Submitted:
15 March 2026
Posted:
17 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Data Sources
2.2. NoSQL-Oriented Data Architecture
2.3. Data Cleaning and Analytic Sample
2.4. Variables
2.5. External Country Stratification
2.6. Statistical Analysis
2.7. Software, Reproducibility, and Ethical Considerations
3. Results
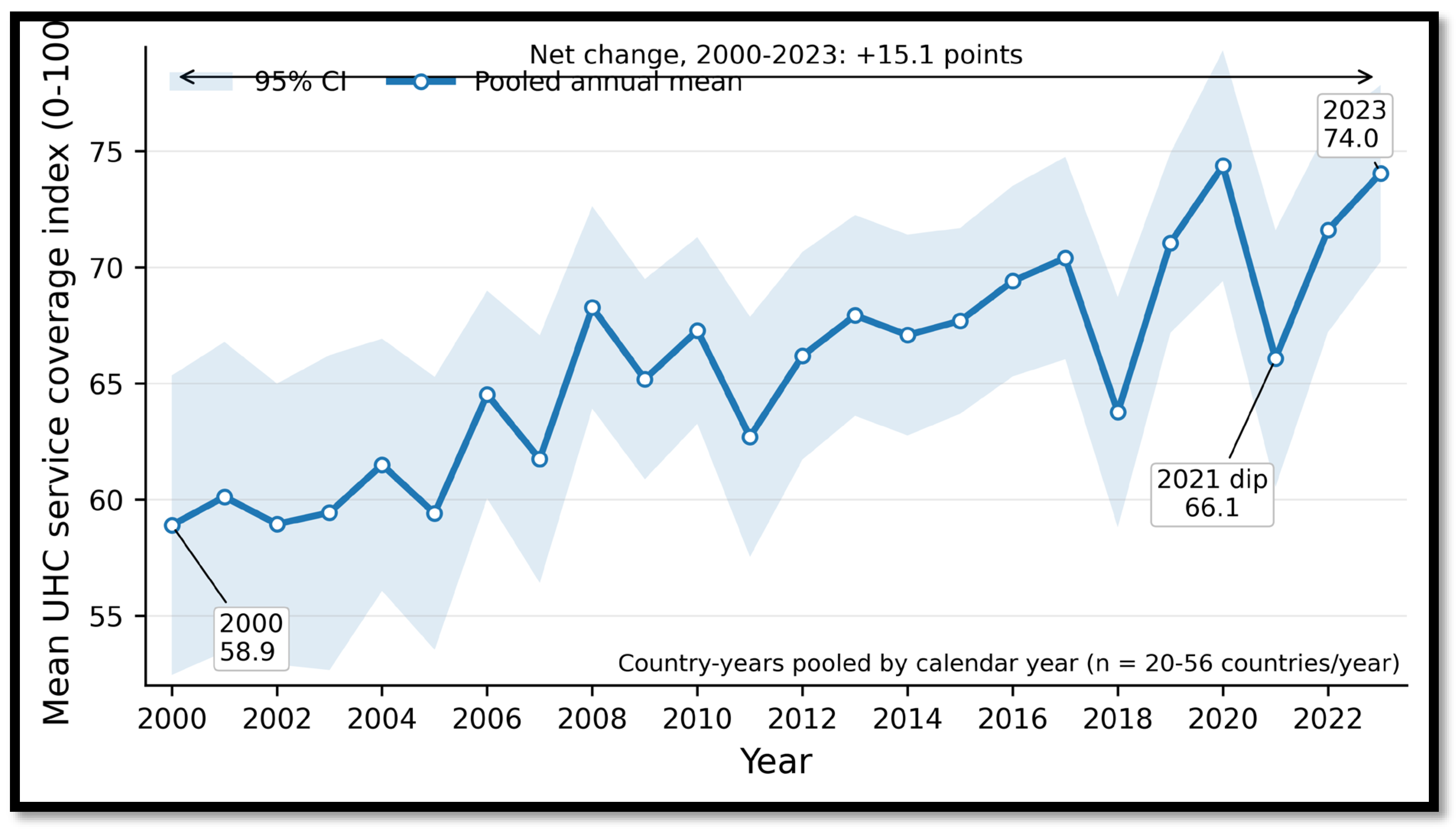
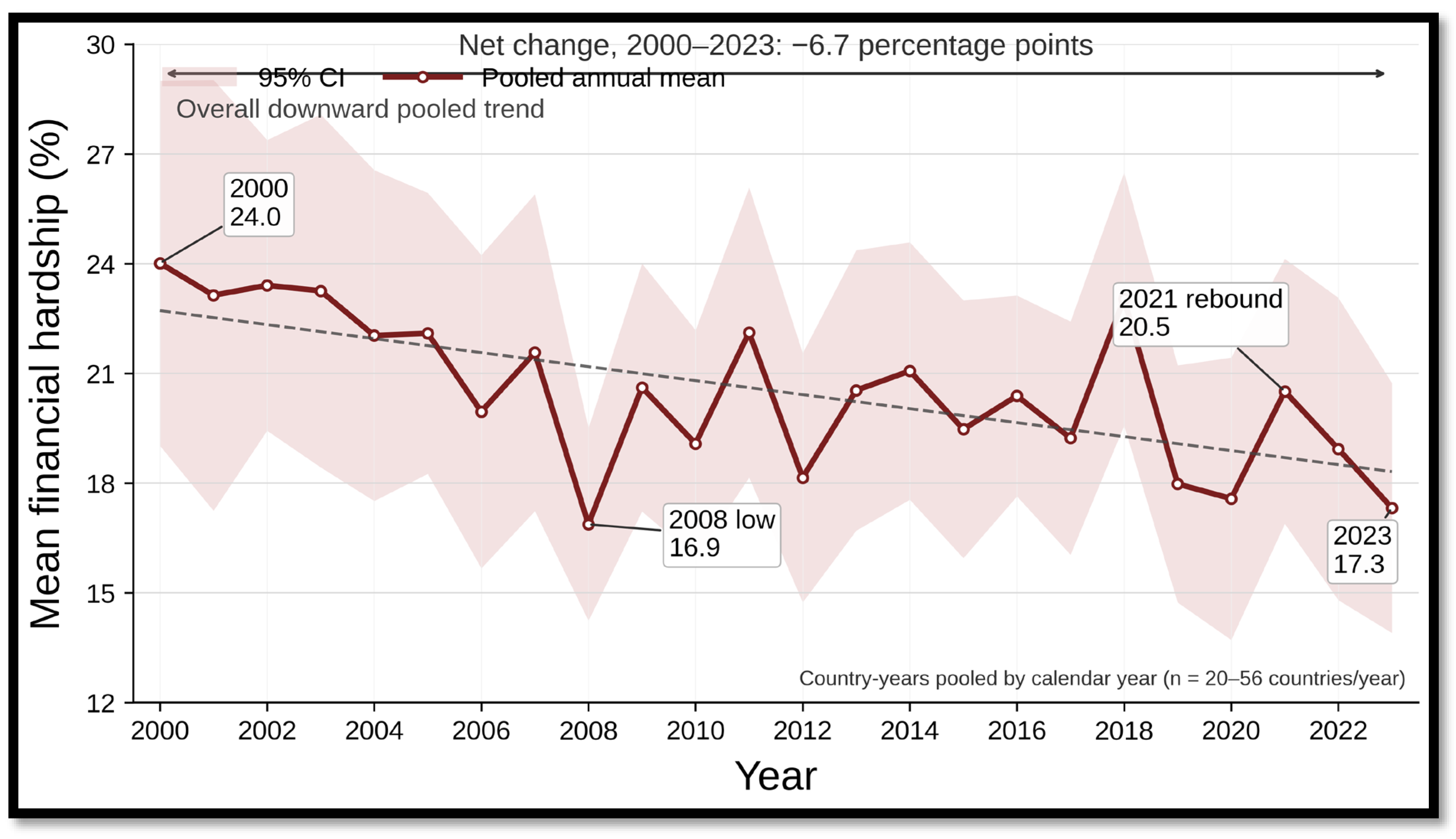
3.1. Global Trends in Service Coverage and Financial Hardship
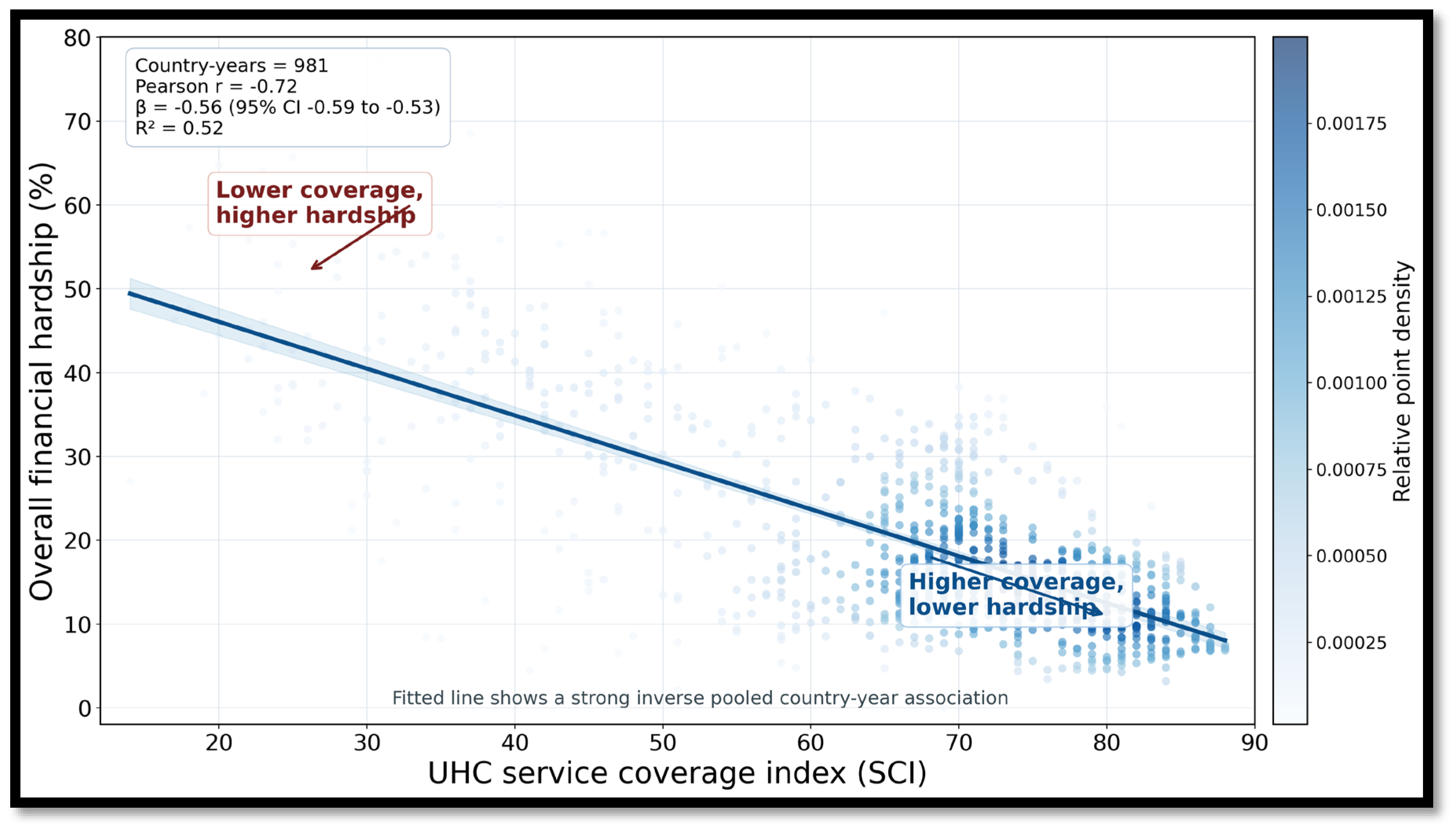
3.2. Main Association Between Service Coverage and Financial Hardship
3.3. Domain-Specific Associations
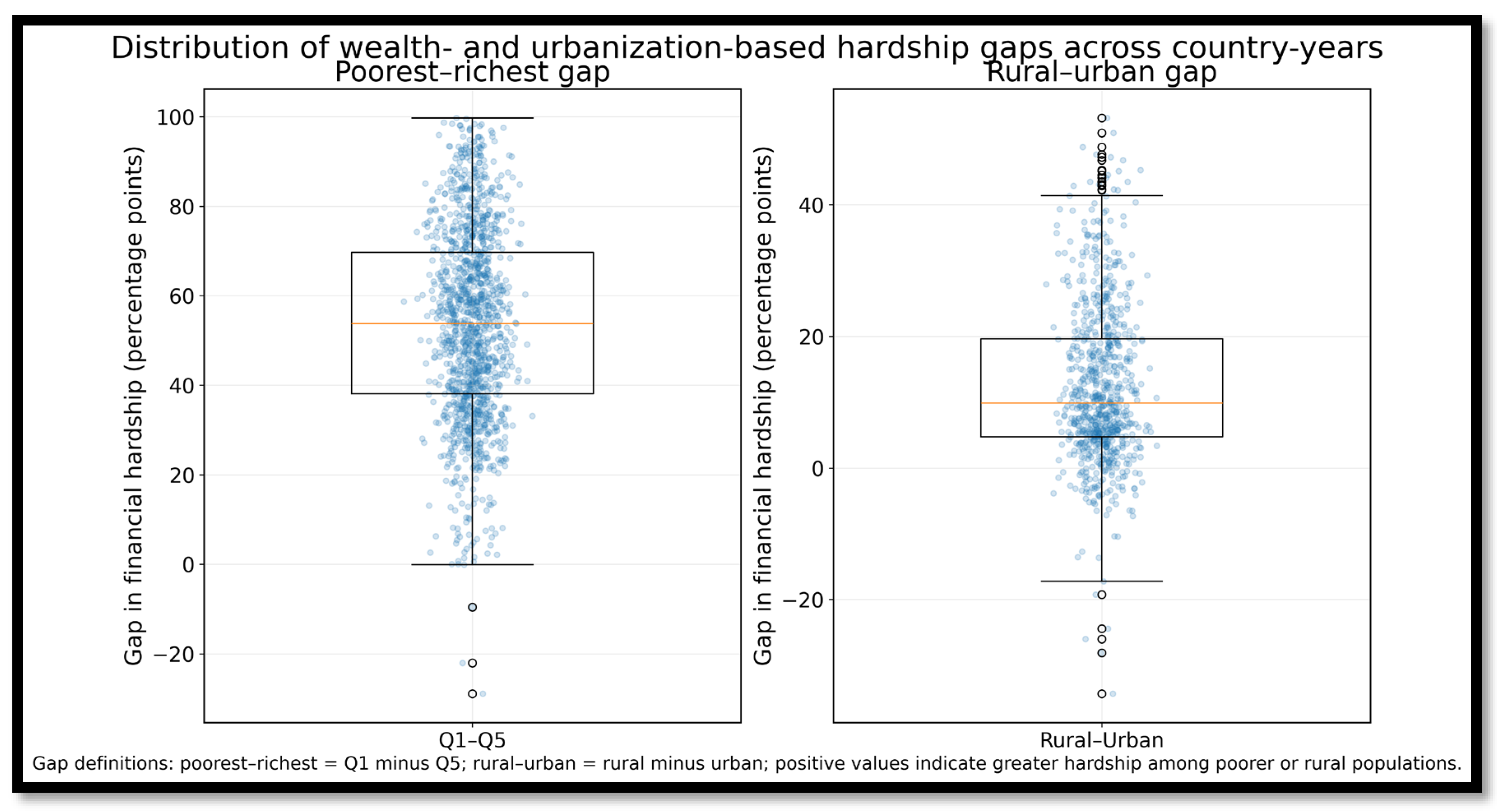
3.4. Inequalities by Wealth Quintile and Urbanization
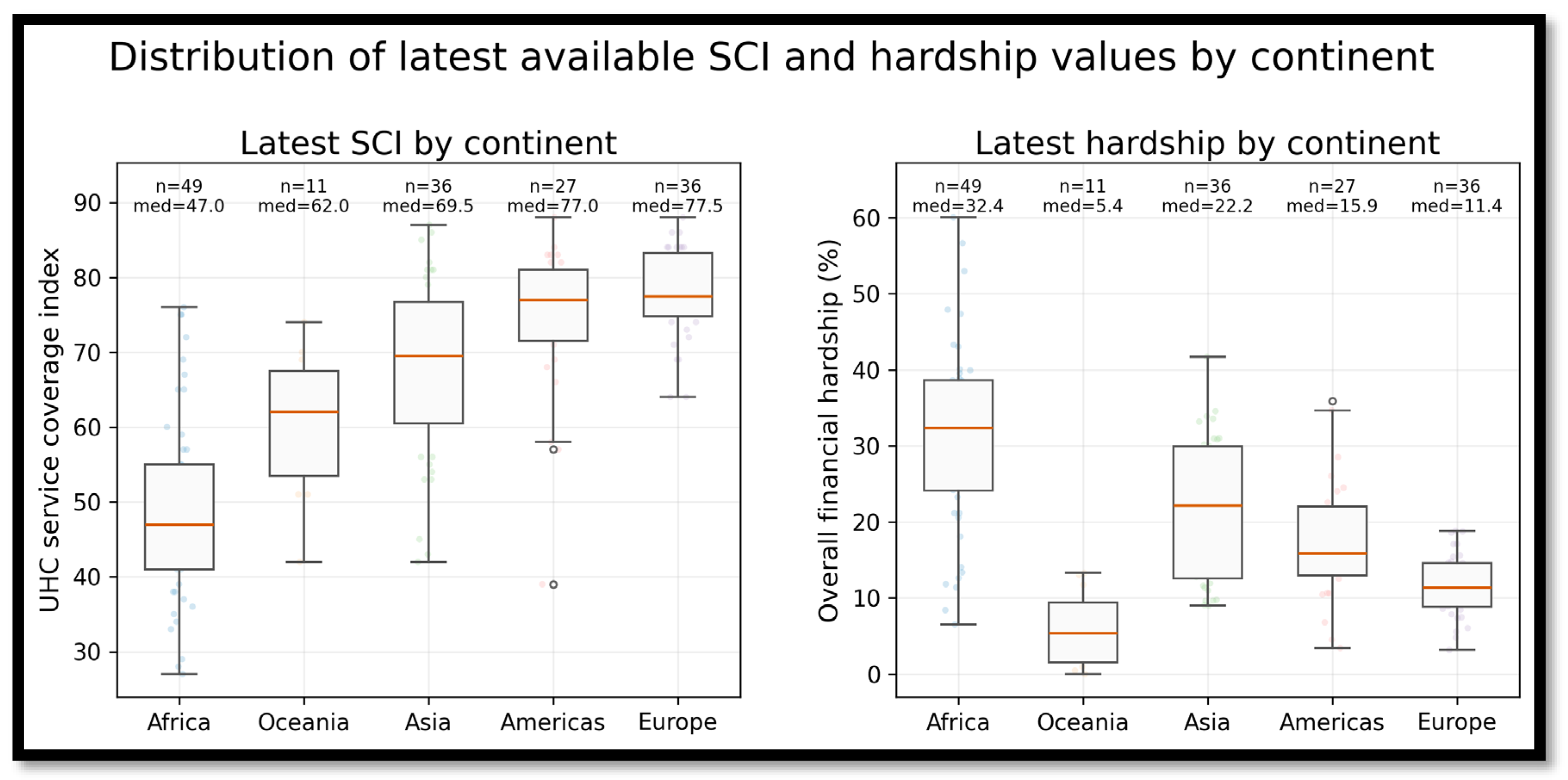
3.5. Cross-Sectional Heterogeneity in Latest Available Values
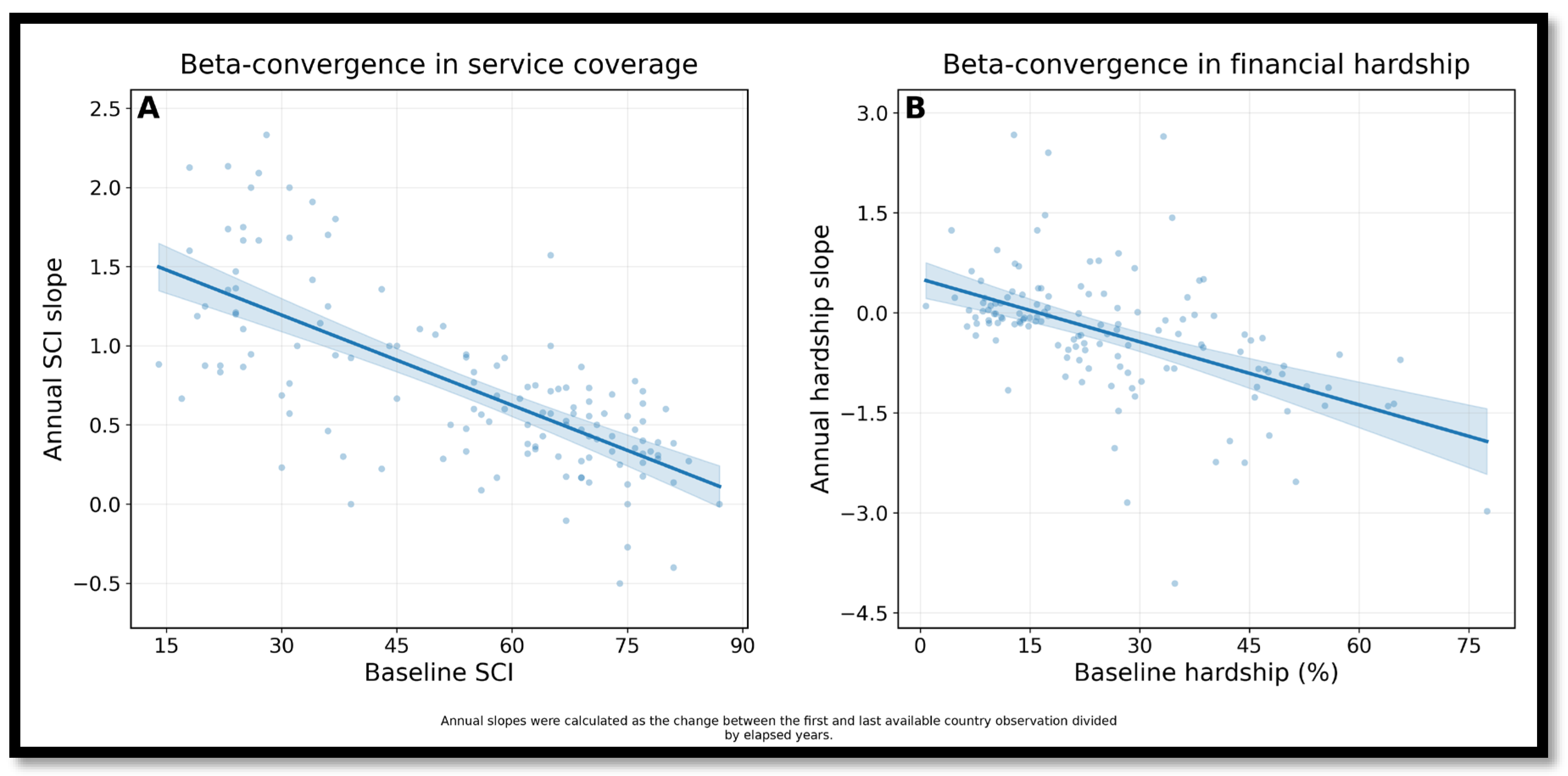
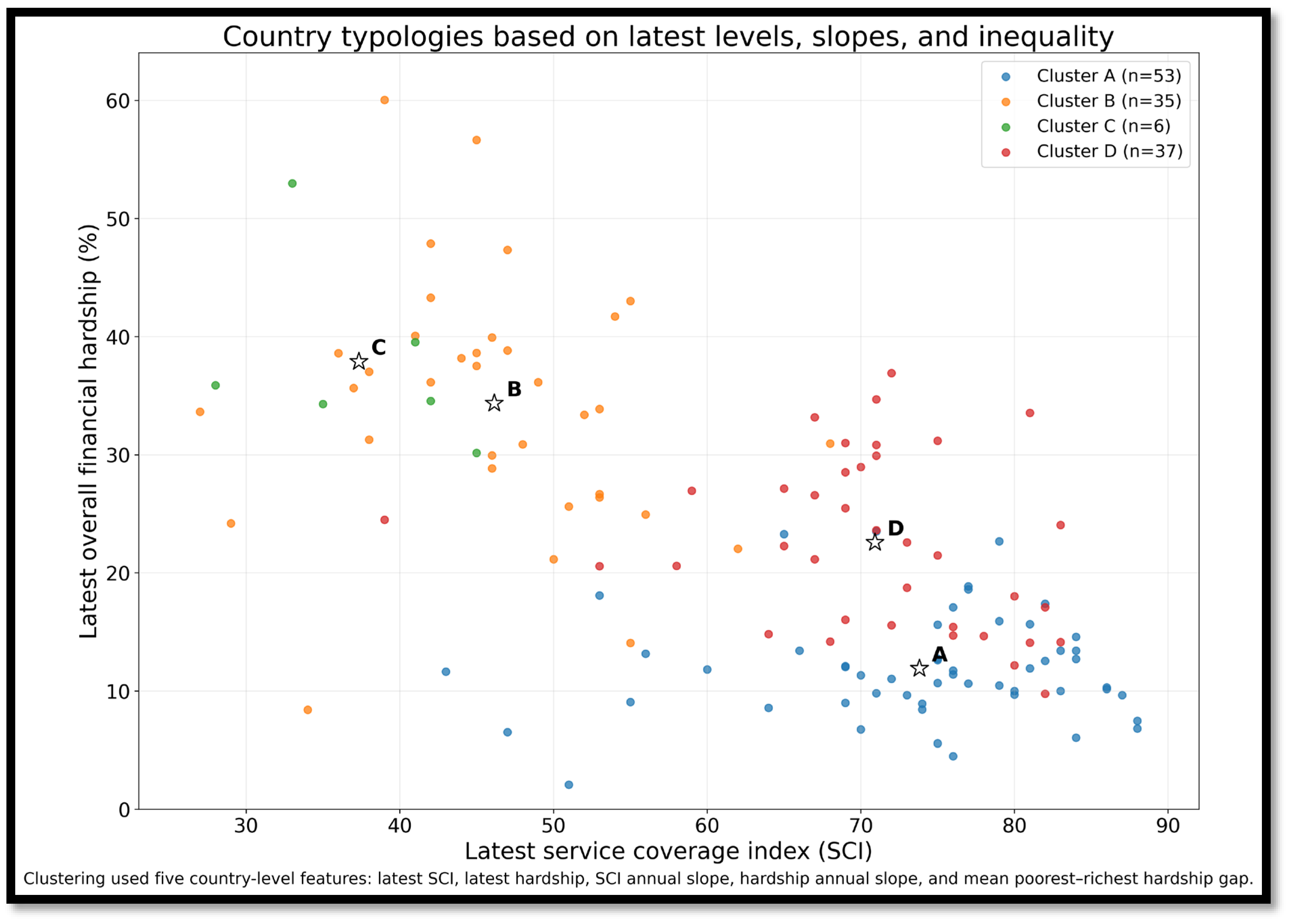
3.6. Stratified Slopes, Convergence, and Country Typologies
4. Discussion
4.1. Strengths and Limitations
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest
Abbreviations
| Abbreviation | Meaning | Abbreviation | Meaning |
| AI | artificial intelligence | CI | confidence interval |
| CICV | Centro de Investigaciones en Ciencias de la Vida | CSV | comma-separated values |
| OOP | out-of-pocket | FH | financial hardship |
| FH40 | financial hardship due to out-of-pocket health spending | GEE | generalized estimating equations |
| 95% CI | 95% confidence interval | WB | World Bank |
| JSON | JavaScript Object Notation | NoSQL | non-relational, document-oriented data architecture |
| ORCID | Open Researcher and Contributor ID | PNG | Portable Network Graphics |
| Q1 | poorest wealth quintile | Q5 | richest wealth quintile |
| RMNCH | reproductive, maternal, newborn, and child health | SCI | service coverage index |
| SD | standard deviation | SDG | Sustainable Development Goal |
| UHC | universal health coverage | WHO | World Health Organization |
References
- Darrudi, A.; Khoonsari, M.H.K.; Tajvar, M. Challenges to achieving universal health coverage throughout the world: a systematic review. J Prev Med Public Health 2022, 55(2), 125–133. [Google Scholar] [CrossRef]
- Ranabhat, C.L.; Acharya, S.P.; Adhikari, C.; Kim, C.-B. Universal health coverage evolution, ongoing trend, and future challenge: a conceptual and historical policy review. Front Public Health 2023, 11, 1041459. [Google Scholar] [CrossRef]
- Endalamaw, A.; Mengistu, T.S.; Khatri, R.B.; et al. Universal health coverage—exploring the what, how, and why using realist review. PLOS Glob Public Health 2025, 5(3), e0003330. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Universal health coverage (UHC). Available online: https://www.who.int/news-room/fact-sheets/detail/universal-health-coverage-%28uhc%29 (accessed on 14 March 2026).
- World Health Organization; World Bank. Tracking universal health coverage: 2025 global monitoring report; World Health Organization: Geneva, Switzerland, 2025; Available online: https://www.who.int/publications/i/item/9789240117808 (accessed on 14 March 2026).
- Takura, T.; Miura, H. Socioeconomic determinants of universal health coverage in the Asian region. Int J Environ Res Public Health 2022, 19(4), 2376. [Google Scholar] [CrossRef]
- Hanson, K.; Brikci, N.; Erlangga, D.; et al. The Lancet Global Health Commission on financing primary health care: putting people at the centre. Lancet Glob Health 2022, 10(5), e715–e772. [Google Scholar] [CrossRef] [PubMed]
- Lal, A.; Erondu, N.A.; Heymann, D.L.; Gitahi, G.; Yates, R. Pandemic preparedness and response: exploring the role of universal health coverage within the global health security architecture. Lancet Glob Health 2022, 10(11), e1675–e1683. [Google Scholar] [CrossRef]
- Dhillon, I.; Jhalani, M.; Thamarangsi, T.; Siyam, A.; Khetrapal Singh, P. Advancing universal health coverage in the WHO South-East Asia Region with a focus on human resources for health. Lancet Reg Health Southeast Asia 2023, 18, 100313. [Google Scholar] [CrossRef]
- Lai, Y.; Liang, D.; Bobogare, A.; Yadamsuren, B.; Yam, E.; Yi, S.; Bugoro, H.; Huang, J. Synergising universal health coverage and global health security in the Western Pacific Region. J Glob Health 2025, 15, 04037. [Google Scholar] [CrossRef]
- Hajjar, K.; Moresky, R.T.; et al. Association between universal health coverage and the disease burden of acute illness and injury at the global level. BMC Public Health 2023, 23, 735. [Google Scholar] [CrossRef] [PubMed]
- Khan, M.R.; Mohammad, K.U.; Rabbani, M.S. Impact of health expenditure on universal health coverage (composite index): global evidence. Health Promot Perspect. 2025, 15(3), 268–277. [Google Scholar] [CrossRef]
- Arhin, K.; Frimpong, A.O.; Acheampong, K. Effect of primary health care expenditure on universal health coverage: evidence from Sub-Saharan Africa. Clinicoecon Outcomes Res. 2022, 14, 643–652. [Google Scholar] [CrossRef]
- Fisher, M.; Freeman, T.; Mackean, T.; Friel, S.; Baum, F. Universal health coverage for non-communicable diseases and health equity: lessons from Australian primary healthcare. Int J Health Policy Manag. 2022, 11(5), 690–700. [Google Scholar] [CrossRef]
- Feng, X.L.; Zhang, Y.; Hu, X.; et al. Tracking progress towards universal health coverage for essential health services in China, 2008–2018. BMJ Glob Health 2022, 7(11), e010552. [Google Scholar] [CrossRef]
- Bayked, E.M.; Toleha, H.N.; Kebede, S.Z.; Workneh, B.D.; Kahissay, M.H. The impact of community-based health insurance on universal health coverage in Ethiopia: a systematic review and meta-analysis. Glob Health Action. 2023, 16(1), 2189764. [Google Scholar] [CrossRef]
- Winkelmann, J.; Listl, S.; van Ginneken, E.; Benzian, H. Universal health coverage cannot be universal without oral health. Lancet Public Health 2023, 8(1), e8–e10. [Google Scholar] [CrossRef]
- Hajji, O.; El Abbadi, B.; Akhnif, E.H.; et al. Systematic review of financing functions for universal health coverage in low- and middle-income countries: reforms, challenges, and lessons learned. Public Health Rev. 2025, 46, 1607745. [Google Scholar] [CrossRef] [PubMed]
- Langat, E.; Gesesew, H.A.; Mwanri, L.; Ward, P.R. Factors influencing the adoption of universal health coverage in Africa: insights from a realist synthesis. Soc Sci Med. 2025, 387, 118709. [Google Scholar] [CrossRef] [PubMed]
- Namyalo, P.K.; Wodnik, B.K.; Michaelides, O.; Kane, S.; Essue, B.; Di Ruggiero, E. Identifying implementation science research and policy priorities to advance universal health coverage: a multi-country modified Delphi study. BMJ Glob Health 2025, 10(8), e018562. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization. Financial hardship in health and components (SDG 3.8.2, 2025 definition), % of the population. Available online: https://www.who.int/data/gho/indicator-metadata-registry/imr-details/376 (accessed on 14 March 2026).
- World Bank Data Help Desk. How does the World Bank classify countries? Available online: https://datahelpdesk.worldbank.org/knowledgebase/articles/378834-how-does-the-world-bank-classify-countries (accessed on 14 March 2026).
- World Bank. Universal health coverage (UHC) service coverage index. Data360. Available online: https://data360.worldbank.org/en/indicator/UHC-SCI (accessed on 14 March 2026).
- World Bank. Universal health coverage (UHC) dataset. Data360. Available online: https://data360.worldbank.org/en/dataset/WB_UHC (accessed on 14 March 2026).
- Thomson, S.; Cylus, J.; Evetovits, T.; et al. Monitoring progress towards universal health coverage in Europe: a descriptive analysis of financial protection in 40 countries. Lancet Reg Health Eur. 2024, 37, 100826. [Google Scholar] [CrossRef]
- Antunes, A.F.; Jithitikulchai, T.; Hohmann, J.; Flessa, S. Revisiting a decade of inequality in healthcare financial burden in Cambodia, 2009–19: trends, determinants and decomposition. Int J Equity Health 2024, 23, 196. [Google Scholar] [CrossRef]
- Okamoto, S.; Sata, M.; Rosenberg, M.; et al. Universal health coverage in the context of population ageing: catastrophic health expenditure and unmet need for healthcare. Health Econ Rev. 2024, 14, 8. [Google Scholar] [CrossRef]
- Damrongplasit, K.; Melnick, G. Utilisation, out-of-pocket payments and access before and after COVID-19: Thailand’s universal health coverage scheme. BMJ Glob Health 2024, 9(5), e015179. [Google Scholar] [CrossRef]
- Nungo, S.; Filippon, J.; Russo, G. Social health insurance for universal health coverage in low- and middle-income countries: a retrospective policy analysis of attainments, setbacks and equity implications of Kenya’s social health insurance model. BMJ Open 2024, 14(12), e085903. [Google Scholar] [CrossRef] [PubMed]
- Gorgodze, T.; et al. Financial protection and universal health coverage in Georgia: an analysis of impoverishing healthcare costs using household income and expenditure surveys. BMJ Glob Health 2025, 10(7), e019150. [Google Scholar] [CrossRef]
- Zhang, Q.; Wang, J.S.H.; He, A.J.; et al. Providing financial protection in health for low-income populations: a comparison of health financing designs in East Asia. Int J Equity Health 2025, 24, 215. [Google Scholar] [CrossRef]
- Azizatunnisa’, L.; Probandari, A.; Kuper, H.; Banks, L.M. Health insurance coverage, healthcare use, and financial protection amongst people with disabilities in Indonesia: analysis of the 2021 National Socioeconomic Survey. Lancet Reg Health Southeast Asia 2025, 39, 100631. [Google Scholar] [CrossRef] [PubMed]
- Hussein, N.; Ng, C.W.; Ramli, R.; et al. Assessing catastrophic health expenditure and impoverishment in adult asthma care: a cross-sectional study of patients attending six public health clinics in Klang District, Malaysia. BMC Health Serv Res. 2024, 24, 327. [Google Scholar] [CrossRef]
- Serván-Mori, E.; Gómez-Dantés, O.; et al. Increase of catastrophic and impoverishing health expenditures in Mexico associated to policy changes and the COVID-19 pandemic. J Glob Health 2023, 13, 06044. [Google Scholar] [CrossRef] [PubMed]
- Cerecero-García, D.; Gómez-Dantés, O.; Hone, T.; et al. Catastrophic and impoverishing health expenditures in fragmented public health systems: lessons from Mexico, 2000–2022. Health Econ Rev. 2026, 16, 22. [Google Scholar] [CrossRef]
- Nguyen, P.T.; Le, P.M. Progress and inequalities in financial risk protection toward universal health coverage: insights from Vietnam. Int J Equity Health 2025, 24, 287. [Google Scholar] [CrossRef]
- Rahman, M.M.; Jung, J.; Islam, M.R.; et al. Global, regional, and national progress in financial risk protection towards universal health coverage, 2000–2030. Soc Sci Med. 2022, 312, 115367. [Google Scholar] [CrossRef] [PubMed]
- Rahman, M.M.; et al. Progress towards universal health coverage in South Asia, 2000–2030: an examination of the twin elements of primary healthcare provision and financial protection. BMJ Glob Health 2025, 10(11), e020052. [Google Scholar] [CrossRef] [PubMed]
- The Lancet Regional Health—Europe. Strengthening primary health care to achieve universal health coverage. Lancet Reg Health Eur. 2024, 39, 100897. [Google Scholar] [CrossRef] [PubMed]
| Dataset | Raw observations | Countries/economies in raw file | Time span | Analytic filters |
|---|---|---|---|---|
| UHC service coverage index (SCI) | 24840 | 207 | 2000-2023 | Full index and four domain subindices |
| Financial hardship (FH40) | 17634 | 180 | 1985-2024 | All household types, total urbanization for overall panel; hardship subcomponents retained |
| Harmonized analytic panel | 981 | 159 | 2000-2023 | Country-year overlap between SCI and FH, continent assigned, and World Bank income group matched where available |
| Variable | Mean | SD | Median | IQR | Min | Max | N |
|---|---|---|---|---|---|---|---|
| SCI full index (0-100) | 65.63 | 16.04 | 70.0 | 19.0 | 14.0 | 88.0 | 981 |
| Financial hardship, all (%) | 20.53 | 12.43 | 16.52 | 15.61 | 0.0 | 77.45 | 981 |
| Large non-impoverishing OOP burden (%) | 3.67 | 2.47 | 3.11 | 3.16 | 0.0 | 15.85 | 959 |
| Impoverishing OOP expenditure (%) | 16.85 | 11.87 | 12.45 | 14.49 | 0.0 | 73.89 | 959 |
| Pushed into poverty (%) | 1.7 | 1.19 | 1.42 | 1.21 | 0.0 | 9.53 | 885 |
| Further impoverished (%) | 15.45 | 11.75 | 10.84 | 13.75 | 0.2 | 72.36 | 885 |
| Model | Beta | CI low | CI high | p-value | N | R2 |
|---|---|---|---|---|---|---|
| Pearson correlation | -0.722 | — | — | <0.001 | 981 | 0.521 |
| Country FE + trend | -0.447 | -0.691 | -0.203 | 0.0003 | 981 | 0.886 |
| Two-way FE | -0.441 | -0.707 | -0.175 | 0.0011 | 981 | 0.889 |
| Mixed model | -0.496 | -0.564 | -0.429 | <0.001 | 981 | — |
| GEE | -0.521 | -0.599 | -0.443 | <0.001 | 981 | — |
| Spline test | — | — | — | 0.0618 | 981 | 0.890 |
| SCI domain | Beta | CI low | CI high | p-value |
|---|---|---|---|---|
| RMNCH subindex | 0.12 | -0.133 | 0.373 | 0.3521 |
| Infectious diseases subindex | -0.206 | -0.336 | -0.076 | 0.0019 |
| Non-communicable diseases subindex | -0.257 | -0.506 | -0.007 | 0.0437 |
| Service capacity and access subindex | -0.076 | -0.172 | 0.019 | 0.1158 |
| Metric | Mean | SD | Median | IQR | Min | Max | N |
|---|---|---|---|---|---|---|---|
| Poorest-richest gap in financial hardship (Q1-Q5) | 53.73 | 21.40 | 53.81 | 31.57 | -28.91 | 99.75 | 1323 |
| Rural-urban gap in financial hardship | 12.50 | 12.02 | 9.88 | 14.90 | -34.30 | 53.23 | 783 |
| Continent | Countries | Mean SII | Median SII |
|---|---|---|---|
| Africa | 49 | 66.93 | 70.59 |
| Americas | 26 | 45.94 | 49.71 |
| Asia | 34 | 56.5 | 59.17 |
| Europe | 36 | 36.8 | 38.81 |
| Oceania | 11 | 20.36 | 20.49 |
| Income group | Countries | Mean SII | Median SII |
|---|---|---|---|
| High income | 44 | 35.73 | 35.38 |
| Upper-middle income | 45 | 46.51 | 43.38 |
| Lower-middle income | 48 | 60.13 | 70.14 |
| Low income | 24 | 68.85 | 70.29 |
| Continent | Countries | SCI mean | SCI median | FH mean | FH median |
|---|---|---|---|---|---|
| Africa | 49 | 49.06 | 47.0 | 31.29 | 32.44 |
| Oceania | 11 | 60.45 | 62.0 | 5.96 | 5.38 |
| Asia | 36 | 68.08 | 69.5 | 21.25 | 22.16 |
| Americas | 27 | 74.48 | 77.0 | 17.51 | 15.91 |
| Europe | 36 | 77.94 | 77.5 | 11.57 | 11.38 |
| Income group | Countries | SCI mean | SCI median | FH mean | FH median |
|---|---|---|---|---|---|
| High income | 41 | 80.05 | 81.00 | 11.49 | 11.00 |
| Upper-middle income | 45 | 71.64 | 71.00 | 16.83 | 14.64 |
| Lower-middle income | 47 | 56.91 | 56.00 | 24.39 | 26.02 |
| Low income | 24 | 42.21 | 42.00 | 36.36 | 36.02 |
| Continent | Beta | CI low | CI high | p-value |
|---|---|---|---|---|
| Africa | -0.495 | -0.779 | -0.211 | 0.0006 |
| Americas | -0.223 | -0.741 | 0.294 | 0.3977 |
| Asia | -0.333 | -0.675 | 0.009 | 0.0567 |
| Europe | -0.175 | -0.689 | 0.339 | 0.5047 |
| Oceania | 0.062 | -0.298 | 0.422 | 0.7344 |
| Income group | Beta | CI low | CI high | p-value |
|---|---|---|---|---|
| High income | -0.021 | -0.383 | 0.341 | 0.9090 |
| Upper-middle income | -0.336 | -0.856 | 0.184 | 0.2059 |
| Lower-middle income | -0.295 | -0.968 | 0.379 | 0.3911 |
| Low income | -1.002 | -1.673 | -0.330 | 0.0035 |
| Outcome | Baseline coefficient | CI low | CI high | p-value | R2 |
|---|---|---|---|---|---|
| SCI annual slope | -0.019 | -0.022 | -0.016 | <0.001 | 0.487 |
| FH annual slope | -0.031 | -0.041 | -0.022 | <0.001 | 0.260 |
| Cluster | Profile | Countries | SCI (latest) | FH all (latest) | SCI annual slope | FH annual slope | Mean Q1-Q5 gap |
|---|---|---|---|---|---|---|---|
| A | High coverage; low hardship | 53 | 73.81 | 11.90 | 0.54 | -0.08 | 36.40 |
| B | Low coverage; rapid gains; high inequality | 35 | 46.14 | 34.37 | 1.37 | -0.91 | 65.65 |
| C | Fragile; rising hardship | 6 | 37.33 | 37.90 | 0.63 | 1.79 | 33.91 |
| D | Mid-high coverage; persistent inequality | 37 | 70.92 | 22.57 | 0.48 | -0.40 | 67.87 |
| Country | Continent | SCI (latest) | FH all (latest) |
|---|---|---|---|
| United States | Americas | 88.0 | 6.81 |
| United Kingdom | Europe | 88.0 | 7.47 |
| Korea, Rep. | Asia | 87.0 | 9.65 |
| Finland | Europe | 86.0 | 10.15 |
| Switzerland | Europe | 86.0 | 10.31 |
| Japan | Asia | 86.0 | 11.0 |
| Israel | Asia | 85.0 | 16.57 |
| Netherlands | Europe | 84.0 | 3.17 |
| Germany | Europe | 84.0 | 4.8 |
| Slovenia | Europe | 84.0 | 6.05 |
| Country | Continent | SCI (latest) | FH all (latest) |
|---|---|---|---|
| Congo, Dem. Rep. | Africa | 39.0 | 60.03 |
| Burundi | Africa | 45.0 | 56.64 |
| Central African Republic | Africa | 33.0 | 52.97 |
| Sierra Leone | Africa | 42.0 | 47.89 |
| Nigeria | Africa | 47.0 | 47.35 |
| Liberia | Africa | 42.0 | 43.29 |
| Malawi | Africa | 55.0 | 43.02 |
| Bangladesh | Asia | 54.0 | 41.7 |
| Mali | Africa | 41.0 | 40.07 |
| Sudan | Africa | 46.0 | 39.92 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




