Submitted:
24 March 2026
Posted:
24 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Case and Ethical Considerations
2.2. Diagnosis of Refractory Nasal Vestibular Stenosis
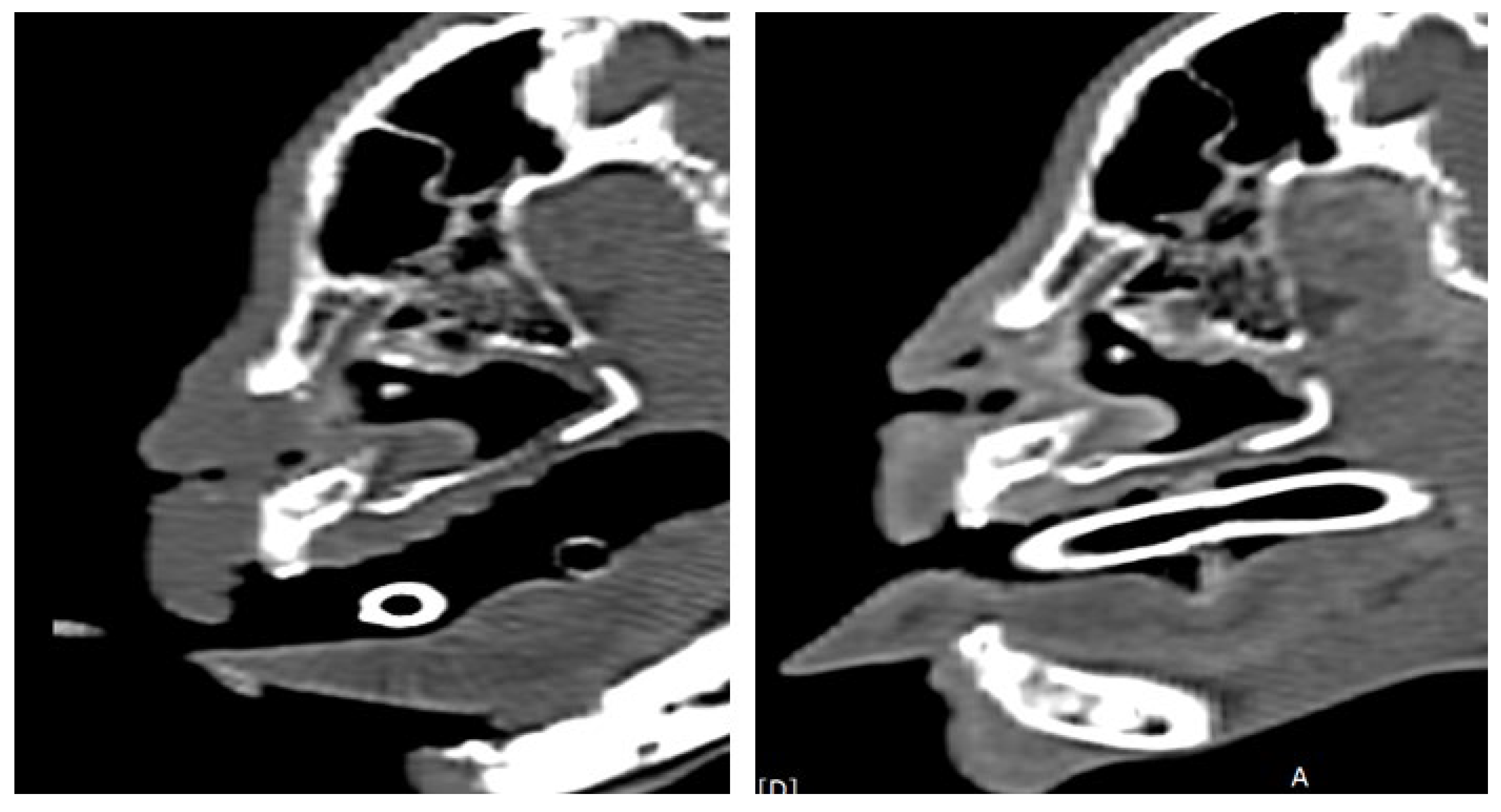
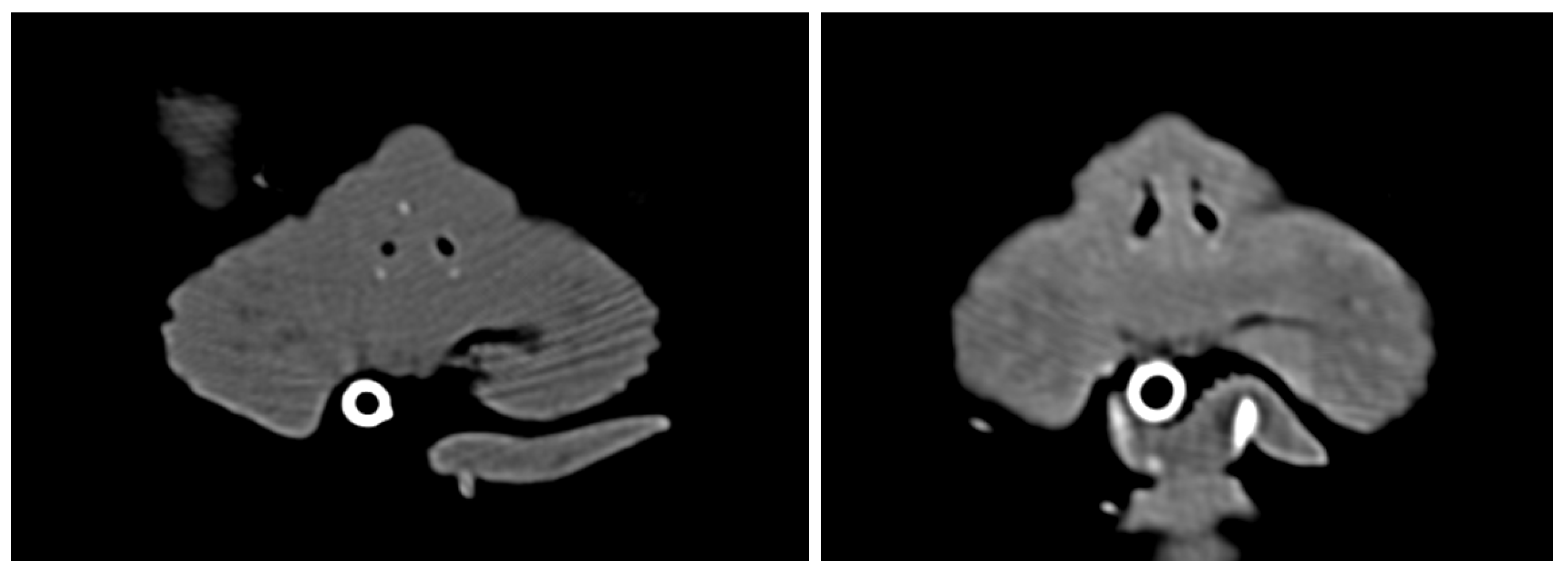
2.3. Preoperative Evaluation
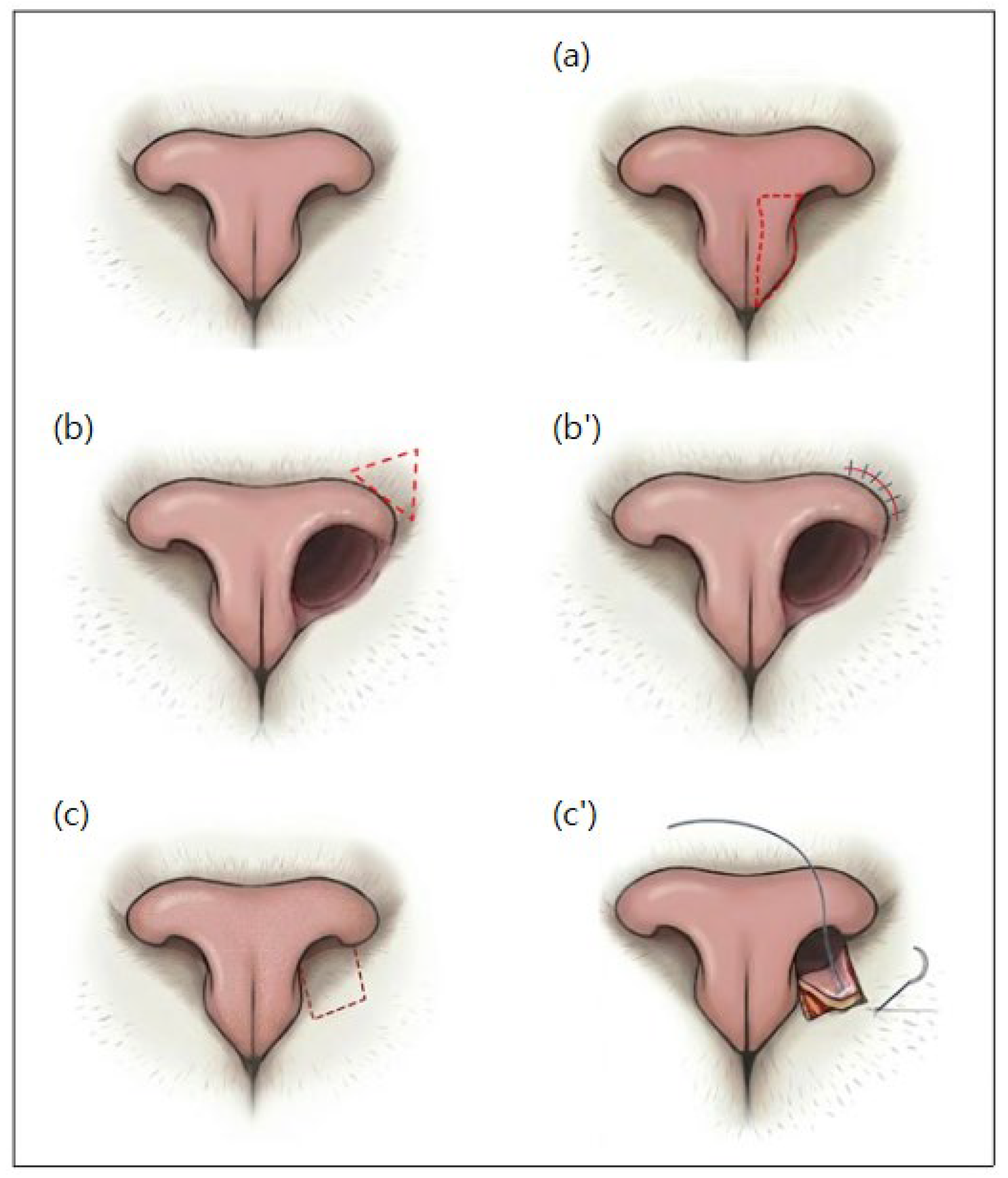
2.4. Surgical Technique
Modified Trader’s Technique
Bilateral Wedge Resection
Single Pedicle Advancement Flap
Placement of a Steroid-Eluting Bioabsorbable Nasal Stent (PROPEL)
2.5. Postoperative Care and Follow-Up
3. Results
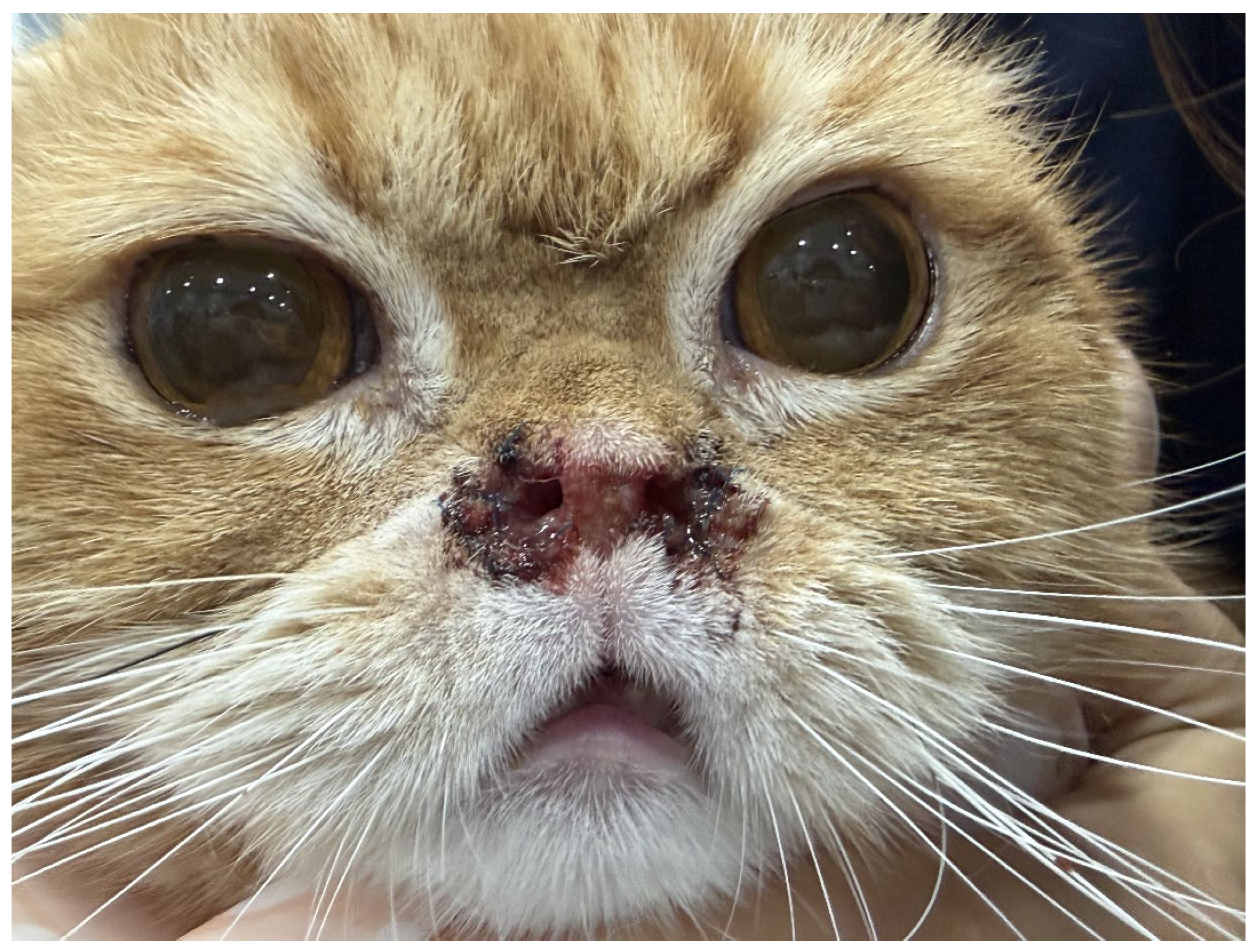
3.1. Medical History and Preoperative Progression
3.2. Intraoperative Findings and Immediate Postoperative Course
3.3. Postoperative Follow-Up and Prognosis
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
References
- Schlueter, C.; Budras, K.D.; Ludewig, E.; Mayrhofer, E.; Baezner, C.; Peppler, C.; Oechtering, G. Brachycephalic feline noses: CT and anatomical study of the relationship between head conformation and the nasolacrimal drainage system. J. Feline Med. Surg. 2009, 11, 891–900. [Google Scholar] [CrossRef] [PubMed]
- Mitze, S.; Barrs, V.R.; Beatty, J.A.; Hobi, S.; Bęczkowski, P.M. Brachycephalic obstructive airway syndrome: much more than a surgical problem. Vet. Q. 2022, 42, 213–223. [Google Scholar] [CrossRef] [PubMed]
- Musulin, A.; Nađ, M. A Comprehensive Review of Brachycephalic Obstructive Airway Disease: Pathophysiology, Diagnosis, Management, and Future Perspectives. Vet. Stanica 2024, 55, 731–743. [Google Scholar] [CrossRef]
- Corgozinho, K.B.; de Souza, H.J.M.; Ferreira, A.M.R.; da Silva, A.L.G. Recurrent pulmonary edema secondary to elongated soft palate in a cat. J. Feline Med. Surg. 2012, 14, 417–419. [Google Scholar] [CrossRef] [PubMed]
- Berns, C.N.; Ter Haar, G.; Brockman, D.J. Single pedicle advancement flap for treatment of feline stenotic nares: technique and results in five cases. J. Feline Med. Surg. 2020, 22, 1238–1242. [Google Scholar] [CrossRef] [PubMed]
- Galletti, C.; Portelli, D.; Ferrisi, M.G.; Gambino, F.; Iuculano, L.; Sanfilippo, B.; Ielo, G.; Freni, L.; Maniaci, A.; Ciodaro, F.; Freni, F.; Galletti, F.; Galletti, B. Endoscopic Endonasal Repair of Bilateral Choanal Atresia in a Neonate with Placement of a Steroid-Eluting Bioabsorbable Nasal Stent (PROPEL) Using a Customised Alternative Insertion Technique: A Case Report and Literature Review. J. Clin. Med. 2025, 14, 8282. [Google Scholar] [CrossRef] [PubMed]
- Farnworth, M.J.; Chen, R.; Packer, R.M.; Caney, S.M.; Gunn-Moore, D.A. Flat feline faces: is brachycephaly associated with respiratory abnormalities in the domestic cat (Felis catus)? PLoS ONE 2016, 11, e0161777. [Google Scholar] [CrossRef] [PubMed]
- Sieslack, J.; Farke, D.; Failing, K.; Kramer, M.; Schmidt, M.J. Correlation of brachycephaly grade with level of exophthalmos, reduced airway passages and degree of dental malalignment in Persian cats. PLoS ONE 2021, 16, e0254420. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y.-C.; Chang, Y.-S. A novel surgical approach for feline stenotic nares: Bilateral wedge resection of the dorsal lateral nasal cartilage in seven cases. Vet. Med. Sci. 2023, 9, 2430–2437. [Google Scholar] [CrossRef] [PubMed]
- Trader, R.L. Nose operation. J. Am. Vet. Med. Assoc. 1949, 114, 210–211. [Google Scholar]
- Huck, J.L.; Stanley, B.J.; Hauptman, J.G. Technique and outcome of nares amputation (Trader’s technique) in immature shih tzus. J. Am. Anim. Hosp. Assoc. 2008, 44, 82–85. [Google Scholar] [CrossRef] [PubMed]
- Alsubaie, H.M.; Almosa, W.H.; Al-Qahtani, A.S.; Margalani, O. Choanal atresia repair with stents and flaps: a systematic review article. Allergy Rhinol. 2021, 12, 21526567211058052. [Google Scholar] [CrossRef] [PubMed]
- De Lorenzi, D.; Bertoncello, D.; Comastri, S.; Bottero, E. Treatment of acquired nasopharyngeal stenosis using a removable silicone stent. J. Feline Med. Surg. 2015, 17, 117–124. [Google Scholar] [CrossRef] [PubMed]
- Wang, P.-P.; Tang, L.-X.; Ge, W.; Zhang, J.-G.; Sun, W.-Y.; Wang, T.; Wen, J.-J.; Ouyang, Z.; Ni, X. Combination of the endoscopic septonasal flap technique and bioabsorbable steroid-eluting stents for repair of congenital choanal atresia in neonates and infants: a retrospective study. J. Otolaryngol. Head Neck Surg. 2021, 50, 51. [Google Scholar] [CrossRef] [PubMed]


Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



