1. Introduction
The opioid crisis in the US population has been marked by a significant rise in invasive infections attributed to substance use, like infective endocarditis, with corresponding rise in healthcare utilization and costs related to management of these infections [
1,
2]. Among people who inject drugs (PWID), infective endocarditis (IE) is a serious infectious complication and commonly involves the tricuspid valve (TV) [
3,
4]. Many patients need surgical management of their IE however this approach is associated with high rates of adverse clinical outcomes, including recurrent IE, need for reintervention and mortality, especially in setting of untreated substance use disorder (SUD) [
5,
6,
7]. Vacuum-assisted percutaneous mechanical aspiration (PMA) which enables percutaneous debulking of valvular vegetations, has emerged as a potential nonoperative strategy for source control. Initially approved by the U.S. Food and Drug Administration in 2014 for intravascular thrombus removal PMA has since been utilized for aspiration of right atrial thrombi, with growing interest in its role in managing TV IE.
Emerging data suggest that PMA may offer favorable short-term outcomes in selected patients. One systematic review of 44 studies including 301 patients reported clinical success in 79.1% and survival rate of 89.7% in patients undergoing PMA [
8]. A single center study reported a 60%-100% decrease in vegetation size with a 100% clearance of bacteremia post PMA [
9]. In a retrospective cohort study, El-Dalati et al. found no difference in 30-day and 1-year mortality of patients who underwent surgical intervention compared with PMA [
10].
Our study aims to describe the real-world outcomes of PWID hospitalized with TV IE at an urban hospital between 2016 and 2025 who were treated either with a PMA procedure or surgical intervention (i.e., TV repair/replacement).
2. Methods
This study was a retrospective cohort of PWID admitted to the University of Maryland Medical Center with infective endocarditis of the TV who underwent an isolated TV procedure between January 2016 and September 2025. The study was reviewed by the University of Maryland’s Institutional Review Board and deemed exempt from full review.
Patients were identified from the Adult Cardiac Surgery registry through the Society of Thoracic Surgeons (STS) database. This list was cross referenced with an electronic health record data search using diagnostic codes for endocarditis of the TV from the International Classification of Diseases, tenth revision (ICD-10). Patients treated with PMA were further identified using Current Procedural Terminology (CPT) codes for percutaneous thrombectomy atrial/ventricular thrombus removal, corresponding ICD-10 Procedure Coding System (PCS) codes, and associated Medicare Severity Diagnosis Related Groups (DRG) categories. These patients were matched to ICD-10 diagnosis codes for SUD associated with injection drug use (
Table S1).
For a comparison group, we identified patients undergoing isolated TV surgery at our site from the STS adult cardiac surgery database. The list was refined to include only those patients who had a co-morbid SUD diagnosis code and underwent an isolated TV procedure. Patients were excluded if they underwent procedures involving other cardiac valves or concomitant procedures, such as pacemaker lead insertion, lead extraction, pacemaker placement, procedure for atrial fibrillation, or repair of patent foramen ovale during the same operative encounter.
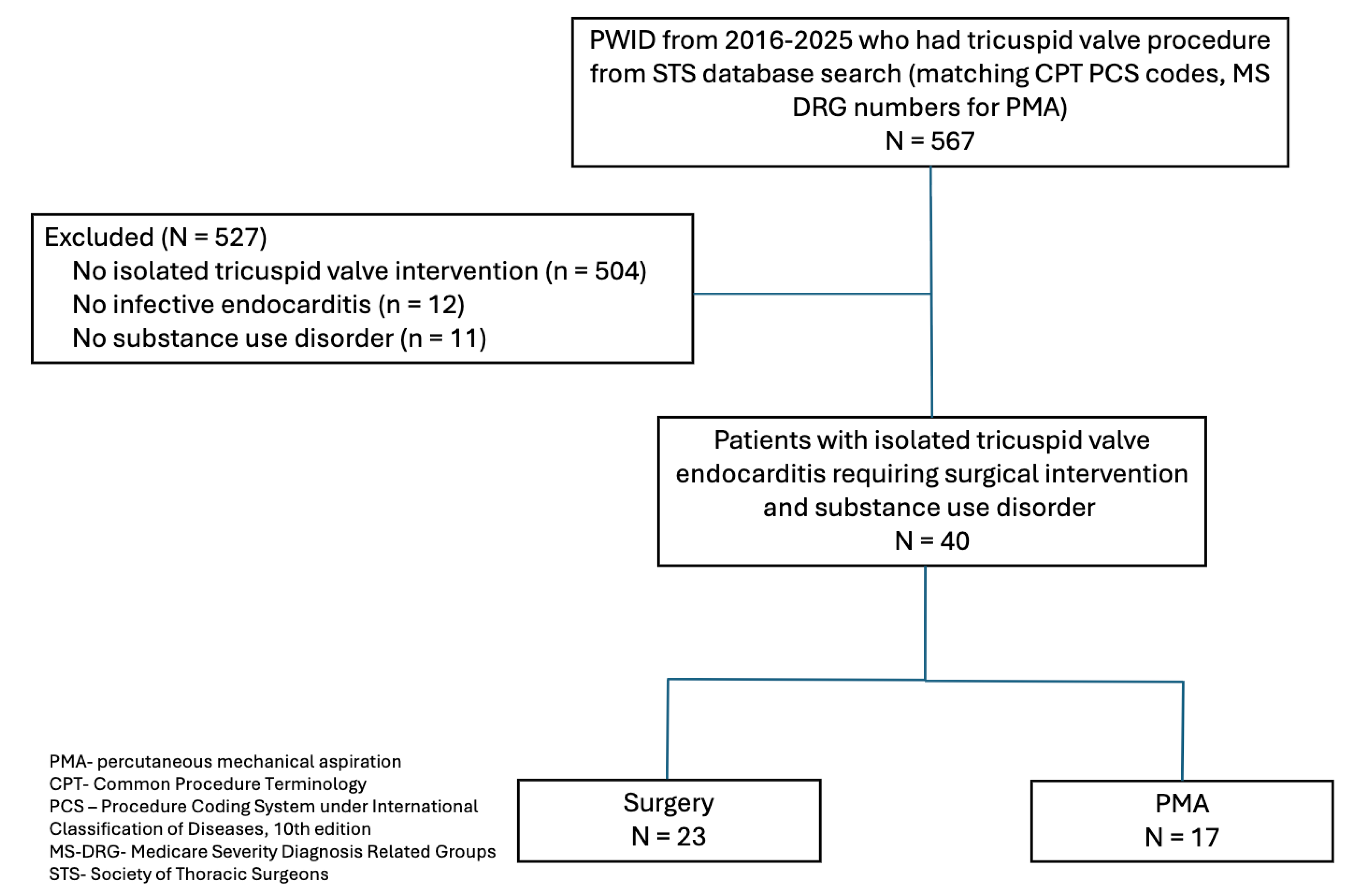
The authors screened both lists for eligibility. Out of the 567 patients who underwent TV procedures, 63 underwent isolated TV intervention of which 51 patients had endocarditis and 40 had TV endocarditis related to substance use (see
Figure 1 for schema). Of the 40 patients who met inclusion criteria, 17 patients had the PMA procedure, and 23 were managed surgically. Five surgeons performed the PMA procedures, and seven performed the surgeries.
The demographic and clinical characteristics of both groups were examined. Variables were selected based on prior literature, as well as consultation with infectious disease physicians and cardiac surgeons well versed with the procedure. We reported categorical variables as number (proportion) and continuous variables as mean (standard deviation). Information collected from the electronic medical record included demographic characteristics; clinical variables (pathogen type, vegetation size (determined by largest dimension on any cardiac imaging), and severity of tricuspid regurgitation); infection-related variables (duration of bacteremia and prior endocarditis episodes); and treatment-related outcomes (length of antibiotic course and re-admissions due to recurrent infection). Substance use information (i.e., substance type, route of entry) was aggregated from medical history and urine toxicology results, where available. All but two patients received a substance use consultation during their hospitalization.
This study had two primary composite outcomes. The first was procedural success, which was defined as >50% reduction in vegetation size and absence of procedural complications. The second was clinical success measured by the absence of procedural or post-procedural complications (i.e., access site complications, bleeding, post operative infection, pericardial effusion, dissection, worsening sepsis, sustained arrhythmias, embolic phenomena and periprocedural mortality), absence of in-hospital mortality, clearance of bacteremia post-surgery without persistence or recurrence, no requirement for subsequent for surgical intervention after procedure, and completion of prescribed antibiotic course. We compared the PMA and surgical groups based on the proportion meeting these success benchmarks.
Secondary outcomes included reintervention within 1 year (i.e., repeat valve surgery), mortality within 1-year, readmission within 30 days, and 1 year, need for permanent pacemaker during or after index procedure, median length of hospital stay, need for intensive care unit care >48 hours (beyond routine post-cardiac procedure monitoring), post-operative vasopressor use lasting >48 hours, and post-operative transfusion requirements beyond 48 hours (i.e., ongoing hemorrhage requiring treatment).
3. Results
3.1. Demographic Characteristics
Baseline demographic and clinical characteristics are shown in
Table 1. The mean age of the cohort was 34 ± 7 years; 27 patients (67.5%) were female, and six (15%) were Black/African American. Most patients (n=32, 80%) had documented polysubstance use, while seven patients (17.5%) had isolated opioid use disorder (OUD).
Baseline demographic data, substance use history, microbiological and clinical characteristics of the study cohort (N = 40). Patients were stratified by having undergone PMA (N = 17) or TV valve repair or replacement (N = 23). Vegetation size data were missing for one patient in each treatment group (subtotal N = 38). Polysubstance use refers to OUD plus the use of at least one additional substance including cannabis, benzodiazepines or amphetamines. Continuous variables are presented as mean (SD); categorical variables are presented as number (percentage). PWID: people who inject drugs; TV: tricuspid valve; IE: infective endocarditis; PMA: percutaneous mechanical aspiration; TVR: tricuspid valve repair/replacement; OUD: Opioid use disorder. SD: standard deviation.
Staphylococcus aureus was the most common causative pathogen, identified in 29 (72.5%) cases. In the PMA cohort, one patient had a fungal infection and two had polymicrobial infections with Gram-positive and Gram-negative bacteria. In the surgical cohort, two patients had fungal infections, and two had polymicrobial/bacterial-fungal infections. 11 patients (27.5%) had a prior endocarditis episode, and six (15.0%) had undergone prior valve surgery. 23 patients (57.5%) were hepatitis C antibody positive. 13 patients (32.5%) had a coexisting mental health diagnosis apart from SUD. 17 patients (42.5%) were not on medication for OUD on admission. 31 patients (77.5%) were discharged on medications for OUD.
The PMA group had a higher proportion of patients with large vegetations (>2 cm) compared with the surgical group (68.8% vs. 59.1%). Severe tricuspid regurgitation prior to surgery was more common in the surgical group (60.9%), compared with the PMA group (58.8%). Mean duration of bacteremia was shorter in the surgical group (5.7 vs. 6.4 days), while time from bacteremia onset to intervention was longer (17.6 vs. 11.8 days). Documented reasons PMA patients were deemed poor surgical candidates included high operative risk (n=10), comorbid substance use (n=5), team preference (n=1), and hemodynamic instability (n=1).
Discharge disposition was varied, and most PMA patients were discharged to skilled nursing facilities (n=12), though some went home (n=4) with a plan to complete antibiotic therapy with long acting lipoglycopeptide therapy/dalbavancin (n=2). For surgical patients, the vast majority were discharged to skilled nursing facilities (n=18). One person in each group had a patient directed premature hospital discharge.
3.2. Outcomes
Outcomes between PMA and tricuspid surgery are compared in
Table 2. Clinical success was higher in the surgical group compared to the PMA group (73.9% vs. 58.8%). Among PMA patients, failure to achieve clinical success was most commonly due to incomplete completion of systemic antibiotic therapy (n=5) and worsening tricuspid regurgitation requiring valve reintervention within one year (n=1). Two PMA procedures were classified as procedural failures due to worsening tricuspid regurgitation and <50% reduction in vegetation size, respectively.
Comparison of primary composite outcomes, secondary clinical outcomes and postoperative hospital course between PWID with IE treated with PMA (N = 17) or TVR (N = 23). Categorical variables as presented as number (percentage) and length of stay is presented as median (interquartile range). PWID: people who inject drugs; TV: tricuspid valve; IE: infective endocarditis; PMA: percutaneous mechanical aspiration; TVR: tricuspid valve repair/replacement; ICU: intensive care unit.
In the surgical group clinical failures were due to incomplete antibiotic therapy (n=4), need for valve reintervention within 1 year (n=1), and procedural complication resulting in worsening heart failure (n=1). One patient from the surgical group and two from the PMA group needed TV repair within one year (4.3% vs. 11.8%). Two patients each in the PMA group and in the surgical group were deceased at one year after the procedure (11.8% vs. 8.7%). The need for a permanent pacemaker placed in the operating room was higher in the surgical group (13.0% vs. 5.9%).
Median hospital length of stay was longer among PMA patients (18 days [IQR 14–36]) compared with surgical patients (16 days [IQR 11–19]). Rates of intensive care unit stay exceeding 48 hours were similar between groups (35.3% PMA vs. 30.4% surgical). No PMA patients required post-operative blood transfusion beyond 48 hours, whereas one surgical patient did (4.3%). Prolonged post-operative vasopressor use (>48 hours) was more frequent in the PMA group (29.4% vs. 8.7%). Thirty-day and one-year readmission rates were numerically higher in the surgical group (34.8% and 65.2%, respectively) compared with the PMA group (23.5% and 47.1%).
3.3. PMA Group Analysis
Within the PMA cohort, two patients had a prior episode of endocarditis, and two had prior valve surgery. Baseline tricuspid regurgitation severity was mild in three patients, moderate in four, and severe in ten. Vegetation sizes ranged from 1 × 1 cm to 4 × 1 cm. At one year, PMA patients demonstrated higher rates of valve reintervention and mortality compared with surgical patients (
Table 2). Of the two PMA patients who died within one year, one had fungal endocarditis and the other had MRSA endocarditis.
Regarding antimicrobial management, two PMA patients received long acting lipoglycopeptides; four were transitioned to oral antibiotics to complete therapy, and the remaining 11 completed treatment with intravenous antibiotics. One PMA patient required permanent pacemaker placement following the intervention.
4. Discussion
Percutaneous mechanical aspiration (PMA) is proposed as a debulking strategy for source control in IE, with the goal of enhancing the effectiveness of antimicrobial therapy through earlier blood culture sterilization or reducing local valve destruction or embolic risk. In populations at high risk for recurrent IE, particularly PWI, PMA has been proposed as a potential alternative to surgical intervention, with the theoretical advantages of reduced procedural morbidity and shorter recovery time [
11,
12].
In this study, we found a lower percentage of patients in the PMA procedure group met the composite procedural and clinical success metrics, compared with the surgical management group. Despite lower overall clinical success, several secondary outcomes may suggest that PMA may offer some selective peri-procedural advantages. Rates of prolonged critical care utilization, as well as lack of post-operative transfusion requirements, may suggest easier recovery. However, a higher proportion of PMA patients needing vasopressor support >48 hours, seems to suggest that vasopressor requirements may be the primary driver of ICU utilization for PMA patients.
Notably, PMA treated patients had lower rates of 30-day hospital readmission as well as acute care utilization one year post procedure. Procedural success rates in the PMA group were comparable to prior reports. In a systematic review of 44 studies including 301 patients, PMA achieved vegetation reduction in 89.2% of cases [
8]; our observed rate of 88.2% is consistent with these findings. However, clinical success in our PMA cohort was lower than previously reported (58.8% vs. 79.1%), likely reflecting our more stringent composite definition that included completion of antibiotic therapy, absence of complications, and freedom from reintervention.
Prior comparative studies evaluating PMA, medical management, and surgery have reported no differences in one-year mortality across treatment strategies [
10]. In our cohort, the absolute number of deaths at one year was identical between groups, though the proportion was higher in the PMA group due to a smaller denominator. Given the limited sample size, we are unable to determine whether observed differences in morbidity or mortality reflect true treatment effects or are driven by patient-level factors, procedural selection, or residual confounding. Furthermore, there could be institution specific variation in practices or preferences or volumes of these procedures which may affect outcomes. For example, in the study by El-Dalati et al., the hospital length of stay was nearly 2 times longer than patients in our group, and the number of PMA procedures performed was higher than surgical procedures. Although PMA may offer peri-procedural advantages in select patients, these benefits were not consistently associated with shorter hospital stays or improved short- or long-term clinical outcomes.
A notable finding in our PMA cohort was the use of nontraditional antimicrobial strategies, including long-acting lipoglycopeptides (LA-LGPs) and oral antibiotic regimens. This likely reflects challenges in arranging outpatient parenteral antimicrobial therapy in PWID who face various individual, system level or structural barriers in accessing this care [
13]. Clinician hesitancy to discharge PWID on IV antibiotics, driven by concerns regarding active substance use, concerns for loss to follow-up, and underlying psychosocial issues, has been well documented [
14]. While such approaches may be perceived as salvage strategies for patients who decline surgery or are deemed poor surgical candidates [
15,
16], our institutional experience suggests that PMA, when paired with alternative antimicrobial strategies, may represent a viable option within a patient-centered, shared decision-making framework.
Interdisciplinary endocarditis teams have explored the option of coordinated clinical care in a patient centered framework. Therapies like PMA and non-traditional antibiotic management strategies should be considered within the context of other management options that may fall outside the current guidelines but may be more acceptable or relevant in patients who face challenges in uptake of guideline recommended treatment options. Larger implementation studies evaluating combined nontraditional strategies (e.g., PMA plus oral or LA-LGP therapy) are needed, particularly as such approaches may better align with patient priorities around substance use recovery and life stability [
17].
This study has a number of strengths. Our use of multiple data sources to identify patients increased the likelihood of capturing all relevant TV IE cases. We developed a comparable and more homogenous overall study population by excluding cases that did not have confirmed SUD or patients who had multi valve endocarditis and patients with surgical management outside of the time period the PMA cases were completed in. The retrospective design was well suited to evaluating an emerging intervention with limited real-world uptake and enabled comprehensive assessment of clinically meaningful composite and secondary outcomes, including one-year reintervention and mortality. Additionally, almost everyone in this cohort was seen by addiction medicine and 78% of patients were discharged on MOUD, which represented a 35% increase in new initiations of MOUD. Both these interventions are clearly associated with improved mortality in PWID with endocarditis [
10,
18].
Despite the study’s strengths, we acknowledge many limitations. The factors which influence the decision to choose PMA versus surgery are sometimes not clear, and ascertainment is limited by our retrospective design. The potential for provider bias in directing one procedure versus another is not measured or excluded. Although vegetation size did not appear to systematically favor one treatment group, patients with smaller vegetations (<1 cm) were managed surgically, suggesting nuanced selection considerations. We did not separate or compare the various TV surgical approaches due to small sample size though evidence seems to suggest that valve repair may be associated with lower risk of pacemaker need or recurrent IE [
4]. No patients in our cohort underwent only tricuspid valvectomy, which has demonstrated worse clinical outcomes [
19]. The nontraditional choices of antibiotic therapy in the PMA group may be reflective of possible hesitancy to pursue conventional management strategies, including surgery, which may add some degree of confounding by indication.
Surgeon perspectives on addiction-related IE further contextualize these findings. Prior surveys indicate that substance use influences operative decision-making, including concerns regarding anticoagulation adherence, valve selection, and technical complexity (e.g., type of valve selected and scar tissue) [
20]. Although interdisciplinary case conferences have been shown to facilitate shared understanding and improve care coordination, such a formalized team was not in place at our institution during the study period. Future qualitative and mixed-methods research may better elucidate how early interdisciplinary discussions shape treatment selection and outcomes for PWID with IE.
5. Conclusion
This study aimed to assess outcomes for PWID who developed TV infective endocarditis and underwent either valve surgery or PMA. Our study found that a lower percentage of patients met the composite procedural and clinical success metrics in the PMA procedure group compared with the surgical management group. This suggests PMA may be inferior to surgical management of TV IE in PWID although the observed differences may be due to baseline imbalances in the groups due to unaccounted for bias at the time of treatment selection. Further research with larger sample sizes in real world scenarios is necessary to understand the appropriate indications for PMA and ensure the most favorable outcomes for PWID with TV IE.
Supplementary Materials
The following supporting information can be downloaded at the website of this paper posted on Preprints.org.
Author Contributions
Conceptualization, Shivakumar Narayanan; Methodology, Nazary Nebeluk, Murtaza Dawood and Shivakumar Narayanan; Validation, Nazary Nebeluk; Formal analysis, Juliana Sherchan, Lauren Bernard and Nazary Nebeluk; Investigation, Juliana Sherchan, Lauren Bernard, Nazary Nebeluk and Shivakumar Narayanan; Data curation, Juliana Sherchan, Lauren Bernard, David Zapata, Murtaza Dawood, Douglas Anderson, Ramon Riojas and Shivakumar Narayanan; Writing—original draft, Juliana Sherchan, Lauren Bernard, Nazary Nebeluk, David Zapata and Shivakumar Narayanan; Writing—review & editing, Juliana Sherchan, Lauren Bernard, Nazary Nebeluk, David Zapata, Murtaza Dawood, Douglas Anderson, Ramon Riojas and Shivakumar Narayanan; Supervision, Ramon Riojas and Shivakumar Narayanan; Project administration, Nazary Nebeluk. All authors have read and agreed to the published version of the manuscript.
Funding
This research received no external funding.
Institutional Review Board Statement
This study was a retrospective cohort of PWID admitted to the University of Mar-yland Medical Center with infective endocarditis of the TV who underwent an isolated TV procedure between January 2016 and September 2025. The study was reviewed by the University of Maryland’s Institutional Review Board and deemed exempt from full review.
Acknowledgments
The authors would like to thank the patients in this cohort, as well as Emily Brown-Umosella and Alex Phoinix for help with data procurement.
Conflicts of Interest
The authors declare no conflict of interest.
References
- McCarthy, N.L.; Baggs, J.; See, I.; Reddy, S.C.; A Jernigan, J.; Gokhale, R.H.; E Fiore, A. Bacterial Infections Associated with Substance Use Disorders, Large Cohort of United States Hospitals, 2012–2017. Clin. Infect. Dis. 2020, 71, e37–e44. [Google Scholar] [CrossRef] [PubMed]
- Schranz, A.J.; Fleischauer, A.; Chu, V.H.; Wu, L.-T.; Rosen, D.L. Trends in Drug Use–Associated Infective Endocarditis and Heart Valve Surgery, 2007 to 2017. Ann. Intern. Med. 2019, 170, 31–40. [Google Scholar] [CrossRef] [PubMed]
- Ortiz-Bautista, C.; López, J.; García-Granja, P.E.; Sevilla, T.; Vilacosta, I.; Sarriá, C.; Olmos, C.; Ferrera, C.; Sáez, C.; Gómez, I.; et al. Current profile of infective endocarditis in intravenous drug users: The prognostic relevance of the valves involved. Int. J. Cardiol. 2015, 187, 472–474. [Google Scholar] [CrossRef] [PubMed]
- Yanagawa, B.; Elbatarny, M.; Verma, S.; Hill, S.; Mazine, A.; Puskas, J.D.; Friedrich, J.O. Surgical Management of Tricuspid Valve Infective Endocarditis: A Systematic Review and Meta-Analysis. Ann. Thorac. Surg. 2018, 106, 708–714. [Google Scholar] [CrossRef] [PubMed]
- Mori, M.; Bin Mahmood, S.U.; Schranz, A.J.; Sultan, I.; Axtell, A.L.; Sarsour, N.; Hiesinger, W.; Boskovski, M.T.; Hirji, S.; Kaneko, T.; et al. Risk of reoperative valve surgery for endocarditis associated with drug use. J. Thorac. Cardiovasc. Surg. 2020, 159, 1262–1268.e2. [Google Scholar] [CrossRef]
- Geirsson, A.; Schranz, A.; Jawitz, O.; Mori, M.; Feng, L.; Zwischenberger, B.A.; Iribarne, A.; Dearani, J.; Rushing, G.; Badhwar, V.; et al. The Evolving Burden of Drug Use Associated Infective Endocarditis in the United States. 56th Annual Meeting of the Society-of-Thoracic-Surgeons. Ann. Thorac. Surg. 2020, vol. 110, 1185–1192. [Google Scholar]
- Shrestha, N.K.; Jue, J.; Hussain, S.T.; Jerry, J.M.; Pettersson, G.B.; Menon, V.; Navia, J.L.; Nowacki, A.S.; Gordon, S.M. Injection Drug Use and Outcomes After Surgical Intervention for Infective Endocarditis. Ann. Thorac. Surg. 2015, 100, 875–882. [Google Scholar] [CrossRef] [PubMed]
- Mhanna, M.; Beran, A.; Al-Abdouh, A.; Jabri, A.; Sajdeya, O.; Alharbi, A.; Khuder, S.A.; A Eltahawy, E. AngioVac for Vegetation Debulking in Right-sided Infective Endocarditis: A Systematic Review and Meta-Analysis. Curr. Probl. Cardiol. 2022, 47, 101353. [Google Scholar] [CrossRef] [PubMed]
- Chakravarthy, M.; Lasorda, D.; Bhanot, N.; Cherukuri, K.; Ghosh, P.; Abbadi, D.; Mareddy, C. TCT-568 Effectiveness and Safety of Vacuum-Assisted Thrombectomy Device (AngioVac) for Extraction of Vegetations on Intra-Cardiac Devices and Valves Prior to Device Removal: A Single Center Experience. JACC 2019, 74, B560–B560. [Google Scholar] [CrossRef]
- El-Dalati, S.; Sinner, G.; Leung, S.; Reda, H.; Sekela, M.; Heier, K.; Alnabelsi, T. Comparison of Medical Therapy, Valve Surgery, and Percutaneous Mechanical Aspiration for Tricuspid Valve Infective Endocarditis. Am. J. Med. 2024, 137, 888–895.e2. [Google Scholar] [CrossRef] [PubMed]
- Yucel, E.; Bearnot, B.; Paras, M.L.; Zern, E.K.; Dudzinski, D.M.; Soong, C.-P.; Jassar, A.S.; Rosenfield, K.; Lira, J.; Lambert, E.; et al. Diagnosis and Management of Infective Endocarditis in People Who Inject Drugs. JACC 2022, 79, 2037–2057. [Google Scholar] [CrossRef] [PubMed]
- El Sabbagh, A.; Yucel, E.; Zlotnick, D.; Moriarty, J.M.; Younes, S.; Hamid, N.; Akhtar, Y.; Baddour, L.M.; O’gAra, P.; Starck, C.; et al. Percutaneous Mechanical Aspiration in Infective Endocarditis: Applications, Technical Considerations, and Future Directions. J. Soc. Cardiovasc. Angiogr. Interv. 2024, 3, 101269. [Google Scholar] [CrossRef] [PubMed]
- Hurley, H.; Sikka, M.; Jenkins, T.; Cari, E.V.; Thornton, A. Outpatient Antimicrobial Treatment for People Who Inject Drugs. Infect. Dis. Clin. North Am. 2020, 34, 525–538. [Google Scholar] [CrossRef] [PubMed]
- Bork, J. T.; Heil, Emily L; Berry, Shanna; Lopes, Eurides; Davé, Rohini; Gilliam, Bruce L; Amoroso, Anthony. Dalbavancin Use in Vulnerable Patients Receiving Outpatient Parenteral Antibiotic Therapy for Invasive Gram-Positive Infections. Infect. Dis. Ther. 2019, vol. 8, 171–184. [Google Scholar] [CrossRef] [PubMed]
- Bryson-Cahn, C.; Beieler, A.; Chan, J.; Senter, S.; Harrington, R.; Dhanireddy, S. “Poster Abstracts Session: 141. Clinical Practice Issues Friday,” Oct. 2017. Available online: https://academic.oup.com/ofid/article/4/suppl_1/S336/4294722.
- Turner, N.A.; Zaharoff, S.; King, H.; Evans, S.; Hamasaki, T.; Lodise, T.; Ghazaryan, V.; Beresnev, T.; Riccobene, T.; Patel, R.; et al. Dalbavancin as an option for treatment of S. aureus bacteremia (DOTS): study protocol for a phase 2b, multicenter, randomized, open-label clinical trial. Trials 2022, 23, 1–15. [Google Scholar] [CrossRef] [PubMed]
- Baddour, L.M.; Weimer, M.B.; Wurcel, A.G.; McElhinney, D.B.; Marks, L.R.; Fanucchi, L.C.; Garrigos, Z.E.; Pettersson, G.B.; DeSimone, D.C.; Disease, K.D.C.O.T.C.O.L.C.H.; et al. Management of Infective Endocarditis in People Who Inject Drugs: A Scientific Statement From the American Heart Association. Circulation 2022, 146, E187–E201. [Google Scholar] [CrossRef] [PubMed]
- Kimmel, S.D.; Walley, A.Y.; Li, Y.; Linas, B.P.; Lodi, S.; Bernson, D.; Weiss, R.D.; Samet, J.H.; Larochelle, M.R. Association of Treatment With Medications for Opioid Use Disorder With Mortality After Hospitalization for Injection Drug Use–Associated Infective Endocarditis. JAMA Netw. Open 2020, 3, e2016228–e2016228. [Google Scholar] [CrossRef] [PubMed]
- Slaughter, M.S.; Badhwar, V.; Ising, M.; Ganzel, B.L.; Sell-Dottin, K.; Jawitz, O.K.; Zhang, S.; Trivedi, J.R. Optimum surgical treatment for tricuspid valve infective endocarditis: An analysis of the Society of Thoracic Surgeons national database. In 99th Annual Meeting of the American-Association-for-Thoracic-Surgery (AATS) Journal of Thoracic and Cardiovascular Surgery; Mosby Inc., Apr 2021; pp. 1227–1235.e1. [Google Scholar]
- Wurcel, A.G.; Zubiago, J.; Reyes, J.; Smyth, E.; Balsara, K.R.; Avila, D.; Barocas, J.A.; Beckwith, C.G.; Bui, J.; Chastain, C.A.; et al. Surgeons’ Perspectives on Valve Surgery in People with Drug Use-Associated Infective Endocarditis. Ann. Thorac. Surg. 2022, 116, 492–498. [Google Scholar] [CrossRef]
|
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).