Submitted:
18 January 2023
Posted:
24 January 2023
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design
2.2. Study Setting
2.3. Sampling
2.4. Procedures
2.5. Measures
2.6. Data Analysis
2.7. Ethical Considerations
3. Results
3.1. Participants’ Socio-Demographics
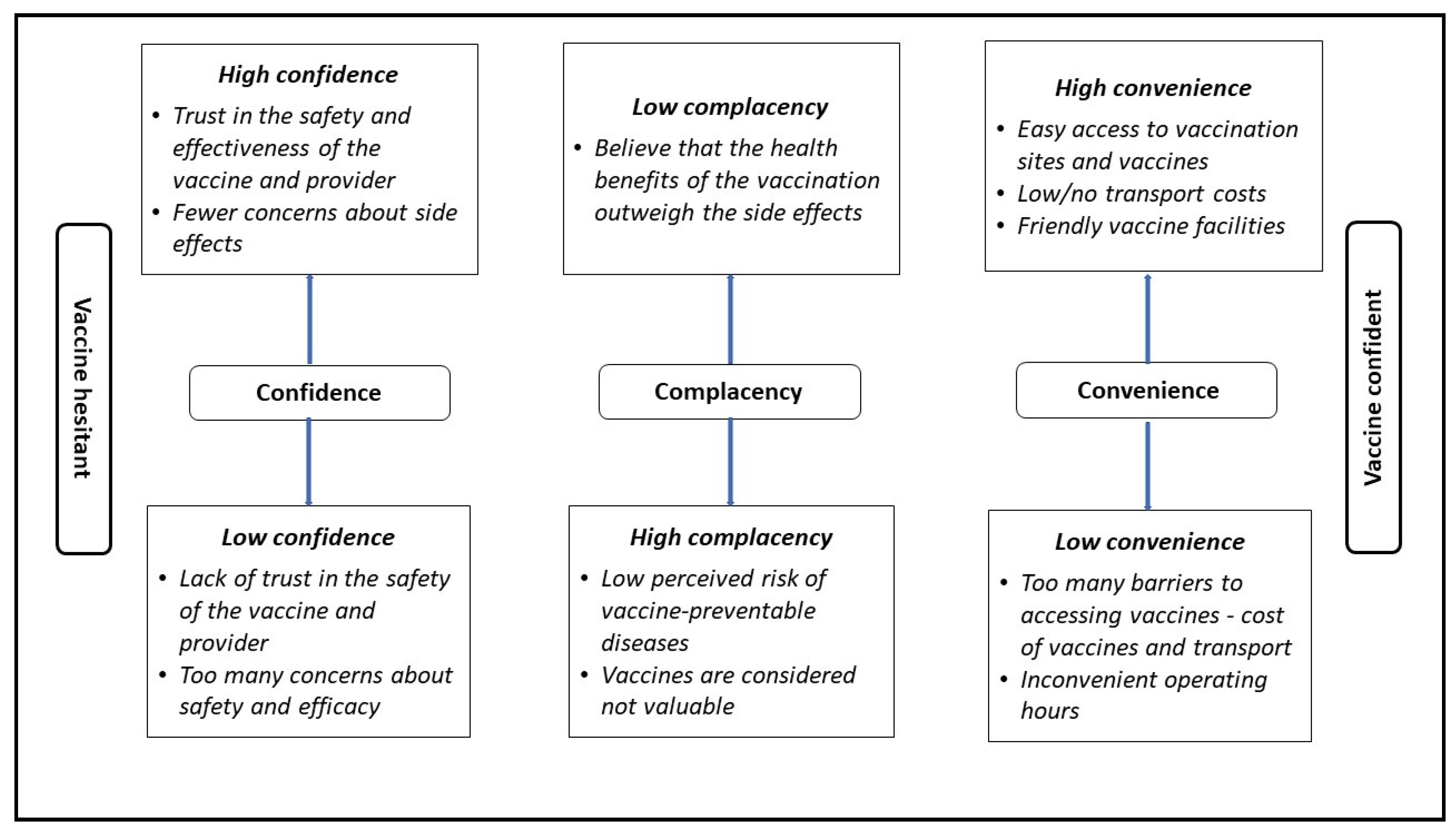
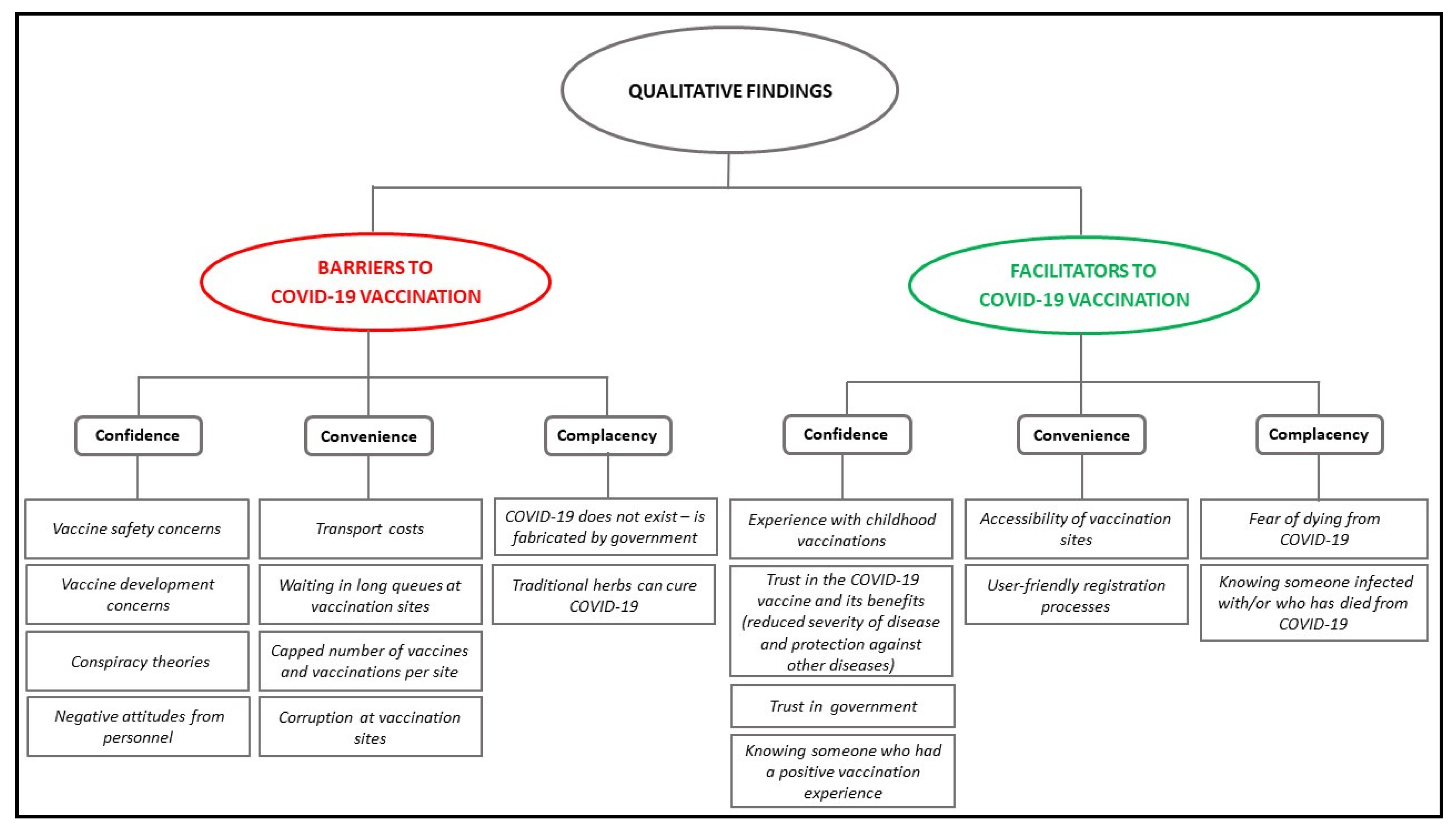
3.2. Barriers to COVID-19 Vaccination
3.2.1. Lack of Convenience as Barrier
“If there’s a line, so most of the people isn’t going because no one wants to stand in the line.”(UV_18–35_WC)
“There were a lot of people at the vaccination site to an extent that someone wakes up around 4 am but could not get the number to be vaccinated. It’s true there were now many people who knew they now needed to be vaccinated. Without blaming the nurses, some people lost interest and eventually stayed at home.”(V_45+_ZIM)
“I just think what’s preventing people … in fact from the time you enter through the gate here going to the point where they vaccinate you, maybe I’m expecting to spend 30 minutes. After spending the one hour here, I will also tell people back home that I almost died of hunger there at the hospital whilst they linger and vaccinate us at their own pace, so the ones I tell will hesitate to come.”(V_45+_ZIM)
“… But when I returned for the second time, the challenge was [that] there were only two of us, so we had to wait for an additional four people to come so that they could open a batch of vaccines and inject us. We came in early, and we had to wait close to an hour, waiting for people trickling in. That one was also the challenge.”(V_50+_GP)
“Some people said, ‘we don’t get the vaccine; we buy vaccination cards’. So I feel like the whole system was bad.”(V_45+_ZIM)
“Some would come and stand at the gate with money on a paper and hand it to someone … That discouraged me because I will have come in time. The person who would’ve come will just hand over money and do not get vaccinated and leave you on the queue pretending as if they have been vaccinated.”(V_18-44_ZIM)
3.2.2. Low Confidence as a Barrier
“… Cancer and HIV have always been here but now there is COVID-19 and they managed to get the vaccine so quick. When did they do the research? So quick there is vaccine, and they collect it from the airport. When did they manufacture the vaccine? There is this disease, but already they manufactured this. When did they mix the medications and see how they function? They cannot get the cure for HIV/AIDS, cancer, high blood, and sugar [diabetes].”(V_35–49_11_GP)
“… But people are saying we are going to change in two or three years’ time and become zombies, all those who are vaccinated. I am so scared to be vaccinated and I am not ready yet.”(UV_35–49_WC)
“So, this is why we couldn’t get vaccinated because of what we heard in the community—people saying ‘Ahh, this vaccine was brought to clear [reduce] the population, it’s clearing and it’s killing’.”(UV_18–44_ZIM)
3.2.3. High Complacency as a Barrier
“I am also not concerned because the COVID symptoms are just in your head, and if you tell yourself that you have COVID, that’s when you’ll see symptoms; otherwise, you have to treat yourself.”(UV_18–26_GP)
“No, you will use your tablets or homemade medication like garlic and olive leaves. I still have garlic in my refrigerator. I don’t want to be vaccinated; I am healthy.”(UV_50+_WC)
“Here I support what they are saying, that I can be vaccinated but I am safe if I get zumbani or whatever and just drink.”(UV_45+_ZIM)
3.3. Motivators for COVID-19 Vaccine Uptake
3.3.1. Convenience as a Motivator
“Yes, because we have many vaccination sites that side, so it was not difficult at all.”(V_18–35_GP)
“It is easy, because you go there—even if you are not registered online, you go there, and they register you at the table. It is an easy process.”(V_36–49_GP)
3.3.2. Confidence as a MOTIVATOR
“The reason I got vaccinated is that I trust the government will not kill the people. I am still alive … the government and the department of health will not kill [the] people. If they say there is a disease, and they say we should vaccinate, surely they want us to live.”(V_50+_GP)
“What really made me to get vaccinated is I heard that if you are vaccinated, it prevents the severity of COVID disease, and you experience less pain when it affects you because our immunity ... they attack each other. Even my sister got COVID, and she had minor symptoms because she was vaccinated. Because of this, I decided to get vaccinated.”(V_45+_ZIM)
3.3.3. Low Complacency as a Motivator
“I vaccinated because I survived two times from Corona. I had Corona, so I saw a need to vaccinate since they said there will be [a] fourth wave, maybe I will not survive this time. So, I decided to get vaccinated to help myself because I nearly died as I had Corona for two times. Yeah, I only wanted to stay alive.”(V_36–49_GP)
“What forced me to be vaccinated was I was afraid of dying and being crippled. I was scared, [and] that’s why I was vaccinated.”(V_18-44_ZIM)
“I saw a person who was ill with COVID. He had difficulty in breathing, and you could feel pity for him. So it made me realize that getting vaccinated is the best and that’s what pushed me to get vaccinated.”(V_18–44_ZIM)
“I vaccinated because I survived two times from Corona. I had Corona, so I saw a need to vaccinate since they said there will be fourth wave maybe I will not survive this time. So, I decided to get vaccinated to help myself because I nearly died as I had Corona for two times, I only wanted to stay alive”- Participant 15, VIN_FGD_V_36-49 years_11-MAR-2022 GP.
4. Discussion
4.1. Confidence as a Barrier and Motivator
4.2. Convenience as a Barrier and Motivator
4.3. Complacency as a Barrier and Motivator
5. Limitations
6. Conclusion
Authors Contributions
Conflict of interest
| 1 | In Brown, 2000, p 198: “any person of ‘mixed- blood’ including children as well as descendants from Black-White, Black-Asian, White-Asian, and Black-Colored unions” is an officially acceptable racial classification referred to as ‘Colored’. Multiracial ethnic communities in South Africa may have ancestry from more than one population inhabiting the region, including, Malaysian slave, other slave, European, African, or a combination [16]. |
| 2 | O levels are the Zimbabwean equivalent of grade 12 in South Africa. |
| 3 | Zumbani is an herbal tea and immune booster for the treatment or prophylaxis of various ailments, including influenza |
References
- Wang, C.; Wang, Z.; Wang, G.; Lau, J.Y.; Zhang, K.; Li, W. COVID-19 in early 2021: current status and looking forward. Signal Transduct Target Ther 2021, 6, 114. [Google Scholar] [CrossRef]
- World Health Organization. WHO Coronavirus (COVID-19) Dashboard. Available online: https://covid19.who.int (accessed on 16 January).
- World Health Organization. WHO Coronavirus (COVID-19) South Africa. Available online: https://covid19.who.int/region/afro/country/za (accessed on 16 January).
- World Health Organization. WHO Coronavirus (COVID-19) Zimbabwe. Available online: https://covid19.who.int/region/afro/country/zw (accessed on 16 January).
- Dzinamarira, T.; Nachipo, B.; Phiri, B.; Musuka, G. COVID-19 Vaccine Roll-Out in South Africa and Zimbabwe: Urgent Need to Address Community Preparedness, Fears and Hesitancy. Vaccines (Basel) 2021, 9. [Google Scholar] [CrossRef]
- Makadzange, A.T.; Gundidza, P.; Lau, C.; Dietrich, J.; Beta, N.; Myburgh, N.; Elose, N.; Ndhlovu, C.; James, W.; Stanberry, L. Attitudes to Vaccine Mandates among Late Adopters of COVID-19 Vaccines in Zimbabwe. Vaccines (Basel) 2022, 10. [Google Scholar] [CrossRef]
- Larson, H.J.; Jarrett, C.; Eckersberger, E.; Smith, D.M.; Paterson, P. Understanding vaccine hesitancy around vaccines and vaccination from a global perspective: a systematic review of published literature, 2007-2012. Vaccine 2014, 32, 2150–2159. [Google Scholar] [CrossRef]
- National Department of Health. Coronavirus COVID-19 Alert Level 1. Available online: https://www.gov.za/covid-19/about/coronavirus-covid-19-alert-level-1 (accessed on 28 September).
- COVID-19 Law Lab. Statutory Instrument; SI 2022-067 Public Health (COVID-19 Prevention, Containment and Treatment) (National Lockdown) (No. 2) (Amendment) Order, 2022 (No. 41); 2022.
- Department of Health Republic of South Africa. South Africa COVID-19 and vaccine social listening report 30 May 2022, report 51; 2022.
- Burger, R.; Köhler, T.; Golos, A.M.; Buttenheim, A.M.; English, R.; Tameris, M.; Maughan-Brown, B. Longitudinal changes in COVID-19 vaccination intent among South African adults: evidence from the NIDS-CRAM panel survey, February to May 2021. BMC Public Health 2022, 22, 422. [Google Scholar] [CrossRef] [PubMed]
- Campbell, S.; Greenwood, M.; Prior, S.; Shearer, T.; Walkem, K.; Young, S.; Bywaters, D.; Walker, K. Purposive sampling: complex or simple? Research case examples. Journal of research in Nursing 2020, 25, 652–661. [Google Scholar] [CrossRef] [PubMed]
- Penrod, J.; Preston, D.B.; Cain, R.E.; Starks, M.T. A discussion of chain referral as a method of sampling hard-to-reach populations. Journal of Transcultural nursing 2003, 14, 100–107. [Google Scholar] [CrossRef] [PubMed]
- Schurink, E. Designing qualitative research. In Research at Grass Roots: A Primer for the Caring Professions, de Vos, A., Ed.; van Schaik: Pretoria, South Africa, 1998; pp. 252–276. [Google Scholar]
- Srivastava, A.; Thomson, S.B. Framework analysis: a qualitative methodology for applied policy research. Administration and Governance 2009, 4, 72–79. [Google Scholar]
- Adhikari, M. 'God made the white man, God made the black man...': Popular racial stereotyping of Coloured people in apartheid South Africa. South African Historical Journal 2006, 55, 142–164. [Google Scholar] [CrossRef]
- Barrall, A.L.; Hoff, N.A.; Nkamba, D.M.; Musene, K.; Ida, N.; Bratcher, A.; Dzogang, C.; Tangney, S.; Beia, M.; Nzaji, M.K.; et al. Hesitancy to receive the novel coronavirus vaccine and potential influences on vaccination among a cohort of healthcare workers in the Democratic Republic of the Congo. Vaccine 2022, 40, 4998–5009. [Google Scholar] [CrossRef]
- Pugliese-Garcia, M.; Heyerdahl, L.W.; Mwamba, C.; Nkwemu, S.; Chilengi, R.; Demolis, R.; Guillermet, E.; Sharma, A. Factors influencing vaccine acceptance and hesitancy in three informal settlements in Lusaka, Zambia. Vaccine 2018, 36, 5617–5624. [Google Scholar] [CrossRef]
- Magadmi, R.M.; Kamel, F.O. Beliefs and barriers associated with COVID-19 vaccination among the general population in Saudi Arabia. BMC Public Health 2021, 21, 1–8. [Google Scholar] [CrossRef]
- Cascini, F.; Pantovic, A.; Al-Ajlouni, Y.; Failla, G.; Ricciardi, W. Attitudes, acceptance and hesitancy among the general population worldwide to receive the COVID-19 vaccines and their contributing factors: A systematic review. EClinicalMedicine 2021, 40, 101113. [Google Scholar] [CrossRef]
- Gerretsen, P.; Kim, J.; Caravaggio, F.; Quilty, L.; Sanches, M.; Wells, S.; Brown, E.E.; Agic, B.; Pollock, B.G.; Graff-Guerrero, A. Individual determinants of COVID-19 vaccine hesitancy. PLoS One 2021, 16, e0258462. [Google Scholar] [CrossRef] [PubMed]
- Crawshaw, J.; Konnyu, K.; Castillo, G.; van Allen, Z.; Grimshaw, J.M.; Presseau, J. Behavioural determinants of COVID-19 vaccination acceptance among healthcare workers: a rapid review. Public Health 2022, 210, 123–133. [Google Scholar] [CrossRef] [PubMed]
- Sherman, S.M.; Smith, L.E.; Sim, J.; Amlôt, R.; Cutts, M.; Dasch, H.; Rubin, G.J.; Sevdalis, N. COVID-19 vaccination intention in the UK: results from the COVID-19 vaccination acceptability study (CoVAccS), a nationally representative cross-sectional survey. Hum Vaccin Immunother 2021, 17, 1612–1621. [Google Scholar] [CrossRef]
- Usher, K.; Bhullar, N.; Durkin, J.; Gyamfi, N.; Jackson, D. Family violence and COVID-19: Increased vulnerability and reduced options for support. Int J Ment Health Nurs 2020, 29, 549–552. [Google Scholar] [CrossRef] [PubMed]
- Wynen, J.; Op de Beeck, S.; Verhoest, K.; Glavina, M.; Six, F.; Van Damme, P.; Beutels, P.; Hendrickx, G.; Pepermans, K. Taking a COVID-19 Vaccine or Not? Do Trust in Government and Trust in Experts Help Us to Understand Vaccination Intention? Administration & Society 2022, 54, 1875–1901. [Google Scholar] [CrossRef]
- Mokgobi, M.G. Understanding traditional African healing. Afr J Phys Health Educ Recreat Dance 2014, 20, 24–34. [Google Scholar]
- Krah, E.; de Kruijf, J.; Ragno, L. Integrating Traditional Healers into the Health Care System: Challenges and Opportunities in Rural Northern Ghana. J Community Health 2018, 43, 157–163. [Google Scholar] [CrossRef]
- Audet, C.M.; Clemens, E.M.; Ngobeni, S.; Mkansi, M.; Sack, D.E.; Wagner, R.G. Throwing the bones to diagnose HIV: Views of rural South African traditional healers on undertaking HIV counselling and testing. AIDS Care 2021, 33, 1316–1320. [Google Scholar] [CrossRef]
- Kwedi Nolna, S.; Ntonè, R.; Fouda Mbarga, N.; Mbainda, S.; Mutangala, W.; Boua, B.; Niba, M.; Okoko, A. Integration of Traditional Healers in Human African Trypanosomiasis Case Finding in Central Africa: A Quasi-Experimental Study. Trop Med Infect Dis 2020, 5. [Google Scholar] [CrossRef] [PubMed]
- Lessard, D.; Ortiz-Paredes, D.; Park, H.; Varsaneux, O.; Worthington, J.; Basta, N.E.; MacDonald, S.E.; Lebouché, B.; Cox, J.; Ismail, S.J.; et al. Barriers and facilitators to COVID-19 vaccine acceptability among people incarcerated in Canadian federal prisons: A qualitative study. Vaccine: X 2022, 10, 100150. [Google Scholar] [CrossRef] [PubMed]
- Klassen, A.C.; Milliron, B.-J.; Reynolds, L.; Bakhtibekova, Z.; Mamadraimov, S.; Bahruddinov, M.; Shokamolova, S.; Shuster, M.; Mukhtar, S.; Gafurova, M.; et al. Formative research to address vaccine hesitancy in Tajikistan. Vaccine 2021, 39, 1516–1527. [Google Scholar] [CrossRef] [PubMed]
| Age (years) |
South Africa n (%) |
Zimbabwe n (%) |
Total n (%) |
|---|---|---|---|
| 18–19 20–29 30–39 40–49 50–59 60+ |
– 22 (27.2) 18 (22.2) 13 (16.0) 22 (27.2) 6 (7.4) |
6 (12.5) 8 (16.7) 10 (20.8) 17 (35.4) 3 (6.3) 4 (8.3) |
6 (4.7) 30 (23.2) 28 (21.7) 30 (23.2) 25 (19.4) 10 (7.8) |
| South Africa (n = 81) |
Zimbabwe (n = 48) |
Total (n = 129) |
|
|---|---|---|---|
|
Gender Female Male |
56 (69.1%) 25 (30.9%) |
29 (60.4%) 19 (39.6%) |
85 (65.9) 44 (34.1) |
| Median age (IQR): | 40 (23) | 39.5 (19) | 40 (22) |
|
Race Black Colored |
65 (80.2) 16 (19.8) |
48 (100) |
113 (87.6) 16 (12.4) |
|
HIV status Negative Positive |
**Not assessed |
40 (83.3) 8 (16.7) |
N/A |
|
Education Primary Secondary O level A level Post matric diploma Bachelor’s degree |
9 (11.1) 61 (75.3) – – 9 (11.1) 2 (2.5) |
3 (6.2) 9 (18.8) 32 (66.7) 3 (6.2) 1 (2.1) – |
12 (9.3) 70 (54.3) 32 (24.8) 3 (2.3) 9 (7) 3 (2.3) |
|
Employment Unemployed Self-employed Employed part time Volunteer work Employed full time Pensioner |
63 (77.8) 2 (2.5) 3 (3.7) 7 (8.6) 6 (7.4) – |
14 (29.2) 22 (45.8) 2 (4.2) 1 (2.1) 8 (16.6) 1 (2.1) |
77 (59.7) 24 (18.6) 5 (3.9) 8 (6.2) 14 (10.9) 1 (0.7) |
|
Vaccination status Unvaccinated Vaccinated |
37 (45.7) 44 (54.3) |
24 (50) 24 (50) |
61 (49.3) 68 (52.7) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2023 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




