Submitted:
26 March 2026
Posted:
27 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
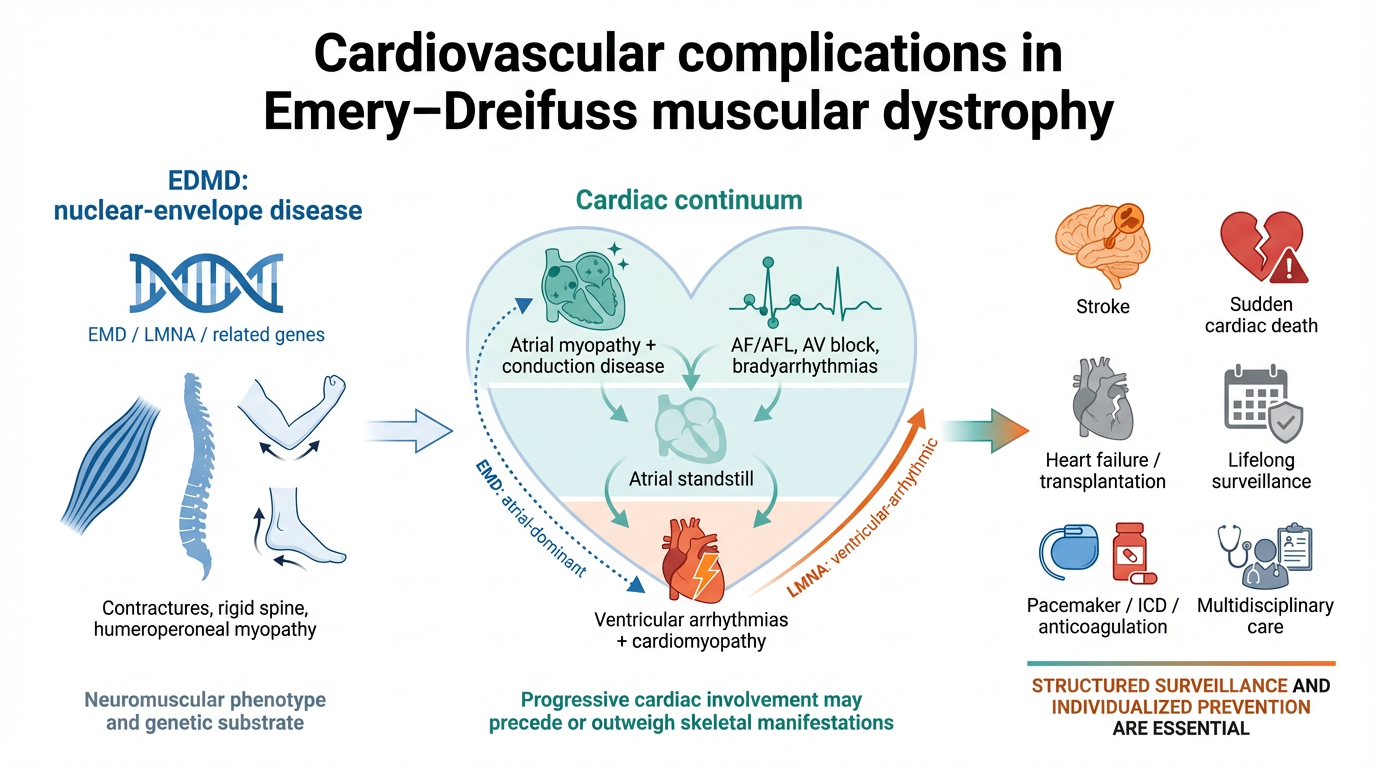
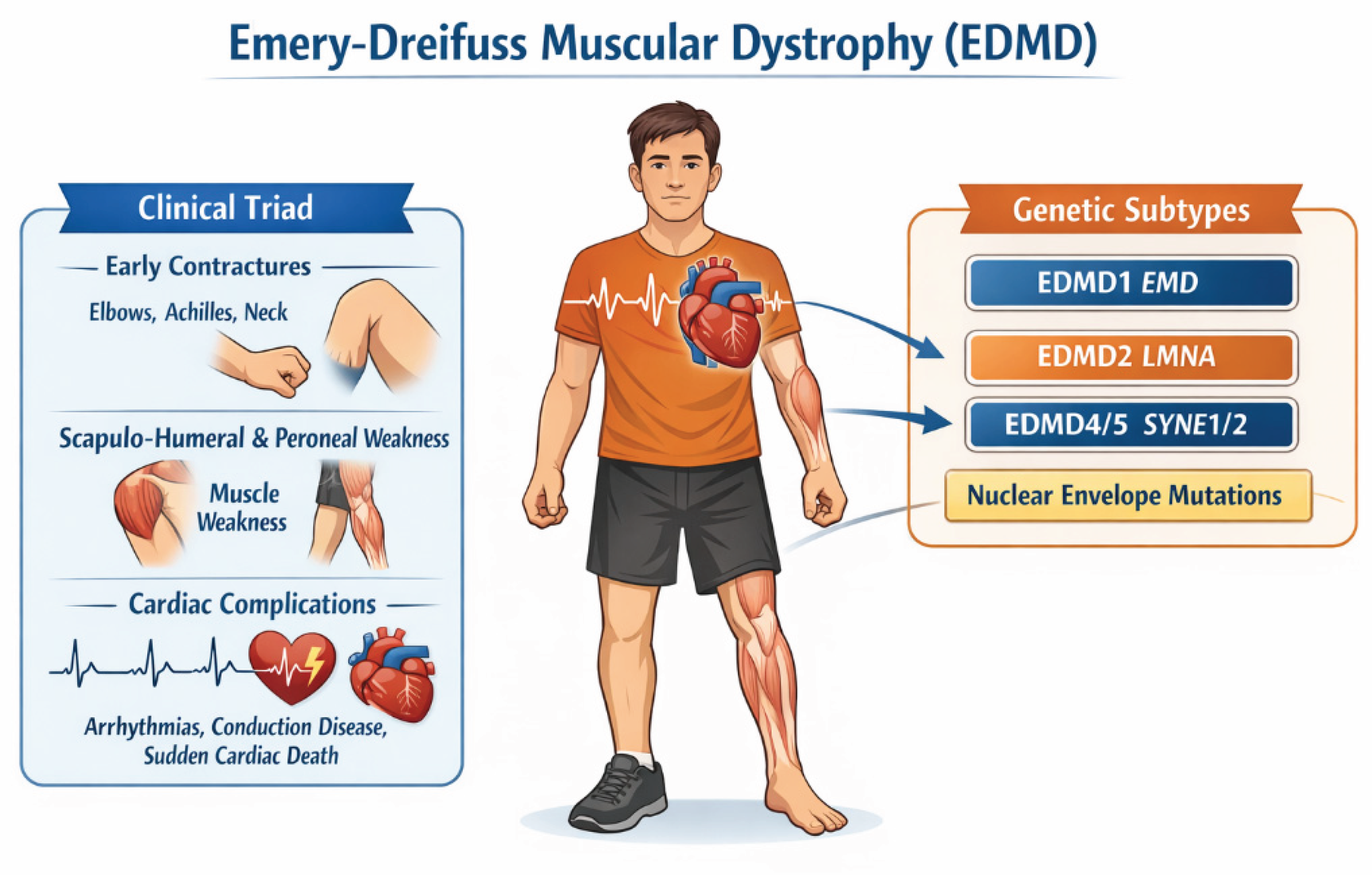
- early contractures (particularly involving the elbows, Achilles tendons, and cervical spine), often preceding the onset of muscle weakness;
- slowly progressive myopathy with a scapulohumeral and peroneal distribution;
- cardiac involvement with conduction system disease, responsible for syncope and sudden cardiac death, already recognized as an integral component of the disorder
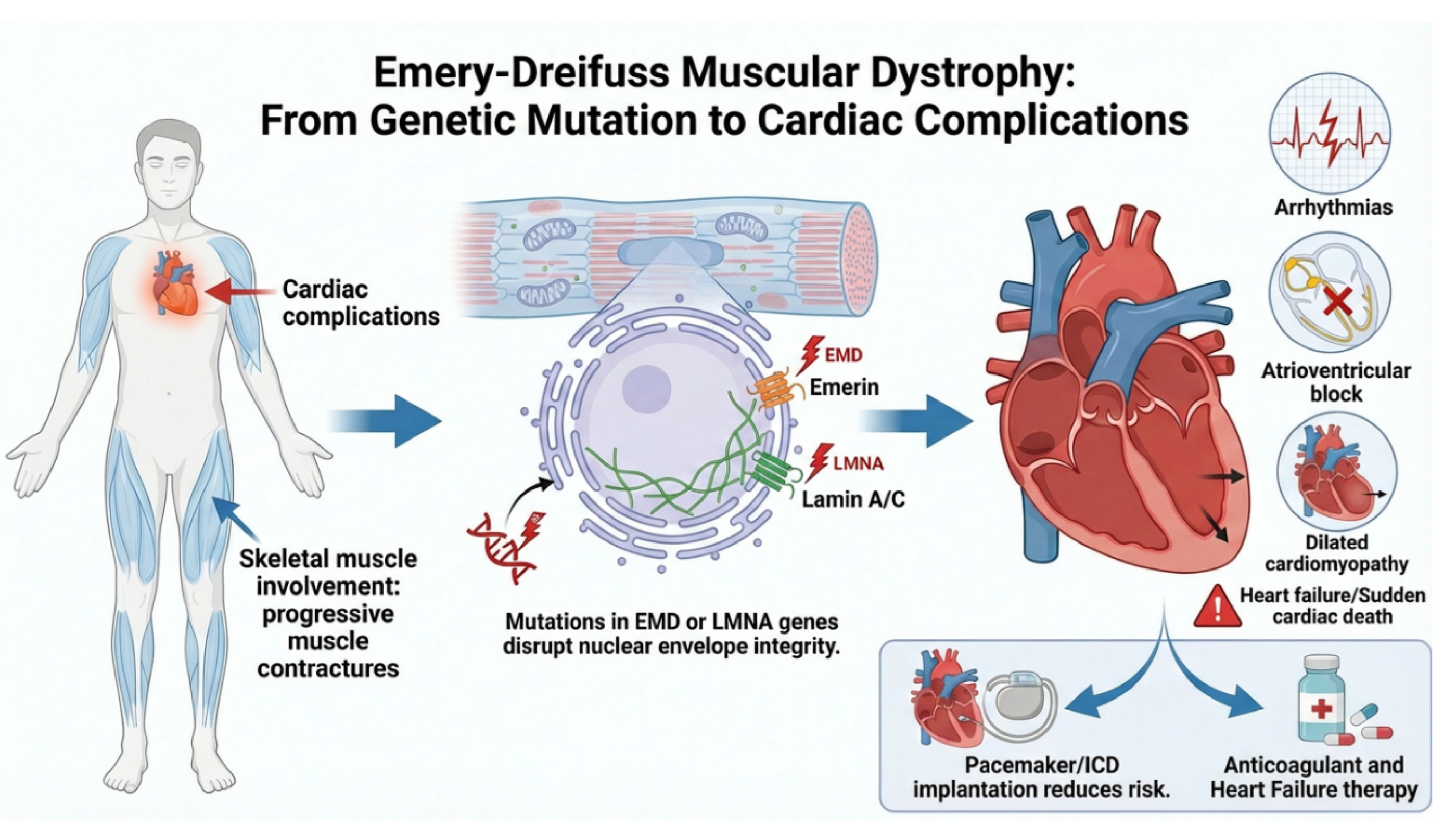
- EDMD1 (X-linked transmission), the most frequently diagnosed form, linked to mutations in the EMD gene, which encodes the protein “emerin”, a component of the inner nuclear membrane;
- EDMD2 (laminopathy, autosomical dominant transmission), caused by mutations in the lamin gene (LMNA);
- EDMD4 and EDMD5, caused by mutations in the SYNE1 or SYNE2 genes, respectively, encoding nesprin-1 or nesprin-2.
2. Materials and Methods
3. Results
3.1. Epidemiology, Diagnostic Criteria, and Neuromuscular Involvement
3.1.1. Age and Sex Distribution
3.1.2. Neuromuscular Involvement: The Diagnostic Core of EDMD
3.1.3. Peripheral Neuropathy: Accessory Feature and Overlap Phenotypes
3.1.4. Integrated Diagnostic Criteria
- Typical neuromuscular phenotype: early selective contractures plus humeroperoneal myopathy and/or rigid spine.
- Compatible cardiac phenotype: conduction disease, early atrial arrhythmias, ventricular arrhythmias and/or heart failure.
- Genetic confirmation: identification of a pathogenic or likely pathogenic variant in EMD, LMNA, or related nuclear envelope genes, followed by genetic counselling and cascade family screening.
3.2. Cardiac Involvement
3.2.1. Overview of Cardiac Complications in Emery-Dreifuss
3.2.2. Cardiac Imaging: Echocardiography and Cardiac Magnetic Resonance
3.2.3. Heart Failure and Heart Transplantation
3.2.4. ECG Abnormalities, Conduction Alterations and Brady-Arrhythmias
3.2.5. Atrial Arrhythmias
3.2.6. Ventricular Arrhythmias and Sudden Cardiac Death
- Sudden cardiac death
- Appropriate ICD shock for the termination of ventricular tachyarrhythmias (VT)
- Ventricular tachyarrhythmias associated with hemodynamic instability and other clinical manifestations
- Male sex
- Baseline left ventricular ejection fraction <45%
- Non-missense genetic mutations
- Non-sustained ventricular tachycardia
- AVB
3.2.7. Cardiac Implantable Electronic Device and Ablation Therapy
3.3. Current and Future Directions
4. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Permissions/Copyright
Conflicts of Interest
Abbreviations
| A | late transmitral diastolic filling velocity |
| AF | atrial fibrillation |
| AFL | atrial flutter |
| AI | artificial intelligence |
| APBs | atrial premature beats |
| AT | atrial tachycardia |
| AV | atrioventricular |
| AVB | atrioventricular block |
| BMD | Becker muscular dystrophy |
| CK | creatine kinase |
| CMR | cardiac magnetic resonance |
| CRISPR/Cas | clustered regularly interspaced short palindromic repeats/CRISPR-associated system |
| CRT | cardiac resynchronization therapy |
| CTG | cytosine-thymine-guanine repeat expansion |
| DCM | dilated cardiomyopathy |
| DDD | dual-chamber paced, dual-chamber sensed, dual response to sensing |
| DMD | Duchenne muscular dystrophy |
| E | early transmitral diastolic filling velocity |
| ECG | electrocardiogram/electrocardiography |
| ECV | extracellular volume |
| EDMD | Emery-Dreifuss muscular dystrophy |
| EMD | emerin gene |
| EMG | electromyography |
| ESC | European Society of Cardiology |
| HF | heart failure |
| HRS | Heart Rhythm Society |
| HV | His-ventricular interval |
| ICD | implantable cardioverter-defibrillator |
| ICMJE | International Committee of Medical Journal Editors |
| iPSC | induced pluripotent stem cell |
| LGE | late gadolinium enhancement |
| LINC | linker of nucleoskeleton and cytoskeleton |
| LMNA | lamin A/C gene |
| LV | left ventricle/left ventricular |
| LVEF | left ventricular ejection fraction |
| LTVTA | life-threatening ventricular tachyarrhythmias |
| MACE | major adverse cardiovascular events |
| miRNA | microRNA |
| NDLVC | non-dilated left ventricular cardiomyopathy |
| NSVT | non-sustained ventricular tachycardia |
| NYHA | New York Heart Association |
| PM | pacemaker |
| RNA | ribonucleic acid |
| SCD | sudden cardiac death |
| SVT | supraventricular tachyarrhythmias |
| SYNE1 | spectrin repeat containing nuclear envelope protein 1 gene |
| SYNE2 | spectrin repeat containing nuclear envelope protein 2 gene |
| TGFβ | transforming growth factor beta |
| VA | ventricular arrhythmias |
| VF | ventricular fibrillation |
| VVI | ventricular paced, ventricular sensed, inhibited response |
| VT | ventricular tachycardia |
References
- Emery, A. E.; Dreifuss, F. E. Unusual Type of Benign X-Linked Muscular Dystrophy. Journal of Neurology, Neurosurgery & Psychiatry 1966, 29(4), 338–342. [Google Scholar] [CrossRef]
- Wang, S.; Peng, D. Cardiac Involvement in Emery-Dreifuss Muscular Dystrophy and Related Management Strategies. Int. Heart J. 2019, 60(1), 12–18. [Google Scholar] [CrossRef] [PubMed]
- Pillers, DA; Von Bergen, NH. Emery-Dreifuss muscular dystrophy: a test case for precision medicine. Appl Clin Genet. 2016, 9, 27–32. [Google Scholar] [CrossRef] [PubMed]
- Cattin, E.; Schena, E.; Mattioli, E.; Marcuzzo, S.; Bonanno, S.; Cavalcante, P.; Corradi, F.; Benati, D.; Farinazzo, G.; Cattaneo, M.; et al. Profibrotic Molecules Are Reduced in CRISPR-Edited Emery–Dreifuss Muscular Dystrophy Fibroblasts. Cells 2025, 14(17), 1321. [Google Scholar] [CrossRef]
- Heller, S. A.; Shih, R.; Kalra, R.; Kang, P. B. Emery-Dreifuss Muscular Dystrophy. Muscle and Nerve 2020, 61(4), 436–448. [Google Scholar] [CrossRef] [PubMed]
- Sanna, T. Cardiac Features of Emery–Dreifuss Muscular Dystrophy Caused by Lamin A/C Gene Mutations. European Heart Journal 2003, 24(24), 2227–2236. [Google Scholar] [CrossRef]
- Merlini, L.; Granata, C.; Dominici, P.; Bonfiglioli, S. Emery—Dreifuss Muscular Dystrophy: Report of Five Cases in a Family and Review of the Literature. Muscle and Nerve 1986, 9(6), 481–485. [Google Scholar] [CrossRef]
- Ishikawa, T.; Mishima, H.; Barc, J.; Takahashi, M. P.; Hirono, K.; Terada, S.; Kowase, S.; Sato, T.; Mukai, Y.; Yui, Y.; et al. N. Cardiac Emerinopathy: A Nonsyndromic Nuclear Envelopathy With Increased Risk of Thromboembolic Stroke Due to Progressive Atrial Standstill and Left Ventricular Noncompaction. Circ: Arrhythmia and Electrophysiology 2020, 13(10). [Google Scholar] [CrossRef]
- Arbelo, E.; Protonotarios, A.; Gimeno, J. R.; Arbustini, E.; Barriales-Villa, R.; Basso, C.; Bezzina, C. R.; Biagini, E.; Blom, N. A.; De Boer, R. A.; et al. 2023 ESC Guidelines for the Management of Cardiomyopathies. European Heart Journal 2023, 44(37), 3503–3626. [Google Scholar] [CrossRef]
- Mah, J. K.; Korngut, L.; Fiest, K. M.; Dykeman, J.; Day, L. J.; Pringsheim, T.; Jette, N. A Systematic Review and Meta-Analysis on the Epidemiology of the Muscular Dystrophies. Can. J. Neurol. Sci. 2016, 43(1), 163–177. [Google Scholar] [CrossRef]
- Norwood, F. L. M.; Harling, C.; Chinnery, P. F.; Eagle, M.; Bushby, K.; Straub, V. Prevalence of Genetic Muscle Disease in Northern England: In-Depth Analysis of a Muscle Clinic Population. Brain 2009, 132(11), 3175–3186. [Google Scholar] [CrossRef]
- Viggiano, E.; Madej-Pilarczyk, A.; Carboni, N.; Picillo, E.; Ergoli, M.; Del Gaudio, S.; Marchel, M.; Nigro, G.; Palladino, A.; Politano, L. X-Linked Emery–Dreifuss Muscular Dystrophy: Study Of X-Chromosome Inactivation and Its Relation with Clinical Phenotypes in Female Carriers. Genes 2019, 10(11), 919. [Google Scholar] [CrossRef]
- Ben Yaou, R.; Leturcq, F.; Bonne, G. Emery-Dreifuss Muscular Dystrophy GeneReviews; University of Washington: Seattle: Seattle (WA), 2004. [Google Scholar]
- Orphanet. Emery-Dreifuss Muscular Dystrophy (ORPHA:261) [Internet]. Orphanet. 20 Mar 2026. Available online: Https://Www.Orpha.Net/En/Disease/Detail/261.
- Hershberger, R. E.; Givertz, M. M.; Ho, C. Y.; Judge, D. P.; Kantor, P. F.; McBride, K. L.; Morales, A.; Taylor, M. R. G.; Vatta, M.; Ware, S. M. Genetic Evaluation of Cardiomyopathy—A Heart Failure Society of America Practice Guideline. Journal of Cardiac Failure 2018, 24(5), 281–302. [Google Scholar] [CrossRef]
- Cannie, D. E.; Syrris, P.; Protonotarios, A.; Bakalakos, A.; Pruny, J.-F.; Ditaranto, R.; Martinez-Veira, C.; Larrañaga-Moreira, J. M.; Medo, K.; Bermúdez-Jiménez, F. J.; et al. Emery–Dreifuss Muscular Dystrophy Type 1 Is Associated with a High Risk of Malignant Ventricular Arrhythmias and End-Stage Heart Failure. European Heart Journal 2023, 44(48), 5064–5073. [Google Scholar] [CrossRef] [PubMed]
- Captur, G.; Arbustini, E.; Bonne, G.; Syrris, P.; Mills, K.; Wahbi, K.; Mohiddin, S. A.; McKenna, W. J.; Pettit, S.; Ho, C. Y.; et al. Lamin and the Heart. Heart 2018, 104(6), 468–479. [Google Scholar] [CrossRef] [PubMed]
- Kramarenko, D.; Walsh, R. Emery–Dreifuss Muscular Dystrophy: A Closer Look at Cardiac Complications. European Heart Journal 2023, 44(48), 5074–5076. [Google Scholar] [CrossRef]
- Madej-Pilarczyk, A. Clinical Aspects of Emery-Dreifuss Muscular Dystrophy. Nucleus 2018, 9(1), 268–274. [Google Scholar] [CrossRef] [PubMed]
- Maggi, L.; Carboni, N.; Bernasconi, P. Skeletal Muscle Laminopathies: A Review of Clinical and Molecular Features. Cells 2016, 5(3), 33. [Google Scholar] [CrossRef] [PubMed]
- 21 Yunisova, G.; Ceylaner, S.; Oflazer, P.; Deymeer, F.; Parman, Y. G.; Durmus, H. Clinical and Genetic Characteristics of Emery-Dreifuss Muscular Dystrophy Patients from Turkey: 30 Years Longitudinal Follow-up Study. Neuromuscular Disorders 2022, 32(9), 718–727. [Google Scholar] [CrossRef]
- Emery, AEH. Diagnostic Criteria for Neuromuscular Disorders, 2nd Ed. ed; Royal Society of Medicine Press: London, 1997. [Google Scholar]
- Bécane, H. M.; Bonne, G.; Varnous, S.; Muchir, A.; Ortega, V.; Hammouda, E. H.; Urtizberea, J. A.; Lavergne, T.; Fardeau, M.; Eymard, B.; et al. High Incidence of Sudden Death with Conduction System and Myocardial Disease Due to Lamins A and C Gene Mutation. Pacing Clin Electrophysiol 2000, 23 11 Pt 1, 1661–1666. [Google Scholar] [CrossRef]
- Steckiewicz, R.; Stolarz, P.; Świętoń, E.; Madej-Pilarczyk, A.; Grabowski, M.; Marchel, M.; Pieniak, M.; Filipiak, K. J.; Hausmanowa-Petrusewicz, I.; Opolski, G. Cardiac Pacing in 21 Patients with Emery-Dreifuss Muscular Dystrophy: A Single-Centre Study with a 39-Year Follow-Up. Kardiol Pol 2016, 74(6), 576–583. [Google Scholar] [CrossRef] [PubMed]
- Groh, W. J.; Bhakta, D.; Tomaselli, G. F.; Aleong, R. G.; Teixeira, R. A.; Amato, A.; Asirvatham, S. J.; Cha, Y.-M.; Corrado, D.; Duboc, D.; et al. 2022 HRS Expert Consensus Statement on Evaluation and Management of Arrhythmic Risk in Neuromuscular Disorders. Heart Rhythm 2022, 19(10), e61–e120. [Google Scholar] [CrossRef]
- Valenti, A. C.; Albini, A.; Imberti, J. F.; Vitolo, M.; Bonini, N.; Lattanzi, G.; Schnabel, R. B.; Boriani, G. Clinical Profile, Arrhythmias, and Adverse Cardiac Outcomes in Emery–Dreifuss Muscular Dystrophies: A Systematic Review of the Literature. Biology 2022, 11(4), 530. [Google Scholar] [CrossRef] [PubMed]
- Boriani, G.; Gallina, M.; Merlini, L.; Bonne, G.; Toniolo, D.; Amati, S.; Biffi, M.; Martignani, C.; Frabetti, L.; Bonvicini, M.; et al. Clinical Relevance of Atrial Fibrillation/Flutter, Stroke, Pacemaker Implant, and Heart Failure in Emery-Dreifuss Muscular Dystrophy: A Long-Term Longitudinal Study. Stroke 2003, 34(4), 901–908. [Google Scholar] [CrossRef] [PubMed]
- Marchel, M.; Madej-Pilarczyk, A.; Tymińska, A.; Steckiewicz, R.; Kochanowski, J.; Wysińska, J.; Ostrowska, E.; Balsam, P.; Grabowski, M.; Opolski, G. Echocardiographic Features of Cardiomyopathy in Emery-Dreifuss Muscular Dystrophy. Cardiology Research and Practice 2021, 2021, 1–7. [Google Scholar] [CrossRef]
- Blagova, O.; Nedostup, A.; Shumakov, D.; Poptsov, V.; Shestak, A.; Zaklyasminskaya, E. Dilated Cardiomyopathy with Severe Arrhythmias in Emery-Dreifuss Muscular Dystrophy: From Ablation to Heart Transplantation. J Atr Fibrillation 2016, 9(4), 1468. [Google Scholar] [CrossRef]
- Draminska, A.; Kuch-Wocial, A.; Szulc, M.; Zwolinska, A.; Styczynski, G.; Kostrubiec, M.; Hausmanowa-Petrusewicz, I.; Pruszczyk, P. Echocardiographic Assessment of Left Ventricular Morphology and Function in Patients with Emery–Dreifuss Muscular Dystrophy. International Journal of Cardiology 2005, 102(2), 207–210. [Google Scholar] [CrossRef]
- Smith, G.; Kinali, M.; Prasad, S.; Bonne, G.; Muntoni, F.; Pennell, D.; Nihoyannopoulos, P. Primary Myocardial Dysfunction in Autosomal Dominant EDMD. A Tissue Doppler and Cardiovascular Magnetic Resonance Study. Journal of Cardiovascular Magnetic Resonance 2006, 8(5), 723–730. [Google Scholar] [CrossRef]
- Haugaa, K. H.; Hasselberg, N. E.; Edvardsen, T. Mechanical Dispersion by Strain Echocardiography: A Predictor of Ventricular Arrhythmias in Subjects With Lamin A/C Mutations. JACC: Cardiovascular Imaging 2015, 8(1), 104–106. [Google Scholar] [CrossRef]
- Ditaranto, R.; Boriani, G.; Biffi, M.; Lorenzini, M.; Graziosi, M.; Ziacchi, M.; Pasquale, F.; Vitale, G.; Berardini, A.; Rinaldi, R.; et al. Differences in Cardiac Phenotype and Natural History of Laminopathies with and without Neuromuscular Onset. Orphanet J Rare Dis 2019, 14(1), 263. [Google Scholar] [CrossRef]
- Blaszczyk, E.; Gröschel, J.; Schulz-Menger, J. Role of CMR Imaging in Diagnostics and Evaluation of Cardiac Involvement in Muscle Dystrophies. Curr Heart Fail Rep 2021, 18(4), 211–224. [Google Scholar] [CrossRef]
- Bulmer, L.; Ljungman, C.; Hallin, J.; Dahlberg, P.; Polte, C. L.; Hedberg-Oldfors, C.; Oldfors, A.; Gummesson, A. EMD Missense Variant Causes X-Linked Isolated Dilated Cardiomyopathy with Myocardial Emerin Deficiency. Eur J Hum Genet 2025, 33(6), 775–783. [Google Scholar] [CrossRef]
- Russo, V.; Hudelo, J.; Marcel, M.; Florence, J.; Soulat, G.; Manka, R.; Pontana, F.; Dacher, J. N.; Toupin, S.; Nazarian, S.; et al. Role of Cardiovascular Magnetic Resonance in Diagnosis and Management of Muscular Dystrophies. J Cardiovasc Magn Reson 2026, 102693. [Google Scholar] [CrossRef]
- Holmström, M.; Kivistö, S.; Heliö, T.; Jurkko, R.; Kaartinen, M.; Antila, M.; Reissell, E.; Kuusisto, J.; Kärkkäinen, S.; Peuhkurinen, K.; et al. Late Gadolinium Enhanced Cardiovascular Magnetic Resonance of Lamin A/C Gene Mutation Related Dilated Cardiomyopathy. J Cardiovasc Magn Reson 2011, 13(1), 30. [Google Scholar] [CrossRef] [PubMed]
- Topriceanu, C.-C.; Al-Farih, M.; Joy, G.; Chan, F.; Webber, M.; Ilie-Ablachim, D. C.; Shiwani, H.; Tamang, M.; Banks, C.; Pettit, S.; et al. The Cardiovascular Magnetic Resonance Phenotype of Lamin Heart Disease. JACC Cardiovasc Imaging 2025, 18(6), 644–660. [Google Scholar] [CrossRef] [PubMed]
- Bonne, G; Mercuri, E; Muchir, A; Urtizberea, A; Bécane, HM; Recan, D; Merlini, L; Wehnert, M; Boor, R; Reuner, U; et al. Clinical and Molecular Genetic Spectrum of Autosomal Dominant Emery-Dreifuss Muscular Dystrophy Due to Mutations of the Lamin A/C Gene. Ann Neurol 2000, 48(2), 170–80. [Google Scholar] [CrossRef]
- Boriani, G.; Biagini, E.; Ziacchi, M.; Malavasi, V. L.; Vitolo, M.; Talarico, M.; Mauro, E.; Gorlato, G.; Lattanzi, G. Cardiolaminopathies from Bench to Bedside: Challenges in Clinical Decision-Making with Focus on Arrhythmia-Related Outcomes. Nucleus 2018, 9(1), 442–459. [Google Scholar] [CrossRef]
- Feingold, B.; Mahle, W. T.; Auerbach, S.; Clemens, P.; Domenighetti, A. A.; Jefferies, J. L.; Judge, D. P.; Lal, A. K.; Markham, L. W.; Parks, W. J.; et al. Management of Cardiac Involvement Associated With Neuromuscular Diseases: A Scientific Statement From the American Heart Association. Circulation 2017, 136(13). [Google Scholar] [CrossRef]
- Finocchiaro, G.; Merlo, M.; Sheikh, N.; De Angelis, G.; Papadakis, M.; Olivotto, I.; Rapezzi, C.; Carr-White, G.; Sharma, S.; Mestroni, L.; et al. The Electrocardiogram in the Diagnosis and Management of Patients with Dilated Cardiomyopathy. European Journal of Heart Failure 2020, 22(7), 1097–1107. [Google Scholar] [CrossRef] [PubMed]
- Cesar, S.; Campuzano, O.; Cruzalegui, J.; Fiol, V.; Moll, I.; Martínez-Barrios, E.; Zschaeck, I.; Natera-de Benito, D.; Ortez, C.; Carrera, L.; et al. Characterization of Cardiac Involvement in Children with LMNA-Related Muscular Dystrophy. Front. Cell Dev. Biol. 2023, 11, 1142937. [Google Scholar] [CrossRef]
- Taylor, M. R. G.; Fain, P. R.; Sinagra, G.; Robinson, M. L.; Robertson, A. D.; Carniel, E.; Di Lenarda, A.; Bohlmeyer, T. J.; Ferguson, D. A.; Brodsky, G. L.; et al. Natural History of Dilated Cardiomyopathy Due to Lamin A/C Gene Mutations. Journal of the American College of Cardiology 2003, 41(5), 771–780. [Google Scholar] [CrossRef]
- Van Berlo, J. H.; De Voogt, W. G.; Van Der Kooi, A. J.; Van Tintelen, J. P.; Bonne, G.; Yaou, R. B.; Duboc, D.; Rossenbacker, T.; Heidbüchel, H.; De Visser, M.; et al. Meta-Analysis of Clinical Characteristics of 299 Carriers of LMNA Gene Mutations: Do Lamin A/C Mutations Portend a High Risk of Sudden Death? J Mol Med 2005, 83(1), 79–83. [Google Scholar] [CrossRef] [PubMed]
- Marchel, M.; Madej-Pilarczyk, A.; Tymińska, A.; Steckiewicz, R.; Ostrowska, E.; Wysińska, J.; Russo, V.; Grabowski, M.; Opolski, G. Cardiac Arrhythmias in Muscular Dystrophies Associated with Emerinopathy and Laminopathy: A Cohort Study. JCM 2021, 10(4), 732. [Google Scholar] [CrossRef]
- Bialer, M. G.; Mcdaniel, N. L.; Kelly, T. E. Progression of Cardiac Disease in Emery-dreifuss Muscular Dystrophy. Clinical Cardiology 1991, 14(5), 411–416. [Google Scholar] [CrossRef]
- Bonne, G.; Mercuri, E.; Muchir, A.; Urtizberea, A.; Bécane, H. M.; Recan, D.; Merlini, L.; Wehnert, M.; Boor, R.; Reuner, U.; et al. Clinical and Molecular Genetic Spectrum of Autosomal Dominant Emery-Dreifuss Muscular Dystrophy Due to Mutations of the Lamin A/C Gene. Ann Neurol 2000, 48(2), 170–180. [Google Scholar] [CrossRef] [PubMed]
- Priori, S. Task Force on Sudden Cardiac Death of the European Society of Cardiology. European Heart Journal 2001, 22(16), 1374–1450. [Google Scholar] [CrossRef]
- Rootwelt-Norberg, C.; Skjølsvik, E. T.; Chivulescu, M.; Bogsrud, M. P.; Ribe, M. P.; Aabel, E. W.; Beitnes, J. O.; Brekke, P. H.; Håland, T. F.; Hasselberg, N. E.; et al. Disease Progression Rate Is a Strong Predictor of Ventricular Arrhythmias in Patients with Cardiac Laminopathies: A Primary Prevention Cohort Study. EP Europace 2023, 25(2), 634–642. [Google Scholar] [CrossRef] [PubMed]
- Peretto, G.; Sala, S.; Lazzeroni, D.; Palmisano, A.; Gigli, L.; Esposito, A.; De Cobelli, F.; Camici, P. G.; Mazzone, P.; Basso, C.; et al. Septal Late Gadolinium Enhancement and Arrhythmic Risk in Genetic and Acquired Non-Ischaemic Cardiomyopathies. Heart, Lung and Circulation 2020, 29(9), 1356–1365. [Google Scholar] [CrossRef]
- Escobar-Lopez, L.; Ochoa, J. P.; Mirelis, J. G.; Espinosa, M. Á.; Navarro, M.; Gallego-Delgado, M.; Barriales-Villa, R.; Robles-Mezcua, A.; Basurte-Elorz, M. T.; Gutiérrez García-Moreno, L.; et al. Association of Genetic Variants With Outcomes in Patients With Nonischemic Dilated Cardiomyopathy. J Am Coll Cardiol 2021, 78(17), 1682–1699. [Google Scholar] [CrossRef]
- Kayvanpour, E.; Sedaghat-Hamedani, F.; Amr, A.; Lai, A.; Haas, J.; Holzer, D. B.; Frese, K. S.; Keller, A.; Jensen, K.; Katus, H. A.; Meder, B. Genotype-Phenotype Associations in Dilated Cardiomyopathy: Meta-Analysis on More than 8000 Individuals. Clin Res Cardiol 2017, 106(2), 127–139. [Google Scholar] [CrossRef]
- van Rijsingen, I. A. W.; Arbustini, E.; Elliott, P. M.; Mogensen, J.; Hermans-van Ast, J. F.; van der Kooi, A. J.; van Tintelen, J. P.; van den Berg, M. P.; Pilotto, A.; Pasotti, M.; et al. Risk Factors for Malignant Ventricular Arrhythmias in Lamin a/c Mutation Carriers a European Cohort Study. J Am Coll Cardiol 2012, 59(5), 493–500. [Google Scholar] [CrossRef]
- Wahbi, K.; Ben Yaou, R.; Gandjbakhch, E.; Anselme, F.; Gossios, T.; Lakdawala, N. K.; Stalens, C.; Sacher, F.; Babuty, D.; Trochu, J.-N.; et al. Development and Validation of a New Risk Prediction Score for Life-Threatening Ventricular Tachyarrhythmias in Laminopathies. Circulation 2019, 140(4), 293–302. [Google Scholar] [CrossRef]
- Glikson, M.; Nielsen, J. C.; Kronborg, M. B.; Michowitz, Y.; Auricchio, A.; Barbash, I. M.; Barrabés, J. A.; Boriani, G.; Braunschweig, F.; Brignole, M.; et al. 2021 ESC Guidelines on Cardiac Pacing and Cardiac Resynchronization Therapy. European Heart Journal 2021, 42(35), 3427–3520. [Google Scholar] [CrossRef]
- Golzio, P. G.; Chiribiri, A.; Gaita, F. “Unexpected” Sudden Death Avoided by Implantable Cardioverter Defibrillator in Emery Dreifuss Patient. Europace 2007, 9(12), 1158–1160. [Google Scholar] [CrossRef]
- Wyse, D. G.; Nath, F. C.; Brownell, A. K. W. Benign X-Linked (Emery-Dreifuss) Muscular Dystrophy Is Not Benign. Pacing Clinical Electrophis 1987, 10(3), 533–536. [Google Scholar] [CrossRef]
- Zeppenfeld, K.; Tfelt-Hansen, J.; De Riva, M.; Winkel, B. G.; Behr, E. R.; Blom, N. A.; Charron, P.; Corrado, D.; Dagres, N.; De Chillou, C.A. 2022 ESC Guidelines for the Management of Patients with Ventricular Arrhythmias and the Prevention of Sudden Cardiac Death. European Heart Journal 2022, 43(40), 3997–4126. [Google Scholar] [CrossRef]
- Walker, S. Biventricular Implantable Cardioverter Defibrillator Use in a Patient with Heart Failure and Ventricular Tachycardia Secondary to Emery-Dreifuss Syndrome. Europace 1999, 1(3), 206–209. [Google Scholar] [CrossRef] [PubMed]
- Carvalho, A. A.; Levy, J. A.; Gutierrez, P. S.; Marie, S. K.; Sosa, E. A.; Scanavaca, M. Emery-Dreifuss Muscular Dystrophy: Anatomical-Clinical Correlation (Case Report). Arq Neuropsiquiatr 2000, 58(4), 1123–1127. [Google Scholar] [CrossRef] [PubMed]
- Butt, K.; Ambati, S. Atrial Arrhythmias in Emery-Dreifuss Muscular Dystrophy: Approach to Successful Ablation. HeartRhythm Case Rep 2020, 6(6), 318–321. [Google Scholar] [CrossRef] [PubMed]
- Valverde Soria, L.; Sanchez-Millan, P. J.; Fernandez-Sanchez, J. A.; Macías-Ruiz, R.; Jimenez-Jaimez, J.; Tercedor, L. Successful Ablation of Purkinje-Related Ventricular Ectopy Leading to Ventricular Fibrillation in Emery-Dreifuss Dilated Cardiomyopathy. J Interv Card Electrophysiol 2025, 68(5), 957–960. [Google Scholar] [CrossRef]
- Zeppenfeld, K. Ventricular Tachycardia Ablation in Nonischemic Cardiomyopathy. JACC Clin Electrophysiol 2018, 4(9), 1123–1140. [Google Scholar] [CrossRef] [PubMed]
| Domain | Key features | Clinical relevance | Diagnostic tools | Implications for management |
| Neuromuscular phenotype | Early selective contractures involving elbows, Achilles tendons, and cervical/paraspinal muscles; humeroperoneal muscle weakness; rigid spine | Core phenotypic hallmark of classical EDMD and major clue for clinical suspicion | Neurological examination, musculoskeletal assessment, functional evaluation | Triggers targeted cardiological assessment and genetic testing |
| Skeletal muscle laboratory/electrophysiology | Serum CK often normal or only mildly elevated; EMG usually shows non-specific myopathic changes | Helpful as supportive but non-definitive findings; normal CK does not exclude EDMD | Serum CK, electromyography | Supports integrated work-up; should not delay molecular testing |
| Peripheral neuropathy / overlap phenotype | Occasional neurogenic features, mainly in selected LMNA-related cases; myopathy–neuropathy overlap may occur | Does not exclude EDMD when the typical contracture–myopathy pattern is present; helps refine phenotype | Nerve conduction studies, EMG, neurological re-evaluation | Broadens differential diagnosis and may justify extended genetic testing |
| Cardiac phenotype | Conduction disease, sinus node dysfunction, atrial fibrillation/flutter, atrial standstill, ventricular arrhythmias, cardiomyopathy, heart failure | Major determinant of morbidity and mortality; may precede overt neuromuscular manifestations | 12-lead ECG, prolonged Holter monitoring, echocardiography, CMR when available | Enables early rhythm surveillance, anticoagulation assessment, and device-based risk stratification |
| Family history | Sudden cardiac death, pacemaker implantation, cardiomyopathy, muscular dystrophy, stroke, unexplained syncope | Strengthens suspicion of inherited cardio-neuromuscular disease | Pedigree analysis, family interview | Supports cascade screening and anticipatory evaluation of relatives |
| Genetic confirmation | Pathogenic/likely pathogenic variants in EMD, LMNA, SYNE1, SYNE2, or related nuclear-envelope/LINC complex genes | Confirms diagnosis, refines prognosis, and supports genotype-oriented follow-up | Targeted gene testing, cardiomyopathy/neuromuscular gene panels, variant interpretation | Enables counselling, longitudinal risk stratification, and family screening |
| Female carrier / genotype-positive relative evaluation | Female EMD carriers or asymptomatic relatives may show delayed or isolated cardiac involvement | Clinically relevant because cardiac disease may emerge late and independently of skeletal manifestations | ECG, Holter, echocardiography, genetic counselling | Supports lifelong cardiac surveillance even in apparently asymptomatic carriers |
| Integrated final diagnosis | Combined recognition of typical neuromuscular pattern, compatible cardiac phenotype, and molecular confirmation | Contemporary diagnosis is multidisciplinary and aetiology-driven rather than purely descriptive | Joint neurology–cardiology–genetics assessment | Supports individualized monitoring and prevention of arrhythmic, thromboembolic, and heart failure complications |
| Genotype / disease subgroup | Inheritance | Typical extra-cardiac phenotype | Predominant cardiac phenotype | Characteristic clinical course | Main management implications |
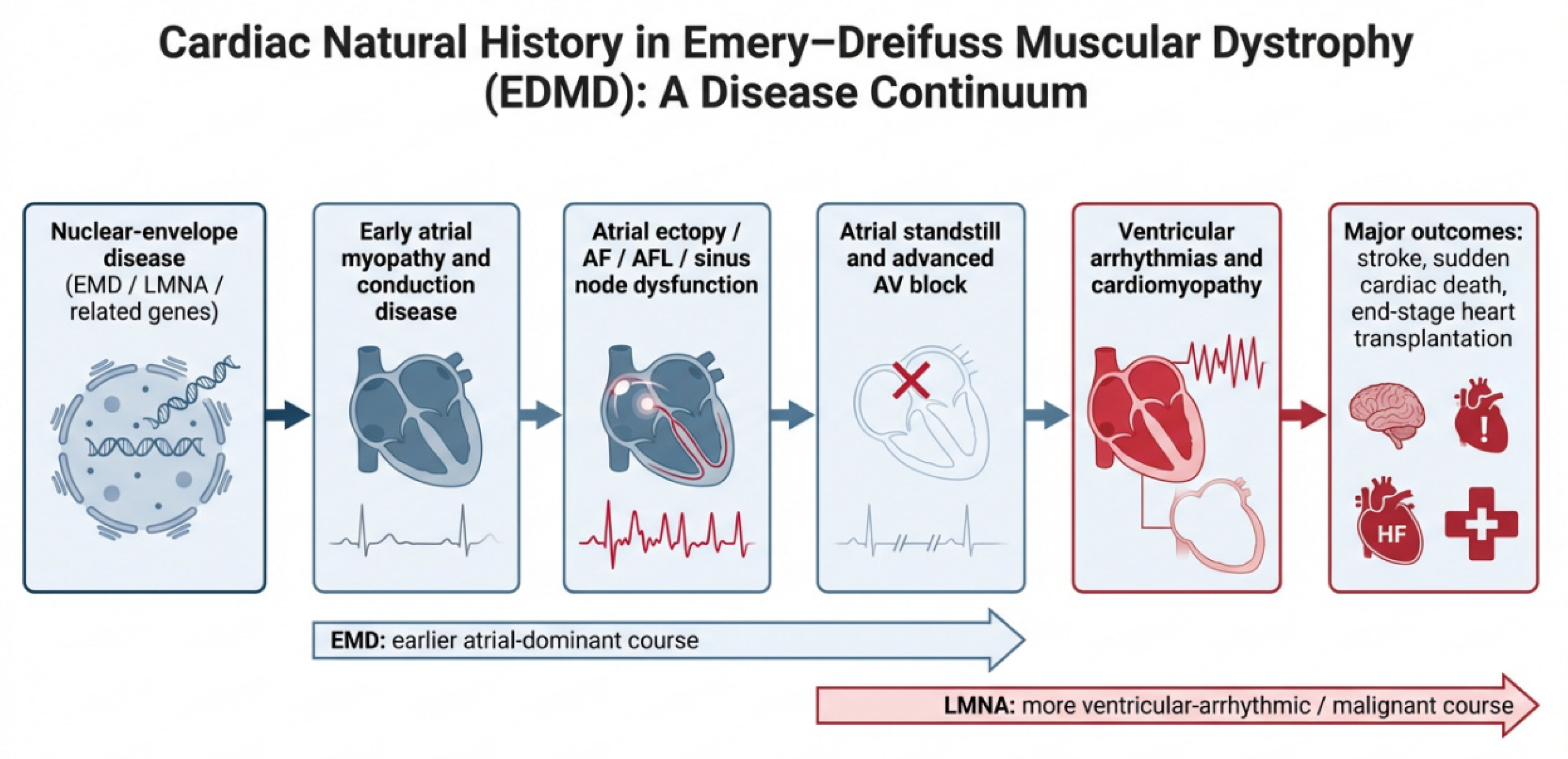
| EMD-related EDMD (EDMD1 / emerinopathy) | X-linked | Classical early contractures, humeroperoneal weakness, rigid spine; full phenotype mainly in males; female carriers often milder and later | Early atrial disease and conduction abnormalities; AF/AFL, atrial standstill, sinus node dysfunction, AV block; ventricular dysfunction may occur later | Often atrial-dominant in the early phase, with progression from atrial ectopy/tachyarrhythmias to atrial standstill and thromboembolic risk; malignant ventricular arrhythmias may still occur in selected patients | Lifelong rhythm surveillance; strong attention to atrial arrhythmias, atrial standstill, and thromboembolic prevention; pacing frequently required, but ICD may be needed in selected higher-risk cases |
| LMNA-related EDMD / laminopathy (EDMD2 and overlapping laminopathic cardiomyopathy phenotypes) | Usually autosomal dominant | Neuromuscular phenotype may be classical, subtle, delayed, or even overshadowed by cardiac manifestations; both sexes affected | Conduction disease, atrial arrhythmias, ventricular arrhythmias, dilated cardiomyopathy, progressive LV dysfunction, heart failure | Often more ventricular-arrhythmic and malignant, with higher risk of NSVT/VT/VF, sudden cardiac death, and end-stage heart failure; cardiac-first presentation is common | Early ICD-oriented risk stratification is crucial; CMR and LMNA-specific risk models may refine prognosis; surveillance must address both arrhythmias and HF progression |
| SYNE1 / SYNE2-related EDMD (EDMD4/5 and related LINC-complex phenotypes) | Usually autosomal dominant or recessive depending on variant/context | Variable contractures and myopathy; phenotype often heterogeneous and less classically defined than EMD/LMNA forms | Cardiac phenotype less well characterized; may include conduction abnormalities, arrhythmias, and cardiomyopathic features | Natural history remains less clearly defined because of limited cohort data; penetrance and severity appear variable | Requires individualized follow-up within inherited cardio-neuromuscular programs; management usually extrapolated from broader EDMD/laminopathy principles |
| Female EMD carriers / genotype-positive relatives with limited neuromuscular phenotype | X-linked carrier state | Often absent, subtle, or delayed skeletal manifestations | Late-onset conduction disease, atrial arrhythmias, and other isolated cardiac manifestations may occur | Cardiac disease may emerge independently of overt muscular phenotype, often later in life | Cardiac surveillance should not be omitted on the basis of a mild skeletal phenotype or female sex |
| “Cardiac emerinopathy” / isolated or cardiac-predominant EMD phenotype | X-linked | Minimal or absent clinically relevant skeletal muscle involvement | Progressive atrial arrhythmias, atrial standstill, conduction disease, stroke risk; possible ventricular involvement/non-compaction in selected cases | Demonstrates that cardiac disease can dominate the phenotype and may be the presenting manifestation | Highlights the need to suspect EDMD-spectrum disease even in apparently isolated inherited arrhythmic/conduction phenotypes |
| Cardiac domain | Typical manifestations | Main clinical consequences | Prognostic significance | Preferred monitoring tools |
| Conduction system disease / bradyarrhythmias | Sinus bradycardia, sinoatrial block, first-degree AV block, bundle branch block, Mobitz II AV block, complete AV block | Fatigue, presyncope, syncope, pacemaker requirement, low-output symptoms | Hallmark of EDMD; often progressive and may precede overt cardiomyopathy | Serial ECG, prolonged Holter monitoring, device interrogation |
| Atrial myopathy and atrial ectopy | Atrial premature beats, atrial tachycardia, electrical instability at a young age | Symptoms, progression to AF/AFL, marker of evolving atrial disease | Often an early manifestation, especially in EMD-related disease | ECG, extended rhythm monitoring, device diagnostics when available |
| Atrial fibrillation / atrial flutter | Paroxysmal or persistent AF/AFL, often occurring early in life | Palpitations, haemodynamic intolerance, thromboembolic risk, progression to atrial standstill | Major determinant of stroke risk and marker of advanced atrial remodelling | ECG, prolonged Holter, device diagnostics, echocardiographic atrial assessment |
| Atrial standstill | Absence of P waves, atrial electrical silence, lack of atrial contraction, loss of atrial capture | Severe bradycardia, ineffective atrial pacing, thromboembolism, stroke | End-stage expression of atrial disease with major pacing and anticoagulation implications | ECG, echocardiography, device interrogation |
| Ventricular arrhythmias | Ventricular ectopy, NSVT, sustained VT, VF | Sudden cardiac death, ICD therapies, recurrent hospitalizations | One of the main determinants of prognosis, particularly in LMNA-related disease | Holter monitoring, ICD diagnostics, CMR, risk score integration in LMNA |
| Structural cardiomyopathy | Atrial enlargement, LV systolic dysfunction, dilated phenotype, occasional regional dysfunction | Reduced exercise tolerance, progressive ventricular remodelling, arrhythmic substrate | Variable across genotypes but strongly linked to HF progression and arrhythmic burden | Echocardiography, CMR, serial imaging follow-up |
| Heart failure | LV dysfunction, NYHA III–IV symptoms, progressive congestion, end-stage disease | Hospitalization, reduced survival, transplantation in selected cases | Major cause of mortality together with sudden cardiac death | Clinical follow-up, echocardiography, CMR, device-based follow-up |
| Thromboembolism / stroke | Cerebral embolic events, often in association with AF/AFL or atrial standstill | Permanent disability, recurrent events, increased mortality | Disproportionately high risk relative to patient age; requires proactive prevention | Rhythm surveillance, atrial mechanical assessment, anticoagulation-oriented evaluation |
| Imaging modality / parameter | Main findings in EDMD | Stage of disease in which useful | Potential clinical value | Main limitations |
| Standard transthoracic echocardiography | Atrial enlargement, variable LV systolic dysfunction, occasional dilated cardiomyopathy phenotype, chamber remodelling | Baseline and longitudinal follow-up across all stages | First-line structural and functional surveillance; identifies progression toward cardiomyopathy and HF | May underestimate early myocardial disease or subtle tissue abnormalities |
| Conventional Doppler / diastolic assessment | Impaired relaxation, altered E/A ratio, prolonged isovolumetric relaxation time, restrictive filling in advanced disease | Early subclinical dysfunction to overt cardiomyopathy | Detects early functional abnormalities beyond gross chamber dimensions | Interpretation may be affected by rhythm status, especially AF/AFL |
| Tissue Doppler imaging | Abnormal myocardial velocities despite preserved conventional indices in some patients | Early/subclinical stages | May reveal early myocardial dysfunction before overt LV remodelling | Operator-dependent and not fully standardized across centres |
| Speckle-tracking echocardiography / strain | Reduced deformation indices, impaired longitudinal mechanics, possible increased mechanical dispersion | Subclinical and intermediate disease stages | May refine early phenotyping and help identify patients at higher arrhythmic risk | Limited availability and limited EDMD-specific validation |
| Cardiac magnetic resonance: functional assessment | More accurate quantification of chamber volumes and ventricular function; detection of regional abnormalities | Particularly useful when echo findings are equivocal or disease progression is suspected | Improves phenotype definition and longitudinal characterization | Access and expertise may be limited |
| Cardiac magnetic resonance: tissue characterization | Mid-wall or septal LGE, increased extracellular volume, abnormal mapping indices, evidence of fibrosis substrate | Early to advanced disease, especially in LMNA-related phenotypes | Supports arrhythmic risk refinement and identification of subclinical myocardial involvement | Evidence in EDMD-specific cohorts remains limited and partly extrapolated from laminopathy series |
| Combined imaging approach | Echo for serial surveillance plus CMR for phenotypic clarification and tissue characterization | Across the disease continuum | Best overall strategy for integrated follow-up and risk assessment | Resource-dependent and not always feasible in routine practice |
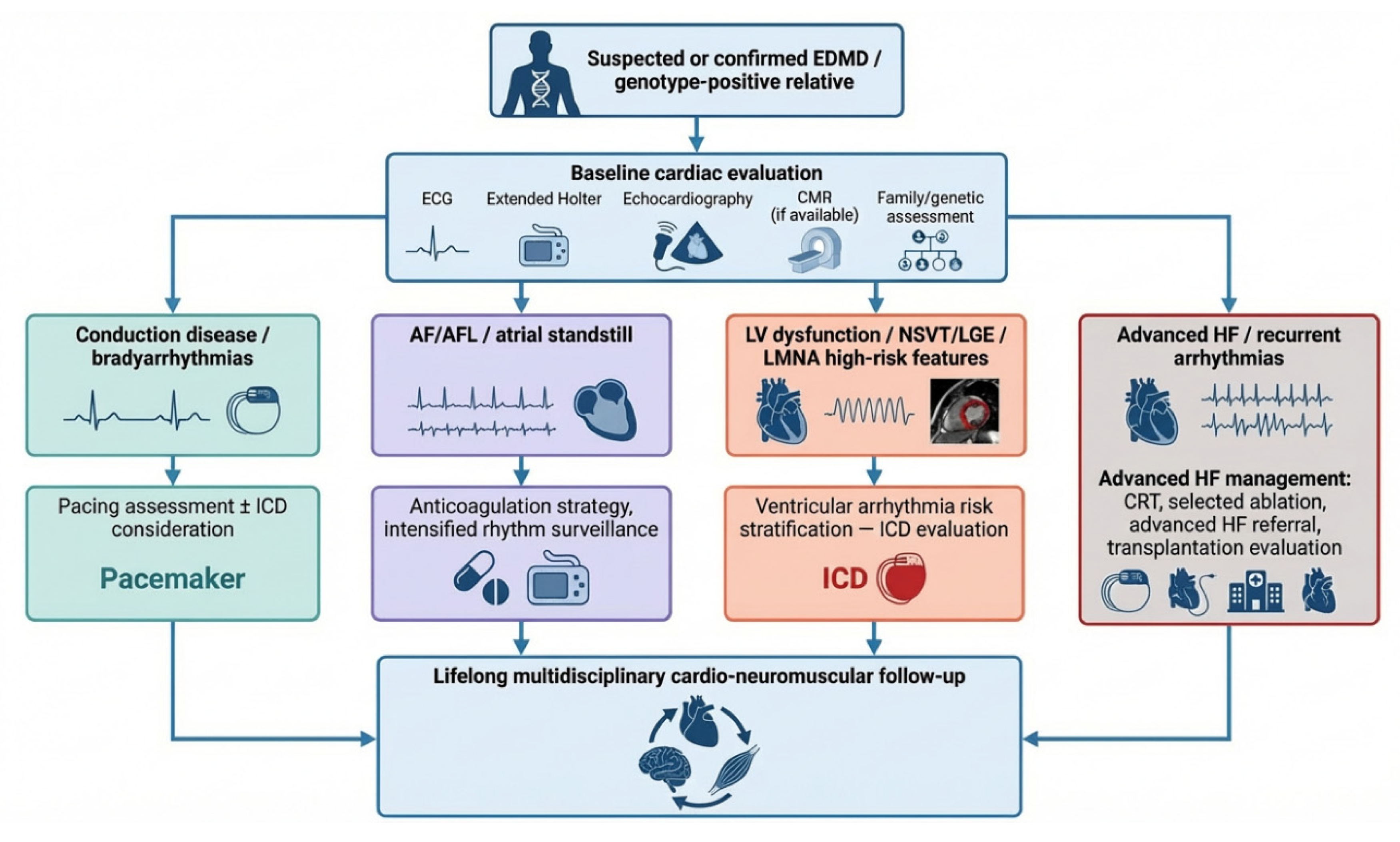
| Clinical scenario | Main problem | Suggested management approach | Key caveats in EDMD | Escalation options |
| Asymptomatic genotype-positive patient / early phenotype | Silent progression of conduction disease, atrial disease, or myocardial involvement | Lifelong structured surveillance with ECG, prolonged Holter, echocardiography, and CMR when available | Cardiac manifestations may precede or outweigh skeletal symptoms | Earlier referral to inherited cardiomyopathy / neuromuscular centre |
| Progressive conduction disease / bradyarrhythmias | Symptomatic bradycardia, advanced AV block, chronotropic incompetence | Permanent pacing according to guideline-based indications | Pacemaker therapy does not abolish the risk of malignant ventricular arrhythmias or sudden death | Consider ICD instead of pacing alone in selected high-risk patients |
| AF / AFL | Tachyarrhythmia, symptoms, stroke risk, progression of atrial disease | Rate/rhythm control strategy plus anticoagulation when indicated | Brady–tachy syndrome and coexisting conduction disease are common | Intensified rhythm monitoring, device-guided surveillance |
| Atrial standstill | Severe atrial myopathy, absent atrial contraction, embolic risk, atrial lead failure/loss of capture | Individualized pacing strategy and strong consideration of anticoagulation | Represents advanced atrial disease and may complicate device management | Device revision, specialist electrophysiology input |
| Ventricular arrhythmias / high-risk arrhythmic phenotype | NSVT, sustained VT/VF, sudden death risk | ICD-oriented risk stratification, especially in LMNA-related disease or when additional high-risk markers are present | Ventricular arrhythmias may occur despite only mild or moderate LV dysfunction | ICD implantation, tertiary arrhythmia referral |
| LV dysfunction / heart failure | Progressive cardiomyopathy with symptomatic HF | Guideline-directed medical therapy, serial imaging, clinical reassessment, device optimization when appropriate | EDMD-specific HF evidence is limited; progression may be genotype-dependent | CRT consideration, advanced HF referral |
| Recurrent arrhythmias despite drug/device therapy | Recurrent ICD therapies, refractory flutter/VT, electrical instability | Selected catheter ablation in expert centres | Diffuse fibrosis, intramural/atrial substrate, and disease progression may reduce success rates | Repeat ablation, combined advanced device/HF strategy |
| End-stage disease | Medically refractory HF and/or severe arrhythmic burden | Evaluation for advanced heart failure therapies | Rare but clinically relevant in advanced EDMD | Heart transplantation |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




