Submitted:
02 March 2026
Posted:
03 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
Study Design
Setting and Participants
Interventions
Statistical Analysis
3. Results
3.1. Demographics
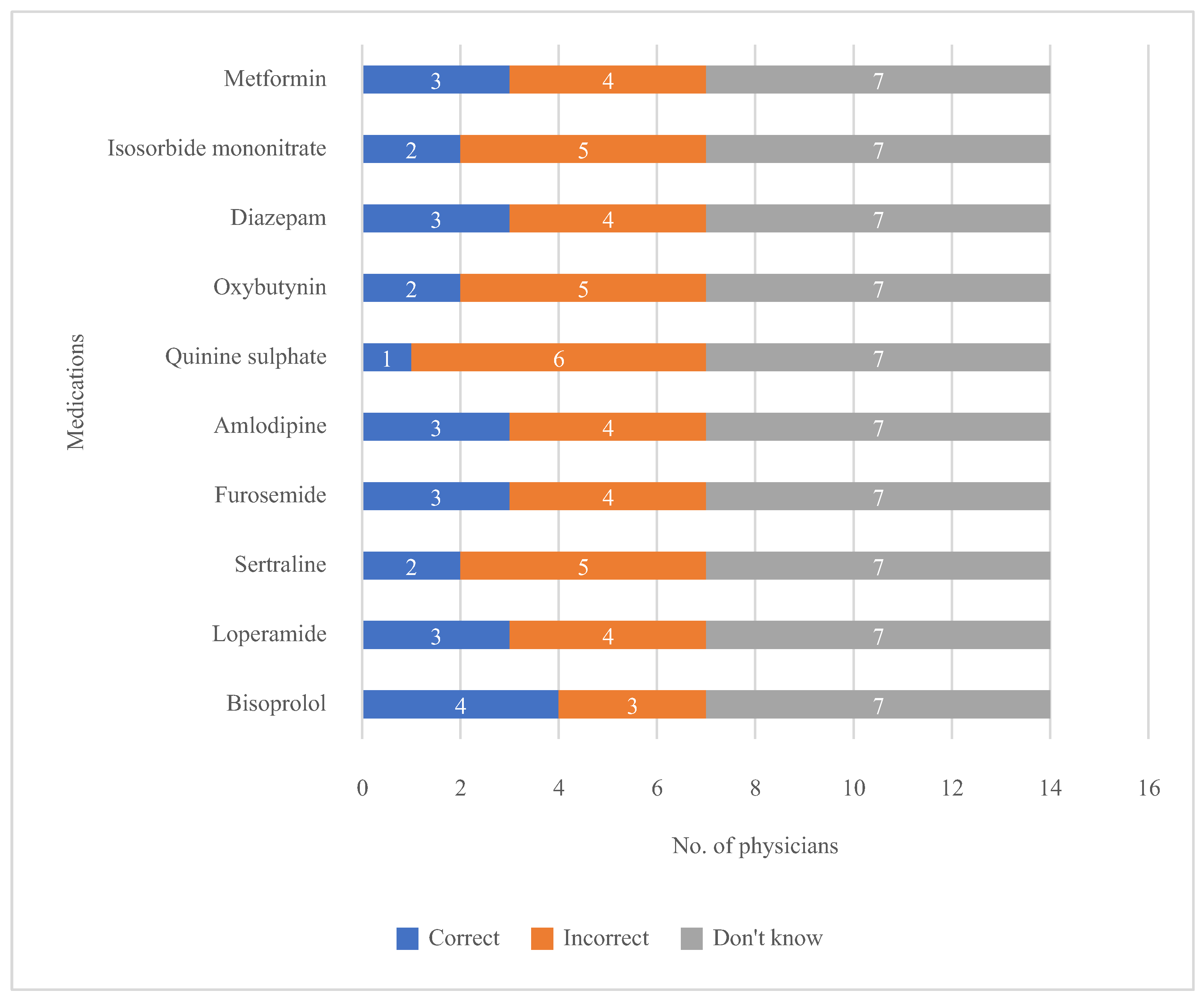
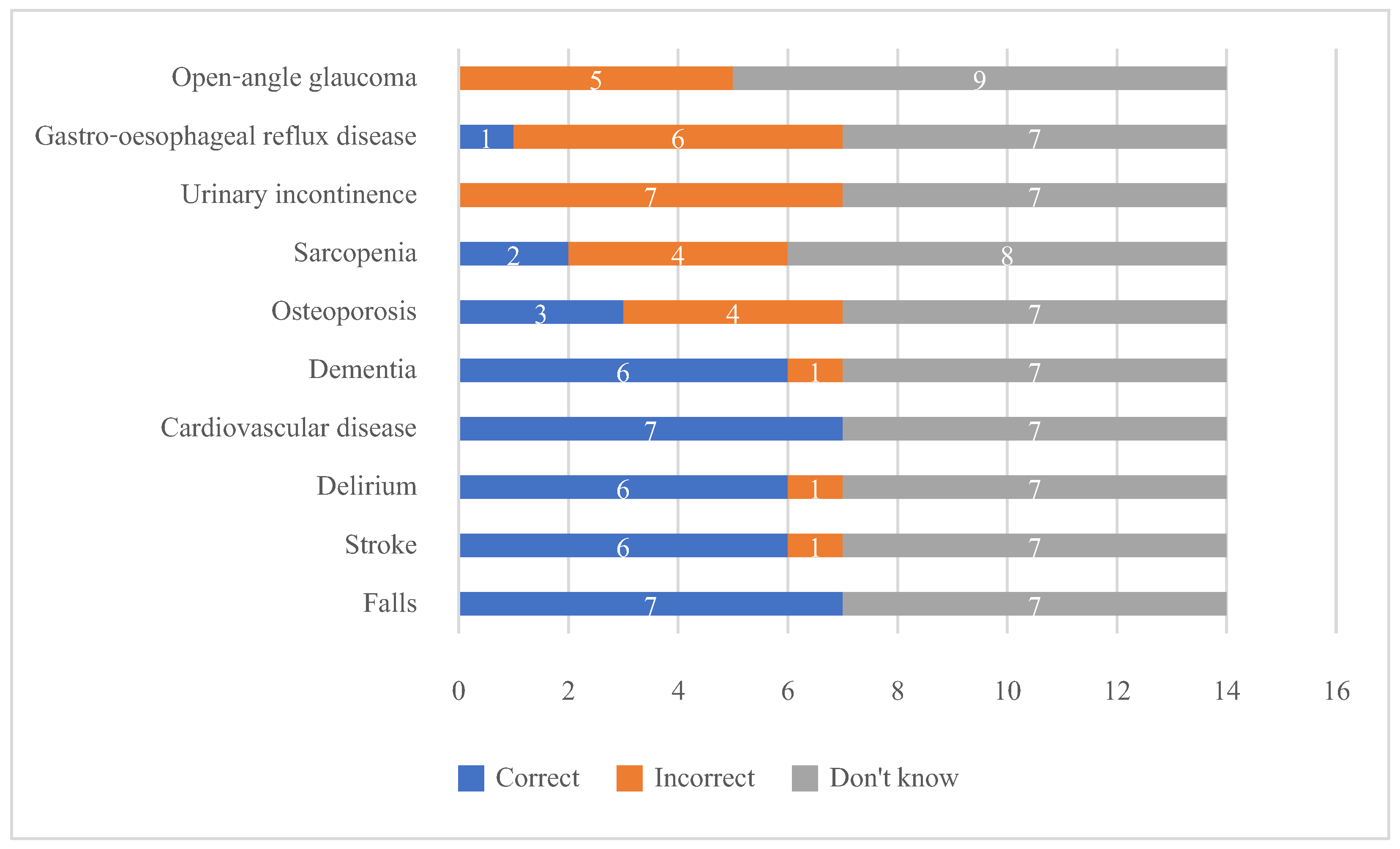
3.2. Knowledge
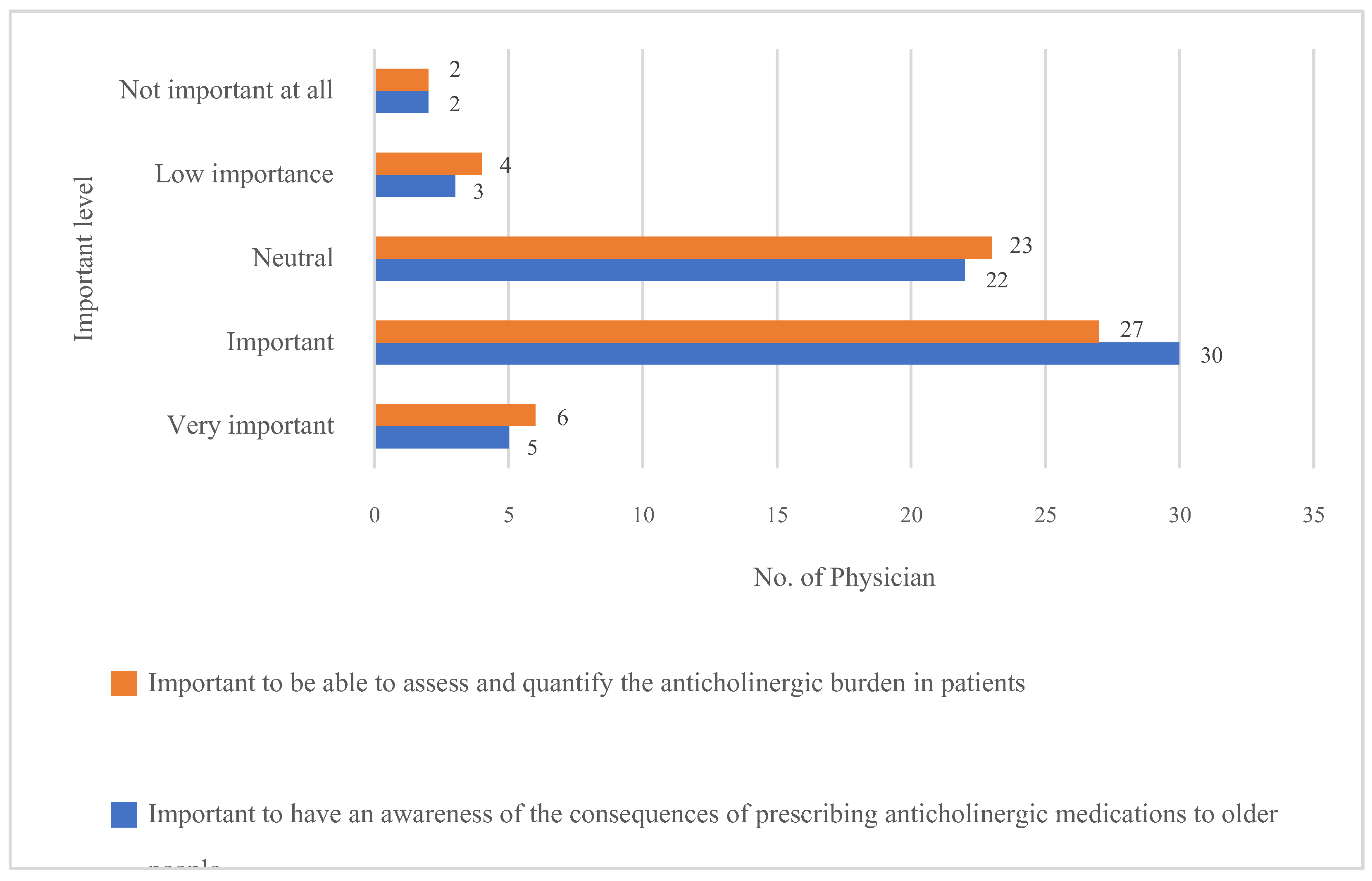
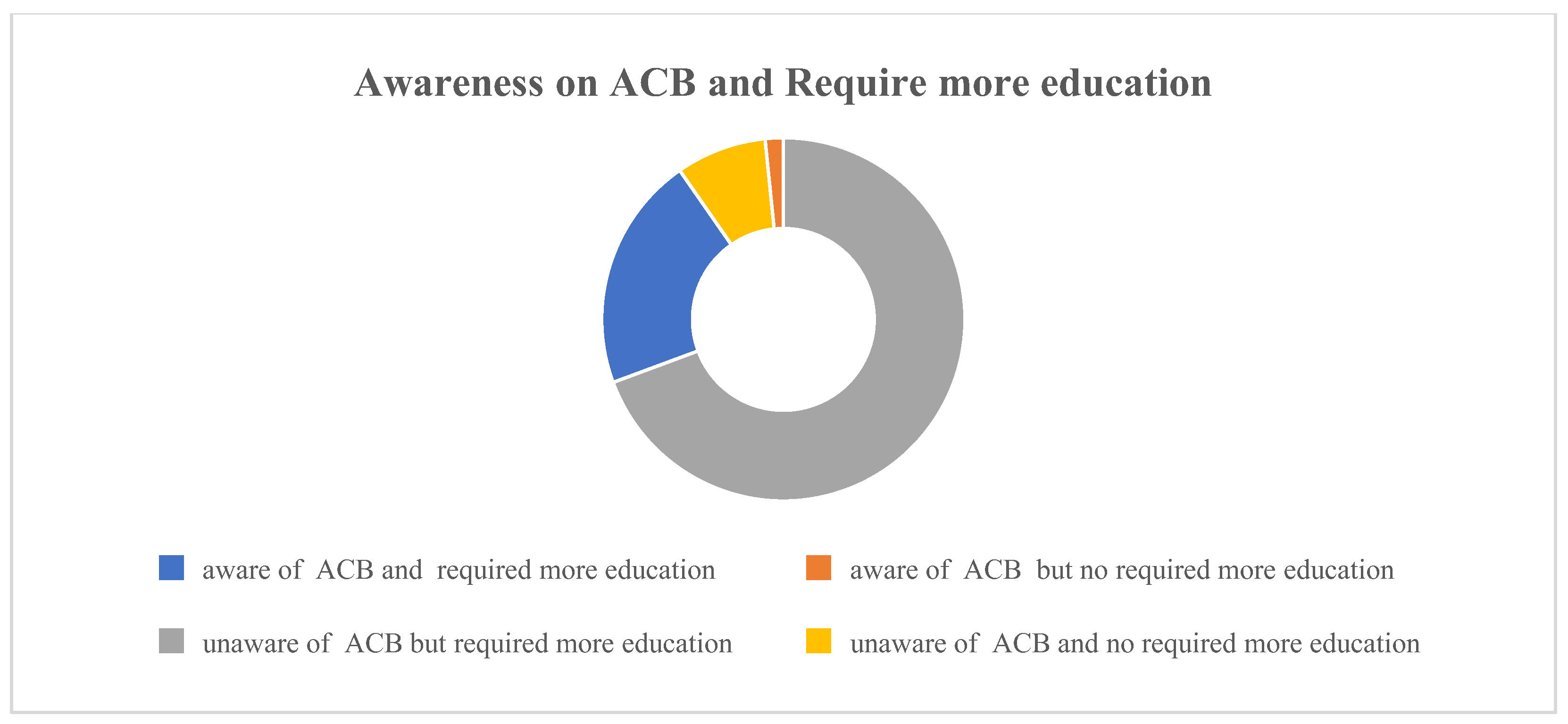
3.3. Attitude
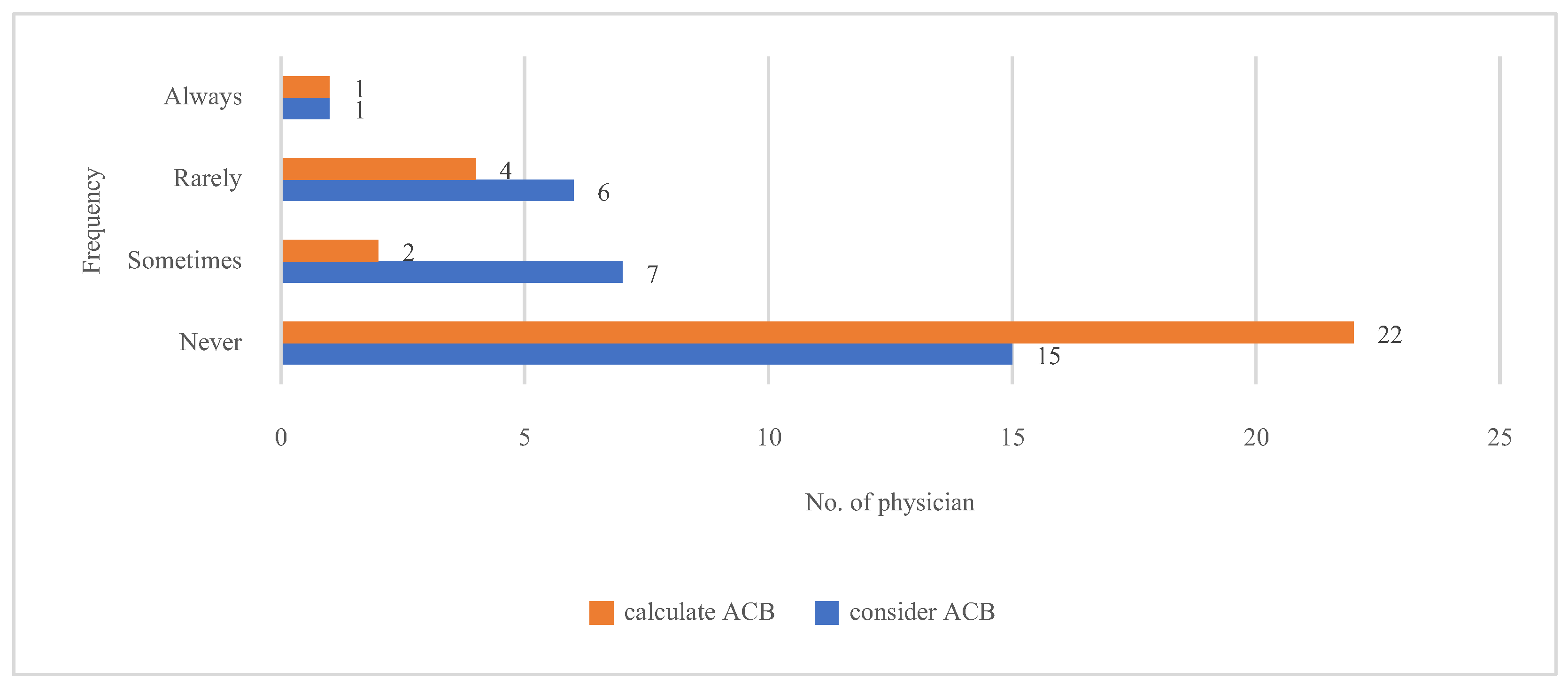
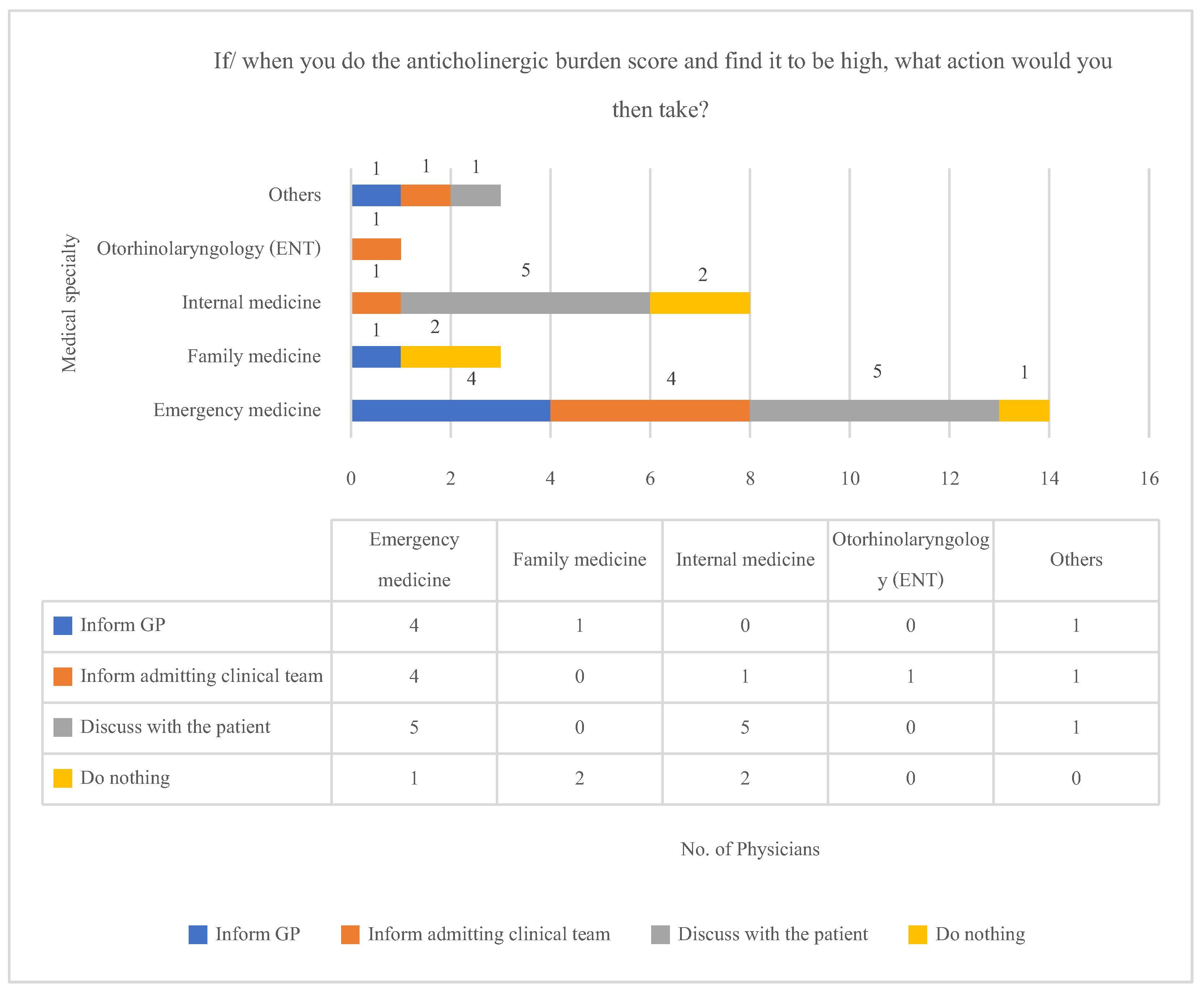
3.4. Practice
4. Discussion
5. Conclusions
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
Abbreviations
| ACB | Anticholinergic burden |
| ACoB | Anticholinergic Cognitive Burden |
| DBI | Drug Burden Index |
| REDCap | Research Electronic Data Capture |
References
- Suresh, A.V.; Sargent, P. Reducing anti-cholinergic burden in older patients. Clin Med (Lond) 2022, 22 (Suppl 4), 75–76. [Google Scholar] [CrossRef] [PubMed]
- Hilmer, S.N.; Gnjidic, D. The anticholinergic burden: From research to practice. Aust Prescr. 2022, 45(4), 118–120. [Google Scholar] [CrossRef] [PubMed]
- Hay-Smith, J.; Herbison, P.; Ellis, G.; Moore, K. Anticholinergic drugs versus placebo for overactive bladder syndrome in adults. Cochrane Database Syst Rev 2002, (3), CD003781. [Google Scholar] [CrossRef]
- Hilmer, S.N.; Mager, D.E.; Simonsick, E.M.; Cao, Y.; Ling, S.M.; Windham, B.G.; et al. A drug burden index to define the functional burden of medications in older people. Arch Intern Med. 2007, 167(8), 781–787. [Google Scholar] [CrossRef] [PubMed]
- Lee C.Y.; Cheng Y.D.; Cheng W.Y.; Tsai T.H.; Huang K.H. The prevalence of anticholinergic drugs and correlation with pneumonia in elderly patients: A population-based study in Taiwan. Int J Environ Res Public Health. 2020;17(17):6260. Published 2020 Aug 28. [CrossRef] [PubMed]
- Huang, W.; Yang, A.S.; Tsai, D.H.; Shao, S.; Lin, S.; Lai, E.C.; et al. Association between recently raised anticholinergic burden and risk of acute cardiovascular events: Nationwide case-case-time-control study. BMJ 2023, 382, e076045. [Google Scholar] [CrossRef] [PubMed]
- Liu, Y.P.; Chien, W.C.; Chung, C.H.; Chang, H.A.; Kao, Y.C.; Tzeng, N.S. Are anticholinergic medications associated with increased risk of dementia and behavioral and psychological symptoms of dementia? A Nationwide 15-Year Follow-Up Cohort Study in Taiwan. Front Pharmacol. Published. 2020, 11, 30. [Google Scholar] [CrossRef] [PubMed]
- Phutietsile, G.O.; Nishtala, P.S. Rethinking anticholinergic burden in older adults: Innovative approaches to detection and management. Expert Review of Clinical Pharmacology 2025, 18(8), 551–562. [Google Scholar] [CrossRef] [PubMed]
- Dilokthornsakul, P.; Stewart, C.; Moss, P.; Soiza, R.L.; Birse, F.; Subbarayan, S.; et al. Evaluating the Anticholinergic Burden in Older Patients: Comprehensive Insights from a Nationwide Survey Among Emergency Medicine Specialists in the UK. Geriatrics (Basel) Published. 2025, 10(6), 137. [Google Scholar] [CrossRef] [PubMed]
- Harris, P.A.; Taylor, R.; Minor, B.L.; Elliott, V.; Fernandez, M.; O’Neal, L.; et al. The REDCap consortium: Building an international community of software platform partners. J Biomed Inform. 2019, 95, 103208. [Google Scholar] [CrossRef] [PubMed]
- Tran Y.; Liao H.H.; Yeh E.H.; Ellis L.A.; Clay-Williams R.; Braithwaite J. Examining the pathways by which work-life balance influences safety culture among healthcare workers in Taiwan: Path analysis of data from a cross-sectional survey on patient safety culture among hospital staff. BMJ Open. 2021;11(11):e054143. Published 2021 Nov 2. [CrossRef] [PubMed]
- Anticholinergic Burden Calculator. Available online: https://www.acbcalc.com (accessed on 29 March 2024).
- Lozano-Ortega, G.; Johnston, K.M.; Cheung, A.; Wagg, A.; Campbell, N.L.; Dmochowski, R.; et al. A review of published anticholinergic scales and measures and their applicability in database analyses. Arch Gerontol Geriatr. 2020, 87, 103885. [Google Scholar] [CrossRef] [PubMed]
- Tiranaprakij, P.; Srisuma, S.; Putthipokin, K.; Ruangritchankul, S. Anticholinergic burden and clinical outcomes among older adults admitted in a tertiary hospital: A prospective cohort study. PLoS ONE. 2025, 20(9), E0332946. [Google Scholar] [CrossRef] [PubMed]
| Medical specialty |
Hospital classification |
No. of Physicians |
No. Physicians who are aware of ACB | |
|---|---|---|---|---|
| Yes | No | |||
| Emergency medicine | Medical center | 27 | 3 | 24 |
| Regional hospital | 3 | 1 | 2 | |
| District hospital | 1 | 1 | 0 | |
| Clinic | 1 | 1 | 0 | |
| Family Medicine | Medical center | 6 | 1 | 5 |
| Clinic | 1 | 1 | 0 | |
| Internal Medicine | Medical center | 7 | 1 | 6 |
| Regional hospital | 2 | 1 | 1 | |
| Orthopedics | Medical center | 1 | 0 | 1 |
| Otorhinolaryngology (ENT) | Medical center | 1 | 1 | 0 |
| Rehabilitation Medicine | Clinic | 1 | 0 | 1 |
| Others | Medical center | 9 | 3 | 6 |
| Clinic | 2 | 0 | 2 | |
| Total | 62 | 14 | 48 | |
| Medication | ACB score | |
|---|---|---|
| Bisoprolol | 0 | |
| Quinine sulphate | 0 | |
| Furosemide | 0 | |
| Amlodipine | 0 | |
| Sertraline | 0 | |
| Metformin | 1 | |
| Diazepam | 1 | |
| Isosorbide mononitrate | 1 | |
| Loperamide | 1 | |
| Oxybutynin | 3 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




