Submitted:
18 March 2026
Posted:
19 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Sample
2.2. Data Definitions
2.3. Statistical Analysis
2.4. Ethical Approval
3. Results
4. Discussion
Study Strengths and Limitations
5. Conclusions
Acknowledgments
Author Contributions
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Funding Statement
References
- Amini, M; Zayeri, F; Salehi, M. Trend analysis of cardiovascular disease mortality, incidence, and mortality-to-incidence ratio: results from global burden of disease study 2017. BMC Public Health 2021, 21(1), 401. [Google Scholar] [CrossRef]
- Zuin, M; Rigatelli, G; Temporelli, P; Di Fusco, SA; Colivicchi, F; Pasquetto, G; Bilato, C. Trends in acute myocardial infarction mortality in the European Union, 2012-2020. Eur J Prev Cardiol. 2023, 30(16), 1758–1771. [Google Scholar] [CrossRef] [PubMed]
- Kallström, A; Holopainen, I; Kambur, O; Perola, M; Salomaa, V; Havulinna, AS; Ramste, M; Sinisalo, J. Divergent trends in the incidence and mortality of acute myocardial ischaemic syndrome, especially in women. Evidence from Finland in 1996-2021. Ann Med. 2024, 56(1), 2424455. [Google Scholar] [CrossRef] [PubMed]
- Vázquez-Oliva, G; Zamora, A; Ramos, R; Marti, R; Subirana, I; Grau, M; Dégano, IR; Marrugat, J; Elosua, R. Acute Myocardial Infarction Population Incidence and Mortality Rates, and 28-day Case-fatality in Older Adults. The REGICOR Study. In Rev Esp Cardiol (Engl Ed); English, Spanish, 2018; Volume 71, 9, pp. 718–725. [Google Scholar] [CrossRef]
- Dégano, IR; Salomaa, V; Veronesi, G; Ferriéres, J; Kirchberger, I; Laks, T; Havulinna, AS; Ruidavets, JB; Ferrario, MM; Meisinger, C. Acute Myocardial Infarction Trends in Europe (AMITIE) Study Investigators. Twenty-five-year trends in myocardial infarction attack and mortality rates, and case-fatality, in six European populations. Heart 2015, 101(17), 1413–21. [Google Scholar] [CrossRef]
- DeFilippis, EM; Collins, BL; Singh, A; Biery, DW; Fatima, A; Qamar, A; Berman, AN; Gupta, A; Cawley, M; Wood, MJ; et al. Women who experience a myocardial infarction at a young age have worse outcomes compared with men: the Mass General Brigham YOUNG-MI registry. Eur Heart J. 2020, 41(42), 4127–4137. [Google Scholar] [CrossRef] [PubMed]
- Berg, J; Björck, L; Nielsen, S; Lappas, G; Rosengren, A. Sex differences in survival after myocardial infarction in Sweden, 1987-2010. Heart 2017, 103(20), 1625–1630. [Google Scholar] [CrossRef]
- Izadnegahdar, M; Singer, J; Lee, MK; Gao, M; Thompson, CR; Kopec, J; Humphries, KH. Do younger women fare worse? Sex differences in acute myocardial infarction hospitalization and early mortality rates over ten years. J Womens Health (Larchmt) 2014, 23(1), 10–7. [Google Scholar] [CrossRef]
- Krämer, C; Meisinger, C; Kirchberger, I; Heier, M; Kuch, B; Thilo, C; Linseisen, J; Amann, U. Epidemiological trends in mortality, event rates and case fatality of acute myocardial infarction from 2004 to 2015: results from the KORA MI registry. Ann Med. 2021, 53(1), 2142–2152. [Google Scholar] [CrossRef]
- Sulo, G; Igland, J; Vollset, SE; Ebbing, M; Egeland, GM; Ariansen, I; Tell, GS. Trends in incident acute myocardial infarction in Norway: an updated analysis to 2014 using national data from the CVDNOR project. Eur J Prev Cardiol. 2018, 25(10), 1031–1039. [Google Scholar] [CrossRef]
- Amann, U; Kirchberger, I; Heier, M; Golüke, H; von Scheidt, W; Kuch, B; Peters, A; Meisinger, C. Long-term survival in patients with different combinations of evidence-based medications after incident acute myocardial infarction: results from the MONICA/KORA Myocardial Infarction Registry. Clin Res Cardiol. 2014, 103(8), 655–64. [Google Scholar] [CrossRef]
- Dixon, DL; Sharma, G; Sandesara, PB; Yang, E; Braun, LT; Mensah, GA; Sperling, LS; Deedwania, PC; Virani, SS. Therapeutic Inertia in Cardiovascular Disease Prevention: Time to Move the Bar. J Am Coll Cardiol. 2019, 74(13), 1728–1731. [Google Scholar] [CrossRef]
- Toso, A; Leoncini, M; Maioli, M; Villani, S; Bellandi, F; PRATO-ACS. Residual risk after acute coronary syndrome: the PRATO-ACS registry. Eur Heart J. 2021, 42 (Supplement_1), 2466. [Google Scholar] [CrossRef]
- Del Buono, MG; Montone, RA; Iannaccone, G; Rinaldi, R; La Vecchia, G; Camilli, M; Gurgoglione, FL; Russo, M; Lombardi, M; D’amario, D; Niccoli, G. Redefining residual inflammatory risk after acute coronary syndrome. Future Cardiol. 2022, 18(2), 115–123. [Google Scholar] [CrossRef] [PubMed]
- Lou, B; Liu, H; Luo, Y; Jiang, GT; Wu, H; Wang, C; Wu, Y; Zhou, B; Yuan, Z; She, J; Liu, J. In-hospital initiation of PCSK9 inhibitor and short-term lipid control in patients with acute myocardial infarction. Lipids Health Dis. 2022, 21(1), 105. [Google Scholar] [CrossRef] [PubMed]
- Chen, Y; Qiu, J; Ai, T; Wu, Y. The Role of Oral β-Blockers in Patients With Acute Myocardial Infarction with Preserved or Mildly Reduced Left Ventricular Systolic Function: A Systematic Review and Meta-Analysis. Clin Ther. 2025, 47(9), 788–797. [Google Scholar] [CrossRef]
- Weininger, D; Cordova, JP; Wilson, E; Eslava, DJ; Alviar, CL; Korniyenko, A; Bavishi, CP; Hong, MK; Chorzempa, A; Fox, J; Tamis-Holland, JE. Delays to Hospital Presentation in Women and Men with ST-Segment Elevation Myocardial Infarction: A Multi-Center Analysis of Patients Hospitalized in New York City. Ther Clin Risk Manag 2022, 18, 1–9. [Google Scholar] [CrossRef]
- Cangiano, L; Bonomi, A; Cosentino, N; Leoni, O; Trombara, F; Myasoedova, VA; Poggio, P; Trabattoni, D; Agostoni, P; Marenzi, G. Exploring sex differences in mortality among acute myocardial infarction. Open Heart 2025, 12(2), e003517. [Google Scholar] [CrossRef]
- World Health Organization MONICA Project. MONICA Manual; World Health Organization MONICA Project: Geneva, Switzerland, 1990. [Google Scholar]
- Lithuanian Hygiene Institute. 2026. Available online: https://www.hi.lt/sveikatos-informacijos-centras-mirties-atveju-ir-ju-pr.. (accessed on 15 January 2026).
- ICD-10 Codes. Available online: https://icd.who.int/browse10/2019/en#/IX (accessed on 8 January 2026).
- Ahmad, OB; Boschi-Pinto, C; Lopez, AD; Murray, CJL; Lozano, R; Inoue, M. Age Standardization of Rates: A New WHO Standard; (GPE Discussion Paper Series: No. 31. EIP/GPE/EBD); WHO: Geneva, Switzerland, 2001. [Google Scholar]
- Joinpoint Trend Analysis Software. Available online: https://surveillance.cancer.gov/joinpoint/ (accessed on 20 January 2026).
- Kim, HJ; Fay, MP; Feuer, EJ; Midthune, DN. Permutation tests for joinpoint regression with applications to cancer rates. Stat. Med. 2000, 19, 335–351. [Google Scholar] [CrossRef]
- Smolina, K; Wright, FL; Rayner, M; Goldacre, MJ. Determinants of the decline in mortality from acute myocardial infarction in England between 2002 and 2010: linked national database study. BMJ 2012, 344, d8059. [Google Scholar] [CrossRef]
- Meirhaeghe, A; Montaye, M; Biasch, K; Huo Yung Kai, S; Moitry, M; Amouyel, P; Ferrières, J; Dallongeville, J. Coronary heart disease incidence still decreased between 2006 and 2014 in France, except in young age groups: results from the French MONICA registries. Eur J Prev Cardiol. 2020, 27(11), 1178–1186. [Google Scholar] [CrossRef] [PubMed]
- De Luca, L; Cicala, SD; D’Errigo, P; Cerza, F; Mureddu, GF; Rosato, S; Badoni, G; Seccareccia, F; Baglio, G. Impact of age, gender and heart failure on mortality trends after acute myocardial infarction in Italy. Int J Cardiol. 2022, 348, 147–151. [Google Scholar] [CrossRef]
- Asaria, P; Bennett, JE; Elliott, P; Rashid, T; Iyathooray Daby, H; Douglass, M; Francis, DP; Fecht, D; Ezzati, M. Contributions of event rates, pre-hospital deaths, and deaths following hospitalisation to variations in myocardial infarction mortality in 326 districts in England: a spatial analysis of linked hospitalisation and mortality data. Lancet Public Health 2022, 7(10), e813–e824. [Google Scholar] [CrossRef]
- Xu, X; Bao, H; Strait, K; Spertus, JA; Lichtman, JH; D’Onofrio, G; Spatz, E; Bucholz, EM; Geda, M; Lorenze, NP; Bueno, H; Beltrame, JF; Krumholz, HM. Sex differences in perceived stress and early recovery in young and middle-aged patients with acute myocardial infarction. Circulation 2015, 131(7), 614–23. [Google Scholar] [CrossRef]
- Wilmot, KA; O’Flaherty, M; Capewell, S; Ford, ES; Vaccarino, V. Coronary heart disease mortality declines in the United States from 1979 through 2011: evidence for stagnation in young adults, especially women. Circulation 2015, 132(11), 997–1002. [Google Scholar] [CrossRef]
- Camacho, X; Nedkoff, L; Wright, FL; Nghiem, N; Buajitti, E; Goldacre, R; Rosella, LC; Seminog, O; Tan, EJ; Hayes, A; et al. Relative contribution of trends in myocardial infarction event rates and case fatality to declines in mortality: an international comparative study of 1·95 million events in 80·4 million people in four countries. Lancet Public Health 2022, 7(3), e229–e239. [Google Scholar] [CrossRef]
- Antman, EM; Anbe, DT; Armstrong, PW; Bates, ER; Green, LA; Hand, M; Hochman, JS; Krumholz, HM; Kushner, FG; Lamas, GA. American College of Cardiology; American Heart Association Task Force on Practice Guidelines; Canadian Cardiovascular Society. ACC/AHA guidelines for the management of patients with ST-elevation myocardial infarction: a report of the American College of Cardiology/American Heart Association Task Force on Practice Guidelines (Committee to Revise the 1999 Guidelines for the Management of Patients with Acute Myocardial Infarction). Circulation 2004, 110(9), e82-292. [Google Scholar] [PubMed]
- Amann, U; Kirchberger, I; Heier, M; von Scheidt, W; Kuch, B; Peters, A; Meisinger, C. Acute myocardial infarction in the elderly: treatment strategies and 28-day-case fatality from the MONICA/KORA myocardial infarction registry. Catheter Cardiovasc Interv. 2016, 87(4), 680–688. [Google Scholar] [CrossRef] [PubMed]
- Nef, HM; Elsässer, A; Möllmann, H; Abdel-Hadi, M; Bauer, T; Brück, M; Eggebrecht, H; Ehrlich, JR; Ferrari, MW; Fichtlscherer, S. CoVCAD–Study Group. Impact of the COVID-19 pandemic on cardiovascular mortality and catherization activity during the lockdown in central Germany: an observational study. Clin Res Cardiol. 2021, 110(2), 292–301. [Google Scholar] [CrossRef]
- Cipriani, A; Capone, F; Donato, F; Molinari, L; Ceccato, D; Saller, A; Previato, L; Pesavento, R; Sarais, C; Fioretto, P; et al. Cardiac injury and mortality in patients with Coronavirus disease 2019 (COVID-19): insights from a mediation analysis. Intern Emerg Med. 2021, 16(2), 419–427. [Google Scholar] [CrossRef] [PubMed]
- Kiss, P; Carcel, C; Hockham, C; Peters, SAE. The impact of the COVID-19 pandemic on the care and management of patients with acute cardiovascular disease: a systematic review. Eur Heart J Qual Care Clin Outcomes 2021, 7(1), 18–27. [Google Scholar] [CrossRef]
- Čelutkienė, J; Čerlinskaitė-Bajorė, K; Bajoras, V; Višinskienė, R; Lizaitis, M; Budrys, P; Buivydas, R; Gurevičius, R; Šerpytis, P; Davidavičius, G. Collateral effect of the COVID-19 pandemic on cardiology service provision and cardiovascular mortality in a population-based study: COVID-COR-LT. Clin Res Cardiol. 2022, 111(10), 1130–1146. [Google Scholar] [CrossRef] [PubMed]
- Zandecki, L; Sadowski, M; Janion, M; Gierlotka, M; Gasior, M; Polonski, L. Trends in sex differences in clinical characteristics, treatment strategies, and mortality in patients with ST-elevation myocardial infarction in Poland from 2005 to 2011. Coron Artery Dis. 2017, 28(5), 417–425. [Google Scholar] [CrossRef]
- Steg, PG; Dabbous, OH; Feldman, LJ; Cohen-Solal, A; Aumont, MC; López-Sendón, J; Budaj, A; Goldberg, RJ; Klein, W; Anderson, FA, Jr. Global Registry of Acute Coronary Events Investigators. Determinants and prognostic impact of heart failure complicating acute coronary syndromes: observations from the Global Registry of Acute Coronary Events (GRACE). Circulation 2004, 109(4), 494–9. [Google Scholar] [CrossRef] [PubMed]
- Desta, L; Jernberg, T; Löfman, I; Hofman-Bang, C; Hagerman, I; Spaak, J; Persson, H. Incidence, temporal trends, and prognostic impact of heart failure complicating acute myocardial infarction. The SWEDEHEART Registry (Swedish Web-System for Enhancement and Development of Evidence-Based Care in Heart Disease Evaluated According to Recommended Therapies): a study of 199,851 patients admitted with index acute myocardial infarctions, 1996 to 2008. JACC Heart Fail. 2015, 3(3), 234–42. [Google Scholar] [CrossRef]
- Gerber, Y; Weston, SA; Jiang, R; Roger, VL. The changing epidemiology of myocardial infarction in Olmsted County, Minnesota, 1995-2012. Am J Med. 2015, 128(2), 144–51. [Google Scholar] [CrossRef]
- Wellings, J; Kostis, JB; Sargsyan, D; Cabrera, J; Kostis, WJ. Myocardial Infarction Data Acquisition System (MIDAS 31) Study Group. Risk Factors and Trends in Incidence of Heart Failure Following Acute Myocardial Infarction. Am J Cardiol. 2018, 122(1), 1–5. [Google Scholar] [CrossRef]
- Greco, C; Rosato, S; D’Errigo, P; Mureddu, GF; Lacorte, E; Seccareccia, F. Trends in mortality and heart failure after acute myocardial infarction in Italy from 2001 to 2011. Int J Cardiol. 2015, 184, 115–121. [Google Scholar] [CrossRef]
- Kotseva, K; De Bacquer, D; Jennings, C; Gyberg, V; De Backer, G; Rydén, L; Amouyel, P; Bruthans, J; Cifkova, R; Deckers, JW. EUROASPIRE Investigators. Time Trends in Lifestyle, Risk Factor Control, and Use of Evidence-Based Medications in Patients With Coronary Heart Disease in Europe: Results From 3 EUROASPIRE Surveys, 1999-2013. Glob Heart 2017, 12(4), 315–322.e3. [Google Scholar] [CrossRef]
- Barauskas, M; Unikas, R; Žiubrytė, G. Outcomes of in-hospital treatment of cardiac patients who survived cardiac arrest and experienced coronary angiography. Arch Med Sci Atheroscler Dis. 2018, 3, e1–e7. [Google Scholar] [CrossRef]
- Cosentino, N; Bonomi, A; Campodonico, J; Veglia, F; De Ferrari, GM; Genovese, S; Marenzi, G. Can the in-hospital mortality gap between STEMI patients with and without diabetes mellitus be reduced? The cardio-renal hypothesis. Nutr Metab Cardiovasc Dis. 2021, 31(5), 1516–1520. [Google Scholar] [CrossRef] [PubMed]
- Cosentino, N; Resta, ML; Somaschini, A; Campodonico, J; Lucci, C; Moltrasio, M; Bonomi, A; Cornara, S; Camporotondo, R; Demarchi, A; et al. Acute kidney injury and in-hospital mortality in patients with ST-elevation myocardial infarction of different age groups. Int J Cardiol. 2021, 344, 8–12. [Google Scholar] [CrossRef]
- Weizman, O; Marijon, E; Narayanan, K; Boveda, S; Defaye, P; Martins, R; Deharo, JC; Laurent, G; Klug, D; Sadoul, N. FAST-MI Program Investigators. Incidence, Characteristics, and Outcomes of Ventricular Fibrillation Complicating Acute Myocardial Infarction in Women Admitted Alive in the Hospital. J Am Heart Assoc. 2022, 11(17), e025959. [Google Scholar] [CrossRef]
- Crea, F; Battipaglia, I; Andreotti, F. Sex differences in mechanisms, presentation and management of ischaemic heart disease. Atherosclerosis 2015, 241(1), 157–68. [Google Scholar] [CrossRef] [PubMed]
- Aggarwal, NR; Patel, HN; Mehta, LS; Sanghani, RM; Lundberg, GP; Lewis, SJ; Mendelson, MA; Wood, MJ; Volgman, AS; Mieres, JH. Sex Differences in Ischemic Heart Disease: Advances, Obstacles, and Next Steps. Circ Cardiovasc Qual Outcomes 2018, 11(2), e004437. [Google Scholar] [CrossRef] [PubMed]
- Bugiardini, R; Manfrini, O; Cenko, E. Female sex as a biological variable: A review on younger patients with acute coronary syndrome. Trends Cardiovasc Med. 2019, 29(1), 50–55. [Google Scholar] [CrossRef]
- Dekleva, M; Djordjevic, A; Zivkovic, S; Lazic, JS. Specificities of Myocardial Infarction and Heart Failure in Women. J Clin Med. 2024, 13(23), 7319. [Google Scholar] [CrossRef]
- European Health Information Gateway. Available online: https://gateway.euro.who.int/en/ (accessed on 29 January 2026).
- Banach, M; Mastalerz-Migas, A; Wita, K; Myśliwiec, M. Poland takes a lead in effective lipid disorders management healthcare programmes in Europe. Am J Prev Cardiol. 2025, 24, 101346. [Google Scholar] [CrossRef] [PubMed]
- Bruthans, J; Mayer, O; Jarkovsky, J; Zvolsky, M; Bruthans, J. Long-term trends in the incidence, treatment, hospital fatality and subsequent mortality from acute myocardial infarction in the Czech Republic. Biomed Pap Med Fac Univ Palacky Olomouc Czech Repub. 2021, 165(3), 283–290. [Google Scholar] [CrossRef]
- Nedkoff, L; Briffa, TG; Knuiman, M; Hung, J; Norman, PE; Hankey, GJ; Thompson, PL; Geelhoed, E; Sanfilippo, FM; Hickling, S; et al. Temporal trends in the incidence and recurrence of hospitalised atherothrombotic disease in an Australian population, 2000-07: data linkage study. Heart 2012, 98(19), 1449–56. [Google Scholar] [CrossRef]
- Lloyd-Jones, DM; Martin, DO; Larson, MG; Levy, D. Accuracy of death certificates for coding coronary heart disease as the cause of death. Ann Intern Med. 1998, 129(12), 1020–6. [Google Scholar] [CrossRef]
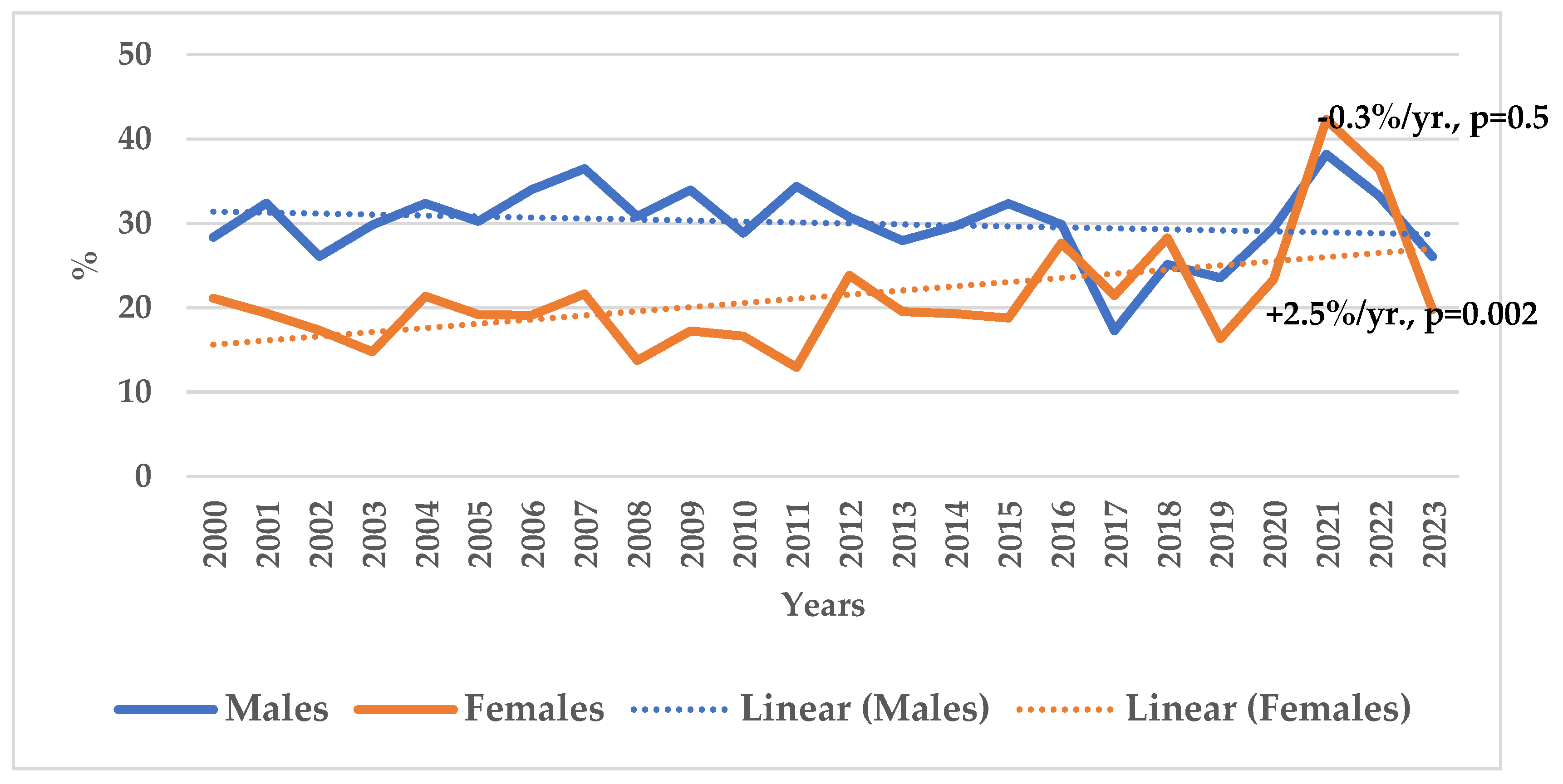
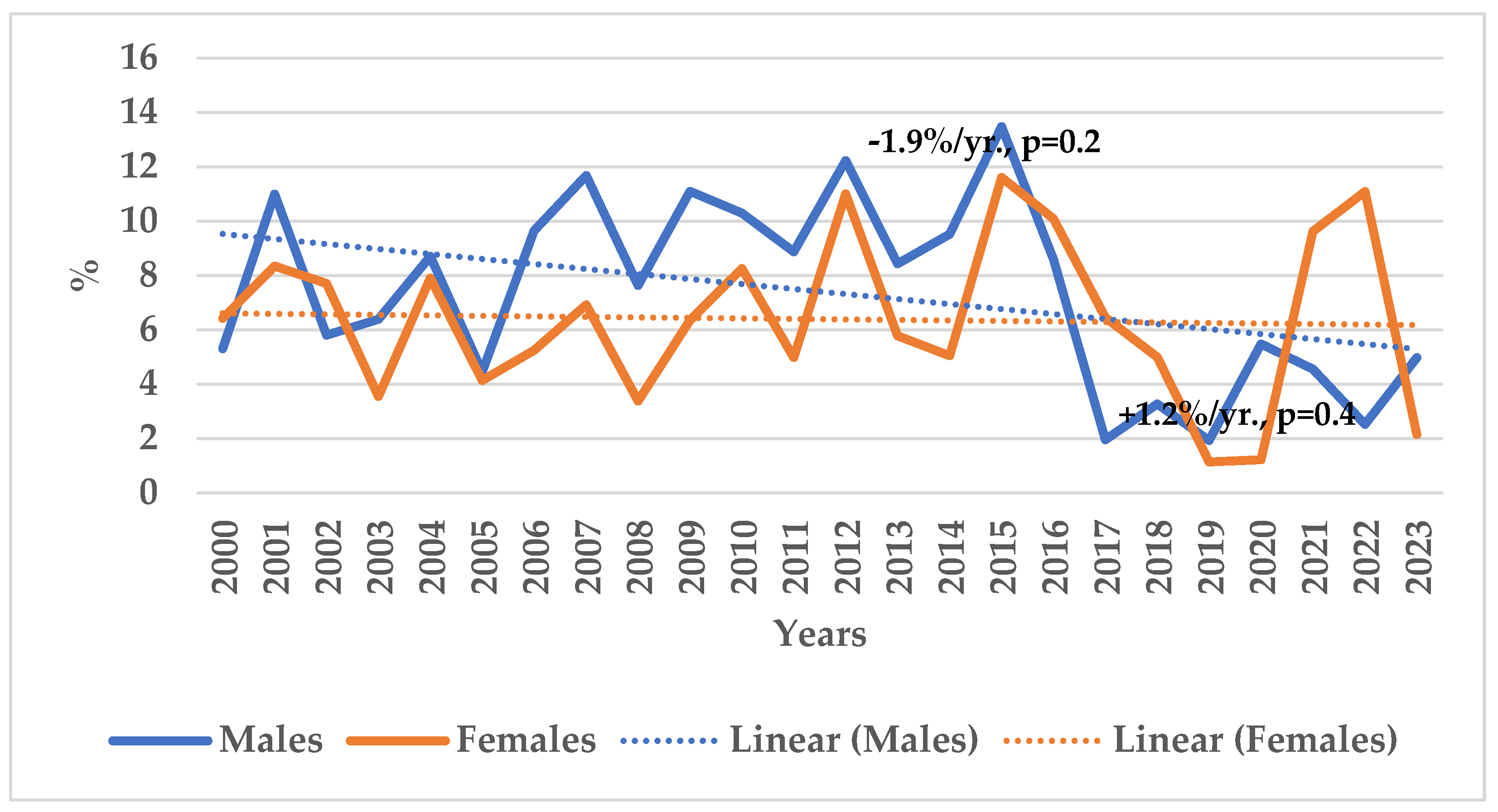
| Years | Males | Females | |||
|---|---|---|---|---|---|
| 25-54 | 55-64 | 25-54 | 55-64 | ||
| 2000 | 23.43 | 32.75 | 13.17 | 25.27 | |
| 2001 | 22.17 | 39.25 | 24.23 | 16.67 | |
| 2002 | 18.30 | 32.56 | 16.22 | 17.89 | |
| 2003 | 24.89 | 33.99 | 11.26 | 16.48 | |
| 2004 | 30.39 | 33.74 | 9.30 | 25.69 | |
| 2005 | 26.57 | 32.82 | 8.75 | 23.15 | |
| 2006 | 29.36 | 37.16 | 21.23 | 18.00 | |
| 2007 | 36.76 | 36.24 | 22.63 | 21.28 | |
| 2008 | 27.99 | 32.87 | 18.05 | 11.58 | |
| 2009 | 28.31 | 37.29 | 16.56 | 17.65 | |
| 2010 | 22.02 | 33.62 | 7.63 | 19.57 | |
| 2011 | 24.56 | 41.50 | 15.53 | 11.49 | |
| 2012 | 21.85 | 36.04 | 15.23 | 27.06 | |
| 2013 | 18.99 | 34.78 | 10.40 | 24.62 | |
| 2014 | 17.34 | 37.89 | 14.11 | 21.54 | |
| 2015 | 23.35 | 38.25 | 11.23 | 22.22 | |
| 2016 | 27.32 | 31.58 | 15.59 | 32.81 | |
| 2017 | 12.64 | 20.13 | 21.86 | 21.25 | |
| 2018 | 23.44 | 26.29 | 50.00 | 18.46 | |
| 2019 | 12.62 | 29.86 | 0.01 | 22.97 | |
| 2020 | 25.16 | 32.27 | 17.62 | 26.47 | |
| 2021 | 37.05 | 38.76 | 27.15 | 51.22 | |
| 2022 | 18.72 | 40.12 | 24.69 | 41.86 | |
| 2023 | 11.99 | 32.86 | 10.08 | 25.00 | |
| Average | 23.55 | 34.28 | 16.77 | 23.34 | |
| AAPC1 and | -0.9%/yr., | -0.2%/yr., | +2.2%/yr., | +3.0%/yr., | |
| p-value | 0.3 | 0.6 | 0.2 | 0.002 | |
| Years | Males | Females | ||
|---|---|---|---|---|
| 25-54 | 55-64 | 25-54 | 55-64 | |
| 2000 | 2.74 | 7.78 | 5.72 | 6.85 |
| 2001 | 5.81 | 15.03 | 10.68 | 7.14 |
| 2002 | 0.01 | 11.04 | 8.82 | 7.14 |
| 2003 | 3.26 | 9.24 | 3.07 | 3.80 |
| 2004 | 6.08 | 10.56 | 0.01 | 10.99 |
| 2005 | 3.86 | 4.92 | 3.10 | 4.60 |
| 2006 | 7.32 | 11.35 | 8.51 | 3.53 |
| 2007 | 11.25 | 12.03 | 8.62 | 6.33 |
| 2008 | 7.62 | 7.64 | 5.56 | 2.33 |
| 2009 | 4.75 | 14.94 | 5.85 | 6.67 |
| 2010 | 6.81 | 12.99 | 3.97 | 9.76 |
| 2011 | 5.24 | 12.03 | 2.79 | 6.10 |
| 2012 | 5.64 | 16.47 | 0.01 | 15.07 |
| 2013 | 6.21 | 10.45 | 0.01 | 9.26 |
| 2014 | 3.17 | 14.49 | 0.01 | 7.27 |
| 2015 | 4.53 | 19.86 | 5.95 | 14.29 |
| 2016 | 4.67 | 11.18 | 5.80 | 12.24 |
| 2017 | 2.42 | 1.65 | 4.58 | 7.35 |
| 2018 | 3.53 | 3.09 | 9.64 | 3.64 |
| 2019 | 0.01 | 3.27 | 0.01 | 1.72 |
| 2020 | 6.02 | 5.10 | 0.01 | 1.96 |
| 2021 | 4.91 | 4.39 | 0.01 | 16.67 |
| 2022 | 2.04 | 2.83 | 0.01 | 16.67 |
| 2023 | 4.34 | 5.37 | 5.31 | 0.01 |
| Average | 4.68 | 9.49 | 4.09 | 7.56 |
| AAPC1 and | -1.7%/yr. | -2.0%/yr. | -6.7%/yr. | +2.7%/yr. |
| p-value | 0.6 | 0.2 | 0.2 | 0.2 |
| Age groups | Sex | Joinpoints (Years) |
Period 1 |
APC with 95% CI | Period 2 |
APC with 95% CI |
|---|---|---|---|---|---|---|
| 25-64 | Males | 2006 | 2000-2006 | 2.2 (-5.4; 10.4) | 2006-2023 | -0.8 (-2.4; 0.7) |
| Females | 2010 | 2000-2010 | -1.5 (-7.6; 4.9) | 2010-2023 | 5.1 (1.3; 9.1)* | |
| 25-54 | Males | 2021 | 2000-2021 | -0.2 (-2.0; 1.6) | 2021-2023 | -28.2 (-69.8; 70.7) |
| Females | 2021 | 2000-2021 | 3.0 (-1.7; 8.0) | 2021-2023 | -26.4 (-90.1; 450.2) | |
| 55-64 | Males | 2019 | 2000-2019 | -0.7 (-1.9; 0.6) | 2019-2023 | 4.1 (-8.7; 18.7) |
| Females | 2009 | 2000-2009 | -2.5 (-10.7; 6.5) | 2009-2023 | 5.7 (1.7; 9.8)* |
| Age group | Sex | Joinpoints (Years) |
Period 1 |
APC with 95% CI | Period 2 |
APC with 95% CI |
|---|---|---|---|---|---|---|
| 25-64 | Males | 2015 | 2000-2015 | 2.2 (-1.5; 6.1) | 2015-2023 | -14.7 (-24.7; -3.5)* |
| Females | 2003 | 2000-2003 | -7.9 (-52.9; 80.1) | 2003-2023 | 1.8 (-2.0; 5.8) | |
| 25-54 | Males | 2007 | 2000-2007 | 19.1 (-18.1; 73.3) | 2007-2023 | -6.4 (-15.7; 4.0) |
| Females | 2021 | 2000-2021 | -8.0 (-18.4; 3.7) | 2021-2023 | 48.1 (-100.0; 467140.0) | |
| 55-64 | Males | 2015 | 2000-2015 | 2.5 (-1.1; 6.3) | 2015-2023 | -18.3 (-28.5; -6.8)* |
| Females | 2021 | 2000-2021 | 4.0 (-0.2; 8.5) | 2021-2023 | -40.6 (-96.8; 988.9) |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




