Submitted:
09 April 2026
Posted:
16 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Methods
2.1. Study Design and Setting
2.2. Study Participants
3. Data Collection and Study Measures
3.1. Variable Definition
3.2. Statistical Analysis
4. Ethical Considerations
5. Results
6. Discussion
6. Conclusions
Funding
Institutional Review Board Statement
Informed Consent Statement
Clinical trial number
Consent for publication
Conflicts of Interest
References
- Global tuberculosis report 2023. Available online: https://www.who.int/publications/i/item/9789240083851 (accessed on 18 Jun 2024).
- Vishwakarma, D.; Gaidhane, A.; Sahu, S.; Rathod, A.S.; Vishwakarma, D.; Gaidhane, A.; et al. Multi-Drug Resistance Tuberculosis (MDR-TB) Challenges in India: A Review. Cureus 2023, 15. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Xu, J.; Chen, Y.; Wu, R.; Ji, H.; Pan, Y.; et al. The relationship among social support, experienced stigma, psychological distress, and quality of life among tuberculosis patients in China. Sci Rep. 2021, 11, 24236. [Google Scholar] [CrossRef] [PubMed]
- Craig, G.M.; Daftary, A.; Engel, N.; O’Driscoll, S.; Ioannaki, A. Tuberculosis stigma as a social determinant of health: a systematic mapping review of research in low incidence countries. International Journal of Infectious Diseases 2017, 56, 90–100. [Google Scholar] [CrossRef] [PubMed]
- Liboon Aranas, L.; Alam, K.; Gyawali, P.; Alam, R.M. Drug-Resistant Tuberculosis Stigma Among HealthCare Workers Toward the Development of a Stigma-Reduction Strategy: A Scoping Review. INQUIRY 2023, 60, 00469580231180754. [Google Scholar] [CrossRef] [PubMed]
- Redwood, L.; Mitchell, E.M.H.; Nguyen, T.A.; Viney, K.; Duong, L.; Phạm, H.T.; et al. Adaptation and validation of the Van Rie tuberculosis stigma scale in Vietnam. International Journal of Infectious Diseases 2022, 114, 97–104. [Google Scholar] [CrossRef] [PubMed]
- Naidu, T.; Pillay, S.R.; Ramlall, S.; Mthembu, S.S.; Padayatchi, N.; Burns, J.K.; et al. Major Depression and Stigma among Individuals with Multidrug-Resistant Tuberculosis in South Africa. 2020. [Google Scholar] [CrossRef] [PubMed]
- Knowledge, Attitude and Practice(KAP) of tuberculosis patients enrolled on treatment in Juba City, South Sudan2010. A pilot study. Available online: http://www.southsudanmedicaljournal.com/archive/may-2014/knowledge-attitude-and-practicekap-of-tuberculosis-patients-enrolled-on-treatment-in-juba-city-south-sudan2010.-a-pilot-study.html (accessed on 12 Jul 2022).
- Hoa, N.B.; Nhung, N.V.; Khanh, P.H.; Hai, N.V.; Quyen, B.T.T. Adverse events in the treatment of MDR-TB patients within and outside the NTP in Pham Ngoc Thach hospital, Ho Chi Minh City, Vietnam. BMC Research Notes 2015, 8, 809. [Google Scholar] [CrossRef] [PubMed]
- Van Rie, A.; Sengupta, S.; Pungrassami, P.; Balthip, Q.; Choonuan, S.; Kasetjaroen, Y.; et al. Measuring stigma associated with tuberculosis and HIV/AIDS in southern Thailand: exploratory and confirmatory factor analyses of two new scales. Trop Med Int Health 2008, 13, 21–30. [Google Scholar] [CrossRef] [PubMed]
- Yan, S.; Zhang, S.; Tong, Y.; Yin, X.; Lu, Z.; Gong, Y. Nonadherence to Antituberculosis Medications: The Impact of Stigma and Depressive Symptoms. Am J Trop Med Hyg. 2018, 98, 262–5. [Google Scholar] [CrossRef] [PubMed]
- Redwood, L.; Mitchell, E.M.H.; Viney, K.; Snow, K.; Nguyen, T.A.; Dung La, T.; et al. Depression, stigma and quality of life in people with drug-susceptible TB and drug-resistant TB in Vietnam. Int J Tuberc Lung Dis. 2021, 25, 461–7. [Google Scholar] [CrossRef] [PubMed]
- Pradhan, A.; Koirala, P.; Bhandari, S.S.; Dutta, S.; García-Grau, P.; Sampath, H.; et al. Internalized and Perceived Stigma and Depression in Pulmonary Tuberculosis: Do They Explain the Relationship Between Drug Sensitivity Status and Adherence? Front Psychiatry 2022, 13. [Google Scholar] [CrossRef] [PubMed]
- Isara, A.R.; Akpodiete, A. Concerns about the knowledge and attitude of multidrug-resistant tuberculosis among health care workers and patients in Delta State, Nigeria. Niger J Clin Pract. 2015, 18, 664–9. [Google Scholar] [CrossRef] [PubMed]
- Redwood, L.; Fox, G.J.; Nguyen, T.A.; Bernarys, S.; Mason, P.; Vu, V.A.; et al. Good citizens, perfect patients, and family reputation: Stigma and prolonged isolation in people with drug-resistant tuberculosis in Vietnam. PLOS Global Public Health 2022, 2, e0000681. [Google Scholar] [CrossRef] [PubMed]
- Morris, M.D.; Quezada, L.; Bhat, P.; Moser, K.; Smith, J.; Perez, H.; et al. Social, economic, and psychological impacts of MDR-TB treatment in Tijuana, Mexico: a patient’s perspective. Int J Tuberc Lung Dis. 2013, 17, 954–60. [Google Scholar] [CrossRef] [PubMed]
- Agarwal, N.; Sarthi, P. The necessity of psychological interventions to improve compliance with Tuberculosis treatment and reduce psychological distress. J Family Med Prim Care 2020, 9, 4174–80. [Google Scholar] [CrossRef] [PubMed]
- Alemu, A.; Bitew, Z.W.; Worku, T. Poor treatment outcome and its predictors among drug-resistant tuberculosis patients in Ethiopia: A systematic review and meta-analysis. International Journal of Infectious Diseases 2020, 98, 420–39. [Google Scholar] [CrossRef] [PubMed]
- Courtwright, A.; Turner, A.N. Tuberculosis and stigmatization: pathways and interventions. Public Health Rep. 2010, 125 Suppl 4, 34–42. [Google Scholar] [CrossRef] [PubMed]
| Variable | Total (n = 528) |
|---|---|
| Age, years | 42.61 ± 13.62 |
| Sex | |
| Male | 364 (68.94) |
| Female | 164 (31.06) |
| Occupation | |
| Informal/manual work | 256 (48.48) |
| Not currently employed | 117 (22.16) |
| Business/service | 80 (15.15) |
| Other | 75 (14.20) |
| Study site | |
| Ho Chi Minh | 278 (52.65) |
| An Giang | 109 (20.64) |
| Can Tho | 52 (9.85) |
| Ha Noi | 39 (7.39) |
| Thanh Hoa | 24 (4.55) |
| Tien Giang | 20 (3.79) |
| Da Nang | 6 (1.14) |
| Variable | Spearman's ρ0. | P-value |
|---|---|---|
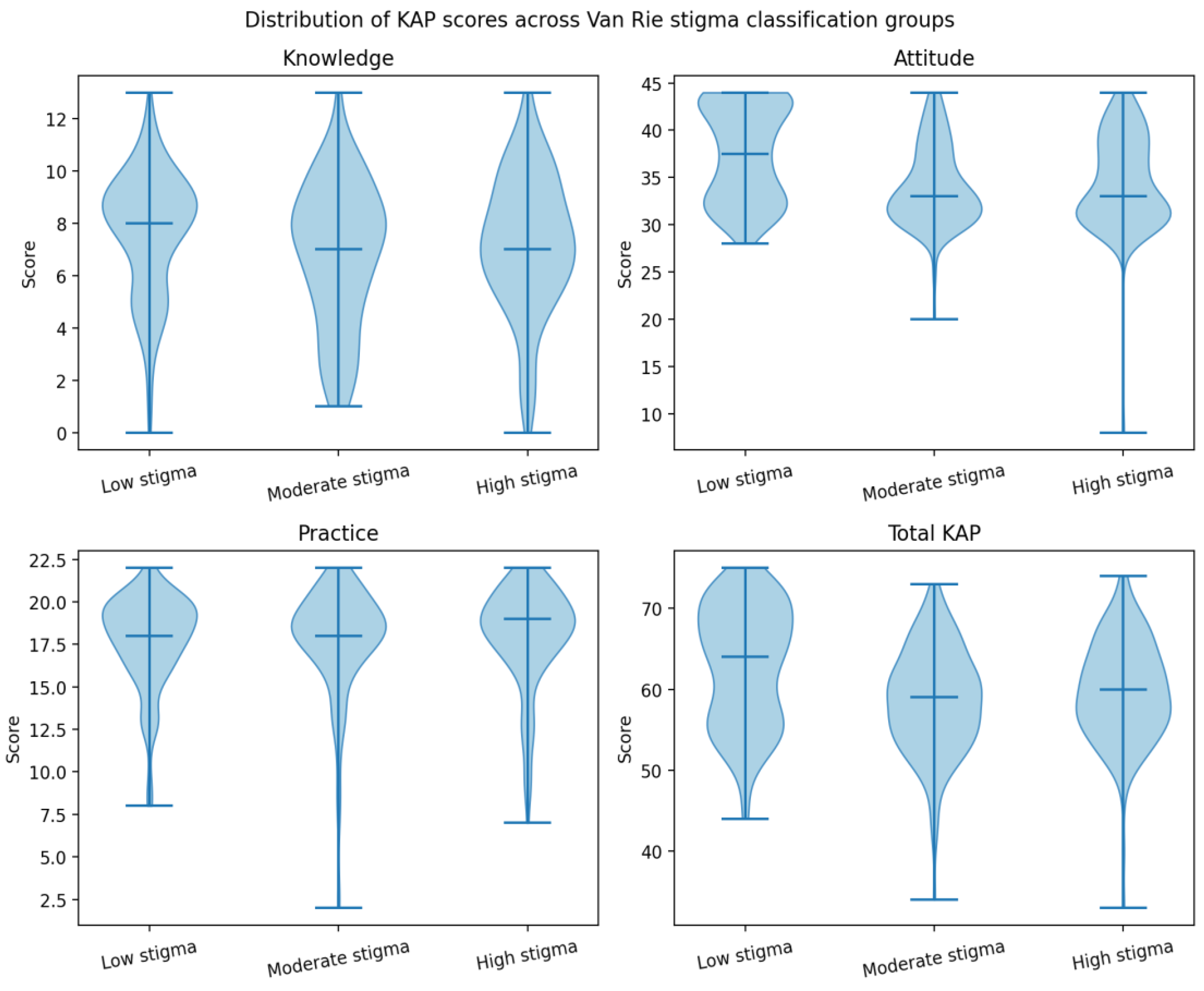
| Knowledge total | -0.095 | 0.030 |
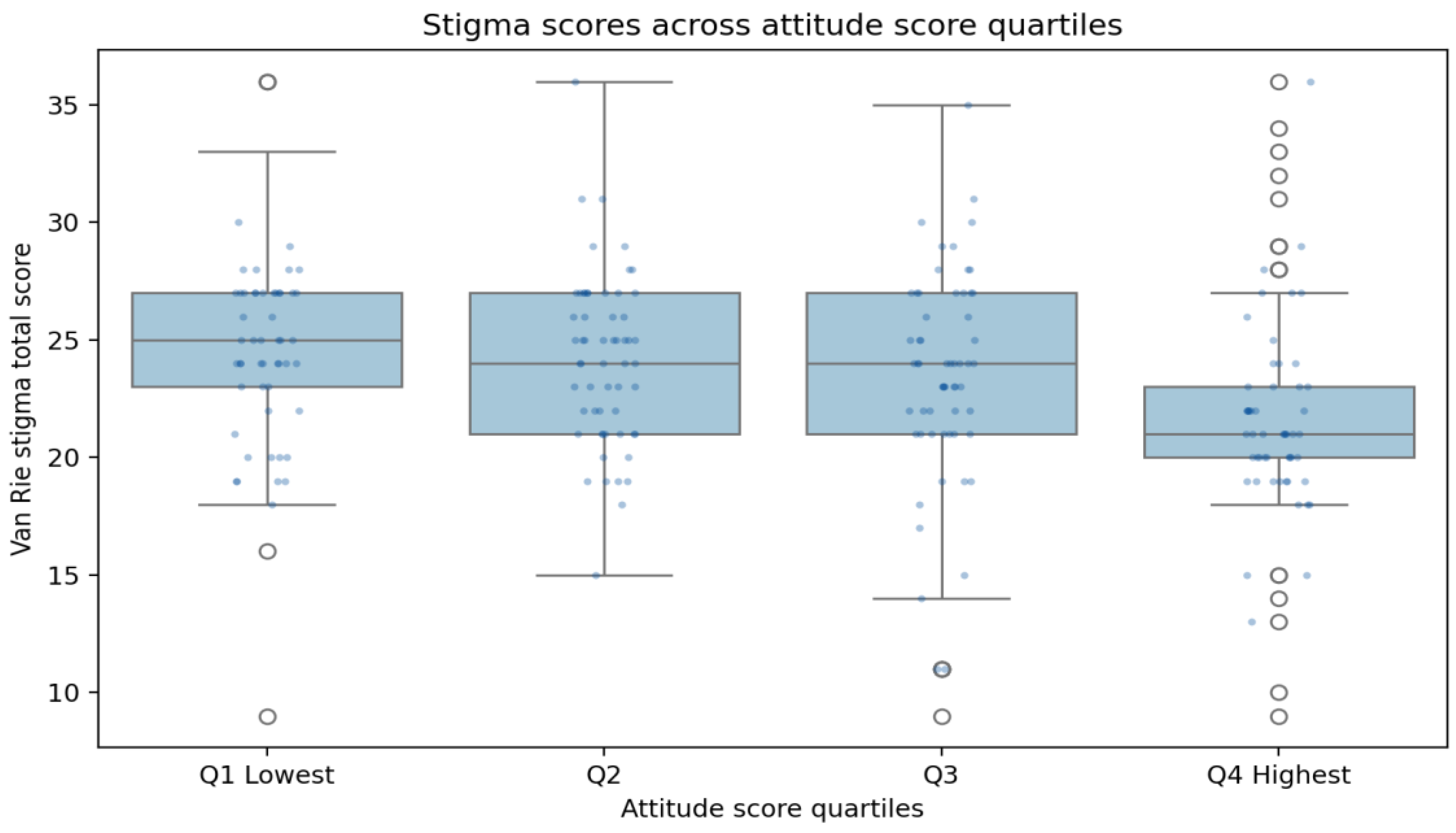
| Attitude total | -0.270 | < 0.001 |
| Practice total | 0.081 | 0.065 |
| Total KAP | -0.192 | < 0.001 |
| Variable | Unstandardized β | 95% Confidence Interval (CI) | P-value |
|---|---|---|---|
| (Constant) | 32.319 | [28.571, 36.068] | < 0.001 |
| Knowledge total | 0.089 | [-0.059, 0.237] | 0.237 |
| Attitude total | -0.229 | [-0.306, -0.153] | < 0.001 |
| Practice total | -0.058 | [-0.187, 0.071] | 0.374 |
| Age | 0.021 | [-0.006, 0.047] | 0.124 |
| Female | -0.139 | [-0.900, 0.622] | 0.720 |
| On treatment | -1.966 | [-2.716, -1.216] | < 0.001 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




