Submitted:
15 April 2026
Posted:
17 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
1.1. Burden of Chronic Respiratory Symptoms in Advanced Lung Cancer
1.2. Challenges in Transitioning from Intensive Care to Home Care
1.3. Rationale for Wearable Smart Inhalers in Chronic Respiratory Management
2. Pathophysiology and Clinical Need
2.1. Chronic Bronchospasm, Dyspnoea, and Cough in Advanced Lung Cancer
2.2. Impact of Comorbid Obstructive Lung Diseases
2.3. Limitations of Conventional Inhaler-Based Therapy
3. Evolution of Inhaler Technology
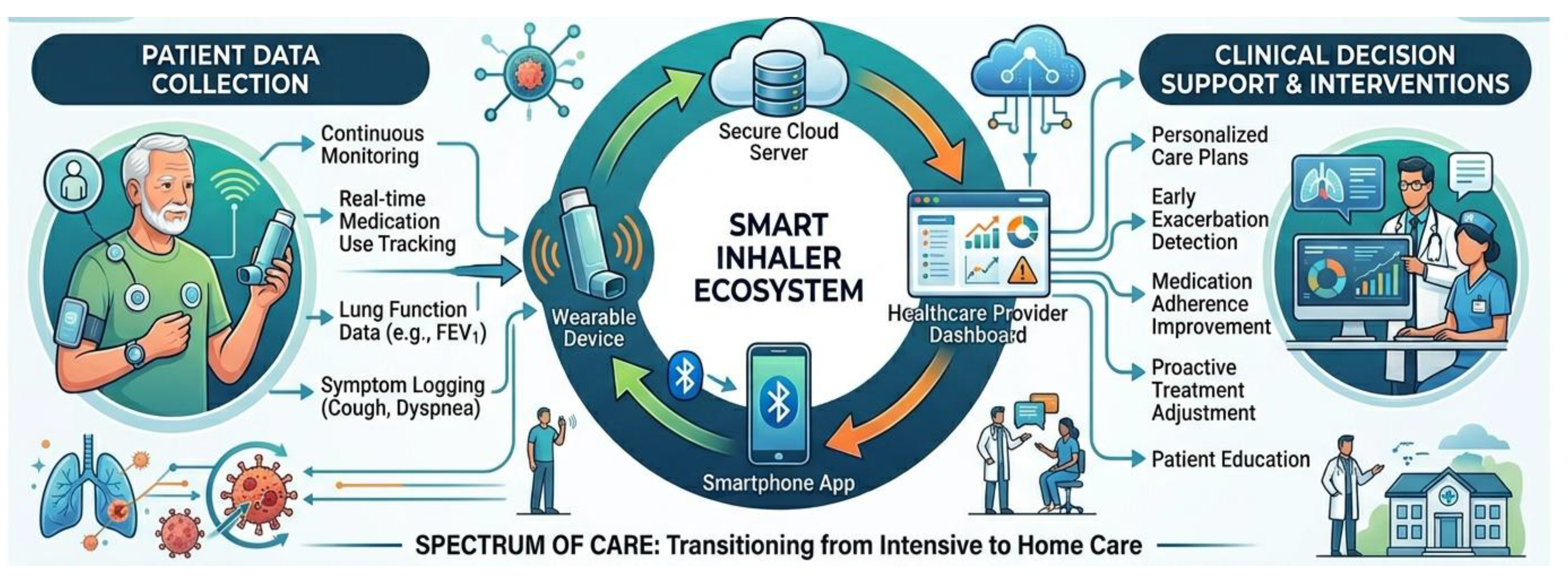
3.1. From Metered-Dose Inhalers to Smart Connected Devices
3.2. Role of Sensors, Connectivity, and Data Analytics
3.3. Current Evidence from Asthma and COPD Cohorts
4. Wearable Smart Inhalers, Design and Functionality
| Feature / Device Type | Conventional MDI/DPI | Smart Inhaler (Basic) | Wearable Smart Inhaler (Advanced) |
|---|---|---|---|
| Dose delivery mechanism | Manual actuation | Manual actuation | Manual or sensor-guided actuation |
| Technique feedback | None | Simple LED/audio cue | Flow-based technique scoring |
| Connectivity | None | Bluetooth to smartphone | BLE + IoT/cloud integration |
| Adherence tracking | Subjective recall only | Daily usage logs | Time-stamped adherence index |
| Environmental/physio sensing | No | Limited (timestamp, location) | Integrated with wearables (SpO2, RR) |
| AI-based decision support | No | Basic alerts | Personalized regimen suggestions |
| Suitable setting | Outpatient, home | Home, ambulatory care | ICU → home, chronic management |
4.1. Sensor Modules for Inhalation Technique and Timing
4.2. Wireless Data Transmission and Cloud-Based Platforms
4.3. Real-Time Feedback and User-Interface Design for Patients
5. Application in Advanced Lung Cancer
5.1. Selection Criteria and Patient Suitability
5.2. Monitoring Adherence, Technique, and Symptom Patterns
5.3. Integration with Existing Oncology and Palliative Care Regimens
6. Transition from Intensive Care to Home Care
6.1. Handover Protocols Incorporating Smart Inhaler Data
6.2. Remote Monitoring During Post-ICU Recovery
6.3. Roles of Home-Care Nurses, Respiratory Therapists, and Caregivers
7. Data-Driven Decision Support
7.1. AI and Machine-Learning Models for Early Exacerbation Prediction
7.2. Personalized Adjustment of Bronchodilator and Inhaler Regimens
7.3. Privacy, Security, and Regulatory Considerations
8. Clinical Outcomes and Patient-Reported Benefits
8.1. Reduction in Exacerbations and Hospital Readmissions
8.2. Improvement in Symptom Control and Quality of Life
8.3. Usability, Acceptance, and Barriers Among Advanced-Stage Patients
9. Implementation Challenges and Future Directions
9.1. Cost, Reimbursement, and Health-System Integration
9.2. Training Clinicians and Caregivers in Digital-Device Use
9.3. Next-Generation Smart Inhalers and Hybrid Respiratory Platforms
Conclusions
References
- Thangamani, M.; Anandakumar, D.; Indirajith, K.; Vijayaragavan, S.; Gandhimathi, M. (2026, March). Enhanced multimodal BERT-based deep learning method to predict prostate cancer from clinical data. In Sixth International Conference on Optical and Wireless Technologies (OWT 2025) (Vol. 14168, pp. 831-837). SPIE.
- Thamilarasi, V. Auditory Library Guide: A Digital Solution for Visually Impaired Readers. ITEGAM-JETIA 2026, 12(58), 108–117. [Google Scholar] [CrossRef]
- Suganya, V.; Vijayakumar, L.; Annur, E. A.; Praveen, R. V. S.; Bharathi, A.; Amsa, M. (2025, September). A Hybrid LSTM-Fuzzy Inference Model for Uncertainty-Aware Stock Market Forecasting. In 2025 International Conference on Electronics and Computing, Communication Networking Automation Technologies (ICEC2NT) (pp. 1-6). IEEE.
- Chellam, S.; Kalyani, S. Power flow tracing based transmission congestion pricing in deregulated power markets. International Journal of Electrical Power & Energy Systems 2016, 83, 570–584. [Google Scholar] [CrossRef]
- Govarthan, V.; Thangamani, M.; Anandakumar, D.; Tamizharasu, S.; Rajasekhara Babu, L.; Gandhimathi, K. (2026, March). Federated learning-enabled inverse design of photonic crystals with blockchain-secured collaboration for next-generation AI hardware. In Sixth International Conference on Optical and Wireless Technologies (OWT 2025) (Vol. 14168, pp. 552-557). SPIE.
- Shrivastava, A.; Praveen, R.; Alfilh, R. H.; Singh, N.; Yadav, K.; Rajalakshmi, B. (2025, September). AI-Driven Fault Resilience: Integrating Deep Graph Neural Networks in Spatio-Temporal Smart Grid Monitoring. In 2025 International Conference on Computing and Communications (COMPUTINGCON) (pp. 1-7). IEEE.
- Indoria, D.; Devi, K. Analyzing the effect of COVID-19 in the financial behavior of consumers and investors. International journal of health sciences 2022, 6(S5), 5976–5988. [Google Scholar] [CrossRef]
- Thamilarasi, V.; Sivakumar, J.; Roselin, R.; Jeysankar, N.; Wanjale, K. H.; Susila, S. J. G. (2026). Exploring AI Tools and Framework for Supply Chain Management. In Industry 6.0 and Digital Transformation in Supply Chain, Assets, and Services (pp. 65-98). IGI Global Scientific Publishing.
- Praveen, R. V. S.; Alsalami, Z.; Varshney, N.; Rajalakshmi, B.; Prasad, K. S.; Boob, N. S. (2025, September). AI-Integrated Demand Response with Dynamic Pricing in Prosumer-Driven Renewable Microgrids. In 2025 International Conference on Computing and Communications (COMPUTINGCON) (pp. 1-6). IEEE.
- Arunmohan, A. M.; Lakshmi, M. Analysis of modern construction projects using montecarlo simulation technique. International Journal of Engineering & Technology 2018, 7(2.19), 41–44. [Google Scholar] [CrossRef]
- Indoria, D. Ethical Challenges in Accounting Practice in the Era of Performance-Based Reporting. Minnesota Journal of Business Law and Entrepreneurship 2026, (1), 32–45. [Google Scholar]
- Sundaramoorthy, P.; Praveen, R. V. S.; Puli, B.; Tiwari, A.; Kanimozhi, S.; Keerthana, N. V. (2025, October). Decentralized Anomaly Detection in IoT Networks Using Federated Learning Models. In 2025 International Conference on Cognitive, Green and Ubiquitous Computing (IC-CGU) (pp. 1-6). IEEE.
- Thankappan, M.; Narayanan, N.; Sanaj, M. S.; Manoj, A.; Menon, A. P.; Krishna, M. G. (2024, April). Machine Learning and Deep Learning Architectures for Intrusion Detection System (IDS): A Survey. In 2024 1st International Conference on Trends in Engineering Systems and Technologies (ICTEST) (pp. 01-06). IEEE.
- Ravi, V.; Srivastava, V. K.; Singh, M. P.; Burila, R. K.; Chippagiri, S.; Pasam, V. R.; Prova, N. N. I. (2025, February). AI-powered fraud detection in real-time financial transactions. In International Conference on Web 6.0 and Industry 6.0 (pp. 431-447). Singapore: Springer Nature Singapore.
- Murugadoss, R.; Praveen, R. V. S.; Kunjumohamad, S. C.; PS, B. Osegnet-F-Unext: O-Segnet-Fusion-Unext for pulmonary lobe segmentation of Covid-19 using Computed Tomography image. European Spine Journal 2025, 1–17. [Google Scholar] [CrossRef]
- Jajini, M.; Kamaraj, N.; Santhiya, M.; Chellam, S. (2023). Blockchain-enabled electric vehicle charging. In Blockchain-Based Systems for the Modern Energy Grid (pp. 189-201). Academic Press.
- Dasari, D. R.; Bindu, G. H. Feature Selection Model-based Intrusion Detection System for Cyberattacks on the Internet of Vehicles Using Cat and Mouse Optimizer. J. Wirel. Mob. Networks Ubiquitous Comput. Dependable Appl. 2024, 15(2), 251–269. [Google Scholar] [CrossRef]
- Lavanya, K.; Thangamani, M.; Ganthimathi, M.; Priyanka, S.; Peter, V. J.; Sapthika, J. A Multi-Class Deep Neural Network Framework Driven Automated Classification Of Diabetic Retinopathy Using Retinal Fundus Images. Genetics and Molecular Research 2026, 25(1). [Google Scholar]
- Joshi, S. C.; Kumar, A. (2016, January). Design of multimodal biometrics system based on feature level fusion. In 2016 10th International Conference on Intelligent Systems and Control (ISCO) (pp. 1-6). IEEE.
- Praveen, R.; Simhadati, P.; Kavitha, K.; Majeeth, N. D. A.; Sethumadhavan, R.; Chauhan, A. (2024, December). Emotion Detection and Psychological Prediction Using Capsule Networks and Recurrent Neural Networks. In 2024 4th International Conference on Mobile Networks and Wireless Communications (ICMNWC) (pp. 1-6). IEEE.
- Thamilarasi, V.; Sivaraman, G.; Krishnan, R. H.; Kavitha, S. K.; Pushpa, P. EnhancinEnhancing Personalized Brand Recommendations through Machine Learning-Driven Analysis of User Behavior and Brand Interaction. In Intelligent Business Analytics (pp. 156-173). Auerbach Publications.
- Lakhekar, G. V.; Waghmare, L. M.; Roy, R. G. Disturbance observer-based fuzzy adapted S-surface controller for spatial trajectory tracking of autonomous underwater vehicle. IEEE Transactions on Intelligent Vehicles 2019, 4(4), 622–636. [Google Scholar] [CrossRef]
- Punitha, A.; Ramani, P. Dynamically stabilized recurrent neural network optimized with intensified sand cat swarm optimization for intrusion detection in wireless sensor network. Computers & Security 2025, 148, 104094. [Google Scholar]
- Kalaiselvi, M.; Dasa, S. K.; Malik, N.; Praveen, R. V. S. (2025, July). Intrusion Detection and Security Challenges in 6G Networks Using Stochastic Graph Neural Networks. In 2025 International Conference on Information, Implementation, and Innovation in Technology (I2ITCON) (pp. 1-6). IEEE.
- Kumar, G. H.; Elicherla, S. L. R.; Kumar, G. S.; Rai, B. K.; Saini, D. K. J. B.; Kumar, G. Proof-of-Metrology (PoM): A Blockchain Consensus for Tamper-Proof Calibration in Adversarial Cyber-Physical Systems. IEEE Access 2025, 13, 195937–195952. [Google Scholar] [CrossRef]
- Devarajanayaka, K. M.; Banu, S. S.; Desai, D. J.; TV, V.; Palav, M. R.; Dash, S. K. Machine learning-based pricing optimization for dynamic pricing in online retail. Journal of Informatics Education and Research 2024, 4(3). [Google Scholar]
- Chellam, S.; Kalyani, S. Optimization technique based power flow tracing in deregulated power system. Advances in Natural and Applied Sciences 2014, 8(20), 60–67. [Google Scholar]
- Shrivastava, A.; Habelalmateen, M. I.; Kaur, A.; Praveen, R. V. S.; Badhoutiya, A.; Kumar, A. (2025, August). Green Diagnosis: Deep Learning-Based Guava Leaf Disease Classification. In 2025 IEEE Madhya Pradesh Section Conference (MPCON) (pp. 267-273). IEEE.
- Sawant, V.; Zambare, P. DC fast charging stations for electric vehicles: A review. Energy Conversion and Economics 2024, 5(1), 54–71. [Google Scholar] [CrossRef]
- Arunmohan, A. M.; Bharathi, S.; Kokila, L.; Ponrooban, E.; Naveen, L.; Prasanth, R. An experimental investigation on utilisation of red soil as replacement of fine aggregate in concrete. Psychology and Education Journal 2021, 58. [Google Scholar]
- Poikaryil, O. B.; Babu, T. B.; Sagar, G.; Krishna, V.; Mitra, S. (2024). Transformative Fusion: Leveraging Blockchain and AI for Educational Data Analytics in Modern Education Systems. In Blockchain and AI in Shaping the Modern Education System (pp. 182-208). CRC Press.
- Shrivastava, A.; Praveen, R. V. S.; MuhsnHasan, M.; Bansal, S.; Dwivedi, S. P.; Krishna, O. (2025, September). Industry 4.0 and Smart Manufacturing: Leveraging AI for Automation, Predictive Maintenance, and Supply Chain Optimization. In 2025 International Conference on Computing and Communications (COMPUTINGCON) (pp. 1-6). IEEE.
- Chellam, S.; Kuruseelan, S.; & Jasmine Gnanamalar, A. Wind Energy Conversion System using Cascading H-Bridge Multilevel Inverter in High Ripple Scenario. International Journal of Electrical and Electronics Research 2024, 12(1), 178–186. [Google Scholar] [CrossRef]
- Prova, N. N. I.; Ravi, V.; Singh, M. P.; Srivastava, V. K.; Chippagiri, S.; Singh, A. P. Multilingual sentiment analysis in e-commerce customer reviews using GPT and deep learning-based weighted-ensemble model. International Journal of Cognitive Computing in Engineering 2025. [Google Scholar] [CrossRef]
- Radhika, A.; Karuppiah, N.; Soundradevi, G.; Mounica, P. (2024, July). Monitoring and Coordinated Control of Hybrid Power System with Energy Storage Device Using Arduino. In 2024 2nd International Conference on Sustainable Computing and Smart Systems (ICSCSS) (pp. 10-17). IEEE.
- Padmaja, A. R. L.; Mani, M. S. R. M.; Thangam, A.; Praveen, R. V. S.; Tikhe, K.; Sharma, M. S. (2025, September). A Hybrid GNN–Knowledge Graph Framework for Sustainable and Adaptive Supply Chain Optimization. In 2025 IEEE 4th International Conference for Advancement in Technology (ICONAT) (pp. 1-6). IEEE.
- Dasari, D. R.; Bindu, G. H. An Intelligent Intrusion Detection System in IoV Using Machine Learning and Deep Learning Models. International Journal of Communication Systems 2025, 38(10), e70131. [Google Scholar] [CrossRef]
- Indoria, D.; Devi, K. Exploring The Impact of Creative Accounting on Financial Reporting and Corporate Responsibility: A Comprehensive Analysis in Earnings Manipulation in Corporate Accounts. Journal of Marketing & Social Research 2025, 2, 668–677. [Google Scholar]
- Thamilarasi, V.; Krishnan, R. H.; Vijayalakshmi, V. (2025, July). Artificial Intelligence Driven Kyphosis. In Proceedings of Fourth International Conference on Computing and Communication Networks: ICCCN 2024, Volume 4 (Vol. 4, p. 177). Springer Nature.
- Eswari, S.; Nadgaundi, S. K.; Praveen, R. V. S.; Trakroo, K. (2025, November). Hybrid Genetic Algorithm–Fuzzy Logic Framework for Optimized Seed Quality Assessment and Yield Enhancement. In 2025 5th International Conference on Ubiquitous Computing and Intelligent Information Systems (ICUIS) (pp. 1074-1079). IEEE.
- Devi, K.; Indoria, D. Significance of employee training and development programs for skill enhancement, career growth, and employee retention. Asian Journal of Management and Commerce 2023, 4(2), 212–221. [Google Scholar] [CrossRef]
- Gurram, N. T. (2025, December). AI-Based Intrusion Detection Systems Using Deep Learning and Network Traffic Analysis. In 2025 OITS International Conference on Information Technology (OCIT) (pp. 492-497). IEEE.
- Kshirsagar, K. P. Key Frame Selection for One-Two Hand Gesture Recognition with HMM. International Journal of Advanced Computer Research 2015, 5(19), 192. [Google Scholar]
- Rajyaguru, M. H.; Shrivastava, A.; Praveen, R. V. S.; Vemuri, H. K.; Sista, S.; Al-Fatlawy, R. R. Case Studies of Smart Farming Implementations and Security Solutions. Sustainable Agriculture Production Using Blockchain Technology 2027, 239–251. [Google Scholar]
- Surendiran, R.; Chellam, S.; Jothin, R.; Ahilan, A.; Vallisree; Jasmine Gnana Malar, S.; Sathiamoorthy, A.J. (2023, April). Modified Elephant Herd Optimization-Based Advanced Encryption Standard. In International Conference on Frontiers of Intelligent Computing: Theory and Applications (pp. 519-528).
- Joshi, S.; Kumar, A. (2013, January). Feature extraction using DWT with application to offline signature identification. In Proceedings of the Fourth International Conference on Signal and Image Processing 2012 (ICSIP 2012) Volume 2 (pp. 285-294). India: Springer India.
- Sanaj, M. S.; Prathap, P. J. An infrastructure for embedded systems using task scheduling. Microprocessors and Microsystems 2020, 77, 103190. [Google Scholar] [CrossRef]
- Vignesh, V.; Karthik Babu, N. B.; Arun Mohan, A. M.; Sathees Kumar, S.; Nagaprasad, N.; Ayrilmis, N.; Krishnaraj, R. Development of hybrid fiber-reinforced vinyl ester composites for civil and automotive applications. Scientific Reports 2025, 15(1), 37174. [Google Scholar] [CrossRef] [PubMed]
- Sholapurapu, P. K.; Riadhusin, R.; Praveen, R. V. S.; Boob, N. S.; Singh, N.; Gudainiyan, J. Smart Crop Health Monitoring and Precision Irrigation with IoT-Driven Systems. Sustainable Agriculture Production Using Blockchain Technology 2027, 115–126. [Google Scholar]
- Akat, G. B. Structural Analysis of Ni1-xZnxFe2O4 Ferrite System. MATERIAL SCIENCE 2023, 22(05). [Google Scholar]
- Ramasubramanian, M.; Rathish babu, T. K. S.; Anantha Krishna, V.; Syed, K. (2021, July). Design of intelligent control and monitoring system for agriculture based on renewable energy and IoT. In Journal of Physics: Conference Series (Vol. 1964, No. 4, p. 042031). IOP Publishing.
- Punitha, A.; Manickam, J. M. L. Privacy preservation and authentication on secure geographical routing in VANET. Journal of ExpErimEntal & thEorEtical artificial intElligEncE 2017, 29(3), 617–628. [Google Scholar]
- Shrivastava, A.; Hundekari, S.; Praveen, R. V. S.; Alabdeli, H.; Labde, V. V.; Bansal, S. Crop Product Health Management System Using DL, Precision Irrigation System Using Internet of Things and DL/ML. Sustainable Agriculture Production Using Blockchain Technology 2027, 27–38. [Google Scholar]
- Srivastava, V. K.; Ravi, V.; Singh, M. P.; Prova, N. N. I. (2025, November). Federated Learning Optimization for Privacy-Preserving AI in Cloud Environments. In 2nd International Conference on Sustainable Business Practices and Innovative Models (ICSBPIM-2025) (pp. 825-840). Atlantis Press.
- Shivaraj, R. K.; Ramesh, S. N.; Shaheeda Banu, S. Effect of TM and loop length on drape coefficient of single jersey knitted fabrics. Int J Adv Res Eng Technol 2015, 6(1), 1–6. [Google Scholar]
- Bharath, B.; Shashidhar, V.; Santhosh Kumar, G. (2025, October). Trustworthy AI-Powered Multimodal Biofeedback for Stress Management: An Explainable, Privacy-Preserving, and Fairness-Aware Framework. In 2025 7th International Conference on Innovative Data Communication Technologies and Application (ICIDCA) (pp. 1250-1255). IEEE.
- Chunawala, H.; Ihsan, M.; Praveen, R. V. S.; Boob, N. S.; Thethi, H. P.; Badhoutiya, A. Agriculture Supply Chain Management System Using Blockchain. Sustainable Agriculture Production Using Blockchain Technology 2027, 15–26. [Google Scholar]
- Dasari, D. R.; Gottumukkala, H. An efficient intrusion detection system in iov using improved random forest model. International Journal of Transport Development and Integration 2024, 8(4). [Google Scholar] [CrossRef]
- Lakhekar, G. V.; Waghmare, L. M.; Jadhav, P. G.; Roy, R. G. Robust diving motion control of an autonomous underwater vehicle using adaptive neuro-fuzzy sliding mode technique. IEEE Access 2020, 8, 109891–109904. [Google Scholar] [CrossRef]
- Indoria, D.; Devi, K. (2021). An Analysis On The Consumers Perception Towards Upi.
- Wadate, M. P. R.; Deshmukh, P. S.; Kadam, V. V.; Kadam, C. T.; Navgire, M. A study of electric bike-future needs. International Journal for Research in Applied Science & Engineering Technology 2019, 2(5), 1331–1334. [Google Scholar]
- Victor, S.; Kumar, K. R.; Praveen, R. V. S.; Aida, R.; Kaur, H.; Bhadauria, G. S. (2025, August). GAN and RNN Based Hybrid Model for Consumer Behavior Analysis in E-Commerce. In 2025 2nd International Conference on Intelligent Algorithms for Computational Intelligence Systems (IACIS) (pp. 1-6). IEEE.
- Anand, J.; Thamilarasi, V.; Rayal, A.; Gupta, H. K.; Jyothi, K.; Vishwakarma, P. (2025, February). Fuzzy Logic-Based Deep Learning for Human-Machine Interaction and Gesture Recognition in Uncertain and Noisy Environments. In 2025 First International Conference on Advances in Computer Science, Electrical, Electronics, and Communication Technologies (CE2CT) (pp. 435-440). IEEE.
- Aravindhan, K.; Soundradevi, G. Power flow control of hybrid micro-grids using modified UIPC. Materials Today: Proceedings 2020, 33, 3810–3818. [Google Scholar] [CrossRef]
- NAZIR, M. W.; RABBANI, A. A.; ABDULLAEVA, I.; WARSI, A. Z.; NURULLAYEVA, N.; SULTANA, F.; FAROOQ, B. The role of green supply chains in enhancing corporate social responsibility and consumer engagement. TPM–Testing, Psychometrics, Methodology in Applied Psychology 2025, 32 (S1 (2025): Posted, 1557–1566. [Google Scholar]
- Praveen, R. V. S.; Peri, S. S. S. R. G.; Vemuri, H.; Sista, S.; Vemuri, S. S.; Aida, R. (2025, September). Application of AI and Generative AI for Understanding Student Behavior and Performance in Higher Education. In 2025 International Conference on Intelligent Communication Networks and Computational Techniques (ICICNCT) (pp. 1-6). IEEE.
- Akat, G. B.; Magare, B. K. Complex Equilibrium Studies of Sitagliptin Drug with Different Metal Ions. Asian Journal of Organic & Medicinal Chemistry 2022. [Google Scholar]
- Devi, K.; Indoria, D. Impact of Russia-Ukraine War on the Financial Sector of India. Drishtikon: A Management Journal 2024, 15(1). [Google Scholar]
- Zambare, P.; Liu, Y. (2023, October). An optimized graph neural network-based approach for intrusion detection in smart vehicles. In IFIP International Internet of Things Conference (pp. 3-17). Cham: Springer Nature Switzerland.
- Kumar, S.; Praveen, R. V. S.; Aida, R.; Varshney, N.; Alsalami, Z.; Boob, N. S. (2025, September). Enhancing AI Decision-Making with Explainable Large Language Models (LLMs) in Critical Applications. In 2025 IEEE International Conference on Advances in Computing Research On Science Engineering and Technology (ACROSET) (pp. 1-6). IEEE.
- Mohan, A. A.; Vignesh, V.; Nagaprasad, N.; Krishnaraj, R. Mechanical and thermal behaviour of waste spent coffee ground filler reinforced vinyl-ester composites for civil construction applications. Scientific Reports 2025. [Google Scholar] [CrossRef]
- Akat, G. B.; Magare, B. K. Mixed Ligand Complex Formation of Copper (II) with Some Amino Acids and Metoprolol. Asian Journal of Organic & Medicinal Chemistry 2022. [Google Scholar]
- Pavan Kumar, U.; Santhosh Kumar, G.; Hemanth Kumar, G.; Aryalekshmi, B. N.; Saxena, S. (2025, June). Fault Detection in Power Line Communication Systems for Smart Grids by Using One Class Support Vector Machine-Based Autoencoder. In International Conference on 6G Communications Networking and Signal Processing (pp. 333-344). Singapore: Springer Nature Singapore.
- Praveen, R. V. S.; Aida, R.; Trakroo, K.; Rambhatla, A. K.; Srivastava, K.; Perada, A. (2025, October). Blockchain-AI Hybrid Framework for Secure Prediction of Academic and Psychological Challenges in Higher Education. In 2025 10th International Conference on Communication and Electronics Systems (ICCES) (pp. 1618-1623). IEEE.
- Palaniappan, K.; Krishna, V. A.; Ramasubramanian, M.; Babu, T. R. (2023, January). A blockchain based virtual machine detection system app market. In AIP Conference Proceedings (Vol. 2523, No. 1, p. 020013). AIP Publishing LLC. AIP Conference Proceedings. [CrossRef]
- Joshi, S. (2021, November). Discrete Wavelet Transform Based Approach for Touchless Fingerprint Recognition. In Proceedings of International Conference on Data Science and Applications: ICDSA 2021, Volume 1 (pp. 397-412). Singapore: Springer Singapore.
- Suganthi, D. B.; Vidhyalakshmi, M. K.; Punitha, A.; Raghupathi, S.; Subhapradha, M. A Review on Transdisciplinary Approach and Challenges on Wearable Technology. Recent Progress in Science and Technology 2023, Vol. 7(7), 161–173. [Google Scholar]
- Praveen, R. V. S.; Aida, R.; Rambhatla, A. K.; Trakroo, K.; Maran, M.; Sharma, S. (2025, October). Hybrid Fuzzy Logic-Genetic Algorithm Framework for Optimized Supply Chain Management in Smart Manufacturing. In 2025 10th International Conference on Communication and Electronics Systems (ICCES) (pp. 1487-1492). IEEE.
- Kumar, G. H.; Saini, D. K. J.; Kalpana, V.; Kumar, Y. D. (2025, December). Secure Edge AI: A Federated Learning Approach to Cache Side-Channel Attack Detection in Vehicular Networks. In 2025 IEEE 17th International Conference on Computational Intelligence and Communication Networks (CICN) (pp. 1046-1052). IEEE.
- Scientific, L. L. AN EFFICIENT AND EXTREME LEARNING MACHINE FOR AUTOMATED DIAGNOSIS OF BRAIN TUMOR. Journal of Theoretical and Applied Information Technology 2025, 103(17). [Google Scholar]
- Shrivastava, A.; Praveen, R. V. S.; Aida, R.; Vemuri, K.; Vemuri, S. S.; Husain, S. O. (2025, September). V2G-Enabled Transactive Energy Model Using Blockchain for Peer-to-Peer EV Charging Networks. In 2025 International Conference on Computing and Communications (COMPUTINGCON) (pp. 1-7). IEEE.
- Singh, M. P.; Ravi, V.; Srivastava, V. K.; Prova, N. (2025, August). AI-Driven Autonomous API Orchestration for Multi-Cloud Integration. In 2025 International Conference on Sustainability, Innovation & Technology (ICSIT) (pp. 1-6). IEEE.
- Sanaj, M. S.; Prathap, P. J. (2020, July). An enhanced Round robin (ERR) algorithm for effective and efficient task scheduling in cloud environment. In 2020 Advanced Computing and Communication Technologies for High Performance Applications (ACCTHPA) (pp. 107-110). IEEE.
- Praveen, R. V. S.; Sista, S.; Aida, R.; Vemuri, S. S.; Yusuf, N.; Sankar, B. (2025, September). Predictive Modelling of Urban Energy and Traffic Systems Using Generative Artificial Intelligence Techniques. In 2025 IEEE 4th International Conference for Advancement in Technology (ICONAT) (pp. 1-6). IEEE.
- Kshirsagar, K. P.; Doye, D. (2010, October). Object Based Key Frame Selection for Hand Gesture Recognition. In 2010 International Conference on Advances in Recent Technologies in Communication and Computing (pp. 181-185). IEEE.
- Lakhekar, G. V.; Roy, R. G. (2014, March). Heading control of an underwater vehicle using dynamic fuzzy sliding mode controller. In 2014 International Conference on Circuits, Power and Computing Technologies [ICCPCT-2014] (pp. 1448-1454). IEEE.
- Praveen, R. V. S.; Sista, S.; Aida, R.; Vemuri, S. S.; Chagi, S.; Sankar, B. (2025, September). Intelligent Integration of Generative AI in Medical Diagnostics and Data Analysis for Next-Generation Healthcare Systems. In 2025 IEEE 4th International Conference for Advancement in Technology (ICONAT) (pp. 1-6). IEEE.
- Kumar, R. S. P.; Banu, S. S. An exploration of strategies in marketing of organic fruits and vegetables. South Eastern European Journal of Public Health 2025. [Google Scholar] [CrossRef]
- Praveen, R. V. S.; Vemuri, H.; Peri, S. S. S. R. G.; Aida, R.; Vemuri, S. S.; Yusuf, N. (2025, September). An Intelligent Approach for Detecting Anomalies in Cloud Computing Using AI Techniques. In 2025 IEEE 4th International Conference for Advancement in Technology (ICONAT) (pp. 1-6). IEEE.
- Saxena, S.; Pavan Kumar, U.; Santhosh Kumar, G.; Hemanth Kumar, G.; Aryalekshmi, B. N. (2025, June). Signal Processing Approaches for Secure Channel Estimation and Data Transmission in 5G/6G. In International Conference on 6G Communications Networking and Signal Processing (pp. 193-203). Singapore: Springer Nature Singapore.
- Bindu, G. H.; Dasari, D. R. Federated Learning Framework for Intrusion Detection System in Internet of Vehicles with Memory-Augmented Deep Autoencoder. 2024. [Google Scholar] [CrossRef]
- Praveen, R. V. S.; Sista, S.; Aida, R.; Vemuri, S. S.; Yusuf, N.; Sankar, B. (2025, October). A Hybrid CNN-LSTM Framework for Real-Time Human Intrusion Detection in Wireless Sensor Networks. In 2025 IEEE 6th Global Conference for Advancement in Technology (GCAT) (pp. 1-6). IEEE.
- Devi, K.; Indoria, D. Recent Trends of Financial Growth and Policy Interventions in the Higher Educational System. Advances in Consumer Research 2025, 2(2). [Google Scholar]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




