Submitted:
07 March 2023
Posted:
08 March 2023
Read the latest preprint version here
Abstract
Keywords:
Introduction
Mthods
Study Design
Participants
Procedures
Postural Exercise Training
Measurements
Statistical Analysis
Results
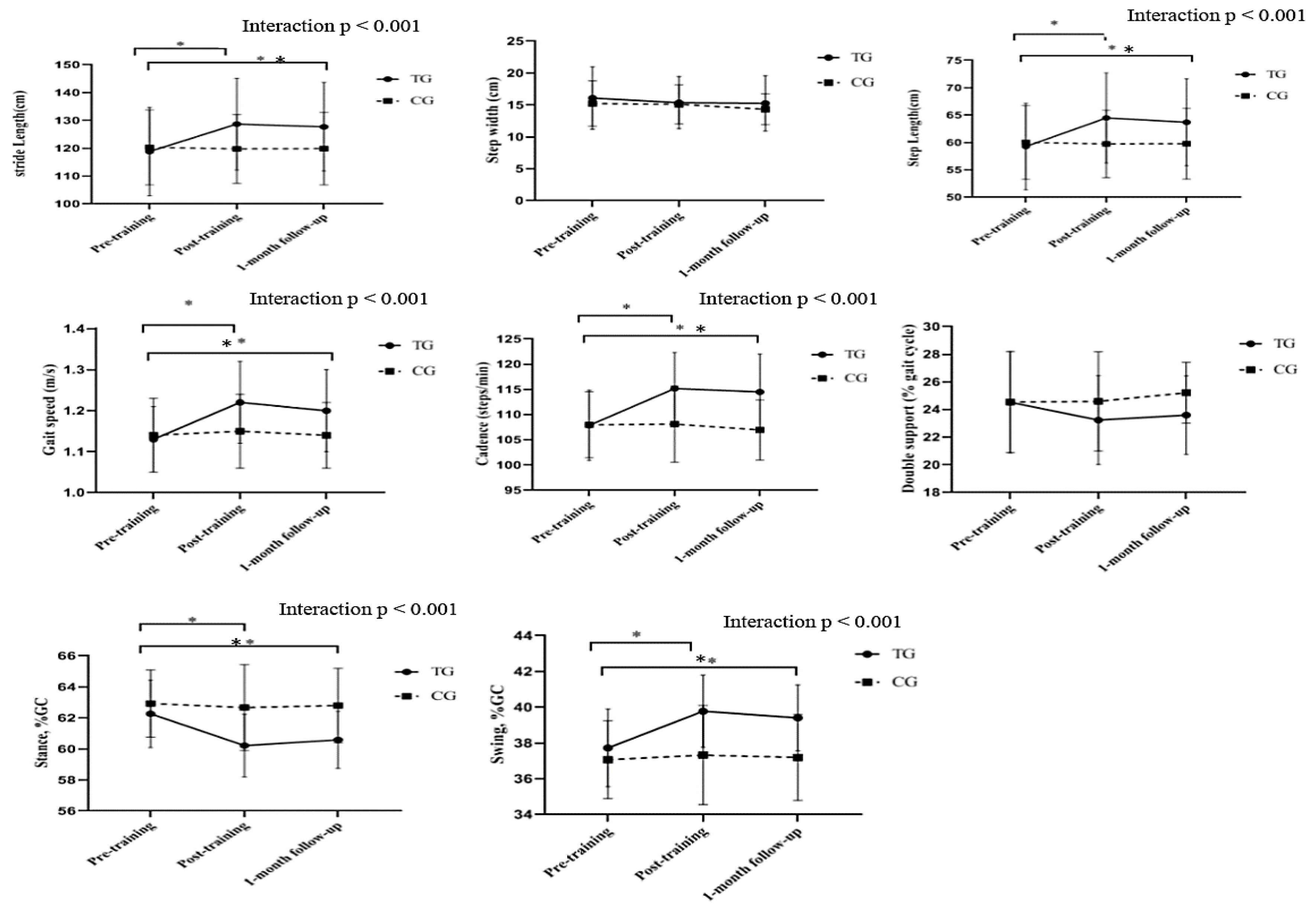
Gait Parameters
Discussion
Limitations
Implications and Suggestions for Future Research
Conclusions
Submission deceleration
Acknowledgment
Disclosure statement
Funding source
Informed Consent Statement
References
- Ahmadi, N., Peyk, F., Hovanloo, F., & Hemati Garekani, S. (2020). Effect of functional strength training on gait kinematics, muscle strength and static balance of young adults with Down syndrome. International Journal of Motor Control and Learning 2, 1–10. [CrossRef]
- Almuhtaseb, S., Oppewal, A., & Hilgenkamp, T. I. (2014). Gait characteristics in individuals with intellectual disabilities: A literature review. Research in developmental disabilities 35, 2858–2883. [CrossRef] [PubMed]
- Angulo-Barroso, R. M., Wu, J., & Ulrich, D. A. (2008). Long-term effect of different treadmill interventions on gait development in new walkers with Down syndrome. Gait & posture 27, 231–238. [CrossRef] [PubMed]
- Ardestani, M. M., Ferrigno, C., Moazen, M., & Wimmer, M. A. (2016). From normal to fast walking: impact of cadence and stride length on lower extremity joint moments. Gait & posture 46, 118–125. [CrossRef] [PubMed]
- Bahiraei, S., Daneshmandi, H., Norasteh, A. A., & Sokhangoei, Y. (2018). The Study of Biomechanical Gait Cycle and Balance Characteristics in Intellectual Disabilities: A Systematic Review. Physical Treatments - Specific Physical Therapy 8, 63–76. [CrossRef]
- Bahiraei, S., Daneshmandi, H., Norasteh, A.A., Yahya, S. (2019). Balance stability in intellectual disability: Introductory evidence for the balance evaluation systems test (BESTest). Life Span and Disability 22, 7–28.
- Behm, D. G., Anderson, K., & Curnew, R. S. (2002). Muscle force and activation under stable and unstable conditions. The Journal of Strength & Conditioning Research 16, 416–422.
- Berg, K. O., Wood-Dauphinee, S. L., Williams, J. I., & Maki, B. (1991). Measuring balance in the elderly: validation of an instrument. Canadian journal of public health 39, 7–11.
- Blomqvist, S., Wester, A., Sundelin, G., & Rehn, B. (2012). Test–retest reliability, smallest real difference and concurrent validity of six different balance tests on young people with mild to moderate intellectual disability. Physiotherapy 98, 313–319. [CrossRef]
- Carmeli, E., Kessel, S., Coleman, R., & Ayalon, M. (2002). Effects of a treadmill walking program on muscle strength and balance in elderly people with Down syndrome. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences 57, M106–M110. [CrossRef]
- Cioni, M., Cocilovo, A., Rossi, F., Paci, D., & Valle, M. S. (2001). Analysis of ankle kinetics during walking in individuals with Down syndrome. American Journal on Mental Retardation 106, 470–478. [CrossRef]
- Cleaver, S., Hunter, D., & Ouellette-Kuntz, H. (2009). Physical mobility limitations in adults with intellectual disabilities: a systematic review. Journal of Intellectual Disability Research 53, 93–105. [CrossRef] [PubMed]
- Elshemy, S. A. (2013). Comparative study: Parameters of gait in Down syndrome versus matched obese and healthy children. Egyptian Journal of Medical Human Genetics 14, 285–291. [CrossRef]
- Enkelaar, L., Smulders, E., van Schrojenstein Lantman-de Valk, H., Geurts, A. C., & Weerdesteyn, V. (2012). A review of balance and gait capacities in relation to falls in persons with intellectual disability. Research in developmental disabilities 33, 291–306. [CrossRef] [PubMed]
- Galli, M., Rigoldi, C., Brunner, R., Virji-Babul, N., & Giorgio, A. (2008). Joint stiffness and gait pattern evaluation in children with Down syndrome. Gait & posture 28, 502–506. [CrossRef] [PubMed]
- Galli, M., Rigoldi, C., Mainardi, L., Tenore, N., Onorati, P., & Albertini, G. (2008). Postural control in patients with Down syndrome. Disability and rehabilitation 30, 1274–1278. [CrossRef] [PubMed]
- Giagazoglou, P., Kokaridas, D., Sidiropoulou, M., Patsiaouras, A., Karra, C., & Neofotistou, K. (2013). Effects of a trampoline exercise intervention on motor performance and balance ability of children with intellectual disabilities. Research in developmental disabilities 34, 2701–2707. [CrossRef] [PubMed]
- Hartman, E., Houwen, S., Scherder, E., & Visscher, C. (2010). On the relationship between motor performance and executive functioning in children with intellectual disabilities. Journal of Intellectual Disability Research 54, 468–477. [CrossRef] [PubMed]
- Horak, F. B., Wrisley, D. M., & Frank, J. (2009). The balance evaluation systems test (BESTest) to differentiate balance deficits. Physical therapy 89(5), 484–498. [CrossRef]
- Huri, M., Huri, E., Kayihan, H., & Altuntas, O. (2015). Effects of occupational therapy on quality of life of patients with metastatic prostate cancer: a randomized controlled study. Saudi medical journal 36, 954. [CrossRef]
- JudgeRoy, J. O., Davis III, B., & Õunpuu, S. (1996). Step length reductions in advanced age: the role of ankle and hip kinetics. The Journals of Gerontology Series A: Biological Sciences and Medical Sciences 51, M303–M312. [CrossRef]
- Kachouri, H., Laatar, R., Borji, R., Rebai, H., & Sahli, S. (2020). Using a dual-task paradigm to investigate motor and cognitive performance in children with intellectual disability. Journal of Applied Research in Intellectual Disabilities 33, 172–179. [CrossRef]
- Kubilay, N. S., Yildirim, Y., Kara, B., & Harutoglu-Akdur, H. (2011). Effect of balance training and posture exercises on functional level in mental retardation. Fizyoterapi Rehabilitasyon 22(2), 55–64.
- Lee, K., Lee, M., & Song, C. (2016). Balance training improves postural balance, gait, and functional strength in adolescents with intellectual disabilities: Single-blinded, randomized clinical trial. Disability and health journal 9, 416–422. [CrossRef]
- Lee, K. J., Lee, M. M., Shin, D. C., Shin, S. H., & Song, C. H. (2014). The effects of a balance exercise program for enhancement of gait function on temporal and spatial gait parameters in young people with intellectual disabilities. Journal of physical therapy science 26(4), 513–516. [CrossRef]
- Lin, L.-P., Hsia, Y.-C., Hsu, S.-W., Loh, C.-H., Wu, C.-L., & Lin, J.-D. (2013). Caregivers’ reported functional limitations in activities of daily living among middle-aged adults with intellectual disabilities. Research in developmental disabilities 34, 4559–4564. [CrossRef]
- Lipfert, S. W., Günther, M., Renjewski, D., & Seyfarth, A. (2014). Impulsive ankle push-off powers leg swing in human walking. Journal of experimental biology 217, 1218–1228. [CrossRef]
- Llorens-Martin, M., Rueda, N., Tejeda, G. S., Flórez, J., Trejo, J. L., & Martínez-Cué, C. (2010). Effects of voluntary physical exercise on adult hippocampal neurogenesis and behavior of Ts65Dn mice, a model of Down syndrome. Neuroscience 171(4), 1228–1240. [CrossRef]
- Long, J., Feng, Y., Liao, H., Zhou, Q., & Urbin, M. (2018). Motor sequence learning is associated with hippocampal subfield volume in humans with medial temporal lobe epilepsy. Frontiers in Human Neuroscience 12, 367. [CrossRef]
- Lopes Pedralli, M., & Schelle, G. H. (2013). Gait evaluation in individuals with Down syndrome. Brazilian Journal of Biomotricity 7(1), 21–27.
- Maas, S., Festen, D., Hilgenkamp, T. I., & Oppewal, A. (2020). The association between medication use and gait in adults with intellectual disabilities. Journal of Intellectual Disability Research 64, 793–803. [CrossRef]
- Nam, H.-C., Cha, H.-G., & Kim, M.-K. (2016). The effects of exercising on an unstable surface on the gait and balance ability of normal adults. Journal of physical therapy science 28(7), 2102–2104. [CrossRef]
- Novak, I., & Morgan, C. (2019). High-risk follow-up: early intervention and rehabilitation. Handbook of clinical neurology 162, 483–510. [CrossRef]
- Oppewal, A., Festen, D. A., & Hilgenkamp, T. I. (2018). Gait characteristics of adults with intellectual disability. American journal on intellectual and developmental disabilities 123(3), 283–299. [CrossRef]
- Oppewal, A., & Hilgenkamp, T. I. (2019). The dual task effect on gait in adults with intellectual disabilities: is it predictive for falls? Disability and rehabilitation 41, 26–32. [CrossRef]
- Pal, J. Pal, J., Hale, L., Mirfin-Veitch, B., & Claydon, L. (2014). Injuries and falls among adults with intellectual disability: A prospective New Zealand cohort study. Journal of Intellectual and Developmental Disability 39(1), 35–44. [CrossRef]
- Reguera-García, M. M., Leirós-Rodríguez, R., Fernández-Baro, E., & Álvarez-Barrio, L. (2021). Reliability and Validity of the Six Spot Step Test in People with Intellectual Disability. Brain Sciences 11, 201. [CrossRef]
- Rigoldi, C., Galli, M., & Albertini, G. (2011). Gait development during lifespan in subjects with Down syndrome. Research in developmental disabilities 32(1), 158–163. [CrossRef]
- Rigoldi, C., Galli, M., Cimolin, V., Camerota, F., Celletti, C., Tenore, N., & Albertini, G. (2012). Gait strategy in patients with Ehlers-Danlos syndrome hypermobility type and Down syndrome. Research in developmental disabilities 33, 1437–1442. [CrossRef]
- Rodenbusch, T. L., Ribeiro, T. S., Simão, C. R., Britto, H. M., Tudella, E., & Lindquist, A. R. (2013). Effects of treadmill inclination on the gait of children with Down syndrome. Research in developmental disabilities 34(7), 2185–2190. [CrossRef]
- Rosen, S. (1997). Kinesiology and sensorimotor function. Foundations of orientation and mobility 170–199.
- Rosenthal, J. A. (1996). Qualitative descriptors of strength of association and effect size. Journal of social service Research, 21, 37–59. [CrossRef]
- Schalock, R. L., Luckasson, R., & Tassé, M. J. Intellectual Disability: Definition, Classification, and Systems of Supports. AAIDD, 12th ed.; American Association on Intellectual and Developmental Disabilities: Washington, USA, 2021. [Google Scholar]
- Shashidhara, M. (2018). The effect of eight-week yoga exercise on balance and gait in girls with intellectual disability. International Journal of Yoga and Allied Sciences 7, 31–35.
- Sibley, K. M., Beauchamp, M. K., Van Ooteghem, K., Straus, S. E., & Jaglal, S. B. (2015). Using the systems framework for postural control to analyze the components of balance evaluated in standardized balance measures: a scoping review. Archives of physical medicine and rehabilitation 96, 122–132.e129. [CrossRef]
- Smith, B. A., Ashton-Miller, J. A., & Ulrich, B. D. (2010). Gait adaptations in response to perturbations in adults with Down syndrome. Gait & posture 32, 149–154. [CrossRef] [PubMed]
- Smith, B. A., & Ulrich, B. D. (2008). Early onset of stabilizing strategies for gait and obstacles: older adults with Down syndrome. Gait & posture 28, 448–455. [CrossRef] [PubMed]
- Souza, A. P. S. d., Silva, L. C. d., & Fayh, A. P. T. (2021). Nutritional Intervention Contributes to the Improvement of Symptoms Related to Quality of Life in Breast Cancer Patients Undergoing Neoadjuvant Chemotherapy: A Randomized Clinical Trial. Nutrients 13, 589. [CrossRef]
- Tong, L., Shen, H., Perreau, V. M., Balazs, R., & Cotman, C. W. (2001). Effects of exercise on gene-expression profile in the rat hippocampus. Neurobiology of disease 8, 1046–1056. [CrossRef]
- TS, H. (2008). The effects of run/walk exercise on physical fitness and sport skills on individuals with mental retardation. NCYU Phys Educ Health Recreat J 7, 44–58.
- Ulrich, D. A., Ulrich, B. D., Angulo-Kinzler, R. M., & Yun, J. (2001). Treadmill training of infants with Down syndrome: evidence-based developmental outcomes. Pediatrics 108, e84. [CrossRef]
- Verghese, J., Holtzer, R., Lipton, R. B., & Wang, C. (2009). Quantitative gait markers and incident fall risk in older adults. The Journals of Gerontology: Series A 64, 896–901. [CrossRef]
- Vinagre, I. N., Cámara, M. B., & Gadella, J. B. (2016). Gait analysis and Bobath physiotherapy in adults with Down syndrome. International Medical Review on Down Syndrome 20(1), 8–14. [CrossRef]
- World Health Organization. International Classification of Functioning, Disability and Health: ICF, Geneva, Switzerland, 2001.
- World Medical Association. (2013). World medical association declaration of Helsinki. JAMA 310(20), 2191–2194. [CrossRef] [PubMed]
| Variables | Training Group (n=19) |
Control Group (n=15) |
t | p |
|---|---|---|---|---|
| M ± SD | M ± SD | |||
| Age (year) | 20.47±4.59 | 20.27±2.31 | 0.16 | 0.87 |
| Height (cm) | 168.53±8.1 | 168.27±6.68 | 2.09 | 0.141 |
| Weight (kg) | 69.05±15.16 | 66.77±11.32 | 1.00 | 0.92 |
| BMI (kg/m2) | 24.25±4.67 | 23.57±3.83 | 0.46 | 0.65 |
| IQ | 50-70 | 50-70 | ||
| Note: data are expressed as mean ± standard deviation. Abbreviations: BMI: body mass index; IQ: intelligence quotient. | ||||
| Activities | Duration | Activities performed as part of the program | Goal |
|---|---|---|---|
| Warm-up activities | 10 min | Slow and fast walk/ run /stretching |
|
| Postural Exercises Based on BESTest | 40 min | 1- Double leg stance with eyes closed; 2- Single leg stance with eyes open; 3- Sitting on the Swiss ball; 4- Sitting on a Swiss ball, lifting the lower extremity and putting on and taking off footwear; 5- Sitting on a Swiss ball and assuming a standing position; participants were asked to reach a shelf with their upper extremity, take off a toy and return to a sitting position; 6- Walking and increasing step length; 7- Emily post relay walking; 8- Walking posture; 9- Dual-task walking; 10- Standing on the floor with the ball overhead and moving it to the sides; 11- Jumping jacks on the mini-trampoline; 12- Jump on a mini-trampoline and receiving and throwing a ball; 13- Standing on two air cushions and catching a ball thrown by a therapist; 14- Autonomic strategic exercise of the ankle and hip; 15- Automatic strategic exercise (front, back and side) using resistance bands. |
|
| Cool-down activities | 10 min | light stretching/flexibility training |
|
| Outcomes | TG (n = 19) | CG (n = 15) | ||||
|---|---|---|---|---|---|---|
| Pre-training | Post-training | 1-month follow-up | Pre-training | Post-training | 1-month follow-up | |
| Step length (cm) | 59.27±7.90 | 64.19±8.22a,b | 63.70±7.94c,a | 60.01±6.72 | 59.74±6.16 | 59.79±6.47 |
| stride length (cm) | 118.83±15.85 | 128.69±16.48a,b | 127.71±15.92c,a | 120.31±13.47 | 119.78±12.35 | 119.88±12.97 |
| Cadence (steps/min) | 107.88±6.98 | 115.17±7.14a,b | 114.51±7.50c,a | 107.98±6.54 | 108.13±7.56 | 106.96±5.95 |
| Step width (cm) | 16.08±4.90 | 15.37±4.08 | 15.26±4.32 | 15.23±3.56 | 15.10±3.06 | 14.33±2.4 |
| Gait speed (m/s) | 1.13±0.08 | 1.22±0.10a,b | 1.20±0.10c,a | 1.14±0.09 | 1.15±0.09 | 1.14±0.08 |
| Double support %GC | 24.53±3.67 | 23.24±3.22 | 23.60±2.84 | 24.55±3.65 | 24.59±3.59 | 25.22±2.20 |
| Stance, %GC | 62.27±2.17 | 60.22±2.01a,b | 60.59±1.84c,a | 62.93±2.17 | 62.67±2.77 | 62.80±2.4 |
| Swing, %GC | 37.73±2.17 | 39.78±2.01a,b | 39.41±1.84c,a | 37.07±2.17 | 37.33±2.77 | 37.20±2.4 |
| Note: data are expressed as mean ± standard deviation Abbreviations: TG: Training Group; CG: Control Group; %GC: percentage of the gait cycle. a Within-TG differences from pre-training values (p < 0.05). b Between-group differences at post-test (p < 0.05). c Between-group differences at follow-up test (p < 0.05). | ||||||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




