Submitted:
02 April 2026
Posted:
02 April 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Cognition in Older Adults
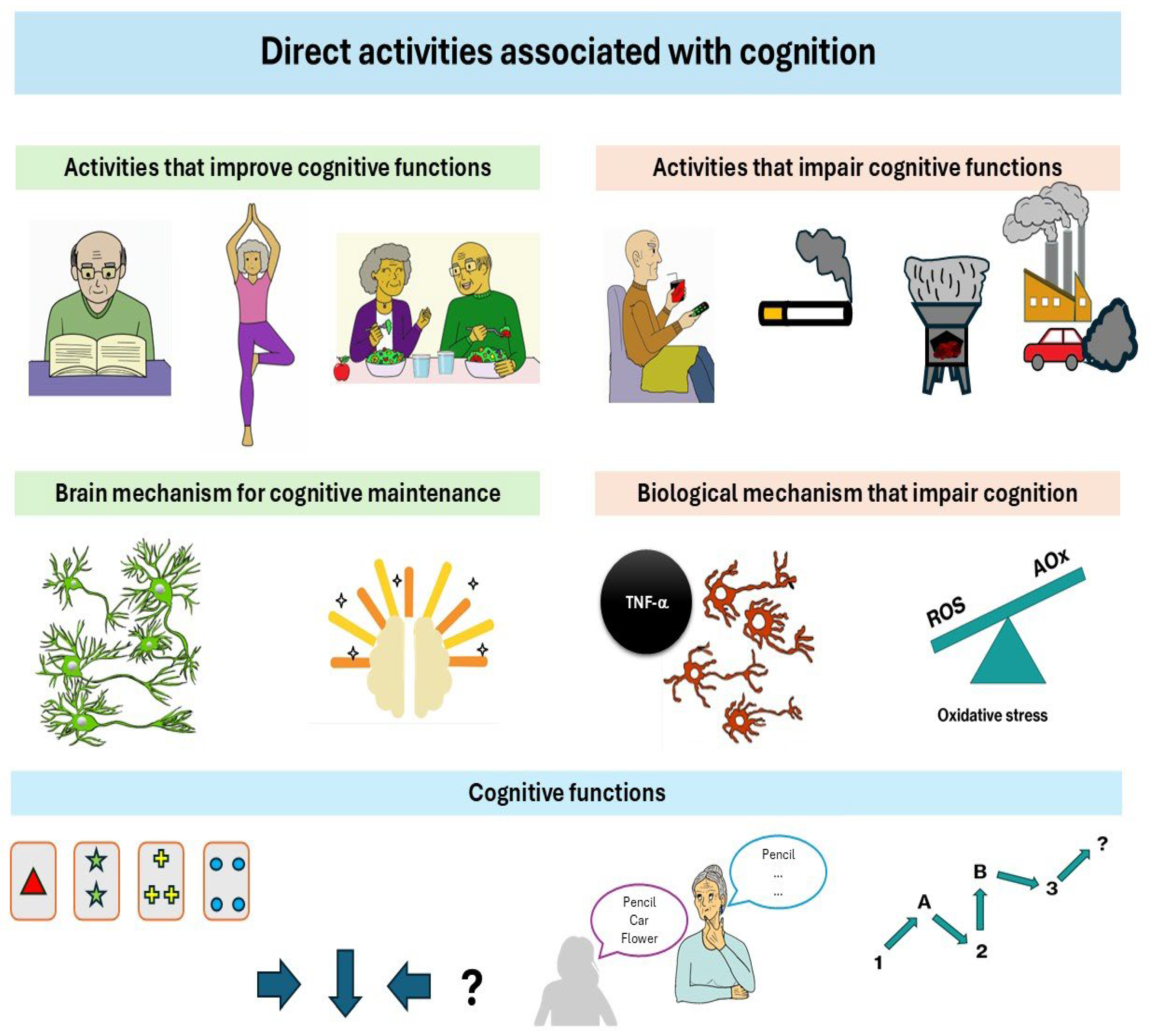
3. Direct Factors That Affect Cognitive Functions
3.1. Intellectually Stimulating Activities
3.2. Physical Activity and Exercise
3.3. Diet
3.4. Psychological Stress and Depression
3.4. Pollution
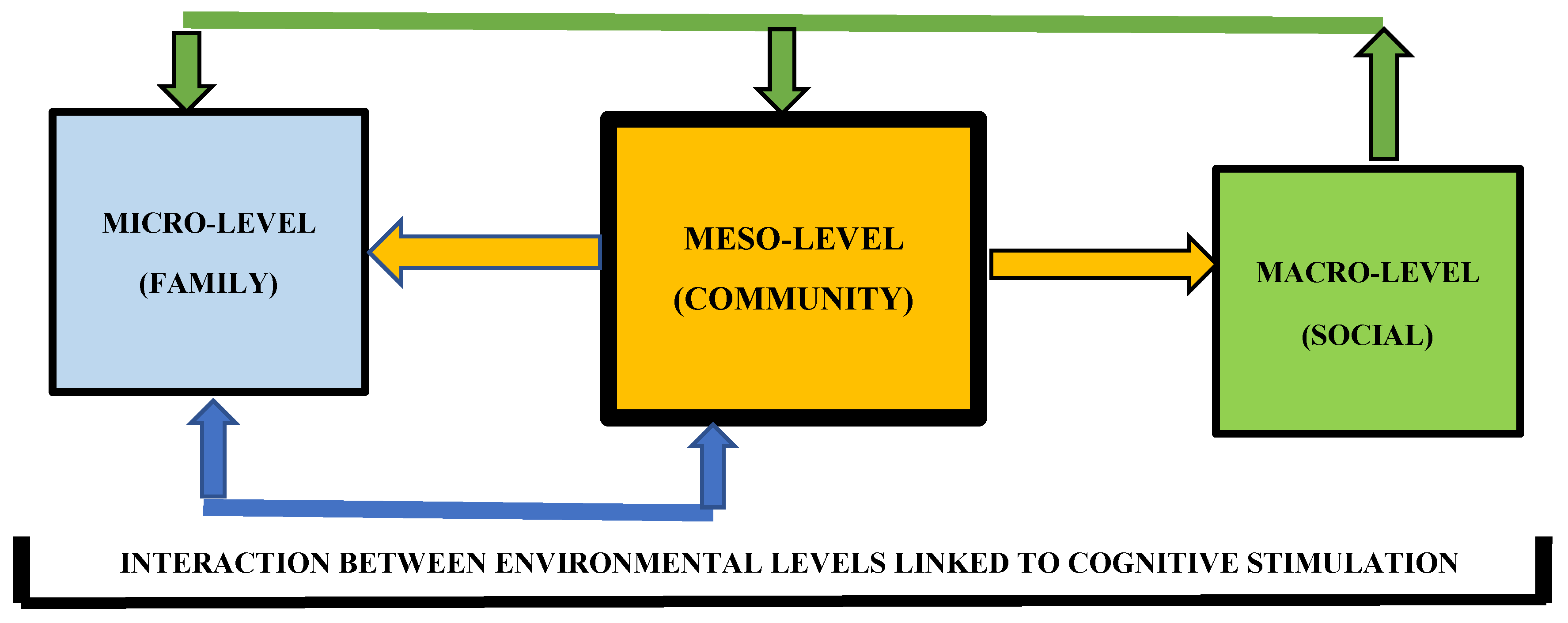
4. Relationship of Different Environmental Levels with Cognitive Functions
4.1. Environment Micro-Level (Family)
4.1.1. Social Interactions
4.1.2. Physical Elements of the Environment
4.2. Environment Meso-Level (Community)
4.2.1. Land Use Patterns
4.2.2. Transportation System
4.2.3. Environmental Design
4.2.4. Open Spaces
4.3. Environment Macro-Level (Social)
4.3.1. Ageism
4.3.2. Public Policies
5. Conclusions
Author Contributions
Funding
Conflicts of Interest
Abbreviations
| MCI | Mild Cognitive Impairment |
| PM | Particulate Matter |
| NO2 | Nitrogen Dioxide |
| ROS | Reactive Oxygen Species |
References
- World Health Organization. Ageing and Health; WHO: Geneva, 2021. [Google Scholar]
- World Health Organization. World Report on Ageing and Health; WHO: Geneva, 2015. [Google Scholar]
- O’Neill, D.J. Ageing Workforce: Sustaining the “Longevity Dividend.”. BMJ 2019, 367. [Google Scholar] [CrossRef]
- Olshansky, S.J.; Perry, D.; Miller, R.A.; Butler, R.N. Pursuing the Longevity Dividend: Scientific Goals for an Aging World. Ann. N. Y. Acad. Sci. 2007, 1114, 11–13. [Google Scholar] [CrossRef] [PubMed]
- Scott, A.J. Achieving a Three-Dimensional Longevity Dividend. Nat. Aging 2021, 1, 500–505. [Google Scholar] [CrossRef] [PubMed]
- Wiles, J.L.; Jayasinha, R. Care for Place: The Contributions Older People Make to Their Communities. J. Aging Stud. 2013, 27, 93–101. [Google Scholar] [CrossRef]
- Chen, P.W.; Chen, L.K.; Huang, H.K.; Loh, C.H. Productive Aging by Environmental Volunteerism: A Systematic Review. Arch. Gerontol. Geriatr. 2022, 98. [Google Scholar] [CrossRef] [PubMed]
- George, P.P.; Lun, P.; Ong, S.P.; Lim, W.S. A Rapid Review of the Measurement of Intrinsic Capacity in Older Adults. Journal of Nutrition, Health and Aging 2021, 25, 774–782. [Google Scholar] [CrossRef]
- Liang, Y.; Shang, S.; Gao, Y.; Zhai, J.; Cheng, X.; Yang, C.; Zhang, R. Measurements of Intrinsic Capacity in Older Adults: A Scoping Review and Quality Assessment. J. Am. Med. Dir. Assoc. 2023, 24, 267–276.e2. [Google Scholar] [CrossRef]
- Mendoza-Núñez, V.M.; Vivaldo-Martínez, M. Community Gerontology Model for Healthy Aging Developed in Mexico Framed in Resilience and Generativity. J. Cross. Cult. Gerontol. 2019, 34, 439–459. [Google Scholar] [CrossRef]
- Greenfield, E.A.; Black, K.; Buffel, T.; Yeh, J. Community Gerontology: A Framework for Research, Policy, and Practice on Communities and Aging. Gerontologist 2019, 59, 803–810. [Google Scholar] [CrossRef]
- Zhang, K.; Ma, Y.; Luo, Y.; Song, Y.; Xiong, G.; Ma, Y.; Sun, X.; Kan, C. Metabolic Diseases and Healthy Aging: Identifying Environmental and Behavioral Risk Factors and Promoting Public Health. Front. Public Health 2023, 11. [Google Scholar] [CrossRef]
- Hernández, E.D.; Cobo, E.A.; Cahalin, L.P.; Seron, P. Impact of Environmental Interventions Based on Social Programs on Physical Activity Levels: A Systematic Review. Front. Public Health 2023, 11. [Google Scholar] [CrossRef]
- Hernandez, E.D.; Guzman, C.A.; Seron, P. Interventions Based on Environmental Determinants for Nutritional and Physical Activity Behaviours in Colombia: A Scoping Review. BMJ Open 2022, 12. [Google Scholar] [CrossRef]
- Aliberti, S.M.; Capunzo, M. The Power of Environment: A Comprehensive Review of the Exposome’s Role in Healthy Aging, Longevity, and Preventive Medicine—Lessons from Blue Zones and Cilento. Nutrients 2025, 17. [Google Scholar] [CrossRef] [PubMed]
- Lawton, M.P. Environment and Other Determinants of Weil-Being in Older People. Gerontologist 1983, 23, 349–357. [Google Scholar] [CrossRef]
- Finlay, J.; Esposito, M.; Langa, K.M.; Judd, S.; Clarke, P. Cognability: An Ecological Theory of Neighborhoods and Cognitive Aging. Soc. Sci. Med. 2022, 309, 115220. [Google Scholar] [CrossRef] [PubMed]
- Chen, X.; Lee, C.; Huang, H. Neighborhood Built Environment Associated with Cognition and Dementia Risk among Older Adults: A Systematic Literature Review. Soc. Sci. Med. 2022, 292. [Google Scholar] [CrossRef]
- Da, L.; Song, X.; Jia, Z.; Myers, N.G.L.; Sun, J.; Wei, J.; Jung, D.; Li, F.; Song, S. Objectively Measured Environmental Features and Their Association with Cognition and Dementia: A Systematic Review and Meta-Analysis. Ageing Res. Rev. 2025, 104, 102630. [Google Scholar] [CrossRef]
- Wu, Y.T.; Prina, A.M.; Brayne, C. The Association between Community Environment and Cognitive Function: A Systematic Review. Soc. Psychiatry Psychiatr. Epidemiol. 2015, 50, 351–362. [Google Scholar] [CrossRef]
- Craik, F.I.M.; Bialystok, E. Cognition through the Lifespan: Mechanisms of Change. Trends Cogn. Sci. 2006, 10, 131–138. [Google Scholar] [CrossRef] [PubMed]
- Tucker-Drob, E.M.; Brandmaier, A.M.; Lindenberger, U. Coupled Cognitive Changes in Adulthood: A Meta-Analysis. Psychol. Bull. 2019, 145, 273–301. [Google Scholar] [CrossRef]
- Salthouse, T.A. Decomposing Age Correlations on Neuropsychological and Cognitive Variables. J Int Neuropsychol Soc 2009, 15, 650–661. [Google Scholar] [CrossRef]
- Sokolovič, L.; Hofmann, M.J.; Mohammad, N.; Kukolja, J. Neuropsychological Differential Diagnosis of Alzheimer’s Disease and Vascular Dementia: A Systematic Review with Meta-Regressions. Front. Aging Neurosci. 2023, 15. [Google Scholar] [CrossRef]
- Petersen, R. Mild Cognitive Impairment. Continuum (Minneap Minn) 2016, 22, 404–418. [Google Scholar] [CrossRef]
- Tangalos, E.G.; Petersen, R.C. Mild Cognitive Impairment in Geriatrics. Clin. Geriatr. Med. 2018, 34, 563–589. [Google Scholar] [CrossRef]
- Salthouse, T.A. Mental Exercise and Mental Aging: Evaluating the Validity of the “Use It or Lose It” Hypothesis. Perspect. Psychol. Sci. 2006, 1, 68–87. [Google Scholar] [CrossRef] [PubMed]
- Schooler, C. Use It-and Keep It, Longer, Probably: A Reply to Salthouse (2006). Perspect. Psychol. Sci. 2007, 2, 24–29. [Google Scholar] [CrossRef] [PubMed]
- Lindenberger, U.; Lövdén, M. Brain Plasticity in Human Lifespan Development: The Exploration–Selection–Refinement Model. Annu. Rev. Dev. Psychol. 2019, 1, 197–222. [Google Scholar] [CrossRef]
- Reuter-Lorenz, P.A.; Park, D.C. Cognitive Aging and the Life Course: A New Look at the Scaffolding Theory. Curr. Opin. Psychol. 2024, 56, 101781. [Google Scholar] [CrossRef]
- Lövdén, M.; Wenger, E.; Mårtensson, J.; Lindenberger, U.; Bäckman, L. Structural Brain Plasticity in Adult Learning and Development. Neurosci. Biobehav. Rev. 2013, 37, 2296–2310. [Google Scholar] [CrossRef] [PubMed]
- Park, D.C.; Reuter-Lorenz, P. The Adaptive Brain: Aging and Neurocognitive Scaffolding. Annu. Rev. Psychol. 2009, 60, 173–196. [Google Scholar] [CrossRef]
- Hou, J.; Jiang, T.; Fu, J.; Su, B.; Wu, H.; Sun, R.; Zhang, T. The Long-Term Efficacy of Working Memory Training in Healthy Older Adults: A Systematic Review and Meta-Analysis of 22 Randomized Controlled Trials. Journals of Gerontology - Series B Psychological Sciences and Social Sciences 2020, 75, E174–E188. [Google Scholar] [CrossRef] [PubMed]
- Nguyen, L.; Murphy, K.; Andrews, G. Immediate and Long-Term Efficacy of Executive Functions Cognitive Training in Older Adults: A Systematic Review and Meta-Analysis. Psychol. Bull. 2019, 145, 698–733. [Google Scholar] [CrossRef] [PubMed]
- Wei, Z.; Zhao, X.; Liu, Y. A Meta-Analysis of the Consequences of Cognitive Training on the Cognitive Function of Aged Mild Cognitive Impairment Patients. Psychogeriatrics 2024, 24, 1371–1388. [Google Scholar] [CrossRef]
- Basak, C.; Qin, S.; O’Connell, M.A. Differential Effects of Cognitive Training Modules in Healthy Aging and Mild Cognitive Impairment: A Comprehensive Meta-Analysis of Randomized Controlled Trials. Psychol. Aging 2020, 35, 220–249. [Google Scholar] [CrossRef]
- Melby-Lervåg, M.; Redick, T.S.; Hulme, C. Working Memory Training Does Not Improve Performance on Measures of Intelligence or Other Measures of “Far Transfer”: Evidence From a Meta-Analytic Review. Perspectives on Psychological Science 2016, 11, 512–534. [Google Scholar] [CrossRef]
- Teixeira-Santos, A.C.; Moreira, C.S.; Magalhães, R.; Magalhães, C.; Pereira, D.R.; Leite, J.; Carvalho, S.; Sampaio, A. Reviewing Working Memory Training Gains in Healthy Older Adults: A Meta-Analytic Review of Transfer for Cognitive Outcomes. Neurosci. Biobehav. Rev. 2019, 103, 163–177. [Google Scholar] [CrossRef]
- Wu, R.; Rodriguez, T.M.; Tavenner, B.P.; de Queiroz, I.F.L.; Boot, W.; Parisi, J.; Carlson, M.; Lövdén, M.; Beier, M.E.; Gow, A. Optimizing Cognitive Interventions to Improve Real-World Function for Healthy Older Adults. Eur. J. Ageing 2025, 22, 1–9. [Google Scholar] [CrossRef]
- Sánchez-Nieto, J.M.; De La Luz Martínez-Maldonado, M.; Lena, M.M.L.; Mendoza-Núñez, V.M. Effect of a Mental Stimulation Program of Computer and Internet Learning on Cognitive Functions and Wellbeing in Older Community-Dwelling Mexicans. Brain Sci. 2019, 9. [Google Scholar] [CrossRef]
- Gao, H.; Harris, J.; Maupin, D.; Schneider, S.; Hernandez, R.; Jin, H. Early Identification of Cognitive Impairment in Older Adults from Advanced Activities of Daily Living (AADL): A Scoping Review. Public Health 2025, 246. [Google Scholar] [CrossRef]
- Iizuka, A.; Suzuki, H.; Ogawa, S.; Kobayashi-Cuya, K.E.; Kobayashi, M.; Takebayashi, T.; Fujiwara, Y. Can Cognitive Leisure Activity Prevent Cognitive Decline in Older Adults? A Systematic Review of Intervention Studies. Geriatr. Gerontol. Int. 2019, 19, 469–482. [Google Scholar] [CrossRef] [PubMed]
- Cunha, C.; Voss, G.; Andrade, R.; Delerue-Matos, A. Is Formal Social Participation Associated with Cognitive Function in Middle-Aged and Older Adults? A Systematic Review with Meta-Analysis of Longitudinal Studies. Behavioral Sciences 2024, 14. [Google Scholar] [CrossRef] [PubMed]
- Sharifi, S.; Babaei Khorzoughi, K.; Rahmati, M. The Relationship between Volunteering and Cognitive Performance in Older Adults: A Systematic Review. Geriatr. Nurs. (Minneap). 2024, 55, 89–96. [Google Scholar] [CrossRef] [PubMed]
- Kelly, M.E.; Loughrey, D.; Lawlor, B.A.; Robertson, I.H.; Walsh, C.; Brennan, S. The Impact of Cognitive Training and Mental Stimulation on Cognitive and Everyday Functioning of Healthy Older Adults: A Systematic Review and Meta-Analysis. Ageing Res. Rev. 2014, 15, 28–43. [Google Scholar] [CrossRef] [PubMed]
- Gómez-Soria, I.; Iguacel, I.; Aguilar-Latorre, A.; Peralta-Marrupe, P.; Latorre, E.; Zaldívar, J.N.C.; Calatayud, E. Cognitive Stimulation and Cognitive Results in Older Adults: A Systematic Review and Meta-Analysis. Arch. Gerontol. Geriatr. 2023, 104. [Google Scholar] [CrossRef]
- Schwaighofer, M.; Fischer, F.; Bühner, M. Does Working Memory Training Transfer? A Meta-Analysis Including Training Conditions as Moderators. Educ. Psychol. 2015, 50, 138–166. [Google Scholar] [CrossRef]
- Carlson, M.C.; Parisi, J.M.; Xia, J.; Xue, Q.L.; Rebok, G.W.; Bandeen-Roche, K.; Fried, L.P. Lifestyle Activities and Memory: Variety May Be the Spice of Life. The Women’s Health and Aging Study II. Journal of the International Neuropsychological Society 2012, 18, 286–294. [Google Scholar] [CrossRef]
- Noice, H.; Noice, T. An Arts Intervention for Older Adults Living in Subsidized Retirement Homes. Aging, Neuropsychology, and Cognition 2008, 16, 56–79. [Google Scholar] [CrossRef]
- Zhao, Y.; Li, Y.; Wang, L.; Song, Z.; Di, T.; Dong, X.; Song, X.; Han, X.; Zhao, Y.; Wang, B.; et al. Physical Activity and Cognition in Sedentary Older Adults: A Systematic Review and Meta-Analysis. Journal of Alzheimer’s Disease 2022, 87, 957–968. [Google Scholar] [CrossRef]
- Gallardo-Gómez, D.; del Pozo-Cruz, J.; Noetel, M.; Álvarez-Barbosa, F.; Alfonso-Rosa, R.M.; del Pozo Cruz, B. Optimal Dose and Type of Exercise to Improve Cognitive Function in Older Adults: A Systematic Review and Bayesian Model-Based Network Meta-Analysis of RCTs. Ageing Res. Rev. 2022, 76. [Google Scholar] [CrossRef]
- Northey, J.M.; Cherbuin, N.; Pumpa, K.L.; Smee, D.J.; Rattray, B. Exercise Interventions for Cognitive Function in Adults Older than 50: A Systematic Review with Meta-Analysis. Br. J. Sports Med. 2018, 52, 154–160. [Google Scholar] [CrossRef]
- Cheng, A.; Zhao, Z.; Liu, H.; Yang, J.; Luo, J. The Physiological Mechanism and Effect of Resistance Exercise on Cognitive Function in the Elderly People. Front. Public Health 2022, 10. [Google Scholar] [CrossRef]
- Mahalakshmi, B.; Maurya, N.; Da Lee, S.; Kumar, V.B. Possible Neuroprotective Mechanisms of Physical Exercise in Neurodegeneration. Int. J. Mol. Sci. 2020, 21, 1–17. [Google Scholar] [CrossRef]
- Puri, S.; Shaheen, M.; Grover, B. Nutrition and Cognitive Health: A Life Course Approach. Front. Public Health 2023, 11. [Google Scholar] [CrossRef] [PubMed]
- Gavelin, H.M.; Dong, C.; Minkov, R.; Bahar-Fuchs, A.; Ellis, K.A.; Lautenschlager, N.T.; Mellow, M.L.; Wade, A.T.; Smith, A.E.; Finke, C.; et al. Combined Physical and Cognitive Training for Older Adults with and without Cognitive Impairment: A Systematic Review and Network Meta-Analysis of Randomized Controlled Trials. Ageing Res. Rev. 2021, 66. [Google Scholar] [CrossRef] [PubMed]
- Dominguez, L.J.; Veronese, N.; Vernuccio, L.; Catanese, G.; Inzerillo, F.; Salemi, G.; Barbagallo, M. Nutrition, Physical Activity, and Other Lifestyle Factors in the Prevention of Cognitive Decline and Dementia. Nutrients 2021, 13. [Google Scholar] [CrossRef]
- Pei, H.; Liu, S.; Li, L.; Zhou, M. Association of Dietary Pattern and Cognitive Function in the Elderly: A Systematic Review and Meta-Analysis. Geriatr. Nurs. (Minneap). 2025, 63, 470–475. [Google Scholar] [CrossRef] [PubMed]
- Loughrey, D.G.; Lavecchia, S.; Brennan, S.; Lawlor, B.A.; Kelly, M.E. The Impact of the Mediterranean Diet on the Cognitive Functioning of Healthy Older Adults: A Systematic Review and Meta-Analysis. Advances in Nutrition 2017, 8, 571–586. [Google Scholar] [CrossRef]
- Gillespie, K.M.; White, M.J.; Kemps, E.; Moore, H.; Dymond, A.; Bartlett, S.E. The Impact of Free and Added Sugars on Cognitive Function: A Systematic Review and Meta-Analysis. Nutrients 2024, 16. [Google Scholar] [CrossRef]
- Taylor, Z.B.; Stevenson, R.J.; Ehrenfeld, L.; Francis, H.M. The Impact of Saturated Fat, Added Sugar and Their Combination on Human Hippocampal Integrity and Function: A Systematic Review and Meta-Analysis. Neurosci. Biobehav. Rev. 2021, 130, 91–106. [Google Scholar] [CrossRef]
- Liu, H.; Liu, Y.; Shi, M.; Zhou, Y.; Zhao, Y.; Xia, Y. Meta-Analysis of Sugar-Sweetened Beverage Intake and the Risk of Cognitive Disorders. J. Affect. Disord. 2022, 313, 177–185. [Google Scholar] [CrossRef]
- Chen, X.; Maguire, B.; Brodaty, H.; O’Leary, F. Dietary Patterns and Cognitive Health in Older Adults: A Systematic Review. Journal of Alzheimer’s Disease 2019, 67, 583–619. [Google Scholar] [CrossRef]
- Zheng, B.; Tal, R.; Yang, Z.; Middleton, L.; Udeh-Momoh, C. Cortisol Hypersecretion and the Risk of Alzheimer’s Disease: A Systematic Review and Meta-Analysis. Ageing Res. Rev. 2020, 64. [Google Scholar] [CrossRef]
- Resmini, E.; Santos, A.; Webb, S.M. Cortisol Excess and the Brain. Front. Horm. Res. 2016, 46, 74–86. [Google Scholar] [CrossRef] [PubMed]
- Gardner, M.; Lightman, S.; Kuh, D.; Comijs, H.; Deeg, D.; Gallacher, J.; Geoffroy, M.C.; Kivimaki, M.; Kumari, M.; Power, C.; et al. Dysregulation of the Hypothalamic Pituitary Adrenal (HPA) Axis and Cognitive Capability at Older Ages: Individual Participant Meta-Analysis of Five Cohorts. Sci. Rep. 2019, 9. [Google Scholar] [CrossRef] [PubMed]
- Orihashi, R.; Imamura, Y.; Yamada, S.; Monji, A.; Mizoguchi, Y. Association between Cortisol and Aging-Related Hippocampus Volume Changes in Community-Dwelling Older Adults: A 7-Year Follow-up Study. BMC Geriatr. 2022, 22. [Google Scholar] [CrossRef]
- Mourao, R.J.; Mansur, G.; Malloy-Diniz, L.F.; Castro Costa, E.; Diniz, B.S. Depressive Symptoms Increase the Risk of Progression to Dementia in Subjects with Mild Cognitive Impairment: Systematic Review and Meta-Analysis. Int. J. Geriatr. Psychiatry 2016, 31, 905–911. [Google Scholar] [CrossRef] [PubMed]
- Bergmann, E.; Harlev, D.; Wolpe, N. Depressive Symptoms Are Linked to Age-Specific Neuroanatomical and Cognitive Variations. J. Affect. Disord. 2025, 369, 1013–1020. [Google Scholar] [CrossRef]
- Chalmers, R.A.; Cervin, M.; Choo, C.; Baune, B.T.; Trollor, J.N.; Numbers, K.; Sachdev, P.S.; Brodaty, H.; Kochan, N.A.; Medvedev, O.N. Networks of Inflammation, Depression, and Cognition in Aging Males and Females. Aging Clinical and Experimental Research 2022, 2022 34 34, 2387–2398. [Google Scholar] [CrossRef]
- Gałecki, P.; Talarowska, M.; Anderson, G.; Berk, M.; Maes, M. Mechanisms Underlying Neurocognitive Dysfunctions in Recurrent Major Depression. Med. Sci. Monit. 2015, 21, 1535–1547. [Google Scholar] [CrossRef]
- Thompson, R.; Smith, R.B.; Karim, Y.B.; Shen, C.; Drummond, K.; Teng, C.; Toledano, M.B. Air Pollution and Human Cognition: A Systematic Review and Meta-Analysis. Science of the Total Environment 2023, 859. [Google Scholar] [CrossRef]
- Chandra, M.; Rai, C.B.; Kumari, N.; Sandhu, V.K.; Chandra, K.; Krishna, M.; Kota, S.H.; Anand, K.S.; Oudin, A. Air Pollution and Cognitive Impairment across the Life Course in Humans: A Systematic Review with Specific Focus on Income Level of Study Area. Int. J. Environ. Res. Public Health 2022, 19. [Google Scholar] [CrossRef] [PubMed]
- Andrade, A.; D’Oliveira, A.; De Souza, L.C.; Bastos, A.C.R. de F.; Dominski, F.H.; Stabile, L.; Buonanno, G. Effects of Air Pollution on the Health of Older Adults during Physical Activities: Mapping Review. Int. J. Environ. Res. Public Health 2023, 20. [Google Scholar] [CrossRef]
- Ma, Y.H.; Chen, H.S.; Liu, C.; Feng, Q.S.; Feng, L.; Zhang, Y.R.; Hu, H.; Dong, Q.; Tan, L.; Kan, H.D.; et al. Association of Long-Term Exposure to Ambient Air Pollution With Cognitive Decline and Alzheimer’s Disease–Related Amyloidosis. Biol. Psychiatry 2023, 93, 780–789. [Google Scholar] [CrossRef]
- Iaccarino, L.; La Joie, R.; Lesman-Segev, O.H.; Lee, E.; Hanna, L.; Allen, I.E.; Hillner, B.E.; Siegel, B.A.; Whitmer, R.A.; Carrillo, M.C.; et al. Association between Ambient Air Pollution and Amyloid Positron Emission Tomography Positivity in Older Adults with Cognitive Impairment. JAMA Neurol. 2021, 78, 197–207. [Google Scholar] [CrossRef]
- Haghighi, P.; Littler, E.A.L.; Mauer-Vakil, D.; Miller, M.; Oremus, M. Exploring the Relationship between Marital Quality and Cognitive Function: A Systematic Review. Soc. Sci. Med. 2024, 355. [Google Scholar] [CrossRef]
- Sharifi, S.; Babaei Khorzoughi, K.; Khaledi-Paveh, B.; Rahmati, M. Association of Intergenerational Relationship and Supports with Cognitive Performance in Older Adults: A Systematic Review. Geriatr. Nurs. (Minneap). 2023, 52, 146–151. [Google Scholar] [CrossRef]
- Luo, K.; Wei, D.; He, B.; Fei, Y. Association between the Indoor Visual Environment and Cognition in Older Adults: A Systematic Review. Buildings 2024, 14, 3066. [Google Scholar] [CrossRef]
- Yang, Q.; Yang, J.; Zheng, L.; Song, W.; Yi, L. Impact of Home Parenting Environment on Cognitive and Psychomotor Development in Children Under 5 Years Old: A Meta-Analysis. Front. Pediatr. 2021, 9, 658094. [Google Scholar] [CrossRef]
- Hale, K.; Østbye, T.; Perera, B.; Bradley, R.; Maselko, J. A Novel Adaptation of the HOME Inventory for Elders: The Importance of the Home Environment Across the Life Course. International Journal of Environmental Research and Public Health 2019, 16, 2826. [Google Scholar] [CrossRef] [PubMed]
- Meng, H.; Lv, X.; Zhang, R.; Feng, Y.; Wang, J.; Liu, J.; Zhang, J. Occurrence and Risk Factors for Cognitive Decline Shared by Couples: A Systematic Review and Meta-Analysis. J. Alzheimers Dis. 2024, 100, 29–40. [Google Scholar] [CrossRef] [PubMed]
- Singham, T.; Bell, G.; Saunders, R.; Stott, J. Widowhood and Cognitive Decline in Adults Aged 50 and over: A Systematic Review and Meta-Analysis. Ageing Res. Rev. 2021, 71. [Google Scholar] [CrossRef]
- Zhao, D.; Li, J.; Fu, P.; Hao, W.; Yuan, Y.; Yu, C.; Jing, Z.; Wang, Y.; Zhou, C. Cognitive Frailty and Suicidal Ideation among Chinese Rural Empty-Nest Older Adults: Parent-Child Geographic Proximity as a Possible Moderator? J. Affect. Disord. 2021, 282, 348–353. [Google Scholar] [CrossRef] [PubMed]
- Harrington, K.D.; Vasan, S.; Kang, J.E.; Sliwinski, M.J.; Lim, M.H. Loneliness and Cognitive Function in Older Adults Without Dementia: A Systematic Review and Meta-Analysis. Journal of Alzheimer’s Disease 2023, 91, 1243–1259. [Google Scholar] [CrossRef]
- Lee, J.H.; Sutin, A.R.; Hajek, A.; Karakose, S.; Aschwanden, D.; O’Súilleabháin, P.S.; Stephan, Y.; Terracciano, A.; Luchetti, M. Loneliness and Cognition in Older Adults: A Meta-Analysis of Harmonized Studies from the United States, England, India, China, South Africa, Mexico, and Chile. Psychol. Med. 2025, 55. [Google Scholar] [CrossRef]
- Ryan, R.M.; Deci, E.L. Intrinsic and Extrinsic Motivation from a Self-Determination Theory Perspective: Definitions, Theory, Practices, and Future Directions. Contemp. Educ. Psychol. 2020, 61, 101860. [Google Scholar] [CrossRef]
- Ryff, C.D. Psychological Well-Being Revisited: Advances in the Science and Practice of Eudaimonia. Psychother. Psychosom. 2014, 83, 10–28. [Google Scholar] [CrossRef] [PubMed]
- Zou, C.; Amos-Richards, D.; Jagannathan, R.; Kulshreshtha, A. Effect of Home-Based Lifestyle Interventions on Cognition in Older Adults with Mild Cognitive Impairment: A Systematic Review. BMC Geriatrics 2024, 24, 1–11. [Google Scholar] [CrossRef]
- Silva, R.; Bobrowicz-Campos, E.; Santos-Costa, P.; Cruz, A.R.; Apóstolo, J. A Home-Based Individual Cognitive Stimulation Program for Older Adults With Cognitive Impairment: A Randomized Controlled Trial. Front. Psychol. 2021, 12. [Google Scholar] [CrossRef] [PubMed]
- Saenz, J.L.; Adar, S.D.; Zhang, Y.S.; Wilkens, J.; Chattopadhyay, A.; Lee, J.; Wong, R. Household Use of Polluting Cooking Fuels and Late-Life Cognitive Function: A Harmonized Analysis of India, Mexico, and China. Environ. Int. 2021, 156, 106722. [Google Scholar] [CrossRef]
- Shaw, S.; Kundu, S.; Chattopadhyay, A.; Rao, S. Indoor Air Pollution and Cognitive Function among Older Adults in India: A Multiple Mediation Approach through Depression and Sleep Disorders. BMC Geriatr. 2024, 24, 1–13. [Google Scholar] [CrossRef]
- Luo, H.; Hu, H.; Zheng, Z.; Sun, C.; Yu, K. The Impact of Living Environmental Factors on Cognitive Function and Mild Cognitive Impairment: Evidence from the Chinese Elderly Population. BMC Public Health 2024, 24, 1–11. [Google Scholar] [CrossRef]
- Wang, M.; Cho, Y.; Li, J. Air Pollution and Sleep Health in Middle-Aged and Older Adults: A Systematic Review and Meta-Analysis. Sleep Med. Rev. 2025, 83. [Google Scholar] [CrossRef]
- Li, L.; Yang, A.; He, X.; Liu, J.; Ma, Y.; Niu, J.; Luo, B. Indoor Air Pollution from Solid Fuels and Hypertension: A Systematic Review and Meta-Analysis. Environmental Pollution 2020, 259. [Google Scholar] [CrossRef]
- Zhang, X.; Ding, L.; Yang, F.; Qiao, G.; Gao, X.; Xiong, Z.; Zhu, X. Association between Indoor Air Pollution and Depression: A Systematic Review and Meta-Analysis of Cohort Studies. BMJ Open 2024, 14. [Google Scholar] [CrossRef]
- Wang, W.; Chen, J.; Jin, X.; Ping, Y.; Wu, C. Association between Indoor Ventilation Frequency and Cognitive Function among Community-Dwelling Older Adults in China: Results from the Chinese Longitudinal Healthy Longevity Survey. BMC Geriatr. 2022, 22, 1–9. [Google Scholar] [CrossRef] [PubMed]
- Yeo, N.L.; Elliott, L.R.; Bethel, A.; White, M.P.; Dean, S.G.; Garside, R. Indoor Nature Interventions for Health and Wellbeing of Older Adults in Residential Settings: A Systematic Review. Gerontologist 2020, 60, e184–e199. [Google Scholar] [CrossRef] [PubMed]
- Hou, K.; Xu, X. Ambient Temperatures Associated with Reduced Cognitive Function in Older Adults in China. Sci. Rep. 2023, 13. [Google Scholar] [CrossRef] [PubMed]
- Baniassadi, A.; Yu, W.; Travison, T.; Day, R.; Lipsitz, L.; Manor, B. Home Ambient Temperature and Self-Reported Attention in Community-Dwelling Older Adults. The Journals of Gerontology: Series A 2025, 80, 286. [Google Scholar] [CrossRef]
- Trezza, B.M.; Apolinario, D.; de Oliveira, R.S.; Busse, A.L.; Gonçalves, F.L.T.; Saldiva, P.H.N.; Jacob-Filho, W. Environmental Heat Exposure and Cognitive Performance in Older Adults: A Controlled Trial. Age (Dordr). 2015, 37. [Google Scholar] [CrossRef]
- Melin, L.; Götestam, K.G. THE EFFECTS OF REARRANGING WARD ROUTINES ON COMMUNICATION AND EATING BEHAVIORS OF PSYCHOGERIATRIC PATIENTS. J. Appl. Behav. Anal. 1981, 14, 47–51. [Google Scholar] [CrossRef]
- Marquardt, G.; Schmieg, P. Dementia-Friendly Architecture: Environments That Facilitate Wayfinding in Nursing Homes. Am. J. Alzheimers Dis. Other Demen. WEBSITE:WEBSITE:SAGE;JOURNAL:JOURNAL:AJAE;WGROUP:STRING:PUBLICATION. 2009, 24, 333–340. [Google Scholar] [CrossRef]
- Motzek, T.; Bueter, K.; Marquardt, G. Environmental Cues in Double-Occupancy Rooms to Support Patients With Dementia. HERD 2016, 9, 106–115. [Google Scholar] [CrossRef]
- Wang, Z.Y.; Cho, J.Y. Older Adults’ Response to Color Visibility in Indoor Residential Environment Using Eye-Tracking Technology. Sensors (Basel) 2022, 22. [Google Scholar] [CrossRef]
- Motzek, T.; Bueter, K.; Marquardt, G. Investigation of Eligible Picture Categories for Use as Environmental Cues in Dementia-Sensitive Environments. HERD 2017, 10, 64–73. [Google Scholar] [CrossRef] [PubMed]
- Hwang, Y.R. Influence of Building Materials with Directional Textures on the Visual Perceptions of Elderly with Alzheimer’s Disease. Int. J. Gerontol. 2014, 8, 147–151. [Google Scholar] [CrossRef]
- Dickinson, J.I.; McLain-Kark, J.; Marshall-Baker, A. The Effects of Visual Barriers on Exiting Behavior in a Dementia Care Unit. Gerontologist 1995, 35, 127–130. [Google Scholar] [CrossRef]
- Wideman, T.H.; Sullivan, M.J.L. Built Environment. Encyclopedia of Behavioral Medicine 2020, 312–314. [Google Scholar] [CrossRef]
- Song, Y.; Liu, Y.; Bai, X.; Yu, H. Effects of Neighborhood Built Environment on Cognitive Function in Older Adults: A Systematic Review. BMC Geriatr. 2024, 24. [Google Scholar] [CrossRef]
- Wu, Y.T.; Prina, A.M.; Jones, A.; Matthews, F.E.; Brayne, C. The Built Environment and Cognitive Disorders: Results From the Cognitive Function and Ageing Study II. Am. J. Prev. Med. 2017, 53, 25–32. [Google Scholar] [CrossRef]
- Wu, Y.T.; Prina, A.M.; Jones, A.P.; Barnes, L.E.; Matthews, F.E.; Brayne, C. Community Environment, Cognitive Impairment and Dementia in Later Life: Results from the Cognitive Function and Ageing Study. Age Ageing 2015, 44, 1005–1011. [Google Scholar] [CrossRef]
- Ng, T.P.; Nyunt, M.S.Z.; Shuvo, F.K.; Eng, J.Y.; Yap, K.B.; Hee, L.M.; Chan, S.P.; Scherer, S. The Neighborhood Built Environment and Cognitive Function of Older Persons: Results from the Singapore Longitudinal Ageing Study. Gerontology 2018, 64, 149–156. [Google Scholar] [CrossRef] [PubMed]
- Motohiro, A.; Abe, T.; Okuyama, K.; Onoda, K.; Ito, T.; Isomura, M.; Nabika, T.; Kumakura, S. Environmental Factors Affecting Cognitive Function among Community-Dwelling Older Adults: A Longitudinal Study. Int. J. Environ. Res. Public Health 2021, 18. [Google Scholar] [CrossRef]
- Wu, Y.T.; Brayne, C.; Liu, Z.; Huang, Y.; Sosa, A.L.; Acosta, D.; Prina, M. Neighbourhood Environment and Dementia in Older People from High-, Middle- And Low-Income Countries: Results from Two Population-Based Cohort Studies. BMC Public Health 2020, 20. [Google Scholar] [CrossRef]
- Chan, O.F.; Liu, Y.; Guo, Y.; Lu, S.; Chui, C.H.K.; Ho, H.C.; Song, Y.; Cheng, W.; Chiu, R.L.H.; Webster, C.; et al. Neighborhood Built Environments and Cognition in Later Life. Aging Ment. Health 2023, 27, 466–474. [Google Scholar] [CrossRef] [PubMed]
- Clarke, P.J.; Ailshire, J.A.; House, J.S.; Morenoff, J.D.; King, K.; Melendez, R.; Langa, K.M. Cognitive Function in the Community Setting: The Neighbourhood as a Source of “Cognitive Reserve”? J. Epidemiol. Community Health (1978) 2012, 66, 730–736. [Google Scholar] [CrossRef]
- Guo, Y.; Chan, C.H.; Chang, Q.; Liu, T.; Yip, P.S.F. Neighborhood Environment and Cognitive Function in Older Adults: A Multilevel Analysis in Hong Kong. Health Place 2019, 58, 102146. [Google Scholar] [CrossRef]
- Besser, L.M.; Rodriguez, D.A.; McDonald, N.; Kukull, W.A.; Fitzpatrick, A.L.; Rapp, S.R.; Seeman, T. Neighborhood Built Environment and Cognition in Non-Demented Older Adults: The Multi-Ethnic Study of Atherosclerosis. Soc. Sci. Med. 2018, 200, 27–35. [Google Scholar] [CrossRef]
- Katayama, O.; Lee, S.; Makino, K.; Chiba, I.; Bae, S.; Shinkai, Y.; Harada, K.; Shimada, H. The Association between Neighborhood Amenities and Cognitive Function: Role of Lifestyle Activities. J. Clin. Med. 2020, 9, 1–12. [Google Scholar] [CrossRef]
- Tani, Y.; Suzuki, N.; Fujiwara, T.; Hanazato, M.; Kondo, K. Neighborhood Food Environment and Dementia Incidence: The Japan Gerontological Evaluation Study Cohort Survey. Am. J. Prev. Med. 2019, 56, 383–392. [Google Scholar] [CrossRef]
- Kim, B.; Thorpe, R.J.; Szanton, S.L.; Adkins-Jackson, P.B.; Samuel, L.J. Disparities in Neighborhood Food Environment and Cognitive Decline among US Older Adults: A Cohort Study. BMC Med. 2025, 23, 259. [Google Scholar] [CrossRef] [PubMed]
- Watts, A.; Ferdous, F.; Moore, K.D.; Burns, J.M. Neighborhood Integration and Connectivity Predict Cognitive Performance and Decline. Gerontol. Geriatr. Med. 2015. [Google Scholar] [CrossRef] [PubMed]
- Luo, Y.; Zhang, L.; Pan, X. Neighborhood Environments and Cognitive Decline among Middle-Aged and Older People in China. Journals of Gerontology - Series B Psychological Sciences and Social Sciences 2019, 74, e60–e71. [Google Scholar] [CrossRef]
- Besser, L.; Galvin, J.E.; Rodriguez, D.; Seeman, T.; Kukull, W.; Rapp, S.R.; Smith, J. Associations between Neighborhood Built Environment and Cognition Vary by Apolipoprotein E Genotype: Multi-Ethnic Study of Atherosclerosis. Health Place 2019, 60. [Google Scholar] [CrossRef]
- Yu, W.; Esposito, M.; Li, M.; Clarke, P.; Judd, S.; Finlay, J. Neighborhood ‘Disamenities’: Local Barriers and Cognitive Function among Black and White Aging Adults. BMC Public Health 2023, 23. [Google Scholar] [CrossRef]
- Yang, T.C.; Kim, S.; Choi, S. won E.; Halloway, S.; Mitchell, U.A.; Shaw, B.A. Neighborhood Features and Cognitive Function: Moderating Roles of Individual Socioeconomic Status. Am. J. Prev. Med. 2024, 66, 454–462. [Google Scholar] [CrossRef]
- Chen, H.; Kwong, J.C.; Copes, R.; Tu, K.; Villeneuve, P.J.; van Donkelaar, A.; Hystad, P.; Martin, R. V.; Murray, B.J.; Jessiman, B.; et al. Living near Major Roads and the Incidence of Dementia, Parkinson’s Disease, and Multiple Sclerosis: A Population-Based Cohort Study. The Lancet 2017, 389, 718–726. [Google Scholar] [CrossRef]
- Yuchi, W.; Sbihi, H.; Davies, H.; Tamburic, L.; Brauer, M. Road Proximity, Air Pollution, Noise, Green Space and Neurologic Disease Incidence: A Population-Based Cohort Study. Environ. Health 2020, 19. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Jin, X.; Cao, K.; Zhao, M.; Zhu, T.; Zhang, J.; Zeng, Y. Residential Proximity to Major Roadways and Cognitive Function among Chinese Adults 65 Years and Older. Science of the Total Environment 2021, 766. [Google Scholar] [CrossRef]
- Wellenius, G.A.; Boyle, L.D.; Coull, B.A.; Milberg, W.P.; Gryparis, A.; Schwartz, J.; Mittleman, M.A.; Lipsitz, L.A. Residential Proximity to Nearest Major Roadway and Cognitive Function in Community-Dwelling Seniors: Results from the Mobilize Boston Study. J. Am. Geriatr. Soc. 2012, 60, 2075–2080. [Google Scholar] [CrossRef] [PubMed]
- Hyun, J.; Lovasi, G.S.; Katz, M.J.; Derby, C.A.; Lipton, R.B.; Sliwinski, M.J. Perceived but Not Objective Measures of Neighborhood Safety and Food Environments Are Associated with Longitudinal Changes in Processing Speed among Urban Older Adults. BMC Geriatr. 2024, 24. [Google Scholar] [CrossRef]
- Lee, H.; Waite, L.J. Cognition in Context: The Role of Objective and Subjective Measures of Neighborhood and Household in Cognitive Functioning in Later Life. Gerontologist 2018, 58, 159–169. [Google Scholar] [CrossRef] [PubMed]
- Zaheed, A.B.; Sharifian, N.; Kraal, A.Z.; Sol, K.; Hence, A.; Zahodne, L.B. Unique Effects of Perceived Neighborhood Physical Disorder and Social Cohesion on Episodic Memory and Semantic Fluency. Archives of Clinical Neuropsychology 2019, 34, 1346–1355. [Google Scholar] [CrossRef]
- Estrella, M.L.; Durazo-Arvizu, R.A.; Gallo, L.C.; Isasi, C.R.; Perreira, K.M.; Vu, T.H.T.; Vasquez, E.; Sachdeva, S.; Zeng, D.; Llabre, M.M.; et al. Associations between Perceived Neighborhood Environment and Cognitive Function among Middle-Aged and Older Women and Men: Hispanic Community Health Study/Study of Latinos Sociocultural Ancillary Study. Soc. Psychiatry Psychiatr. Epidemiol. 2020, 55, 685–696. [Google Scholar] [CrossRef]
- Abhijith, K. V.; Kumar, P.; Gallagher, J.; McNabola, A.; Baldauf, R.; Pilla, F.; Broderick, B.; Di Sabatino, S.; Pulvirenti, B. Air Pollution Abatement Performances of Green Infrastructure in Open Road and Built-up Street Canyon Environments – A Review. Atmos. Environ. 2017, 162, 71–86. [Google Scholar] [CrossRef]
- Liu, S.; Ho, H.C.; Wilson, J.P. Effects of Urban Green Space on Human Cognition: A Systematic Search and Scoping Review. Urban Clim. 2025, 60, 102372. [Google Scholar] [CrossRef]
- Hu, X.; Wang, J.; Yang, T.; Jin, J.; Zeng, Q.; Aboubakri, O.; Feng, X.L.; Li, G.; Huang, J. Role of Residential Greenspace in the Trajectory of Major Neurological Disorders: A Longitudinal Study in UK Biobank. Science of The Total Environment 2024, 912, 168967. [Google Scholar] [CrossRef]
- Paul, L.A.; Hystad, P.; Burnett, R.T.; Kwong, J.C.; Crouse, D.L.; van Donkelaar, A.; Tu, K.; Lavigne, E.; Copes, R.; Martin, R. V.; et al. Urban Green Space and the Risks of Dementia and Stroke. Environ. Res. 2020, 186. [Google Scholar] [CrossRef]
- Astell-Burt, T.; Navakatikyan, M.A.; Feng, X. Why Might Urban Tree Canopy Reduce Dementia Risk? A Causal Mediation Analysis of 109,688 Adults with 11 Years of Hospital and Mortality Records. Health Place 2023, 82. [Google Scholar] [CrossRef]
- Cherrie, M.P.C.; Shortt, N.K.; Mitchell, R.J.; Taylor, A.M.; Redmond, P.; Thompson, C.W.; Starr, J.M.; Deary, I.J.; Pearce, J.R. Green Space and Cognitive Ageing: A Retrospective Life Course Analysis in the Lothian Birth Cohort 1936. Soc. Sci. Med. 2018, 196, 56–65. [Google Scholar] [CrossRef] [PubMed]
- Zhu, A.; Wu, C.; Yan, L.L.; Wu, C.-D.; Bai, C.; Shi, X.; Zeng, Y.; Ji, J.S. Association between Residential Greenness and Cognitive Function: Analysis of the Chinese Longitudinal Healthy Longevity Survey. BMJ Nutr. Prev. Health 2019, 2, 72–79. [Google Scholar] [CrossRef] [PubMed]
- Cerin, E.; Barnett, A.; Shaw, J.E.; Martino, E.; Knibbs, L.D.; Tham, R.; Wheeler, A.J.; Anstey, K.J. Urban Neighbourhood Environments, Cardiometabolic Health and Cognitive Function: A National Cross-Sectional Study of Middle-Aged and Older Adults in Australia. Toxics 2022, 10. [Google Scholar] [CrossRef]
- Zhu, A.; Yan, L.; Shu, C.; Zeng, Y.; Ji, J.S. APOE Ε4 Modifies Effect of Residential Greenness on Cognitive Function among Older Adults: A Longitudinal Analysis in China. Sci. Rep. 2020, 10. [Google Scholar] [CrossRef] [PubMed]
- Fangfang, H.; Xiao, H.; Shuai, Z.; Qiong, W.; Jingya, Z.; Guodong, S.; Yan, Z. Living Environment, Built Environment and Cognitive Function among Older Chinese Adults: Results from a Cross-Sectional Study. Journal of Prevention of Alzheimer’s Disease 2022, 9, 126–135. [Google Scholar] [CrossRef]
- World Health Organization. Informe Mundial Sobre El Edadismo; Pan American Health Organization: Washington, 2022. [Google Scholar]
- Kong, C.; Reuter, A.; Buffel, T.; Xu, W. A Scoping Review on Older Adults’ Participation in Policymaking. J. Aging Soc. Policy 2025, 1–31. [Google Scholar] [CrossRef]
- Hansen, K.L.; Golubovic, S.; Eriksen, C.U.; Jørgensen, T.; Toft, U. Effectiveness of Food Environment Policies in Improving Population Diets: A Review of Systematic Reviews. Eur. J. Clin. Nutr. 2022, 76, 637–646. [Google Scholar] [CrossRef]
- Jia, S.S.; Todd, A.R.; Vanderlee, L.; Farrell, P.; Allman-Farinelli, M.; Sacks, G.; Gibson, A.A.; Partridge, S.R. Offline to Online: A Systematic Mapping Review of Evidence to Inform Nutrition-Related Policies Applicable to Online Food Delivery Platforms. BMC Medicine 2024, 22 22, 1–21. [Google Scholar] [CrossRef]
- Hu, R.X.; Luo, M.; Zhang, A.; Li, L.W. Associations of Ageism and Health: A Systematic Review of Quantitative Observational Studies. Res. Aging 2021, 43, 311–322. [Google Scholar] [CrossRef] [PubMed]
- Marquet, M.; Missotten, P.; Adam, S. Ageism and Overestimation of Cognitive Difficulties in Older People: A Review. Geriatr. Psychol. Neuropsychiatr. Vieil. 2016, 14, 177–186. [Google Scholar] [CrossRef] [PubMed]
- Tully-Wilson, C.; Bojack, R.; Millear, P.M.; Stallman, H.M.; Allen, A.; Mason, J. Self-Perceptions of Aging: A Systematic Review of Longitudinal Studies. Psychol. Aging 2021, 36, 773–789. [Google Scholar] [CrossRef]
- Ma, G.; Chen, Z.; Zou, W.; Zhang, X. To Help or Not: Negative Aging Stereotypes Held by Younger Adults Could Promote Helping Behaviors toward Older Adults. Curr. Psychol. 2023, 43, 1041–1051. [Google Scholar] [CrossRef]
- Jing, Y.; Wang, W.; Peng, W.; Wang, M.; Chen, X.; Liu, X.; Wang, P.; Yan, F.; Yang, Y.; Wang, X.; et al. Social Support and Cognitive Function in Chinese Older Adults Who Experienced Depressive Symptoms: Is There an Age Difference? Front. Aging Neurosci. 2023, 15. [Google Scholar] [CrossRef] [PubMed]
- Sims, R.C.; Hosey, M.; Levy, S.A.; Whitfield, K.E.; Katzel, L.I.; Waldstein, S.R. Distinct Functions of Social Support and Cognitive Function among Older Adults. Exp. Aging Res. 2014, 40, 40–59. [Google Scholar] [CrossRef]
- Mendoza-Núñez, V.M.; Mendoza-Soto, A.B. Is Aging a Disease? A Critical Review Within the Framework of Ageism. Cureus 2024, 16. [Google Scholar] [CrossRef]
- Levy, B.R.; Slade, M.D.; Chang, E.S.; Kannoth, S.; Wang, S.Y. Ageism Amplifies Cost and Prevalence of Health Conditions. Gerontologist 2020, 60, 174–181. [Google Scholar] [CrossRef]
- Ng, R.; Chow, T.Y.J.; Yang, W. The Impact of Aging Policy on Societal Age Stereotypes and Ageism. Gerontologist 2022, 62, 598–606. [Google Scholar] [CrossRef]
- Wang, F.; Zhu, J.; Xiao, D. The Impact of Community-Organised/Sponsored Activities on Health Outcomes in Older Adults: A Systematic Review. Gerontologist 2025. [Google Scholar] [CrossRef]
- Chandrashekhar, A.; Thakur, H.P. Efficacy of Government-Sponsored Community Health Programs for Older Adults: A Systematic Review of Published Evaluation Studies. Public Health Rev. 2022, 43. [Google Scholar] [CrossRef]
- You, J.; Ganann, R.; Wilson, M.; Carusone, S.C.; MacNeil, M.; Whitmore, C.; Dafel, A.; Dhamanaskar, R.; Ling, E.; Dingman, L.; et al. Public Engagement in Health Policy-Making for Older Adults: A Systematic Search and Scoping Review. Health Expect. 2024, 27. [Google Scholar] [CrossRef]
- Falanga, R.; Cebulla, A.; Principi, A.; Socci, M. The Participation of Senior Citizens in Policy-Making: Patterning Initiatives in Europe. International Journal of Environmental Research and Public Health 2021, 18, 34. [Google Scholar] [CrossRef]
- Townsend, B.G.; Chen, J.T.H.; Wuthrich, V.M. Barriers and Facilitators to Social Participation in Older Adults: A Systematic Literature Review. Clin. Gerontol. 2021, 44, 359–380. [Google Scholar] [CrossRef] [PubMed]
- Gelius, P.; Messing, S.; Goodwin, L.; Schow, D.; Abu-Omar, K. What Are Effective Policies for Promoting Physical Activity? A Systematic Review of Reviews. Prev. Med. Rep. 2020, 18. [Google Scholar] [CrossRef]
- Kohler, S.; Dippon, L.; Helsper, N.; Rütten, A.; Abu-Omar, K.; Birkholz, L.; Pfeifer, K.; Weber, P.; Semrau, J. Population-Based Physical Activity Promotion with a Focus on Health Equity: A Review of Reviews. Int. J. Equity Health 2023, 22. [Google Scholar] [CrossRef]
- Wang, L.; Zhong, B.; Vardoulakis, S.; Zhang, F.; Pilot, E.; Li, Y.; Yang, L.; Wang, W.; Krafft, T. Air Quality Strategies on Public Health and Health Equity in Europe-A Systematic Review. Int. J. Environ. Res. Public Health 2016, 13. [Google Scholar] [CrossRef]
- Burns, J.; Boogaard, H.; Polus, S.; Pfadenhauer, L.M.; Rohwer, A.C.; van Erp, A.M.; Turley, R.; Rehfuess, E.A. Interventions to Reduce Ambient Air Pollution and Their Effects on Health: An Abridged Cochrane Systematic Review. Environ. Int. 2020, 135. [Google Scholar] [CrossRef]
- Jonidi Jafari, A.; Charkhloo, E.; Pasalari, H. Urban Air Pollution Control Policies and Strategies: A Systematic Review. J. Environ. Health Sci. Eng. 2021, 19, 1911. [Google Scholar] [CrossRef] [PubMed]
- Yao, Y.; Lv, X.; Qiu, C.; Li, J.; Wu, X.; Zhang, H.; Yue, D.; Liu, K.; Eshak, E.S.; Lorenz, T.; et al. The Effect of China’s Clean Air Act on Cognitive Function in Older Adults: A Population-Based, Quasi-Experimental Study. Lancet Healthy Longev. 2022, 3, e98. [Google Scholar] [CrossRef] [PubMed]
- Sharifian, N.; Spivey, B.N.; Zaheed, A.B.; Zahodne, L.B. Psychological Distress Links Perceived Neighborhood Characteristics to Longitudinal Trajectories of Cognitive Health in Older Adulthood. Soc. Sci. Med. 2020, 258. [Google Scholar] [CrossRef] [PubMed]
| Environment | Elements that improve cognition | Elements that damage cognition |
|---|---|---|
|
Micro-level (family) |
|
|
|
Meso-level (community) |
land use patterns | |
|
|
|
| Transport | ||
|
|
|
| Environmental design | ||
|
|
|
| Open spaces | ||
|
||
|
Macro-level (society) |
|
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




