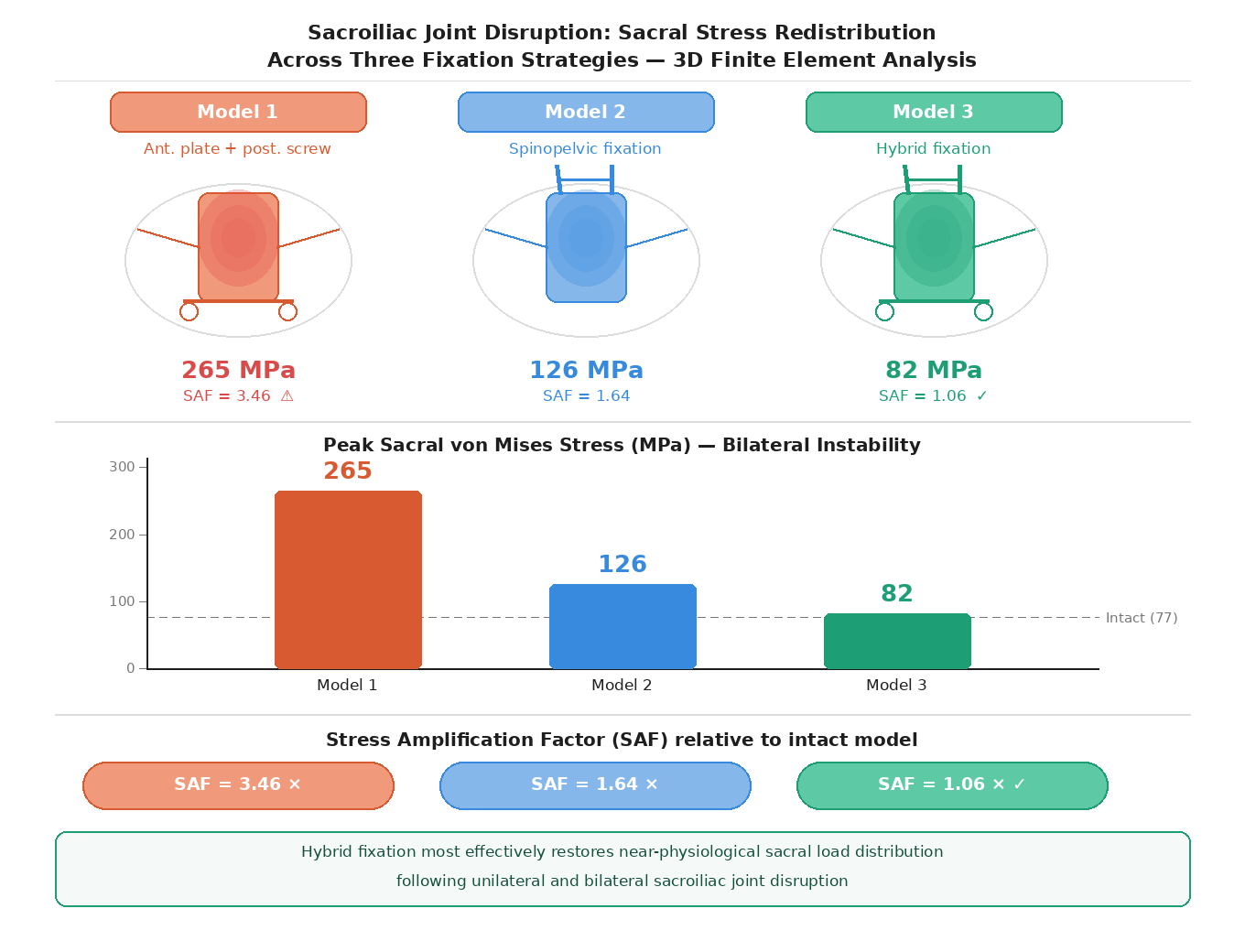
Background: Sacroiliac joint (SIJ) disruption alters posterior pelvic ring stability and may result in abnormal sacral stress redistribution. The biomechanical effects of different fixation strategies on sacral load transfer remain controversial. This study aimed to compare sacral stress patterns under unilateral and bilateral SIJ instability using three fixation techniques in a three-dimensional finite element model. Methods: A three-dimensional lumbosacral–pelvic finite element model was reconstructed from computed tomography data of a healthy adult and validated against previously published pelvic biomechanical data. SIJ instability was simulated by reducing the friction coefficient to represent ligamentous failure. Three fixation constructs were analyzed: anterior plate with posterior screw fixation, spinopelvic fixation, and hybrid fixation. A 750 N axial compressive load was applied to simulate static standing conditions; dynamic loading scenarios such as walking or sitting were not included. Peak sacral von Mises stress and stress amplification factors were calculated and compared with the intact model. Results: Anterior plate combined with posterior screw fixation produced the highest sacral stress amplification (SAF = 3.46 under unilateral instability; peak stress 265.40 MPa), exceeding three times the intact value, particularly under unilateral left instability (SAF = 3.46). Spinopelvic fixation significantly reduced peak sacral stress (125.66 MPa under bilateral instability; SAF = 1.64) but remained above physiological levels. Hybrid fixation demonstrated sacral stress values closest to the intact condition (81.64 MPa; SAF = 1.06), with minimal amplification and near-symmetrical load distribution. Conclusions: Fixation strategy significantly influences sacral load redistribution following SIJ disruption. Hybrid fixation most effectively restored near-physiological sacral stress patterns, whereas anterior plate with posterior screw fixation resulted in excessive stress concentration. Hybrid stabilization may provide a biomechanically balanced approach for unstable posterior pelvic injuries.