Submitted:
15 February 2026
Posted:
03 March 2026
You are already at the latest version
Abstract
Keywords:
1. Introduction
2. Materials and Methods
3. Results
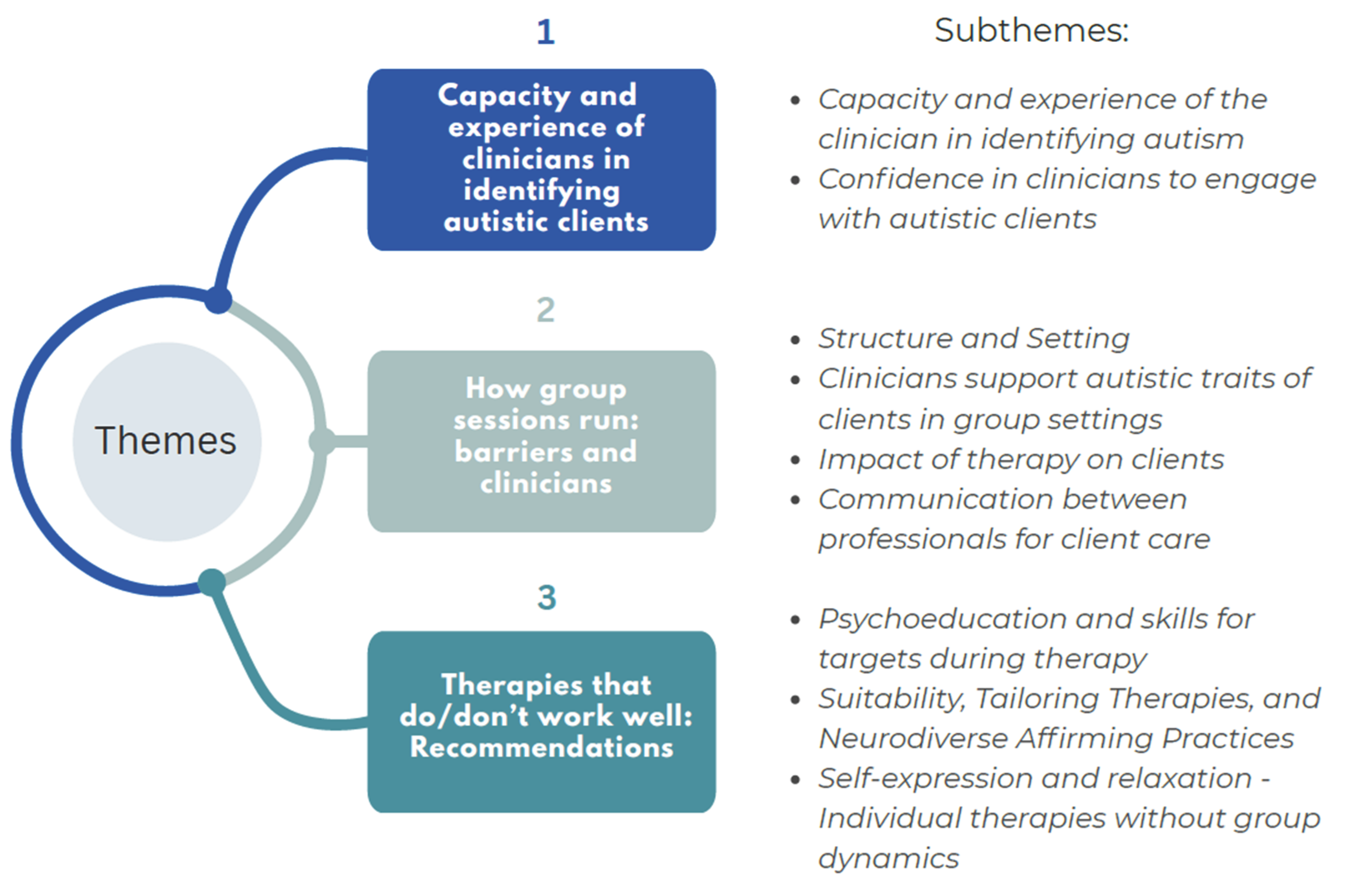
“Probably, what eye contact, sometimes is a, is something that I notice or observe as eye contact or their behavior in the room. Um, social skills, I guess, kind of in the waiting room or here with the nurses, sometimes I notice.” Female, Clinical Psychologist.
“…she didn’t make sense to me because …I didn’t think I saw many…girls with autism. And I think that’s another sort of factor is that in girls, it tends to be, we don’t tend to think of the diagnosis straightaway. It comes, it comes later. And only when she represented to me at the age of 15, after several years, and it was much clearer then.” Male, Consultant Psychiatrist
“So in any case, I also don’t think there is enough education with the staff members on autism, in how it’s presented. Like for example, I learned a lot going to, [Prominent Autism clinician/researcher]… I attended this seminar on eating disorders and Autism. And that was such an eye opener…” Female, Nurse.
“…a lot of people with autism need a sense of connectedness…. Being in the group itself gives them that sense of connectedness and therefore, giving them tools to be connected, meaning a lot of icebreaker stuff.” Female, Nurse.
“So sort of using those interests, like you talked about earlier, to help develop a therapeutic alliance, and then using that as a platform to build the therapy.” Female, Art therapist
“… perhaps even in the physical environment, so these lights here would be too overwhelming, for well, for this particular client, and she reported that. So considering the physical environment and how it can be more sensory friendly” Female, Occupational Therapist.
“I think it’s just the EMP [Emotion Management Program] and DBT [Dialectical Behaviour Therapy] in general is very structured, quite logical. And sequential, there’s an order, steps that you need to do.” Female, Nurse
“…this is from the feedback that they gave us, they felt that the skills, as they were taught, were quite neurotypical, and sort of designed for people who had a neurotypical outlook.” Male, Social Worker
“...you know, [client] “people don’t seem to understand me, I’m probably not all that”, the low self-esteem that comes along with it as well. So what’s been interesting is when people actually receive a diagnosis, it’s, especially women. It’s like this revelation, you know, of “Oh right, okay”.” Female, Psychiatry Registrar
“So he’s only about 26 and you know, I’m very concerned about him. So I said to him that I’m going to get in touch with his psychiatrist and GP and see if we can organize a way of him getting a proper assessment and also then perhaps with a view to me helping him perhaps apply for NDIS, or something like that.” Female, Clinical Neuropsychologist.
“”I guess, I think DBT would be very beneficial too, in terms of the interpersonal effectiveness and skill building, for regulating emotions. I think that that really can suit that client group…. I guess. In terms of OT [Occupational Therapy]. I definitely think sensory modulation is helpful in lots of ways. And I’ve seen it to be helpful.” Female, Occupational Therapist.
“...but the content of DBT… I think would be so advantageous, but set up in a different way. And I don’t know what that way would look like. But it’s just not enough time and too much content to sort of sink like a barrage of words, I think…. And, obviously, an array of like visual and verbal, you know, like, a number of different ways to take in… I don’t know, giving as many [real] life examples.” Female, general Psychologist.
“[in reference to an art therapy approach] I mean, I may be biassed here, but I obviously definitely recommend it. Just as an example to like, whether they’re working through all those things I talked about before and you know, emotional regulation and that sort of thing, even just connecting with their sense of identity and self.” Female, Art Therapist”
4. Discussion
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Acknowledgments
Conflicts of Interest
References
- Lai, M. C.; Kassee, C.; Besney, R.; Bonato, S.; Hull, L.; Mandy, W.; Szatmari, P.; Ameis, S. H. Prevalence of Co-Occurring Mental Health Diagnoses in the Autism Population: A Systematic Review and Meta-Analysis. Lancet Psychiatry, 2019, 6 (10), 819–829. [CrossRef]
- Camm-Crosbie, L.; Bradley, L.; Shaw, R.; Baron-Cohen, S.; Cassidy, S. ‘People like Me Don’t Get Support’: Autistic Adults’ Experiences of Support and Treatment for Mental Health Difficulties, Self-Injury and Suicidality. Autism, 2019, 23 (6), 1431–1441. [CrossRef]
- Lipinski, S.; Boegl, K.; Blanke, E. S.; Suenkel, U.; Dziobek, I. A Blind Spot in Mental Healthcare? Psychotherapists Lack Education and Expertise for the Support of Adults on the Autism Spectrum. Autism, 2022, 26 (6), 1509–1521. [CrossRef]
- Bemmer, E. R.; Boulton, K. A.; Thomas, E. E.; Larke, B.; Lah, S.; Hickie, I. B.; Guastella, A. J. Modified CBT for Social Anxiety and Social Functioning in Young Adults with Autism Spectrum Disorder. Mol. Autism, 2021, 12 (1), 1–15. [CrossRef]
- Bemmouna, D.; Coutelle, R.; Weibel, S.; Weiner, L. Feasibility, Acceptability and Preliminary Efficacy of Dialectical Behavior Therapy for Autistic Adults without Intellectual Disability: A Mixed Methods Study. J. Autism Dev. Disord., 2022, 52 (10), 4337–4354. [CrossRef]
- Cooper, K.; Loades, M. E.; Russell, A. Adapting Psychological Therapies for Autism. Res. Autism Spectr. Disord., 2018, 45, 43–50. [CrossRef]
- Hartmann, K.; Urbano, M.; Manser, K.; Okwara, L. Modified Dialectical Behavior Therapy to Improve Emotion Regulation in Autism Spectrum Disorders; 2012.
- Fisher, C. A.; Grace, N.; Tsang, E.; Lewis, J.; Pieters, J. Neuropsychology Strengths-Based Approach for the Assessment of Autism in Adults: Qualitative Thematic Analysis of Clients’ Experiences of the Diagnosis and Feedback Process. J. Autism Dev. Disord., 2025. [CrossRef]
- Fisher, C. A.; Grace, N.; Tsang, E.; Pieters, J. Development of a Group Mental Health Therapy Program for Autistic Adults Using a Partial Consumer Co-Design Framework. Academia Mental Health and Wellbeing (Accepted, In press).
- Fisher, C. A.; Pieters, J.; Tsang, E.; Lewis, J.; Stolz-Grobusch, B.; Grace, N. Qualitative Content Analysis of Ten Autistic Adults’ Experiences of Mental Health Therapy and Their Interest and Preferences for a Group Program: Informing Co-Production. Under review.
- Green, T.; Bonner, A.; Teleni, L.; Bradford, N.; Purtell, L.; Douglas, C.; Yates, P.; Macandrew, M.; Dao, H. Y.; Chan, R. J. Use and Reporting of Experience-Based Codesign Studies in the Healthcare Setting: A Systematic Review. BMJ Quality and Safety. BMJ Publishing Group January 1, 2020, pp 64–76. [CrossRef]
- Braun, V.; Clarke, V. Successful Qualitative Research: A Practical Guide for Beginners; Sage: London, 2013.
- Charmaz, K. Constructivist Grounded Theory. J. Posit. Psychol., 2017, 12 (3), 299–300. [CrossRef]
- Flower, R. L.; Benn, R.; Bury, S.; Camin, M.; Muggleton, J.; Richardson, E. K.; Bulluss, E. K.; Calabria, B.; Curran, A.; Giugni, M.; et al. Defining Neurodiversity Affirming Psychology Practice for Autistic Adults: A Delphi Study Integrating Psychologist and Client Perspectives. Autism in Adulthood, 2025. [CrossRef]
- Jellett, R.; Flower, R. L. How Can Psychologists Meet the Needs of Autistic Adults? Autism. SAGE Publications Ltd. February 1, 2024, pp 520–522. [CrossRef]
- Fisher, C.; Pieters, J.; Tsang, E.; Lewis, J.; Stolz-Grobusch, B. J.; Grace, N. Qualitative Content Analysis of Ten Autistic Adults’ Experiences of Mental Health Therapy and Their Interest and Preferences for a Group Program: Informing Co-Production. February 2, 2026. [CrossRef]
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).



