Submitted:
17 March 2026
Posted:
17 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Surgical Procedures and Postoperative Management
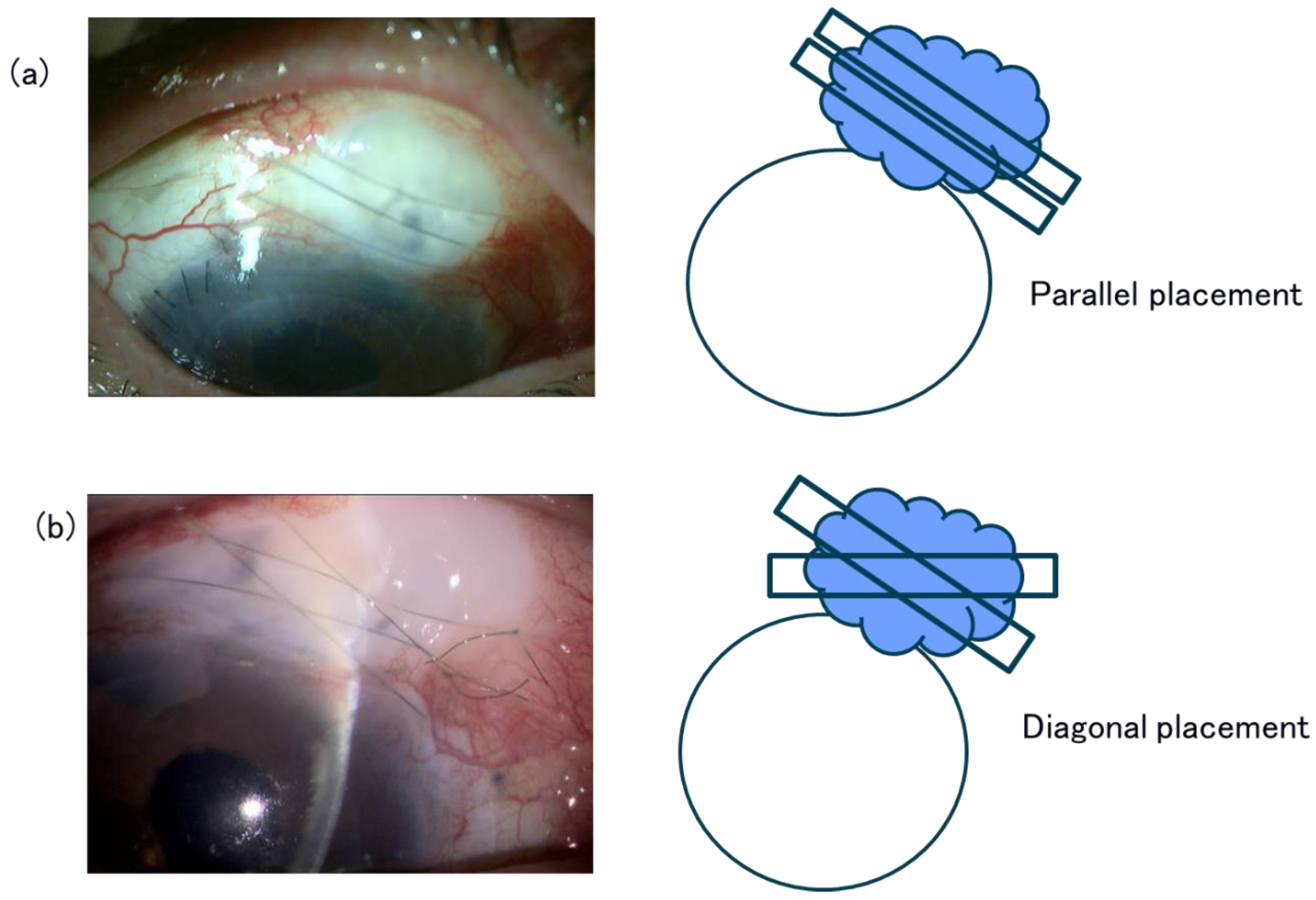
2.2. Data Collection and Analysis
3. Results
3.1. Postoperative IOP at the Acute (2 H After DSAEK) and Chronic Phases (a Few Weeks After DSAEK)
3.2. Air Ingress into the Filtration Bleb
3.3. Air Rebubbling
3.3. Intraoperative Complications
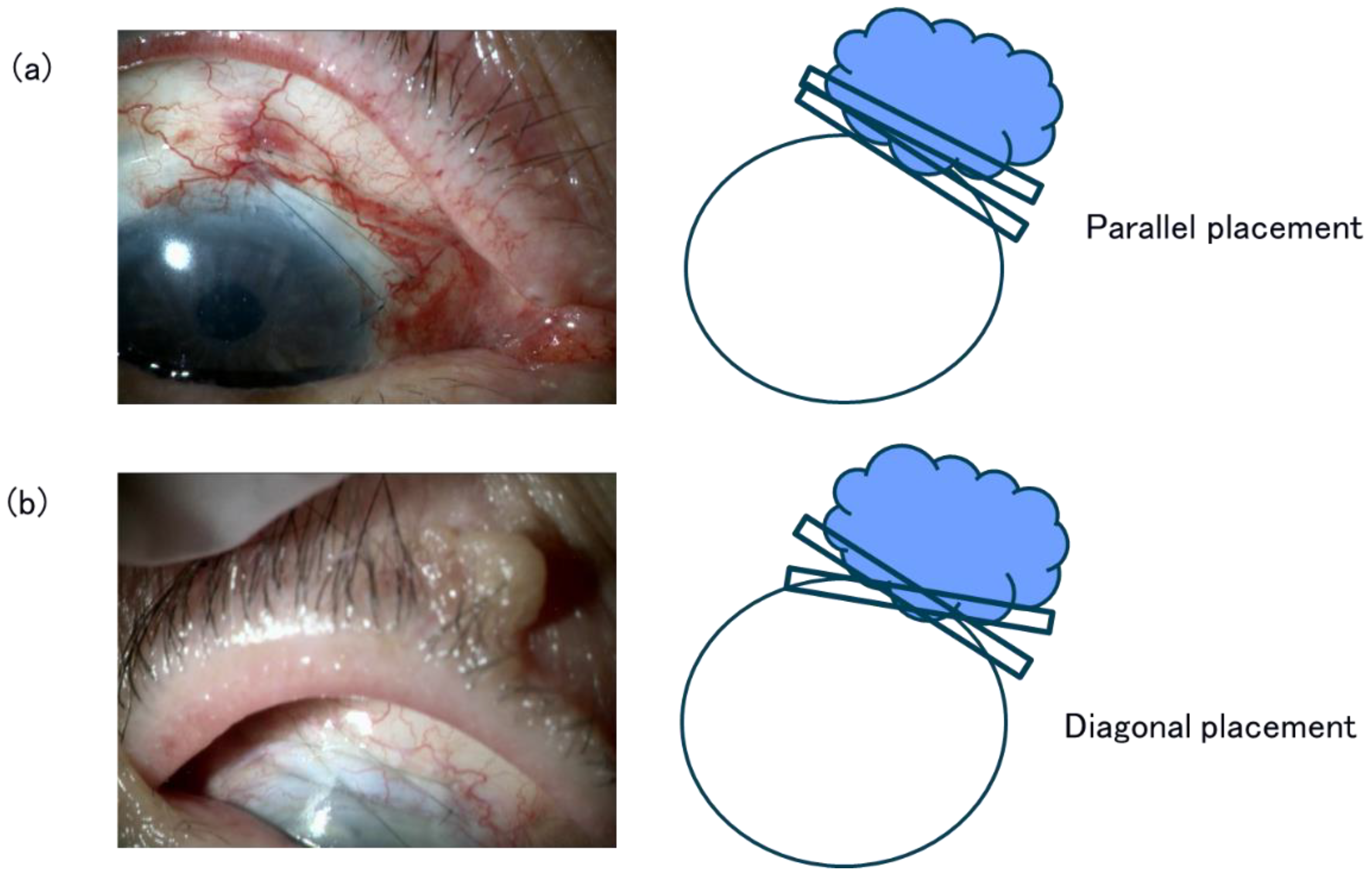
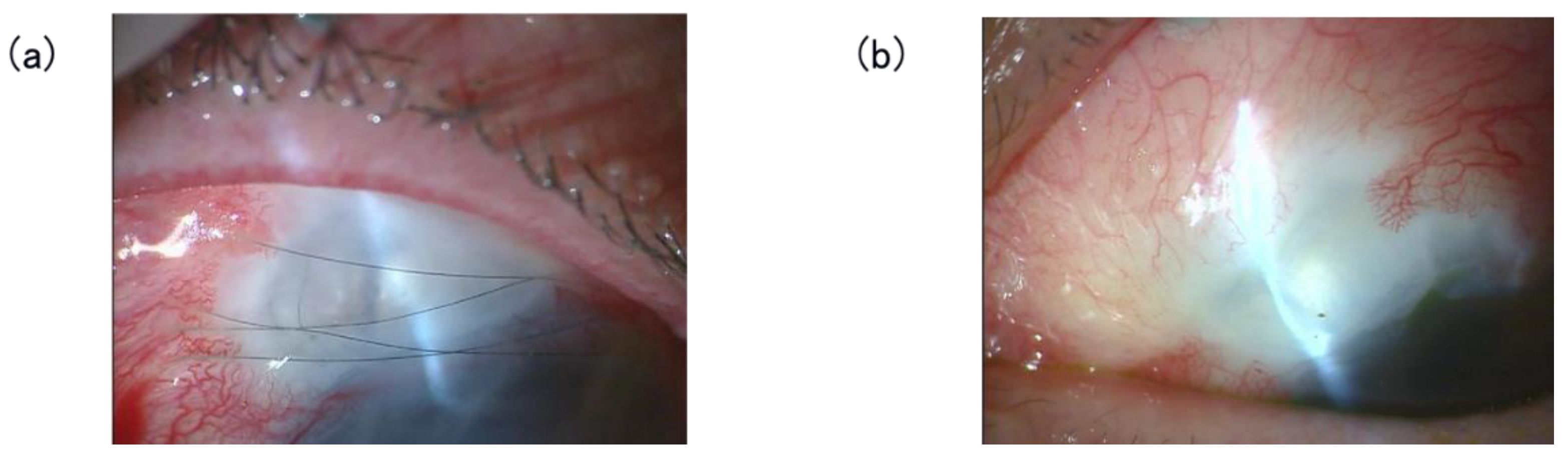
3.4. Removal of Compressive Sutures
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| DSAEK | Descemet stripping automated endothelial keratoplasty |
| BK | Bullous keratopathy |
| IOP | Intraocular pressure |
References
- Jung, Y.H.; Choi, H.J.; Kim, M.K.; Oh, Y.J. Etiology and outcome of penetrating keratoplasty in bullous keratopathy after cataract surgery versus glaucoma surgery. PLoS ONE 2023, 18, e0285455. [Google Scholar] [CrossRef] [PubMed]
- Vajaranant, T.S.; Price, M.O.; Price, F.W.; Gao, W.; Wilensky, J.T.; Edward, D.P. Visual acuity and intraocular pressure after Descemet’s stripping endothelial keratoplasty in eyes with and without preexisting glaucoma. Ophthalmology 2009, 116, 1644–1650. [Google Scholar] [CrossRef] [PubMed]
- Wiaux, C.; Baghdasaryan, E.; Lee, O.L.; Bourges, J.L.; Deng, S.X.; Yu, F.; Aldave, A.J. Outcomes after Descemet stripping endothelial keratoplasty in glaucoma patients with previous trabeculectomy and tube shunt implantation. Cornea 2011, 30, 1304–1311. [Google Scholar] [CrossRef] [PubMed]
- Aldave, A.J.; Chen, J.L.; Zaman, A.S.; Deng, S.X.; Yu, F. Outcomes after DSEK in 101 eyes with previous trabeculectomy and tube shunt implantation. Cornea 2014, 33, 223–229. [Google Scholar] [CrossRef] [PubMed]
- Anshu, A.; Price, M.O.; Price, F.W. Descemet’s stripping endothelial keratoplasty: Long-term graft survival and risk factors for failure in eyes with preexisting glaucoma. Ophthalmology 2012, 119, 1982–1987. [Google Scholar] [CrossRef] [PubMed]
- Kang, J.J.; Ritterband, D.C.; Lai, K.; Liebmann, J.M.; Seedor, J.A. Descemet’s stripping endothelial keratoplasty in eyes with previous glaucoma surgery. Cornea 2016, 35, 1520–1525. [Google Scholar] [CrossRef] [PubMed]
- Alshaker, S.; Mimouni, M.; Batawi, H.; Cohen, E.; Trinh, T.; Santaella, G.; Chan, C.C.; Slomovic, A.R.; Rootman, D.S.; Sorkin, N. Four-year survival comparison of endothelial keratoplasty techniques in patients with previous glaucoma surgery. Cornea 2021, 40, 1282–1289. [Google Scholar] [CrossRef] [PubMed]
- Takemori, H.; Higashide, T.; Kobayashi, A.; Yokogawa, H.; Sugiyama, K. Glaucoma-related risk factors for endothelial cell loss and graft failure after Descemet’s stripping automated endothelial keratoplasty. Cornea 2023, 42, e95–e102. [Google Scholar] [CrossRef] [PubMed]
- Kim, P.; Amiran, M.D.; Lichtinger, A.; Yeung, S.N.; Slomovic, A.R.; Rootman, D.S. Outcomes of Descemet stripping automated endothelial keratoplasty in patients with glaucoma drainage devices. Cornea 2012, 31, 172–175. [Google Scholar] [CrossRef] [PubMed]
- Kusano, Y.; Yamaguchi, T.; Nishisako, S.; Matsumura, T.; Fukui, M.; Higa, K.; Inoue, T.; Shimazaki, J. Aqueous cytokine levels are associated with progression of peripheral anterior synechiae after Descemet stripping automated endothelial keratoplasty. Transl. Vis. Sci. Technol. 2021, 10, 12. [Google Scholar] [CrossRef] [PubMed]
- Goshe, J.M.; Terry, M.A.; Li, J.Y.; Straiko, M.D.; Davis-Boozer, D. Graft dislocation and hypotony after Descemet stripping automated endothelial keratoplasty in patients with previous glaucoma surgery. Ophthalmology 2012, 119, 1130–1133. [Google Scholar] [CrossRef] [PubMed]
- Banitt, M.; Arrieta-Quintero, E.; Parel, J.M.; Fantes, F. Technique for air bubble management during endothelial keratoplasty in eyes after penetrating glaucoma surgery. Cornea 2011, 30, 184–188. [Google Scholar] [CrossRef] [PubMed]
- Oyakawa, I.; Hayashi, T.; Shimizu, T.; Kato, N. Modified Descemet stripping automated endothelial keratoplasty: The use of ophthalmic viscoelastic devices in hypotonic eyes that had undergone glaucoma filtering surgeries. Case Rep. Ophthalmol. Med. 2018, 2018, 9387810. [Google Scholar] [CrossRef] [PubMed]
- Phillips, P.M.; Terry, M.A.; Shamie, N.; Chen, E.S.; Hoar, K.; Dhoot, D.; Shah, A.K.; Friend, D.J.; Rao, N.K.; Davis-Boozer, D.D. Descemet stripping automated endothelial keratoplasty in eyes with previous trabeculectomy and tube shunt procedure: Intraoperative and early postoperative complications. Cornea 2010, 29, 534–540. [Google Scholar] [CrossRef] [PubMed]
- Saeedi, O.J.; Jefferys, J.L.; Solis, J.F.; Jampel, H.D.; Quigley, H.A. Risk factors for adverse consequences of low intraocular pressure after trabeculectomy. J. Glaucoma 2014, 23, e60–e68. [Google Scholar] [CrossRef] [PubMed]
- Haynes, W.L.; Akduman, L. Combination of autologous blood injection and bleb compression sutures to treat hypotony maculopathy. J. Glaucoma 1999, 8, 384–387. [Google Scholar] [CrossRef] [PubMed]
- Kosior-Jarecka, E.; Wróbel-Dudzińska, D.; Sweich, A.; Żarnowski, T. Bleb compressive sutures in the management of hypotony maculopathy after glaucoma surgery. J. Clin. Med. 2021, 10, 2223. [Google Scholar] [CrossRef] [PubMed]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



