Submitted:
28 April 2026
Posted:
29 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Preoperative Evaluation
2.2. Statistical Analysis
3. Results
| Odds Ratio | 95% CI | P | |
| Age | 1.07 | (1.031 to 1.11) | 0.0005 |
| Time to surgery | 1.03 | (1.01 to 1.07) | 0.0423 |
| BADL >4 | 0.85 | (0.74 to 0.98) | 0.0286 |
| Anemia<10 g/dl Hb | 3.41 | (1.82 to 6.37) | 0.0001 |
| Cancer | 1.95 | (1.18 to 3.21) | 0.0084 |
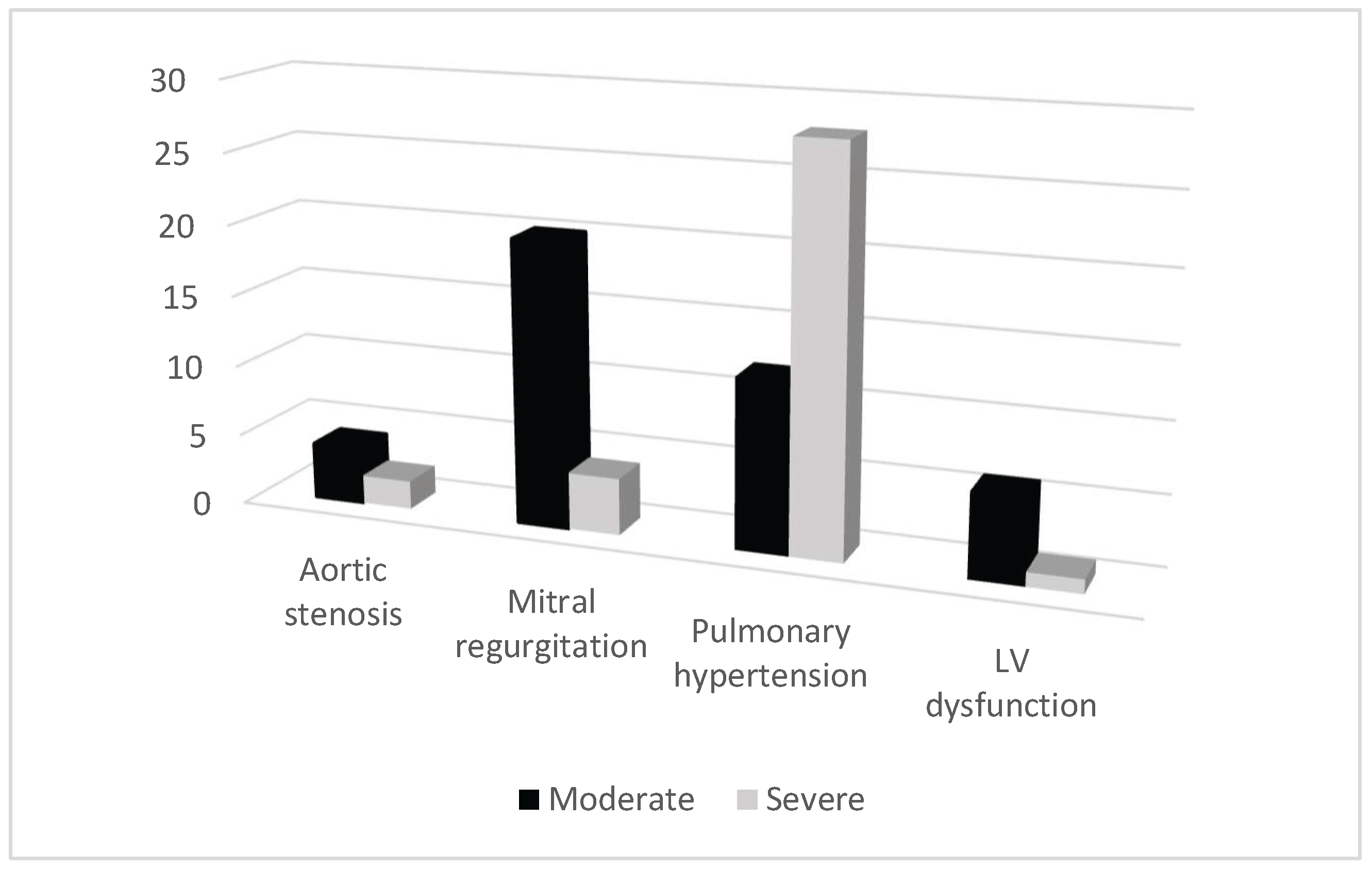
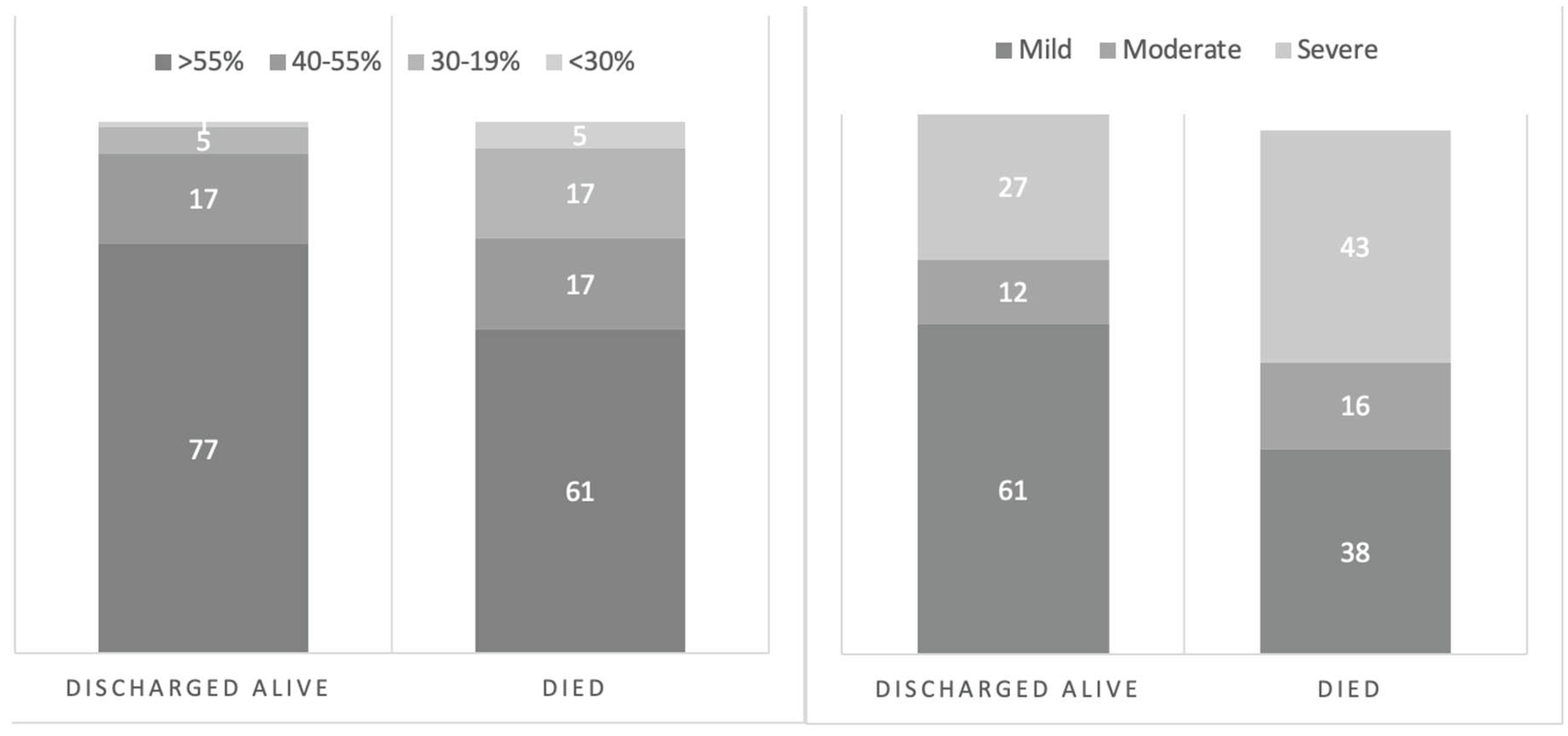
| Left Ventricular ejection fraction | 1.45 | (1.07 to 1.99) | 0.0189 |
| Pulmonary hypertension | 1.22 | (1.02 to 1.47) | 0.0257 |
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Smilowitz NR, Berger JS. Perioperative Cardiovascular Risk Assessment and Management for Noncardiac Surgery: A Review. JAMA. 2020 Jul 21;324(3):279-290. [CrossRef]
- Wijeysundera DN, Beattie WS, Karkouti K, Neuman MD, Austin PC, Laupacis A. Association of echocardiography before major elective non-cardiac surgery with postoperative survival and length of hospital stay: population based cohort study. BMJ. 2011 Jun 30;342:d3695. [CrossRef]
- Chang HY, Chang WT, Liu YW. Application of transthoracic echocardiography in patients receiving intermediate- or high-risk noncardiac surgery. PLoS One. 2019 Apr 25;14(4):e0215854. [CrossRef] [PubMed]
- Chao TC, Lee HP, Wu JC, Hsu CJ. Analysis of Cardiac Events and the Subsequent Impact for Geriatric Patients Undergoing Hip Fracture Surgeries. J Clin Med. 2023 Aug 14;12(16):5276. [CrossRef]
- Halvorsen S, Mehilli J, Cassese S, Hall TS, Abdelhamid M, Barbato E, et al. 2022 ESC Guidelines on cardiovascular assessment and management of patients undergoing non-cardiac surgery. Eur Heart J. 2022;14:3826– 3924. [CrossRef]
- Thompson A, Fleischmann KE, Smilowitz NR, de Las Fuentes L, Mukherjee D, Aggarwal NR, Ahmad FS, Allen RB, Altin SE, Auerbach A, Berger JS, Chow B, Dakik HA, Eisenstein EL, Gerhard-Herman M, Ghadimi K, Kachulis B, Leclerc J, Lee CS, Macaulay TE, Mates G, Merli GJ, Parwani P, Poole JE, Rich MW, Ruetzler K, Stain SC, Sweitzer B, Talbot AW, Vallabhajosyula S, Whittle J, Williams KA Sr; Peer Review Committee Members. 2024 AHA/ACC/ACS/ASNC/HRS/SCA/SCCT/SCMR/SVM Guideline for Perioperative Cardiovascular Management for Noncardiac Surgery: A Report of the American College of Cardiology/American Heart Association Joint Committee on Clinical Practice Guidelines. Circulation. 2024 Nov 5;150(19):e351-e442. https://doi.org/10.1161/CIR.0000000000001285. Epub 2024 Sep 24. [CrossRef]
- Scottish Intercollegiate Guidelines Network Management of hipfracture in older people. National Clinical Guideline111. 2009. http://www.sign.ac.uk/pdf/ sign111.pdf.
- Pincus D, Ravi B, Wasserstein D, Huang A, Paterson JM, Nathens AB, Kreder HJ, Jenkinson RJ, Wodchis WP. Association Between Wait Time and 30-Day Mortality in Adults Undergoing Hip Fracture Surgery. JAMA. 2017 Nov 28;318(20):1994-2003. [CrossRef]
- Mazarello Paes V, Ting A, Paes MVI, Masters J, Graham SM, Costa ML; HIPCARE Investigators*. What is the association between time to surgery and patient outcome after hip fracture? : a systematic review. Bone Joint J. 2026 Jan 1;108-B(1):30-38. [CrossRef]
- Hawley S, Javad MK, Prieto-Alhambra D, Lippet J , Sheard S, Arden NK, Cooper C, Judge A . The Refresch study group , Clinical effectiveness of orhtogeriatric and fracture liason service models of care for hip fracture patients : population-based longitudinal study . Age an Ageing 2016:45:236-2.
- Morris AH, Zuckerman JD. National consensus conference on improving the continuum of care for patients with hip fracture. J Bone Joint Surg Am 2002;84-A:670–674.
- Alibhai M, Sharma A, Alibhai MK, Fawdington RA, Moreau AP. Does pre-operative echocardiography delay hip fracture surgery Indian J Anaesth. 2013 Jul;57(4):408-10.
- Loxdale SJ, Sneyd JR, Donovan A, Werrett G, Viira DJ. The role of routine pre-operative bedside echocardiography in detecting aortic stenosis in patients with a hip fracture. Anaesthesia. 2012;67:51-54. [CrossRef]
- Moran CG, Wenn RT, Sikand M, Taylor AM. Early mortality after hip fracture: is delay before surgery important? J Bone Joint Surg Am 2005 Mar;87(3):483e9.
- Canty DJ, Royse CF, Kilpatrick D, Bowman L, Royse AG. The impact of focused transthoracic echocardiography in the pre-operativeclinic. Anaesthesia. 2012;67(6):618-25. [CrossRef]
- Yonekura H, Ide K, Onishi Y, Nahara I, Takeda C, Kawakami K. Preoperative Echocardiography for Patients With Hip Fractures Undergoing Surgery: A Retrospective Cohort Study Using a Nationwide Database. Anesth Analg. 2019 Feb;128(2):213-220. [CrossRef]
- AbuSharar SP, Bess L, Hennrikus E. Pre-operative echocardiograms in acute fragility hip fractures: How effective are the guidelines? Medicine (Baltimore). 2021 Mar 26;100(12):e25151. [CrossRef]
- Douglas PS, Khandheria B, Stainback RF, et al. ACCF/ASE/ACEP/ASNC/SCAI/SCCT/SCMR 2007 appropriateness criteria for transthoracic and transesophageal echocardiography: a report of the American College of Cardiology Foundation Quality Strategic Directions Committee Appropriateness Criteria Working Group, American Society of Echocardiography, American College of Emergency Physicians, American Society of Nuclear Cardiology, Society for Cardiovascular Angiography and Interventions, Society of Cardiovascular Computed Tomography, and the Society for Cardiovascular Magnetic Resonance. Endorsed by the American College of Chest Physicians and the Society of Critical Care Medicine. J Am Soc Echocardiogr 2007;20:787–805Chen X, Ma Y, Deng Z, Li Q, Liao J, Zheng Q. Prediction of Early Postoperative Major Cardiac Events and In-Hospital Mortality in Elderly Hip Fracture Patients: The Role of Different Types of Preoperative Cardiac Abnormalities on Echocardiography Report. Clin Interv Aging. 2020 May 27;15:755-762. [CrossRef]
- Chang HY, Chang WT, Liu YW. Application of transthoracic echocardiography in patients receiving intermediate- or high-risk noncardiac surgery. PLoS One. 2019 Apr 25;14(4):e0215854. [CrossRef]
- Lu LY, Rowe K, Johnson M, Desai V, Varady NH, Lange JK, Chen AF. How do preoperative echocardiograms in geriatric hip fracture patients affect care? A matched cohort study. Arch Orthop Trauma Surg. 2025 Jun 14;145(1):344. [CrossRef]
- Cid-Serra X, Royse A, Bowyer A, Canty D, Sessler D, Clarke-Errey S, Denault A, LoGiudice D, Ludbrook G, Lin DY, Yang Y, Haji K, Zucherrelli L, Palmer AJ, Piper B, Lwin TN, Dieleman S, Eccleston D, Chuan A, Cooper R, Henderson G, Royse C. Preoperative focused echocardiography on patients with fractured neck of femur. ECHONOF-III trial: study protocol for a multicenter randomized controlled trial. Trials. 2025 Sep 1;26(1):333. [CrossRef]
| Total | 2274 | COMORBIDITIES | |
| Gender (N°, % female ) | 1637(71%) | Atrial fibrillation | 526 (23.1%) |
| Age (mean) | 83.8+8.7 | COPD | 208 (9.1%) |
| TYPE OF FRACTURE | Diabetes | 405 (17.8%) | |
| Neck Femur | 1106 (48%) | Neoplasms | 467 (20.5%) |
| Pertrochanteric | 1033 (46%) | Heart failure | 184 (8.1%) |
| Subtrochanteric | 135 (6%) | Dementia | 476 (20.9%) |
| TIPO DI INTERVENTO | CAD | 361 (15.9%) | |
| Intramedullary nail | 1113 (49%) | Peripheral arteriopathy | 545 (23.9%) |
| Cephalic prosthesis | 568 (24%) | Hypertension | 1464 (64.3%) |
| Total prosthesis | 338 (15%) | Renal failure –(creat clearance <25 ml/min/1.73m2) | 305 (13.4%) |
| Screws | 228 (1146%) | Transfusion | 1125 (49.4%) |
| No surgery | 24 (1%) | Anemia | 152 (6.7%) |
| TIME TO SURGERY | Comorbidites ≥ 2 | 1419 (62.4%) | |
| < 48h | 1649 (76.5%) | PRESERVED BADL | |
| < 4 | 575 (28.2%) |
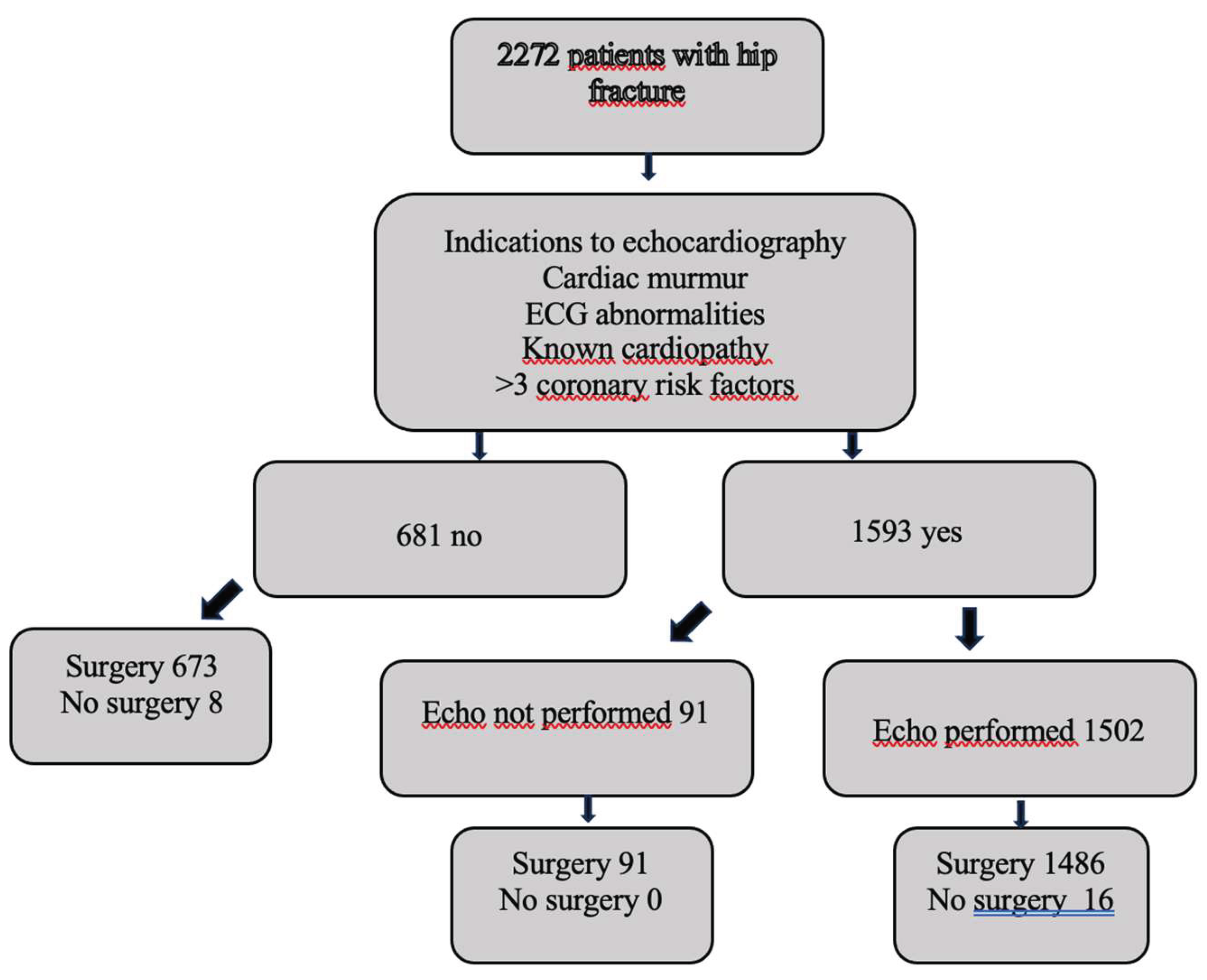
| No echo = 681 |
No echo with indication = 91 |
Echo = 1502 | p | |
| M F |
170 (25%) 511 (75%) |
38 (40%) 53 (60%) |
431 (28.7%) 1071 (71.3%) |
0.02 |
| Mean age (years) | 80.4 ± 11.2 | 84+ 8 | 85.4 ± 7.9 | <0.0001 |
| Type of fracture Neck Perthrocanteric Subthrocanteric |
360 (52.7%) 291 (43.3%) 30 (4.1%) |
44 44 3 |
702(46,8%) 695 (46,4%) 102 (6.8%) |
=0.01 |
| TIME TO SURGERY (days) | 2.1 ± 2.3 | 2.9 +3.7 | 2.7 ± 4.1 | <0.001 |
| SURGERY < 48H (%) | 80% | 75% | 74% | <0.0001 |
| PRESERVED BADL < 4 | 171 (22.8%) | 14 (15%) | 411 (31.1%) | <0.001 |
| Anemia <10g/dHb | 113 (14%) | 8 (9%) | 31 (4,1%) | ns |
| Type of surgery No surgery |
8 (1%) | 0 (0%) | 16 (1%) | 0.05 |
| Intramedullary nail | 320 (46%) | 50 (54%) | 743 (49%) | |
| Cephalic prosthesis | 132 (19%) | 17 (19%) | 422 (28%) | |
| Total prosthesis | 130 (19%) | 18 (20%) | 190 (13%) | |
| Screws | 91 (1549%) | 6 (7%) | 131 (9%) |
| COMORBIDITY | NO ECHO n 681 |
NO ECHO with indications n 91 |
ECHO n 1502 |
P |
| ATRIAL FIBRILLATION | 0 | 57 (62%) | 469 (31%) | <0.0001 |
| COPD | 25 (4%) | 11 (12%) | 167 (11%) | <0.0001 |
| DIABETES | 99 (14%) | 17 (18%) | 299 (20%) | ns |
| CANCER | 113 (16%) | 27 (29%) | 327 (21%) | ns |
| HEART FAILURE | 0 | 27 (29%) | 169 (11%) | <0.0001 |
| DEMENTIA | 141 (20%) | 21(23%) | 320 (21%) | ns |
| CORONARY DISEASE | 0 | 28 (30%) | 337 (22%) | <0.0001 |
| PERIPHERAL ARTERY DIS. | 103 (15%) | 30 (33%) | 412 (27%) | <0.0001 |
| HYPERTENSION | 358 (52%) | 59 (64%) | 1045 (69%) | <0.0001 |
| ≥ 2 COMORBITIES | 263 (38%) | 70 (73%) | 1088 (72%) | <0.0001 |
| RENAL FAILURE | 43 (6%) | 13 (15%) | 263 (17%) | 0.002 |
| TRANSFUSION | 284(41%) | 42 (44%) | 811 (53%) | <0.0001 |
| NO ECHO (681) | NO ECHO with indications ( 91) |
ECHO (1502) |
|||||
| Discharged alive (666-98%) | Died (15-2%) |
Discharged alive (82-90%) | Died (9-10%) |
Discharged Alive (1392-92.7%) | Died (110-7.3%) |
P <0.0001 |
|
| Female Male |
500 (75%) 166 (25%) |
9(60%) 6 (40%) |
50 (60%) 32(40%) |
5 (58%) 4 (42%) |
1006 (72%) 386 (28%) |
65 (59,1%) 45(40,9%)§ |
<0.0001 |
| Mean age | 79.8±11,4 | 86.1±6.8,1° | 81.3+7.5 | 87.2+7* | 85.4±7,9 | 88.9±6,4* | 0.005 |
| Time to surgery (gg) | 2.1±2.3 | .3.1±6.8 | 2.5+2.0 | 9.3+13 | 2.6±4.1 | 4.0±10,§ | <0.001 |
| SURGERY < 24 h (%) | 80% | 61%* | 64% | 4.4% | 74% | 52%* | <0.0001 |
| PRESERVED BADL <4 | 94 (13%) | 9 (60%)* | 21 (25%) | 5 (55%) | 517 (37%) | 51 (58%)* | <0.0001 |
| Comorbidity | Discharged alive (666) | Died (15) | p |
| Anemia | 100 (15%) | 9 (41%) | <0.0001 |
| COPD | 24 (4%) | 3 (12%) | ns |
| Diabetes | 105 (17%) | 3 (12%) | ns |
| Cancer | 139 (20%) | 7 (29%) | ns |
| Dementia | 137 (20%) | 11 (45%) | 0.002 |
| Peripheral vascular dis | 141 (21%) | 7 (29%) | ns |
| Hypertension | 353 (53%) | 13 (54%) | ns |
| Comorbidities ≥ 2 | 256 (38%) | 14 (58%) | ns |
| Renal failure | 39 (6%) | 3 (12%) | ns |
| Transfusion | 277 (41%) | 12(50%) | ns |
| ECHO (1502) No ECHO with indication (91) | ||||||
| Comorbidity |
Discharged alive n 1392 |
Died n 110 |
Discharged alive n 82 |
Died n 9 |
p | |
| Atrial fibrillation | 423 (30%) | 46 (42%)* | 55 (60%) | 2 (22%)* | 0.0001 | |
| Anemia | 86 (6%) | 24 (21%)° | 4 (5%) | 5 (55%)# | 0.0001 | |
| COPD | 146 (10%) | 21 (19%)* | 7 (9%) | 2 (22%) | 0.02 | |
| Diabetes | 279 (20%) | 20 (18%) | 15 (18%) | 1 (11%) | ns | |
| Cancer | 292 (21%) | 35 (32%)* | 21 (25%) | 3 (33%) | 0.04 | |
| Heart failure | 147 (10%) | 22 (20%)# | 14 (17%) | 7 (77%)# | 0.0001 | |
| Dementia | 286 (20%) | 34 (30%)* | 13 (16%) | 4 (44%)* | 0.02 | |
| Coronary artery disease | 305 (22%) | 32 (29%) | 22 (26%) | 3 (33%) | ns | |
| Peripheral vascular dis | 375 (7%) | 37 (33%)* | 18 ( 21%) | 6(66%)# | 0.002 | |
| Hypertension | 977 (70%) | 68 (62%)* | 53 (64%) | 6 (66%) | 0.02 | |
| Comorbidities ≥ 2 | 992 (71%) | 96 (87%)° | 63 (76%) | 7 (77%) | 0.004 | |
| Renal failure | 225 (16%) | 38 (34%)° | 10 (12%) | 3 (33%) | 0.0001 | |
| Transfusion | 757 (54%) | 54 (49%) | 37 (45%) | 5 (55%) | ns | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




