Submitted:
01 April 2026
Posted:
03 April 2026
You are already at the latest version
Abstract
Background: Psychological inflexibility (PI) is a transdiagnostic risk factor for emotional distress and diminished quality of life (QoL), yet the indirect pathways linking PI to QoL through distress remain largely untested in breast cancer. Methods: This exploratory secondary analysis used a publicly available longitudinal dataset of 40 women with non-metastatic breast cancer assessed at baseline and 2-month follow-up. Bootstrapped mediation (5,000 resamples, BCa CIs) tested whether depression, anxiety, and stress (DASS-21) statistically mediated the association between PI (AAQ-II) and QoL (WHOQOL-BREF) across 27 models. Hierarchical regressions, Kruskal–Wallis tests, and extended correlations supplemented the analysis. Results: At follow-up, all nine cross-sectional indirect effects were significant (all 95% BCa CIs excluding zero), with distress accounting for 33–51% of the total association between PI and QoL. The largest indirect effects were observed for depression on psychological QoL (indirect = −0.845, p < .001) and anxiety on physical QoL (indirect = −0.739, p < .001). No indirect effects were significant at baseline or for change scores (all p > .05). Concurrent PI independently predicted psychological QoL (ΔR² = .094, p = .002), general QoL (ΔR² = .084, p = .015), and anxiety (ΔR² = .122, p = .004) in hierarchical regressions. Anxiety severity was associated with impairment across all five QoL domains (all p_adj < .05). Conclusions: These preliminary findings suggest that emotional distress may partially account for the association between PI and QoL in breast cancer, consistent with predictions from the ACT model. However, the small sample size and cross-sectional nature of the follow-up indirect effects preclude causal inference. Replication in adequately powered prospective designs is essential.
Keywords:
1. Introduction
2. Materials and Methods
3. Results
3.1. Descriptive Statistics
3.2. DASS-21 Clinical Severity Distribution
3.3. Temporal Stability: Paired Comparisons
3.4. Internal Consistency
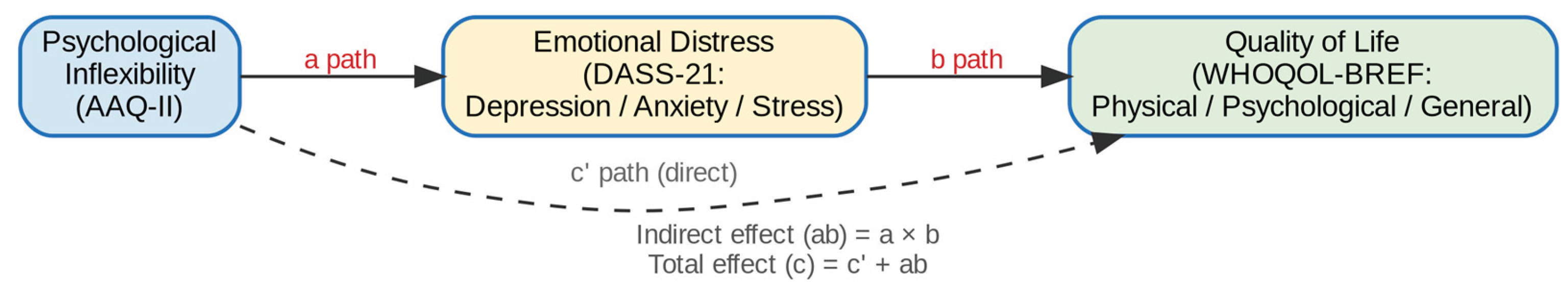
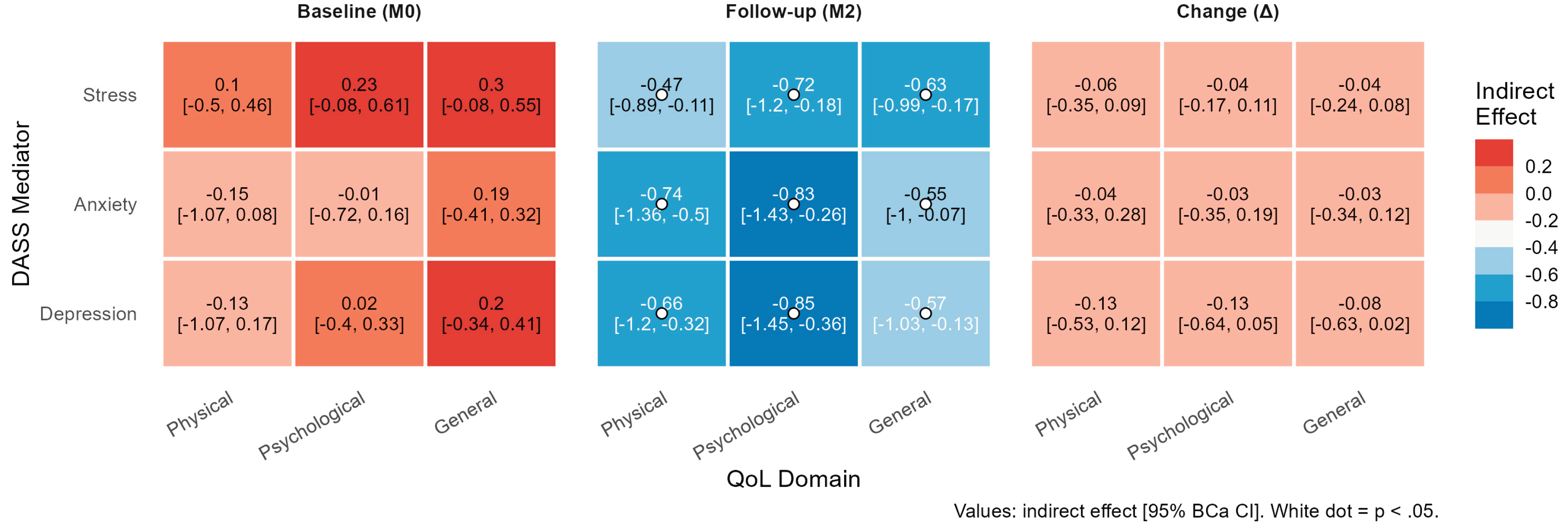
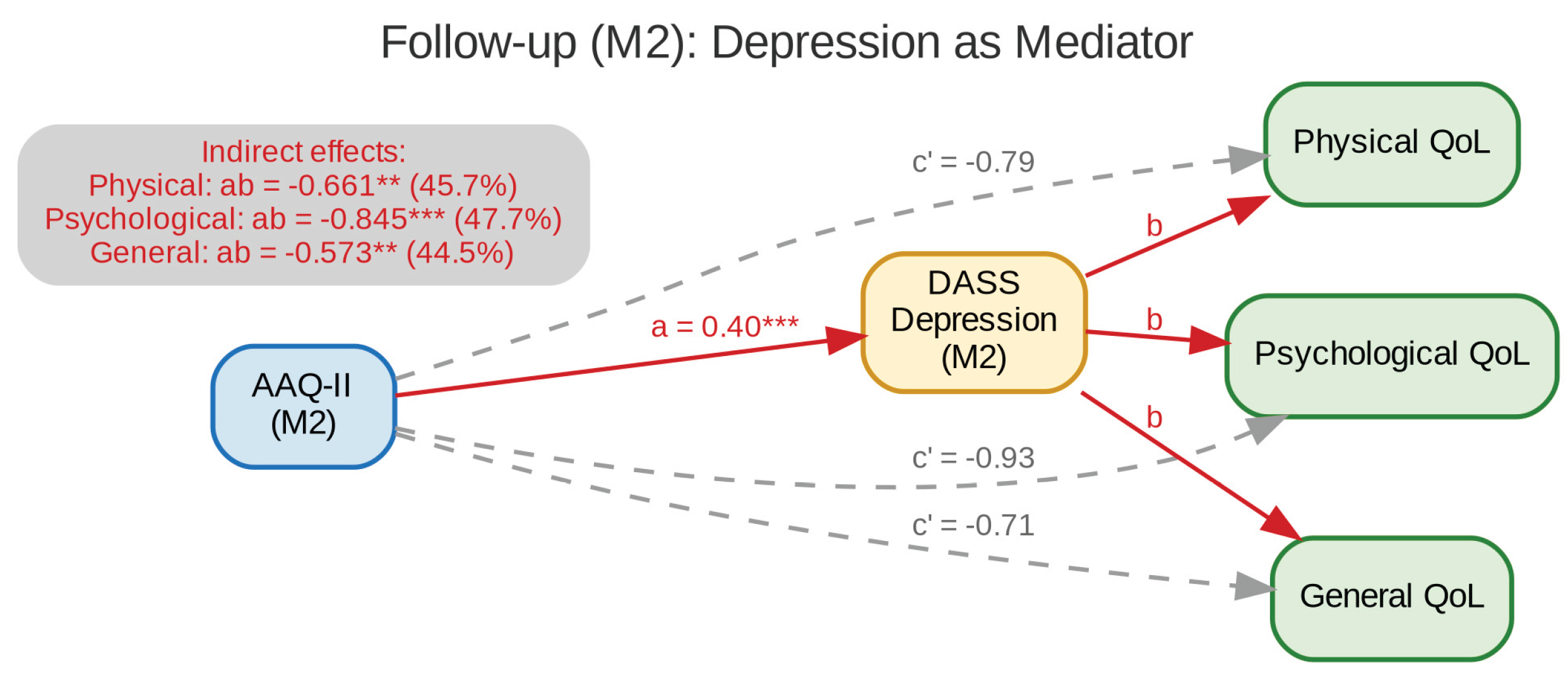
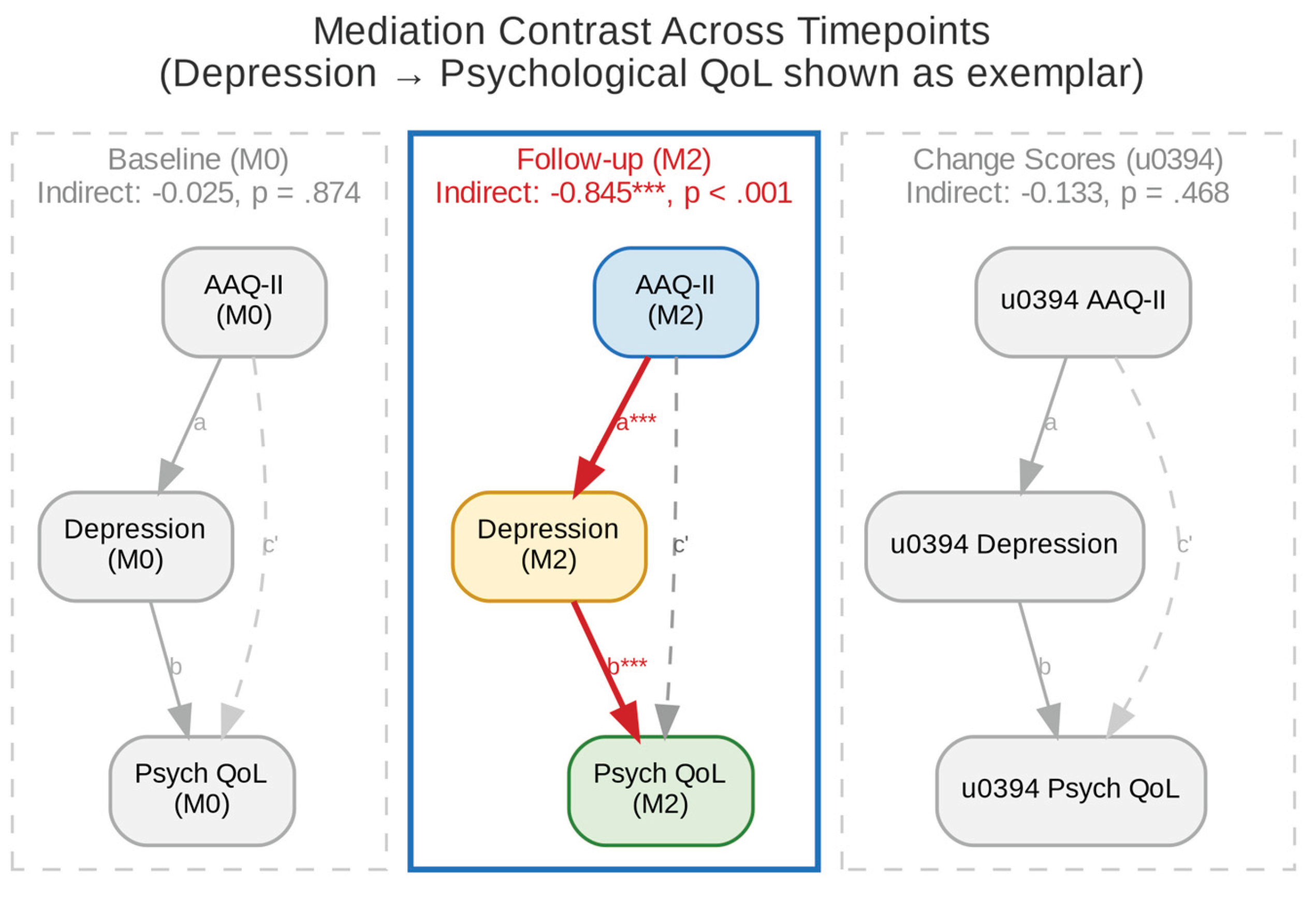
3.5. Mediation Analysis
3.6. Hierarchical Regression
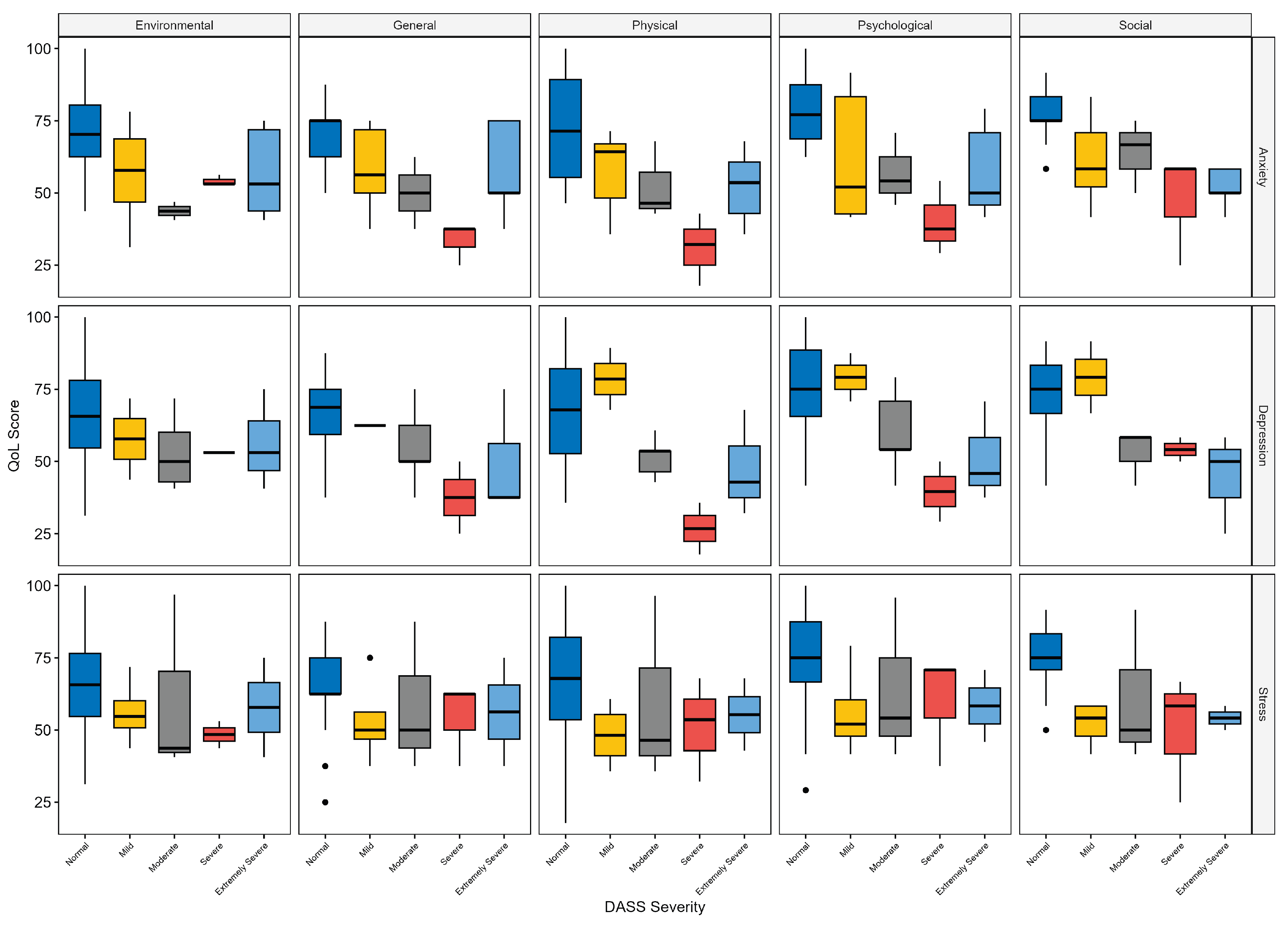
3.7. DASS-21 Clinical Severity and Quality of Life
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| ACT | Acceptance and Commitment Therapy |
| BC | Breast Cancer |
| PI | Psychological Inflexibility |
| QoL | Quality of Life |
Appendix A
| Measure | Time | n | M | SD | Mdn | Skew | Kurt | SW p |
|---|---|---|---|---|---|---|---|---|
| AAQ-II | M0 | 40 | 17.35 | 9.32 | 17.00 | 0.61 | -0.76 | .003 |
| AAQ-II | M2 | 40 | 15.95 | 7.71 | 14.00 | 0.60 | -0.77 | .004 |
| DASS Depression | M0 | 40 | 4.08 | 5.32 | 2.00 | 1.30 | 0.69 | <.001 |
| DASS Depression | M2 | 40 | 3.35 | 5.13 | 1.00 | 1.89 | 2.99 | <.001 |
| DASS Anxiety | M0 | 39 | 4.03 | 4.75 | 3.00 | 1.34 | 1.47 | <.001 |
| DASS Anxiety | M2 | 40 | 3.75 | 4.93 | 1.50 | 1.64 | 2.36 | <.001 |
| DASS Stress | M0 | 39 | 5.74 | 5.14 | 5.00 | 0.90 | -0.26 | .001 |
| DASS Stress | M2 | 40 | 4.70 | 4.25 | 4.50 | 1.50 | 3.48 | <.001 |
| QoL Physical | M0 | 40 | 62.77 | 20.04 | 64.29 | 0.06 | -0.80 | .395 |
| QoL Physical | M2 | 40 | 66.34 | 17.86 | 69.64 | -0.18 | -0.91 | .331 |
| QoL Psychological | M0 | 40 | 69.48 | 19.11 | 70.83 | -0.23 | -1.00 | .213 |
| QoL Psychological | M2 | 40 | 70.52 | 18.40 | 75.00 | -0.76 | -0.19 | .016 |
| QoL Social | M0 | 40 | 68.54 | 15.84 | 75.00 | -0.47 | -0.27 | .042 |
| QoL Social | M2 | 40 | 67.50 | 17.38 | 66.67 | -0.29 | -0.73 | .147 |
| QoL Environmental | M0 | 39 | 63.46 | 16.97 | 62.50 | 0.33 | -0.65 | .359 |
| QoL Environmental | M2 | 40 | 63.28 | 17.97 | 65.62 | 0.11 | -0.63 | .450 |
| QoL General | M0 | 40 | 61.88 | 15.75 | 62.50 | -0.36 | -0.78 | .008 |
| QoL General | M2 | 40 | 63.75 | 15.45 | 62.50 | -0.18 | -0.28 | .008 |
| Subscale | Time | Normal | Mild | Moderate | Severe | Ext. Severe |
|---|---|---|---|---|---|---|
| Depression | M0 | 28 (70.0%) | 2 (5.0%) | 5 (12.5%) | 2 (5.0%) | 3 (7.5%) |
| Depression | M2 | 29 (72.5%) | 3 (7.5%) | 4 (10.0%) | 1 (2.5%) | 3 (7.5%) |
| Anxiety | M0 | 22 (56.4%) | 6 (15.4%) | 3 (7.7%) | 3 (7.7%) | 5 (12.8%) |
| Anxiety | M2 | 26 (65.0%) | 4 (10.0%) | 3 (7.5%) | 2 (5.0%) | 5 (12.5%) |
| Stress | M0 | 27 (69.2%) | 4 (10.3%) | 3 (7.7%) | 3 (7.7%) | 2 (5.1%) |
| Stress | M2 | 34 (85.0%) | 2 (5.0%) | 2 (5.0%) | 1 (2.5%) | 1 (2.5%) |
| Measure | M (M0) | M (M2) | Δ | Test | p | d | Sig |
|---|---|---|---|---|---|---|---|
| AAQ-II | 17.35 | 15.95 | -1.40 | Wilcoxon | .493 | -0.20 | ns |
| DASS Depression | 4.08 | 3.35 | -0.72 | Wilcoxon | .423 | -0.16 | ns |
| DASS Anxiety | 4.03 | 3.72 | -0.31 | Wilcoxon | .957 | -0.07 | ns |
| DASS Stress | 5.74 | 4.59 | -1.15 | Wilcoxon | .126 | -0.28 | ns |
| QoL Physical | 62.77 | 66.34 | 3.57 | Paired t | .103 | 0.26 | ns |
| QoL Psychological | 69.48 | 70.52 | 1.04 | Wilcoxon | .843 | 0.08 | ns |
| QoL Social | 68.54 | 67.50 | -1.04 | Wilcoxon | .500 | -0.09 | ns |
| QoL Environmental | 63.46 | 63.70 | 0.24 | Paired t | .882 | 0.02 | ns |
| QoL General | 61.88 | 63.75 | 1.88 | Wilcoxon | .409 | 0.15 | ns |
| Timepoint | Mediator | Outcome | Indirect [95% CI] | p | Direct | Total | % Med |
|---|---|---|---|---|---|---|---|
| Baseline (M0) | Depression | Physical | -0.133 [-1.07, 0.17] | .513 | -1.25 | -1.39 | 9.6% |
| Depression | Psychological | 0.025 [-0.40, 0.33] | .874 | -1.67 | -1.64 | -1.5% | |
| Depression | General | 0.200 [-0.34, 0.41] | .297 | -1.56 | -1.36 | -14.7% | |
| Anxiety | Physical | -0.151 [-1.07, 0.08] | .370 | -1.25 | -1.40 | 10.8% | |
| Anxiety | Psychological | -0.010 [-0.72, 0.16] | .903 | -1.68 | -1.69 | 0.6% | |
| Anxiety | General | 0.186 [-0.41, 0.33] | .316 | -1.59 | -1.40 | -13.3% | |
| Stress | Physical | 0.096 [-0.50, 0.46] | .673 | -1.49 | -1.39 | -6.9% | |
| Stress | Psychological | 0.227 [-0.08, 0.61] | .156 | -1.87 | -1.64 | -13.8% | |
| Stress | General | 0.301 [-0.08, 0.55] | .092 | -1.66 | -1.36 | -22.1% | |
| Follow-up (M2) | Depression | Physical | -0.661 [-1.20, -0.32]* | .002 | -0.79 | -1.45 | 45.7% |
| Depression | Psychological | -0.845 [-1.45, -0.37]* | <.001 | -0.93 | -1.77 | 47.7% | |
| Depression | General | -0.573 [-1.03, -0.13]* | .009 | -0.71 | -1.29 | 44.5% | |
| Anxiety | Physical | -0.739 [-1.36, -0.50]* | <.001 | -0.71 | -1.45 | 51.1% | |
| Anxiety | Psychological | -0.830 [-1.43, -0.26]* | .007 | -0.94 | -1.77 | 46.9% | |
| Anxiety | General | -0.551 [-1.00, -0.07]* | .023 | -0.74 | -1.29 | 42.8% | |
| Stress | Physical | -0.474 [-0.89, -0.11]* | .022 | -0.97 | -1.45 | 32.8% | |
| Stress | Psychological | -0.723 [-1.20, -0.18]* | .005 | -1.05 | -1.77 | 40.8% | |
| Stress | General | -0.628 [-0.99, -0.17]* | .008 | -0.66 | -1.29 | 48.8% | |
| Change (Δ) | Depression | Physical | -0.126 [-0.53, 0.12] | .480 | -0.08 | -0.20 | 61.6% |
| Depression | Psychological | -0.133 [-0.64, 0.06] | .468 | -0.46 | -0.59 | 22.4% | |
| Depression | General | -0.084 [-0.63, 0.02] | .405 | -0.52 | -0.60 | 13.9% | |
| Anxiety | Physical | -0.035 [-0.33, 0.28] | .812 | -0.15 | -0.18 | 19.5% | |
| Anxiety | Psychological | -0.035 [-0.35, 0.19] | .817 | -0.58 | -0.61 | 5.6% | |
| Anxiety | General | -0.028 [-0.34, 0.12] | .768 | -0.60 | -0.63 | 4.4% | |
| Stress | Physical | -0.059 [-0.35, 0.09] | .545 | -0.16 | -0.22 | 26.9% | |
| Stress | Psychological | -0.037 [-0.17, 0.12] | .776 | -0.57 | -0.61 | 6.1% | |
| Stress | General | -0.037 [-0.24, 0.08] | .696 | -0.56 | -0.60 | 6.2% |
| Outcome | R² S1 | R² S2 | ΔR² | AAQ M2 (S2) | R² S3 | AAQ M2 (S3) | AAQ M0 (S3) |
|---|---|---|---|---|---|---|---|
| QoL Psychological | .606 | .700 | .094 | -.97** | .703 | -.91** | -.18 |
| QoL Social | .603 | .609 | .006 | -.23 | .609 | -.21 | -.07 |
| QoL Environmental | .698 | .729 | .031 | -.51† | .735 | -.64* | .24 |
| QoL General | .438 | .522 | .084 | -.75* | .523 | -.71* | -.10 |
| DASS Anxiety | .416 | .538 | .122 | .26** | .593 | .15 | .20* |
| DASS | QoL Domain | H | df | p | p (adj) | Sig |
|---|---|---|---|---|---|---|
| Anxiety | Physical | 14.99 | 4 | .005 | .016 | * |
| Anxiety | Psychological | 15.49 | 4 | .004 | .016 | * |
| Anxiety | Social | 20.41 | 4 | <.001 | .006 | ** |
| Anxiety | Environmental | 11.03 | 4 | .026 | .049 | * |
| Anxiety | General | 14.11 | 4 | .007 | .017 | * |
| Depression | Physical | 11.84 | 4 | .019 | .040 | * |
| Depression | Psychological | 9.70 | 4 | .046 | .076 | ns |
| Depression | Social | 16.67 | 4 | .002 | .016 | * |
| Depression | Environmental | 4.33 | 4 | .363 | .411 | ns |
| Depression | General | 7.67 | 4 | .104 | .156 | ns |
| Stress | Physical | 6.21 | 4 | .184 | .251 | ns |
| Stress | Psychological | 5.31 | 4 | .257 | .321 | ns |
| Stress | Social | 14.66 | 4 | .005 | .016 | * |
| Stress | Environmental | 4.17 | 4 | .384 | .411 | ns |
| Stress | General | 3.75 | 4 | .441 | .441 | ns |
References
- Bray, F; Laversanne, M; Sung, H; Ferlay, J; Siegel, RL; Soerjomataram, I; et al. Global Cancer Statistics 2022: GLOBOCAN Estimates of Incidence and Mortality Worldwide for 36 Cancers in 185 Countries. CA Cancer J Clin. 2024, 74(3), 229–263. [Google Scholar] [CrossRef] [PubMed]
- Penberthy, JK; Stewart, AL; Centeno, CF; Penberthy, DR. Psychological Aspects of Breast Cancer. Psychiatr Clin North Am. 2023, 46(3), 551–570. [Google Scholar] [CrossRef] [PubMed]
- Carreira, H; Williams, R; Müller, M; Harewood, R; Stanway, S; Bhaskaran, K. Associations between Breast Cancer Survivorship and Adverse Mental Health Outcomes: A Systematic Review. J Natl Cancer Inst. 2018, 110(12), 1311–1327. [Google Scholar] [CrossRef]
- Wang, YH; Li, JQ; Shi, JF; Que, JY; Liu, JJ; Lappin, JM; et al. Depression and Anxiety in Relation to Cancer Incidence and Mortality: A Systematic Review and Meta-Analysis of Cohort Studies. Mol Psychiatry 2020, 25(7), 1487–1499. [Google Scholar] [CrossRef]
- Mitchell, AJ; Chan, M; Bhatti, H; Halton, M; Grassi, L; Johansen, C; et al. Prevalence of Depression, Anxiety, and Adjustment Disorder in Oncological, Haematological, and Palliative-Care Settings: A Meta-Analysis of 94 Interview-Based Studies. Lancet Oncol. 2011, 12(2), 160–174. [Google Scholar] [CrossRef]
- Hayes, SC; Strosahl, KD; Wilson, KG. Acceptance and Commitment Therapy: The Process and Practice of Mindful Change, 2nd Ed ed; Guilford Press: New York, 2012. [Google Scholar]
- Bond, FW; Hayes, SC; Baer, RA; Carpenter, KM; Guenole, N; Orcutt, HK; et al. Preliminary Psychometric Properties of the Acceptance and Action Questionnaire-II: A Revised Measure of Psychological Inflexibility and Experiential Avoidance. Behav Ther. 2011, 42(4), 676–688. [Google Scholar] [CrossRef]
- Zhang, CQ; Leeming, E; Smith, P; Chung, PK; Hagger, MS; Hayes, SC. Acceptance and Commitment Therapy for Health Behavior Change: A Contextually-Driven Approach. Front Psychol. 2018, 8, 2350. [Google Scholar] [CrossRef]
- Fashler, SR; Weinrib, AZ; Azam, MA; Katz, J. The Use of Acceptance and Commitment Therapy in Oncology Settings: A Narrative Review. Psychol Rep. 2018, 121(2), 229–252. [Google Scholar] [CrossRef]
- Li, H; Wu, J; Ni, Q; Zhang, J; Wang, Y; He, G. Systematic Review and Meta-Analysis of Effectiveness of Acceptance and Commitment Therapy in Patients with Breast Cancer. Nurs Res. 2021, 70(4), E152–E160. [Google Scholar] [CrossRef]
- Johns, SA; Stutz, PV; Talib, TL; Cohee, AA; Beck-Coon, KA; Brown, LF; et al. Acceptance and Commitment Therapy for Breast Cancer Survivors with Fear of Cancer Recurrence: A 3-Arm Pilot Randomized Controlled Trial. Cancer 2020, 126(1), 211–218. [Google Scholar] [CrossRef] [PubMed]
- Ghorbani, V; Zanjani, Z; Omidi, A; Sarvizadeh, M. Efficacy of Acceptance and Commitment Therapy on Depression, Pain Acceptance, and Psychological Flexibility in Married Women with Breast Cancer: A Pre- and Post-Test Clinical Trial. Trends Psychiatry Psychother. 2021, 43(2), 126–133. [Google Scholar] [CrossRef]
- Yela, JR; Gómez-Martínez, MÁ; Crego, A; Jiménez-García, C. Reductions in Experiential Avoidance Explain Changes in Anxiety, Depression and Well-Being after a Mindfulness and Self-Compassion (MSC) Training. Psychol Psychother. 2022, 95(1), 72–86. [Google Scholar] [CrossRef] [PubMed]
- Mohammadkhani, P; Forouzan, AS; Hooshyari, Z; Abasi, I. The Role of Neuroticism and Experiential Avoidance in Predicting Anxiety and Depression Symptoms: Mediating Role of Emotion Regulation. Iran J Psychiatry Behav Sci. 2016, 10(3), E5047. [Google Scholar] [CrossRef]
- Klimczak, KS; San Miguel, GG; Mukasa, MN; Twohig, MP; Levin, ME. A Systematic Review and Meta-Analysis of Self-Guided Online Acceptance and Commitment Therapy as a Transdiagnostic Self-Help Intervention. Cogn Behav Ther. 2023, 52(3), 269–294. [Google Scholar] [CrossRef]
- Trindade, IA; Marta-Simões, J; Mendes, AL; Borrego, M; Ponte, A; Carvalho, C; et al. A Longitudinal Preliminary Analysis on the Role of Experiential Avoidance in Breast Cancer Patients’ Reported Health Outcomes. Psychooncology 2020, 29(4), 812–814. [Google Scholar] [CrossRef] [PubMed]
- Trindade, IA. Experiential Avoidance and Breast Cancer [Dataset]. In Mendeley Data; 2019. [Google Scholar] [CrossRef]
- Lovibond, SH; Lovibond, PF. Manual for the Depression Anxiety Stress Scales, 2nd Ed ed; Psychology Foundation of Australia: Sydney, 1995. [Google Scholar]
- The WHOQOL Group. Development of the World Health Organization WHOQOL-BREF Quality of Life Assessment. Psychol Med. 1998, 28(3), 551–558. [Google Scholar] [CrossRef]
- Akbari, M; Seydavi, M; Hosseini, ZS; Krafft, J; Levin, ME. Experiential Avoidance in Depression, Anxiety, Obsessive-Compulsive Related, and Posttraumatic Stress Disorders: A Comprehensive Systematic Review and Meta-Analysis. J Context Behav Sci. 2022, 24, 65–78. [Google Scholar] [CrossRef]
- Al-Abbadey, M; Tomescu-Stachie, S; Kaklamanou, D; Jarrett, N; Merwood, A; Tyndall, I; et al. The Role of Psychological Flexibility in Relation to Health Outcomes in People in Remission from Cancer. Br J Health Psychol. 2025, 30(3), E12807. [Google Scholar] [CrossRef]
- Tingley, D; Yamamoto, T; Hirose, K; Keele, L; Imai, K. Mediation: R Package for Causal Mediation Analysis. J Stat Softw. 2014, 59(5), 1–38. [Google Scholar] [CrossRef]
- Fritz, MS; MacKinnon, DP. Required Sample Size to Detect the Mediated Effect. Psychol Sci. 2007, 18(3), 233–239. [Google Scholar] [CrossRef]
- Donahue, ML; Levin, ME; Olson, K; Panza, E; Lillis, J. Examining the Role of Experiential Avoidance and Valued Action in the Negative Effects of Weight Self-Stigma. J Behav Med. 2023, 46(3), 517–524. [Google Scholar] [CrossRef]
- Bardeen, JR; Fergus, TA; Orcutt, HK. Experiential Avoidance as a Moderator of the Relationship between Anxiety Sensitivity and Perceived Stress. Behav Ther. 2013, 44(3), 459–469. [Google Scholar] [CrossRef]
- Panjwani, AA; Applebaum, AJ; Revenson, TA; Erblich, J; Rosenfeld, B. Intolerance of Uncertainty, Experiential Avoidance, and Trust in Physician: A Moderated Mediation Analysis of Emotional Distress in Advanced Cancer. J Behav Med. 2024, 47(1), 71–81. [Google Scholar] [CrossRef]
- Kashdan, TB; Morina, N; Priebe, S. Post-Traumatic Stress Disorder, Social Anxiety Disorder, and Depression in Survivors of the Kosovo War: Experiential Avoidance as a Contributor to Distress and Quality of Life. J Anxiety Disord. 2009, 23(2), 185–196. [Google Scholar] [CrossRef]
- Bullock, JG; Green, DP; Ha, SE. Yes, but What’s the Mechanism? (Don’t Expect an Easy Answer). J Pers Soc Psychol. 2010, 98(4), 550–558. [Google Scholar] [CrossRef] [PubMed]
- Stein, AT; Medina, JL; Rosenfield, D; Otto, MW; Smits, JAJ. Examining Experiential Avoidance as a Mediator of the Relation between Anxiety Sensitivity and Depressive Symptoms. Cogn Behav Ther. 2019, 49(1), 41–54. [Google Scholar] [CrossRef]
- Burgess, C; Cornelius, V; Love, S; Graham, J; Richards, M; Ramirez, A. Depression and Anxiety in Women with Early Breast Cancer: Five Year Observational Cohort Study. BMJ 2005, 330(7493), 702. [Google Scholar] [CrossRef] [PubMed]
- Lim, CC; Devi, MK; Ang, E. Anxiety in Women with Breast Cancer Undergoing Treatment: A Systematic Review. Int J Evid Based Healthc. 2011, 9(3), 215–235. [Google Scholar] [PubMed]
- Hughes, S; Jaremka, LM; Alfano, CM; Glaser, R; Povoski, SP; Lipari, AM; et al. Social Support Predicts Inflammation, Pain, and Depressive Symptoms: Longitudinal Relationships among Breast Cancer Survivors. Psychoneuroendocrinology 2014, 42, 38–44. [Google Scholar] [CrossRef]
- Marinkovic, M; Djordjevic, N; Djordjevic, L; Ignjatovic, N; Djordjevic, M; Karanikolic, V. Assessment of the Quality of Life in Breast Cancer Depending on the Surgical Treatment. Support Care Cancer 2021, 29(6), 3257–3266. [Google Scholar] [CrossRef]
- Simard, S; Thewes, B; Humphris, G; Dixon, M; Hayden, C; Mireskandari, S; et al. Fear of Cancer Recurrence in Adult Cancer Survivors: A Systematic Review of Quantitative Studies. J Cancer Surviv. 2013, 7(3), 300–322. [Google Scholar] [CrossRef]
- Brunault, P; Toledano, A; Aguerre, C; Suzanne, I; Garaud, P; Trzepidur-Edom, M; et al. Impact of Late Treatment-Related Radiotherapy Toxicity, Depression, and Anxiety on Quality of Life in Long-Term Breast Cancer Survivors. Bull Cancer 2012, 99(5), 589–598. [Google Scholar] [CrossRef]
- Riba, MB; Donovan, KA; Andersen, B; Braun, I; Breitbart, WS; Brewer, BW; et al. Distress Management, Version 3.2019, NCCN Clinical Practice Guidelines in Oncology. J Natl Compr Canc Netw. 2019, 17(10), 1229–1249. [Google Scholar] [CrossRef] [PubMed]
- Graham, CD; Gouick, J; Kravariti, E; Gillanders, D. A Systematic Review of the Use of Acceptance and Commitment Therapy (ACT) in Chronic Disease and Long-Term Conditions. Clin Psychol Rev. 2016, 46, 46–58. [Google Scholar] [CrossRef]
- Gonzalez-Fernandez, S; Fernandez-Rodriguez, C. Acceptance and Commitment Therapy in Cancer: Review of Applications and Findings. Behav Med. 2019, 45(3), 255–269. [Google Scholar] [CrossRef] [PubMed]
- MacKinnon, DP; Fairchild, AJ; Fritz, MS. Mediation Analysis. Annu Rev Psychol. 2007, 58, 593–614. [Google Scholar] [CrossRef]
- Hayes, AF. Introduction to Mediation, Moderation, and Conditional Process Analysis: A Regression-Based Approach, 3rd Ed ed; Guilford Press: New York, 2022. [Google Scholar]
- Cheng, HG; Phillips, MR. Secondary Analysis of Existing Data: Opportunities and Implementation. Shanghai Arch Psychiatry 2014, 26(6), 371–375. [Google Scholar]
- Doolan, DM; Froelicher, ES. Using an Existing Data Set to Answer New Research Questions: A Methodological Review. Res Theory Nurs Pract. 2009, 23(3), 203–215. [Google Scholar] [CrossRef] [PubMed]
- Hulbert-Williams, NJ; Storey, L; Wilson, KG. Psychological Interventions for Patients with Cancer: Psychological Flexibility and the Potential Utility of Acceptance and Commitment Therapy. Eur J Cancer Care 2015, 24(1), 15–27. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




