Submitted:
05 June 2023
Posted:
05 June 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Measures
2.3. Statistical Analyses
3. Results
3.1. Descriptive Statistics and Attrition Analysis
3.2. Changes in the Severity of Symptoms
3.3. Structural Equation Modeling
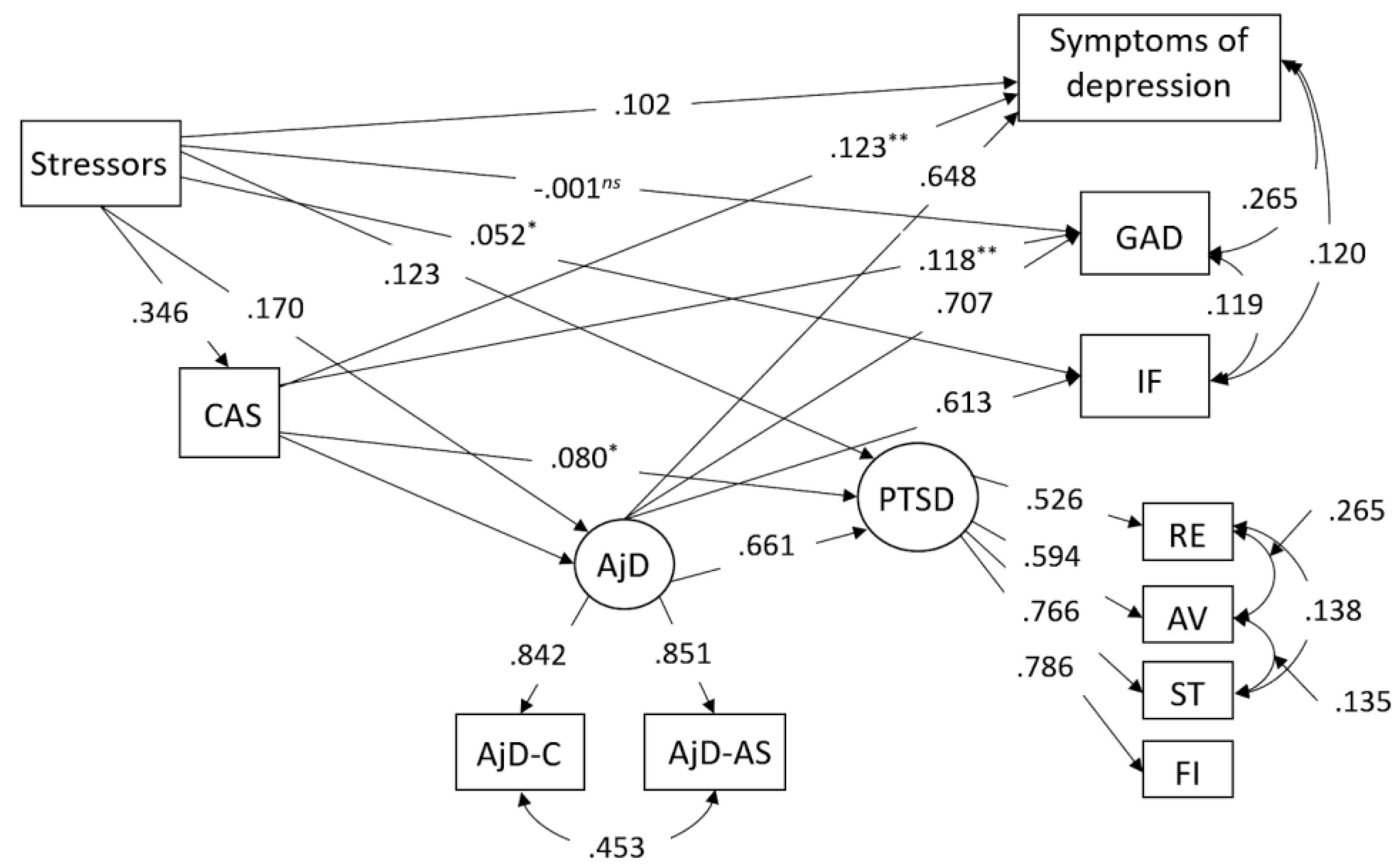
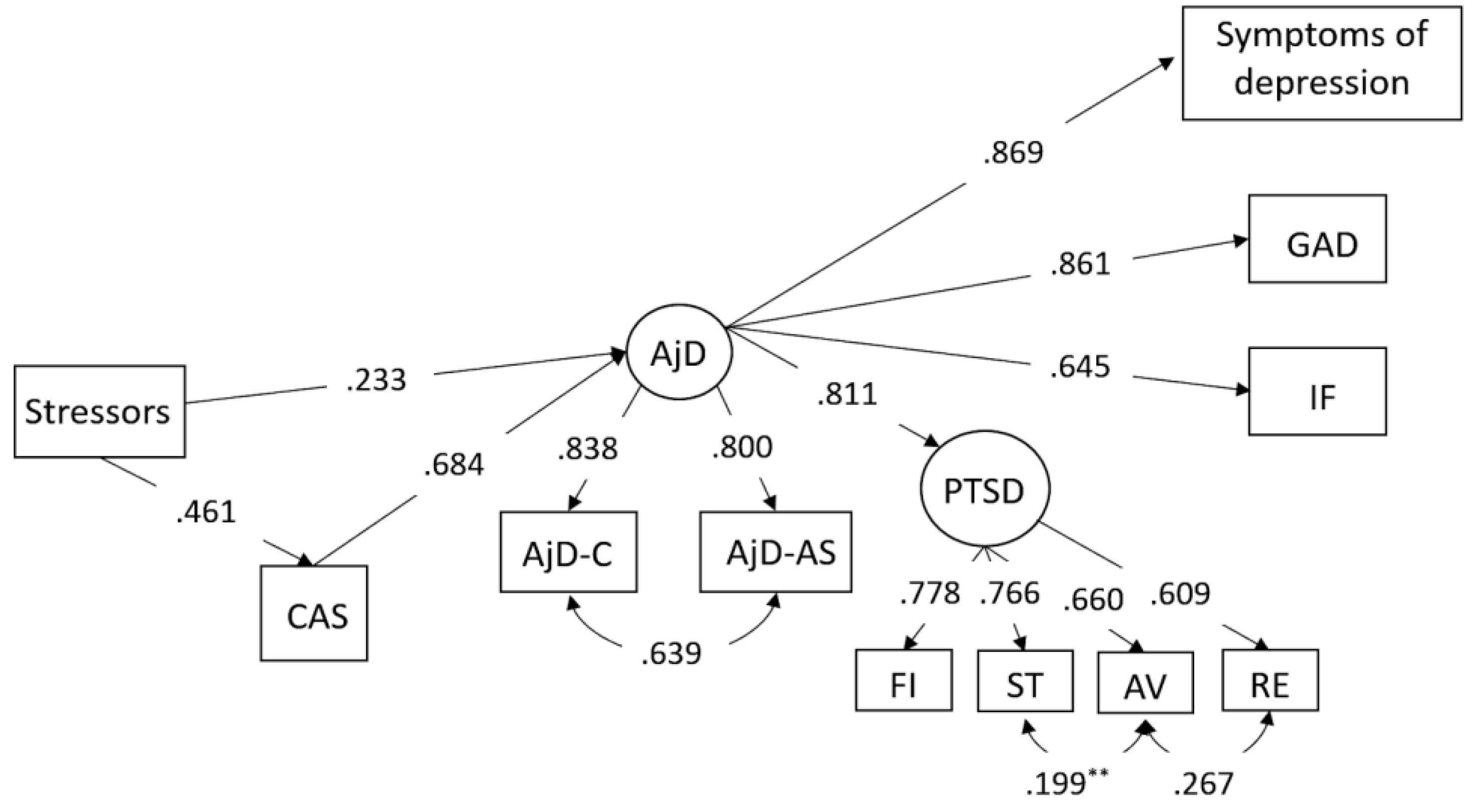
| Effects | T1 Estimate |
T2 Estimate |
|||
|---|---|---|---|---|---|
| 90% CI | p | 90% CI | p | ||
| Stressors –> CAS –> PTSD | .028 .006–.050 |
.038 | .070 -.012–.152 |
.162 | |
| Stressors –> AjD –> PTSD | .112 .085–.139 |
<.001 | .145 .071–.219 |
.001 | |
| Stressors –> CAS –> AjD –> PTSD | .153 .128–.178 |
<.001 | .211 .137–.284 |
<.001 | |
| Stressors –> AjD –> IF | .104 .080–.128 |
<.001 | .124 .061–.186 |
.001 | |
| Stressors –> CAS –> AjD –> IF | .142 .123–.161 |
< 001 | .180 .129–.231 |
<.001 | |
| Stressors –> AjD –> Depression Symptoms | .110 .083–.137 |
<.001 | .174 .076–.272 |
.003 | |
| Stressors –> CAS –> Depression Symptoms | .042 .020–.065 |
.002 | .025 -.076–.127 |
.681 | |
| Stressors –> CAS –> AjD –> Depression Symptoms | .150 .124–.150 |
<.001 | .254 .149–.359 |
<.001 | |
| Stressors –> CAS –> GAD | .041 .021–.061 |
.001 | .016 -.059–.091 |
.730 | |
| Stressors –> AjD –> GAD | .120 .091–.149 |
<.001 | .168 .079–.257 |
.002 | |
| Stressors –> CAS –> AjD –> GAD | .164 .139–.189 |
<.001 | .244 .158–.330 |
<.001 | |
4. Discussion
5. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Wells A. Metacognitive therapy for anxiety and depression. New York: Guilford Press; 2009.
- Wells, A.; Matthews, G. Attention and emotion: A clinical perspective. Hove Lawrence Erlbaum, UK; 1994.
- Wells A; Matthews G. Modeling cognition in emotional disorder: The S-REF model. Behav. Res. Ther. 1996; 34(11):881–8. [CrossRef]
- Kowalski, J.; Dragan, M. Cognitive-attentional syndrome – The psychometric properties of the CAS-1 and multi-measure CAS-based clinical diagnosis. Compr. Psychiatry 2019; 91:13-21. [CrossRef]
- Capobianco, L.; Nordahl, H. A brief history of metacognitive therapy: From cognitive science to clinical practice. Cogn. Behav. Pract. 2023; 30(1):45-54, . [CrossRef]
- Sun, X.; Zhu, C.; So, S.H.W. Dysfunctional metacognition across psychopathologies: A meta-analytic review. Eur Psychiatry 2017; 45:139-153. [CrossRef]
- Gkika, S.; Wittkowski, A.; Wells, A. (2017). Social cognition and metacognition in social anxiety: a systematic review. Clin. Psychol. Psychother. 25, 10–30. [CrossRef]
- Brown, R.L. et al. The metacognitive model of post-traumatic stress disorder and metacognitive therapy for post-traumatic stress disorder: A systematic review. Clin. Psychol. Psychother. 2022; 29(1):131-146. [CrossRef]
- Dragan, M.; Kowalski, J. Childhood adversities and psychopathology in participants with high and low severity of cognitive-attentional syndrome symptoms. Eur. J. Trauma Dissociation 2020: 4:100112. [CrossRef]
- Dragan, M.; Grajewski, P.; Shevlin, M. Adjustment disorder, traumatic stress, depression and anxiety in Poland during an early phase of the COVID-19 pandemic. Eur. J. Psychotraumatol 2021; 12(1):1860356. [CrossRef]
- Rossi, R. et al. Stressful life events and resilience during the COVID-19 lockdown measures in Italy: association with mental health outcomes and age. Front. Psychiatry 2021; 12:635832. [CrossRef]
- Hyland, P. et al. Anxiety and depression in the Republic of Ireland during the COVID-19 pandemic. Acta Psychiatr. Scand. 2020; 142(3):249-256. [CrossRef]
- Shevlin, M. et al. Anxiety, depression, traumatic stress and COVID-19-related anxiety in the UK general population during the COVID-19 pandemic. BJPsych open 2020; 6(6): e125. [CrossRef]
- Gambin, M. et al. Generalized anxiety and depressive symptoms in various age groups during the COVID-19 lockdown in Poland. Specific predictors and differences in symptoms severity. Compr. Psychiatry 2021; 105:152222. [CrossRef]
- Olff, M. et al. Mental health responses to COVID-19 around the world. Eur. J. Psychotraumatol 2021; 12(1):1929754.
- Fergus, T.A., Bardeen, J.R., Orcutt, H.K. Attentional control moderates the relationship between activation of the cognitive attentional syndrome and symptoms of psychopathology. Personal. Individ. Differ. 2012; 53(3): 213-217. [CrossRef]
- Mundt, J. C.; Marks, I. M.; Shear, M. K.; Greist, J. M. The Work and Social Adjustment Scale: A simple measure of impairment in functioning. Br. J. Psychiatry 2002; 180:461–464. [CrossRef]
- Einsle, F.; Köllner, V.; Dannemann, S.; Maercker, A. Development and validation of a self-report for the assessment of adjustment disorders. Psychol. Health Med. 2010; 15:584–595. [CrossRef]
- Lorenz, L.; Bachem, R. C.; Maercker, A. The Adjustment Disorder–New Module 20 as a screening instrument: Cluster analysis and cut-off values. Int. J. Occup. Environ. Med. 2016; 7:215-220. [CrossRef]
- Shevlin, M. et al. Measuring ICD-11 adjustment disorder: The development and initial validation of the International Adjustment Disorder Questionnaire. Acta Psychiatr. Scand. 2020; 141(3):265-274. [CrossRef]
- Cloitre, M.; Shevlin, M.; Brewin, C. R.; Bisson, J. I.; Roberts, N. P.; Maercker, A.; Karatzias T.; Hyland, P. The International Trauma Questionnaire: Development of a self-report measure of ICD-11 PTSD and complex PTSD. Acta Psychiatr. Scand. 2018; 138:1-11. [CrossRef]
- Redican, E. et al. The latent structure of ICD-11 posttraumatic stress disorder (PTSD) and complex PTSD in a general population sample from USA: a factor mixture modelling approach. J. Anxiety Disord. 2022; 85:102497. [CrossRef]
- Kroenke, K.; Spitzer, R. L.; Williams, J. B. W. The PHQ-9. J. Gen. Intern. Med. 2001; 16:606–613.
- Kokoszka, A.; Jastrzębski, A.; Obrębski, M. Psychometric properties of the Polish version of Patient Health Questionnaire-9. Psychiatria 2016; 13:187–193.
- Manea, L.; Gilbody, S.; McMillan, D. A diagnostic meta-analysis of the Patient Health Questionnaire-9 (PHQ-9) algorithm scoring method as a screen for depression. Gen. Hospit. Psychiatr. 2015; 37:67–75. [CrossRef]
- Spitzer, R. L.; Kroenke, K.; Williams, J. B. W.; Löwe, B. A brief measure for assessing generalized anxiety disorder. Arch. Intern. Med. 2006; 166:1092.
- Rutter, L. A.; Brown, T. A. Psychometric properties of the Generalized Anxiety Disorder Scale-7 (GAD-7) in outpatients with anxiety and mood disorders. J. Psychopathol. Behav. Assess. 2016; 39:140–146. [CrossRef]
- Lin, L.; Aloe, A. M. Evaluation of various estimators for standardized mean difference in meta-analysis. Stat. Med. 2021; 40(2):403–426. [CrossRef]
- Nicholson, J. S.; Deboeck, P. R.; Howard, W. Attrition in developmental psychology: A review of modern missing data reporting and practices. Int. J. Behav. Dev. 2017; 41(1):143–153.
- Muthén, L. K.; Muthén, B. O. MPlus user’s Guide 8th version (March). Los Angeles: Authors; 2017.
- Hu, L.; Bentler, P.M. Cutoff criteria for fit indexes in covariance structure analysis: Conventional criteria versus new alternatives. Struct. Equ. Modeling 1999; 6(1):1–55. [CrossRef]
- Cheung, Gordon W.; Rensvold, Roger B. Evaluating goodness-of-fit indexes for testing measurement invariance. Struct. Equ. Modeling 2002; 9(2):233–255.
| T1 | T2 | ||||
|---|---|---|---|---|---|
| Variables | M | SD | M | SD | n |
| Adjustment Disorder | |||||
| Number of Stressors | 5.34 | 2.25 | 5.42 | 2.50 | 360 |
| Core Symptoms | 21.23 | 6.55 | 20.11 | 6.67 | 330 |
| Accessory Symptoms | 31.59 | 8.88 | 29.98 | 9.68 | 330 |
| Preoccupation | 11.33 | 3.55 | 10.50 | 3.56 | 330 |
| Failure to Adapt | 9.90 | 3.53 | 9.61 | 3.63 | 330 |
| Avoidance | 9.94 | 3.42 | 9.57 | 3.67 | 330 |
| Depressive Mood | 8.32 | 2.56 | 7.89 | 2.65 | 330 |
| Anxiety | 5.41 | 1.86 | 5.10 | 1.94 | 330 |
| Impulsivity | 7.92 | 2.81 | 7.41 | 2.87 | 330 |
| PTSD | |||||
| Re-experiencing | 2.78 | 2.36 | 4.86 | 2.48 | 287 |
| Avoidance | 3.59 | 2.53 | 5.53 | 2.62 | 287 |
| Sense of Threat | 3.68 | 2.61 | 5.37 | 2.77 | 287 |
| PTSD Functional Impairment | 4.31 | 3.87 | 4.07 | 3.90 | 287 |
| Depression Symptoms | 11.20 | 6.52 | 10.05 | 6.55 | 279 |
| Symptoms of Seneralized anxiety | 9.55 | 5.87 | 7.71 | 5.72 | 366 |
| Cognitive–Attentional syndrome | 75.40 | 19.88 | 73.96 | 20.33 | 279 |
| Impaired Functioning | 21.13 | 8.59 | 18.23 | 10.54 | 362 |
| Prevalence | |||||
| Impaired Functioning | |||||
| Mild Functional Impairment | 13% | n = 215 | 30% | n = 109 | |
| Moderately Severe Functional Impairment | 35% | n = 601 | 26% | n = 96 | |
| Severe Functional Impairment | 52% | n = 877 | 44% | n = 161 | |
| Depression | 31% | n = 520 | 19% | n = 70 | |
| Generalized Anxiety | 45% | n = 764 | 33% | n = 122 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




