Submitted:
09 March 2026
Posted:
09 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
2.1. Study Design and Setting
2.2. Study Variables
2.3. Statistical Analysis
3. Results
3.1. Participant Characteristics
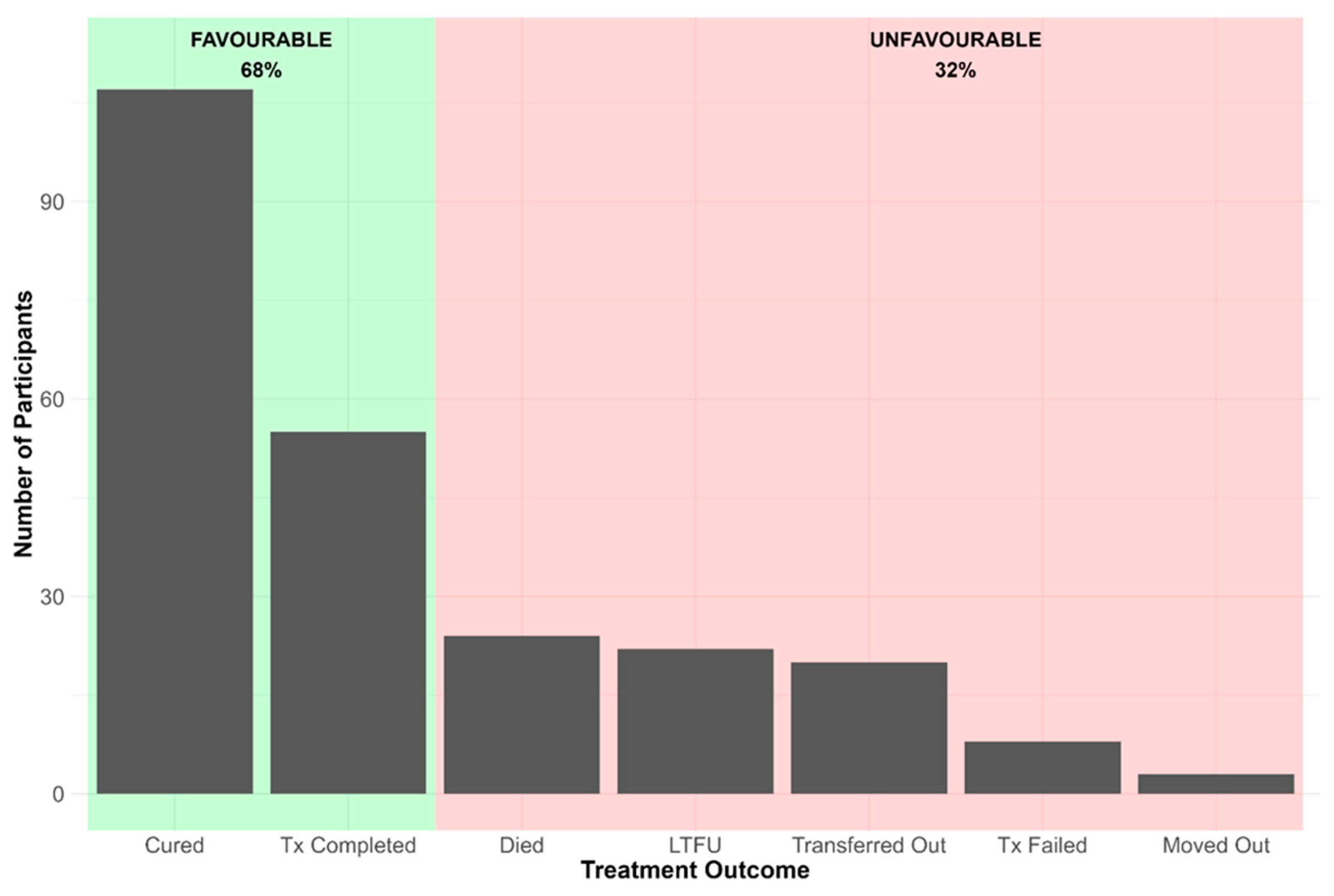
3.1.2. Socio-Demographic Characteristics
3.1.3. Age Distribution
3.1.4. Gender
3.1.5. Education Level
3.1.6. Income Status
3.1.7. Occupation
3.1.8. Social History
3.1.9. Clinical Characteristics
3.1.10. Previous Drug History
3.1.11. Patient Category
3.1.12. Type of Resistance (Mono vs Poly Drug Resistance)
3.1.13. Type of DR-TB
3.1.14. Comorbidity
3.2. Univariate Analysis
3.3. Multivariable Logistic Regression
3.3.1. Type of DR-TB
3.3.2. Income
3.3.3. Age and Gender
3.3.4. Comorbidity Type
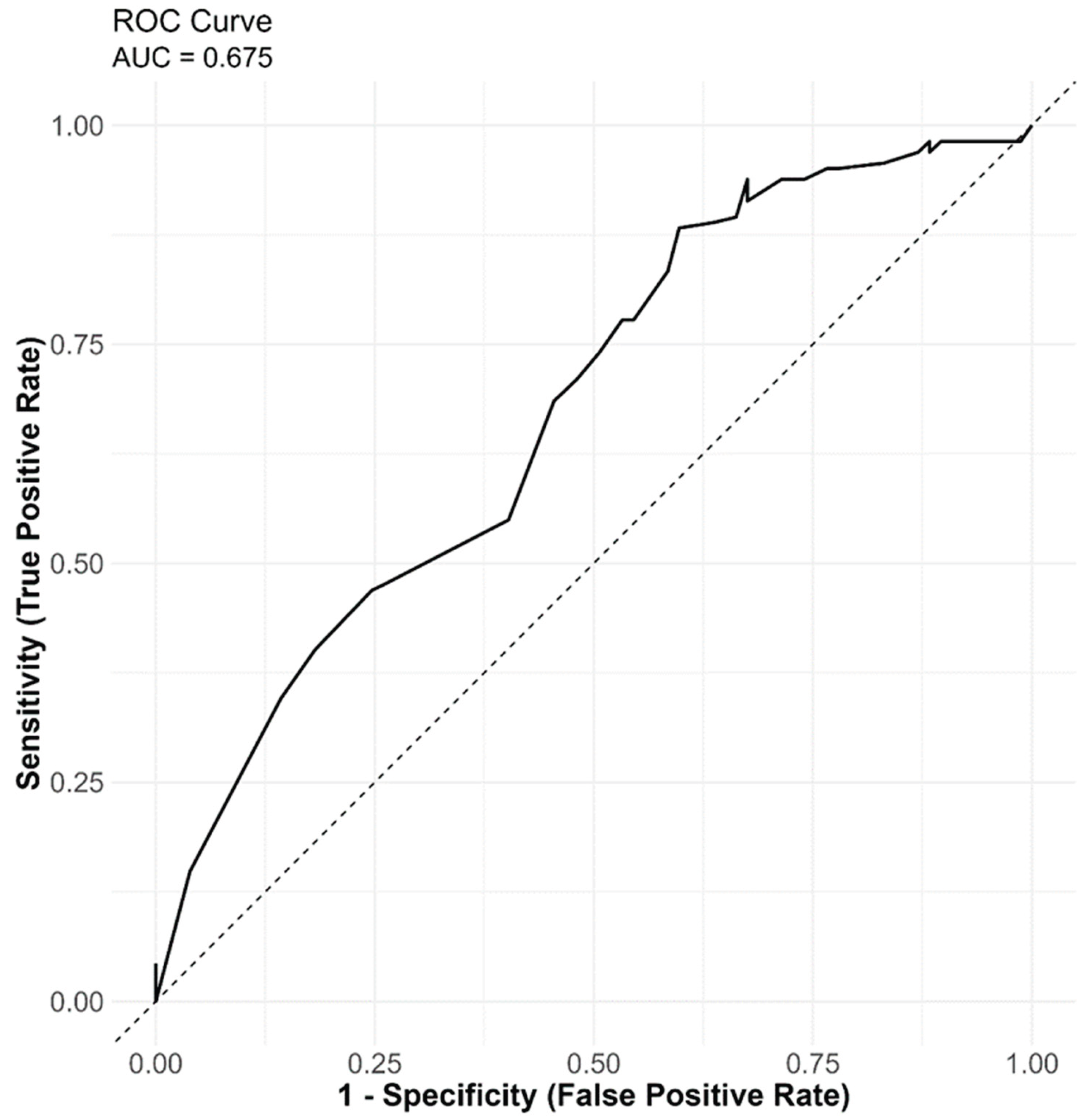
3.4. Model Performance
| Variable | GVIF^(1/(2*Df)) | Interpretation |
| Age group | 1.01 | Very low; no multicollinearity |
| Gender | 1.02 | Very low; no multicollinearity |
| Type of DR-TB | 1.01 | Very low; no multicollinearity |
| Income | 1.04 | Very low; no multicollinearity |
| Comorbidity type | 1.05 | Very low; no multicollinearity |
4. Discussion
4.1. Descriptive Patterns in Socio-Demographic Characteristics
4.2. Descriptive Patterns in Clinical Characteristics
4.3. Univariate Associations
4.4. Independent Predictors of Treatment Outcome
4.5. Model Performance and Implications
5. Strengths and Limitations
6. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| TB | Tuberculosis |
| DR-TB | Drug resistant tuberculosis |
| RR-TB | Rifampicin resistant tuberculosis |
| MDR-TB | Multi drug resistant tuberculosis |
| Pre-XDR-TB | Pre-extensively drug-resistant |
| XDR-TB | Extensively drug-resistant |
| WHO | World Health Organization |
| HIV | Human immunodeficiency virus |
References
- Tiberi, S; Utjesanovic, N; Galvin, J; Centis, R; D'Ambrosio, L; van den Boom, M; Zumla, A; Migliori, GB. Drug resistant TB–latest developments in epidemiology, diagnostics and management. International Journal of Infectious Diseases 2022, 124, S20–5. [Google Scholar] [CrossRef] [PubMed]
- Chowdhury, K; Ahmad, R; Sinha, S; Dutta, S; Haque, M. Multidrug-resistant TB (MDR-TB) and extensively drug-resistant TB (XDR-TB) among children: where we stand now. Cureus 2023, 15(2), e35154. [Google Scholar] [CrossRef] [PubMed]
- Dlatu, N; Faye, LM; Apalata, T. Outcomes of Treating Tuberculosis Patients with Drug-Resistant Tuberculosis, Human Immunodeficiency Virus, and Nutritional Status: The Combined Impact of Triple Challenges in Rural Eastern Cape. International Journal of Environmental Research and Public Health 2025, 22(3), 319. [Google Scholar] [CrossRef]
- Hosu, MC; Faye, LM; Apalata, T. Comorbidities and treatment outcomes in patients diagnosed with drug-resistant tuberculosis in rural Eastern Cape Province, South Africa. Diseases 2024, 12(11), 296. [Google Scholar] [CrossRef]
- Singh, A; Prasad, R; Balasubramanian, V; Gupta, N. Drug-resistant tuberculosis and HIV infection: current perspectives. HIV/AIDS-Research and Palliative Care 2020, 9–31. [Google Scholar] [CrossRef] [PubMed]
- Teferi, MY; El-Khatib, Z; Boltena, MT; Andualem, AT; Asamoah, BO; Biru, M; Adane, HT. Tuberculosis treatment outcome and predictors in Africa: a systematic review and meta-analysis. International journal of environmental research and public health 2021, 18(20), 10678. [Google Scholar] [CrossRef]
- Dlatu, N; Faye, LM; Sineke, N; Apalata, T. Predictors of drug-resistant TB outcomes: Body mass index, HIV, and comorbidities. African Journal of Primary Health Care & Family Medicine 2025, 17(1), 4953. [Google Scholar] [CrossRef]
- SeyedAlinaghi, S; Afsahi, AM; Moradi, A; Parmoon, Z; Habibi, P; Mirzapour, P; Dashti, M; Ghasemzadeh, A; Karimi, E; Sanaati, F; Hamedi, Z. Current ART, determinants for virologic failure and implications for HIV drug resistance: an umbrella review. AIDS research and therapy 2023, 20(1), 74. [Google Scholar] [CrossRef]
- Alara, JA; Alara, OR. An overview of the global alarming increase of multiple drug resistant: a major challenge in clinical diagnosis. Infectious Disorders-Drug TargetsDisorders 2024, 24(3), 26–42. [Google Scholar] [CrossRef]
- Borah, P; Deb, PK; Venugopala, KN; Al-Shar'i, NA; Singh, V; Deka, S; Srivastava, A; Tiwari, V; Mailavaram, RP. Tuberculosis: an update on pathophysiology, molecular mechanisms of drug resistance, newer anti-TB drugs, treatment regimens and host-directed therapies. Current Topics in Medicinal Chemistry 2021, 21(6), 547–70. [Google Scholar] [CrossRef]
- Odoom, A; Osman, AH; Dzuvor, CK. Recent advances in immunotherapeutic and vaccine-based approaches for the treatment of drug-resistant bacterial infections. ACS Infectious Diseases 2025, 11(6), 1366–402. [Google Scholar] [CrossRef]
- Faye, LM; Hosu, MC; Dlatu, N; Iruedo, J; Apalata, T. Predicting treatment adherence in patients with drug-resistant tuberculosis: insights from socioeconomic, demographic, and clinical factors of patients in the rural Eastern Cape. Frontiers in Tuberculosis 2025, 3, 1659333. [Google Scholar] [CrossRef]
- Kimani, E; Muhula, S; Kiptai, T; Orwa, J; Odero, T; Gachuno, O. Factors influencing TB treatment interruption and treatment outcomes among patients in Kiambu County, 2016-2019. PloS one 2021, 16(4), e0248820. [Google Scholar] [CrossRef]
- Reddy, SC; Mohan, KG; Jain, K. Impact of socioeconomic factors on the treatment of tuberculosis. In InEmerging Paradigms in Delivery Systems for Antitubercular Therapy; Academic Press, 1 Jan 2025; pp. 353–369. [Google Scholar]
- Gilmour, B; Alene, KA. Ending tuberculosis: Challenges and opportunities. Frontiers in Tuberculosis 2024, 2, 1487518. [Google Scholar] [CrossRef]
- Dookie, N; Ngema, SL; Perumal, R; Naicker, N; Padayatchi, N; Naidoo, K. The changing paradigm of drug-resistant tuberculosis treatment: successes, pitfalls, and future perspectives. Clinical Microbiology Reviews 2022, 35(4), e00180-19. [Google Scholar] [CrossRef] [PubMed]
- Soedarsono, S; Mertaniasih, NM; Kusmiati, T; Permatasari, A; Ilahi, WK; Anggraeni, AT. Characteristics of previous tuberculosis treatment history in patients with treatment failure and the impact on acquired drug-resistant tuberculosis. Antibiotics 2023, 12(3), 598. [Google Scholar] [CrossRef] [PubMed]
- Shah, HD; Nazli Khatib, M; Syed, ZQ; Gaidhane, AM; Yasobant, S; Narkhede, K; Bhavsar, P; Patel, J; Sinha, A; Puwar, T; Saha, S. Gaps and interventions across the diagnostic care cascade of TB patients at the level of patient, community and health system: a qualitative review of the literature. Tropical Medicine and Infectious Disease 2022, 7(7), 136. [Google Scholar] [CrossRef] [PubMed]
- Al-Worafi, YM. Tuberculosis management in developing countries. In InHandbook of Medical and Health Sciences in Developing Countries: Education, Practice, and Research; Springer International Publishing: Cham, 30 Nov 2023; pp. 1–40. [Google Scholar]
- Matambo, R.; Nyandoro, G.; Sandy, C.; Nkomo, T.; Mutero-Munyati, S.; Mharakurwa, S.; Chikaka, E.; Ngwenya, M.; Ndongwe, G.; Pepukai, V.M. Predictors of mortality and treatment success of multi-drug resistant and Rifampicin resistant tuberculosis in Zimbabwe: a retrospective cohort analysis of patients initiated on treatment during 2010 to 2015. The Pan African Medical Journal 2021, 39, 128. [Google Scholar] [CrossRef]
- Nangombe, V.N.T. Predictors of treatment success among patients with drug resistant Tuberculosis in Namibia. Doctoral dissertation, University of Namibia, 2022. [Google Scholar]
- Johnson, J.M.; Mohapatra, A.K.; Velladath, S.U.; Shettigar, K.S. Predictors of treatment outcomes in drug resistant tuberculosis-observational retrospective study. The International Journal of Mycobacteriology 2022, 11(1), 38–46. [Google Scholar] [CrossRef]
- Leketa, M.M.; Zondi, S.; Cele, L.; Mathibe, M.; Ngwepe, P. Factors associated with unfavourable treatment outcomes among tuberculosis patients at health facilities of Maseru, Lesotho. South African Family Practice 2024, 66(1), 6004. [Google Scholar] [CrossRef]
- Nxumalo, E. L.; Sineke, N.; Dlatu, N.; Apalata, T.; Faye, L. M. Treatment Outcomes of Tuberculosis in the Eastern Cape: Clinical and Socio-Demographic Predictors from Two Rural Clinics. International Journal of Environmental Research and Public Health 2025, 22(12), 1804. [Google Scholar] [CrossRef]
- Hosu, M. C.; Faye, L. M.; Apalata, T. Optimizing Drug-Resistant Tuberculosis Treatment Outcomes in a High HIV-Burden Setting: A Study of Sputum Conversion and Regimen Efficacy in Rural South Africa. Pathogens 2025, 14(5), 441. [Google Scholar] [CrossRef]
- Fekadu, G.; Turi, E.; Kasu, T.; Bekele, F.; Chelkeba, L.; Tolossa, T.; Labata, B. G.; Dugassa, D.; Fetensa, G.; Diriba, D. C. Impact of HIV status and predictors of successful treatment outcomes among tuberculosis patients: A six-year retrospective cohort study. Annals of medicine and surgery (2012) 2020, 60, 531–541. [Google Scholar] [CrossRef]
- Baluku, J.B.; Mukasa, D.; Bongomin, F.; et al. Gender differences among patients with drug resistant tuberculosis and HIV co-infection in Uganda: a countrywide retrospective cohort study. BMC Infect Dis 2021, 21, 1093. [Google Scholar] [CrossRef] [PubMed]
- Barteka, G.; Bwayo, D.; Matovu, J.K.; Wanume, B.; Alunyo, J.P.; Sseguya, R.; Masaba, J.P.; Obbo, J.S. Treatment outcomes and predictors of success for multidrug resistant tuberculosis MDR TB in Ugandan regional referral hospitals. Scientific Reports 2025, 15(1), 14144. [Google Scholar] [CrossRef]
- Tian, M.; Ding, H.; Lu, P.; et al. Determinants of treatment success and cost implications in MDR/RR-TB patients: a prospective cohort study in China. Sci Rep 2025, 15, 34370. [Google Scholar] [CrossRef]
- Mbuh, T.P.; Mendjime, P.; Goupeyou-Wandji, I.A.; Donkeng-Donfack, V.F.; Kahou, J.; Endale Mangamba, L.M.; Mefoug, S.; Bisso Ngono, P.A.; Esso, L.; Etoundi Mballa, G.A. Trends of drug-resistant tuberculosis and risk factors to poor treatment-outcome: a database analysis in Littoral region-Cameroon, 2013–2022. BMC Public Health 2024, 24(1), 3195. [Google Scholar] [CrossRef]
- World Health Organization. Global tuberculosis report 2020: executive summary.
- Safaev, K.; Parpieva, N.; Liverko, I.; Yuldashev, S.; Dumchev, K.; Gadoev, J.; Korotych, O.; Harries, A. D. Trends, Characteristics and Treatment Outcomes of Patients with Drug-Resistant Tuberculosis in Uzbekistan: 2013–2018. International Journal of Environmental Research and Public Health 2021, 18(9), 4663. [Google Scholar] [CrossRef] [PubMed]
- Varshney, K.; Anaele, B.; Molaei, M.; Frasso, R.; Maio, V. Risk Factors for Poor Outcomes Among Patients with Extensively Drug-Resistant Tuberculosis (XDR-TB): A Scoping Review. Infection and Drug Resistance 2021, 14, 5429–5448. [Google Scholar] [CrossRef] [PubMed]
- Saukkonen, JJ; Duarte, R; Munsiff, SS; Winston, CA; Mammen, MJ; Abubakar, I; Acuña-Villaorduña, C; Barry, PM; Bastos, ML; Carr, W; Chami, H. Updates on the treatment of drug-susceptible and drug-resistant tuberculosis: an official ATS/CDC/ERS/IDSA clinical practice guideline. American Journal of Respiratory and Critical Care Medicine 2025, 211(1), 15–33. [Google Scholar] [CrossRef]
- Pedersen, O.S.; Butova, T.; Kapustnyk, V.; Miasoiedov, V.; Kuzhko, M.; Hryshchuk, L.; Kornaha, S.; Borovok, N.; Raznatovska, O.; Fedorec, A.; Bogomolov, A. Treatment outcomes and risk factors for an unsuccessful outcome among patients with highly drug-resistant tuberculosis in Ukraine. Clinical Microbiology and Infection 2024, 30(3), 360–367. [Google Scholar] [CrossRef] [PubMed]
- Nidoi, J.; Muttamba, W.; Walusimbi, S.; Imoko, J.F.; Lochoro, P.; Ictho, J.; Mugenyi, L.; Sekibira, R.; Turyahabwe, S.; Byaruhanga, R.; Putoto, G. Impact of socio-economic factors on Tuberculosis treatment outcomes in north-eastern Uganda: a mixed methods study. BMC Public Health 2021, 21(1), 2167. [Google Scholar] [CrossRef] [PubMed]
- Ngari, M.M.; Rashid, M.A.; Sanga, D.; Mathenge, H.; Agoro, O.; Mberia, J.K.; Katana, G.G.; Vaillant, M.; Abdullahi, O.A. Burden of HIV and treatment outcomes among TB patients in rural Kenya: a 9-year longitudinal study. BMC infectious diseases 2023, 23(1), 362. [Google Scholar] [CrossRef] [PubMed]
- Ngala, S. M.; Tantoh, D. M.; Nfor, O. N.; Francis, G. D.; Fitame, A.; Chu, Y. W. Age-specific relationship between HIV and TB treatment outcomes in the West Region of Cameroon: a cross-sectional study. BMC infectious diseases 2025, 25(1), 475. [Google Scholar] [CrossRef] [PubMed]
- Faye, LM; Dlatu, N; Hosu, MC; Chitha, WW; Apalata, T. Community-engaged clinical governance and machine learning for optimizing tuberculosis management in rural Eastern Cape. Frontiers in Public Health 2026, 13, 1713401. [Google Scholar] [CrossRef]
| Characteristic | Category |
Overall N = 2391 |
Favourable N = 1621 |
Unfavourable N = 771 |
| Age group | ≤39 | 139 (58%) | 99 (61%) | 40 (52%) |
| 40–49 | 59 (25%) | 39 (24%) | 20 (26%) | |
| ≥50 | 41 (17%) | 24 (15%) | 17 (22%) | |
| Gender | Female | 96 (40%) | 60 (37%) | 36 (47%) |
| Male | 143 (60%) | 102 (63%) | 41 (53%) | |
| Education | Low | 46 (19%) | 31 (19%) | 15 (19%) |
| Medium | 168 (70%) | 114 (70%) | 54 (70%) | |
| High | 25 (10%) | 17 (10%) | 8 (10%) | |
| Income | No income | 192 (80%) | 136 (84%) | 56 (73%) |
| Some income | 47 (20%) | 26 (16%) | 21 (27%) | |
| Occupation | Employed | 25 (10%) | 19 (12%) | 6 (7.8%) |
| Unemployed | 214 (90%) | 143 (88%) | 71 (92%) | |
| Social history | None | 145 (61%) | 95 (59%) | 50 (65%) |
| Single substance | 63 (26%) | 45 (28%) | 18 (23%) | |
| Multiple substances | 31 (13%) | 22 (14%) | 9 (12%) |
| Characteristic | Category |
Overall N = 2391 |
Favourable N = 1621 |
Unfavourable N = 771 |
| Previous drug history | New | 97 (41%) | 67 (41%) | 30 (39%) |
| Previous treatment | 142 (59%) | 95 (59%) | 47 (61%) | |
| Patient category | New | 101 (42%) | 71 (44%) | 30 (39%) |
| Relapse | 95 (40%) | 63 (39%) | 32 (42%) | |
| Treatment failure | 43 (18%) | 28 (17%) | 15 (19%) | |
| Type of resistance | MONO | 93 (39%) | 65 (40%) | 28 (36%) |
| POLY | 146 (61%) | 97 (60%) | 49 (64%) | |
| Type of DR-TB | MDR | 95 (40%) | 68 (42%) | 27 (35%) |
| RR | 127 (53%) | 89 (55%) | 38 (49%) | |
| XDR | 17 (7.1%) | 5 (3.1%) | 12 (16%) | |
| Comorbidity | Multiple | 10 (4.2%) | 8 (4.9%) | 2 (2.6%) |
| Single | 229 (96%) | 154 (95%) | 75 (97%) |
| Variable | Category vs Reference | OR (95% CI) | p-value |
| Age group | 40–49 vs <40 | 0.79 (0.44–1.41) | 0.474 |
| ≥50 vs <40 | 0.57 (0.29–1.12) | 0.127 | |
| Gender | Male vs Female | 1.49 (0.85–2.61) | 0.153 |
| Occupation | Unemployed vs Employed | 0.64 (0.27–1.52) | 0.356 |
| Type of DR-TB | RR vs MDR | 0.93 (0.53–1.63) | 0.808 |
| XDR vs MDR | 0.17 (0.06–0.50) | 0.002 | |
| Income | Some income vs No income | 0.51 (0.27–0.95) | 0.043 |
| Comorbidity type | Single vs Multiple | 0.51 (0.24–1.10) | 0.079 |
| Type of resistance | POLY vs Mono | 0.85 (0.43–1.67) | 0.578 |
| Education | Medium vs Low | 1.02 (0.54–1.93) | 0.952 |
| High vs Low | 1.03 (0.41–2.57) | 0.958 | |
| Previous drug history | Previous treatment vs None | 0.91 (0.49–1.69) | 0.724 |
| Social history | Single substance vs None | 1.32 (0.60–2.90) | 0.404 |
| Multiple substances vs None | 1.29 (0.49–3.39) | 0.560 | |
| Patient category | Relapse vs New | 0.83 (0.44–1.56) | 0.549 |
| Treatment failure vs New | 0.79 (0.37–1.69) | 0.540 |
| Variable | Category vs Reference | Adjusted OR (95% CI) | p-value |
| Age group | 40–49 vs <40 | 0.87 (0.44–1.71) | 0.706 |
| ≥50 vs <40 | 0.51 (0.24–1.09) | 0.089 | |
| Gender | Male vs Female | 1.55 (0.87–2.77) | 0.146 |
| Type of DR-TB | RR vs MDR | 0.91 (0.50–1.66) | 0.749 |
| XDR vs MDR | 0.18 (0.06–0.58) | 0.004 | |
| Income | Some income vs No income | 0.46 (0.23–0.92) | 0.036 |
| Comorbidity type | Single vs Multiple | 0.29 (0.06–1.38) | 0.143 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




