Submitted:
04 March 2026
Posted:
06 March 2026
You are already at the latest version
Abstract
Keywords:
Introduction:
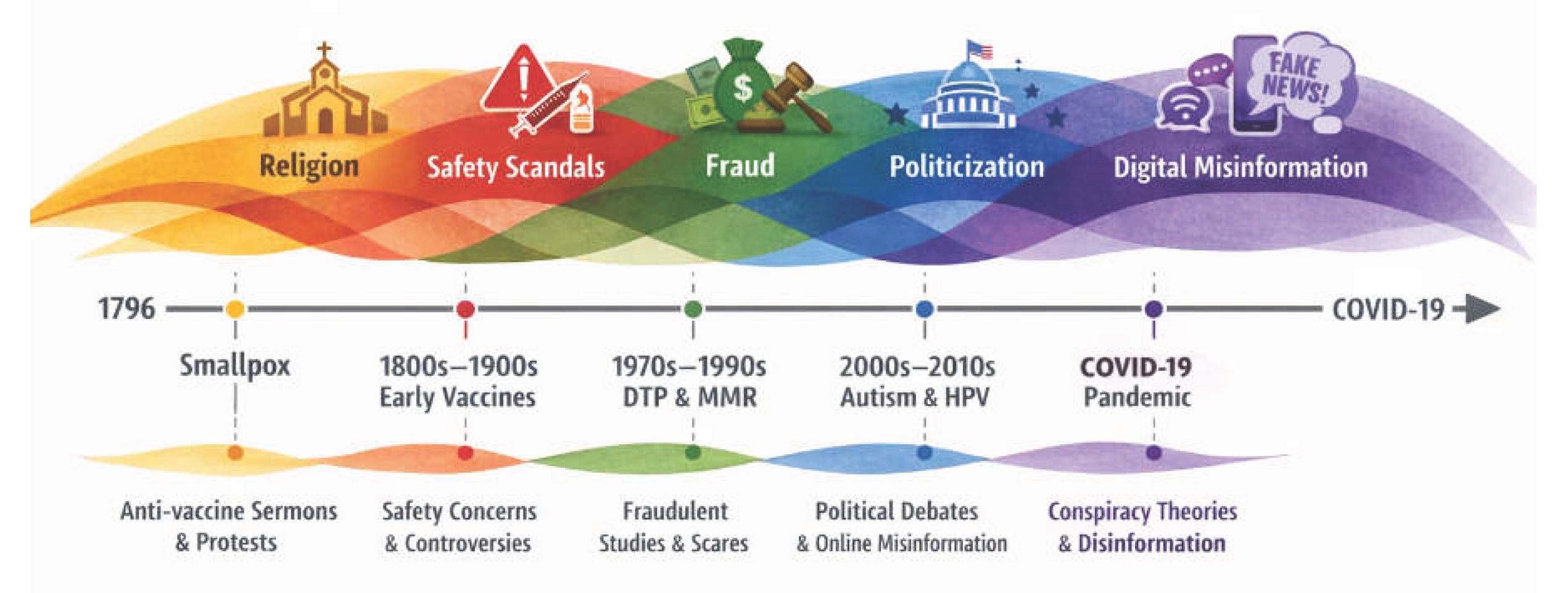
II. Historical Perspective on Vaccine Hesitancy
- A.
- Early Hesitancy: Resistance to Smallpox Vaccination (18th–19th Centuries)
- B.
- Mid-20th Century: Mass Immunization Campaigns and Emerging Concerns
- C.
- Modern Vaccine Hesitancy: MMR Controversy and COVID-19 Vaccine Skepticism
- Misinformation and Conspiracy Theories: False claims about microchips, infertility, and DNA alteration proliferated across social media [23].
- Political Polarization: In countries like the U.S., vaccine attitudes became entangled with political ideologies, with some groups viewing mandates as government overreach [24].
- Historical Mistrust: Communities with histories of medical exploitation, such as African American populations in the U.S. (e.g., the Tuskegee Syphilis Study), exhibited lower vaccine confidence [25].
- D.
- Patterns and Shifts in Vaccine Hesitancy Over Time
- From Local to Global Resistance: Early hesitancy was often regionally contained, whereas modern movements leverage global digital networks to spread skepticism.
- The Role of Media: While historical vaccine hesitancy was fueled by print pamphlets and political cartoons, today’s misinformation spreads through social media and online communities.
- Scientific Advancements vs. Public Doubt: Despite significant improvements in vaccine safety and efficacy, public concerns have evolved rather than disappeared, reflecting deeper societal anxieties rather than purely scientific skepticism.
III. Sociocultural Drivers of Vaccine Hesitancy
- A.
- Religious and Cultural Beliefs: Resistance Due to Faith-Based Perspectives
- For example, in the Netherlands, the Bible Belt, a region with a high concentration of conservative Protestant communities, has experienced periodic measles outbreaks due to religious objections to vaccination [28]. Some members of these communities believe that immunization demonstrates a lack of faith in divine protection.
- Similarly, in Pakistan and Afghanistan, vaccine hesitancy, particularly regarding polio vaccination, has been linked to religious misinformation and conspiracy theories [29]. Some Islamic clerics have propagated the belief that vaccines contain haram (forbidden) ingredients such as pork-derived gelatin or that they are a Western ploy to sterilize Muslim populations. These narratives have contributed to violent resistance against vaccination campaigns, including attacks on healthcare workers.
- In the United States, some Christian fundamentalist groups reject vaccines on moral and ethical grounds [30]. Hesitancy surrounding the human papillomavirus (HPV) vaccine has been particularly pronounced among religious conservatives, who argue that vaccinating adolescents against a sexually transmitted infection may promote promiscuity [31]. Despite evidence showing that the HPV vaccine significantly reduces cervical cancer risk, these religious concerns have slowed its uptake.
- During the 2014–2016 Ebola outbreak, rumors spread that foreign medical teams were using vaccines to infect people rather than protect them. Such mistrust led some communities to reject vaccination efforts, exacerbating the crisis [32].
- B.
- Misinformation and Social Media Influence: The Role of Digital Platforms in Amplifying Hesitancy
- In Brazil, misinformation campaigns led some populations to reject COVID-19 vaccines, particularly in rural and Indigenous communities. Similarly, in India, viral WhatsApp messages falsely claimed that the COVID-19 vaccine contained cow blood, sparking resistance among Hindu communities [33].
- C.
- Community Trust and Perceptions of Healthcare Systems: The Impact of Historical Medical Injustices on Trust
- D.
- Geographical Differences: Vaccine Hesitancy Trends in High-Income vs. Low-Income Countries
IV. Psychological Factors Influencing Vaccine Hesitancy
- A.
- Cognitive Biases and Risk Perception: How Heuristics Shape Vaccine Decision-Making
- Omission Bias: Many vaccine-hesitant individuals prefer inaction over action, even when action (vaccination) is objectively safer. This occurs because the psychological burden of experiencing an adverse event due to vaccination feels greater than the risk of harm from inaction (contracting the disease). A study in Vaccine found that parents who refused childhood vaccines often cited concerns about the possibility of vaccine side effects, even when the likelihood of harm from the disease was significantly higher [43].
- Negativity Bias: Negative information has a greater impact on decision-making than positive information. Anti-vaccine content on social media exploits this bias by emphasizing rare adverse effects, often ignoring the overwhelming benefits of vaccines. A study analyzing Twitter vaccine discussions found that negative vaccine-related tweets were shared more frequently than positive ones, reinforcing vaccine hesitancy [44].
- Confirmation Bias: Individuals tend to seek information that confirms their existing beliefs and ignore evidence that contradicts them. Vaccine-hesitant individuals are more likely to engage with anti-vaccine content and dismiss scientific studies that support vaccination [45]. This creates echo chambers where misinformation flourishes.
- B.
- Fear, Anxiety, and Conspiracy Theories: Psychological Barriers to Vaccine Uptake
- Vaccine Safety Concerns and Anxiety Disorders
- 2.
- The Role of Conspiracy Theories
- Depopulation Myths: Claims that vaccines are designed to sterilize populations, which have been particularly prevalent in some African and South Asian communities [51].
- Empirical studies have demonstrated a strong correlation between conspiracy thinking and vaccine refusal. One study published in Psychological Medicine found that individuals who believed in COVID-19-related conspiracies were three times more likely to refuse the vaccine [52].
- 3.
- Countering Fear and Misinformation
- Cognitive-behavioral approaches can help individuals manage vaccine-related anxiety.
- Misinformation debunking should focus on preemptively correcting false narratives before they spread.
- Trusted messengers, such as community leaders and doctors, should engage in transparent communication to rebuild trust [53].
- C.
- Health Belief Model & Behavioral Theories: Explaining Hesitancy Using Psychological Frameworks
- Health Belief Model (HBM)
- Perceived Susceptibility: How likely they believe they are to contract the disease.
- Perceived Severity: How serious they think the disease is.
- Perceived Benefits: The extent to which they believe vaccination will protect them.
- Perceived Barriers: Factors preventing vaccination, such as fear of side effects.
- 2.
- Theory of Planned Behavior (TPB)
- Attitudes: Beliefs about vaccines.
- Subjective Norms: Social pressure from family, peers, or authorities.
- Perceived Behavioral Control: Whether they feel capable of accessing and receiving the vaccine.
- Empirical studies have shown that positive social norms (e.g., seeing friends and family get vaccinated) can significantly increase vaccine uptake. Campaigns that emphasize "most people are getting vaccinated" have been effective in overcoming hesitancy [55].
- 3.
- Dual-Process Theory: System 1 vs. System 2 Thinking
- System 1 (fast, intuitive): Emotional, automatic responses (e.g., "I heard vaccines are dangerous, so I won’t take them").
- System 2 (slow, analytical): More rational, evidence-based reasoning.
V. Political and Policy-Driven Factors in Vaccine Hesitancy
- A.
- Government Policies and Mandates: The Impact of Mandatory Vaccination Laws
- i.
- Mandatory Vaccination and Public Resistance
-
The U.S. Experience:
- -
- All 50 U.S. states require childhood vaccinations for school enrollment, but philosophical, religious, and medical exemptions vary [57].
- -
- States with lenient exemption policies (e.g., Texas, and Oregon) report higher rates of vaccine-preventable diseases due to the clustering of unvaccinated individuals [58].
- -
- The 2019 measles outbreak in New York led to removing religious exemptions, demonstrating how policy adaptation can curb vaccine hesitancy [59].
-
Europe’s Mixed Approaches:
-
Low- and Middle-Income Countries (LMICs):
- -
- -
- Government efforts to enforce immunization (e.g., linking vaccination to welfare benefits) have had mixed results, with some communities perceiving them as authoritarian interventions.
- B.
- Political Polarization and Mistrust: How Politics Shapes Vaccine Attitudes
-
Partisan Divide in Vaccine Attitudes
- In the United States, vaccine acceptance became a partisan issue, with Republicans expressing more significant skepticism than Democrats [64].
- Surveys showed that individuals with conservative political beliefs were more likely to oppose vaccine mandates, linking them to government overreach and loss of personal freedoms [65].
- In Brazil, political loyalty to former president Jair Bolsonaro correlated with lower vaccine uptake due to his dismissive stance on COVID-19 [66].
-
Mistrust in Government and Health Institutions
- In many LMICs, vaccine hesitancy is fueled by historical distrust in governments and Western-funded health initiatives.
- Kenya’s 2014 tetanus vaccine campaign faced resistance from religious and political leaders who falsely claimed the vaccine was a sterilization too [67].
- In Eastern Europe, low trust in government institutions correlates with higher vaccine refusal rates, particularly in countries with authoritarian histories [68].
- C.
- Pharmaceutical Industry and Economic Influences: Public Perception of Big Pharma’s Role
-
Concerns Over Profit-Driven Motives
- The global vaccine market is valued at over $50 billion annually, leading to accusations that pharmaceutical companies prioritize profits over public health [69].
- During the COVID-19 pandemic, debates over vaccine patents and pricing fueled skepticism, particularly in low-income countries that struggled with vaccine access while wealthier nations secured large stockpiles.
-
Past Pharmaceutical Scandals and Trust Erosion
- The 1999 Rotavirus vaccine recall due to safety concerns increased pediatric vaccine hesitancy in the early 2000s [72].
-
Industry-Government Ties and Perceived Conflicts of Interest
- The fast-tracked approval of COVID-19 vaccines under Operation Warp Speed led some to believe that political and economic incentives influenced regulatory decisions more than safety data [73].
- Transparency in clinical trial data and independent oversight are crucial in counteracting narratives that vaccines are rushed or unsafe.
- D.
- COVID-19 Case Study: How Political Responses Affected Vaccine Uptake
-
Divergent Government Responses
- Countries with centralized public health messaging (e.g., New Zealand) saw higher trust and compliance, whereas nations with fragmented messaging (e.g., U.S., Brazil) experienced greater vaccine hesitancy [75].
-
Misinformation and Political Leaders’ Influence
-
Vaccine Equity and Global Hesitancy
- Vaccine hoarding by high-income countries through advance purchase agreements led to delayed access in LMICs, reinforcing distrust in Western pharmaceutical companies.
- The suspension of AstraZeneca’s vaccine in Europe due to rare clotting events amplified global hesitancy, despite the vaccine’s overall safety profile [78].
VI. Impact on Immunization Programs and Public Health
- A.
- Vaccine Coverage and Disease Outbreaks: Correlation Between Hesitancy and Resurgence of Diseases
-
Case Studies: Resurgence of Diseases
-
Measles Outbreaks in the United States:
- -
- Measles, once virtually eliminated in the U.S., experienced a dramatic resurgence in recent years. According to CDC data, the number of measles cases surged from just 37 in 2010 to 1,282 in 2019, with unvaccinated populations contributing significantly to the outbreaks [79]. Vaccine hesitancy among communities that rejected the MMR vaccine was a major driver of these outbreaks, particularly in areas with high exemption rates [7,19].
- -
- The 2019 outbreak highlighted how communities with pockets of unvaccinated individuals can become hotspots for the spread of preventable diseases. In New York, for example, a large outbreak of measles occurred in Orthodox Jewish communities due to lower vaccination coverage [80].
-
- Polio Resurgence in Afghanistan and Pakistan:
- In Pakistan, religious and political opposition to vaccination efforts has resulted in persistent low vaccination rates, contributing to the continued circulation of the virus. In 2020, Pakistan reported 84 cases of polio, despite major efforts to eradicate the disease [83].
- Misinformation and conspiracy theories surrounding the safety of vaccines, often promoted by local political and religious leaders, have slowed vaccination campaigns, leaving entire regions vulnerable.
- iii.
- Diphtheria Outbreaks in Yemen:
- Resistance to immunization due to religious and cultural beliefs has also fueled the spread of preventable diseases, complicating efforts to eradicate diseases like diphtheria.
- B.
- Herd Immunity Challenges: The Consequences of Declining Vaccination Rates
-
The Declining Threshold for Herd Immunity
-
For diseases like measles, the required vaccination coverage to achieve herd immunity is about 95%. However, recent outbreaks have shown that many communities are falling below this threshold due to hesitancy and refusal.
- -
- For instance, in 2019, a significant portion of Europe and North America fell below the required coverage, leading to measles resurgence [85].
- -
- The impact of this was especially severe in the global South, where infrastructure challenges and lack of access to vaccines combined with hesitancy led to reduced coverage and a loss of herd immunity, particularly for diseases like polio and measles.
-
-
Impact on Immunization Programs
-
Declining Immunization Rates: A decline in vaccination rates, driven by hesitancy, weakens the immune buffer provided by herd immunity. As a result, diseases that were once controlled begin to re-emerge.
- -
- Polio in Afghanistan and Pakistan continues to circulate in regions where less than 80% of children are vaccinated [86]. This leads to localized outbreaks, delaying the global eradication of the disease.
- -
- Rubella and Congenital Rubella Syndrome (CRS), which were near-eliminated in many parts of the world, are on the rise due to incomplete vaccination coverage [87].
-
Increased Healthcare Burden: Resurgent diseases place a heavy burden on healthcare systems, especially in low-resource settings.
- -
- A study in Sub-Saharan Africa found that measles outbreaks caused unprecedented spikes in hospital admissions, putting pressure on an already strained healthcare infrastructure [88].
- -
- Additional resources are needed to contain outbreaks, manage the treatment of affected individuals, and address the public health consequences.
-
- C.
- Country-Specific Interventions and Lessons Learned: Review Successful Strategies
- i.
- Nigeria: Community Engagement in Vaccine Campaigns
-
The “Stop Polio Now” campaign in Nigeria successfully leveraged local religious and community leaders to engage skeptical populations [89].
- -
- In Northern Nigeria, where vaccine hesitancy was particularly pronounced, local imams and religious leaders were crucial in dispelling myths about the polio vaccine.
- -
- The integration of health campaigns with local governance and trusted community figures created a sense of ownership and accountability, increasing vaccination uptake.
- -
- By tailoring messages to local cultural and religious contexts, these interventions significantly reduced resistance and led to an increase in immunization rates.
- ii.
- Japan: Addressing Vaccine Safety Concerns
-
The Japanese Ministry of Health collaborated with medical professionals to provide clear and transparent information on vaccine efficacy and safety.
- -
- Public campaigns emphasized the importance of vaccination in preventing severe diseases like measles, rubella, and influenza, which had been resurging due to low immunization rates.
- -
- Japan saw a recovery in vaccine confidence after these initiatives, which helped restore high vaccination coverage [90].
- iii.
- Australia: National Immunization Programs
-
Australia implemented state-sponsored financial incentives for parents to vaccinate their children, alongside education campaigns about the importance of immunization.
- -
- These efforts resulted in one of the highest immunization rates globally, with coverage consistently above 90% for all childhood vaccines.
- -
- Australia's strategy of combining incentives with education was particularly effective in overcoming vaccine hesitancy, demonstrating the importance of government leadership in public health campaigns [91].
VII. Strategies to Combat Vaccine Hesitancy
- A.
- Public Health Communication Approaches: Effective Messaging Strategies
- i.
- Tailored Messaging and Audience Segmentation
- For example, parents of young children may be most concerned about vaccine safety, while older adults might be more focused on the effectiveness of vaccines in preventing severe disease.
-
Research on health communication has shown that framing messages to emphasize benefits, such as personal and community protection, resonates more strongly with hesitant populations than focusing on the risks of non-vaccination.
- -
- For example, the "Protect Yourself, Protect Your Community" framing effectively highlights the collective benefits of vaccination while addressing individual concerns.
- -
- Messages should also be empowering rather than coercive. In contrast to scare tactics or fear-based messaging, positive messages focusing on health, protection, and community solidarity have proven to be more persuasive.
- ii.
- Trust and Credibility of the Source
- Endorsements from healthcare providers have been shown to significantly increase vaccine acceptance, particularly when they engage in open and empathetic conversations about vaccine safety [92].
- Community leaders, particularly in marginalized groups, can help mitigate skepticism and reduce mistrust of vaccines. This is evident in Nigeria’s polio eradication campaigns, where local religious leaders served as trusted voices to advocate for vaccination [93].
- iii.
- Crisis Communication and Transparency
- In the case of COVID-19, open discussions about the rapid vaccine development process and post-vaccination monitoring helped reassure the public.
- Governments and health organizations should regularly share evidence regarding vaccine development, efficacy, and safety in an accessible and understandable manner.
- B.
- Community Engagement and Trust-Building: Grassroots Interventions
- i.
- Engaging Local Leaders and Influencers
- Religious leaders and community influencers are uniquely positioned to frame vaccination as part of community responsibility, often in alignment with religious or cultural values. For example, Islamic scholars in Pakistan have worked to dispel myths surrounding the polio vaccine, particularly in regions where religious concerns were a significant driver of vaccine hesitancy [95].
- ii.
- Health Education and Dialogue
- Health education programs that invite open discussions, rather than just broadcasting information, can reduce fear and suspicion. These programs should provide a space for individuals to express doubts, which health workers can then address in real time.
- Community vaccination champions trusted individuals who have received vaccines and can speak to their experience can also help normalize vaccination. These champions can bridge the gap between medical experts and the local population, fostering trust and encouraging peers to get vaccinated [96].
- C.
- Combating Misinformation: The Role of AI and Fact-Checking Initiatives
- i.
- AI-Driven Monitoring and Detection of Misinformation
- Social media platforms such as Twitter and Facebook have partnered with fact-checking organizations to monitor and remove vaccine-related misinformation [97].
- Additionally, AI algorithms can be used to detect patterns in misinformation and identify emerging anti-vaccine trends, enabling proactive intervention by public health authorities [98].
- Natural language processing (NLP) models can assist in identifying false claims by comparing them to verified databases, flagging content for human review and swift action [99].
- ii.
- Collaborative Fact-Checking Initiatives
- These organizations debunk misinformation by presenting evidence-based facts and highlighting the scientific consensus on vaccine safety and efficacy.
- Governments and health organizations should collaborate with these fact-checkers to counter misinformation at the source, especially by disseminating clear, concise, and accurate information that can be easily shared on social media platforms.
- Proactive messaging is equally important fact-checking organizations should not only react to misinformation but also disseminate correct information to prevent the spread of false narratives in the first place [100].
- D.
- Policy Recommendations: Evidence-Based Approaches to Increasing Vaccine Acceptance
- i.
- Mandatory Vaccination with Exemptions
- Countries like Australia and France have implemented no-jab, no-pay policies, which financially incentivize vaccination by limiting access to government benefits for unvaccinated individuals [101,102]. These policies should be implemented ethically and with sensitivity, ensuring that people are not alienated or punished for genuinely held concerns.
- ii.
- Incentives for Vaccination
- Culturally appropriate incentives are particularly effective in low-resource settings. In some African countries, vaccination cards that allow people to access other services have been used as a tool to increase vaccination uptake.
- iii.
- Strengthening Immunization Infrastructure
- Sociocultural Factors: The influence of religious beliefs, cultural norms, misinformation, and social media has been a critical factor in shaping vaccine hesitancy. In particular, misinformation and social media play a pivotal role in amplifying fear, spreading false narratives, and increasing distrust in vaccines. Additionally, historical medical injustices and the lack of trust in healthcare systems exacerbate vaccine resistance, especially in marginalized communities. Understanding and engaging these populations through culturally sensitive and empathetic communication is essential to addressing these challenges.
- Psychological Factors: Cognitive biases, risk perception, and fear are central to understanding vaccine hesitancy. Cognitive heuristics, such as availability bias and confirmation bias, affect how people interpret information related to vaccines. Furthermore, psychological barriers like fear and anxiety about vaccine safety contribute to reluctance. Behavioral frameworks like the Health Belief Model provide useful insights into understanding these psychological dynamics and developing tailored interventions to improve vaccine uptake.
- Political and Policy Factors: Government policies, political polarization, and economic influences also shape attitudes toward vaccination. The global response to COVID-19 highlighted the impact of political polarization on vaccine acceptance. Policies that are clear, transparent, and based on scientific evidence can significantly improve vaccine coverage. Moreover, trust in government health directives can be bolstered by policies that promote community engagement and equity in vaccine distribution.
- Impact on Immunization Programs: Vaccine hesitancy has led to disease outbreaks and undermined efforts to achieve herd immunity. The decline in vaccine coverage in some regions has contributed to the resurgence of preventable diseases, threatening public health efforts globally. Innovative country-specific interventions, such as community-led vaccination campaigns, have demonstrated success in overcoming hesitancy, proving that localized, culturally sensitive approaches are effective.
- Strategies to Combat Vaccine Hesitancy: Multi-pronged strategies that include effective communication, community engagement, and countering misinformation are vital in addressing hesitancy. Public health messaging must be transparent, empathetic, and delivered through trusted local influencers to counter misinformation. AI tools and fact-checking initiatives also play an essential role in debunking myths and providing the public with accurate, evidence-based information.
- The role of digital platforms and AI in spreading both misinformation and reliable information, and how these can be harnessed to combat hesitancy.
- Longitudinal studies examining the evolution of vaccine attitudes over time, particularly in response to major global health events like pandemics.
- Investigating the economic and policy factors influencing vaccine accessibility, equity, and uptake, especially in low-income settings where hesitancy may be compounded by systemic barriers to healthcare.
- The need to address vaccine hesitancy has never been more urgent. With emerging infectious diseases and ongoing challenges like COVID-19, global health experts, policymakers, and community leaders must prioritize addressing the root causes of vaccine hesitancy to safeguard public health.
- As we continue to face new threats from preventable diseases, a collaborative, interdisciplinary approach will be essential. Governments, global health organizations, and civil society must invest in targeted communication campaigns, community outreach programs, and policy reforms that empower individuals to make informed decisions about vaccination. Local communities must be at the center of these efforts, ensuring that interventions are culturally appropriate and resonate with the concerns of the people they aim to serve.
- To truly overcome vaccine hesitancy, stakeholders must not only focus on changing individual behaviors but also on transforming the systems that perpetuate mistrust. This requires a long-term commitment to building health system resilience, promoting health equity, and ensuring that vaccination programs are accessible, trustworthy, and well-resourced. As global health experts, it is our responsibility to amplify the voices of the marginalized, address misinformation, and champion vaccination as a global public good.
- Let us move forward with renewed determination, collaboration, and a shared commitment to overcoming vaccine hesitancy and achieving global health security for all. Together, we can build a future where vaccines protect the most vulnerable and prevent the resurgence of deadly diseases worldwide.
Author Contributions
Funding
Acknowledgments
Ethical Approval
Conflicts of Interest
References
- Ten threats to global health in 2019. n.d. Available online: https://www.who.int/news-room/spotlight/ten-threats-to-global-health-in-2019.
- Mahase, E. WHO warns “measles is back” as virus spreads across Europe, America, and Afghanistan. BMJ 2025, r528. [Google Scholar] [CrossRef]
- Sinuraya, R. K.; Nuwarda, R. F.; Postma, M. J.; Suwantika, A. A. Vaccine hesitancy and equity: lessons learned from the past and how they affect the COVID-19 countermeasure in Indonesia. Globalization and Health 2024, 20(1). [Google Scholar] [CrossRef]
- Kopel, J. An exploration of vaccination in the 19th century through the eyes of Dr. Albert Mackey. Baylor University Medical Center Proceedings 2022b, 35(4), 505–509. [Google Scholar] [CrossRef]
- History of polio vaccination. n.d. Available online: https://www.who.int/news-room/spotlight/history-of-vaccination/history-of-polio-vaccination.
- Taylor, B.; Miller, E.; Farrington, C.; Petropoulos, M.; Favot-Mayaud, I.; Li, J.; Waight, P. A. Autism and measles, mumps, and rubella vaccine: no epidemiological evidence for a causal association. The Lancet 1999b, 353(9169), 2026–2029. [Google Scholar] [CrossRef] [PubMed]
- Rao, T. S.; Andrade, C. The MMR vaccine and autism: Sensation, refutation, retraction, and fraud. Indian Journal of Psychiatry 2011b, 53(2), 95. [Google Scholar] [CrossRef]
- Kricorian, K.; Civen, R.; Equils, O. COVID-19 vaccine hesitancy: misinformation and perceptions of vaccine safety. Human Vaccines & Immunotherapeutics 2021, 18(1). [Google Scholar] [CrossRef] [PubMed]
- World Health Organization; WHO. Smallpox. 1 November 2019. Available online: https://www.who.int/health-topics/smallpox.
- United Kingdom Vaccination Act 1853 Policy Navigator. n.d. Available online: https://navigator.health.org.uk/theme/united-kingdom-vaccination-act-1853.
- Hussain, A.; Ali, S.; Ahmed, M.; Hussain, S. The Anti-vaccination movement: a regression in modern medicine; Cureus, 2018. [Google Scholar] [CrossRef]
- Strassburg, M. A. The global eradication of smallpox. American Journal of Infection Control 1982, 10(2), 53–59. [Google Scholar] [CrossRef]
- History of smallpox vaccination. n.d. Available online: https://www.who.int/news-room/spotlight/history-of-vaccination/history-of-smallpox-vaccination.
- Montero, D. A.; Vidal, R. M.; Velasco, J.; Carreño, L. J.; Torres, J. P.; M. a. B., O; Tovar-Rosero, Y.; Oñate, A. A.; O’Ryan, M. Two centuries of vaccination: historical and conceptual approach and future perspectives. Frontiers in Public Health 2024, 11. [Google Scholar] [CrossRef]
- Fitzpatrick, M. The cutter incident: How America’s first polio vaccine led to a growing vaccine crisis. 1 March 2006. Available online: https://pmc.ncbi.nlm.nih.gov/articles/PMC1383764/.
- Historical vaccine concerns Vaccine Safety. 31 July 2024. Available online: https://www.cdc.gov/vaccine-safety/historical-concerns/index.html.
- 50th anniversary of the Expanded Programme on Immunization (EPI). 1 January 2024. Available online: https://www.who.int/news-room/events/detail/2024/01/01/default-calendar/50th-anniversary-of-the-expanded-programme-on-immunization-(epi).
- Shattock, A. J.; Johnson, H. C.; Sim, S. Y.; Carter, A.; Lambach, P.; Hutubessy, R. C. W.; Thompson, K. M.; Badizadegan, K.; Lambert, B.; Ferrari, M. J.; Jit, M.; Fu, H.; Silal, S. P.; Hounsell, R. A.; White, R. G.; Mosser, J. F.; Gaythorpe, K. a. M.; Trotter, C. L.; Lindstrand, A.; Bar-Zeev, N. Contribution of vaccination to improved survival and health: modelling 50 years of the Expanded Programme on Immunization. The Lancet 2024, 403(10441), 2307–2316. [Google Scholar] [CrossRef]
- Eggertson, L. Lancet retracts 12-year-old article linking autism to MMR vaccines. Canadian Medical Association Journal 2010, 182(4), E199–E200. [Google Scholar] [CrossRef] [PubMed]
- Troiano, G.; Nardi, A. Vaccine hesitancy in the era of COVID-19. Public Health 2021, 194, 245–251. [Google Scholar] [CrossRef] [PubMed]
- Mir, S.; Mir, M. The mRNA vaccine, a swift warhead against a moving infectious disease target. Expert Review of Vaccines 2024, 23(1), 336–348. [Google Scholar] [CrossRef] [PubMed]
- Xu, J.; Wu, Z.; Wass, L.; Larson, H. J.; Lin, L. Mapping global public perspectives on mRNA vaccines and therapeutics. Npj Vaccines 2024, 9(1). [Google Scholar] [CrossRef] [PubMed]
- Caceres, M. M. F.; Sosa, J. P.; Lawrence, J. A.; Sestacovschi, C.; Tidd-Johnson, A.; Rasool, M. H. U.; Gadamidi, V. K.; Ozair, S.; Pandav, K.; Cuevas-Lou, C.; Parrish, M.; Rodriguez, I.; Fernandez, J. P. The impact of misinformation on the COVID-19 pandemic. AIMS Public Health 2022, 9(2), 262–277. [Google Scholar] [CrossRef]
- Bolsen, T.; Palm, R. Politicization and COVID-19 vaccine resistance in the U.S. In Progress in Molecular Biology and Translational Science; 2022; pp. 81–100. [Google Scholar] [CrossRef]
- Roat, C.; Webber-Ritchey, K. J.; Spurlark, R. S.; Lee, Y. Black Americans receiving the COVID-19 vaccine and Effective strategies to overcome barriers: An Integrative literature review. Journal of Racial and Ethnic Health Disparities 2022, 10(5), 2577–2587. [Google Scholar] [CrossRef]
- Anderson, K.; Creanza, N. A cultural evolutionary model of the interaction between parental beliefs and behaviors, with applications to vaccine hesitancy. Theoretical Population Biology 2023, 152, 23–38. [Google Scholar] [CrossRef]
- Tiwana, M. H.; Smith, J. Faith and vaccination: a scoping review of the relationships between religious beliefs and vaccine hesitancy. BMC Public Health 2024, 24(1). [Google Scholar] [CrossRef]
- Knol, M. J.; Urbanus, A. T.; Swart, E. M.; Mollema, L.; Ruijs, W. L.; Van Binnendijk, R. S.; Wierik, M. J. T.; De Melker, H. E.; Timen, A.; Hahné, S. J. Large ongoing measles outbreak in a religious community in the Netherlands since May 2013. Eurosurveillance 2013). Large ongoing measles outbreak in a religious community in the Netherlands since May 2013. Eurosurveillance, 18(36, 18(36). [Google Scholar] [CrossRef]
- Ittefaq, M.; Abwao, M.; Rafique, S. Polio vaccine misinformation on social media: turning point in the fight against polio eradication in Pakistan. Human Vaccines & Immunotherapeutics 2021, 17(8), 2575–2577. [Google Scholar] [CrossRef]
- Exline, J. J.; Pait, K. C.; Wilt, J. A.; Schutt, W. A. Demonic and Divine Attributions around COVID-19 Vaccines: Links with Vaccine Attitudes and Behaviors, QAnon and Conspiracy Beliefs, Anger, Spiritual Struggles, Religious and Political Variables, and Supernatural and Apocalyptic Beliefs. Religions 2022, 13(6), 519. [Google Scholar] [CrossRef]
- Morales-Campos, D. Y.; Zimet, G. D.; Kahn, J. A. Human papillomavirus vaccine hesitancy in the United States. Pediatric Clinics of North America 2023, 70(2), 211–226. [Google Scholar] [CrossRef] [PubMed]
- Muzembo, B. A.; Ntontolo, N. P.; Ngatu, N. R.; Khatiwada, J.; Suzuki, T.; Wada, K.; Kitahara, K.; Ikeda, S.; Miyoshi, S. Misconceptions and Rumors about Ebola Virus Disease in Sub-Saharan Africa: A Systematic Review. International Journal of Environmental Research and Public Health 2022, 19(8), 4714. [Google Scholar] [CrossRef] [PubMed]
- Endo, P. T.; Santos, G. L.; De Lima Xavier, M. E.; Campos, G. R. N.; De Lima, L. C.; Silva, I.; Egli, A.; Lynn, T. Illusion of Truth: Analysing and classifying COVID-19 fake news in Brazilian Portuguese language. Big Data and Cognitive Computing 2022, 6(2), 36. [Google Scholar] [CrossRef]
- Di Domenico, G.; Nunan, D.; Pitardi, V. Marketplaces of Misinformation: A study of how vaccine misinformation is legitimized on social media. Journal of Public Policy & Marketing 2022, 41(4), 319–335. [Google Scholar] [CrossRef]
- Winters, M.; Christie, S.; Melchinger, H.; Iddrisu, I.; Hassan, H. A.; Ewart, E.; Mosley, L.; Alhassan, R.; Shani, N.; Nyamuame, D.; Lepage, C.; Thomson, A.; Atif, A. N.; Omer, S. B. Debunking COVID-19 vaccine misinformation with an audio drama in Ghana, a randomized control trial. Scientific Reports 2025, 15(1). [Google Scholar] [CrossRef]
- About the untreated syphilis study at Tuskegee The U.S. Public Health Service Untreated Syphilis Study at Tuskegee. 4 September 2024. Available online: https://www.cdc.gov/tuskegee/about/index.html#:~:text=Background,found%20in%20the%20National%20Archives.&text=Group%20of%20men%20in%20Untreated,in%20research%20are%20ongoing%20today.
- Mayosi, B. M.; Benatar, S. R. Health and Health Care in South Africa — 20 Years after Mandela. New England Journal of Medicine 2014, 371(14), 1344–1353. [Google Scholar] [CrossRef]
- Steenberg, B.; Sokani, A.; Myburgh, N.; Mutevedzi, P.; Madhi, S. A. COVID-19 vaccination rollout: Aspects of hesitancy in South Africa. Vaccines 2023, 11(2), 407. [Google Scholar] [CrossRef]
- Mosby, I.; Swidrovich, J. Medical experimentation and the roots of COVID-19 vaccine hesitancy among Indigenous Peoples in Canada. Canadian Medical Association Journal 2021, 193(11), E381–E383. [Google Scholar] [CrossRef] [PubMed]
- Jourdain, O. Resistance to vaccination in France: History and the influence of social media. Journal of Gynecology Obstetrics and Human Reproduction 2020, 50(7), 101997. [Google Scholar] [CrossRef] [PubMed]
- Ali, H. A.; Hartner, A.; Echeverria-Londono, S.; Roth, J.; Li, X.; Abbas, K.; Portnoy, A.; Vynnycky, E.; Woodruff, K.; Ferguson, N. M.; Toor, J.; Gaythorpe, K. A. Vaccine equity in low and middle income countries: a systematic review and meta-analysis. International Journal for Equity in Health 2022, 21(1). [Google Scholar] [CrossRef]
- Pourrazavi, S.; Fathifar, Z.; Sharma, M.; Allahverdipour, H. COVID-19 vaccine hesitancy: A Systematic review of cognitive determinants. Health Promotion Perspectives 2023, 13(1), 21–35. [Google Scholar] [CrossRef] [PubMed]
- McKee, C.; Bohannon, K. Exploring the reasons behind parental refusal of vaccines. The Journal of Pediatric Pharmacology and Therapeutics 2016, 21(2), 104–109. [Google Scholar] [CrossRef] [PubMed]
- Lanyi, K.; Green, R.; Craig, D.; Marshall, C. COVID-19 Vaccine hesitancy: Analysing Twitter to identify barriers to vaccination in a low uptake region of the UK. Frontiers in Digital Health 2022, 3. [Google Scholar] [CrossRef]
- Biella, M.; Orrù, G.; Ciacchini, R.; Conversano, C.; Marazziti, D.; Gemignani, A. Anti-Vaccination Attitude and vaccination Intentions against COVID-19: A Retrospective Cross-Sectional Study investigating the role of media consumption. PubMed 2023, 20(4), 252–263. [Google Scholar] [CrossRef]
- Love, A. S.; Love, R. J. Considering Needle Phobia among Adult Patients During Mass COVID-19 Vaccinations. Journal of Primary Care & Community Health 2021, 12. [Google Scholar] [CrossRef]
- Rabail, R.; Ahmed, W.; Ilyas, M.; Rajoka, M. S. R.; Hassoun, A.; Khalid, A. R.; Khan, M. R.; Aadil, R. M. The Side Effects and Adverse Clinical Cases Reported after COVID-19 Immunization. Vaccines 2022, 10(4), 488. [Google Scholar] [CrossRef]
- Salman, M.; Mallhi, T. H.; Tanveer, N.; Shehzadi, N.; Khan, H. M.; Mustafa, Z. U.; Khan, T. M.; Hussain, K.; Mohamed, M. S.; Maqbool, F.; Aftab, R. A.; Butt, M. H.; Panda, D. S.; Alotaibi, N. H.; Khedr, A. I. M.; Alanazi, A. S.; Alatawi, A. D.; Alzarea, A. I.; Sulatana, K.; Khan, Y. H. Evaluation of Conspiracy Beliefs, Vaccine Hesitancy, and Willingness to Pay towards COVID-19 Vaccines in Six Countries from Asian and African Regions: A Large Multinational Analysis. Vaccines 2022, 10(11), 1866. [Google Scholar] [CrossRef]
- Blaskiewicz, R. The Big Pharma conspiracy theory. Medical Writing 2013b, 22(4), 259–261. [Google Scholar] [CrossRef]
- Achore, M.; Braimah, J. A.; Dowou, R. K.; Kuuire, V.; Ayanore, M. A.; Bisung, E. Institutional trust, conspiracy beliefs and Covid-19 vaccine uptake and hesitancy among adults in Ghana. PLOS Global Public Health 2024, 4(10), e0003852. [Google Scholar] [CrossRef] [PubMed]
- Foreign anti-vaccine disinformation spreads to West Africa First Draft. 2 September 2022. Available online: https://firstdraftnews.org/long-form-article/foreign-anti-vaccine-disinformation-reaches-west-africa/.
- Islam, M. S.; Kamal, A. M.; Kabir, A.; Southern, D. L.; Khan, S. H.; Hasan, S. M. M.; Sarkar, T.; Sharmin, S.; Das, S.; Roy, T.; Harun, M. G. D.; Chughtai, A. A.; Homaira, N.; Seale, H. COVID-19 vaccine rumors and conspiracy theories: The need for cognitive inoculation against misinformation to improve vaccine adherence. PLoS ONE 2021, 16(5), e0251605. [Google Scholar] [CrossRef]
- Shen, A. K.; Browne, S.; Srivastava, T.; Kornides, M. L.; Tan, A. S. Trusted messengers and trusted messages: The role for community-based organizations in promoting COVID-19 and routine immunizations. Vaccine 2023, 41(12), 1994–2002. [Google Scholar] [CrossRef]
- Zampetakis, L. A.; Melas, C. The health belief model predicts vaccination intentions against COVID-19: A survey experiment approach. Applied Psychology Health and Well-Being 2021, 13(2), 469–484. [Google Scholar] [CrossRef] [PubMed]
- Cucchiarini, V.; Lunn, P.; Robertson, D.; Viale, R. Using social and behavioral science to support COVID-19 pandemic response. In Springer eBooks; 2023; pp. 1–41. [Google Scholar] [CrossRef]
- Greyson, D.; Vriesema-Magnuson, C.; Bettinger, J. A. Impact of school vaccination mandates on pediatric vaccination coverage: a systematic review. CMAJ Open 2019, 7(3), E524–E536. [Google Scholar] [CrossRef]
- Farina, S.; Maio, A.; Gualano, M. R.; Ricciardi, W.; Villani, L. Childhood Mandatory Vaccinations: Current Situation in European Countries and Changes Occurred from 2014 to 2024. Vaccines 2024, 12(11), 1296. [Google Scholar] [CrossRef]
- Bednarczyk, R. A.; King, A. R.; Lahijani, A.; Omer, S. B. Current landscape of nonmedical vaccination exemptions in the United States: impact of policy changes. Expert Review of Vaccines 2018b, 18(2), 175–190. [Google Scholar] [CrossRef]
- Kaushik, A.; Fomicheva, J.; Boonstra, N.; Faber, E.; Gupta, S.; Kest, H. Pediatric vaccine hesitancy in the United States—The growing problem and strategies for management including motivational interviewing. Vaccines 2025, 13(2), 115. [Google Scholar] [CrossRef] [PubMed]
- Vicentini, C.; Garzaro, G.; Cornio, A. R.; Bosio, D.; Bergamaschi, E.; Parravicini, G. P.; Zotti, C. M. The Italian policy of mandating SARS-CoV-2 vaccination for healthcare workers: Analysis of the policy processes and preliminary outcomes. Health Policy 2022, 128, 49–54. [Google Scholar] [CrossRef] [PubMed]
- Larson, H. J.; Clarke, R. M.; Jarrett, C.; Eckersberger, E.; Levine, Z.; Schulz, W. S.; Paterson, P. Measuring trust in vaccination: A systematic review. Human Vaccines & Immunotherapeutics 2018, 14(7), 1599–1609. [Google Scholar] [CrossRef]
- Warraich, H. J. Religious opposition to polio vaccination. Emerging Infectious Diseases 2009, 15(6), 978a–9978. [Google Scholar] [CrossRef] [PubMed]
- Ezezika, O.; Mengistu, M.; Opoku, E.; Farheen, A.; Chauhan, A.; Barrett, K. What are the barriers and facilitators to polio vaccination and eradication programs? A systematic review. PLOS Global Public Health 2022, 2(11), e0001283. [Google Scholar] [CrossRef]
- Motta, M. Republicans, not Democrats, are more likely to endorse Anti-Vaccine misinformation. American Politics Research 2021, 49(5), 428–438. [Google Scholar] [CrossRef]
- Lim, J.; Moon, K. Political ideology and trust in government to ensure vaccine safety: Using a U.S. survey to explore the role of political trust. International Journal of Environmental Research and Public Health 2023, 20(5), 4459. [Google Scholar] [CrossRef] [PubMed]
- Razafindrakoto, M.; Roubaud, F.; Castilho, M. R.; Pero, V.; Saboia, J. Investigating the ‘Bolsonaro effect’ on the spread of the Covid-19 pandemic: An empirical analysis of observational data in Brazil. PLoS ONE 2024, 19(4), e0288894. [Google Scholar] [CrossRef] [PubMed]
- Statement from WHO and UNICEF on the Tetanus Vaccine in Kenya | WHO | Regional Office for Africa. WHO | Regional Office for Africa. 13 March 2025. Available online: https://www.afro.who.int/news/statement-who-and-unicef-tetanus-vaccine-kenya.
- Costa-Font, J.; Garcia-Hombrados, J.; Nicińska, A. The institutional origins of vaccines distrust: Evidence from former-Soviet countries. PLoS ONE 2023, 18(3), e0282420. [Google Scholar] [CrossRef]
- Market Information for Access Initiative (MI4A). Global vaccine market report 2024. VACCINES. 2024. Available online: https://cdn.who.int/media/docs/default-source/immunization/mi4a/who_global_vaccine_market_report_2024_vdraft.pdf?sfvrsn=d7bffd94_5&download=true.
- Van Zee, A. The promotion and marketing of OxyContin: commercial triumph, public health tragedy. American Journal of Public Health 2008, 99(2), 221–227. [Google Scholar] [CrossRef]
- Crofts, P.; Van Rijswijk, H. The horror of corporate harms: purdue pharma and the opioid epidemic. Crime Law and Social Change 2024, 82(4), 935–960. [Google Scholar] [CrossRef]
- Schwartz, J. L. The first rotavirus vaccine and the politics of acceptable risk. Milbank Quarterly 2012, 90(2), 278–310. [Google Scholar] [CrossRef]
- Operation Warp Speed: Accelerated COVID-19 vaccine development status and efforts to address manufacturing challenges. U.S. GAO, 11 February 2021. Available online: https://www.gao.gov/products/gao-21-319.
- Guan, Y. The effectiveness of coercive measures in motivating vaccination: Evidence from China during the COVID-19 pandemic. Global Public Health 2025, 20(1). [Google Scholar] [CrossRef]
- Officer, T. N.; McKinlay, E.; Imlach, F.; Kennedy, J.; Churchward, M.; McBride-Henry, K. Experiences of New Zealand public health messaging while in lockdown. Australian and New Zealand Journal of Public Health 2022, 46(6), 735–737. [Google Scholar] [CrossRef]
- Da Fonseca, E. M.; Nattrass, N.; Lazaro, L. L. B.; Bastos, F. I. Political discourse, denialism and leadership failure in Brazil’s response to COVID-19. Global Public Health 2021, 16(8–9), 1251–1266. [Google Scholar] [CrossRef]
- Thompson, M. R. Brute force governance: public approval despite policy failure during the COVID-19 pandemic in the Philippines. Journal of Current Southeast Asian Affairs 2022, 41(3), 399–421. [Google Scholar] [CrossRef]
- Petersen, M. B.; Jørgensen, F.; Lindholt, M. F. Did the European suspension of the AstraZeneca vaccine decrease vaccine acceptance during the COVID-19 pandemic? Vaccine 2021, 40(4), 558–561. [Google Scholar] [CrossRef]
- Measles cases and outbreaks Measles (Rubeola). 14 March 2025. Available online: https://www.cdc.gov/measles/data-research/index.html.
- McDonald, R.; Ruppert, P. S.; Souto, M.; Johns, D. E.; McKay, K.; Bessette, N.; McNulty, L. X.; Crawford, J. E.; Bryant, P.; Mosquera, M. C.; Frontin, S.; Deluna-Evans, T.; Regenye, D. E.; Zaremski, E. F.; Landis, V. J.; Sullivan, B.; Rumpf, B. E.; Doherty, J.; Sen, K.; Zucker, H. A. Notes from the Field: Measles Outbreaks from Imported Cases in Orthodox Jewish Communities — New York and New Jersey, 2018–2019. MMWR Morbidity and Mortality Weekly Report 2019, 68(19), 444–445. [Google Scholar] [CrossRef]
- GPEI-Hamid Jafari: the polio endgame and its challenges. n.d. Available online: https://polioeradication.org/news-categories/wpv/#:~:text=Afghanistan%20shares%20many%20of%20these,it%20will%20stay%20that%20way.
- Siddiqui, E.; Khalid, M.; Khan, M. S.; Waafira, A. Polio resurgence in Pakistan: unraveling the causes and addressing the consequences. Infection Ecology & Epidemiology 2024, 15(1). [Google Scholar] [CrossRef] [PubMed]
- Mbaeyi, C.; Baig, S.; Khan, Z.; Young, H.; Kader, M.; Jorba, J.; Safdar, M. R.; Jafari, H.; Franka, R. Progress toward Poliomyelitis Eradication — Pakistan, January 2020–July 2021. MMWR Morbidity and Mortality Weekly Report 2021, 70(39), 1359–1364. [Google Scholar] [CrossRef] [PubMed]
- Al-Dar, A. A.; Al-Qassimi, M.; Ezzadeen, F. H.; Qassime, M.; Murtadha, A. M. A.; Ghaleb, Y. Diphtheria resurgence in Sada’a-Yemen, 2017–2020. BMC Infectious Diseases 2022, 22(1). [Google Scholar] [CrossRef]
- Parums, D. V. A Review of the Resurgence of Measles, a Vaccine-Preventable Disease, as Current Concerns Contrast with Past Hopes for Measles Elimination. Medical Science Monitor 2024, 30. [Google Scholar] [CrossRef] [PubMed]
- World Health Organization; WHO. Pakistan and Afghanistan: the final wild poliovirus bastion. 4 January 2019a. Available online: https://www.who.int/news-room/feature-stories/detail/pakistan-and-afghanistan-the-final-wild-poliovirus-bastion.
- Ou, A. C.; Zimmerman, L. A.; Alexander, J. P.; Crowcroft, N. S.; O’Connor, P. M.; Knapp, J. K. Progress toward rubella and Congenital rubella Syndrome Elimination — Worldwide, 2012–2022. MMWR Morbidity and Mortality Weekly Report 2024, 73(8), 162–167. [Google Scholar] [CrossRef]
- Nchasi, G.; Paul, I. K.; Sospeter, S. B.; Mallya, M. R.; Ruaichi, J.; Malunga, J. Measles outbreak in sub-Saharan Africa amidst COVID-19: A rising concern, efforts, challenges, and future recommendations. Annals of Medicine and Surgery 2022, 81. [Google Scholar] [CrossRef]
- World Health Organization; Governments of Nigeria; Pakistan and Afghanistan. GLOBAL EMERGENCY ACTION PLAN 2012-2013 Action to stop polio now in Nigeria, Pakistan and Afghanistan. 2012. Available online: https://polioeradication.org/wp-content/uploads/2016/07/2.5_7IMB.pdf.
- Hosoda, M. Vaccine hesitancy in Japan: From a perspective on medical uncertainty and Trans-Scientific Theory. F1000Research 2023, 11, 1103. [Google Scholar] [CrossRef]
- Commonwealth of Australia; Department of Health; Department of Health. National Immunisation Strategy for Australia 2019–2024. Report No. 12231; National Immunisation Strategy for Australia 2019–2024. 2019. [Google Scholar]
- Fisher, K. A.; Nguyen, N.; Fouayzi, H.; Singh, S.; Crawford, S.; Mazor, K. M. Impact of a physician recommendation on COVID-19 vaccination intent among vaccine hesitant individuals. Patient Education and Counseling 2022, 106, 107–112. [Google Scholar] [CrossRef]
- GPEI-Religious leaders fuelling demand for polio vaccines and health services in Nigeria. n.d. Available online: https://polioeradication.org/news/religious-leaders-fuelling-demand-for-polio-vaccines-and-health-services-in-nigeria/.
- Nasir, S.; Aliyu, G.; Ya’u, I.; Gadanya, M.; Mohammad, M.; Zubair, M.; El-Kamary, S. S. From intense rejection to advocacy: How Muslim clerics were engaged in a polio eradication initiative in northern Nigeria. PLoS Medicine 2014, 11(8), e1001687. [Google Scholar] [CrossRef]
- User, S. In Pakistan, religious leaders help change misconceptions about the polio vaccine. n.d. Available online: https://www.endpolio.com.pk/media-room/field-stories/in-pakistan-religious-leaders-help-change-misconceptions-about-the-polio-vaccine.
- Kaufman, J.; Overmars, I.; Leask, J.; Seale, H.; Chisholm, M.; Hart, J.; Jenkins, K.; Danchin, M. Vaccine Champions Training Program: Empowering community Leaders to advocate for COVID-19 vaccines. Vaccines 2022, 10(11), 1893. [Google Scholar] [CrossRef]
- Broniatowski, D. A.; Simons, J. R.; Gu, J.; Jamison, A. M.; Abroms, L. C. The efficacy of Facebook’s vaccine misinformation policies and architecture during the COVID-19 pandemic. Science Advances 2023b, 9(37). [Google Scholar] [CrossRef]
- Gawande, M. S.; Zade, N.; Kumar, P.; Gundewar, S.; Weerarathna, I. N.; Verma, P. The role of artificial intelligence in pandemic responses: from epidemiological modeling to vaccine development. Molecular Biomedicine 2025, 6(1). [Google Scholar] [CrossRef] [PubMed]
- Boulieris, P.; Pavlopoulos, J.; Xenos, A.; Vassalos, V. Fraud detection with natural language processing. Machine Learning 2023, 113(8), 5087–5108. [Google Scholar] [CrossRef]
- Porter, E.; Wood, T. J. The global effectiveness of fact-checking: Evidence from simultaneous experiments in Argentina, Nigeria, South Africa, and the United Kingdom. Proceedings of the National Academy of Sciences 2021, 118(37). [Google Scholar] [CrossRef]
- Gravagna, K.; Becker, A.; Valeris-Chacin, R.; Mohammed, I.; Tambe, S.; Awan, F. A.; Toomey, T. L.; Basta, N. E. Global assessment of national mandatory vaccination policies and consequences of non-compliance. Vaccine 2020, 38(49), 7865–7873. [Google Scholar] [CrossRef] [PubMed]
- Burns, S.; Bhoyroo, R.; Leavy, J. E.; Portsmouth, L.; Millar, L.; Jancey, J.; Hendriks, J.; Saltis, H.; Tohotoa, J.; Pollard, C. The impact of the no jab no play and no jab no pay legislation in Australia: a scoping review. International Journal of Environmental Research and Public Health 2023, 20(13), 6219. [Google Scholar] [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




