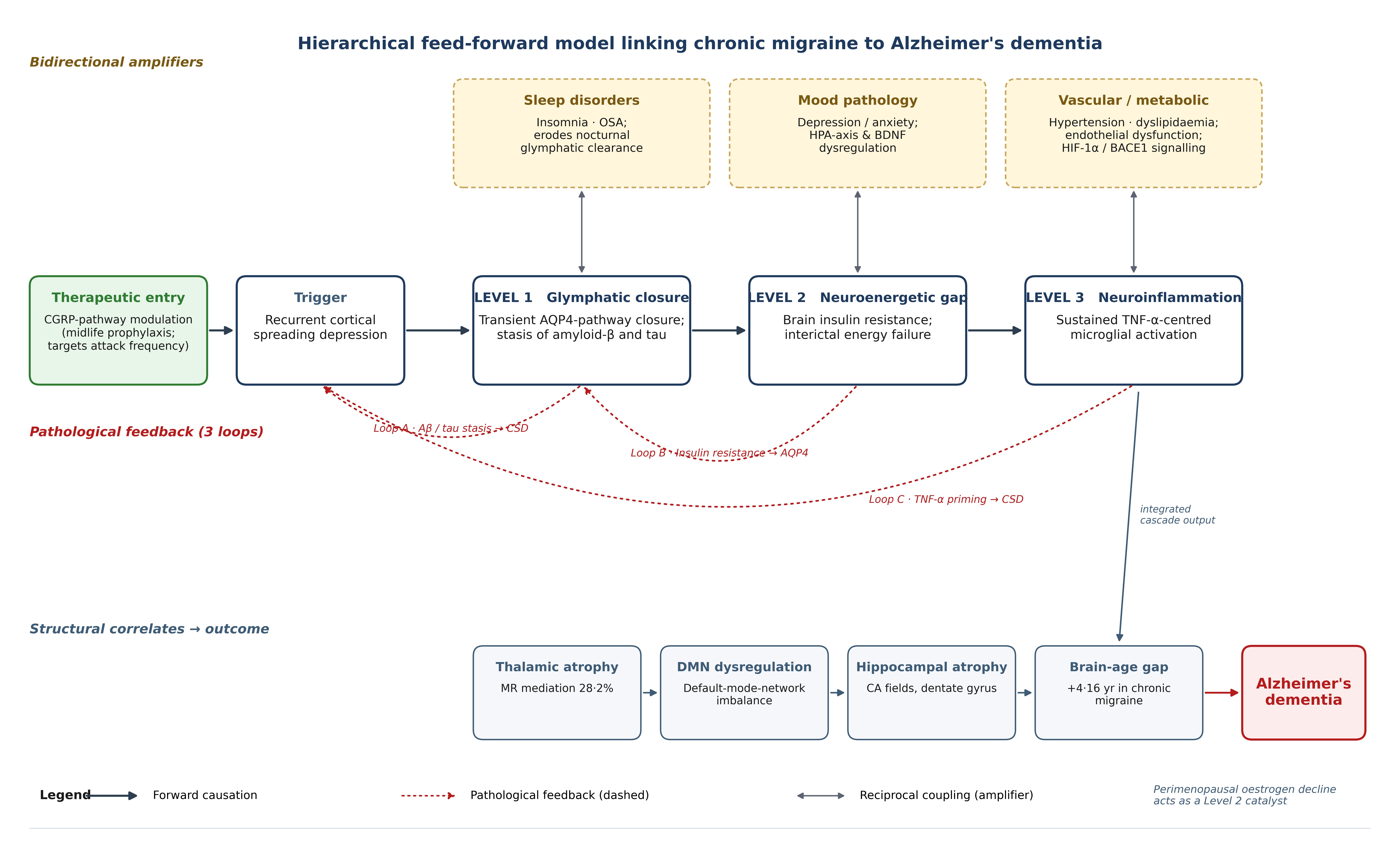
Chronic migraine has traditionally been framed as a disabling but self-limited pain disorder. Recent large-scale epidemiology, Mendelian randomisation, and neuroimaging converge on a different reading: midlife chronic migraine, particularly with aura, precedes and predicts Alzheimer's dementia in a manner consistent with a causal direction rather than mere association. We propose a hierarchical model in which recurrent cortical spreading depression initiates a feed-forward network: transient glymphatic closure with stasis of amyloid-β and tau; brain insulin resistance and interictal energy failure; and sustained, TNF-α-centred neuroinflammation, with each level feeding back to lower the threshold for the others. Sleep, mood, and vascular comorbidities are repositioned as bidirectional amplifiers rather than independent confounders. We outline falsifiable predictions, discuss the ambiguous neurocognitive profile of CGRP-pathway blockade, and argue that midlife migraine prevention warrants evaluation as a candidate disease-modifying strategy for Alzheimer's dementia.