Submitted:
16 April 2026
Posted:
17 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Literature Review
2.1. Discrimination as a Social Determinant of Health
2.2. Migration, Health, and Vulnerability
2.3. South African Policy and Legal Framework
2.4. Medical Xenophobia and Health
2.5. Synthesis and Research Gap
3. Theoretical Framework
3.1. Structural Violence and Health Inequities
3.2. Intersectionality and Migrant Status
3.3. Bureaucratic Discretion and Institutional Practices
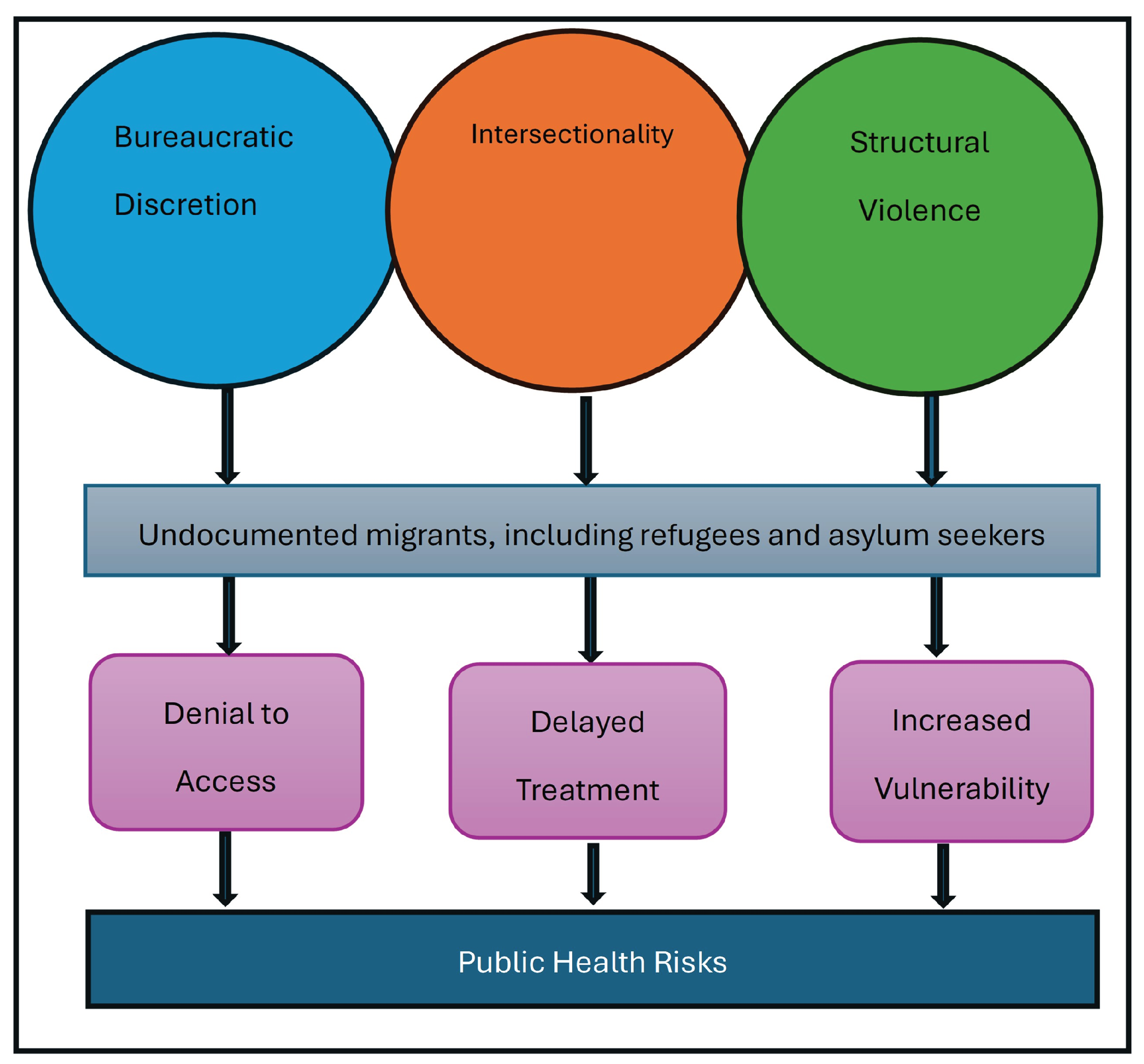
3.4. Integrative Framework
4. Research Methodology
4.1. Research Design
4.2. Data Sources and Sampling Strategy
4.3. Analytical Approach
4.4. Ethical Consideration
4.5. Limitation of Study
5. Results
5.1. Constitutional and Legislative Framework to Healthcare
5.2. Legal Documents and Access to Healthcare
5.3. Institutional Practices and Everyday Discrimination
5.4. Medical Xenophobia
6. Discussion
6.1. Discrimination as a Structural Determinant of Health
6.2. The Role of Institutions and Bureaucratic Discretion
6.3. Intersectionality and the Experience of Exclusion
6.4. Xenophobia, Belonging, and Health
6.5. Implications for Public Health and Health Systems
6.6. Key Contribution to Knowledge
7. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Modiselle, M. P. Opinions, perceptions and experiences of foreign nationals’ healthcare services access in Mamelodi, Pretoria. M.Phil dissertation, University of Stellenbosch, South Africa, 2021. Available online: https://www.healthmanagement.sun.ac.za/opinions-perceptions-and-experiences-of-foreign-nationals-healthcare-services-access-in-mamelodi-pretoria/#:~:text=The%20findings%20revealed%20that%2064,seeking%20experiences%20for%20foreign%20nationals.
- South African Human Rights Commission. Hate speech: Information Sheet. Available online: https://www.sahrc.org.za/home/21/files/Hate%20Speech%20Information%20Sheet-%20print%20ready-.pdf.
- Human Rights Watch. “They have robbed me of my life” – xenophobic violence against non-nationals in South Africa. Available online: https://www.hrw.org/report/2020/09/17/they-have-robbed-me-my-life/xenophobic-violence-against-non-nationals-south#:~:text=Attacks%20on%20the%20Streets,Africans%20to%20mean%20%E2%80%9Cforeigner.%E2%80%9D.
- Xenowatch. Xenophobic discrimination in South Africa: An overview of trends, effects and responses (2022-2025). Available online: https://www.hrw.org/report/2020/09/17/they-have-robbed-me-my-life/xenophobic-violence-against-non-nationals-south#:~:text=Attacks%20on%20the%20Streets,Africans%20to%20mean%20%E2%80%9Cforeigner.%E2%80%9D.
- Pineteh, E.A. Illegal aliens and demons that must be exorcised from South Africa: Framing African migrants and xenophobia in post-apartheid narratives. Cogent Social Sciences 2017, Vol. 3. Available online: https://www.tandfonline.com/doi/full/10.1080/23311886.2017.1391158#abstract. [CrossRef]
- World Health Organization. Closing the gap in a generation: Health equity through action on the social determinant of health, 2008. Available online: https://iris.who.int/server/api/core/bitstreams/cb08095c-55c8-484e-bff6-0e9c78fd38dd/content.
- Solar, O.; Irwin, A.A. A Conceptual framework for action on the social determinants of health; Social Determinants of Health Discussion Paper 2 (Policy and Practice): Geneva, WHO, 2010; Available online: https://iris.who.int/server/api/core/bitstreams/ca294183-3263-470f-a5fe-8e124ec48c72/content.
- Castañeda, H.; Holmes, S.M.; Madrigal, D.S.; Young, M.E.; Beyeler, N.; Quesada, J. Immigration as a social determinant of health. Annu Rev Public Health 2015, Vol.18(36), 375–392. [Google Scholar] [CrossRef] [PubMed]
- Voldby, K.G.; Hellstrom, L.C.; Berg, M.E.; Eplov, L.F. Structural discrimination against people with mental illness; a scoping review. SSM – Mental Health 2022, Vol. 2. [Google Scholar] [CrossRef]
- Abubakar, I.; Aldridge, R.W.; Devakumar, D.; Orcutt, M.; Burns, R.; Barreto, M.L.; Dhavan, P.; Fouad, F.M.; Groce, N.; Guo, Y.; Hargreaves, S.; Knipper, M.; Miranda, J.J.; Madise, N.; Kumar, B.; Mosca, D.; McGovern, T.; Rubenstein, L.; Sammonds, P.; Sawyer, S.M.; Sheikh, K.; Tollman, S.; Spiegel, P.; Zimmerman, C. The UCL-Lancet Commission on Migration and Health: the health of a world on the move. Lancet 2018, Vol. 15. [Google Scholar] [CrossRef]
- Asakitikpi, A.O. The quadruple vulnerability of African feminised migration into South Africa and their invisibility in the face of social and institutional violence. In Gender-Based Violence in Sub-Saharan Africa: Prevalence, Patterns, and Policies; Asakitikpi, A., Murhula, P., Eds.; Lexington Books: Maryland, USA, 2024; p. pp. [Google Scholar]
- Akokuwebe, M.E.; Osuafor, G.N.; Likoko, S.; Idemudia, E.S. Health services satisfaction and medical exclusion among migrant youths in Gauteng Province of South Africa: A cross-sectional analysis of the GCRO survey (2017-2018). PLoS One 2023, Vol. 29;18(11). Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC10686501/. [CrossRef]
- World Health Organization. Refugee and migrant health. 2026. Available online: https://www.who.int/news-room/fact-sheets/detail/refugee-and-migrant-health.
- Kisa, A.; Kisa, S. Structural racism as a fundamental cause of health inequities: a scoping review. Int J Equity Health 2025, 24. [Google Scholar] [CrossRef]
- Marmot, M. The health gap: the challenge of an unequal world. Lancet 2015, Vol. 12. [Google Scholar] [CrossRef]
- Hacker, K.; Anies, M.; Folb, B.; Zallman, L. Barriers to health care for undocumented immigrants: a literature review. Risk Management and Healthcare Policy 2015, 8, 175–183. Available online: https://www.dovepress.com/article/download/24396#:~:text=John%20L.,%E2%80%932):%205%E2%80%9314. [CrossRef]
- Asif, Z.; Kienzler, H. Structural barriers to refugee, asylum seeker and undocumented migrant healthcare access. Perceptions of Doctors of the World caseworkers in the UK. SSM-Mental Health. 2022, Vol. 2. Available online: https://www.sciencedirect.com/science/article/pii/S2666560322000287.
- International Federation of Red Cross and Red Crescent Society. New Walled Order: How barriers to basic services turn migration into a human crisis. Available online: https://www.ifrc.org/sites/default/files/Migration-policy-Report-Final-LR.pdf.
- Diaz-Millon, M.; Olvera-Lobo, M.D. Systematic meta-review on migrant healthcare access: Language barriers and the role of translation. Journal of Migration and Health 2025, Vol. 12. Available online: https://www.sciencedirect.com/science/article/pii/S266662352500056X. [CrossRef]
- Whitaker, K.L.; Krystallidou, D.; Williams, E.D.; Black, G.; Vindrola-Padros, C.; Braun, S.; Gill, P. Addressing language as a barrier to healthcare access and quality. Br J Gen Pract 2021, 31. Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC8714507/. [CrossRef]
- Crush, J.; Tawodzera, G. South-South Migration and Urban Food Security: Zimbabwean Migrants in South African Cities. Int Migr 2017, Vol. 55, 88–102. [Google Scholar] [CrossRef]
- Walker, R.; Vearey, J. “Closing the gap in the wrong direction” migration, health policy, and the exclusion of asylum seekers, refugees and undocumented migrants from healthcare access in South Africa. BMC Public Health. 2025, Vol. 10(25). Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC12604325/. [CrossRef]
- HIAS. Medical xenophobia in South Africa and around the world. Available online: https://hias.org/news/medical-xenophobia-south-africa-and-around-world/#:~:text=In%20South%20Africa%2C%20access%20to%20healthcare%20is,hospital%20entrances**%20*%20**Mis%2D%20and%20disinformation%20online**.
- Malatja, M. Health Xenophobia – The Lived Reality of Many Foreign Nationals. In ProBono.Org Newsletter; 2023. [Google Scholar]
- Vanyoro, K. The complex story of “medical xenophobia” in South Africa, 2019. Available online: https://www.wits.ac.za/news/latest-news/opinion/2019/2019-12/the-complex-story-of-medical-xenophobia-in-south-africa.html.
- Misago, J.P. Political Mobilisation as the Trigger of Xenophobic Violence in Post-Apartheid South Africa. International Journal of Conflict and Management 2019, Vol. 13. Available online: https://www.xenowatch.ac.za/wp-content/uploads/2019/08/Misago-J.P.-2019.-Political-Mobilisation-as-the-Trigger-of-Xenophobic-Violence-in-Post-Apartheid-South-Africa.-International-Journal-of-Conflict-and-Violence-IJCV-13-646..pdf.
- Mamabolo, M.A. Drivers of community xenophobic attacks in South Africa: poverty and unemployment. The Journal for Transdisciplinary Research in Southern Africa 2015, 11(4), 8. [Google Scholar] [CrossRef]
- Masikane, C.M.; Hewitt, M.L.; Toendepi, J. Dynamics informing xenophobia and leadership response in South Africa. Acta Commercii - Independent Research Journal in the Management Sciences 2020, 20(1). Available online: https://actacommercii.co.za/index.php/acta/article/view/704/1362. [CrossRef]
- Dube, G. Afrophobia in Mzansi? Evidence from the 2013 South African Social Attitudes Survey. Journal of Southern African Studies 2018, 44(6), 1005–1021. [Google Scholar] [CrossRef]
- UNISA. Afrophobia versus xenophobia in South Africa. Available online: https://www.unisa.ac.za/sites/corporate/default/News-&-Media/Articles/Afrophobia-versus-xenophobia-in-South-Africa#:~:text=According%20to%20Unisa%20theology%20professor%20Rothney%20Tshaka%2C,other%20from%20north%20of%20the%20Limpopo%20River.
- Galtung, J. Violence, Peace, and Peace Research. Journal of Peace Research 1969, Vol. 6(3), 167–191. [Google Scholar] [CrossRef]
- Farmer, P. The Anthropology of Structural Violence. Current Anthropology 2004, Vol.45(3), 305–325. Available online: https://www.jstor.org/stable/10.1086/382250?seq=1. [CrossRef]
- Macassa, G.; McGrath, C.; Rashid, M.; Soares, J. Structural Violence and Health-Related Outcomes in Europe: A Descriptive Systematic Review. Int J Environ Res Public Health 2021, Vol. 30(13). [Google Scholar] [CrossRef]
- Crenshaw, K. Demarginalizing the Intersection of Race and Sex: A Black Feminist Critique of Antidiscrimination Doctrine, Feminist Theory and Antiracist Politics, 1989, 1; Available online: https://chicagounbound.uchicago.edu/cgi/viewcontent.cgi?article=1052&context=uclf.
- Lipsky, M. Street Level Bureaucracy: Dilemmas of the Individual in Public Services; Russell Sage Foundation: New York, USA, 1980. [Google Scholar]
- Rahman, S.; Burns, P.; Wolfram Cox, J.; Alam, Q. Exercising bureaucratic discretion through selective bridging: A response to institutional complexity in Bangladesh. Public Administration and Development 2024, 44(2), 61–74. [Google Scholar] [CrossRef]
- Creswell, J.W.; Poth, C.N. Qualitative Inquiry and Research Design Choosing among Five Approaches. 4th Edition; SAGE Publications: California, USA, 2018. [Google Scholar]
- Braun, V.; Clarke, V. Using thematic analysis in psychology. Qualitative Research in Psychology 2006, 3(2), 77–101. [Google Scholar] [CrossRef]
- Centre for Child Law. Free healthcare services in South Africa: A case for all mothers and Children. Available online: https://section27.org.za/wp-content/uploads/2022/11/Free-Healthcare-Final-2.pdf.
- Government Gazette, Republic of South Africa. Available online: https://www.gov.za/sites/default/files/gcis_document/201409/a61-03.pdf.
- Spotlight. What the law actually says about migrants’ right to access healthcare in SA. Available online: https://www.spotlightnsp.co.za/2026/04/02/what-the-law-actually-says-about-migrants-right-to-access-healthcare-in-sa/#:~:text=The%20laws%20governing%20healthcare%20for,can%20never%20be%20completely%20denied.
- Chirau, T.J.; Shirinde, J.; McCrindle, C. Access to healthcare by undocumented Zimbabwean migrants in post-apartheid South Africa. Afr J Prim Health Care Fam Med 2024, Vol. 28;16(1). [Google Scholar] [CrossRef]
- Brief, Medical. The right of foreign nationals in accessing SA healthcare. Available online: https://www.medicalbrief.co.za/sadc-citizens-refugees-asylum-seekers-benefit-sas-healthcare-system/#:~:text=The%20vagueness%20of%20the%20legislation’s,do%20you%20need%20to%20know?
- Alfaro-Velcamp, T. “Don’t send your sick here to be treated, our own people need it more”: immigrants’ access to healthcare in South Africa. International Journal of Migration, Health and Social Care 2017, Vol. 13(1), 53–68. [Google Scholar] [CrossRef]
- Scalabrini. Migrant and refugee access to health care. Available online: https://www.scalabrini.org.za/resources/2019-pre-2020/migrant-and-refugee-access-to-public-healthcare-in-south-africa-2/#:~:text=As%20we’ve%20seen%2C%20the,Health%20Act%20and%20Refugees%20Act.
- Thulo, R.; Lokotola, C.; Mash, R. Migrants’ Experiences of Accessing Primary Care in Emfuleni Municipality, South Africa. J Prim Care Community Health 2025, Vol.16. Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC12304633/. [CrossRef]
- Harerimana, A.; Pillay, J.D.; Mchunu, G. Medical xenophobia and healthcare exclusion of refugees and migrants in Africa: A scoping review. J Migr Health 2025, Vol.12. [Google Scholar] [CrossRef]
- White, J.A.; Levin, J.; Rispel, L.C. Migrants’ perceptions of health system responsiveness and satisfaction with health workers in a South African Province. Global Health Action 2020, 13(1). [Google Scholar] [CrossRef]
- Mvundura, L. Institutionalizing anti-migrant discourse in public healthcare: an analysis of medical xenophobia against Zimbabwean migrant women in Johannesburg. Afr. Hum. Mobil. Rev 2024, Vol.10(2), 67–92. [Google Scholar] [CrossRef]
- Georgetown University. Xenophobia: A Pervasive Crisis in Post-Apartheid South Africa. Available online: https://gjia.georgetown.edu/human-rights-development/xenophobia-a-pervasive-crisis-in-post-apartheid-south-africa/.
- United Nations Human Rights. South Africa: UN experts condemn xenophobic violence and racial discrimination against foreign nationals. Available online: https://www.ohchr.org/en/press-releases/2022/07/south-africa-un-experts-condemn-xenophobic-violence-and-racial.
- Doctors Without Borders. Ongoing xenophobic actions puts at risk the lives of several non-South African patients. Available online: https://www.msf.org.za/news-and-resources/press-release/xenophobic-attacks-endanger-non-sa-patients-msf.
- Gilson, L.; Raphaely, N. The terrain of health policy analysis in low and middle income countries: a review of published literature 1994-2007. Health Policy and Planning 2008, Vol. 23(5), 294–307. [Google Scholar] [CrossRef]
- Addae, D.; Quan-Baffour, K.P. Afrophobia, “black on black” violence and the new racism in South Africa: the nexus between adult education and mutual co-existence. Cogent Social Sciences 2022, 8(1). [Google Scholar] [CrossRef]
- Broman, C.L.; Kelly, M.D. A.; Bista, S.; Smith, T.D. Cumulative disadvantage and perceptions of unfair treatment. Ethnic and Racial Studies 2026, 1–26. [Google Scholar] [CrossRef]
- Nurius, P.S.; Prince, D.M.; Rocha, A. Cumulative Disadvantage and Youth Well-Being: A Multi-Domain Examination with Life Course Implications. Child Adolesc Social Work J. 2015, 32(6), 567–576. [Google Scholar] [CrossRef]
- Misago, J.P.; Landau, L.B. ‘Running Them Out of Time:’ Xenophobia, Violence, and Co-Authoring Spatiotemporal Exclusion in South Africa. Geopolitics 2023, Vol. 28(4), 1611–1631. [Google Scholar] [CrossRef]
- DW News. South Africa anti-immigrant group blocks access to hospitals. Available online: https://www.youtube.com/watch?v=lUe8UlQSQDU&t=1s.
- South African Government. Government on blocking of access to healthcare services. Available online: https://www.gov.za/news/media-statements/government-blocking-access-healthcare-services-05-jul-2025.
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



