Submitted:
31 March 2026
Posted:
01 April 2026
You are already at the latest version
Abstract
Keywords:
Introduction
- Comprehensive review of digital technologies such as mobile health(mhealth) applications, electronic health records and use of AI in medication management.
- This study explores how digital health tools facilitate medication prescribing, monitoring, and adherence.
- The research highlights the key challenges regarding digital health technologies such as usability issues, privacy concerns, digital literacy barriers, and system integration problems.
- We examine the future potential of digital health technologies.
Literature Review
Methodology
- Age
- Number of prescribed medicines
- System Usage (0=No usage, 1=Mobile App)
- Medication Adherence Rate (%)
- 1)
- Group A:These were patients which were not using any app → Control Group
- 2)
- Group B: These were patients which were using app → Normal Group
- 3)
- Group C: These were patients which were using smart AI based Reminder System → Special Group
Results
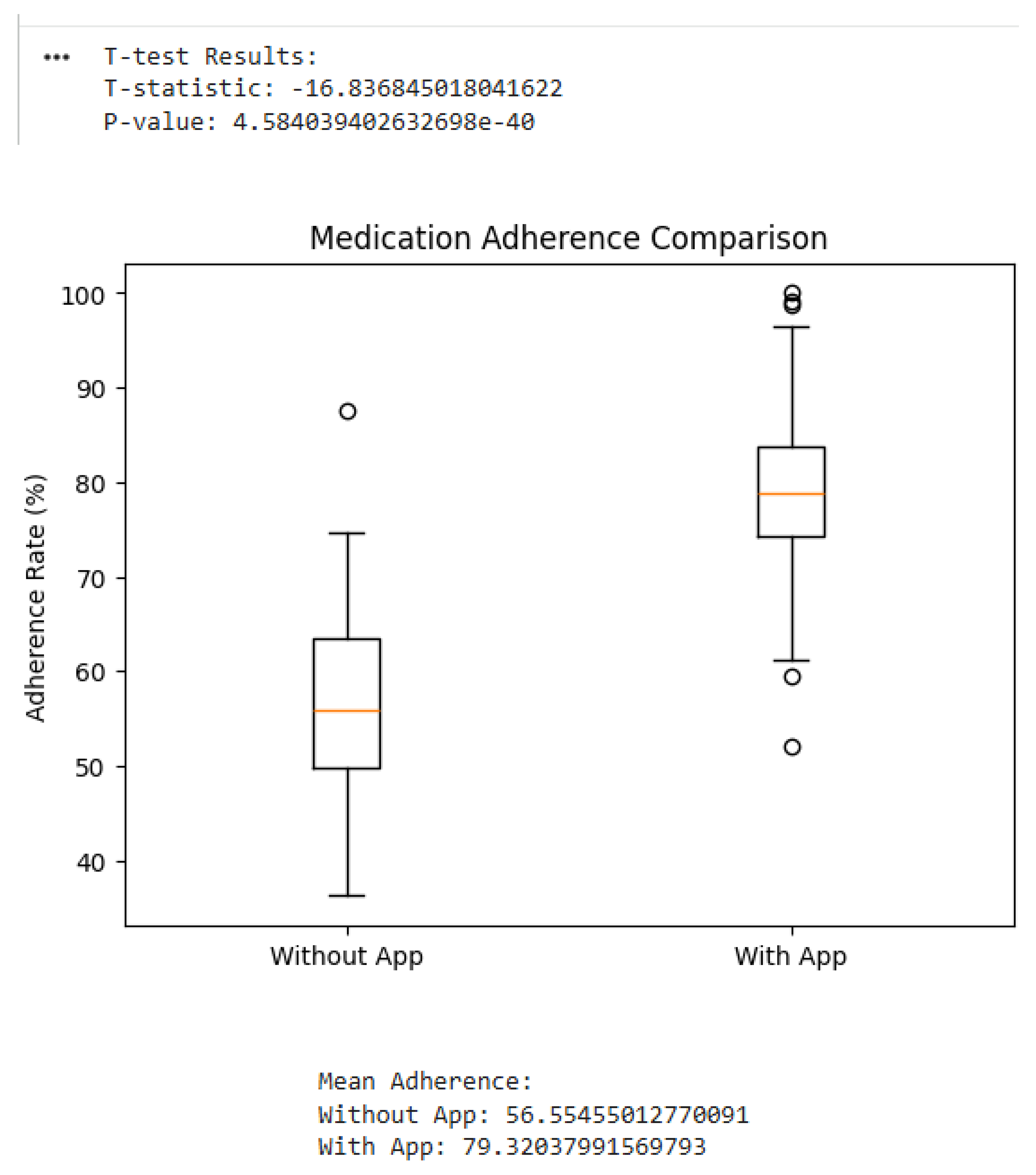
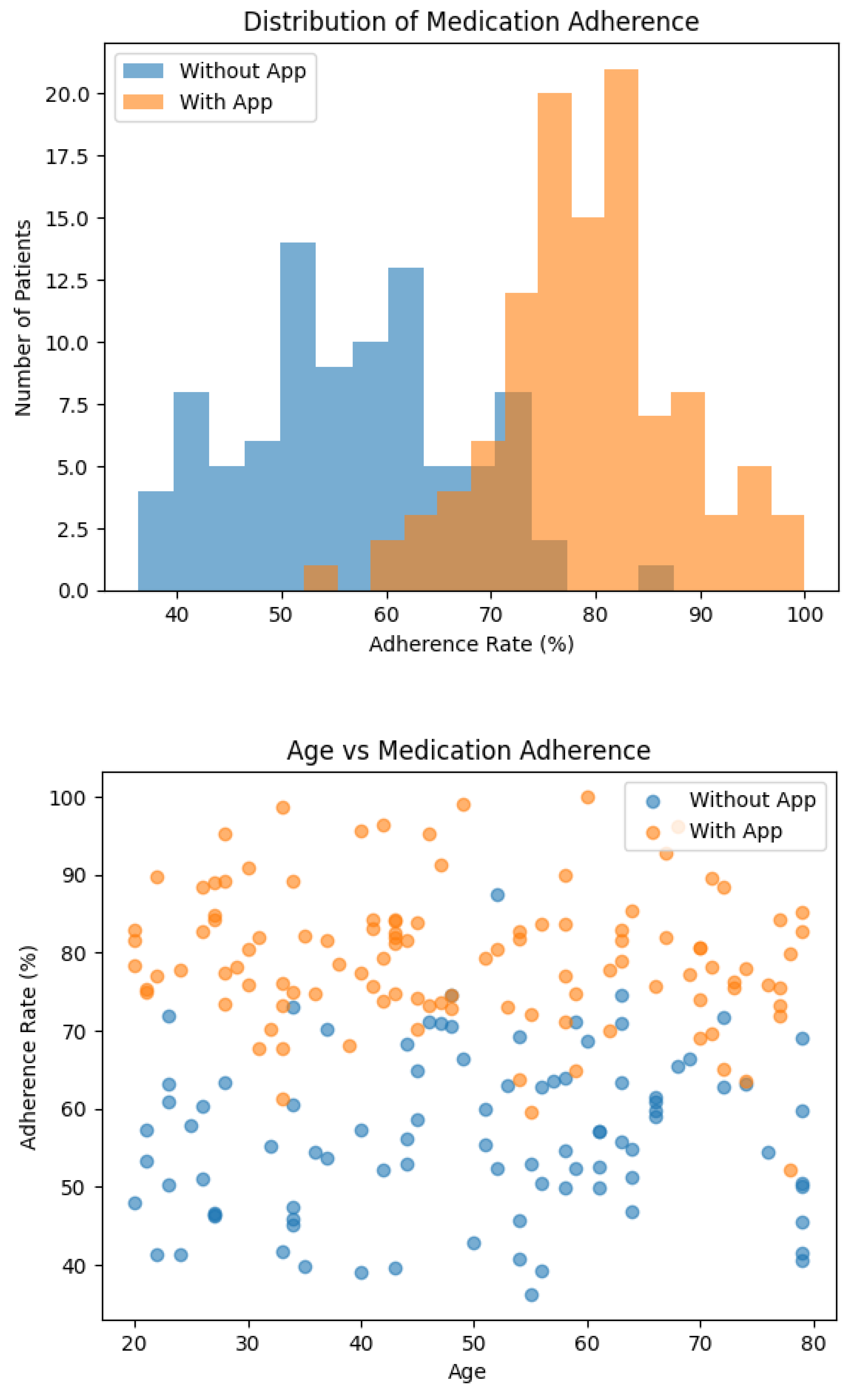
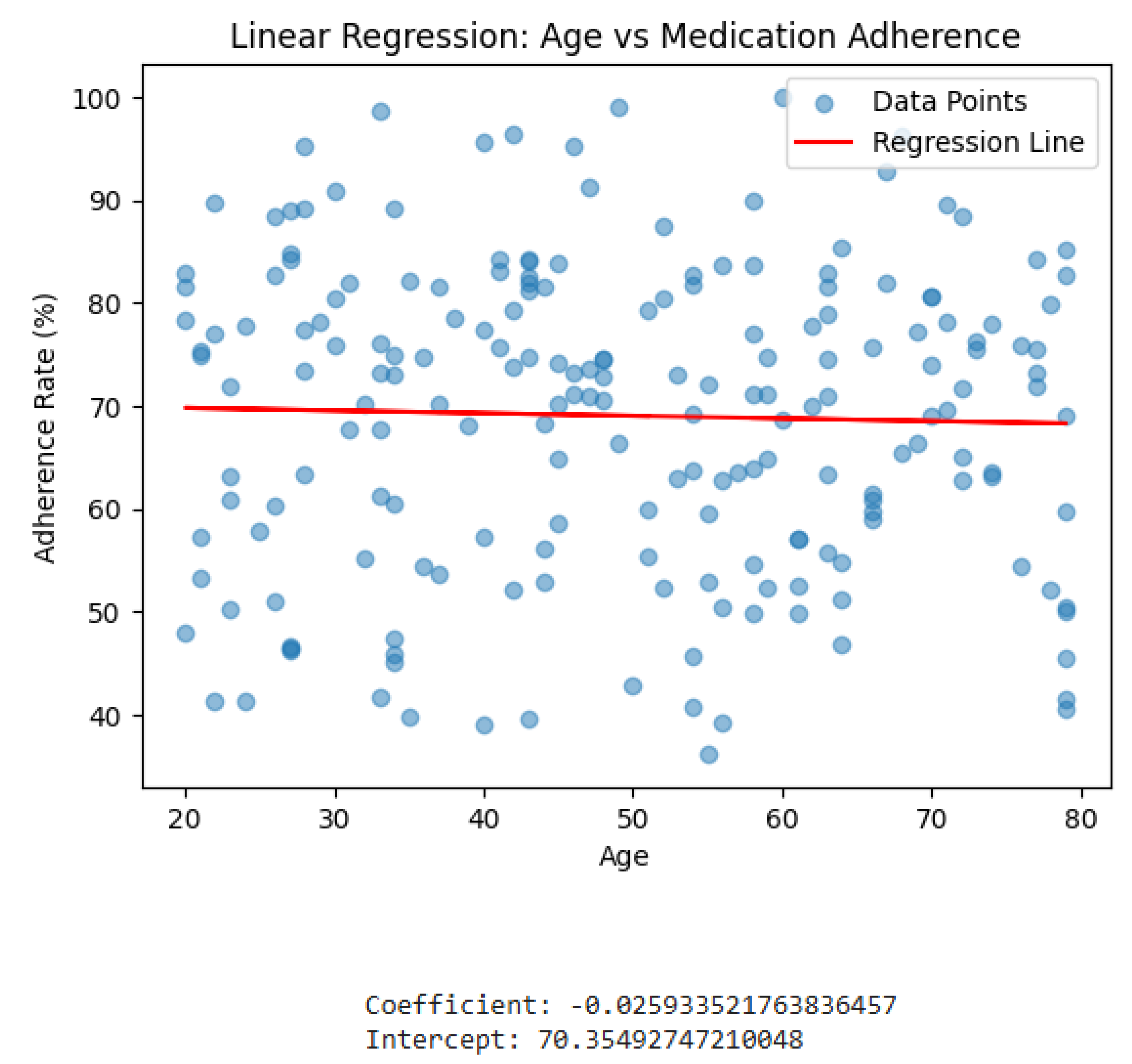
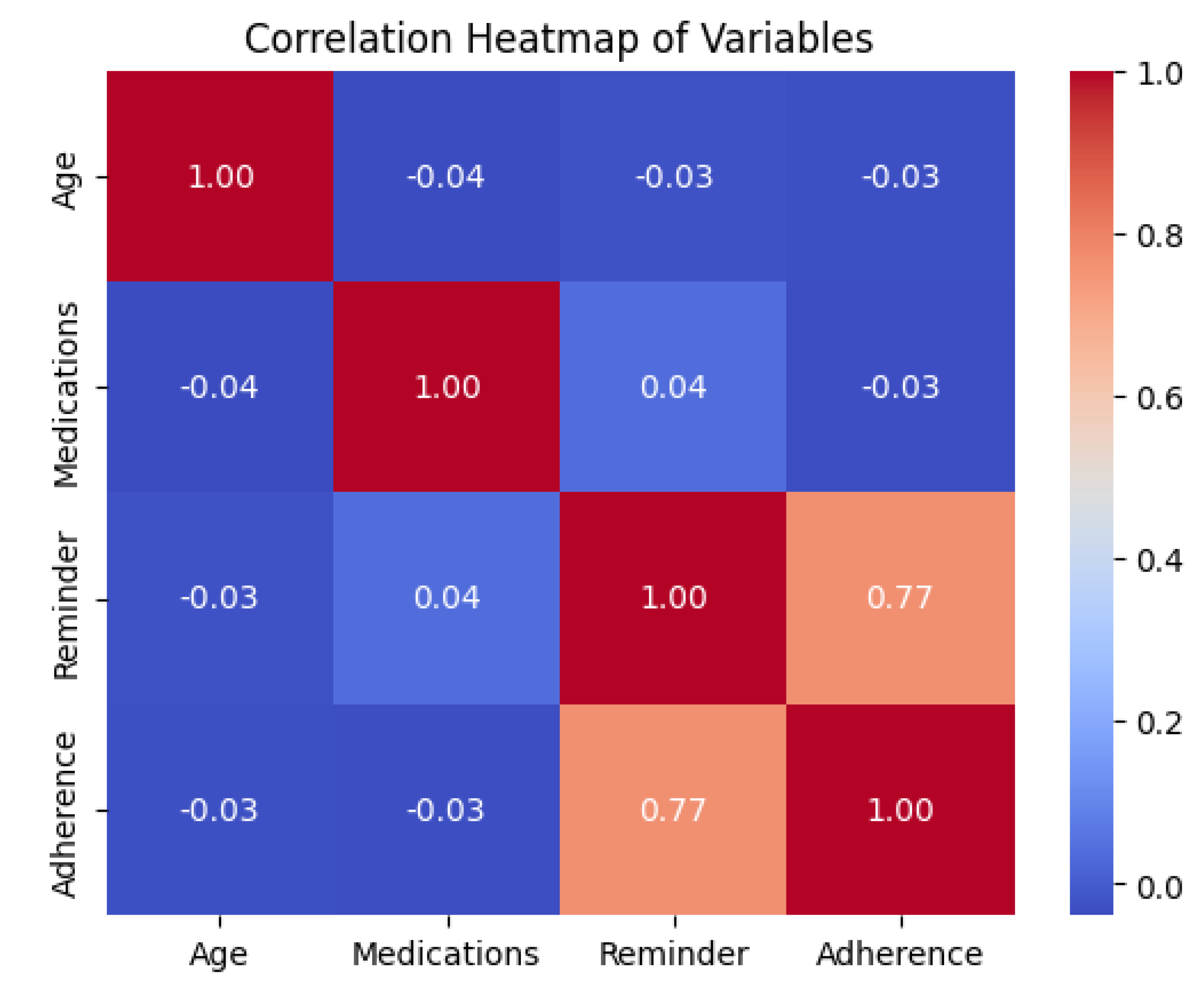
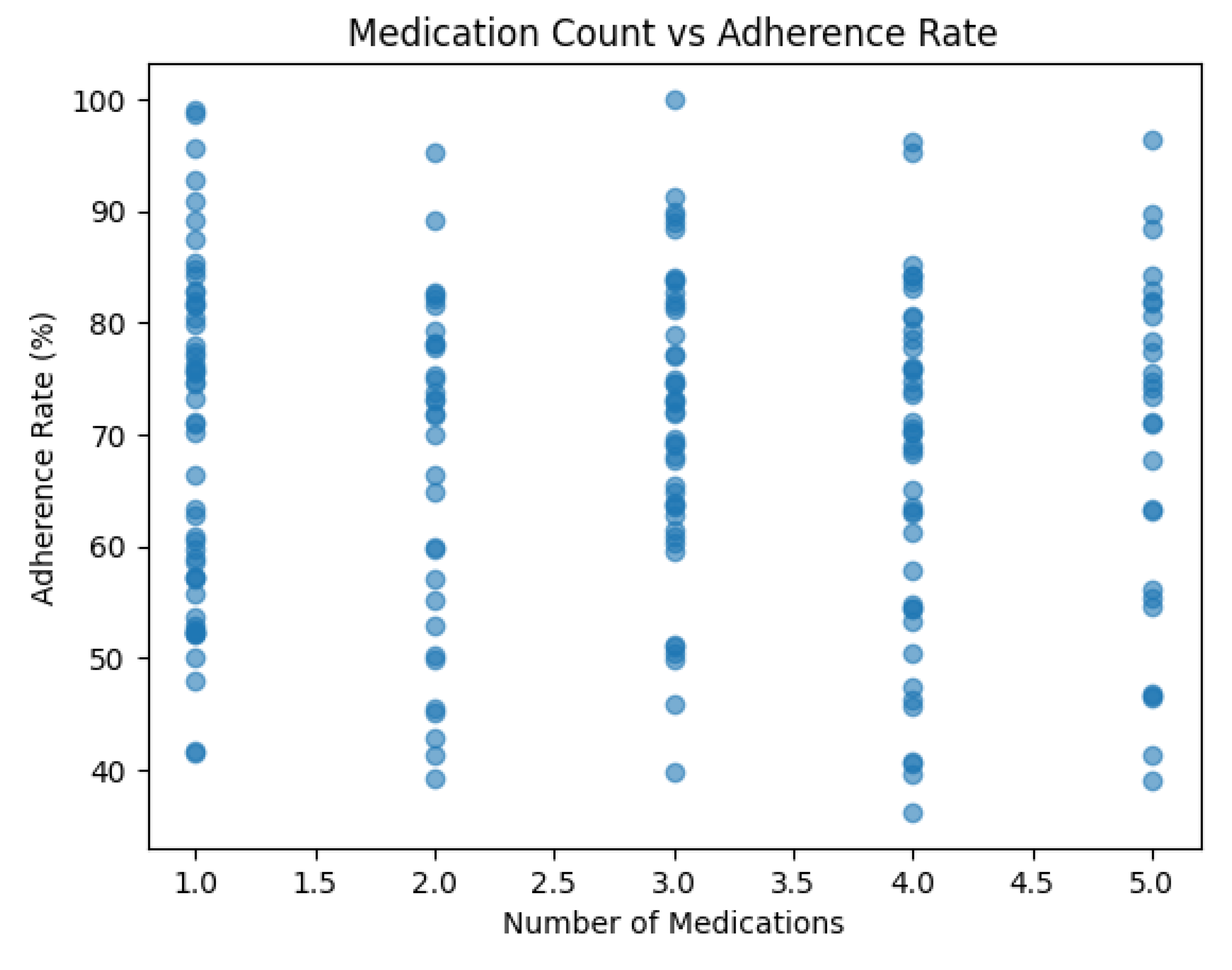
- The heatmap below is the correlation heatmap which visually represent the correlation matrix. The most notable correlation is between Reminder and Adherence (corr = 0.77). This strong positive correlation indicates that the presence of a reminder (app usage) is highly associated with higher medication adherence, reinforcing the findings from the t-test.
- Age and Medications show very weak (close to zero) correlations with Adherence, and also with Reminder, suggesting these factors have minimal linear relationship with adherence in this dataset.
- Group 2: 73 patients
- Group 0: 66 patients
- Group 1: 61 patients
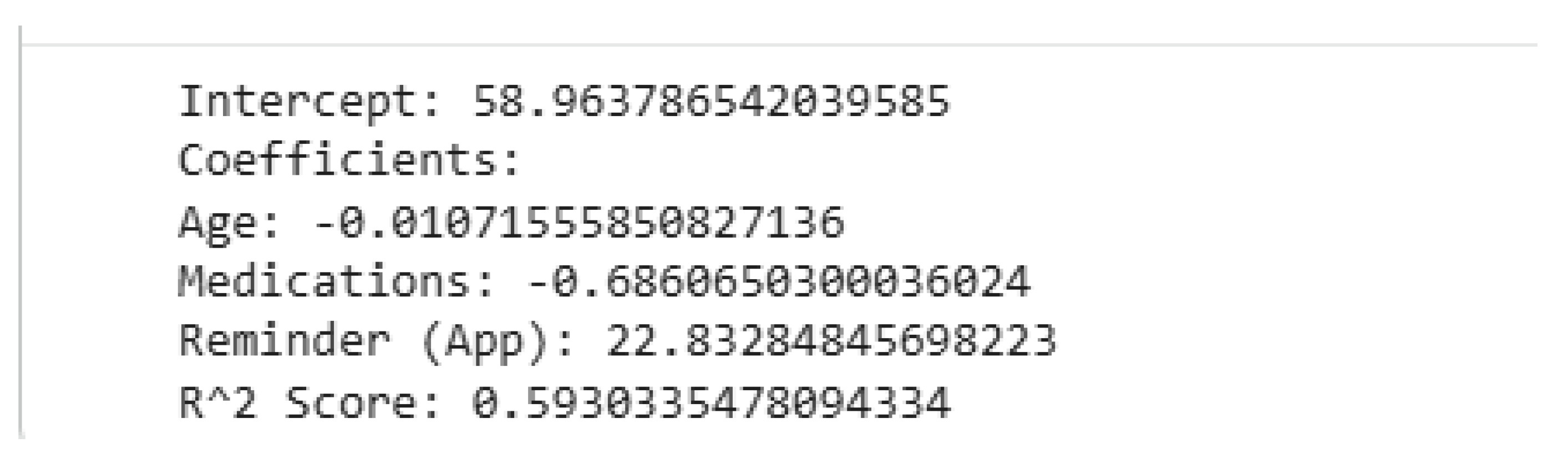
- Age: A very small negative impact, similar to the simple linear regression.
- Medications: For each additional medication, adherence is predicted to decrease by about 0.69 percentage points, holding other variables constant.
- Reminder (App): This is the most impactful factor. Using the app (Reminder = 1) is associated with an increase of about 22.83 percentage points in adherence compared to not using it (Reminder = 0), holding age and medications constant.
- Score: An of 0.593 (or 59.3%) means that approximately 59.3% of the variance in medication adherence can be explained by this model using Age, Medications, and Reminder.


Conclusion
References
- World Health Organization. WHO guideline: recommendations on digital interventions for health system strengthening; WHO: Geneva, 2019. [Google Scholar]
- Iyengar, K.; Upadhyaya, G. K.; Vaishya, R.; Jain, V. COVID-19 and applications of digital health technologies in healthcare. Diabetes & Metabolic Syndrome: Clinical Research & Reviews 2020, 14(4), 733–737. [Google Scholar]
- Torous, J.; Bucci, S.; Bell, I. H.; et al. The growing field of digital psychiatry: current evidence and the future of apps, social media, chatbots, and virtual reality. World Psychiatry 2021, 20(3), 318–335. [Google Scholar] [CrossRef]
- Jimmy, B.; Jose, J. Patient medication adherence: measures in daily practice. Oman Medical Journal 2020, 35(1), e145. [Google Scholar] [CrossRef] [PubMed]
- Keesara, S.; Jonas, A.; Schulman, K. Covid-19 and health care’s digital revolution. New England Journal of Medicine 2020, 382(23), e82. [Google Scholar] [CrossRef] [PubMed]
- Kwan, J. L.; Lo, L.; Sampson, M.; Shojania, K. G. Medication reconciliation during transitions of care as a patient safety strategy. Annals of Internal Medicine 2020, 172(11), 812–821. [Google Scholar] [CrossRef]
- Tariq, R. A.; Vashisht, R.; Sinha, A.; Scherbak, Y. Medication errors; StatPearls, 2021. [Google Scholar]
- Torous, J.; Bucci, S.; Bell, I. H.; et al. The growing field of digital health technologies and their applications in healthcare. World Psychiatry 2021, 20(3), 318–335. [Google Scholar] [CrossRef]
- World Health Organization. WHO guideline: Recommendations on digital interventions for health system strengthening; World Health Organization: Geneva, 2019. [Google Scholar]
- Barbieri, C.; Neri, L.; Stuard, S.; Mari, F. From electronic health records to clinical management systems: How the digital transformation can support healthcare services. Clinical Kidney Journal. 2023. [Google Scholar] [CrossRef]
- Kamangar, S.; Baig, M. A. A.; Azeem; Ahamad, N. A.; Badruddin, I. A. Finite element solution strategy for viscous dissipation in porous medium. In AIP Conference Proceedings; AIP Publishing LLC, 2019; Vol. 2104, p. 030057. [Google Scholar]
- Butcher, C. J. T.; Hussain, W. Digital healthcare: The future. Future Healthcare Journal. 2022. [Google Scholar] [CrossRef]
- Gouda, W.; Almurafeh, M.; Humayun, M.; Jhanjhi, N. Z. Detection of COVID-19 based on chest X-rays using deep learning. Healthcare 2022, 10(2), 343. [Google Scholar] [CrossRef] [PubMed]
- Saeed, M., & Albalawi, K. (2022). Khan, l. Akram, N., Abd El-Rahim, IHA, Alhag, SK, Ahmed, AE, Faiza.
- Bora, P.S.; Sharma, S.; Batra, I.; Malik, A.; Ashfaq, F. Identification and Classification of Rare Medicinal Plants. In Proceedings of the 2024 International Conference on Emerging Trends in Networks and Computer Communications (ETNCC), Windhoek, Namibia, 2024; pp. 1–6. [Google Scholar] [CrossRef]
- Jakob, R.; Harperink, S.; Rudolf, A. M.; Fleisch, E. Factors influencing adherence to mHealth apps for prevention or management of noncommunicable diseases: Systematic review. Journal of Medical Internet Research 2022. [Google Scholar] [CrossRef]
- Jin, X.; Yuan, Z.; Zhou, Z. Understanding the antecedents and effects of mHealth app use in pandemics. International Journal of Environmental Research and Public Health 2023. [Google Scholar] [CrossRef]
- Jabeen, T.; Jabeen, I.; Ashraf, H.; Ullah, A.; Jhanjhi, N. Z.; Ghoniem, R. M.; Ray, S. K. Smart wireless sensor technology for healthcare monitoring system using cognitive radio networks. Sensors 2023, 23(13), 6104. [Google Scholar] [CrossRef]
- Aziz, M.; Erbad, A.; Belhaouari, S. B.; Almourad, M. B. Who uses mHealth apps? Identifying user archetypes of mHealth apps. Digital Health 2023. [Google Scholar] [CrossRef]
- De Keyser, H. H.; Anderson, W. C.; Stempel, D. A. Digital health for asthma management: Electronic medication monitoring for adherence as a case example. Journal of Allergy and Clinical Immunology 2025. [Google Scholar] [CrossRef] [PubMed]
- Divya, R.; Shree, S. S.; Sakthiganesh, V. Digital pills: Enhancing patient outcomes through innovative medication management. Computers in Biology and Medicine 2025. [Google Scholar] [CrossRef]
- Feilong, Q.; Khan, N. A.; Jhanjhi, N. Z.; Ashfaq, F.; Hendrawati, T. D. Improved YOLOv5 Lane Line Real Time Segmentation System Integrating Seg Head Network. Engineering Proceedings 2025, 107(1), 49. [Google Scholar] [CrossRef]
- Yadav, S.; Tiwari, K.S.; Gupta, C.; Tiwari, M.K.; Khan, A.; Sonkar, S.P. A brief review on natural dyes, pigments: Recent advances and future perspectives. Results in Chemistry 2023, 5. [Google Scholar] [CrossRef]
- Li, Z. The impact and benefits of digital health management systems on chronic disease management. BIO Web of Conferences 2024. [Google Scholar]
- Ray, S. K.; Sirisena, H.; Deka, D. LTE-Advanced handover: An orientation matching-based fast and reliable approach. In 38th annual IEEE conference on local computer networks; IEEE, 2013; pp. 280–283. [Google Scholar]
- Brands, M. R.; Gouw, S. C.; Beestrum, M.; Cronin, R. M. Patient-centered digital health records and their effects on health outcomes: Systematic review. Journal of Medical Internet Research 2022. [Google Scholar] [CrossRef]
- Lim, M.; Abdullah, A.; Jhanjhi, N.Z. Performance optimization of criminal network hidden link prediction model with deep reinforcement learning. Journal of King Saud University - Computer and Information Sciences 2021, 33(10), 1202–1210. [Google Scholar] [CrossRef]
- Alon, N.; Torous, J. Current challenges for evaluating mobile health applications. Journal of the American Medical Informatics Association 2023. [Google Scholar] [CrossRef]
- Amagai, S.; Pila, S.; Kaat, A. J.; Nowinski, C. J. Challenges in participant engagement and retention using mobile health apps. Journal of Medical Internet Research 2022. [Google Scholar] [CrossRef] [PubMed]
- Dey, K.; Ray, S.; Bhattacharyya, P. K.; Gangopadhyay, A.; Bhasin, K. K.; Verma, R. D. Salicyladehyde 4-methoxybenzoylhydrazone and diacetylbis (4-methoxybenzoylhydrazone) as ligands for tin, lead and zirconium. J. Indian Chem. Soc. 1985, 62(11). [Google Scholar]
- Fitzpatrick, P. J. Improving health literacy using the power of digital communications to achieve better health outcomes. Frontiers in Digital Health 2023. [Google Scholar] [CrossRef]
- Istepanian, R. S. H. Mobile health (m-Health) in retrospect: The known unknowns. International Journal of Environmental Research and Public Health 2022. [Google Scholar] [CrossRef]
- Abernethy, A.; Adams, L.; Barrett, M.; et al. The promise of digital health: Then, now, and the future. National Academy of Medicine 2022. [Google Scholar] [CrossRef]
- Bajwa, J.; Munir, U.; Nori, A.; Williams, B. Artificial intelligence in healthcare: Transforming the practice of medicine. Future Healthcare Journal. 2021. [Google Scholar] [CrossRef] [PubMed]
- Jakob, R.; Harperink, S.; Rudolf, A. M.; Fleisch, E. Factors influencing adherence to mHealth apps for prevention or management of noncommunicable diseases: Systematic review. Journal of Medical Internet Research 2022. [Google Scholar] [CrossRef]
- Junaid, S. B.; Imam, A. A.; Balogun, A. O.; De Silva, L. C. Recent advancements in emerging technologies for healthcare management systems: A survey. Healthcare 2022. [Google Scholar] [CrossRef]
- Anwesa Chaudhuri, A. C.; Sanjib Ray, S. R. Antiproliferative activity of phytochemicals present in aerial parts aqueous extract of Ampelocissus latifolia (Roxb.) Planch. on apical meristem cells. 2015. [Google Scholar]
- Khairandish, M. O.; Sharma, M.; Jain, V.; Chatterjee, J. M.; Jhanjhi, N. Z. A hybrid CNN-SVM threshold segmentation approach for tumor detection and classification of MRI brain images. IRBM 2022, 43(4), 290–299. [Google Scholar] [CrossRef]
- Naik, N.; Hameed, B. M. Z.; Sooriyaperakasam, N.; et al. Transforming healthcare through a digital revolution: A review of digital healthcare technologies and solutions. Frontiers in Digital Health 2022. [Google Scholar] [CrossRef]
- Peng, Y.; Wang, H.; Fang, Q.; Xie, L.; Shu, L.; Sun, W.; Liu, Q. Effectiveness of Mobile Applications on Medication Adherence in Adults with Chronic Diseases: A Systematic Review and Meta-Analysis. J Manag Care Spec Pharm. 2020, 26(4), 550–561. [Google Scholar] [CrossRef] [PubMed] [PubMed Central]
- Qin, J.; Wu, Z.; Zhang, H.; Qi, X. Designing age-friendly interfaces and wearable–environment integrations to enhance medication adherence: a discrete choice experiment among older adults. Frontiers in Medicine 2026, 13. [Google Scholar] [CrossRef] [PubMed]
- Mehta, P.; Rao, A.; Upadhyay, N.; Mustafa, S.; Digra, V.; Wariar, A.; Soni, N.; Chatterjee, P.; Chakrawarty, A.; Sarwar, N. Use of Mobile Application for Improving Drug Compliance and Clinical Outcomes: A Randomized Controlled Trial. International Journal of Telemedicine and Applications 2026, 2026(1). [Google Scholar] [CrossRef] [PubMed]
- Drapkina, O.; Kontsevaya, A.; Deev, I. Programmatic approach to the prevention and control of hypertension as a key reserve for reducing mortality in the Russian Federation. Cardiovascular Therapy and Prevention 2026, 24(12), 4698. [Google Scholar] [CrossRef]
| Stage of Medication Management | Role of Artificial Intelligence | Benefits | Example AI Technologies | References |
|---|---|---|---|---|
| Medication Prescribing | AI assist physicians in selecting the most appropriate medication and dosage. | Reduces prescribing errors and improves treatment decisions. | Clinical Decision Support Systems (CDSS), Machine Learning algorithms | [23] |
| Medication Dispensing | AI supports pharmacy systems by verifying prescriptions, detecting drug interactions. | Improves accuracy in dispensing and reduces medication errors. | Automated pharmacy systems, AI-based verification tools | [24] |
| Medication Administration | AI systems monitor medication administration processes in hospitals and healthcare facilities to ensure correct drug delivery and timing. | Enhances patient safety and reduces administration mistakes. | Smart infusion pumps, AI monitoring systems | [25] |
| Medication Monitoring | AI analyzes patient health data from electronic health records and wearable devices | Enables early detection of drug-related problems and supports personalized treatment. | Predictive analytics, AI health monitoring platforms | [26] |
| Medication Adherence | AI mobile health applications remind patients to take medications. | Improves patient compliance and treatment outcomes. | mHealth apps, digital health platforms | [27] |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the author. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license.




