Submitted:
06 June 2023
Posted:
07 June 2023
You are already at the latest version
Abstract
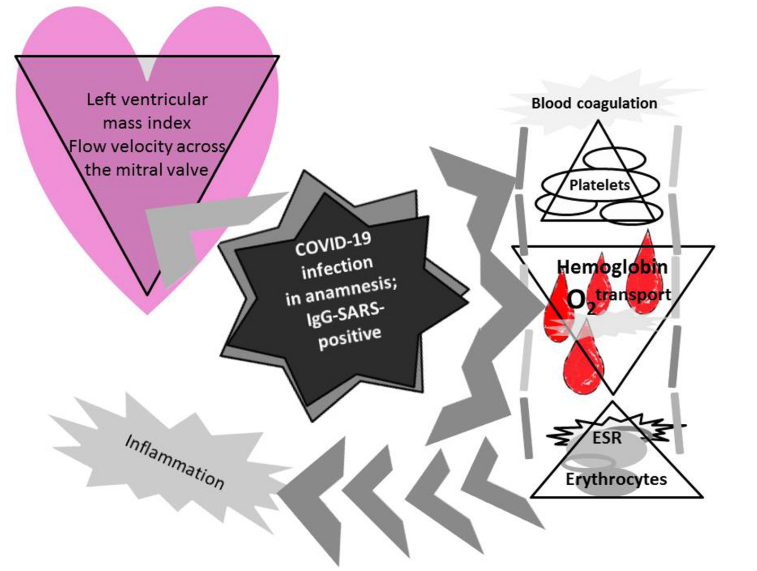
Keywords:
1. Introduction
2. Materials and Methods
Participants
General Examination
Echocardiography
Blood Sampling
Blood Tests
Detection of IgG Antibodies against SARS-CoV-2 S1 RBD
Statistical Analysis
3. Results
4. Discussion
5. Conclusions
Acknowledgements
References
- Garcia-Zamora, S.; Picco, J.M.; Lepori, A.J.; Galello, M.I.; Saad, A.K.; Ayón, M.; Monga-Aguilar, N.; Shehadeh, I.; Manganiello, C.F.; Izaguirre, C.; et al. Abnormal echocardiographic findings after COVID-19 infection: a multicenter registry. Int. J. Cardiovasc. Imaging 2022, 39, 77–85. [Google Scholar] [CrossRef]
- Chung, M.K.; Zidar, D.A.; Bristow, M.R.; Cameron, S.J.; Chan, T.; Harding, C.V.; Kwon, D.H.; Singh, T.; Tilton, J.C.; Tsai, E.J.; et al. COVID-19 and Cardiovascular Disease. Circ. Res. 2021, 128, 1214–1236. [Google Scholar] [CrossRef] [PubMed]
- Gumanova, N.G.; Zlobina, P.D.; Bogdanova, N.L.; Brutyan, H.A.; Kalemberg, E.N.; Metelskaya, V.A.; Davtyan, K.V.; Drapkina, O.M. Associations of adenovirus-reactive immunoglobulins with atrial fibrillation and body mass index. Front. Cardiovasc. Med. 2023, 10, 1190051. [Google Scholar] [CrossRef] [PubMed]
- Calhoun, P.J.; Phan, A.V.; Taylor, J.D.; James, C.C.; Padget, R.L.; Zeitz, M.J.; Smyth, J.W. Adenovirus targets transcriptional and posttranslational mechanisms to limit gap junction function. FASEB J. 2020, 34, 9694–9712. [Google Scholar] [CrossRef] [PubMed]
- Gumanova, N.G.; Gorshkov, A.U.; Bogdanova, N.L.; Korolev, A.I.; Drapkina, O.M. Detection of Anti-SARS-CoV-2-S1 RBD-Specific Antibodies Prior to and during the Pandemic in 2011–2021 and COVID-19 Observational Study in 2019–2021. Vaccines 2022, 10, 581. [Google Scholar] [CrossRef] [PubMed]
- Mitchell, C.; Rahko, P.S.; Blauwet, L.A.; Canaday, B.; Finstuen, J.A.; Foster, M.C.; Horton, K.; Ogunyankin, K.O.; Palma, R.A.; Velazquez, E.J. Guidelines for Performing a Comprehensive Transthoracic Echocardiographic Examination in Adults: Recommendations from the American Society of Echocardiography. J. Am. Soc. Echocardiogr. 2018, 32, 1–64. [Google Scholar] [CrossRef] [PubMed]
- Lang, R.M.; Badano, L.P.; Mor-Avi, V.; Afilalo, J.; Armstrong, A.; Ernande, L.; Flachskampf, F.A.; Foster, E.; Goldstein, S.A.; Kuznetsova, T.; et al. Recommendations for Cardiac Chamber Quantification by Echocardiography in Adults: An Update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur. Heart J. Cardiovasc. Imaging 2015, 16, 233–271. [Google Scholar] [CrossRef] [PubMed]
- Nagueh, S.F.; Appleton, C.P.; Gillebert, T.C.; Marino, P.N.; Oh, J.K.; Smiseth, O.A.; Waggoner, A.D.; Flachskampf, F.A.; Pellikka, P.A.; Evangelisa, A. Recommendations for the Evaluation of Left Ventricular Diastolic Function by Echocardiography. Eur. Hear. J. - Cardiovasc. Imaging 2008, 10, 165–193. [Google Scholar] [CrossRef] [PubMed]
- Mateus, J.; Grifoni, A.; Tarke, A.; Sidney, J.; Ramirez, S.I.; Dan, J.M.; Burger, Z.C.; Rawlings, S.A.; Smith, D.M.; Phillips, E.; et al. Selective and cross-reactive SARS-CoV-2 T cell epitopes in unexposed humans. Science 2020, 370, 89–94. [Google Scholar] [CrossRef]
- Mizukoshi, K.; Takeuchi, M.; Nagata, Y.; Addetia, K.; Lang, R.M.; Akashi, Y.J.; Otsuji, Y. Normal Values of Left Ventricular Mass Index Assessed by Transthoracic Three-Dimensional Echocardiography. J. Am. Soc. Echocardiogr. 2015, 29, 51–61. [Google Scholar] [CrossRef]
- Bella, J.N.; Palmieri, V.; Roman, M.J.; Liu, J.E.; Welty, T.K.; Lee, E.T.; Fabsitz, R.R.; Howard, B.V.; Devereux, R.B. Mitral Ratio of Peak Early to Late Diastolic Filling Velocity as a Predictor of Mortality in Middle-Aged and Elderly Adults. Circ. 2002, 105, 1928–1933. [Google Scholar] [CrossRef]
- Mishra, R.K.; Devereux, R.B.; Cohen, B.E.; Whooley, M.A.; Schiller, N.B. Prediction of Heart Failure and Adverse Cardiovascular Events in Outpatients with Coronary Artery Disease Using Mitral E/A Ratio in Conjunction with E-Wave Deceleration Time: The Heart and Soul Study. J. Am. Soc. Echocardiogr. 2011, 24, 1134–1140. [Google Scholar] [CrossRef]
- Ramsook, A.H.; Dominelli, P.B.; Angus, S.A.; Senefeld, J.W.; Wiggins, C.C.; Joyner, M.J. The oxygen transport cascade and exercise: Lessons from comparative physiology. Comp. Biochem. Physiol. Part A: Mol. Integr. Physiol. 2023, 282, 111442. [Google Scholar] [CrossRef]
- Vera-Pineda, R.; Carrizales-Sepúlveda, E.F.; Morales-Rendón, E.J.; Ordaz-Farías, A.; Solís, J.G.; Benavides-González, M.A.; Flores-Ramírez, R. Echocardiographic manifestations during the first 3 months after an episode of COVID-19 and their relationship with disease severity and persistence of symptoms. Am. J. Med Sci. 2023, 366, 32–37. [Google Scholar] [CrossRef] [PubMed]
- Prado, A.; Cotella, J.; Hasbani, J.; Hasbani, E. Abnormal longitudinal strain reduction of basal left ventricular segments in patients recovered of COVID-19. J. Cardiovasc. Echography 2022, 32, 107–111. [Google Scholar] [CrossRef]
- Kaolawanich, Y.; Boonyasirinant, T. Usefulness of apical area index to predict left ventricular thrombus in patients with systolic dysfunction: a novel index from cardiac magnetic resonance. BMC Cardiovasc. Disord. 2019, 19, 15. [Google Scholar] [CrossRef] [PubMed]
- Appleton, C.P.; Hatle, L.K.; Popp, R.L. Relation of transmitral flow velocity patterns to left ventricular diastolic function: New insights from a combined hemodynamic and Doppler echocardiographic study. J. Am. Coll. Cardiol. 1988, 12, 426–440. [Google Scholar] [CrossRef]
- Rakowski, H.; Appleton, C.; Chan, K.L.; Dumesni, J.G.; Honos, G.; Jue, J.; Koilpillai, C.; Lepage, S.; Martin, R.P.; Mercier, L.A.; O'Kelly, B. Canadian consensus recommendations for the measurement and reporting of diastolic dysfunction by echocardiography. J. Am. Soc. Echocardiogr. 1996, 9, 736–760. [Google Scholar] [CrossRef] [PubMed]
- Kim, M.K.; Kim, B.; Lee, J.Y.; Kim, J.S.; Han, B.-G.; Choi, S.O.; Yang, J.W. Tissue Doppler-derived E/e' ratio as a parameter for assessing diastolic heart failure and as a predictor of mortality in patients with chronic kidney disease. Korean J. Intern. Med. 2013, 28, 35–44. [Google Scholar] [CrossRef]
- Sciaudone, A.; Corkrey, H.; Humphries, F.; Koupenova, M. Platelets and SARS-CoV-2 During COVID-19: Immunity, Thrombosis, and Beyond. Circ. Res. 2023, 132, 1272–1289. [Google Scholar] [CrossRef]
- Xuereb, R.-A.; Borg, M.; Vella, K.; Gatt, A.; Xuereb, R.G.; Barbara, C.; Fava, S.; Magri, C.J. Long COVID Syndrome: A Case-Control Study. Am. J. Med. 2023. [Google Scholar] [CrossRef] [PubMed]
- Islam, M.M.; Islam, S.; Ahmed, R.; Majumder, M.; Sarkar, B.; Himu, E.R.; Kawser; Hossain, A. ; Mia, M.J.; Parag, R.R.; et al. Reduced IFN-γ levels along with changes in hematologic and immunologic parameters are key to COVID-19 severity in Bangladeshi patients. Exp. Hematol. 2022, 118, 53–64. [Google Scholar] [CrossRef] [PubMed]
- Crooks, C.J.; West, J.; Morling, J.R.; Simmonds, M.; Juurlink, I.; Briggs, S.; Cruickshank, S.; Hammond-Pears, S.; Shaw, D.; Card, T.R.; et al. Anaemia of acute inflammation: a higher acute systemic inflammatory response is associated with a larger decrease in blood haemoglobin levels in patients with COVID-19 infection. Clin. Med. 2023, 23, 201–205. [Google Scholar] [CrossRef] [PubMed]
| Parameters | Mean | S.D. |
|---|---|---|
| Age (years) | 44.8 | 8.6 |
| Height (cm) | 175.2 | 8.4 |
| BMI (kg/m2) | 27.2 | 4.3 |
| SBP in office (mm Hg) | 125.4 | 14.9 |
| DBP in office (mm Hg) | 82.3 | 9.9 |
| SBP in 24-h monitoring (mm Hg) | 123.4 | 12.9 |
| DBP in 24-h monitoring (mm Hg) | 80.5 | 9.1 |
| SCORE (%) | 1.85 | 2.3 |
| Echocardiography (normal range) | ||
| AoSV (2.9-4.5 cm) | 3.3 | 0.4 |
| LA (2.7-4.0 cm) | 3.6 | 0.4 |
| LA volume (37-94 ml) | 51.4 | 13.9 |
| LAVI (15-34 ml/m2) | 25.6 | 5.7 |
| LVIDd (3.5-5.6 cm) | 4.9 | 0.5 |
| LVIDs (2.0-4.0 cm) | 2.7 | 0.4 |
| LVEDV (90-150 ml) | 105.1 | 26.5 |
| LVESV (14-61 ml) | 36.6 | 12.7 |
| SV (50-100 ml) | 69.0 | 16.2 |
| CO (5-8 l) | 4.7 | 1.1 |
| LVEF (52-72%) | 65.2 | 4.6 |
| IVSd (0.6-1.0 cm) | 1.0 | 0.2 |
| LVPWd (0.6-1.0 cm) | 0.9 | 0.1 |
| LVM (67-224 g) | 163.4 | 44.0 |
| LVMI (43-115 g/m2) | 80.9 | 16.9 |
| Aortic valve opening amplitude (>1.5 cm) | 2.1 | 0.2 |
| RA volume (24-81 ml) | 44.2 | 13.1 |
| RVOT (<36 mm) | 2.8 | 0.3 |
| PA (15-25 mm) | 2.0 | 0.3 |
| sPAP (<36 mmHg) | 22.3 | 4.6 |
| IVC (0.97 - 2.26 cm) | 1.8 | 0.2 |
| E/A (0.8-2.0) | 1.2 | 0.3 |
| DT (<220 msec) | 181.9 | 26.8 |
| E/e´ (>6) | 6.6 | 1.9 |
| Epicardial fat thickness (0.9-13.5 mm) | 4.8 | 4.2 |
| Aortic valve regurgitation; degree 0, 1, 2 (%) | 75.3; 23.4; 0.1 | NA |
| Mitral valve regurgitation; degree 0, 1, 2 (%) | 4.2; 94.5; 0.65 | NA |
| Tricuspid valve regurgitation; degree 0, 1, 2 (%) | 3.6; 95.4; 0.3 | NA |
| Pulmonary aortic valve regurgitation; degree 0, 1, 2 (%) | 2.9; 97.1; 0 | NA |
| Routine biochemical markers (normal range) | ||
| ESR (0-29 mm/h) | 7.28 | 4.95 |
| Erythrocytes (3.8-5.9 x 1012/l) | 4.95 | 0.81 |
| Hemoglobin (116-166 g/l) | 149.88 | 18.48 |
| Leukocytes (4-11 x 109/l) | 6.49 | 1.77 |
| Platelets (150-450 x 109/l) | 223.24 | 47.95 |
| Total cholesterol (<5.2 mmol/l) | 5.54 | 1.05 |
| HDL-cholesterol (>1 mmol/l) | 1.41 | 0.42 |
| LDL-cholesterol (<3.4 mmol/l) | 3.49 | 0.93 |
| Triglycerides (<1.7 mmol/l) | 1.47 | 1.05 |
| Glucose (3.9-5.6 mmol/l) | 5.85 | 1.79 |
| C-reactive protein (< 3 mg/l) | 2.23 | 5.32 |
| Uric acid (2.7-8.5 mg/dl) | 5.90 | 1.44 |
| Creatinine (44-106 µmol/l) | 80.57 | 14.68 |
| Alanine aminotransferase (4-36 U/l) | 26.18 | 17.81 |
| Aspartate aminotransferase (8-33 U/l) | 22.7 | 15.02 |
| IgG-SARS-negative (N=237) | IgG-SARS-positive (N=70) | Difference | |||
|---|---|---|---|---|---|
| Parameters | mean1 | S.D. | mean2 | S.D. | mean1 - mean2 |
| Age (years) | 44.8 | 8.6 | 45.4 | 9.0 | -0.6 |
| Height (cm) | 176.2 | 7.7 | 175.2 | 10.0 | 1.0 |
| BMI (kg/m2) | 27.4 | 4.2 | 26.8 | 4.7 | 0.7 |
| SBP in office (mm Hg) | 125.9 | 14.4 | 124.4 | 16.7 | 1.4 |
| DBP in office (mm Hg) | 82.9 | 9.4 | 80.5 | 11.6 | 2.4 |
| SBP in 24-h monitoring (mm Hg) | 124.9 | 12.8 | 118.8 | 12.2 | 6.1* |
| DBP in 24-h monitoring (mm Hg) | 81.2 | 9.0 | 78.4 | 9.3 | 2.8* |
| SCORE (%) | 1.9 | 2.5 | 1.6 | 1.7 | 0.3 |
| Echocardiography (normal range) | |||||
| AoSV (2.9-4.5 cm) | 3.3 | 0.4 | 3.3 | 0.4 | 0.1* |
| LA (2.7-4.0 cm) | 3.6 | 0.4 | 3.5 | 0.3 | 0.1* |
| LA volume (37-94 ml) | 52.1 | 13.9 | 48.8 | 13.4 | 3.3* |
| LAVI (15-34 ml/m2) | 25.8 | 5.8 | 25.2 | 5.2 | 0.6 |
| LVIDd (3.5-5.6 cm) | 4.9 | 0.5 | 4.7 | 0.5 | 0.2* |
| LVIDs (2.0-4.0 cm) | 2.7 | 0.4 | 2.8 | 0.4 | -0.1 |
| LVEDV (90-150 ml) | 107.2 | 25.6 | 100.6 | 28.1 | 6.7* |
| LVESV (14-61 ml) | 37.4 | 10.3 | 35.1 | 16.5 | 2.2* |
| SV (50-100 ml) | 70.9 | 16.8 | 65.0 | 14.2 | 6.0* |
| CO (5-8 l) | 4.8 | 1.2 | 4.5 | 0.9 | 0.3 |
| LVEF (52–72%) | 65.1 | 4.1 | 65.3 | 6.0 | -0.2 |
| IVSd (0.6-1.0 cm) | 1.0 | 0.2 | 1.0 | 0.2 | 0.0 |
| LVPWd (0.6-1.0 cm) | 0.9 | 0.1 | 0.9 | 0.1 | 0.1 |
| LVM (67-224 g) | 168.3 | 43.1 | 146.2 | 43.0 | 22.1* |
| LVMI (43-115 g/m2) | 82.9 | 17.0 | 73.9 | 14.8 | 9.1* |
| Aortic valve opening amplitude (>1.5 cm) | 2.2 | 0.3 | 2.1 | 0.2 | 0.1* |
| RA volume (24-81 ml) | 45.3 | 12.7 | 40.5 | 14.0 | 4.8* |
| RVOT (<36 mm) | 2.7 | 0.3 | 22.3 | 5.0 | -19.5 |
| PA (15-25 mm) | 2.0 | 0.3 | 2.8 | 0.3 | -0.8 |
| sPAP (<36 mm Hg) | 22.6 | 4.2 | 21.4 | 5.7 | 1.2* |
| IVC | 1.8 | 0.2 | 1.8 | 0.3 | 0.0 |
| E/A (0.75–1.5) | 1.2 | 0.3 | 1.1 | 0.3 | 0.1* |
| DT (<220 msec) | 184.1 | 27.1 | 174.3 | 24.5 | 9.7* |
| E/e´ (>6) | 6.8 | 1.9 | 6.1 | 1.7 | 0.7* |
| Epicardial fat thickness (0.9-13.5 mm) | 4.8 | 4.6 | 4.7 | 2.5 | 0.1 |
| Aortic valve regurgitation; degree 0, 1, 2 (%) | 82.7; 27.2; 1.2 | NA | 90; 10; 0 | NA | Table 2a |
| Mitral valve regurgitation; degree 0, 1, 2 (%) | 5.5; 93.6; 0.8 | NA | 0; 100; 0 | NA | NS |
| Tricuspid valve regurgitation; degree 0, 1, 2 (%) | 4.7; 95.7; 0.4 | NA | 0; 100; 0 | NA | NS |
| Pulmonary aortic valve regurgitation; degree 0, 1, 2 (%) | 3.8; 96.2; 0 | NA | 0; 100; 0 | NA | NS |
| Routine biochemical markers (normal range) | |||||
| ESR (0-29 mm/h) | 6.71 | 4.32 | 9.13 | 6.29 | -2.42* |
| Erythrocytes (3.8-5.9 x 1012/l) | 4.97 | 0.47 | 4.88 | 1.47 | 0.09* |
| Hemoglobin (116-166 g/l) | 152.27 | 17.97 | 141.86 | 18.01 | 10.41* |
| Leukocytes (4-11 x 109/l) | 6.46 | 1.55 | 6.58 | 2.37 | -0.12 |
| Platelets count (150-450 x 109/l) | 218.20 | 44.11 | 240.13 | 56.14 | -21.93* |
| Total cholesterol (<5.2 mmol/l) | 5.57 | 0.97 | 5.42 | 1.29 | 0.15 |
| HDL-cholesterol (>1 mmol/l) | 1.40 | 0.43 | 1.46 | 0.37 | -0.07 |
| LDL- cholesterol (<3.4 mmol/l) | 3.53 | 0.87 | 3.37 | 1.11 | 0.16 |
| Triglycerides (<1.7 mmol/l) | 1.50 | 1.07 | 1.39 | 0.99 | 0.10 |
| Glucose (3.9–5.6 mmol/l) | 5.84 | 0.75 | 5.86 | 3.54 | -0.02* |
| C-reactive protein (< 3 mg/l) | 2.00 | 3.17 | 3.02 | 9.47 | -1.02 |
| Uric acid (2.7-8.5 mg/dl) | 6.01 | 1.30 | 5.53 | 1.80 | 0.48* |
| Creatinine (44-106 µmol/l) | 82.02 | 13.18 | 75.78 | 18.09 | 6.24* |
| Alanine aminotransferase (4-36 U/l) | 26.99 | 17.38 | 23.51 | 19.04 | 3.48* |
| Aspartate aminotransferase (8-33 U/l) | 23.55 | 16.34 | 19.86 | 8.92 | 2.69* |
| Aortic valve regurgitation | IgG-SARS-negative (N=237) | IgG-SARS-positive (N=70) | Odds ratio; 95% CI | P |
|---|---|---|---|---|
| Degree 0, N | 169 | 63 | 3.6; 1.5-8.3 | 0.0024 |
| Degrees 1 and 2, N | 68 | 7 |
| Parameters in the model | B | S.E. | Wald | P | Exp(B) | 95% CI for EXP(B) | |
|---|---|---|---|---|---|---|---|
| Lower | Upper | ||||||
| SBP in 24-h monitoring | -0.06 | 0.03 | 3.79 | 0.05 | 0.94 | 0.89 | 1.00 |
| DBP in 24-h monitoring | 0.03 | 0.04 | 0.58 | 0.45 | 1.03 | 0.95 | 1.11 |
| AoSV | 0.55 | 0.69 | 0.64 | 0.43 | 1.73 | 0.45 | 6.67 |
| LA | 1.68 | 0.78 | 4.71 | 0.11 | 5.37 | 1.18 | 24.49 |
| LA volume | 0.01 | 0.02 | 0.24 | 0.63 | 1.01 | 0.97 | 1.05 |
| LVIDd | -0.13 | 0.65 | 0.04 | 0.84 | 0.88 | 0.25 | 3.15 |
| LVEDV | -0.02 | 0.04 | 0.16 | 0.69 | 0.99 | 0.91 | 1.06 |
| LVESV | -0.01 | 0.05 | 0.01 | 0.92 | 1.00 | 0.91 | 1.09 |
| SV | -0.01 | 0.04 | 0.02 | 0.88 | 0.99 | 0.92 | 1.08 |
| LVM | 0.01 | 0.01 | 0.54 | 0.46 | 1.01 | 0.98 | 1.04 |
| LVMI | -0.07 | 0.03 | 4.47 | 0.03 | 0.93 | 0.88 | 1.00 |
| Aortic valve opening amplitude | 0.38 | 1.12 | 0.11 | 0.74 | 1.46 | 0.16 | 13.21 |
| RA volume | -0.01 | 0.02 | 0.15 | 0.70 | 0.99 | 0.96 | 1.03 |
| sPAP | -0.01 | 0.04 | 0.11 | 0.74 | 0.99 | 0.92 | 1.06 |
| E/A | -1.60 | 0.75 | 4.54 | 0.03 | 0.20 | -1.60 | 0.75 |
| DT | -0.02 | 0.01 | 5.13 | 0.02 | 0.97 | -0.02 | 0.01 |
| E/e´ | 0.03 | 0.12 | 0.05 | 0.82 | 1.03 | 0.82 | 1.29 |
| Parameters in the model | Model-fitting criteria; -2 log likelihood of reduced model | Likelihood ratio tests | |
|---|---|---|---|
| Chi-squared | P | ||
| ESR | 279.81 | 4.23 | 0.04 |
| Erythrocytes | 275.74 | 0.16 | 0.68 |
| Hemoglobin | 280.79 | 5.21 | 0.02 |
| Platelets | 280.69 | 5.11 | 0.02 |
| Glucose | 275.80 | 0.22 | 0.63 |
| Uric acid | 275.58 | 0.003 | 0.95 |
| Creatinine | 276.63 | 1.06 | 0.30 |
| Alanine aminotransferase | 277.55 | 1.97 | 0.16 |
| Aspartate aminotransferase | 278.56 | 2.98 | 0.08 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




