Submitted:
26 February 2026
Posted:
02 March 2026
You are already at the latest version
Abstract
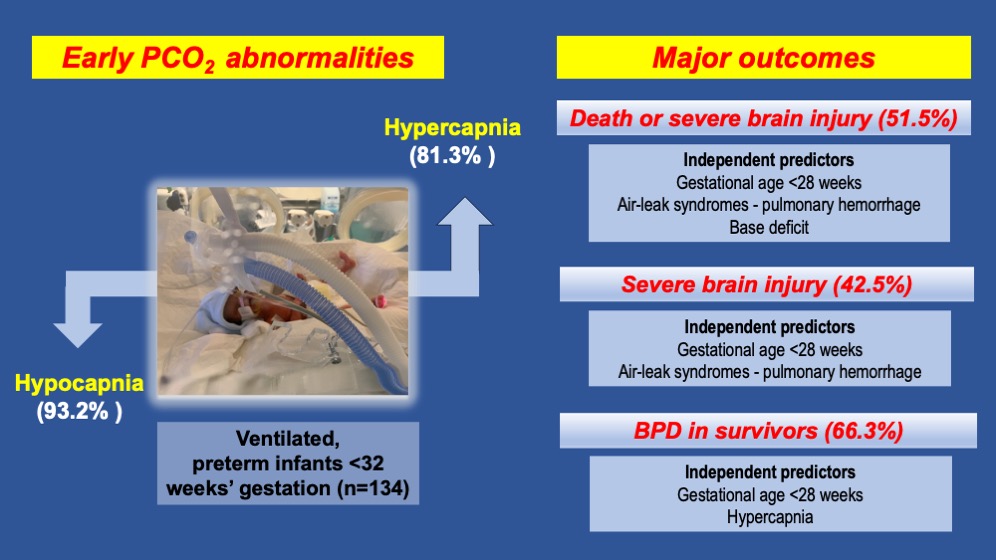
Keywords:
1. Introduction
2. Materials and Methods
2.1. Patients and Data Collection
2.2. Outcomes and Definitions
2.3. Respiratory Management
2.4. Statistical Analysis
3. Results
3.1. Study Population Characteristics
3.2. Variability in PCO₂ During the First 72 Hours
3.3. Outcomes
3.3.1. Death or Severe Brain Injury
3.3.2. Severe Brain Injury
3.3.3. Survivors with and Without BPD
3.4. Multivariable Analyses
4. Discussion
5. Conclusions
Supplementary Materials
Author Contributions
Funding
Institutional Review Board Statement
Informed Consent Statement
Data Availability Statement
Conflicts of Interest Statement
Abbreviations
References
- Norman, M; Jonsson, B; Söderling, J; Björklund, LJ; Håkansson, S. Patterns of Respiratory Support by Gestational Age in Very Preterm Infants. Neonatology 2023, 120, 142–52. [Google Scholar] [CrossRef]
- Mukerji, A; Shah, PS; Kadam, M; Borhan, S; Razak, A. Non-invasive respiratory support in preterm infants as primary mode: a network meta-analysis. Cochrane Database Syst Rev. 2025, 7, CD014895. [Google Scholar]
- Sarafidis, K; Chotas, W; Agakidou, E; Karagianni, P; Drossou, V. The Intertemporal Role of Respiratory Support in Improving Neonatal Outcomes: A Narrative Review. Child Basel Switz. 2021, 8, 883. [Google Scholar] [CrossRef] [PubMed]
- Wong, SK; Chim, M; Allen, J; Butler, A; Tyrrell, J; Hurley, T; et al. Carbon dioxide levels in neonates: what are safe parameters? Pediatr Res. 2022, 91, 1049–56. [Google Scholar] [CrossRef] [PubMed]
- van Kaam, AH; De Jaegere, AP; Rimensberger, PC; Neovent Study Group. Incidence of hypo- and hyper-capnia in a cross-sectional European cohort of ventilated newborn infants. Arch Dis Child Fetal Neonatal Ed. 2013, 98, F323–326. [Google Scholar] [CrossRef] [PubMed]
- Bayoumi El Sebaie, D; Alsharany Abuelhamd, W; Mohamed Abdelmomen, A; Fawzy Kamal, A. Is hyperventilation a common iatrogenic problem in the neonatal intensive care unit? CHILDS Health 2024, 19, 362–7. [Google Scholar] [CrossRef]
- Thome, UH; Ambalavanan, N. Permissive hypercapnia to decrease lung injury in ventilated preterm neonates. Semin Fetal Neonatal Med. 2009, 14, 21–7. [Google Scholar] [CrossRef]
- Brown, MK; Poeltler, DM; Hassen, KO; Lazarus, DV; Brown, VK; Stout, JJ; et al. Incidence of Hypocapnia, Hypercapnia, and Acidosis and the Associated Risk of Adverse Events in Preterm Neonates. Respir Care 2018, 63, 943–9. [Google Scholar] [CrossRef]
- Kaiser, JR; Gauss, CH; Pont, MM; Williams, DK. Hypercapnia during the first 3 days of life is associated with severe intraventricular hemorrhage in very low birth weight infants. J Perinatol Off J Calif Perinat Assoc. 2006, 26, 279–85. [Google Scholar] [CrossRef]
- Fabres, J; Carlo, WA; Phillips, V; Howard, G; Ambalavanan, N. Both extremes of arterial carbon dioxide pressure and the magnitude of fluctuations in arterial carbon dioxide pressure are associated with severe intraventricular hemorrhage in preterm infants. Pediatrics 2007, 119, 299–305. [Google Scholar] [CrossRef]
- Erickson, SJ; Grauaug, A; Gurrin, L; Swaminathan, M. Hypocarbia in the ventilated preterm infant and its effect on intraventricular haemorrhage and bronchopulmonary dysplasia. J Paediatr Child Health 2002, 38, 560–2. [Google Scholar] [CrossRef] [PubMed]
- Ozawa, Y; Miyake, F; Isayama, T. Efficacy and safety of permissive hypercapnia in preterm infants: A systematic review. Pediatr Pulmonol. 2022, 57, 2603–13. [Google Scholar] [CrossRef] [PubMed]
- Travers, CP; Gentle, SJ; Shukla, VV; Aban, I; Yee, AJ; Armstead, KM; et al. Late Permissive Hypercapnia for Mechanically Ventilated Preterm Infants: A Randomized Trial. Pediatr Pulmonol. 2025, 60, e71165. [Google Scholar] [CrossRef]
- Altaany, D; Natarajan, G; Gupta, D; Zidan, M; Chawla, S. Severe Intraventricular Hemorrhage in Extremely Premature Infants: Are high Carbon Dioxide Pressure or Fluctuations the Culprit? Am J Perinatol. 2015, 32, 839–44. [Google Scholar] [CrossRef]
- Pierrat, V; Duquennoy, C; van Haastert, IC; Ernst, M; Guilley, N; de Vries, LS. Ultrasound diagnosis and neurodevelopmental outcome of localised and extensive cystic periventricular leucomalacia. Arch Dis Child Fetal Neonatal Ed. 2001, 84, F151–156. [Google Scholar] [CrossRef]
- Papile, LA; Burstein, J; Burstein, R; Koffler, H. Incidence and evolution of subependymal and intraventricular hemorrhage: a study of infants with birth weights less than 1,500 gm. J Pediatr. 1978, 92, 529–34. [Google Scholar] [CrossRef]
- Jobe, AH; Bancalari, E. Bronchopulmonary dysplasia. Am J Respir Crit Care Med. 2001, 163, 1723–9. [Google Scholar] [CrossRef] [PubMed]
- Röhr, M; Poryo, M; Bay, J; Gortner, L; Meyer, S. Episodes of hypo- and hypercapnia in a cohort of mechanically ventilated VLBW infants: the role of adequate staffing. Wien Med Wochenschr 1946 2017, 167, 256–8. [Google Scholar] [CrossRef]
- Murthy, P; Zein, H; Thomas, S; Scott, JN; Abou Mehrem, A; Esser, MJ; et al. Neuroprotection Care Bundle Implementation to Decrease Acute Brain Injury in Preterm Infants. Pediatr Neurol. 2020, 110, 42–8. [Google Scholar] [CrossRef]
- Thome, UH; Dreyhaupt, J; Genzel-Boroviczeny, O; Bohnhorst, B; Schmid, M; Fuchs, H; et al. Influence of PCO2 Control on Clinical and Neurodevelopmental Outcomes of Extremely Low Birth Weight Infants. Neonatology 2018, 113, 221–30. [Google Scholar] [CrossRef] [PubMed]
- Levene, M. Minimising neonatal brain injury: how research in the past five years has changed my clinical practice. Arch Dis Child. 2007, 92, 261–5. [Google Scholar] [CrossRef]
- Zhou, W; Liu, W. Hypercapnia and hypocapnia in neonates. World J Pediatr WJP 2008, 4, 192–6. [Google Scholar] [CrossRef] [PubMed]
- Shah, PS; Lui, K; Sjörs, G; Mirea, L; Reichman, B; Adams, M; et al. Neonatal Outcomes of Very Low Birth Weight and Very Preterm Neonates: An International Comparison. J Pediatr. 2016, 177, 144–152.e6. [Google Scholar] [CrossRef]
- Razak, A; Johnston, E; Stewart, A; Clark, MAT; Stevens, P; Charlton, M; et al. Temporal Trends in Severe Brain Injury and Associated Outcomes in Very Preterm Infants. Neonatology 2024, 121, 440–9. [Google Scholar] [CrossRef] [PubMed]
- Lee, J; Lee, CYM; Naiduvaje, K; Wong, Y; Bhatia, A; Ereno, IL; et al. Trends in neonatal mortality and morbidity in very-low-birth-weight (VLBW) infants over a decade: Singapore national cohort study. Pediatr Neonatol. 2023, 64, 585–95. [Google Scholar] [CrossRef] [PubMed]
- Subramanian, S; El-Mohandes, A; Dhanireddy, R; Koch, MA. Association of bronchopulmonary dysplasia and hypercarbia in ventilated infants with birth weights of 500-1,499 g. Matern Child Health J. 2011, 15, S17–26. [Google Scholar] [CrossRef]
- Dassios, T. On carbon dioxide and bronchopulmonary dysplasia. Acta Paediatr Oslo Nor 1992 2023, 112, 2248–9. [Google Scholar] [CrossRef]
- Liu, W; Zong, H; Jiang, J; Yang, C; Li, F. High-frequency oscillatory ventilation with volume guarantee in infants: a systematic review. Pediatr Res. 2025, 98, 470–8. [Google Scholar] [CrossRef]
- Solberg, MT; Bjørk, IT; Hansen, TWR. Adherence to oxygenation and ventilation targets in mechanically ventilated premature and sick newborns: a retrospective study. BMC Pediatr. 2013, 13, 126. [Google Scholar] [CrossRef]
- Nadeem, M; Murray, D; Boylan, G; Dempsey, EM; Ryan, CA. Blood carbon dioxide levels and adverse outcome in neonatal hypoxic-ischemic encephalopathy. Am J Perinatol. 2010, 27, 361–5. [Google Scholar] [CrossRef]
- Society, CP. Neuroprotection from acute brain injury in preterm infants | Canadian Paediatric Society [Internet]. 11 Nov 2025. Available online: https://cps.ca/en/documents/position/neuroprotection.
- Sweet, DG; Carnielli, VP; Greisen, G; Hallman, M; Klebermass-Schrehof, K; Ozek, E; et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome: 2022 Update. Neonatology 2023, 120, 3–23. [Google Scholar] [CrossRef] [PubMed]
- Sweet, DG; Carnielli, V; Greisen, G; Hallman, M; Ozek, E; te Pas, A; et al. European Consensus Guidelines on the Management of Respiratory Distress Syndrome – 2019 Update. Neonatology 2019, 115, 432–50. [Google Scholar] [CrossRef] [PubMed]
- de Bijl-Marcus, K; Brouwer, AJ; De Vries, LS; Groenendaal, F; Wezel-Meijler, G; van. Neonatal care bundles are associated with a reduction in the incidence of intraventricular haemorrhage in preterm infants: a multicentre cohort study. Arch Dis Child Fetal Neonatal Ed. 2020, 105, 419–24. [Google Scholar] [CrossRef]
- Erni, I; Bassler, D; Glauser, D; Wolff, M; Grass, B; Adams, M. Quality improvement project to reduce intraventricular haemorrhage in very preterm infants failed due to increased life-sustaining intensive care at low gestational age. BMJ Open Qual. 2025, 14, e003325. [Google Scholar] [CrossRef] [PubMed]
| Variable | Descriptive statistics |
|---|---|
| (n=134) | |
| Gestational age (weeks) | 28 (25; 29) |
| Gestational age < 28 (weeks) | 62 (46.3%) |
| Birth weight (g) | 950 (700; 1230) |
| 5-min Apgar score | 8 (7; 8) |
| Male sex | 63 (47.0%) |
| SGA | 20 (14.9%) |
| Maternal hypertension | 22 (16.4%) |
| Chorioamnionitis | 28 (20.9%) |
| PPROM | 35 (26.1%) |
| Prenatal steroids | 116 (86.6%) |
| Mg administration | 76 (56.7%) |
| Caesarean section | 114 (85.1%) |
| Inborn | 120 (89.6%) |
| Surfactant for RDS | 123 (91.8%) |
| Pulmonary hemorrhage | 31 (23.1%) |
| Air-leak syndromes | 25 (18.7%) |
| PDA | 66 (49.3%) |
| Treated PDA | 54 (40.3%) |
| Severe IVH | 39 (29.1%) |
| SBI | 57 (42.5%) |
| Sepsis (Culture-positive; early/late) | 69 (51.5%) |
| Fentanyl or sedative | 69 (51.5%) |
| NEC (grade II, III) | 17 (12.7%) |
| Rescue HFOV | 69 (51.5%) |
| Duration of invasive ventilation (days) | 5.0 (2.0; 11.0) |
| Survival | 83 (61.9%) |
| Death or SBI | 69 (51.5%) |
| Length of stay (days) | 51 (11; 85) |
| At NICU admission | |
| pH | 7.3 (7.2; 7.4) |
| PCO2 | 36.8 (30.1; 44.0) |
| Base Deficit (absolute value) | 6.8 (5.2; 9.2) |
| During the first 3 days of life | |
| Min PCO2 | 28.0 (± 5.2) |
| Max PCO2 | 55.6 (±13.4) |
| Max-min PCO2 | 24.5 (16.4; 33.4) |
| Clinical outcomes in survivors (n=83) | |
| Any BPD | 54 (65.9%) |
| ROP | 33 (40.2%) |
| Treated ROP | 13 (15.9%) |
| Length of stay (days) | 75 (54; 115) |
| Max PCO2 group | ||||
|---|---|---|---|---|
| Min PCO2 group | 35-45 | 46-55 | 56-65 | >65 |
| <30 | 21 (15.7%) | 27 (20.1%) | 17 (12.7%) | 22 (16.4%) |
| 30-34 | 4 (3%) | 19 (14.2%) | 11 (8.2%) | 4 (3%) |
| 35-45 | 0 (0%) | 5 (3.7%) | 4 (3%) | 0 (0%) |
| Variable | Survival without SBI (n=65) | Death or SBI (n=69) | p-value |
|---|---|---|---|
| Gestational age (weeks) | 29 (28; 30) | 25 (24; 27) | <0.001 |
| Gestational age < 28 weeks | 9 (13.8%) | 53 (76.8%) | <0.001 |
| Birth weight (g) | 1170 (1020; 1380) | 710 (595; 960) | <0.001 |
| 5-min Apgar score | 8 (7; 9) | 7 (7; 8) | 0.006 |
| Male sex | 25 (38.5%) | 38 (55.1%) | 0.054 |
| SGA | 9 (13.8%) | 11 (15.9%) | 0.734 |
| Maternal hypertension | 14 (21.5%) | 8 (11.6%) | 0.120 |
| Chorioamnionitis | 10 (15.4%) | 18 (26.1%) | 0.128 |
| PPROM | 12 (18.5%) | 23 (33.3%) | 0.050 |
| Prenatal steroids | 55 (84.6%) | 61 (88.4%) | 0.520 |
| Mg administration | 35 (53.8%) | 41 (59.4%) | 0.515 |
| Caesarean section | 60 (92.3%) | 54 (78.3%) | 0.029 |
| Inborn | 60 (92.3%) | 60 (87.0%) | 0.401 |
| Surfactant for RDS | 58 (89.2%) | 65 (94.2%) | 0.356 |
| Pulmonary hemorrhage | 5 (7.7%) | 26 (37.7%) | <0.001 |
| Air-leak syndromes | 7 (10.8%) | 18 (26.1%) | 0.023 |
| Treated PDA | 15 (23.1%) | 39 (56.5%) | <0.001 |
| Sepsis (Culture positive; early/late) | 31 (47.7%) | 38 (55.1%) | 0.393 |
| Fentanyl or sedative | 29 (44.6%) | 40 (58.0%) | 0.122 |
| NEC (grade II, III) | 4 (6.2%) | 13 (18.8%) | 0.037 |
| Rescue HFOV | 19 (29.2%) | 50 (72.5%) | <0.001 |
| Duration of invasive ventilation | 4 (1; 9) | 7 (4; 15) | 0.005 |
| At NICU admission | |||
| pH | 7.3 (7.3; 7.4) | 7.3 (7.2; 7.4) | 0.540 |
| PCO2 | 37.4 (31.3; 47.0) | 36.5 (29.4; 42.6) | 0.223 |
| Base Deficit (absolute value) | 5.9 (4.4; 8.5) | 7.4 (5.9; 9.8) | 0.005 |
| During the first 3 days of life | |||
| Min PCO2 | 28.8 (± 5.3) | 27.3 (± 5.0) | 0.116 |
| Max PCO2 | 51.2 (± 10.8) | 59.8 (± 14.3) | <0.001 |
| Max-min PCO2 difference | 20.7 (13.4; 28.1) | 29.1 (22.4; 40.2) | <0.001 |
| Hypercapnia | 47 (72.3%) | 62 (89.9%) | 0.009 |
| Hypocapnia | 60 (92.3%) | 65 (94.2%) | 0.739 |
| Death or Severe brain injury model | ||
| Predictor | OR (95%) | p-value |
| Gestational age < 28 weeks | 22.5 (8.5-68.7) | <0.001 |
| Air-leak syndromes | 4.6 (1.3-17.3) | 0.018 |
| Pulmonary hemorrhage | 3.8 (1.1-15.8) | 0.046 |
| Base Deficit (absolute value) | 1.2 (1-1.4) | 0.022 |
| Severe brain injury model | ||
| Predictor | OR (95%) | p-value |
| Gestational age < 28 weeks | 20.6 (7.7-63.7) | <0.001 |
| Air-leak syndromes | 6.2 (1.8-23.8) | 0.005 |
| Pulmonary hemorrhage | 4.5 (1.4-15.8) | 0.012 |
| Male sex | 2.6 (1-7.1) | 0.052 |
| BPD model for survivors | ||
| Predictor | OR (95%) | p-value |
| Gestational age < 28 weeks | 9.2 (1.4-182.1) | 0.043 |
| Treated PDA | 5.5 (1.2-39.9) | 0.066 |
| Hypercapnia | 3.4 (1.1-11.5) | 0.025 |
Disclaimer/Publisher’s Note: The statements, opinions and data contained in all publications are solely those of the individual author(s) and contributor(s) and not of MDPI and/or the editor(s). MDPI and/or the editor(s) disclaim responsibility for any injury to people or property resulting from any ideas, methods, instructions or products referred to in the content. |
© 2026 by the authors. Licensee MDPI, Basel, Switzerland. This article is an open access article distributed under the terms and conditions of the Creative Commons Attribution (CC BY) license (http://creativecommons.org/licenses/by/4.0/).




