Submitted:
09 April 2026
Posted:
11 April 2026
You are already at the latest version
Abstract
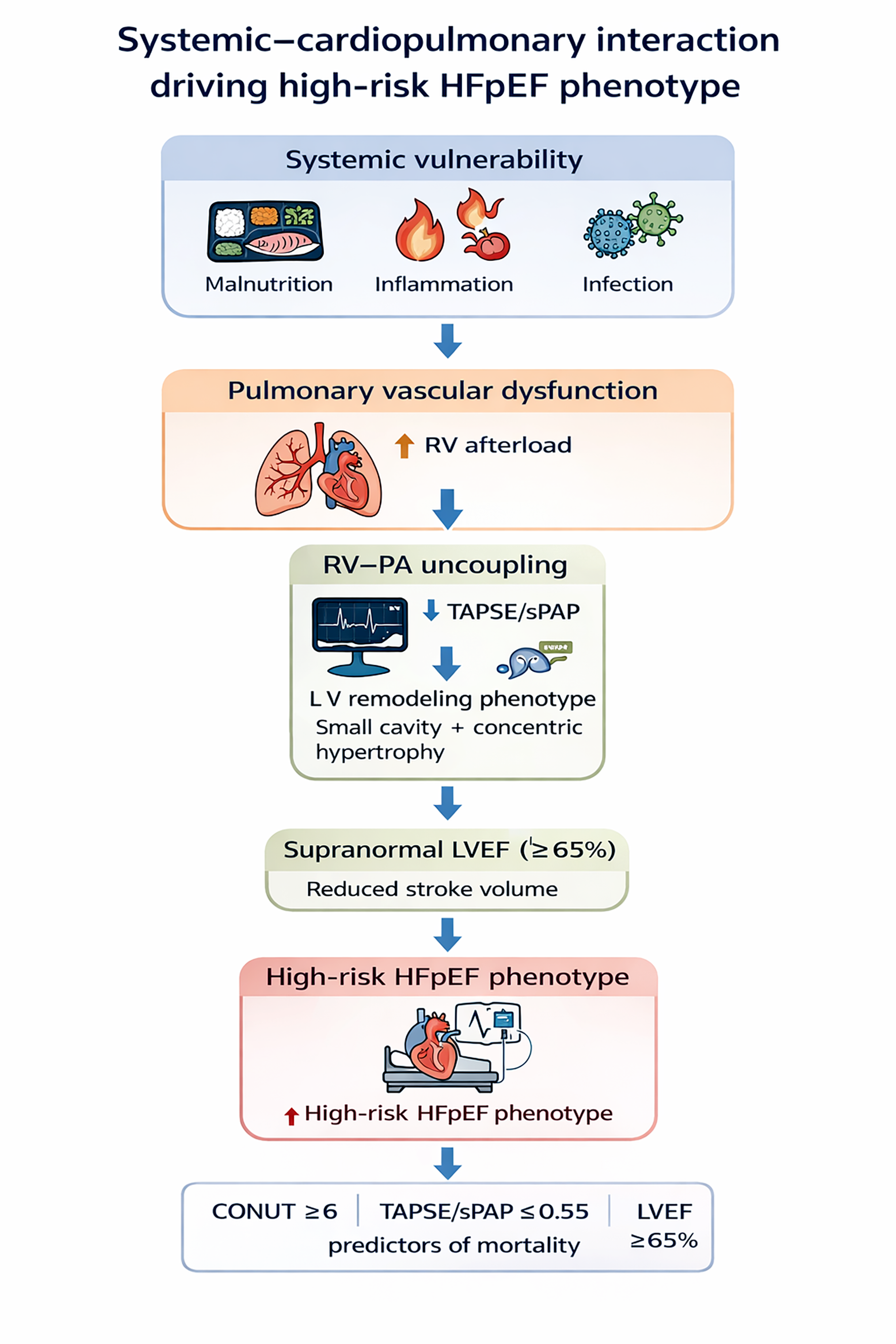
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Population
2.2. Data Collection
2.3. Laboratory Assessment
2.4. Nutritional Risk Scores
2.5. Echocardiographic Assessment
2.6. Follow-Up and Outcome Definition
2.7. Statistical Analysis
2.8. Ethical Approval
2.9. Use of Artificial Intelligence Tools
3. Results
3.1. Baseline Characteristics
3.2. Laboratory Findings and Nutritional Scores
3.3. Instrumental Findings
3.4. Clinical Characteristics, Causes of Admission, and In-Hospital Treatment
3.5. Follow-Up and Clinical Events
3.6. Univariate and Multivariate Cox Regression Analysis
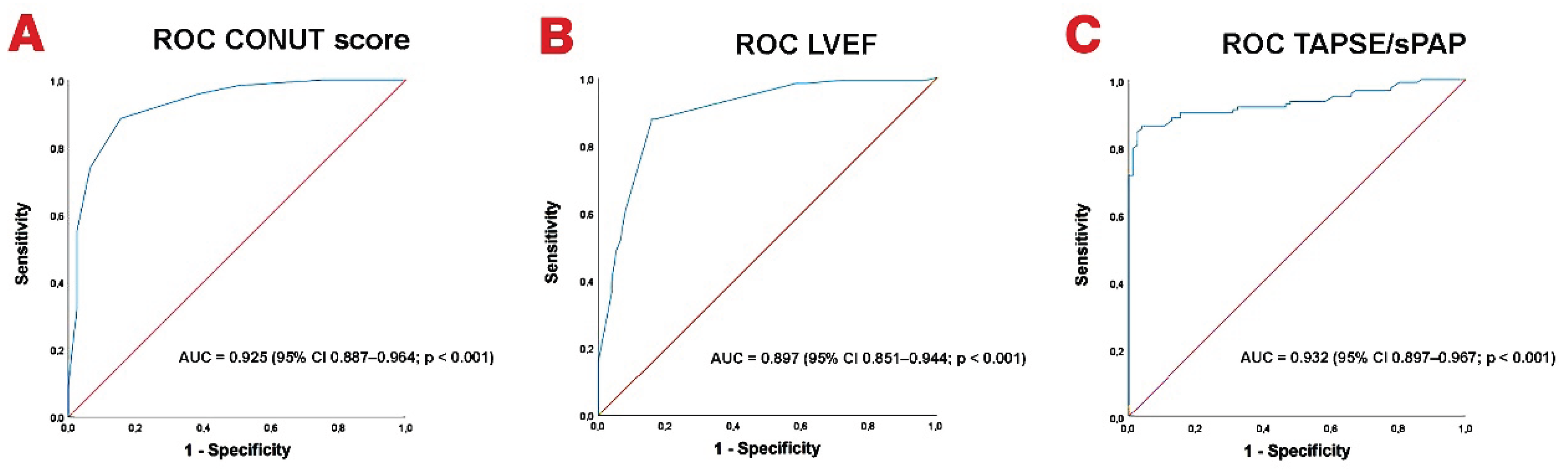
3.7. ROC Analysis
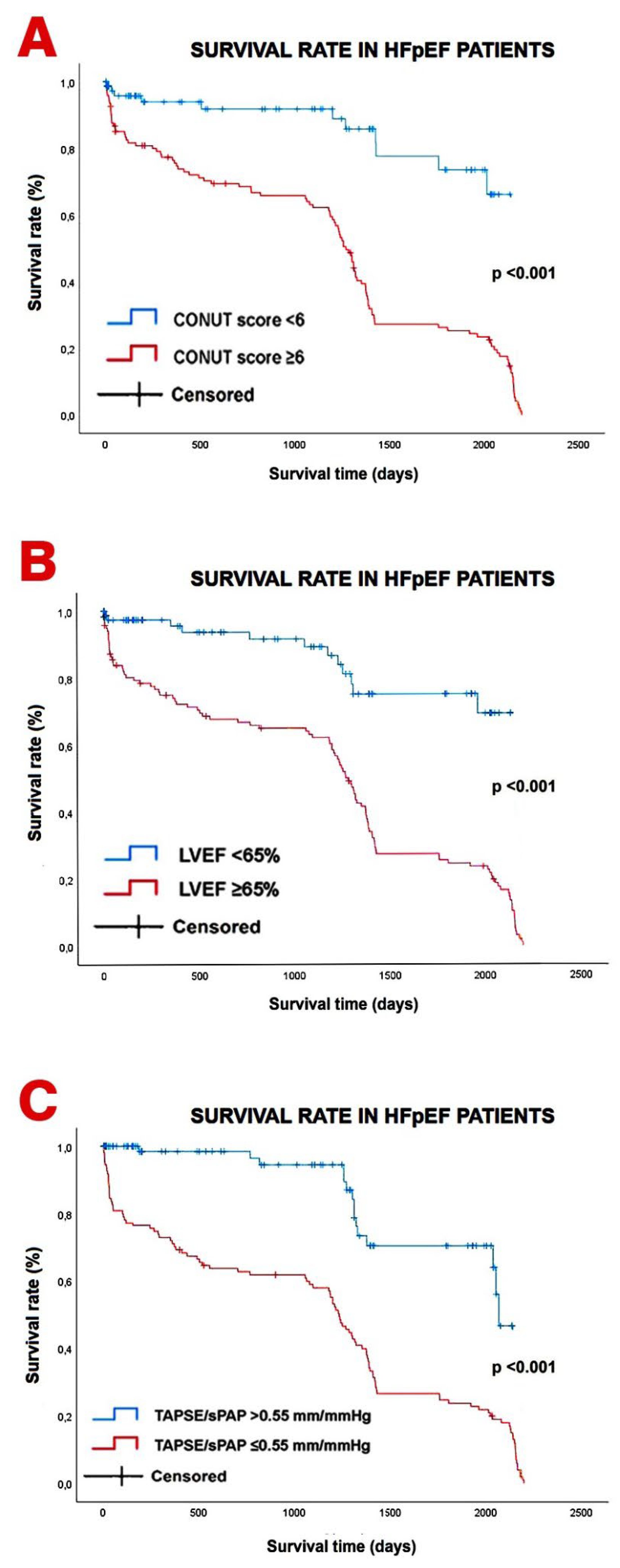
3.8. Kaplan–Meier Survival Analysis
4. Discussion
4.1. Principal Findings
4.2. Interpretation of Findings and Comparison with Previous Studies
4.3. Clinical Implications
4.4. Strengths and Limitations
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Savarese, G.; Becher, P.M.; Lund, L.H.; Seferovic, P.; Rosano, G.M.C.; Coats, A.J.S. Global burden of heart failure: A comprehensive and updated review of epidemiology. Cardiovasc. Res. 2023, 118, 3272–3287. [Google Scholar]
- Montalto, M.; D’Ignazio, F.; Camilli, S.; Di Francesco, S.; Fedele, M.; Landi, F.; Gallo, A. Heart failure in older patients: An update. J. Clin. Med. 2025, 14, 1982. [Google Scholar] [CrossRef] [PubMed]
- Gu, J.; Zheng, Z.; Li, J.; Wu, S.; Sun, H.; Pang, J.; Chen, Y. Global burden of heart failure in older adults: Trends, socioeconomic inequalities, and future projections from 1990 to 2035. Eur. Heart J. Qual. Care Clin. Outcomes 2025, 11, 1123–1136. [Google Scholar] [CrossRef] [PubMed]
- Gök, G.; Zoghi, M.; Sinan, Ü.Y.; Kılıç, S.; Tokgözoğlu, L. Elder-Turk Study Investigators. Demographics of patients with heart failure who were over 80 years old and were admitted to the cardiology clinics in Turkey. Anatol. J. Cardiol. 2019, 21, 196–205. [Google Scholar] [PubMed]
- Boully, C.; Vidal, J.S.; Guibert, E.; Ghazali, F.N.; Pesce, A.; Beauplet, B.; Roger, J.D.; Carrière, I.; Timbely, B.; Idiri, H.; et al. National survey on the management of heart failure in individuals over 80 years of age in French geriatric care units. BMC Geriatr. 2019, 19, 204. [Google Scholar] [CrossRef]
- Svahn, S.; Appelblad, L.; Lövheim, H.; Gustafson, Y.; Olofsson, B.; Gustafsson, M. Prevalence of heart failure and trends in its pharmacological treatment between 2000 and 2017 among very old people. BMC Geriatr. 2024, 24, 701. [Google Scholar] [CrossRef]
- de Boer, R.A.; Abdellatif, M.; Bauersachs, J.; Roger, V.L. Heart failure in the elderly: Epidemiology, mechanisms, and management. Eur. Heart J. 2026, 47, ehag110. [Google Scholar] [CrossRef]
- Upadhya, B.; Kitzman, D.W. Heart failure with preserved ejection fraction in older adults. Heart Fail. Clin. 2017, 13, 485–502. [Google Scholar]
- Tromp, J.; Shen, L.; Jhund, P.S.; Anand, I.S.; Carson, P.E.; Desai, A.S.; Granger, C.B.; Komajda, M.; McKelvie, R.S.; Pfeffer, M.A.; et al. Age-related characteristics and outcomes of patients with heart failure with preserved ejection fraction. J. Am. Coll. Cardiol. 2019, 74, 601–612. [Google Scholar]
- Kobak, K.A.; Zarzycka, W.; Chiao, Y.A. Age and sex differences in heart failure with preserved ejection fraction. Front. Aging 2022, 3, 811436. [Google Scholar] [CrossRef]
- Gharagozloo, K.; Mehdizadeh, M.; Heckman, G.; Rose, R.A.; Howlett, J.; Howlett, S.E.; Nattel, S. Heart failure with preserved ejection fraction in the elderly population: Basic mechanisms and clinical considerations. Can. J. Cardiol. 2024, 40, 1424–1444. [Google Scholar] [CrossRef]
- Juillière, Y.; Venner, C.; Filippetti, L.; Popovic, B.; Huttin, O.; Selton-Suty, C. Heart failure with preserved ejection fraction: A systemic disease linked to multiple comorbidities, targeting new therapeutic options. Arch. Cardiovasc. Dis. 2018, 111, 766–781. [Google Scholar] [CrossRef] [PubMed]
- Roh, J.; Hill, J.A.; Singh, A.; Valero-Muñoz, M.; Sam, F. Heart failure with preserved ejection fraction: Heterogeneous syndrome, diverse preclinical models. Circ. Res. 2022, 130, 1906–1925. [Google Scholar] [CrossRef] [PubMed]
- Epelde, F. Heterogeneity in heart failure with preserved ejection fraction: A systematic review of phenotypic classifications and clinical implications. J. Clin. Med. 2025, 14, 4820. [Google Scholar] [CrossRef] [PubMed]
- Ather, S.; Chan, W.; Bozkurt, B.; Aguilar, D.; Ramasubbu, K.; Zachariah, A.A.; Wehrens, X.H.; Deswal, A. Impact of noncardiac comorbidities on morbidity and mortality in a predominantly male population with heart failure and preserved versus reduced ejection fraction. J. Am. Coll. Cardiol. 2012, 59, 998–1005. [Google Scholar]
- Rakisheva, A.; Soloveva, A.; Shchendrygina, A.; Giverts, I. Heart failure with preserved ejection fraction and frailty: From young to superaged coexisting HFpEF and frailty. Int. J. Heart Fail. 2024, 6, 93–106. [Google Scholar]
- Radakrishnan, A.; Agrawal, S.; Singh, N.; Barbieri, A.; Shaw, L.J.; Gulati, M.; Lala, A. Underpinnings of heart failure with preserved ejection fraction in women—From prevention to improving function. Am. J. Prev. Cardiol. 2025, 23, 100928. [Google Scholar] [CrossRef]
- Tanacli, R.; Trivedi, R.K.; Tajdini, M.; Jani, V.; Tian, J.; Hahn, V.S.; Vaishnav, J.; Damluji, A.A.; Gerstenblith, G.; Buta, B.; et al. Frailty status predicts adverse outcomes in ambulatory heart failure with preserved ejection fraction. JACC Adv. 2026, 5, 102560. [Google Scholar]
- Schiattarella, G.G.; Alcaide, P.; Condorelli, G.; Gillette, T.G.; Heymans, S.; Jones, E.A.V.; Kallikourdis, M.; Lichtman, A.; Marelli-Berg, F.; Shah, S.; et al. Immunometabolic mechanisms of heart failure with preserved ejection fraction. Nat. Cardiovasc. Res. 2022, 1, 211–222. [Google Scholar] [CrossRef]
- Talha, K.M.; Pandey, A.; Fudim, M.; Butler, J.; Anker, S.D.; Khan, M.S. Frailty and heart failure: State-of-the-art review. J. Cachexia Sarcopenia Muscle 2023, 14, 1959–1972. [Google Scholar]
- Zainul, O.; Perry, D.; Pan, M.; Lau, J.; Zarzuela, K.; Kim, R.; Konerman, M.C.; Hummel, S.L.; Goyal, P. Malnutrition in heart failure with preserved ejection fraction. J. Am. Geriatr. Soc. 2023, 71, 3367–3375. [Google Scholar] [CrossRef] [PubMed]
- Zhou, R.; Xia, Y.Y.; Li, Z.; Wu, L.D.; Shi, Y.; Ling, Z.Y.; Zhang, J.X. HFpEF as systemic disease: Insight from a diagnostic prediction model reminiscent of systemic inflammation and organ interaction in HFpEF patients. Sci. Rep. 2024, 14, 5386. [Google Scholar] [CrossRef]
- Gorica, E.; Geiger, M.A.; Di Venanzio, L.; Atzemian, N.; Kleeberger, J.A.; Grigorian, D.; Mongelli, A.; Emini Veseli, B.; Mohammed, S.A.; Ruschitzka, F.; et al. Cardiometabolic heart failure with preserved ejection fraction: From molecular signatures to personalized treatment. Cardiovasc. Diabetol. 2025, 24, 265. [Google Scholar] [CrossRef] [PubMed]
- Wang, B.; Jankauskas, S.S.; Mone, P.; Varzideh, F.; Santulli, G. Immunology of heart failure with preserved ejection fraction. Expert Rev. Clin. Immunol. 2025, 21, 1725–1739. [Google Scholar] [CrossRef] [PubMed]
- Liu, J.; Liu, J.; Wang, J.; Yan, Z.; Liang, Q.; Wang, X.; Wang, Z.; Liu, M.; Luan, X. Prevalence and impact of malnutrition on readmission among hospitalized patients with heart failure in China. ESC Heart Fail. 2022, 9, 4271–4279. [Google Scholar]
- Bansal, N.; Alharbi, A.; Shah, M.; Altorok, I.; Assaly, R.; Altorok, N. Impact of malnutrition on the outcomes in patients admitted with heart failure. J. Clin. Med. 2024, 13, 4215. [Google Scholar] [CrossRef]
- Abe, Y.; Horiuchi, Y.; Akiho, M.; Kimura, M.; Tanaka, H.; Tanaka, J.; Aoki, J.; Tanabe, K. Prognostic significance of malnutrition and physical function in patients with heart failure. Circ. Rep. 2025, 7, 904–912. [Google Scholar] [CrossRef]
- Knobloch, I.D.S.; Zucatti, K.P.; de Carvalho, B.Z.O.; da Costa-Pereira, J.P.; Hartmann, A.S.; Razzera, E.L.; Vale, M.D.M.; Souza, G.C.; Silva, F.M. Prevalence of malnutrition and its association with outcomes in heart failure: A systematic review and meta-analysis. Nutrition 2025, 28 140, 112913. [Google Scholar] [CrossRef]
- Esteban-Fernández, A.; Villar-Taibo, R.; Alejo, M.; Arroyo, D.; Bonilla Palomas, J.L.; Cachero, M.; Joaquin, C.; Méndez Bailón, M.; Pérez-Rivera, J.Á.; Romero-Vigara, J.C.; et al. Diagnosis and management of malnutrition in patients with heart failure. J. Clin. Med. 2023, 12, 3320. [Google Scholar] [CrossRef]
- Maeda, D.; Fujimoto, Y.; Nakade, T.; Abe, T.; Ishihara, S.; Jujo, K.; Matsue, Y. Frailty, sarcopenia, cachexia, and malnutrition in heart failure. Korean Circ. J. 2024, 54, 363–381. [Google Scholar] [CrossRef]
- Liu, M.; Chen, H.; Zhang, F.; Liu, S.; Sun, X.; Xu, Y.; Wu, R.; Chen, L.; Xiong, X. Factors influencing malnutrition in patients with heart failure: A scoping review based on the biopsychosocial model. Risk Manag. Healthc. Policy 2025, 18, 4011–4026. [Google Scholar] [CrossRef] [PubMed]
- Verdu-Rotellar, J.M.; Calero, E.; Duran, J.; Navas, E.; Alonso, S.; Argemí, N.; Casademunt, M.; Furió, P.; Casajuana, E.; Vinyoles, E.; et al. Impact of malnutrition on the quality of life in older patients with advanced heart failure: A cohort study. Rev. Clin. Esp. 2024, 224, 105–113. [Google Scholar] [CrossRef] [PubMed]
- Noda, T.; Maekawa, E.; Maeda, D.; Uchida, S.; Yamashita, M.; Hamazaki, N.; Nozaki, K.; Saito, H.; Saito, K.; Ogasahara, Y.; et al. Prevalence and prognostic value of cachexia diagnosed by new definition for Asian people in older patients with heart failure. J. Cachexia Sarcopenia Muscle 2024, 15, 2660–2668. [Google Scholar] [CrossRef]
- El-Sheikh, M.; El Caidi, N.O.; Kandiah, A.; Tonning, S.H.; Taraldsen, I.A.; Wisborg, F.D.; Andersen, O.; Hove, J.D.; Grand, J. Prevalence and prognostic significance of malnutrition assessed by two scoring systems in hospitalised elderly patients with chronic heart failure. Card. Fail. Rev. 2025, 11, e26. [Google Scholar] [CrossRef] [PubMed]
- Chen, M.Y.; Wen, J.X.; Lu, M.T.; Jian, X.Y.; Wan, X.L.; Xu, Z.W.; Liang, J.Q.; Wu, J.D. Association between prognostic nutritional index and prognosis in patients with heart failure: A meta-analysis. Front. Cardiovasc. Med. 2022, 9, 918566. [Google Scholar] [CrossRef]
- Yoshihisa, A.; Kanno, Y.; Watanabe, S.; Yokokawa, T.; Abe, S.; Miyata, M.; Sato, T.; Suzuki, S.; Oikawa, M.; Kobayashi, A.; et al. Impact of nutritional indices on mortality in patients with heart failure. Open Heart 2018, 5, e000730. [Google Scholar] [CrossRef]
- Zhang, X.; Zhang, J.; Liu, F.; Li, W.; Zhang, T.; Fang, B.; Zhang, Z.; Xie, Q.; Yang, Y.; Li, X. Prognostic nutritional index as a predictor in patients with metabolic syndrome and heart failure. Diabetes Metab. Syndr. Obes. 2023, 16, 2503–2514. [Google Scholar] [CrossRef]
- Solano, S.; Yang, M.; Tolomeo, P.; Kondo, T.; Shen, L.; Jhund, P.S.; Anand, I.S.; Desai, A.S.; Lam, C.S.P.; Maggioni, A.P.; et al. Clinical characteristics and outcomes of patients with heart failure with preserved ejection fraction and with reduced ejection fraction according to the prognostic nutritional index: Findings from PARADIGM-HF and PARAGON-HF. J. Am. Heart Assoc. 2025, 14, e037782. [Google Scholar] [CrossRef]
- Lo Buglio, A.; Bellanti, F.; Capurso, C.; Vendemiale, G. Controlling nutritional status (CONUT) score as a predictive marker in hospitalized frail elderly patients. J. Pers. Med. 2023, 13, 1119. [Google Scholar] [CrossRef]
- Di Vincenzo, O.; D’Elia, L.; Ballarin, G.; Pasanisi, F.; Scalfi, L. Controlling nutritional status (CONUT) score and the risk of mortality or impaired physical function in stroke patients: A systematic review and meta-analysis. Nutr. Metab. Cardiovasc. Dis. 2023, 33, 1501–1510. [Google Scholar] [CrossRef]
- Fărcaș, D.A.; Cerghizan, A.; Maior, R.; Mîndrilă, A.C.; Tarcea, M. CONUT score as a predictor of mortality risk in acute and chronic heart failure: A meta-analytic review. Nutrients 2025, 17, 1736. [Google Scholar] [CrossRef]
- Takada, T.; Jujo, K.; Inagaki, K.; Abe, T.; Kishihara, M.; Shirotani, S.; Endo, N.; Watanabe, S.; Suzuki, K.; Minami, Y.; et al. Nutritional status during hospitalization is associated with the long-term prognosis of patients with heart failure. ESC Heart Fail. 2021, 8, 5372–5382. [Google Scholar] [CrossRef] [PubMed]
- Kinugasa, Y.; Sota, T.; Kamitani, H.; Nakayama, N.; Nakamura, K.; Hirai, M.; Yanagihara, K.; Kato, M.; Ono, T.; Takahashi, M.; et al. Diagnostic performance of nutritional indicators in patients with heart failure. ESC Heart Fail. 2022, 9, 2096–2106. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.; Zheng, H.; He, Y. Prognostic significance of controlling nutritional status in older adults with heart failure with preserved ejection fraction: A prospective comparative study with other objective nutritional indices. Aging Clin. Exp. Res. 2023, 35, 1305–1315. [Google Scholar] [CrossRef] [PubMed]
- Iida, Y.; Kamiya, K.; Adachi, T.; Iwatsu, K.; Kamisaka, K.; Iritani, N.; Imoto, S.; Yamada, S.; FLAGSHIP Collaborators. Prognostic impact of nutrition measures in patients with heart failure varies with coexisting physical frailty. ESC Heart Fail. 2023, 10, 3364–3372. [Google Scholar] [CrossRef]
- Xu, D.; Shen, R.; Hu, M.; Fan, Q.; Wu, J. Prognostic impact of CONUT score in older patients with chronic heart failure. BMC Geriatr. 2024, 24, 738. [Google Scholar] [CrossRef]
- Liu, S.; Fu, T.; Deng, T.; Cai, X.; Zhan, Y.; Zhu, H. Association between inflammation- and nutrition-related indicators and mortality in patients with heart failure: A cohort study. Front. Nutr. 2025, 12, 1617069. [Google Scholar] [CrossRef]
- Lu, H.; Claggett, B.L.; Minamisawa, M.; Ostrominski, J.W.; Foà, A.; Pabón, M.A.; Kalayci, A.; Vaduganathan, M.; Cikes, M.; Shah, A.M.; et al. Prognostic significance of nutritional scores in patients with heart failure: Insights from the PARAGON-HF trial. J. Am. Heart Assoc. 2025, 14, e038872. [Google Scholar] [CrossRef]
- Xie, S.; Xia, Z.; Chen, X.; Hu, H.; Lu, K.; Xiao, H. Prognostic value of CONUT, PNI, albumin, and BMI in patients with heart failure and atrial fibrillation: A retrospective cohort study. Medicine (Baltimore) 2025, 104, e44439. [Google Scholar] [CrossRef]
- Mancinetti, F.; Guazzarini, A.G.; Gaspari, M.; Croce, M.F.; Serra, R.; Mecocci, P.; Boccardi, V. Integrating nutrition, inflammation, and immunity: The CALLY index as a novel prognostic biomarker in acute geriatric care. Nutrients 2025, 17, 3192. [Google Scholar] [CrossRef]
- He, Q.; Cao, Y.; Fan, X.; Li, B.; He, Q.; Zhang, H. Long-term prognostic value of CRP-albumin-lymphocyte index in elderly patients with heart failure with preserved ejection fraction. Exp. Gerontol. 2025, 204, 112744. [Google Scholar] [CrossRef]
- Arın, C.B.; Dahir, O.F.; Adan, A.S.; Abdi, I.A.; Karataş, M. Systemic inflammatory indices and mortality risk in heart failure: A retrospective cohort study. Front. Cardiovasc. Med. 2025, 12, 1626470. [Google Scholar] [CrossRef] [PubMed]
- Zhang, N.; Zhang, S.; Xie, L.; Lu, H.; Wang, Q.; Xiong, Z.; Wu, Z.; Zhang, J.; Jian, Y.; Huang, W.; et al. Evaluating the prognostic significance of the modified prognostic nutritional index-C-reactive protein-to-albumin-to-lymphocyte index in acute decompensated heart failure: Special attention to the impact of diabetes. Front. Nutr. 2025, 12, 1636685. [Google Scholar] [CrossRef] [PubMed]
- Zhu, Y.; Wu, J.; Fu, L.; Xu, D.; Li, Y. Association of the C-reactive protein-albumin-lymphocyte index with heart failure prevalence and mortality risk in older adults with hypertension: A cohort study. J. Int. Med. Res. 2026, 54, 3000605261416756. [Google Scholar] [CrossRef] [PubMed]
- Goyani, P.; Christodoulou, R.; Vassiliou, E. Immunosenescence: Aging and immune system decline. Vaccines 2024, 12, 1314. [Google Scholar] [CrossRef]
- Amara, M.; Stoler, O.; Birati, E.Y. The role of inflammation in the pathophysiology of heart failure. Cells 2025, 14, 1117. [Google Scholar] [CrossRef]
- Palin, V.; Brown, O.; Hamilton, F.; Lillie, P.; Kearney, M.; Cubbon, R.; Drozd, M. Infection in people with heart failure: An overlooked cause of adverse outcomes. Clin. Med. 2025, 25, 100497. [Google Scholar] [CrossRef]
- Lisiak, M.; Jędrzejczyk, M.; Wleklik, M.; Lomper, K.; Czapla, M.; Uchmanowicz, I. Nutritional risk, frailty and functional status in elderly heart failure patients. ESC Heart Fail. 2025, 12, 3426–3434. [Google Scholar] [CrossRef]
- Sonaglioni, A.; Lonati, C.; Scime’, V.; Nicolosi, G.L.; Bruno, A.; Lombardo, M.; Harari, S. Supra-normal ejection fraction at hospital admission stratifies mortality risk in HFpEF patients aged ≥70 years. J. Clin. Med. 2025, 14, 426. [Google Scholar]
- Sonaglioni, A.; Lonati, C.; Tescaro, L.; Nicolosi, G.L.; Proietti, M.; Lombardo, M.; Harari, S. Prevalence and clinical outcome of main echocardiographic and hemodynamic heart failure phenotypes in a population of hospitalized patients 70 years old and older. Aging Clin. Exp. Res. 2022, 34, 1081–1094. [Google Scholar] [CrossRef]
- Sonaglioni, A.; Lonati, C.; Rigamonti, E.; Viganò, M.; Nicolosi, G.L.; Proietti, M.; Lombardo, M.; Harari, S. CHA2DS2-VASc score stratifies mortality risk in heart failure patients aged 75 years and older with and without atrial fibrillation. Aging Clin. Exp. Res. 2022, 34, 1707–1720. [Google Scholar] [CrossRef]
- McDonagh, T.A.; Metra, M.; Adamo, M.; Gardner, R.S.; Baumbach, A.; Böhm, M.; Burri, H.; Butler, J.; Čelutkienė, J.; Chioncel, O.; et al. 2021 ESC Guidelines for the diagnosis and treatment of acute and chronic heart failure. Eur. Heart J. 2021, 42, 3599–3726. [Google Scholar] [CrossRef]
- Levey, A.S.; Stevens, L.A.; Schmid, C.H.; Zhang, Y.L.; Castro, A.F., 3rd; Feldman, H.I.; Kusek, J.W.; Eggers, P.; Van Lente, F.; Greene, T.; et al. A new equation to estimate glomerular filtration rate. Ann. Intern. Med. 2009, 150, 604–612. [Google Scholar] [CrossRef]
- Ignacio de Ulíbarri, J.; González-Madroño, A.; de Villar, N.G.; González, P.; González, B.; Mancha, A.; Rodríguez, F.; Fernández, G. CONUT: A Tool for Controlling Nutritional Status. First Validation in a Hospital Population. Nutr. Hosp. 2005, 20, 38–45. [Google Scholar] [PubMed]
- Lang, R.M.; Badano, L.P.; Mor-Avi, V.; Afilalo, J.; Armstrong, A.; Ernande, L.; Flachskampf, F.A.; Foster, E.; Goldstein, S.A.; Kuznetsova, T.; et al. Recommendations for cardiac chamber quantification by echocardiography in adults: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. Eur. Heart J. Cardiovasc. Imaging 2015, 16, 233–270. [Google Scholar] [CrossRef] [PubMed]
- Nagueh, S.F.; Smiseth, O.A.; Appleton, C.P.; Byrd, B.F., 3rd; Dokainish, H.; Edvardsen, T.; Flachskampf, F.A.; Gillebert, T.C.; Klein, A.L.; Lancellotti, P.; et al. Recommendations for the evaluation of left ventricular diastolic function by echocardiography: An update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J. Am. Soc. Echocardiogr. 2016, 29, 277–314. [Google Scholar] [CrossRef] [PubMed]
- Nishimura, R.A.; Otto, C.M.; Bonow, R.O.; Carabello, B.A.; Erwin, J.P., 3rd; Fleisher, L.A.; Jneid, H.; Mack, M.J.; McLeod, C.J.; O’Gara, P.T.; et al. 2017 AHA/ACC focused update of the 2014 AHA/ACC guideline for the management of patients with valvular heart disease: A report of the American College of Cardiology/American Heart Association Task Force on Clinical Practice Guidelines. Circulation 2017, 135, e1159–e1195. [Google Scholar] [CrossRef]
- Humbert, M.; Kovacs, G.; Hoeper, M.M.; Badagliacca, R.; Berger, R.M.F.; Brida, M.; Carlsen, J.; Coats, A.J.S.; Escribano-Subias, P.; Ferrari, P.; et al. 2022 ESC/ERS Guidelines for the diagnosis and treatment of pulmonary hypertension. Eur. Respir. J. 2023, 61, 2200879. [Google Scholar] [CrossRef]
- Tello, K.; Wan, J.; Dalmer, A.; Vanderpool, R.; Ghofrani, H.A.; Naeije, R.; Roller, F.; Mohajerani, E.; Seeger, W.; Herberg, U.; et al. Validation of the tricuspid annular plane systolic excursion/systolic pulmonary artery pressure ratio for the assessment of right ventricular-arterial coupling in severe pulmonary hypertension. Circ. Cardiovasc. Imaging 2019, 12, e009047. [Google Scholar] [CrossRef]
- Nakagomi, A.; Kohashi, K.; Morisawa, T.; Kosugi, M.; Endoh, I.; Kusama, Y.; Atarashi, H.; Shimizu, W. Nutritional status is associated with inflammation and predicts a poor outcome in patients with chronic heart failure. J. Atheroscler. Thromb. 2016, 23, 713–727. [Google Scholar] [CrossRef]
- Chen, M.; Wang, S.A.; Yang, J.; Bai, J.; Gu, J.; Luo, H.; Zhang, X.; Han, Y.; Shao, J.; Xu, Y.; et al. Association of systemic immune-inflammation index with malnutrition among Chinese hospitalized patients: A nationwide, multicenter, cross-sectional study. Front. Nutr. 2024, 11, 1375053. [Google Scholar] [CrossRef] [PubMed]
- Liu, S.; Fu, T.; Deng, T.; Cai, X.; Zhan, Y.; Zhu, H. Association between inflammation- and nutrition-related indicators and mortality in patients with heart failure: A cohort study. Front. Nutr. 2025, 12, 1617069. [Google Scholar] [CrossRef] [PubMed]
- Guazzi, M.; Bandera, F.; Pelissero, G.; Castelvecchio, S.; Menicanti, L.; Ghio, S.; Temporelli, P.L.; Arena, R. Tricuspid annular plane systolic excursion and pulmonary arterial systolic pressure relationship in heart failure: An index of right ventricular contractile function and prognosis. Am. J. Physiol. Heart Circ. Physiol. 2013, 305, H1373–H1381. [Google Scholar] [PubMed]
- Gorter, T.M.; van Veldhuisen, D.J.; Voors, A.A.; Hummel, Y.M.; Lam, C.S.P.; Berger, R.M.F.; van Melle, J.P.; Hoendermis, E.S. Right ventricular-vascular coupling in heart failure with preserved ejection fraction and pre- vs. post-capillary pulmonary hypertension. Eur. Heart J. Cardiovasc. Imaging 2018, 19, 425–432. [Google Scholar]
- Pestelli, G.; Fiorencis, A.; Trevisan, F.; Luisi, G.A.; Smarrazzo, V.; Mele, D. New measures of right ventricle-pulmonary artery coupling in heart failure: An all-cause mortality echocardiographic study. Int. J. Cardiol. 2021, 329, 234–241. [Google Scholar] [CrossRef]
- Inciardi, R.M.; Abanda, M.; Shah, A.M.; Cikes, M.; Claggett, B.; Skali, H.; Vaduganathan, M.; Prasad, N.; Litwin, S.; Merkely, B.; et al. Right ventricular function and pulmonary coupling in patients with heart failure and preserved ejection fraction. J. Am. Coll. Cardiol. 2023, 82, 489–499. [Google Scholar] [CrossRef]
- Curtis, J.P.; Sokol, S.I.; Wang, Y.; Rathore, S.S.; Ko, D.T.; Jadbabaie, F.; Portnay, E.L.; Marshalko, S.J.; Radford, M.J.; Krumholz, H.M. The association of left ventricular ejection fraction, mortality, and cause of death in stable outpatients with heart failure. J. Am. Coll. Cardiol. 2003, 42, 736–742. [Google Scholar]
- Rosch, S.; Kresoja, K.P.; Besler, C.; Fengler, K.; Schöber, A.R.; von Roeder, M.; Lücke, C.; Gutberlet, M.; Klingel, K.; Thiele, H.; et al. Characteristics of heart failure with preserved ejection fraction across the range of left ventricular ejection fraction. Circulation 2022, 146, 506–518. [Google Scholar] [CrossRef]
- Toma, M.; Ezekowitz, J.A.; Bakal, J.A.; O’Connor, C.M.; Hernandez, A.F.; Sardar, M.R.; Zolty, R.; Massie, B.M.; Swedberg, K.; Armstrong, P.W.; et al. The relationship between left ventricular ejection fraction and mortality in patients with acute heart failure: Insights from the ASCEND-HF Trial. Eur. J. Heart Fail. 2014, 16, 334–341. [Google Scholar]
- Ohte, N.; Kikuchi, S.; Iwahashi, N.; Kinugasa, Y.; Dohi, K.; Takase, H.; Masai, K.; Inoue, K.; Okumura, T.; Hachiya, K.; et al. Unfavourable outcomes in patients with heart failure with higher preserved left ventricular ejection fraction. Eur. Heart J. Cardiovasc. Imaging 2023, 24, 293–300. [Google Scholar]
- Paulus, W.J.; Zile, M.R. From systemic inflammation to myocardial fibrosis: The heart failure with preserved ejection fraction paradigm revisited. Circ. Res. 2021, 128, 1451–1467. [Google Scholar] [CrossRef]
- Wehner, G.J.; Jing, L.; Haggerty, C.M.; Suever, J.D.; Leader, J.B.; Hartzel, D.N.; Kirchner, H.L.; Manus, J.N.A.; James, N.; Ayar, Z.; et al. Routinely reported ejection fraction and mortality in clinical practice: Where does the nadir of risk lie? Eur. Heart J. 2020, 41, 1249–1257. [Google Scholar] [CrossRef]
- Stewart, S.; Playford, D.; Scalia, G.M.; Currie, P.; Celermajer, D.S.; Prior, D.; Codde, J.; Strange, G.; NEDA Investigators. Ejection fraction and mortality: A nationwide register-based cohort study of 499 153 women and men. Eur. J. Heart Fail. 2021, 23, 406–416. [Google Scholar] [CrossRef]
- Kawaguchi, M.; Hay, I.; Fetics, B.; Kass, D.A. Combined ventricular systolic and arterial stiffening in patients with heart failure and preserved ejection fraction: Implications for systolic and diastolic reserve limitations. Circulation 2003, 107, 714–720. [Google Scholar] [CrossRef]
- Cheng, S.; Fernandes, V.R.; Bluemke, D.A.; McClelland, R.L.; Kronmal, R.A.; Lima, J.A. Age-related left ventricular remodeling and associated risk for cardiovascular outcomes: The Multi-Ethnic Study of Atherosclerosis. Circ. Cardiovasc. Imaging 2009, 2, 191–198. [Google Scholar] [CrossRef]
| Index | Calculation | Normal / Low Risk | Mild Nutritional Risk | Moderate–Severe Nutritional Risk |
|---|---|---|---|---|
| PNI | 10 × albumin (g/dL) + 0.005 × lymphocyte count (/mm3) | ≥45–50 | 40–45 | <40 |
| CONUT Score | Based on albumin, total cholesterol, and lymphocyte count | 0–1 | 2–4 | ≥5 |
| CALLy Index | (Albumin × lymphocyte count) / CRP | Higher values indicate better nutritional and inflammatory status; values ≥2–3 generally associated with better prognosis | <2–3 indicates increased risk | Lower values associated with worse prognosis |
| All patients (n = 200) | Dead (n = 123) | Alive (n = 77) | P value | |
|---|---|---|---|---|
| Demographics | ||||
| Age (years) | 86.6 ± 6.5 | 87.0 ± 6.6 | 86.0 ± 6.3 | 0.29 |
| Females (%) | 140 (70.0) | 84 (68.3) | 56 (72.7) | 0.50 |
| Cardiovascular risk factors | ||||
| Hypertension (%) | 151 (75.5) | 91 (74.0) | 60 (77.9) | 0.49 |
| Smoking (%) | 31 (15.5) | 18 (14.6) | 13 (16.9) | 0.65 |
| Diabetes (%) | 57 (28.5) | 38 (30.9) | 19 (24.7) | 0.36 |
| Dyslipidemia (%) | 99 (49.5) | 60 (48.8) | 39 (50.6) | 0.80 |
| Obesity (%) | 25 (12.5) | 15 (12.2) | 10 (13.0) | 0.87 |
| Noncardiovascular comorbidities | ||||
| CKD (%) | 109 (54.5) | 79 (64.2) | 30 (39.0) | <0.001 |
| COPD (%) | 42 (21.0) | 26 (21.1) | 16 (20.8) | 0.96 |
| Hypothyroidism (%) | 37 (18.5) | 25 (20.3) | 12 (15.6) | 0.39 |
| Cognitive impairment (%) | 82 (41.0) | 60 (48.8) | 22 (28.6) | 0.007 |
| Cardiovascular comorbidities | ||||
| History of CAD (%) | 39 (19.5) | 28 (22.8) | 11 (14.3) | 0.16 |
| Previous TIA/stroke (%) | 37 (18.5) | 27 (22.0) | 10 (13.0) | 0.13 |
| PAD (%) | 48 (24.0) | 34 (27.6) | 14 (18.2) | 0.15 |
| Physical examination | ||||
| Dyspnea | 100 (50.0) | 60 (48.8) | 40 (51.9) | 0.68 |
| Leg swelling | 34 (17.0) | 22 (17.9) | 12 (15.6) | 0.65 |
| SBP (mmHg) | 135 (120–150) | 130.8 ± 31.0 | 140 (120–160) | 0.02 |
| DBP (mmHg) | 70 (60–80) | 69.3 ± 15.1 | 70 (60–80) | 0.18 |
| HR (bpm) | 78.5 ± 17.2 | 80.9 ± 13.9 | 74.6 ± 13.3 | 0.01 |
| Body temperature ≥37.5° (%) | 78 (39.0) | 63 (51.2) | 15 (19.5) | <0.001 |
| All patients (n = 200) | Dead (n = 123) | Alive (n = 77) | P value | |
|---|---|---|---|---|
| Blood tests | ||||
| Hemoglobin (g/dl) | 11.1 (9.0–12.8) | 11.1 (9.2–12.1) | 11.1 (9.7–13.2) | 0.37 |
| WBCs (× 109/L) | 9.35 (6.85–13.02) | 10.62 (7.34–14.08) | 9.12 (6.64–12.45) | <0.001 |
| Neutrophils (×109/L) | 7.94 (4.81–11.63) | 8.69 (5.92–14.44) | 6.49 (3.91–9.79) | <0.001 |
| Lymphocytes (×109/L) | 1.10 (0.79–1.59) | 0.94 (0.69–1.19) | 1.40 (0.92–2.01) | 0.01 |
| Platelets (×109/L) | 232 (164–297) | 232 (164–291) | 234 (174–299) | 0.59 |
| Glucose (mg/dL) | 121 (97–155) | 125 (99–157) | 109 (97–135) | 0.92 |
| Iron (µg/dL) | 45 (25–65) | 40 (22–66) | 50 (33–73) | 0.003 |
| Creatinine (mg/dL) | 1.23 (0.87–2.05) | 1.39 (0.92–2.21) | 1.06 (0.65–1.83) | 0.02 |
| eGFR (ml/min/m2) | 39 (23–60) | 38 (23.5–60) | 46 (29–82) | 0.006 |
| Sodium (mEq/L) | 140 (136–144) | 140 (135.3–144.0) | 138 (134–142) | 0.03 |
| Potassium (mEq/L) | 4.15 ± 0.71 | 4.15 ± 0.65 | 3.96 (3.57–4.54) | 0.92 |
| Calcium (mmol/L) | 2.10 (1.14–2.30) | 2.10 (1.34–2.20) | 2.20 (2.10–2.30) | 0.16 |
| Total bilirubin (mg/dL) | 0.70 (0.40–1.10) | 0.60 (0.40–0.90) | 0.70 (0.40–1.10) | 0.15 |
| Albumin (g/dL) | 2.99 (2.57–3.31) | 2.79 (2.42–3.16) | 3.36 (3.05–3.66) | <0.001 |
| Uric acid (mg/dL) | 7.30 (5.40–9.80) | 7.60 (5.55–9.60) | 6.70 (4.90–8.30) | 0.14 |
| Total cholesterol (mg/dL) | 139.5 (119.8–165.2) | 134 (110–160) | 150 (132–174) | <0.001 |
| HDL cholesterol (mg/dL) | 37.0 (27.0–45.0) | 34 (24–42) | 40 (32–55) | <0.001 |
| LDL cholesterol (mg/dL) | 77.0 (60.9–98.8) | 73.4 (51–90.8) | 92 (75–118) | <0.001 |
| Triglycerides (mg/dL) | 107 (86–147) | 107 (85.5–146) | 113 (89–147) | 0.11 |
| TSH (mIU/L) | 1.39 (0.82–2.00) | 1.39 (0.82–2.00) | 1.29 (0.64–2.05) | 0.45 |
| CRP (mg/dL) | 6.20 (1.20–15.80) | 6.50 (2.90–15.36) | 2.95 (0.80–7.50) | <0.001 |
| NT-proBNP (pg/mL) | 1566.5 (345.0–5055.5) | 1750 (396–7331) | 1017 (173–3596) | <0.001 |
| hs-cTn (ng/mL) | 40.0 (20.0–84.5) | 40 (20–140) | 40 (10–80) | 0.27 |
| Nutritional risk scores | ||||
| PNI | 35.9 (31.6–39.7) | 33.3 (29.6–36.8) | 43.7 (36.6–44.7) | <0.001 |
| CONUT score | 7 (5–9) | 8 (7–9) | 3.8 (2–5) | <0.001 |
| CALLy index | 0.063 (0.015–0.199) | 0.035 (0.014–0.075) | 0.22 (0.09–0.46) | <0.001 |
| All patients (n = 200) | Dead (n = 123) | Alive (n = 77) | P value | |
|---|---|---|---|---|
| Chest X-ray findings | ||||
| Normal radiographic pattern (%) | 42 (21.0) | 14 (11.4) | 28 (36.4) | <0.001 |
| Pulmonary congestion (%) | 118 (59.0) | 74 (60.2) | 44 (57.1) | 0.66 |
| Radiographic evidence of pneumonia (%) | 40 (20.0) | 35 (28.4) | 5 (6.5) | <0.001 |
| ECG findings | ||||
| Sinus rhythm (%) | 141 (70.5) | 84 (68.3) | 57 (74) | 0.39 |
| AF (%) | 59 (29.5) | 39 (31.7) | 20 (26) | 0.39 |
| Normal IV conduction (%) | 88 (44.0) | 50 (40.7) | 38 (49.4) | 0.21 |
| LAFB (%) | 54 (27.0) | 32 (26) | 22 (28.6) | 0.68 |
| LBBB (%) | 8 (4.0) | 4 (3.3) | 4 (5.2) | 0.57 |
| RBBB (%) | 50 (25.0) | 37 (30) | 13 (16.9) | 0.04 |
| Conventional TTE parameters | ||||
| IVS (mm) | 13 (12–15) | 14.0 (12.0–16.0) | 13 (12–15) | 0.77 |
| PW (mm) | 10 (9–11) | 10.0 (9.0–11.0) | 10 (9–11) | 0.55 |
| LVEDD (mm) | 42 (39–47) | 41.0 ± 6.5 | 44 (39–48) | 0.001 |
| RWT | 0.50 (0.44–0.55) | 0.50 ± 0.09 | 0.47 ± 0.07 | 0.01 |
| LVEDV (ml) | 60 (45–88) | 55.0 (44.0–75.0) | 66 (50–95) | 0.02 |
| LVESV (ml) | 20 (15–28) | 17.6 (14.4–22.8) | 25.0 (19.3–34.0) | <0.001 |
| LVEF (%) | 65 (60–70) | 68.0 ± 4.8 | 60 (55–65) | <0.001 |
| E/A | 0.77 (0.66–1.55) | 0.82 (0.66–1.55) | 0.70 (0.60–1.25) | 0.08 |
| E/e’ | 16 (11–23) | 17.0 (11.0–23.0) | 16.0 (11.0–21.0) | 0.30 |
| LA A-P diameter (mm) | 46 (41–52) | 47.0 (41.0–53.0) | 46 (40–53) | 0.83 |
| LA longitudinal diameter (mm) | 56 (50–63) | 57.0 (50.0–64.0) | 56 (50–65) | 0.82 |
| LAV (ml) | 77 (55–110) | 85 (55–110) | 75 (57–110) | 0.54 |
| More than mild MR (%) | 63 (31.5) | 38 (30.9) | 25 (32.5) | 0.82 |
| More than mild AR (%) | 8 (4.0) | 3 (2.4) | 5 (6.5) | 0.13 |
| More than mild AS (%) | 23 (11.5) | 13 (10.6) | 10 (13) | 0.63 |
| More than mild TR (%) | 57 (28.5) | 36 (29.3) | 21 (27.3) | 0.77 |
| RVIT (mm) | 30 (26–35) | 30.0 (26.0–35.0) | 31 (27–35) | 0.28 |
| TAPSE (mm) | 18 (14–22) | 16 (11–28) | 22 (20–25) | <0.001 |
| sPAP (mmHg) | 45 (25–100) | 49 (24–100) | 40 (25–100) | <0.001 |
| TAPSE/sPAP (mm/mmHg) | 0.45 (0.31–0.63) | 0.32 (0.25–0.45) | 0.74 (0.63–0.88) | <0.001 |
| Aortic root (mm) | 34.1 ± 4.1 | 33.0 ± 4.7 | 34.5 ± 4.6 | 0.13 |
| Ascending aorta (mm) | 35.3 ± 4.6 | 35.0 ± 4.6 | 36.0 ± 4.7 | 0.14 |
| All patients (n = 200) | Dead (n = 123) | Alive (n = 77) | P value | |
|---|---|---|---|---|
| NYHA functional status at admission | ||||
| NYHA III (%) | 124 (62) | 68 (55.3) | 56 (72.7) | 0.01 |
| NYHA IV (%) | 76 (38) | 55 (44.7) | 21 (27.3) | 0.01 |
| Underlying etiology of heart failure | ||||
| CAD (%) | 64 (32) | 44 (35.8) | 20 (26) | 0.14 |
| VHD (%) | 42 (21) | 26 (21.1) | 16 (20.8) | 0.95 |
| HHD (%) | 60 (30) | 30 (24.4) | 30 (39) | 0.03 |
| PH (%) | 34 (17) | 30 (24.4) | 4 (5.2) | 0.001 |
| Main causes leading to hospital admission | ||||
| CHF (%) | 48 (24) | 10 (8.1) | 38 (49.3) | <0.001 |
| Acute respiratory conditions (%) | 87 (43.5) | 68 (55.3) | 19 (24.7) | <0.001 |
| Gastro-intestinal disorders (%) | 8 (4) | 6 (4.9) | 2 (2.6) | 0.42 |
| Severe anemia (%) | 16 (8) | 11 (8.9) | 5 (6.5) | 0.44 |
| Severe CKD (%) | 9 (4.5) | 5 (4.1) | 4 (5.2) | 0.72 |
| Cancers (%) | 8 (4) | 5 (4.1) | 3 (3.9) | 0.95 |
| Hyponatremia (%) | 16 (8) | 12 (9.8) | 4 (5.2) | 0.22 |
| Hypernatremia (%) | 5 (2.5) | 4 (3.3) | 1 (1.3) | 0.36 |
| Neurological disorders (%) | 3 (1.5) | 2 (1.6) | 1 (1.3) | 0.86 |
| ≥2 causes of admission (%) | 58 (29) | 45 (36.6) | 13 (16.9) | 0.002 |
| Pharmacological therapy during hospitalization | ||||
| Antiplatelets (%) | 74 (37) | 47 (38.2) | 27 (35.1) | 0.64 |
| Anticoagulants (%) | 82 (41) | 50 (40.7) | 32 (41.6) | 0.89 |
| ACEIs/ARBs (%) | 84 (42.0) | 40 (32.5) | 44 (57.1) | <0.001 |
| CCB (%) | 51 (25.5) | 29 (23.6) | 22 (28.6) | 0.46 |
| BB (%) | 115 (57.5) | 68 (55.3) | 47 (61) | 0.43 |
| Digoxin (%) | 59 (29.5) | 39 (31.7) | 20 (26) | 0.36 |
| Loop diuretics (%) | 132 (66) | 82 (66.7) | 50 (64.9) | 0.77 |
| MRAs (%) | 73 (36.5) | 47 (38.2) | 26 (33.8) | 0.55 |
| Statins (%) | 58 (29) | 28 (22.8) | 30 (39.0) | 0.02 |
| Corticosteroids (%) | 58 (29) | 41 (33.3) | 17 (22.1) | 0.08 |
| Antibiotics (%) | 126 (63) | 101 (82.1) | 25 (32.5) | <0.001 |
| Oxygen therapy (%) | 73 (36.5) | 53 (43.1) | 20 (26) | 0.02 |
| Oral hypoglycemic agents (%) | 20 (10) | 10 (8.1) | 10 (13) | 0.28 |
| Insulin (%) | 25 (12.5) | 18 (14.6) | 7 (9.1) | 0.29 |
| LOS (days) | 9.4 ± 6.2 | 10.6 ± 6.5 | 7.5 ± 5.3 | 0.01 |
| Category | n (%) |
|---|---|
| Overall mortality | 123 (61.5) |
| Patients alive at end of follow-up | 77 (38.5) |
| Causes of death (n = 123) | |
| Respiratory infections / respiratory failure | 48 (39.0) |
| Cardiovascular causes (HF progression, acute cardiac events) | 31 (25.2) |
| Multisystem deterioration / frailty-related conditions | 21 (17.1) |
| Other non-cardiovascular causes | 23 (18.7) |
| Non-fatal events among survivors (n = 77) | |
| Respiratory events (dyspnea, infections, COPD exacerbation) | 30 (39.0) |
| Cardiovascular events (HF worsening, ACS) | 14 (18.2) |
| Non-respiratory infections | 10 (13.0) |
| Renal/metabolic complications | 9 (11.7) |
| Trauma/falls/fractures | 8 (10.4) |
| Other medical causes | 6 (7.8) |
| Variable | Univariate HR (95% CI) | P value | Multivariate HR (95% CI) | P value |
|---|---|---|---|---|
| Age | 1.00 (0.97–1.03) | 0.755 | — | — |
| Female sex | 0.70 (0.48–1.03) | 0.077 | — | — |
| Diabetes mellitus | 1.37 (0.93–2.02) | 0.111 | — | — |
| Coronary artery disease | 1.21 (0.79–1.84) | 0.377 | — | — |
| Systolic blood pressure | 0.997 (0.992–1.003) | 0.324 | — | — |
| eGFR | 0.995 (0.986–1.004) | 0.225 | — | — |
| Sodium | 1.002 (0.979–1.026) | 0.872 | — | — |
| Loop diuretics | 1.20 (0.81–1.77) | 0.354 | — | — |
| E/e’ | 1.01 (0.99–1.04) | 0.366 | — | — |
| PNI | 0.935 (0.909–0.961) | <0.001 | 1.001 (0.967–1.036) | 0.940 |
| CONUT score | 1.244 (1.153–1.343) | <0.001 | 1.136 (1.027–1.256) | 0.013 |
| CALLy index | 0.96 (0.69–1.34) | 0.829 | — | — |
| LVEF | 1.093 (1.055–1.132) | <0.001 | 1.056 (1.014–1.099) | 0.008 |
| TAPSE/sPAP ratio | 0.086 (0.035–0.213) | <0.001 | 0.222 (0.082–0.603) | 0.003 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




