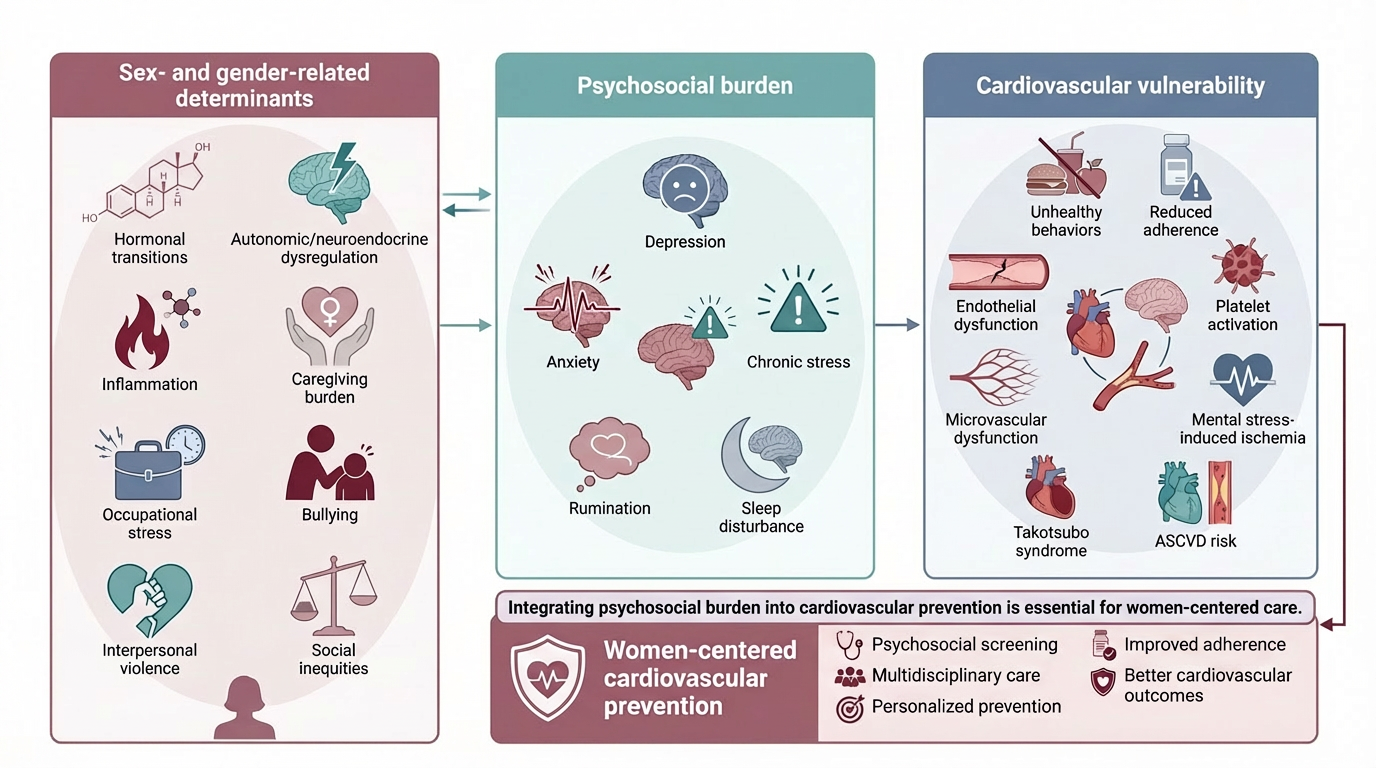
Cardiovascular disease is the leading cause of death in women, yet prevention and management have historically relied on male-centered models. Sex and gender critically influence risk, clinical presentation, and outcomes. Depression, anxiety, and psychosocial stress, more prevalent in women, act as key amplifiers of cardiovascular risk. We conducted a clinically oriented narrative review based on a broad, non-systematic search of major databases, integrating evidence selected for relevance and methodological robustness to clarify biological and psychosocial mechanisms linking mental health and cardiovascular disease in women. Affective disorders and stress contribute to cardiovascular risk through interconnected pathways, including hormonal fluctuations, autonomic and neuroendocrine dysregulation, inflammation, endothelial dysfunction, and heightened platelet reactivity. These mechanisms interact with gender-related exposures such as caregiving burden, occupational stress, and interpersonal violence. Stress-related phenotypes, including mental stress, induced ischemia and takotsubo syndrome, exemplify the heart-brain axis and its clinical implications. Incorporating mental health into cardiovascular risk assessment is essential for precision prevention in women. A women-centered approach should include systematic psychosocial evaluation, multidisciplinary care, and tailored strategies to improve risk control, adherence, and outcomes.