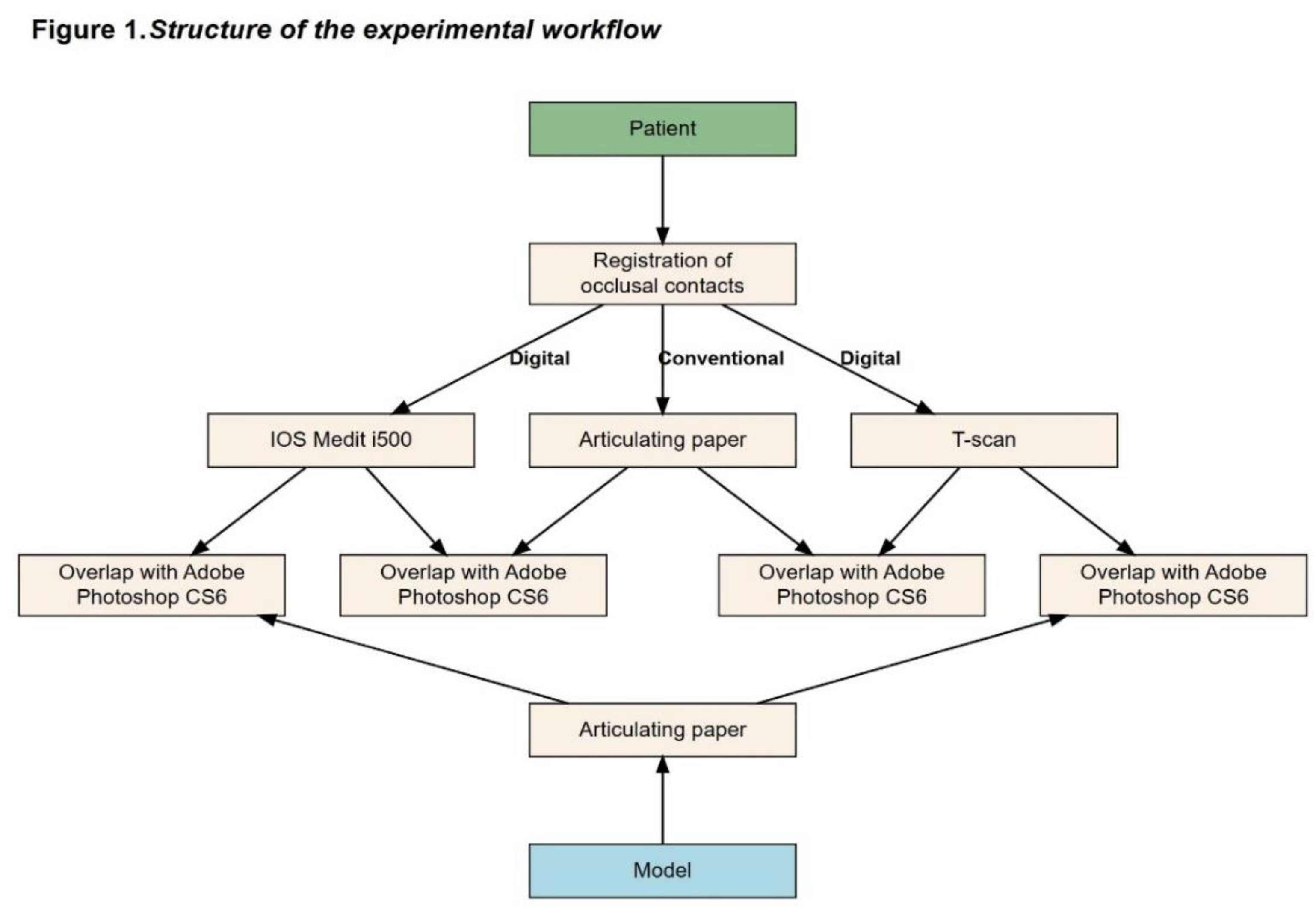
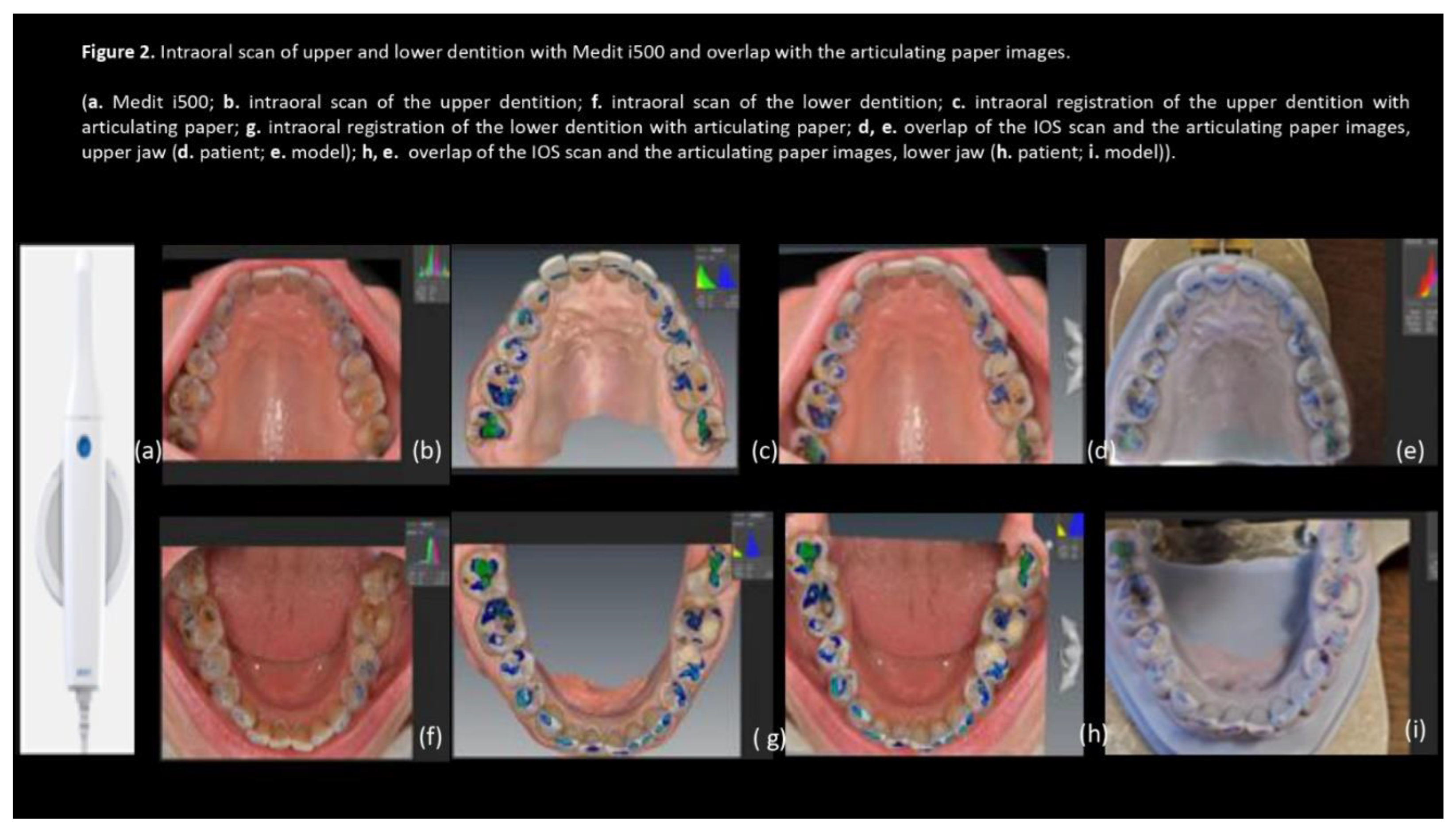
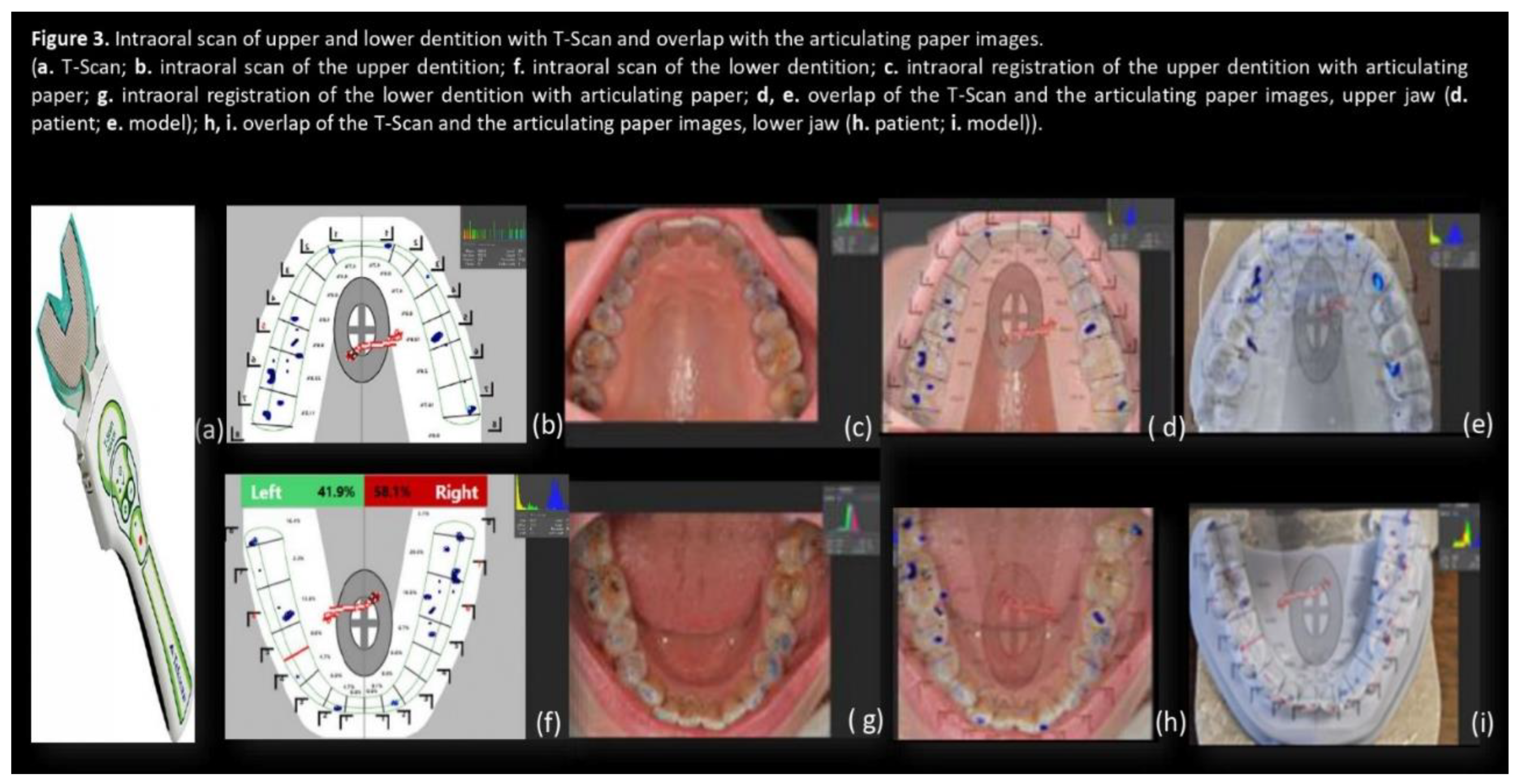
3. Results
Table 1 provides a summary of the mean values and standard deviations for the occlusal contact areas of both the upper and lower arches, as established by the different methods used.
The highest average occlusal contact area coverage in the maxilla is with the Articulating paper method (4540 pixels), followed by Articulating paper with Medit i500 (4345 pixels), and Medit i500 (3430 pixels). The three higher values are registered intraorally on a patient. The standard deviation is also highest for articulating paper and patient, because we have a significant difference between the reported values by color (according to the intensity of contact), which means that we have a serious variation. With Medit i500 we also have a considerable variation, while in Articulating paper with Medit i500 we have less variation and a large average area of coverage, which indicates higher consistency of the method. With a model, the highest coverage is recorded with Articulating paper and Medit i500 (2903 pixels), followed by Articulating paper with T-Scan. The standard deviation is highest for Articulating paper with T-Scan, followed by Articulating paper with Medit i500.
In the lower jaw, we observe the highest average occlusal contact area of coverage registered intraorally on a patient with the Medit i500 (4875 pixels). This method also has the highest standard deviation of 2281 pixels. The T-Scan method has the lowest coverage, as well as the lowest standard deviation, and this is also observed in the upper jaw. In the model, the highest average coverage (2314 pixels) is observed in the overlap of articulating paper with Medit i500, followed by articulating paper (2272 pixels) with the variation there also being higher. The average values reported for each of the three methods used on the model and the patient are similar.
To test for a statistically significant difference in the mean values of occlusal contact area overlap, we used the paired t-test because the study design included multiple measurements on one patient. The method is good when comparing the parameters of several methods that are used on the same subject or sample, which eliminates individual effects and focuses on the differences in the method. All possible pairs of methods examining the maxilla and the mandible were assessed. The adopted significance level was
Table 2 and
Table 3 illustrate the results.
The results of the paired t-tests show significant statistical differences in the mean values of the measurements on the patient’s upper jaw, at 95% confidence interval, between T-Scan and Medit i500 and between Articulating paper & T-Scan and Articulating paper & Medit i500. That is, the average area covered by T-Scan and Medit i500 has a statistically significant difference in the three measurements in terms of the intensity of the contacts expressed in colors. The area covered by Medit i500 is on average 2766.33 pixels larger than that covered by T-Scan. In regard to the patient’s upper jaw, there is statistically significant difference, at level of agreement , when comparing Articulating paper & T-Scan and Articulating paper & Medit i500. The average difference is 3573 pixels in favor of Articulating paper & Medit i500.
When examining the average values of the pixels covered by the different methods regarding the model, no statistically significant differences are found at a 95% confidence interval. If we use a 90% confidence interval, there is a statistically significant difference between Articulating paper and Articulating paper and Medit i500, with the second method having a larger average coverage by 1749.67 pixels (
Table 2).
The results of the paired t-tests on the patient’s lower jaw show that the only statistically significant difference, at a 95% confidence interval, is between T-Scan and Medit i500, with Medit i500 managing to cover an average of 4182.33 pixels more than T-Scan on the patient’s lower jaw (
Table 3). In the model, setting a 95% confidence interval, there are no statistical differences between the three groups of examinations, only at a 90% confidence interval there is a statistically significant difference between Articulating paper and T-Scan and Articulating paper and Medit i500. The former method covers an average of 1528 pixels more than the latter when examining the model’s lower jaw.
The next statistical method we used was the two-way dispersion model (two-way ANOVA). It has more power than paired t-tests because it significantly reduces the risk of accumulating type I error to reject the null hypothesis when it is true. It also includes two factors that can explain the differences in the registered occlusal contact area—regarding the color and the measurement method, which makes the estimate more accurate and reduces stochastic error. First, we tested the relationship between the type of method used and the color of the registered contacts in the patient’s upper jaw (
Table 4).
The table shows that at least one measurement method on a patient has a statistically significant difference in the reported pixel coverage. The color is not statistically significant at the selected 95% confidence interval. With a model with a 90% confidence interval, we have a statistically significant difference in at least one of the three pairs of measurement methods, and at 95% confidence, we have a statistically significant difference in at least one of the pairs of colors.
To accurately determine the differences in the mean values between the method groups and their statistical significance, we applied Fisher’s LSD post-hoc test. Since the number of measurements in our study is not large, we chose this method because it is less conservative than Tukey’s and is preferred for detecting small but statistically significant differences between objects.
Table 5 presents Fisher’s post-hoc analysis for the upper jaw of a patient and a model, and for the model, the contrasts in regard to the color are also given, since this turns out to be statistically significant.
In the Fisher's post-hoc test on a patient, we see that at 95% confidence interval, there are statistically significant differences in the average pixel coverages for the following pairs of applied methods:
Articulating paper–Articulating paper & T-Scan—on average, 3768 pixels more for Articulating paper, which is our control group;
Articulating paper & Medit i500–Articulating paper & T-Scan—on average, 3681 pixels more for Articulating paper and Medit i500;
Articulating paper–T-Scan—on average, 3573 pixels more coverage of the upper jaw with Articulating paper than with T-Scan.
We also have several significant pair differences at 90% confidence interval:
Articulating paper & T-Scan–Medit i500—on average, 2658 pixels more coverage with Medit i500 than with Articulating paper & T-Scan;
Medit i500–T-Scan—on average, 2766 pixels more coverage for Medit i500 than for T-Scan.
In the model, we have one statistically significant difference, at 95% confidence interval, between Articulating paper and Articulating paper with Medit i500, with the second method covering on average 1750 pixels more of the occlusal contact area than that registered with Articulating paper alone. In the contact area registered by colors, according to intensity, we have two statistically significant differences at 95% confidence interval and one at 90% confidence interval. The following pairs are with the ones registered at the higher confidence interval:
blue–green color—the average difference in the occlusal area is 1596 pixels more for the green color;
green–red color—here the difference reported is the largest, the occlusal area covered by the green color is, on average, by 2890 pixels larger than the red area.
At 90% confidence interval, we can say that there is a statistically significant difference between the blue and red coverage areas, with the blue area being, on average, by 1294 pixels larger than the red area (
Table 5).
To see the expected values of the marginal means, for the different methods applied to the mandibular model and patient’s lower jaw, we used a two-way analysis of variance, at a 95% confidence interval.
Table 6 illustrates the results.
The data demonstrate that at least one of the applied measurement methods on a patient has a statistically significant difference, at the selected 95% confidence interval. Here, the color does not come out statistically significant. In the model, no statistically significant difference in the coverage of the occlusal area is established; such is reported only in terms of colors, at a 95% confidence interval. The results from post-hoc test can be seen in
Table 7.
When reporting the results regarding the occlusal coverage of the mandible in a patient, at a 95% confidence interval, the following two pairs of methods are statistically significant:
Articulating paper & T-Scan–Medit i500, with Medit i500 covering an average of 3494 pixels more than Articulating paper with T-Scan;
Medit i500–T-Scan, with Medit i500 covering an average of 4182 pixels more occlusal area than T-Scan.
At a 90% confidence interval, we find statistically significant differences between:
Articulating paper–T-Scan—the coverage of the Articulating paper is, on average, 2295 pixels more compared to T-Scan;
Articulating paper & Medit i500–Medit i500—Medit i500 alone covers an average of 2354 pixels more than Articulating paper combined with Medit i500.
Observing the model, the statistically significant differences in the means, in regard to color, are between the groups: blue–green and green–red, at 95% confidence interval. In the first group the green covers an average of 2141 pixels more than the blue, and in the second group the green covers an average of 2401 pixels more than the red (
Table 7).
Finally, a comparison of the applied occlusal registration methods was conducted by means of a three-way ANOVA analysis (
Table 8).
To check whether there is a statistically significant difference between the registered occlusal contacts by the new articulator (Prototype) and the other methods, the reported results in the last column Pr(>F) were observed. The focus was on values greater than 0.05 and it was found that for the upper jaw the p-value for Prototype is 0.10798 and for the lower jaw it is 0.34941, from which a conclusion is drawn that no statistically significant difference exists between the measurements made with the new device and the other methods, which proves its reliability. Regarding the influence of the factors (Prototype:Method), the results are again good, with the value reported for the upper jaw being 0.05579, which is still above 0.05, and for the lower jaw it is 0.91576. A conclusion can be drawn that the new device performs consistently, regardless of the chosen registration method, especially for the lower jaw.
In
Table 8. the Color factor (contact intensity) is also reported with an asterisk (*), and the p-values are below 0.05 (0.02798 for the upper and 0.01696 for the lower jaw). Here, the reason for the statistically significant differences, at 95% confidence interval, is in the strength of the contacts. It is normal to observe differences there; such were also reported in the two-way variance analyses. From the results in the Mean Sq column, we can assess the precision of the studied prototype for each jaw separately. For the upper jaw the reported value is 6,452,429, and for the lower jaw—1,144,584. Therefore, the precision of the prototype is significantly higher for the lower jaw, because the value is nearly 5.63 times lower than that for the upper one, and in statistics the lower value of Mean Sq indicates less dispersion and higher measurement accuracy.
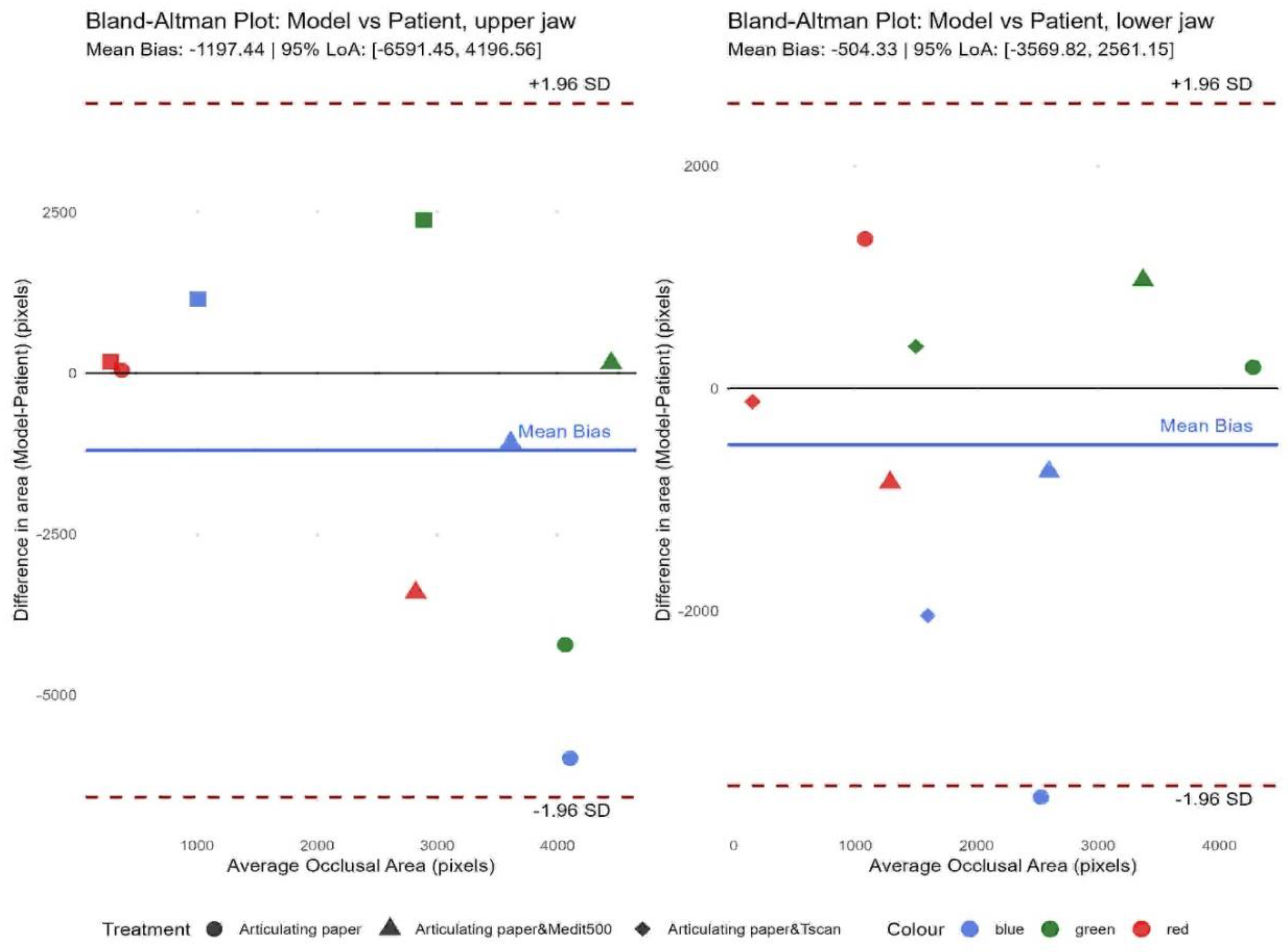
To visualize the differences between the model and the patient, according to the methods used and the three colors of occlusal coverage, we applied the Bland-Altman method (
Figure 4). The graph presents the measured occlusal area in the model and the patient with the three applied methods—Articulating paper, Articulating paper with Medit i500, and Articulating paper with T-Scan, with the left part referring to the maxilla and the right part—to the mandible.
Figure 4 demonstrates that the limits of agreement between the model and the patient are quite wide, with the average difference being 1197 pixels, which signifies that the methods used cover an occlusal contact area in the upper jaw, which is, on average, 1197 pixels larger in the patient than in the model. Despite the differences registered, the observations do not exceed the limits of agreement (the red dashed lines), which proves the reliability of the device. In the lower jaw, an even smaller average difference is observed between the measurements in the patient and the model (504.33 pixels), and they are also within the limit of agreement, at 95% confidence interval. We have only one measurement (with articulating paper, blue color) slightly above the lower limit, but since this is our control, the result does not compromise the reliability of the device.
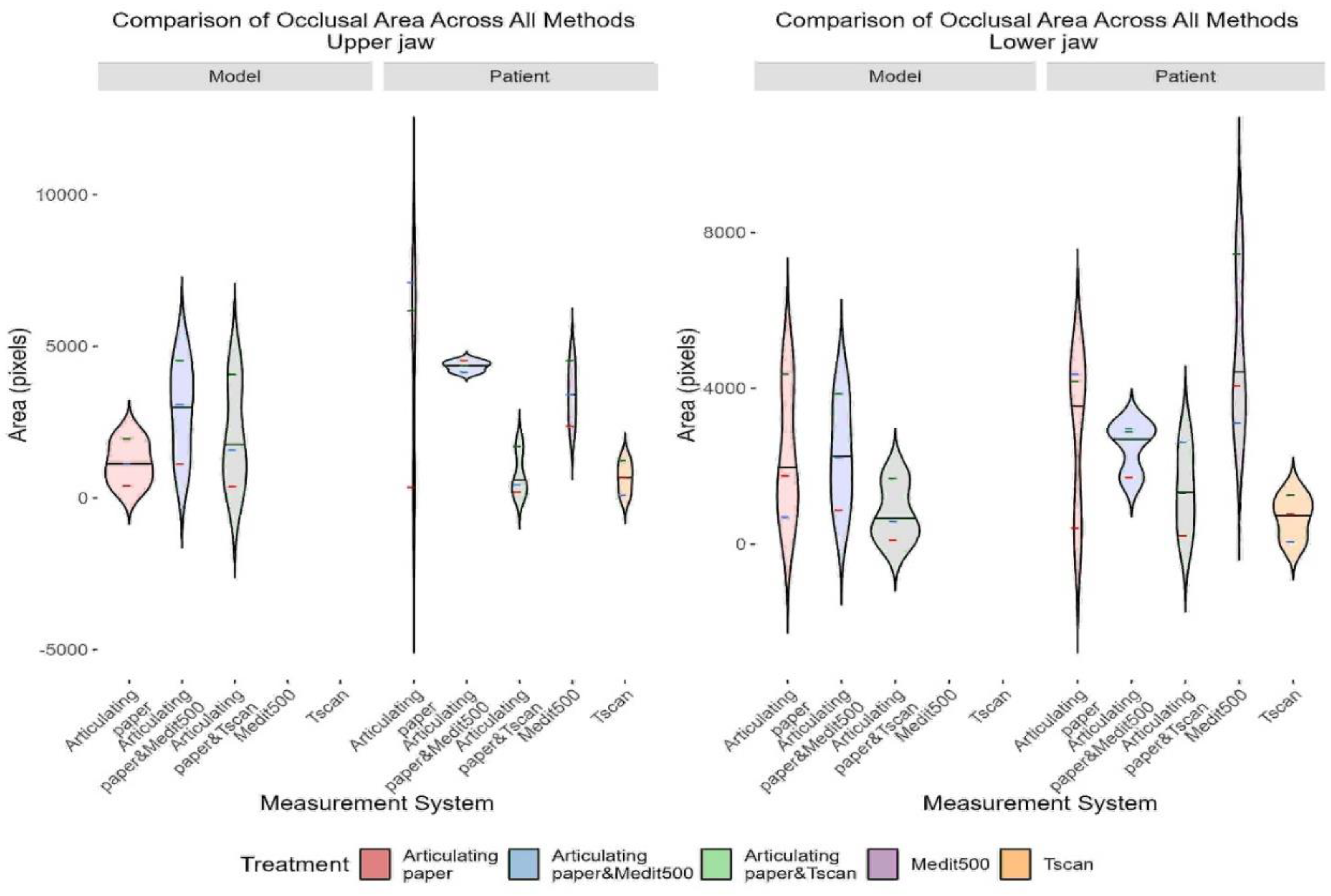
The distribution of the occlusal contact area as per the different methods used was visualized by a violin plot, with the three horizontal dashed lines (colored green, blue, and red) being the arithmetic means of the coverage area for the corresponding colors, with the specified method. The graph is divided into two parts—relative to the model and relative to the patient, with the data for the upper jaw being presented on the left side and that for the lower jaw—on the right (
Figure 5).
The vertical axis represents the measured area in pixels, and the horizontal axis—the applied methods (alone and in combination). In the left part of the graph we see that the most significant difference when comparing the covered area between model and patient is with the articulating paper. In the patient there is much larger coverage by green and blue colors, while for the red it is almost the same as in the model. For Articulating paper with Medit i500 and with T-Scan we have close values of color coverage, especially in Articulating paper with T-Scan, which shows that the upper jaw model has similar coverage with these two methods. In the patient we have the largest occlusal coverage with articulating paper (blue and green colors). In the other two methods we also have very similar coverage for three colors. The right part of the graph, representing the occlusal contact area of the lower jaw is identical, which once again confirms the reliability of the new device.
In conclusion, we can summarize that the results of the comparative laboratory measurement of occlusal contacts registered using articulating paper and the T-Scan and Medit i500 systems have good overlap.