Submitted:
14 April 2026
Posted:
15 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Participants
2.2. Surgical Procedure
2.3. Postoperative Rehabilitation
2.4. Procedure
2.5. Statistical Analysis
3. Results
3.1. General Characteristics of Participants
3.2. Hip Disability and Osteoarthritis Outcome Score (HOOS)
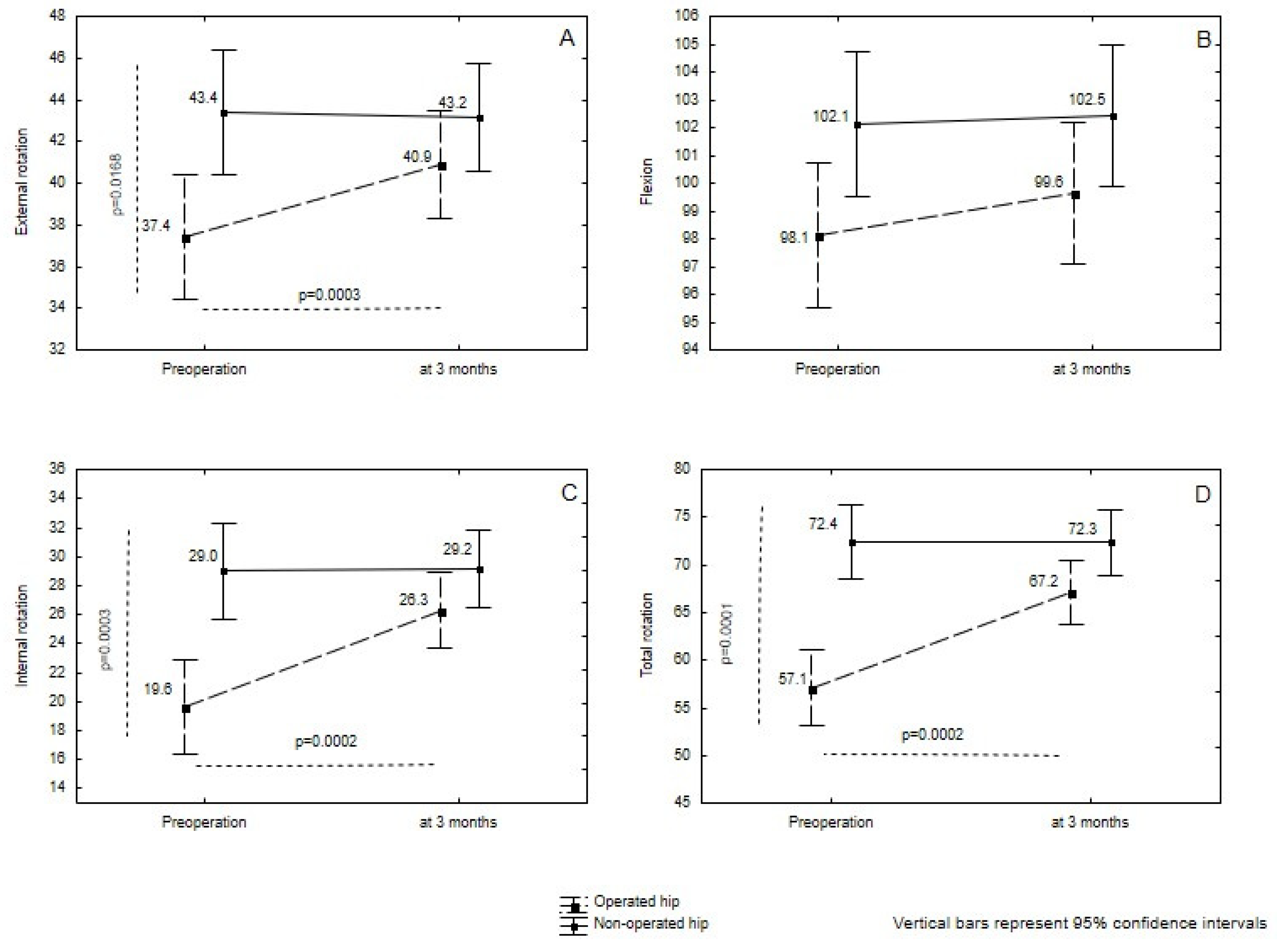
3.3. Active Range of Motion
3.4. Associations Between Hip Range of Motion and HOOS Scores
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Acknowledgments
Conflicts of Interest
References
- Griffin, D.R.; Dickenson, E.J.; O’Donnell, J.; Agricola, R.; Awan, T.; Beck, M.; Clohisy, J.C.; Dijkstra, H.P.; Falvey, E.; Gimpel, M.; et al. The Warwick Agreement on femoroacetabular impingement syndrome (FAI syndrome): An international consensus statement. Br. J. Sports Med. 2016, 50, 1169–1176. [CrossRef]
- Harris, J.D.; Erickson, B.J.; Bush-Joseph, C.A.; Nho, S.J. Treatment of femoroacetabular impingement: A systematic review. Curr. Rev. Musculoskelet. Med. 2013, 6, 207–218. [CrossRef]
- Dasari, S.P.; Kasson, L.B.; Condon, J.J.; Mameri, E.S.; Kerzner, B.; Khan, Z.A.; Jackson, G.R.; Gursoy, S.; Sivasundaram, L.; Hevesi, M.; et al. Systematic review and meta-analysis of studies comparing complete capsular closure against unrepaired hip capsules during hip arthroscopy. Orthop. J. Sports Med. 2023, 11, 23259671231197435. [CrossRef]
- Kemp, J.L.; Collins, N.J.; Roos, E.M.; Crossley, K.M. Psychometric properties of patient-reported outcome measures for hip arthroscopic surgery. Am. J. Sports Med. 2013, 41, 2065–2073. [CrossRef]
- Burnel, J.; Chamu, T.; Bonin, N.; Van Cant, J.; Pairot De Fontenay, B. Strength, mobility, and functional outcomes 2.5 months after hip arthroscopy for femoroacetabular impingement syndrome: A cross-sectional study. Phys. Ther. Sport 2025, 71, 43–52. [CrossRef]
- Garcia-Lopez, E.; Halvorson, R.T.; Foley, A.J.; Zhang, A.L.; Wong, S.E. Restoration of hip kinematics after arthroscopy for femoroacetabular impingement syndrome: A 1-year evaluation of gait and stair performance. Orthop. J. Sports Med. 2025, 13, 23259671251339777. [CrossRef]
- Casartelli, N.C.; Maffiuletti, N.A.; Item-Glatthorn, J.F.; Impellizzeri, F.M.; Leunig, M. Hip muscle strength recovery after hip arthroscopy in a series of patients with symptomatic femoroacetabular impingement. Hip Int.2014, 24, 387–393. [CrossRef]
- Filan, D.; Mullins, K.; Carton, P. Hip range of motion is increased after hip arthroscopy for femoroacetabular impingement: A systematic review. Arthrosc. Sports Med. Rehabil. 2022, 4, e797–e822. [CrossRef]
- Freke, M.D.; Crossley, K.; Sims, K.; Russell, T.; Weinrauch, P.; Gamboa, G.; Semciw, A. Acute and subacute changes in hip strength and range of movement after arthroscopy to address chondrolabral pathology. Am. J. Sports Med. 2019, 47, 1939–1948. [CrossRef]
- Pålsson, A.; Kostogiannis, I.; Ageberg, E. Combining results from hip impingement and range of motion tests can increase diagnostic accuracy in patients with FAI syndrome. Knee Surg. Sports Traumatol. Arthrosc. 2020, 28, 3382–3392. [CrossRef]
- Kannan, A.S.; Hartwell, M.J.; Grace, T.; Hammond, E.; Soriano, K.K.J.; Souza, R.B.; Zhang, A.L. Correlating biomechanical gait analysis with patient-reported outcomes after hip arthroscopy for femoroacetabular impingement syndrome. Orthop. J. Sports Med. 2022, 10, 23259671221121352. [CrossRef]
- Kemp, J.L.; Makdissi, M.; Schache, A.G.; Finch, C.F.; Pritchard, M.G.; Crossley, K.M. Is quality of life following hip arthroscopy in patients with chondrolabral pathology associated with impairments in hip strength or range of motion? Knee Surg. Sports Traumatol. Arthrosc. 2016, 24, 3955–3961. [CrossRef]
- Stołowski, Ł.; Kerkhoffs, G.; Piontek, T. Hip active range of motion in patients with femoroacetabular impingement syndrome. Sensors 2025, 25, 1219. [CrossRef]
- Stołowski, Ł.; Bąkowski, P.; Kiedrowski, B.; Kaszyński, J.; Kerkhoffs, G.; Piontek, T. Rehabilitation protocol after hip arthroscopy. Issue Rehabil. Orthop. Neurophysiol. Sport Promot. 2021, 36, 49–65. [CrossRef]
- Gojło, M.K.; Paradowski, P.T. Polish adaptation and validation of the hip disability and osteoarthritis outcome score (HOOS) in osteoarthritis patients undergoing total hip replacement. Health Qual. Life Outcomes 2020, 18, 135. [CrossRef]
- Polascik, B.A.; Peck, J.; Cepeda, N.; Lyman, S.; Ling, D. Reporting clinical significance in hip arthroscopy: Where are we now? HSS J. 2020, 16, 527–533. [CrossRef]
- Minkara, A.A.; Westermann, R.W.; Rosneck, J.; Lynch, T.S. Systematic review and meta-analysis of outcomes after hip arthroscopy in femoroacetabular impingement. Am. J. Sports Med. 2019, 47, 488–500. [CrossRef]
- Ramisetty, N.; Kwon, Y.; Mohtadi, N. Patient-reported outcome measures for hip preservation surgery—A systematic review of the literature. J. Hip Preserv. Surg. 2015, 2, 15–27. [CrossRef]
- Thorborg, K.; Kraemer, O.; Madsen, A.D.; Hölmich, P. Patient-reported outcomes within the first year after hip arthroscopy and rehabilitation for femoroacetabular impingement and/or labral injury: The difference between getting better and getting back to normal. Am. J. Sports Med. 2018, 46*, 2607–2614. [CrossRef]
- Flores, S.E.; Sheridan, J.R.; Borak, K.R.; Zhang, A.L. When do patients improve after hip arthroscopy for femoroacetabular impingement? A prospective cohort analysis. Am. J. Sports Med. 2018, 46, 3111–3118. [CrossRef]
- Birrell, F.; Croft, P.; Cooper, C.; Hosie, G.; Macfarlane, G.; Silman, A. Predicting radiographic hip osteoarthritis from range of movement. Rheumatology 2001, 40, 506–512. [CrossRef]
- Choi, S.M.; Park, M.S.; Ju, B.C.; Yoon, S.J. Alterations in range of motion and clinical outcomes after femoroplasty in Asians. J. Am. Acad. Orthop. Surg. 2018, 26, e181–e190. [CrossRef]
- Burnel, J.; Chamu, T.; Bonin, N.; Van Cant, J.; Pairot De Fontenay, B. Strength, mobility, and functional outcomes 2.5 months after hip arthroscopy for femoroacetabular impingement syndrome: A cross-sectional study. Phys. Ther. Sport 2025, 71, 43–52. [CrossRef]
- Tijssen, M.; van Cingel, R.; de Visser, E.; Nijhuis-van der Sanden, M. A clinical observational study on patient-reported outcomes, hip functional performance and return to sports activities in hip arthroscopy patients. Phys. Ther. Sport 2016, 20, 45–55. [CrossRef]
- Naili, J.E.; Stålman, A.; Valentin, A.; Skorpil, M.; Weidenhielm, L. Hip joint range of motion is restricted by pain rather than mechanical impingement in individuals with femoroacetabular impingement syndrome. Arch. Orthop. Trauma. Surg. 2022, 142, 1985–1994. [CrossRef]
- Nguyen, K.H.; Shaw, C.; Link, T.M.; Majumdar, S.; Souza, R.B.; Vail, T.P.; Zhang, A.L. Changes in hip capsule morphology after arthroscopic treatment for femoroacetabular impingement syndrome with periportal capsulotomy are correlated with improvements in patient-reported outcomes. Arthroscopy 2022, 38, 394–403. [CrossRef]
- Gomes, D.A.; Heerey, J.; Scholes, M.; Mosler, A.; Jones, D.; Coburn, S.; Johnston, R.; Agricola, R.; et al. More is not always better—Association between hip range of motion and symptom severity in patients with femoroacetabular impingement syndrome: A cross-sectional study. Braz. J. Phys. Ther. 2025, 29, 101189. [CrossRef]
- Freke, M.; Kemp, J.; Crossley, K.; Sims, K.; Russell, T.; Semciw, A. Strength and range of movement deficits are associated with symptom severity in people scheduled for hip arthroscopy. Eur. J. Pain 2019, 23, 1083–1090. [CrossRef]
- Stambaugh, J.; Morrissey, P.; Hurvitz, A.; Bernstein, E.; Barlow, B. Hip-spine relationship in femoroacetabular impingement: Does hip arthroscopy affect pelvic mobility? Clin. Orthop. Relat. Res. 2025, 483, 846–852. [CrossRef]
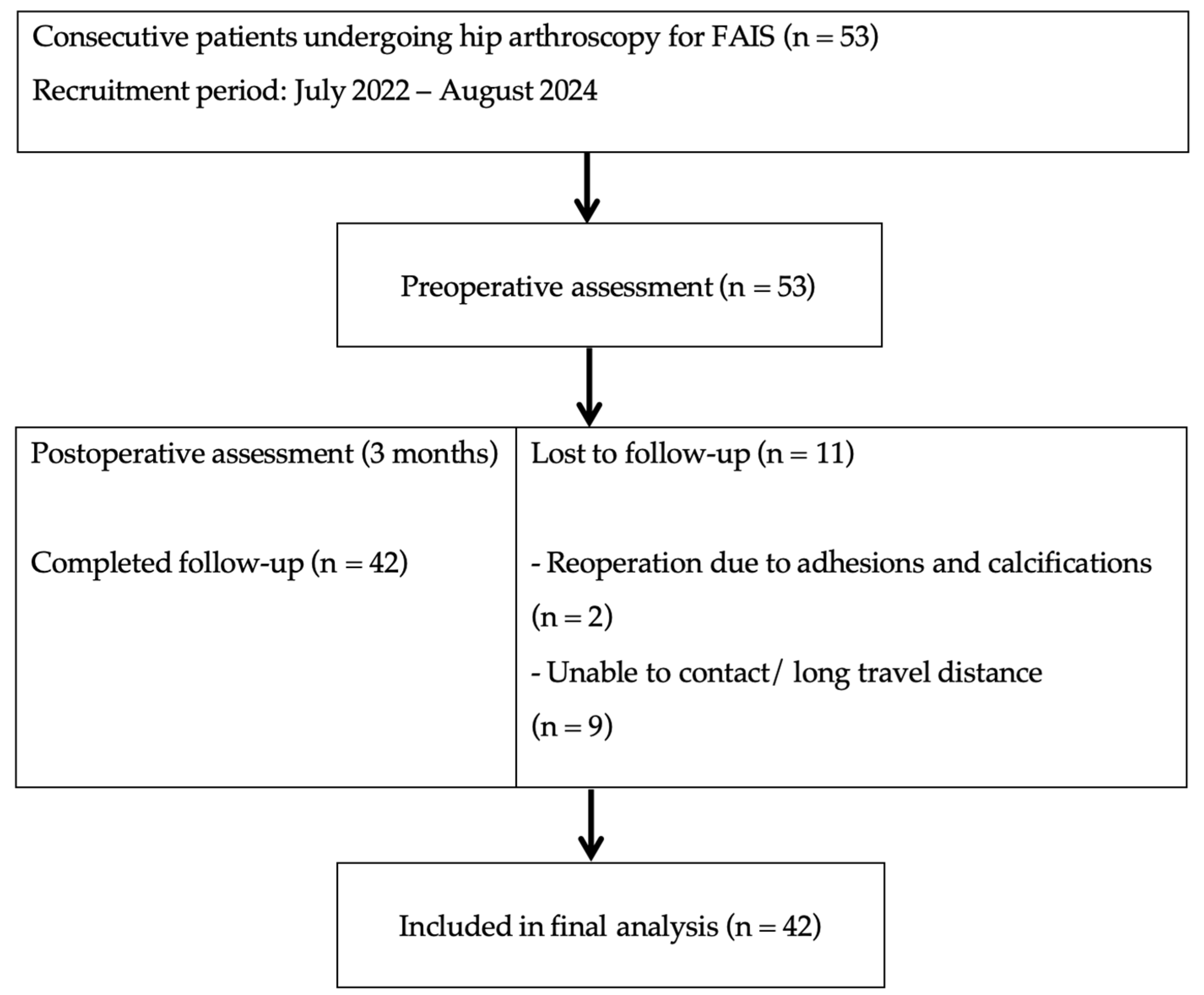
| Variable | Study group (n=42) |
| Sex/men (%, n) | 64.3 (27) |
| mean± SD | |
| Age (years) | 36.0 ± 9.2 |
| Weight (kg) | 74.1 ± 13.5 |
| Height (cm) | 176.0 ± 8.0 |
| BMI (kg/m2) | 23.7 ± 3.2 |
| LCEA (°) | 35.4 ± 5.0 |
| AA AP (°) | 67.4 ± 13.3 |
| AA Dunn (°) | 61.1 ± 10.9 |
| Concomitant procedure(%, n) | |
| Labrum repair | 54.8 (23) |
| Labrum reconstruction | 7.1 (3) |
| Labrum resection | 21.4 (9) |
| Microfracture | 23.8 (10) |
| Variable | Preoperation | at 3 months | p - value | Cohen’s r |
| mean ± SD | ||||
| HOOS Total | 57.3 ± 15.3 | 83.0 ± 11.3 | <0.0001 | 0.85 |
| HOOS Symptoms | 55.2 ± 19.1 | 77.3 ± 15.9 | <0.0001 | 0.68 |
| HOOS Pain | 59.4 ± 16.4 | 85.9 ± 11.0 | <0.0001 | 0.86 |
| HOOS ADL | 65.3 ± 17.8 | 91.0 ± 9.2 | <0.0001 | 0.83 |
| HOOS Sport | 43.6 ± 21.6 | 77.1 ± 16.9 | <0.0001 | 0.80 |
| HOOS QOL | 31.7 ± 14.1 | 57.3 ± 21.9 | <0.0001 | 0.76 |
|
ROM(°) |
Hip | Preoperation |
at 3 months |
F | p - value (interaction) |
| mean ± SD | |||||
| Flexion |
Operated | 98.1 ± 8.7 | 99.6 ± 8.6 | 1.90 | 0.1720 |
| Non-operated | 102.1 ± 8.3 | 102.5 ± 8.0 | |||
| External rotation | Operated | 37.4 ± 10.2 | 40.9 ± 8.3 | 11.55 | 0.0010 |
| Non-operated | 43.4 ± 9.1 | 43.2 ± 8.6 | |||
| Internal rotation |
Operated | 19.6 ± 11.9 | 26.3 ± 8.7 | 36.10 | <0.0001 |
| Non-operated | 29.0 ± 9.3 | 29.2 ± 8.5 | |||
| Total rotation | Operated | 57.1 ± 14.5 | 67.2 ± 11.6 | 60.09 | <0.0001 |
| Non-operated | 72.4 ± 11.1 | 72.3 ± 10.3 | |||
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




