Submitted:
21 April 2026
Posted:
22 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| CRP | C-Reactive Protein |
| US | Ultrasonography |
| MRI | Magnetic Resonance Imaging |
| CT | Computed Tomography |
| IL6 | Interleukin 6 |
| AUC | Area Under the Curve |
References
- Adnexal Torsion in Adolescents: ACOG Committee Opinion No, 783. Obstet Gynecol 2019, 134(2), e56–e63. [CrossRef] [PubMed]
- Rougier, E.; Mar, W.; Della Valle, V.; Morel, B.; Irtan, S.; Audureau, E.; Coulomb-L'Hermine, A.; Ducou Le Pointe, H.; Blondiaux, E. Added value of MRI for the diagnosis of adnexal torsion in children and adolescents after inconclusive ultrasound examination. Diagn Interv Imaging Epub. 2020, 101(11), 747–756. [Google Scholar] [CrossRef] [PubMed]
- Reed, J.L.; Strait, R.T.; Kachelmeyer, A.M.; Byczkowski, T.L.; Ho, M.L.; Huppert, J.S. Biomarkers to distinguish surgical etiologies in females with lower quadrant abdominal pain. Acad Emerg Med. 2011, 18(7), 686–91. [Google Scholar] [CrossRef] [PubMed]
- Kart, C.; Aran, T.; Guven, S.; Karahan, S.C.; Yulug, E. Acute increase in plasma D-dimer level in ovarian torsion: an experimental study. Hum Reprod. 2011, 26(3), 564–8. [Google Scholar] [CrossRef] [PubMed]
- Boscarelli, A.; Giangreco, M.; Valvo, E.; Codrich, D.; Masiello, V.; Iaquinto, M.; Scarpa, M.G.; Olenik, D.; Maita, S.; Campilongo, C.; Guida, E.; Schleef, J. The role of preoperative D-dimer levels in diagnosing adnexal torsion in children and adolescents: a prospective monocentric pilot analysis. Front Med (Lausanne) 2025, 12, 1706633. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Kives, S.; Gascon, S.; Dubuc, É; Van Eyk, N. No. 341-Diagnosis and Management of Adnexal Torsion in Children, Adolescents, and Adults. J Obstet Gynaecol Can. 2017, 39(2), 82–90. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Liu, M.; Zhang, M.; Yang, M.; Weng, Z.; Wu, Q.; He, S. Ultrasonographic scoring system for the diagnosis of adnexal torsion. J Clin Ultrasound 2022, 50(4), 525–531. [Google Scholar] [CrossRef] [PubMed]
- Nichols, D.H.; Julian, P.J. Torsion of the adnexa. Clin Obstet Gynecol 1985, 28(2), 375–80. [Google Scholar] [CrossRef] [PubMed]
- Ghandehari, H.; Kahn, D.; Tomlinson, G.; et al. Ovarian torsion: time limiting factors for ovarian salvage. Emerg Med Open Access 2015, 5, 5. [Google Scholar]
- Yuk, J.S.; Kim, L.Y.; Shin, J.Y.; Choi, D.Y.; Kim, T.Y.; Lee, J.H. A national population-based study of the incidence of adnexal torsion in the Republic of Korea. Int J Gynaecol Obstet 2015, 129(2), 169–70. [Google Scholar] [CrossRef] [PubMed]
- Moribata, Y.; Kido, A.; Yamaoka, T.; Mikami, Y.; Himoto, Y.; Kataoka, M.; Fujimoto, K.; Konishi, I.; Togashi, K. MR imaging findings of ovarian torsion correlate with pathological hemorrhagic infarction. J Obstet Gynaecol Res. 2015, 41(9), 1433–9. [Google Scholar] [CrossRef] [PubMed]
- Adeyemi-Fowode, O.; Lin, E.G.; Syed, F.; Sangi-Haghpeykar, H.; Zhu, H.; Dietrich, J.E. Adnexal Torsion in Children and Adolescents: A Retrospective Review of 245 Cases at a Single Institution. J Pediatr Adolesc Gynecol. 2019, 32(1), 64–69. [Google Scholar] [CrossRef] [PubMed]
- Bolli, P.; Schädelin, S.; Holland-Cunz, S.; Zimmermann, P. Ovarian torsion in children: Development of a predictive score. Medicine (Baltimore) 2017, 96(43), e8299. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Rousseau, V.; Massicot, R.; Darwish, A.A.; Sauvat, F.; Emond, S.; Thibaud, E.; Nihoul-Fékété, C. Emergency management and conservative surgery of ovarian torsion in children: a report of 40 cases. J Pediatr Adolesc Gynecol. 2008, 21(4), 201–6. [Google Scholar] [CrossRef] [PubMed]
- Ssi-Yan-Kai, G.; Rivain, A.L.; Trichot, C.; Morcelet, M.C.; Prevot, S.; Deffieux, X.; De Laveaucoupet, J. What every radiologist should know about adnexal torsion. Emerg Radiol 2018, 25(1), 51–59. [Google Scholar] [CrossRef] [PubMed]
- Minneci, P.C.; Mahida, J.B.; Lodwick, D.L.; Sulkowski, J.P.; Nacion, K.M.; Cooper, J.N.; Ambeba, E.J.; Moss, R.L.; Deans, K.J. Effectiveness of Patient Choice in Nonoperative vs Surgical Management of Pediatric Uncomplicated Acute Appendicitis. JAMA Surg 2016, 151(5), 408–15. [Google Scholar] [CrossRef] [PubMed]
- Schwartz, B.I.; Huppert, J.S.; Chen, C.; Huang, B.; Reed, J.L. Creation of a Composite Score to Predict Adnexal Torsion in Children and Adolescents. J Pediatr Adolesc Gynecol. 2018, 31(2), 132–137. [Google Scholar] [CrossRef] [PubMed]
- King, A.; Keswani, S.; Biesiada, J.; Breech, L.; Crombleholme, T.; Huppert, J. The utility of a composite index for the evaluation of ovarian torsion. Eur J Pediatr Surg. 2014, 24(2), 136–140. [Google Scholar] [CrossRef] [PubMed]
- Marcinkowski, K.; Saul, D.; Gould, S.; Berman, L.; Schwartz, B.I. Application of a Composite Score to Predict Adnexal Torsion in Premenarchal and Menarchal Children and Adolescents. J Pediatr Surg. 2024, 59(3), 509–514. [Google Scholar] [CrossRef] [PubMed]
| n | % | |
|---|---|---|
| Menstruation | ||
| N | 10 | 35.72 |
| Y | 18 | 64.28 |
| Symptoms | ||
| Abdominal Pain |
28 |
100.00 |
| Vomiting | 13 | 46.42 |
| Nausea | 4 | 14.28 |
| Fever | 4 | 14.28 |
| Abdominal mass | 3 | 10.71 |
| Ultrasonography | ||
| N | 0 | 0.00 |
| Y | 28 | 100.00 |
| Computed Tomography | ||
| N | 23 | 82.14 |
| Y | 5 | 17.86 |
| Magnetic Resonance Imaging | ||
| N | 26 | 92.86 |
| Y | 2 | 7.14 |
| Suspected Side | ||
| Left | 11 | 39.29 |
| Right | 17 | 60.71 |
| Surgical Approach | ||
| Laparoscopic | 24 | 85.71 |
| Laparoscopic converted | 2 | 7.14 |
| Open | 2 | 7.14 |
| Torsion confirmed | ||
| N | 11 | 39.29 |
| Y | 17 | 60.71 |
| Side of torsion verified | ||
| Left | 4 | 23.53 |
| Right | 13 | 76.47 |
| Post-operative complications | ||
| N | 28 | 100.00 |
| Y | 0 | 0.00 |
| Value | Torsion | Min | 25° percentile | Median | 75° percentile | Max | Wilcoxon Mann Whitney P-value |
|---|---|---|---|---|---|---|---|
| Age | N | 10 | 12 | 13 | 15 | 17 | 0.48 |
| Y | 4 | 12 | 13 | 14 | 16 | ||
| Weight | N | 43 | 53 | 55 | 65 | 70 | 0.31 |
| Y | 12 | 40 | 54 | 62 | 77 | ||
| WBC | N | 5.8 | 6 | 9.1 | 10.6 | 13.4 | 0.78 |
| Y | 6.1 | 7.6 | 8.8 | 10.9 | 15.9 | ||
| Neu | N | 46.4 | 55.6 | 64.7 | 79.1 | 84.1 | 0.84 |
| Y | 34.4 | 58.3 | 68.2 | 78.3 | 92.1 | ||
| CRP | N | 0.1 | 0.1 | 0.3 | 8.2 | 140.3 | 1.00 |
| Y | 0.1 | 0.1 | 0.5 | 1.8 | 98.7 | ||
| D-dimer | N | 189 | 234 | 327 | 395 | 1788 | 0.09 |
| Y | 189 | 499 | 520 | 877 | 9450 |
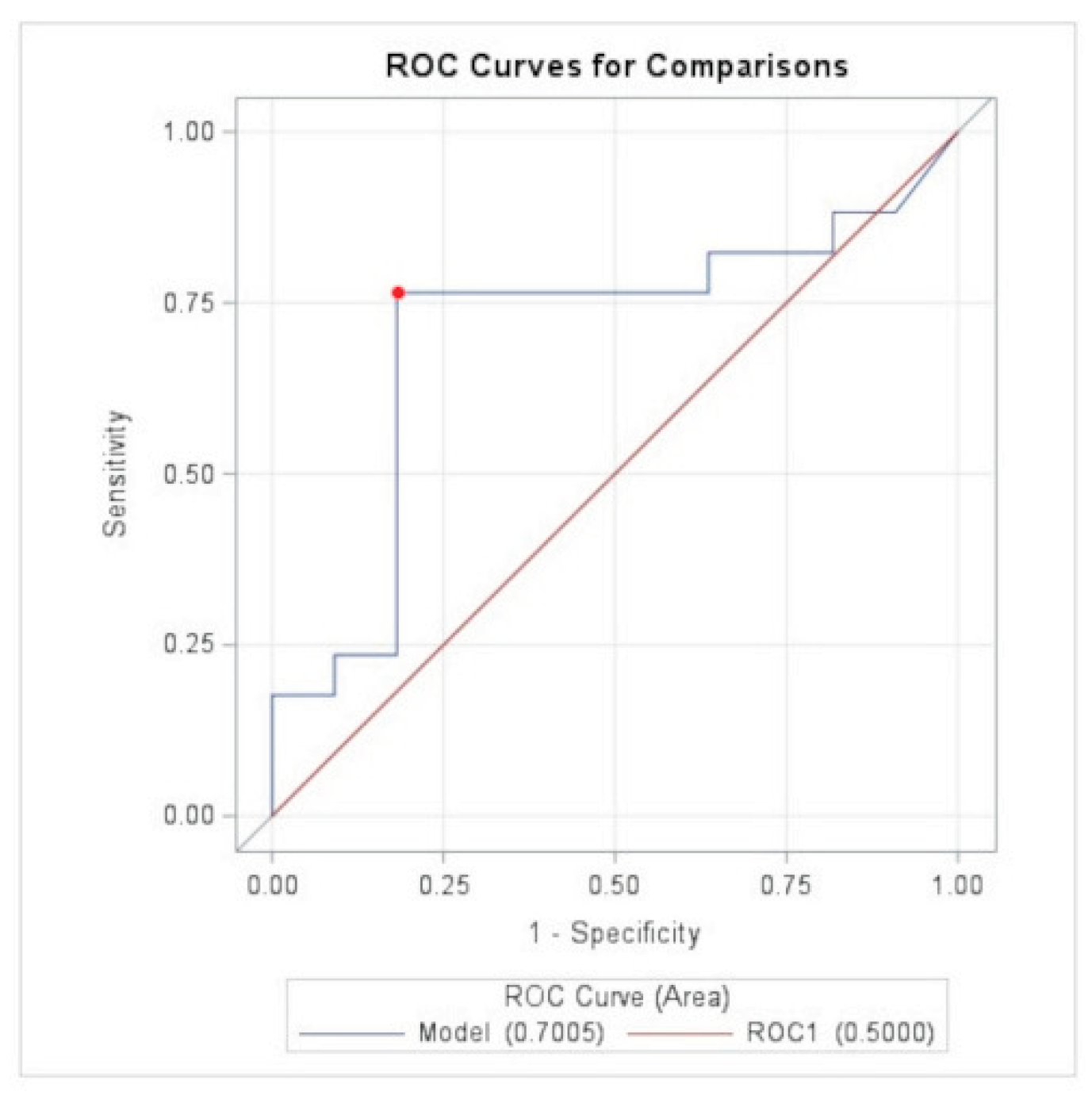
| D-dimer | Univariate model - Torsion | |||
|---|---|---|---|---|
| Odds Ratio | p-value | Sensitivity | Specificity | |
| 1.00 | 0.27 | 0,77 | 0,82 | |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




