of Management. Auton. Neurosci. Basic Clin. 2018, 209, 59–70. [Google Scholar] [CrossRef] [PubMed]
- Hickey, K.J.; Vogel, L.C.; Willis, K.M.; Anderson, C.J. Prevalence and Etiology of Autonomic Dysreflexia in Children with Spinal Cord Injuries. J. Spinal Cord Med. 2004, 27 Suppl 1, S54–60. [Google Scholar] [CrossRef]
- Allen, K.J.; Leslie, S.W. Autonomic Dysreflexia. In StatPearls; StatPearls Publishing: Treasure Island (FL), 2023. [Google Scholar]
- Wan, D.; Krassioukov, A.V. Life-Threatening Outcomes Associated with Autonomic Dysreflexia: A Clinical Review. J. Spinal Cord Med. 2014, 37, 2–10. [Google Scholar] [CrossRef]
- Thomas, A.X.; Riviello, J.J.; Davila-Williams, D.; Thomas, S.P.; Erklauer, J.C.; Bauer, D.F.; Cokley, J.A. Pharmacologic and Acute Management of Spinal Cord Injury in Adults and Children. Curr. Treat. Options Neurol. 2022, 24, 285–304. [Google Scholar] [CrossRef]
- Colloca, L.; Ludman, T.; Bouhassira, D.; Baron, R.; Dickenson, A.H.; Yarnitsky, D.; Freeman, R.; Truini, A.; Attal, N.; Finnerup, N.B.; Eccleston, C.; Kalso, E.; Bennett, D.L.; Dworkin, R.H.; Raja, S.N. Neuropathic Pain. Nat. Rev. Dis. Primer 2017, 3, 17002. [Google Scholar] [CrossRef]
- Powell, A.; Davidson, L. Pediatric Spinal Cord Injury: A Review by Organ System. Phys. Med. Rehabil. Clin. N. Am. 2015, 26, 109–132. [Google Scholar] [CrossRef]
- Merritt, J.L. Management of Spasticity in Spinal Cord Injury. Mayo Clin. Proc. 1981, 56, 614–622. [Google Scholar]
- Hsieh, J.; Wolfe, D.; Connoly, S.; Townson, A. Spasticity After Spinal Cord Injury: An Evidence-Based Review of Current Interventions | Request PDF. Available online: https://www.researchgate.net/publication/285717446_Spasticity_After_Spinal_Cord_Injury_An_Evidence-Based_Review_of_Current_Interventions (accessed on 30 March 2023).
- Kopec, K. Cerebral Palsy: Pharmacologic Treatment of Spasticity. US Pharm 2008, 33, 22–26. [Google Scholar]
- Mathew, A.; Mathew, M.C. Bedtime Diazepam Enhances Well-Being in Children with Spastic Cerebral Palsy. Pediatr. Rehabil. 2005, 8, 63–66. [Google Scholar] [CrossRef]
- Albright, A.L. Intrathecal Baclofen for Childhood Hypertonia. Childs Nerv. Syst. ChNS Off. J. Int. Soc. Pediatr. Neurosurg. 2007, 23, 971–979. [Google Scholar] [CrossRef]
- Goetz, L.L.; Hurvitz, E.A.; Nelson, V.S.; Waring, W. Bowel Management in Children and Adolescents with Spinal Cord Injury. J. Spinal Cord Med. 1998, 21, 335–341. [Google Scholar] [CrossRef] [PubMed]
- Del Popolo, G.; Mosiello, G.; Pilati, C.; Lamartina, M.; Battaglino, F.; Buffa, P.; Redaelli, T.; Lamberti, G.; Menarini, M.; Di Benedetto, P.; De Gennaro, M. Treatment of Neurogenic Bowel Dysfunction Using Transanal Irrigation: A Multicenter Italian Study. Spinal Cord 2008, 46, 517–522. [Google Scholar] [CrossRef] [PubMed]
- Qi, Z.; Middleton, J.W.; Malcolm, A. Bowel Dysfunction in Spinal Cord Injury. Curr. Gastroenterol. Rep. 2018, 20, 47. [Google Scholar] [CrossRef]
- Merenda, L.; Brown, J.P. Bladder and Bowel Management for the Child with Spinal Cord Dysfunction. J. Spinal Cord Med. 2004, 27 Suppl 1, S16–23. [Google Scholar] [CrossRef]
- Akbar, M.; Abel, R.; Seyler, T.M.; Bedke, J.; Haferkamp, A.; Gerner, H.J.; Möhring, K. Repeated Botulinum-A Toxin Injections in the Treatment of Myelodysplastic Children and Patients with Spinal Cord Injuries with Neurogenic Bladder Dysfunction. BJU Int. 2007, 100, 639–645. [Google Scholar] [CrossRef] [PubMed]
- McCarthy, J.J.; Chafetz, R.S.; Betz, R.R.; Gaughan, J. Incidence and Degree of Hip Subluxation/Dislocation in Children with Spinal Cord Injury. J. Spinal Cord Med. 2004, 27 Suppl 1, S80–83. [Google Scholar] [CrossRef]
- Tori, J.A.; Hill, L.L. Hypercalcemia in Children with Spinal Cord Injury. Arch. Phys. Med. Rehabil. 1978, 59, 443–446. [Google Scholar]
- McIntyre, A.; Sadowsky, C.; Behrman, A.; Martin, R.; Augutis, M.; Cassidy, C.; Betz, R.; Ertzgaard, P.; Mulcahey, M. A Systematic Review of the Scientific Literature for Rehabilitation/Habilitation Among Individuals With Pediatric-Onset Spinal Cord Injury. Top. Spinal Cord Inj. Rehabil. 2022, 28, 13–90. [Google Scholar] [CrossRef] [PubMed]
- Williams, R.; Murray, A. Prevalence of Depression after Spinal Cord Injury: A Meta-Analysis. Arch. Phys. Med. Rehabil. 2015, 96, 133–140. [Google Scholar] [CrossRef]
- Anderson, R.C.E.; Kan, P.; Vanaman, M.; Rubsam, J.; Hansen, K.W.; Scaife, E.R.; Brockmeyer, D.L. Utility of a Cervical Spine Clearance Protocol after Trauma in Children between 0 and 3 Years of Age. J. Neurosurg. Pediatr. 2010, 5, 292–296. [Google Scholar] [CrossRef]
- Johnston, T.E.; Smith, B.T.; Mulcahey, M.J.; Betz, R.R.; Lauer, R.T. A Randomized Controlled Trial on the Effects of Cycling with and without Electrical Stimulation on Cardiorespiratory and Vascular Health in Children with Spinal Cord Injury. Arch. Phys. Med. Rehabil. 2009, 90, 1379–1388. [Google Scholar] [CrossRef] [PubMed]
- Johnston, T.E.; Smith, B.T.; Betz, R.R.; Lauer, R.T. Exercise Testing Using Upper Extremity Ergometry in Pediatric Spinal Cord Injury. Pediatr. Phys. Ther. Off. Publ. Sect. Pediatr. Am. Phys. Ther. Assoc. 2008, 20, 146–151. [Google Scholar] [CrossRef] [PubMed]
- Johnston, T.E.; Smith, B.T.; Oladeji, O.; Betz, R.R.; Lauer, R.T. Outcomes of a Home Cycling Program Using Functional Electrical Stimulation or Passive Motion for Children with Spinal Cord Injury: A Case Series. J. Spinal Cord Med. 2008, 31, 215–221. [Google Scholar] [CrossRef] [PubMed]
- Widman, L.M.; Abresch, R.T.; Styne, D.M.; McDonald, C.M. Aerobic Fitness and Upper Extremity Strength in Patients Aged 11 to 21 Years with Spinal Cord Dysfunction as Compared to Ideal Weight and Overweight Controls. J. Spinal Cord Med. 2007, 30 (Suppl 1), S88–96. [Google Scholar] [CrossRef]
- Liusuwan, R.A.; Widman, L.M.; Abresch, R.T.; Styne, D.M.; McDonald, C.M. Body Composition and Resting Energy Expenditure in Patients Aged 11 to 21 Years With Spinal Cord Dysfunction Compared to Controls: Comparisons and Relationships Among the Groups. J. Spinal Cord Med. 2007, 30 (Suppl 1), S105–S111. [Google Scholar] [CrossRef] [PubMed]
- Zebracki, K.; Hwang, M.; Patt, P.L.; Vogel, L.C. Autonomic Cardiovascular Dysfunction and Vitamin D Deficiency in Pediatric Spinal Cord Injury. J. Pediatr. Rehabil. Med. 2013, 6, 45–52. [Google Scholar] [CrossRef]
- Houghton, P.; Campbell, K. ; CPG. Panel Canadian Best Practice Guidelines for the Prevention and Management of Pressure Ulcers in People with Spinal Cord Injury A Resource Handbook for Clinicians.
- Almeida, D.; da Costa, K.N.N.; Castro, R. de A. L.; Almeida, M.L.P.W.; Vianna, R.; Antonio, A.G. Self-Inflicted Oral Injury in an Infant with Transverse Myelitis. Spec. Care Dent. Off. Publ. Am. Assoc. Hosp. Dent. Acad. Dent. Handicap. Am. Soc. Geriatr. Dent. 2009, 29, 254–258. [Google Scholar] [CrossRef]
- Vogel, L.C.; Anderson, C.J. Self-Injurious Behavior in Children and Adolescents with Spinal Cord Injuries. Spinal Cord 2002, 40, 666–668. [Google Scholar] [CrossRef] [PubMed]
- Colville, G.A.; Mok, Q. Psychological Management of Two Cases of Self Injury on the Paediatric Intensive Care Unit. Arch. Dis. Child. 2003, 88, 335–336. [Google Scholar] [CrossRef] [PubMed]
- Vogel, L.C.; Krajci, K.A.; Anderson, C.J. Adults with Pediatric-Onset Spinal Cord Injury: Part 1: Prevalence of Medical Complications. J. Spinal Cord Med. 2002, 25, 106–116. [Google Scholar] [CrossRef] [PubMed]
- Choksi, A.; Townsend, E.L.; Dumas, H.M.; Haley, S.M. Functional Recovery in Children and Adolescents with Spinal Cord Injury. Pediatr. Phys. Ther. Off. Publ. Sect. Pediatr. Am. Phys. Ther. Assoc. 2010, 22, 214–221. [Google Scholar] [CrossRef] [PubMed]
- Vogel, L.C.; Lubicky, J.P. Ambulation with Parapodia and Reciprocating Gait Orthoses in Pediatric Spinal Cord Injury. Dev. Med. Child Neurol. 1995, 37, 957–964. [Google Scholar] [CrossRef]
- Altizer, W.; Noritz, G.; Paleg, G. Use of a Dynamic Gait Trainer for a Child with Thoracic Level Spinal Cord Injury. BMJ Case Rep. 2017, 2017, bcr2017220756. [Google Scholar] [CrossRef]
- Moynahan, M.; Mullin, C.; Cohn, J.; Burns, C.A.; Halden, E.E.; Triolo, R.J.; Betz, R.R. Home Use of a Functional Electrical Stimulation System for Standing and Mobility in Adolescents with Spinal Cord Injury. Arch. Phys. Med. Rehabil. 1996, 77, 1005–1013. [Google Scholar] [CrossRef]
- McCain, K.J.; Farrar, M.; Smith, P.S. Gait Recovery in a Girl with Ischemic Spinal Cord Stroke. Pediatr. Phys. Ther. Off. Publ. Sect. Pediatr. Am. Phys. Ther. Assoc. 2015, 27, 190–199. [Google Scholar] [CrossRef]
- Murillo, N.; Kumru, H.; Opisso, E.; Padullés, J.M.; Medina, J.; Vidal, J.; Kofler, M. Recovery of Assisted Overground Stepping in a Patient with Chronic Motor Complete Spinal Cord Injury: A Case Report. NeuroRehabilitation 2012, 31, 401–407. [Google Scholar] [CrossRef]
- Johnston, T.E.; Betz, R.R.; Smith, B.T.; Benda, B.J.; Mulcahey, M.J.; Davis, R.; Houdayer, T.P.; Pontari, M.A.; Barriskill, A.; Creasey, G.H. Implantable FES System for Upright Mobility and Bladder and Bowel Function for Individuals with Spinal Cord Injury. Spinal Cord 2005, 43, 713–723. [Google Scholar] [CrossRef]
- Betz, R.R.; Johnston, T.E.; Smith, B.T.; Mulcahey, M.J.; McCarthy, J.J. Three-Year Follow-up of an Implanted Functional Electrical Stimulation System for Upright Mobility in a Child with a Thoracic Level Spinal Cord Injury. J. Spinal Cord Med. 2002, 25, 345–350. [Google Scholar] [CrossRef]
- Bonaroti, D.; Akers, J.M.; Smith, B.T.; Mulcahey, M.J.; Betz, R.R. Comparison of Functional Electrical Stimulation to Long Leg Braces for Upright Mobility for Children with Complete Thoracic Level Spinal Injuries. Arch. Phys. Med. Rehabil. 1999, 80, 1047–1053. [Google Scholar] [CrossRef]
- Massagli, T.L. Medical and Rehabilitation Issues in the Care of Children with Spinal Cord Injury. Phys. Med. Rehabil. Clin. N. Am. 2000, 11, 169–182. [Google Scholar] [CrossRef] [PubMed]
- Graham, P.; Weingarden, S.; Murphy, P. School Reintegration: A Rehabilitation Goal for Spinal Cord Injured Adolescents. Rehabil. Nurs. Off. J. Assoc. Rehabil. Nurses 1991, 16, 122–127. [Google Scholar] [CrossRef] [PubMed]
- Badhiwala, J.H.; Ahuja, C.S.; Fehlings, M.G. Time Is Spine: A Review of Translational Advances in Spinal Cord Injury. J. Neurosurg. Spine 2018, 30, 1–18. [Google Scholar] [CrossRef]
- Assinck, P.; Duncan, G.J.; Hilton, B.J.; Plemel, J.R.; Tetzlaff, W. Cell Transplantation Therapy for Spinal Cord Injury. Nat. Neurosci. 2017, 20, 637–647. [Google Scholar] [CrossRef]
- Khazaei, M.; Ahuja, C.S.; Siddiqui, A.M.; Fehlings, M.G. Transplantation of Human-Induced Pluripotent Stem Cell-Derived Neural Precursor Cells for Treatment of Spinal Cord Injury. In Gene Therapy in Neurological Disorders; Elsevier, 2018; pp 299–325. [CrossRef]
- Khazaei, M.; Ahuja, C.S.; Fehlings, M.G. Induced Pluripotent Stem Cells for Traumatic Spinal Cord Injury. Front. Cell Dev. Biol. 2017, 4, 152. [Google Scholar] [CrossRef]
- Karimi-Abdolrezaee, S.; Eftekharpour, E.; Wang, J.; Morshead, C.M.; Fehlings, M.G. Delayed Transplantation of Adult Neural Precursor Cells Promotes Remyelination and Functional Neurological Recovery after Spinal Cord Injury. J. Neurosci. Off. J. Soc. Neurosci. 2006, 26, 3377–3389. [Google Scholar] [CrossRef]
- Parr, A.M.; Kulbatski, I.; Zahir, T.; Wang, X.; Yue, C.; Keating, A.; Tator, C.H. Transplanted Adult Spinal Cord-Derived Neural Stem/Progenitor Cells Promote Early Functional Recovery after Rat Spinal Cord Injury. Neuroscience 2008, 155, 760–770. [Google Scholar] [CrossRef] [PubMed]
- Fellows, C.R.; Matta, C.; Zakany, R.; Khan, I.M.; Mobasheri, A. Adipose, Bone Marrow and Synovial Joint-Derived Mesenchymal Stem Cells for Cartilage Repair. Front. Genet. 2016, 7, 213. [Google Scholar] [CrossRef]
- Law, S.; Chaudhuri, S. Mesenchymal Stem Cell and Regenerative Medicine: Regeneration versus Immunomodulatory Challenges. Am. J. Stem Cells 2013, 2, 22–38. [Google Scholar]
- Ahuja, C.S.; Schroeder, G.D.; Vaccaro, A.R.; Fehlings, M.G. Spinal Cord Injury-What Are the Controversies? J. Orthop. Trauma 2017, 31 Suppl 4, S7–S13. [Google Scholar] [CrossRef]
- Hachem, L.D.; Ahuja, C.S.; Fehlings, M.G. Assessment and Management of Acute Spinal Cord Injury: From Point of Injury to Rehabilitation. J. Spinal Cord Med. 2017, 40, 665–675. [Google Scholar] [CrossRef]
- Furlan, J.C.; Noonan, V.; Cadotte, D.W.; Fehlings, M.G. Timing of Decompressive Surgery of Spinal Cord after Traumatic Spinal Cord Injury: An Evidence-Based Examination of Pre-Clinical and Clinical Studies. J. Neurotrauma 2011, 28, 1371–1399. [Google Scholar] [CrossRef]
- Silva, N.A.; Cooke, M.J.; Tam, R.Y.; Sousa, N.; Salgado, A.J.; Reis, R.L.; Shoichet, M.S. The Effects of Peptide Modified Gellan Gum and Olfactory Ensheathing Glia Cells on Neural Stem/Progenitor Cell Fate. Biomaterials 2012, 33, 6345–6354. [Google Scholar] [CrossRef] [PubMed]
- Ramer, L.M.; Au, E.; Richter, M.W.; Liu, J.; Tetzlaff, W.; Roskams, A.J. Peripheral Olfactory Ensheathing Cells Reduce Scar and Cavity Formation and Promote Regeneration after Spinal Cord Injury. J. Comp. Neurol. 2004, 473, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Chen, P.; Wang, Q.; Chen, Y.; Yu, H.; Ma, J.; Guo, M.; Piao, M.; Ren, W.; Xiang, L. Meta Analysis of Olfactory Ensheathing Cell Transplantation Promoting Functional Recovery of Motor Nerves in Rats with Complete Spinal Cord Transection. Neural Regen. Res. 2014, 9, 1850–1858. [Google Scholar] [CrossRef]
- Watzlawick, R.; Rind, J.; Sena, E.S.; Brommer, B.; Zhang, T.; Kopp, M.A.; Dirnagl, U.; Macleod, M.R.; Howells, D.W.; Schwab, J.M. Olfactory Ensheathing Cell Transplantation in Experimental Spinal Cord Injury: Effect Size and Reporting Bias of 62 Experimental Treatments: A Systematic Review and Meta-Analysis. PLoS Biol. 2016, 14, e1002468. [Google Scholar] [CrossRef] [PubMed]
- Biernaskie, J.; Sparling, J.S.; Liu, J.; Shannon, C.P.; Plemel, J.R.; Xie, Y.; Miller, F.D.; Tetzlaff, W. Skin-Derived Precursors Generate Myelinating Schwann Cells That Promote Remyelination and Functional Recovery after Contusion Spinal Cord Injury. J. Neurosci. Off. J. Soc. Neurosci. 2007, 27, 9545–9559. [Google Scholar] [CrossRef]
- Honmou, O.; Felts, P.A.; Waxman, S.G.; Kocsis, J.D. Restoration of Normal Conduction Properties in Demyelinated Spinal Cord Axons in the Adult Rat by Transplantation of Exogenous Schwann Cells. J. Neurosci. Off. J. Soc. Neurosci. 1996, 16, 3199–3208. [Google Scholar] [CrossRef]
- Kanno, H.; Pearse, D.D.; Ozawa, H.; Itoi, E.; Bunge, M.B. Schwann Cell Transplantation for Spinal Cord Injury Repair: Its Significant Therapeutic Potential and Prospectus. Rev. Neurosci. 2015, 26, 121–128. [Google Scholar] [CrossRef]
- Sparling, J.S.; Bretzner, F.; Biernaskie, J.; Assinck, P.; Jiang, Y.; Arisato, H.; Plunet, W.T.; Borisoff, J.; Liu, J.; Miller, F.D.; Tetzlaff, W. Schwann Cells Generated from Neonatal Skin-Derived Precursors or Neonatal Peripheral Nerve Improve Functional Recovery after Acute Transplantation into the Partially Injured Cervical Spinal Cord of the Rat. J. Neurosci. 2015, 35, 6714–6730. [Google Scholar] [CrossRef] [PubMed]
- Mothe, A.J.; Tam, R.Y.; Zahir, T.; Tator, C.H.; Shoichet, M.S. Repair of the Injured Spinal Cord by Transplantation of Neural Stem Cells in a Hyaluronan-Based Hydrogel. Biomaterials 2013, 34, 3775–3783. [Google Scholar] [CrossRef] [PubMed]
- Mothe, A.J.; Zahir, T.; Santaguida, C.; Cook, D.; Tator, C.H. Neural Stem/Progenitor Cells from the Adult Human Spinal Cord Are Multipotent and Self-Renewing and Differentiate after Transplantation. PloS One 2011, 6, e27079. [Google Scholar] [CrossRef]
- Neuhuber, B.; Timothy Himes, B.; Shumsky, J.S.; Gallo, G.; Fischer, I. Axon Growth and Recovery of Function Supported by Human Bone Marrow Stromal Cells in the Injured Spinal Cord Exhibit Donor Variations. Brain Res. 2005, 1035, 73–85. [Google Scholar] [CrossRef] [PubMed]
- Iwasaki, M.; Wilcox, J.T.; Nishimura, Y.; Zweckberger, K.; Suzuki, H.; Wang, J.; Liu, Y.; Karadimas, S.K.; Fehlings, M.G. Synergistic Effects of Self-Assembling Peptide and Neural Stem/Progenitor Cells to Promote Tissue Repair and Forelimb Functional Recovery in Cervical Spinal Cord Injury. Biomaterials 2014, 35, 2617–2629. [Google Scholar] [CrossRef] [PubMed]
- Zweckberger, K.; Ahuja, C.S.; Liu, Y.; Wang, J.; Fehlings, M.G. Self-Assembling Peptides Optimize the Post-Traumatic Milieu and Synergistically Enhance the Effects of Neural Stem Cell Therapy after Cervical Spinal Cord Injury. Acta Biomater. 2016, 42, 77–89. [Google Scholar] [CrossRef]
- Gupta, D.; Tator, C.H.; Shoichet, M.S. Fast-Gelling Injectable Blend of Hyaluronan and Methylcellulose for Intrathecal, Localized Delivery to the Injured Spinal Cord. Biomaterials 2006, 27, 2370–2379. [Google Scholar] [CrossRef]
- Pakulska, M.; Tator, C.; Shoichet, M. Local Delivery of Chondroitinase ABC with or without Stromal Cell-Derived Factor 1α Promotes Functional Repair in the Injured Rat Spinal Cord. Biomaterials 2017, 134. [Google Scholar] [CrossRef]
- Fehlings, M.G.; Moghaddamjou, A.; Harrop, J.S.; Stanford, R.; Ball, J.R.; Aarabi, B.; Freeman, B.J.; Arnold, P.; Guest, J.; Kurpad, S.N.; Schuster, J.M.; Nassr, A.; Schmitt, K.M.; Wilson, J.R.; Brodke, D.; Ahmad, F.U.; Yee, A.; Ray, W.Z.; Brooks, N.; Wilson, J.; Chow, D.; Toups, E.G.; Kopjar, B. Safety and Efficacy of Riluzole in Acute Spinal Cord Injury (RISCIS): A Multi-Center, Randomized, Placebo-Controlled, Double-Blinded Trial. J. Neurotrauma 2023. [Google Scholar] [CrossRef]
- Nagoshi, N.; Nakashima, H.; Fehlings, M.G. Riluzole as a Neuroprotective Drug for Spinal Cord Injury: From Bench to Bedside. Mol. Basel Switz. 2015, 20, 7775–7789. [Google Scholar] [CrossRef]
- Meshkini, A.; Salehpour, F.; Aghazadeh, J.; Mirzaei, F.; Naseri Alavi, S.A. Riluzole Can Improve Sensory and Motor Function in Patients with Acute Spinal Cord Injury. Asian J. Neurosurg. 2018, 13, 656–659. [Google Scholar] [CrossRef] [PubMed]
- Geisler, F.H.; Coleman, W.P.; Grieco, G.; Poonian, D.; Sygen Study Group. The Sygen Multicenter Acute Spinal Cord Injury Study. Spine 2001, 26 (24 Suppl), S87–98. [Google Scholar] [CrossRef] [PubMed]
- Gibson, C.L.; Jones, N.C.; Prior, M.J.W.; Bath, P.M.W.; Murphy, S.P. G-CSF Suppresses Edema Formation and Reduces Interleukin-1beta Expression after Cerebral Ischemia in Mice. J. Neuropathol. Exp. Neurol. 2005, 64, 763–769. [Google Scholar] [CrossRef] [PubMed]
- Srinivas, S.; Wali, A.R.; Pham, M.H. Efficacy of Riluzole in the Treatment of Spinal Cord Injury: A Systematic Review of the Literature. Neurosurg. Focus 2019, 46, E6. [Google Scholar] [CrossRef]
- Lord-Fontaine, S.; Yang, F.; Diep, Q.; Dergham, P.; Munzer, S.; Tremblay, P.; McKerracher, L. Local Inhibition of Rho Signaling by Cell-Permeable Recombinant Protein BA-210 Prevents Secondary Damage and Promotes Functional Recovery Following Acute Spinal Cord Injury. J. Neurotrauma 2008, 25, 1309–1322. [Google Scholar] [CrossRef]
- Cheng, H.; Cao, Y.; Olson, L. Spinal Cord Repair in Adult Paraplegic Rats: Partial Restoration of Hind Limb Function. Science 1996, 273, 510–513. [Google Scholar] [CrossRef]
- Lee, Y.-S.; Hsiao, I.; Lin, V.W. Peripheral Nerve Grafts and AFGF Restore Partial Hindlimb Function in Adult Paraplegic Rats. J. Neurotrauma 2002, 19, 1203–1216. [Google Scholar] [CrossRef]
- Zörner, B.; Schwab, M.E. Anti-Nogo on the Go: From Animal Models to a Clinical Trial. Ann. N. Y. Acad. Sci. 2010, 1198 Suppl 1, E22–34. [Google Scholar] [CrossRef]
- Freund, P.; Wannier, T.; Schmidlin, E.; Bloch, J.; Mir, A.; Schwab, M.E.; Rouiller, E.M. Anti-Nogo-A Antibody Treatment Enhances Sprouting of Corticospinal Axons Rostral to a Unilateral Cervical Spinal Cord Lesion in Adult Macaque Monkey. J. Comp. Neurol. 2007, 502, 644–659. [Google Scholar] [CrossRef]
- Jacobson, P.B.; Goody, R.; Lawrence, M.; Mueller, B.K.; Zhang, X.; Hooker, B.A.; Pfleeger, K.; Ziemann, A.; Locke, C.; Barraud, Q.; Droescher, M.; Bernhard, J.; Popp, A.; Boeser, P.; Huang, L.; Mollon, J.; Mordashova, Y.; Cui, Y.-F.; Savaryn, J.P.; Grinnell, C.; Dreher, I.; Gold, M.; Courtine, G.; Mothe, A.; Tator, C.H.; Guest, J.D. Elezanumab, a Human Anti-RGMa Monoclonal Antibody, Promotes Neuroprotection, Neuroplasticity, and Neurorecovery Following a Thoracic Hemicompression Spinal Cord Injury in Non-Human Primates. Neurobiol. Dis. 2021, 155, 105385. [Google Scholar] [CrossRef]
- Mothe, A.J.; Coelho, M.; Huang, L.; Monnier, P.P.; Cui, Y.-F.; Mueller, B.K.; Jacobson, P.B.; Tator, C.H. Delayed Administration of the Human Anti-RGMa Monoclonal Antibody Elezanumab Promotes Functional Recovery Including Spontaneous Voiding after Spinal Cord Injury in Rats. Neurobiol. Dis. 2020, 143, 104995. [Google Scholar] [CrossRef] [PubMed]
- Mothe, A.J.; Jacobson, P.B.; Caprelli, M.; Ulndreaj, A.; Rahemipour, R.; Huang, L.; Monnier, P.P.; Fehlings, M.G.; Tator, C.H. Delayed Administration of Elezanumab, a Human Anti-RGMa Neutralizing Monoclonal Antibody, Promotes Recovery Following Cervical Spinal Cord Injury. Neurobiol. Dis. 2022, 172, 105812. [Google Scholar] [CrossRef] [PubMed]
- Kapadia, N.; Masani, K.; Catharine Craven, B.; Giangregorio, L.M.; Hitzig, S.L.; Richards, K.; Popovic, M.R. A Randomized Trial of Functional Electrical Stimulation for Walking in Incomplete Spinal Cord Injury: Effects on Walking Competency. J. Spinal Cord Med. 2014, 37, 511–524. [Google Scholar] [CrossRef] [PubMed]
- Thrasher, T.A.; Flett, H.M.; Popovic, M.R. Gait Training Regimen for Incomplete Spinal Cord Injury Using Functional Electrical Stimulation. Spinal Cord 2006, 44, 357–361. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



