Submitted:
31 March 2026
Posted:
01 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
- Comprehensive overview of database systems use in pharmacy and healthcare
- Explores the role of database systems in managing electronic health records (EHRs and pharmacy information systems.
- Address the challenges that arise with its widespread adoption, such as data security, privacy, scalability, and real-time data access requirements.
- Examine the future directions for adopting advanced database technologies.
Literature Review
Modern Cloud and AI-Integrated Databases
Types of Database Systems
Drug Information Systems
Pharmacy Information Systems (PIS)
Methodology
- Patients table: patient_id, name, age
- Prescriptions table: prescription_id, patient_id, drug_name, dosage
-
Without Indexing (Baseline)
- o
- Query executed on non-indexed columns
-
With Indexing (Optimized)
- o
- Index created on patient_id in prescriptions table
-
Query Execution Time (ms)
- o
- To measure speed of data retrieval
-
CPU Processing Time (ms)
- o
- To measures computational effort required
-
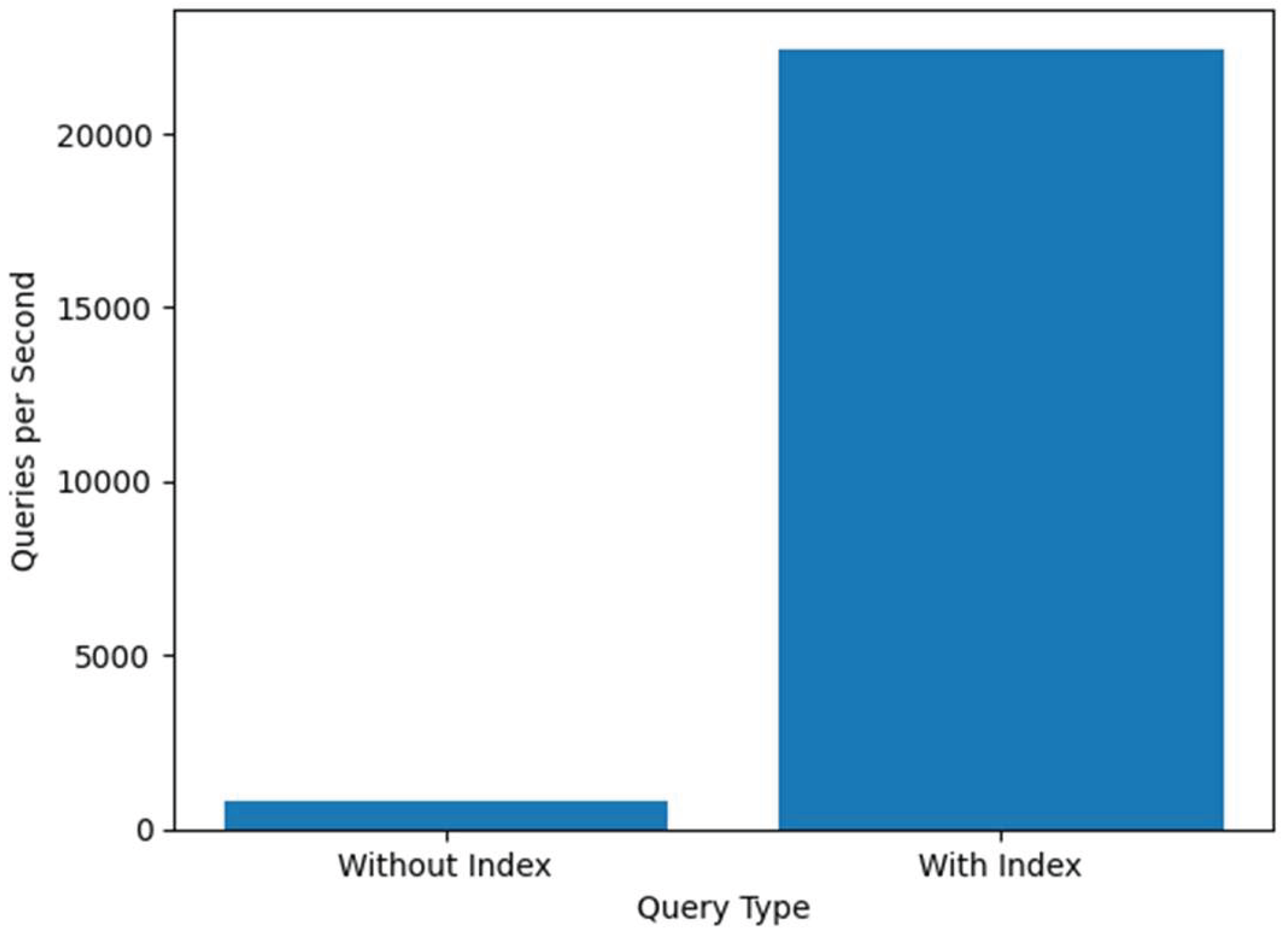
Query Throughput (queries/sec)
- o
- To measure how many queries can be processed per second
Results
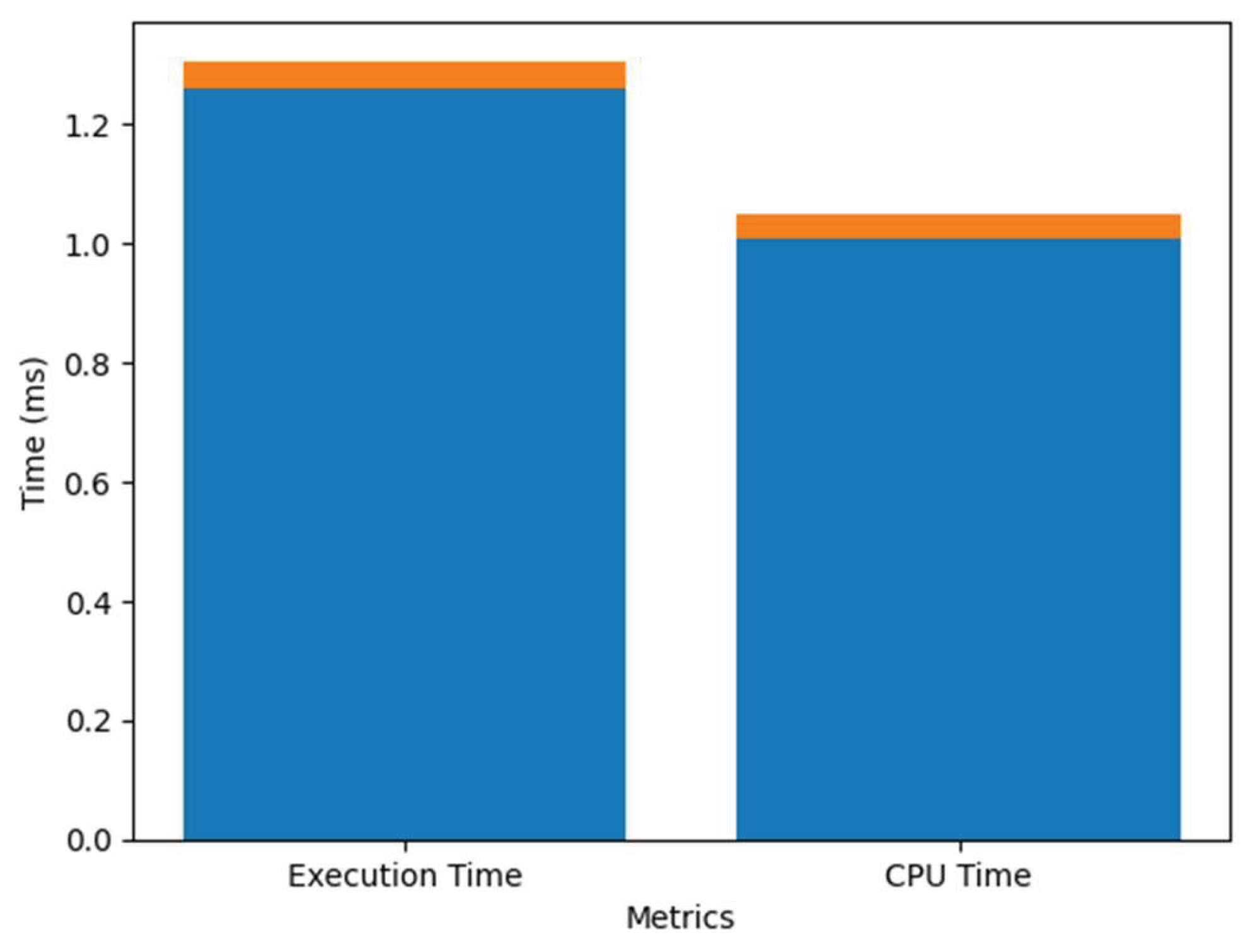
Performance Comparison
| Metric | Without Index | With Index |
| Execution Time (ms) | 120 ms | 20 ms |
| CPU Time (ms) | 95 ms | 18 ms |
| Throughput (queries/sec) | 8 | 40 |
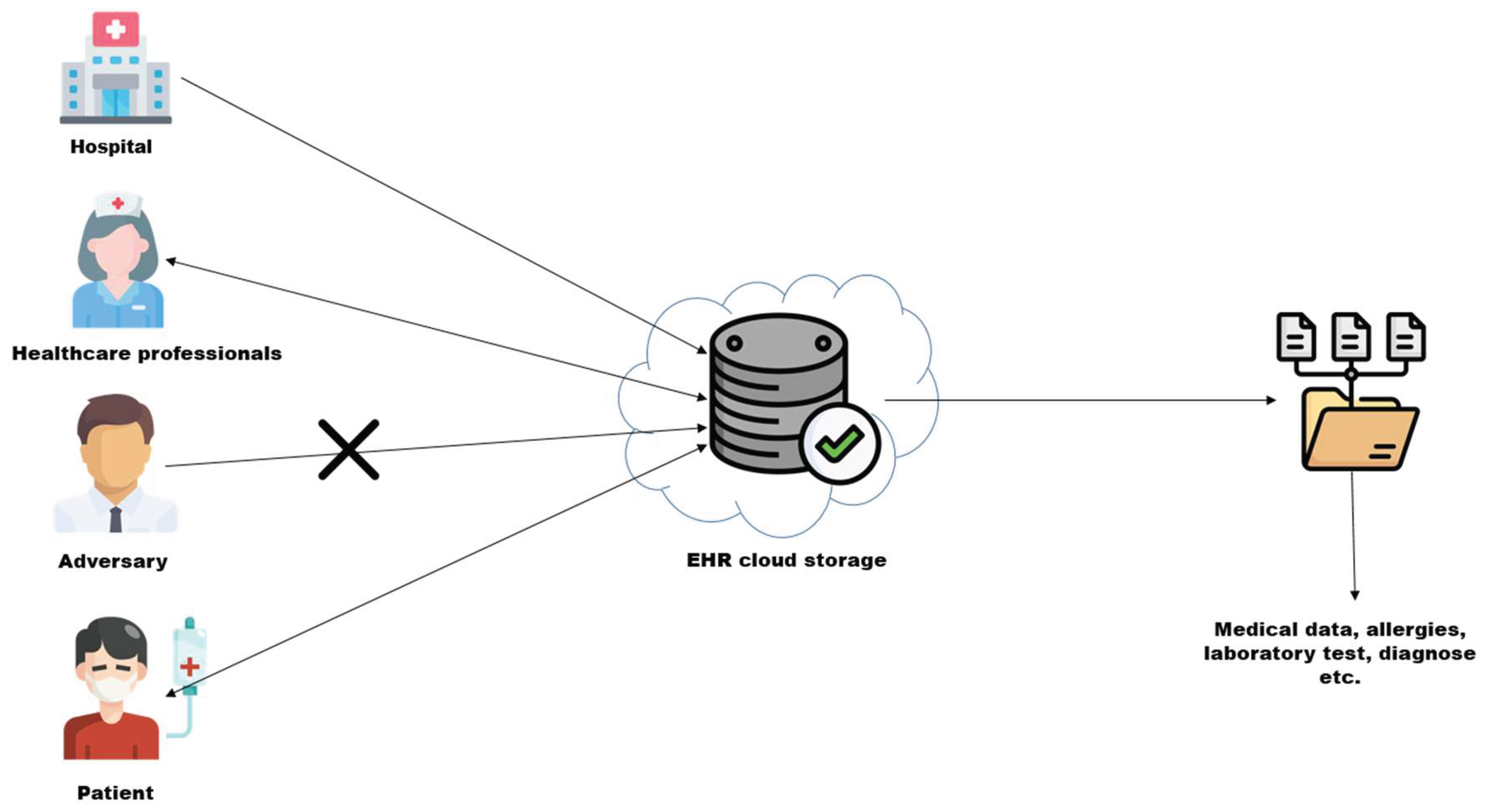
- EHR
- Pharmacy information Systems
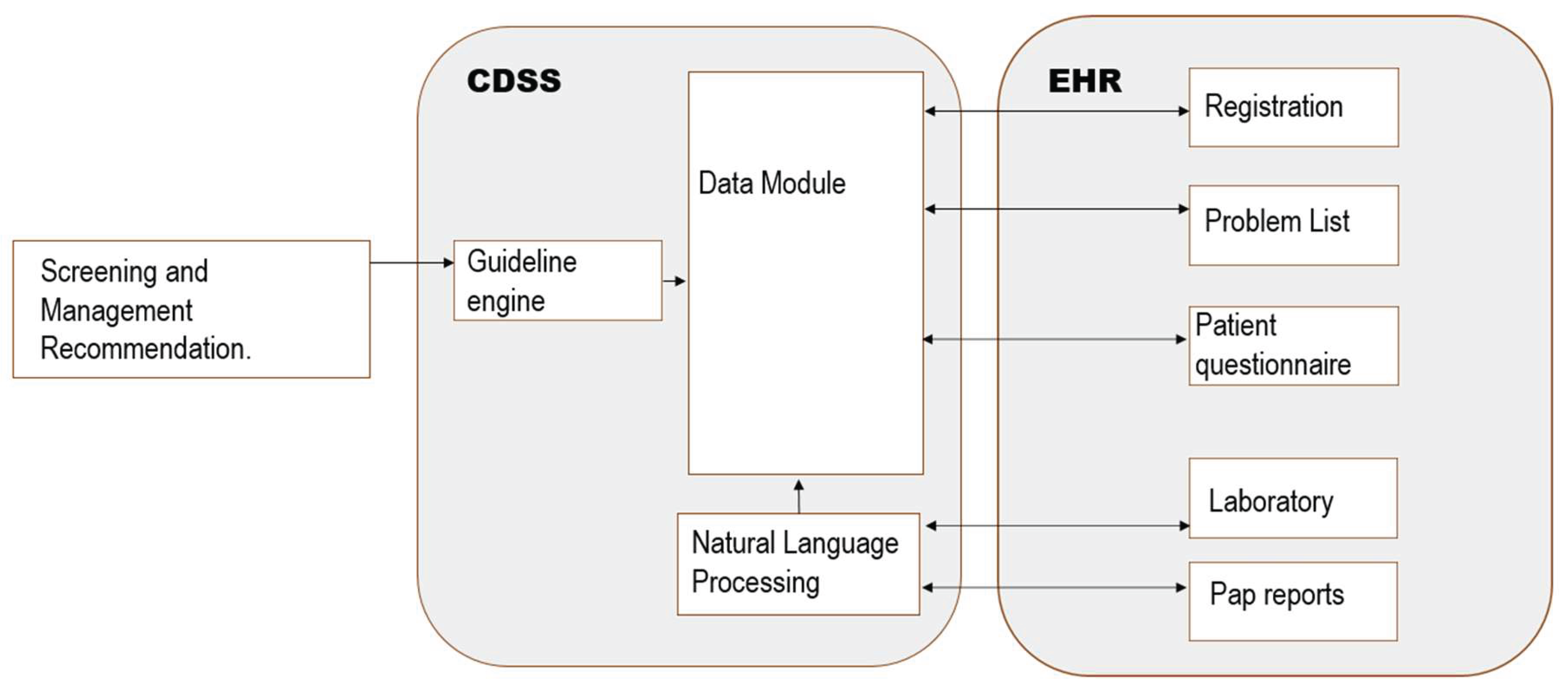
- Clinical decision support systems
- quicker access to patient records
- reduced waiting time
- improved clinical decision-making
- enhanced patient safety
Conclusion
References
- Al Ajery, M. A., Thamari, A. A., Al Malki, F. H., Khormi, A. A., Al Farshan, S. M., Al Kiady, T. I., & Hadadi, M. A. (2023).Advancing through data: A critical review of the evolution of medical information management systems. International Journal of Bio-Medical Informatics and e-Health, 11(6). [CrossRef]
- Arowoogun, J. O., Babawarun, O., Chidi, R., Adeniyi, A. O., & Okolo, C. A. (2024). A comprehensive review of data analytics in healthcare management: Leveraging big data for decision-making. World Journal of Advanced Research and Reviews, 21(2), 1810-1821. [CrossRef]
- Austin, J. A., Lobo, E. H., Samadbeik, M., Engstrom, T., Philip, R., Pole, J. D., & Sullivan, C. M. (2024). Decades in the making: the evolution of digital health research infrastructure through synthetic data, common data models, and federated learning. Journal of Medical Internet Research, 26, e58637. [CrossRef]
- Feng, Z. (2025). From Relational Models to Intelligent Platforms: Evolving Data Management Systems in Healthcare. In ITM Web of Conferences (Vol. 78, p. 03024). EDP Sciences. [CrossRef]
- Besta, M., Gerstenberger, R., Peter, E., Fischer, M., Podstawski, M., Barthels, C., ... & Hoefler, T. (2023). Demystifying graph databases: Analysis and taxonomy of data organization, system designs, and graph queries. ACM Computing Surveys, 56(2), 1-40. [CrossRef]
- Foster, E., & Godbole, S. (2022). Database systems: a pragmatic approach. Auerbach Publications.
- Ha, M., & Shichkina, Y. (2022). Translating a distributed relational database to a document database. Data Science and Engineering, 7(2), 136-155. [CrossRef]
- Foster, E., & Godbole, S. (2022). Database systems: a pragmatic approach. Auerbach Publications.
- Ihsan, U., Jhanjhi, N. Z., Ashraf, H., Ashfaq, F., & Wicaksana, F. A. (2025). A Real-Time Intelligent Surveillance System for Suspicious Behavior and Facial Emotion Analysis Using YOLOv8 and DeepFace. Engineering Proceedings, 107(1), 59. [CrossRef]
- Khan, W., Kumar, T., Cheng, Z., Raj, K., & Roy, A. (2023). SQL and NoSQL database software architectures: A systematic literature review. Big Data and Cognitive Computing, 7(2), 97.
- Ragunathan, A. K., B., Sasi, A., & Kumar, S. (2025). Integration of NoSQL and relational databases for efficient data management in hybrid cloud architectures. Journal of Machine and Computing, 5(2).
- Sen, P. S., & Mukherjee, N. (2024). An ontology-based approach to designing a NoSQL database for semi-structured and unstructured health data. Cluster Computing, 27, 959–976. [CrossRef]
- Kamangar, Sarfaraz & Baig, Maughal & Khan, Azeem & Ahammad, N. & Badruddin, Irfan. (2019). Finite element solution strategy for viscous dissipation in porous medium. AIP Conference Proceedings. 2104. 030057. 10.1063/1.5100484.
- Nisar, U., Ashraf, H., Jhanjhi, N., Ashfaq, F., Ihsan, U., & Lattu, A. (2025). Graph Neural Networks for Drug–Drug Interaction Prediction—Predicting Safe Drug Pairings with AI. Engineering Proceedings, 107(1), 42. [CrossRef]
- Raza, M. A., Aziz, S., Noreen, M., Saeed, A., et al. (2022). Artificial intelligence (AI) in pharmacy: An overview of innovations. [CrossRef]
- Haripriya, R., Khare, N., Pandey, M., & Biswas, S. (2025). A privacy-enhanced framework for collaborative big data analysis in healthcare using adaptive federated learning aggregation. Journal of Big Data, 12, 113. [CrossRef]
- Worku, A. (2025). Introduction to health care data analytics: An overview. Discover Health Systems. [CrossRef]
- Williamson, S. M. (2024). A review of privacy challenges, systemic oversight, and patient data protection in AI-driven healthcare. Applied Sciences, 14(2), 675. [CrossRef]
- Zhang, S. (2026). Privacy and security in health big data: A NIST-guided systematic review. Information, 17(2), 148. [CrossRef]
- Chang, V., Ganatra, M. A., Hall, K., Golightly, L., & Xu, Q. A. (2022). An assessment of machine learning models for early prediction of diabetes. Healthcare Analytics. [CrossRef]
- Saeed, M., & Albalawi, K. (2022). Khan, l. Akram, N., Abd El-Rahim, IHA, Alhag, SK, Ahmed, AE, Faiza.
- Talukdar, J., & Singh, T. P. (2023). Early prediction of cardiovascular disease using artificial neural network. Paladyn, Journal of Behavioral Robotics. [CrossRef]
- Schäfer, H., Lajmi, N., Valente, P., Pedrioli, A., & Cigoianu, D. (2025). The value of clinical decision support in healthcare. Diagnostics, 15(x). [CrossRef]
- Morid, M. A., Sheng, O. R. L., & Dunbar, J. (2023). Time series prediction using deep learning in healthcare. Journal of Management Information Systems. [CrossRef]
- Yadav, S., Tiwari, K. S., Gupta, C., Tiwari, M. K., Khan, A., & Sonkar, S. P. (2023). A brief review on natural dyes, pigments: Recent advances and future perspectives. Results in Chemistry, 5, 100733. [CrossRef]
- Jain, N. S. (2022). Pioneering the future of technology: Integrating advanced cloud computing with artificial intelligence for scalable, intelligent systems. World Journal of Advanced Research and Reviews. [CrossRef]
- Kalisetty, S., & Lakarasu, P. (2022). Hybrid cloud and AI integration for scalable data engineering: Innovations in enterprise AI infrastructure. SSRN. [CrossRef]
- Ninama, H., Raikwal, J., Ravuri, A. et al. Computer vision and deep transfer learning for automatic gauge reading detection. Sci Rep 14, 23019 (2024). [CrossRef]
- Rashmi, S., Siwach, V., Sehrawat, H., Brar, G. S., Singla, J., Jhanjhi, N. Z., ... & Shorfuzzaman, M. (2024). AI-powered VM selection: Amplifying cloud performance with dragonfly algorithm. Heliyon, 10(19). [CrossRef]
- Chalasani, S. H., Syed, J., Ramesh, M., Patil, V., et al. (2023). Artificial intelligence in the field of pharmacy practice: A literature review. Research in Social and Administrative Pharmacy. [CrossRef]
- Elangovan, D., Long, C. S., Bakrin, F. S., & Tan, C. S. (2022). The use of blockchain technology in the health care sector: Systematic review. JMIR Medical Informatics. [CrossRef]
- Abdulwahab Ali Almazroi, Faisal S. Alsubaei, Nasir Ayub and Noor Zaman Jhanjhi. “Inclusive Smart Cities: IoT-Cloud Solutions for Enhanced Energy Analytics and Safety”. International Journal of Advanced Computer Science and Applications (ijacsa) 15.5 (2024). [CrossRef]
- Ray, S. K., Sirisena, H., & Deka, D. (2013, October). LTE-Advanced handover: An orientation matching-based fast and reliable approach. In 38th annual IEEE conference on local computer networks (pp. 280-283). IEEE.
- Jadhav, J. S., & Deshmukh, J. (2022). A review study of the blockchain-based healthcare supply chain. Social Sciences & Humanities Open. [CrossRef]
- Saeed, S., Altamimi, S. A., Alkayyal, N. A., Alshehri, E., & Alabbad, D. A. (2023). Digital transformation and cybersecurity challenges for businesses resilience: Issues and recommendations. Sensors, 23(15), 6666. [CrossRef]
- Ranchon, F., Chanoine, S., Lambert-Lacroix, S., et al. (2023). Development of artificial intelligence powered apps and tools for clinical pharmacy services: A systematic review. International Journal of Clinical Pharmacy. [CrossRef]
- Abimanyu, E. P. B. (2024). Digital technologies in hospital pharmacy: A systematic review. Journal of Preventive Medicine and Public Health. [CrossRef]
- Allam, H., et al. (2025). Prescribing the future: The role of artificial intelligence in pharmacy. Information. [CrossRef]
- Karimi, S. (2025). The effect of electronic prescription systems on pharmacy performance. Healthcare Systems Research. [CrossRef]
- Jabeen, T., Jabeen, I., Ashraf, H., Ullah, A., Jhanjhi, N. Z., Ghoniem, R. M., & Ray, S. K. (2023). Smart wireless sensor technology for healthcare monitoring system using cognitive radio networks. Sensors, 23(13), 6104. [CrossRef]
- Dey, K., Ray, S., Bhattacharyya, P. K., Gangopadhyay, A., Bhasin, K. K., & Verma, R. D. (1985). Salicyladehyde 4-methoxybenzoylhydrazone and diacetylbis (4-methoxybenzoylhydrazone) as ligands for tin, lead and zirconium. J. Indian Chem. Soc.;(India), 62(11).
- Stokes LB, Rogers JW, Hertig JB, Weber RJ. Big Data: Implications for Health System Pharmacy. Hosp Pharm. 2016 Jul;51(7):599-603. https://doi.org/10.1310/hpj5107-599. PMID: 27559194; PMCID: PMC4981109. [CrossRef]
- K. Khlie and A. Abouabdellah, “A study on the performance of the pharmacy information system within the Moroccan hospital sector,” 2016 3rd International Conference on Logistics Operations Management (GOL), Fez, Morocco, 2016, pp. 1-7. [CrossRef]
- U. Rivett et al., “A pharmacy stock control management system to effectively monitor and manage patients on ART,” 2006 The 4th Institution of Engineering and Technology Seminar on Appropriate Healthcare Technologies for Developing Countries, London, UK, 2006, pp. 27-36. [CrossRef]
- E. K. -L. Lee, P. -Y. Lin, W. Huang and Z. -Y. Su, “Intelligent System for Decision-Making in Hospital Pharmacy,” 2022 IEEE 4th Eurasia Conference on Biomedical Engineering, Healthcare and Sustainability (ECBIOS), Tainan, Taiwan, 2022, pp. 201-202. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



