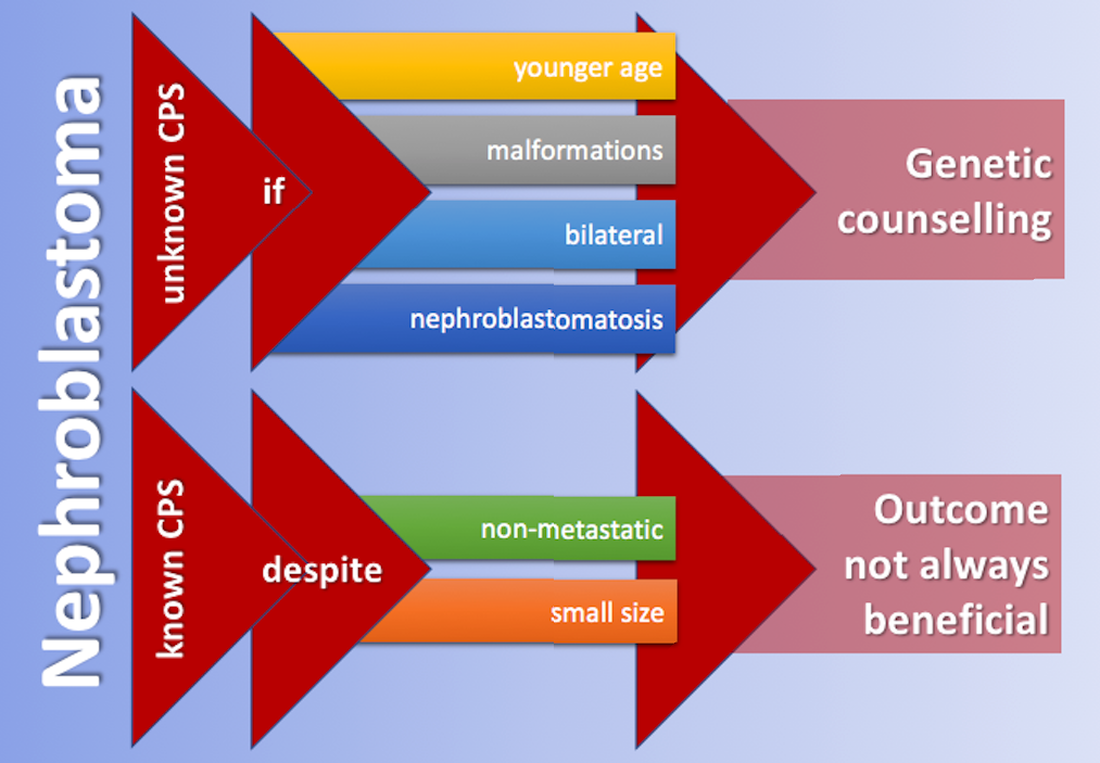
Background: About 10% of Wilms Tumor (WT) patients have a malformation or cancer predisposition syndrome (CPS) with causative germline genetic or epigenetic variants. Knowledge on CPS is essential for genetic counselling. Methods: This retrospective analysis focused on 2927 consecutive patients with WTs registered between 1989 and 2017 in the SIOP/GPOH studies. Results: (GU, N=66, 2,3%), Beckwith-Wiedemann spectrum (BWS, N=32, 1,1%), isolated hemihypertrophy (IHH, N=29, 1,0%), Denys-Drash syndrome (DDS, N=24, 0,8%) and WAGR syndrome (N=20, 0,7%) were reported most frequently. Compared to others, these patients were younger at WT diagnosis (median age 24,5 months vs. 39,0 months), had smaller tumors (334,8mL vs. 496,9mL), less often metastasis (8,2% vs. 18%), but more often nephroblastomatosis (12,9% vs. 1,9%). WT with IHH was associated with blastemal WT and DDS with stromal subtype. Bilateral WTs were common in WAGR (30%), DDS (29%) and BWS (31%). Chemotherapy induced reduction in tumor volume was poor in DDS (7,7% increase) and favorable in BWS (84,6% reduction). The event-free survival (EFS) of patients with BWS was significantly (p=0,002) worse than in others. Conclusions: CPS should be considered in WTs with specific clinical features resulting in referral to a geneticist. Their outcome was not always favorable.